VentilatorAssociated Event VAESurveillance What Does It Mean BJ

Ventilator-Associated Event (VAE)Surveillance What Does It Mean? BJ HELTON, MPH, CIC MANAGER PATIENT SAFETY &QUALITY COVENANT HEALTHCARE

After this session, you will be able to— Discuss the ramifications of ventilatorassociated events (VAEs) Describe methods to evaluate VAEs Understand the implications of objective VAE surveillance Identify ways to use data to drive improvement LEARNING OBJECTIVES AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 2

Affects ~5 -10% of ventilated patients Increases ICU length of stay by ~4 -7 days Increases hospital length of stay by ~14 days Crude mortality rate 30 -50% Attributable Adds mortality 8 -12% ~$10 -50, 000 to cost of hospital stay VENTILATOR-ASSOCIATED PNEUMONIA AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 3

AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 4

Many complications of critical care present with subjective clinical signs that mimic VAP: Radiographic opacities Fever Abnormal Impaired white blood cell count oxygenation Increased pulmonary secretions THE CHALLENGE OF VAP DIAGNOSIS AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 5

AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 6

Collecting Connect VAE data can be used to— the dots to harm Avoid failure of infection prevention efforts due to “silo mentality” View interventions under the larger context of patient safety WHY COLLECT VAE DATA? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 7

A retrospective cohort study examining 20, 356 episodes of mechanical ventilation (MV)1 VAEs 1, 141 ventilator-associated conditions (VACs) 431 infection-related VACs (IVACs) 266 possible cases of ventilator-associated pneumonia (PVAP) Patients with a VAE have— More days to extubation More days to discharge Higher mortality rate WHY DO I WANT TO KNOW ABOUT VACS AND IVACS? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 8

CONNECT THE SAFETY DOTS Immobility Atelectasis Morbidity Ventilator Harm Pulmonary edema (PE) VAC Acute respiratory distress syndrome (ARDS) AHRQ Safety Program for Mechanically Ventilated Patients Mortality Increased length of stay (LOS) IVAC Antibiotic resistance Cost VAP Clostridium difficile colitis VAE Surveillance 9

Screening ventilator settings for VAC captures a similar set of complications to traditional VAP surveillance but is faster, more objective, and a superior predictor of outcomes. 2 Objective surveillance definitions that include quantitative evidence of respiratory deterioration after a period of stability strongly predict increased LOS and hospital mortality. 3 WHY USE THE NEW VAE SURVEILLANCE DEFINITIONS? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 10

• One of the main reasons is interrater reliability. This occurs when two people separately look at the same set of criteria and do, or don’t, come up with the same conclusion • Criteria are subjective, leading to disagreement between reviewers ) WHY THE CHANGE? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 11

Broaden the focus Shifting focus of surveillance from pneumonia alone to complications in general emphasizes the importance of preventing all complications of MV, not just pneumonia When definitions are objective, caregivers can focus on what went wrong rather than debate the definition WHY THE SHIFT? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 12

The definition of VAE is intentionally broader than traditional VAP surveillance Common VACs: ARDS PE Thromboembolic disease Sepsis Clinical ramifications? Respiratory deterioration in previously stable patients is a risk factor for increased morbidity and mortality BROADENING THE SURVEILLANCE AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 13

Multicenter, retrospective study Evaluated a novel surveillance paradigm for VACs: screening ventilator settings Blinded critical care physician reviewed 52 randomly selected patients with VAC (defined by protocol) or VAP (determined by IPs based on VAP definition) Screening ventilator settings for VAC captures a similar set of complications to traditional VAP surveillance ANALYSIS OF VAC VS. VAP 2 AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 14
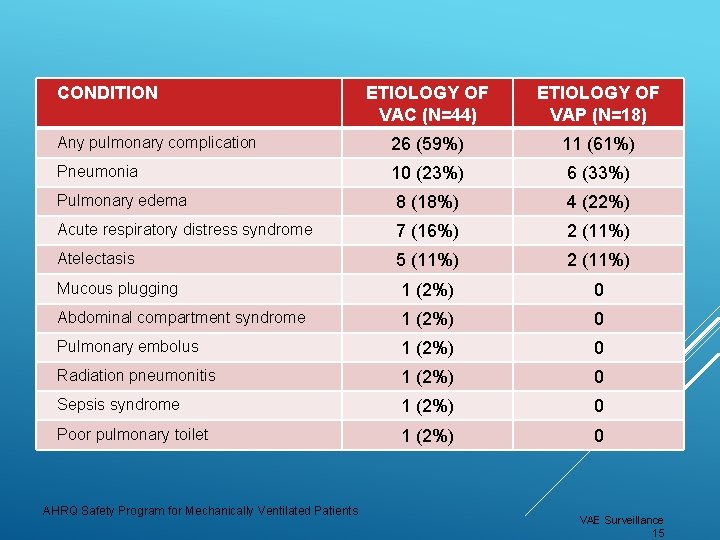
CONDITION ETIOLOGY OF VAC (N=44) ETIOLOGY OF VAP (N=18) Any pulmonary complication 26 (59%) 11 (61%) Pneumonia 10 (23%) 6 (33%) Pulmonary edema 8 (18%) 4 (22%) Acute respiratory distress syndrome 7 (16%) 2 (11%) Atelectasis 5 (11%) 2 (11%) Mucous plugging 1 (2%) 0 Abdominal compartment syndrome 1 (2%) 0 Pulmonary embolus 1 (2%) 0 Radiation pneumonitis 1 (2%) 0 Sepsis syndrome 1 (2%) 2 ANALYSIS OF VAC VS. VAP Poor pulmonary toilet 1 (2%) AHRQ Safety Program for Mechanically Ventilated Patients 0 0 VAE Surveillance 15

Many providers feel some of the conditions associated with VAEs are pre-existing Preliminary data from the first year of VAE data collection showed approximately 79 percent of VAEs were in patients who were either on MV for ≥ 5 days or in the hospital for ≥ 5 days at the time of VAE onset 6 Time to onset data suggest that the majority of VAEs are likely hospital-associated based on previous criteria 7, 8 ARE VAES PREVENTABLE? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 16

Strategies to Prevent Ventilator. Associated Pneumonia in Acute Care Hospitals: 2014 Update 9 Contributions from— Society of Healthcare Epidemiology of America Infectious Diseases Society of American Hospital Association for Professionals in Infection Control and Epidemiology The Joint Commission PREVENTION STRATEGIES AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 17
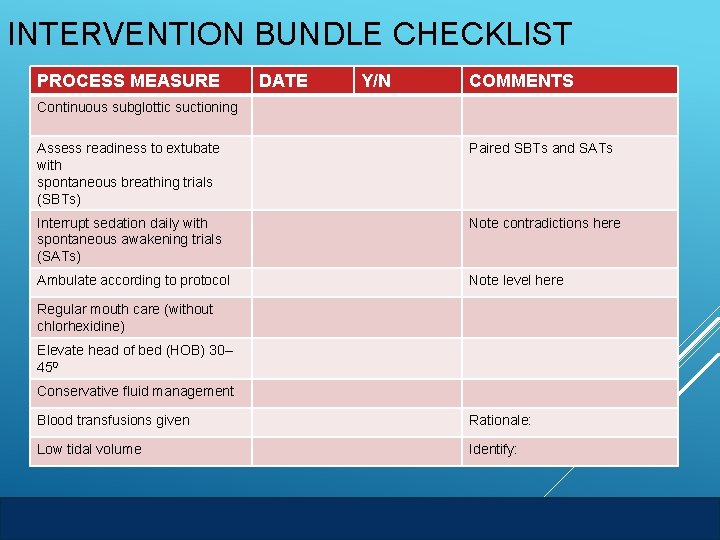
INTERVENTION BUNDLE CHECKLIST PROCESS MEASURE DATE Y/N COMMENTS Continuous subglottic suctioning Assess readiness to extubate with spontaneous breathing trials (SBTs) Paired SBTs and SATs Interrupt sedation daily with spontaneous awakening trials (SATs) Note contradictions here Ambulate according to protocol Note level here Regular mouth care (without chlorhexidine) Elevate head of bed (HOB) 30– 450 Conservative fluid management Blood transfusions given Rationale: Low tidal volume Identify: AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 18

RECOMMENDATION INTERVENTION Basic practice • • Use noninvasive positive pressure ventilation in selected populations Manage patients without sedation whenever possible Interrupt sedation daily Assess readiness to extubate daily Perform SATs with sedatives turned off Facilitate early mobility Use endotracheal tubes with subglottic secretion drainage ports for patients expected to require greater than 48 or 72 hours of MV Change the ventilator circuit only if visibly soiled or malfunctioning Elevate HOB to 30– 45° • • Select oral or digestive decontamination Regular oral care with chlorhexidine Prophylactic probiotics Ultrathin polyurethane endotracheal tube cuffs Automated control of endotracheal tube cuff pressure Saline instillation before tracheal suctioning Mechanical tooth brushing • • • Silver-coated endotracheal tubes Kinetic beds Prone positioning • • Special approaches BEST PRACTICES FOR VAE REDUCTION Generally not recommended AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 19

Routine oral care with chlorhexidine 10 Prevents nosocomial pneumonia in cardiac surgery patients May not decrease VAP risk in noncardiac surgery patients Does not affect— Mortality Duration of MV Intensive care unit (ICU) LOS WHAT ABOUT ORAL CARE WITH CHLORHEXIDINE? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 20
AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 21

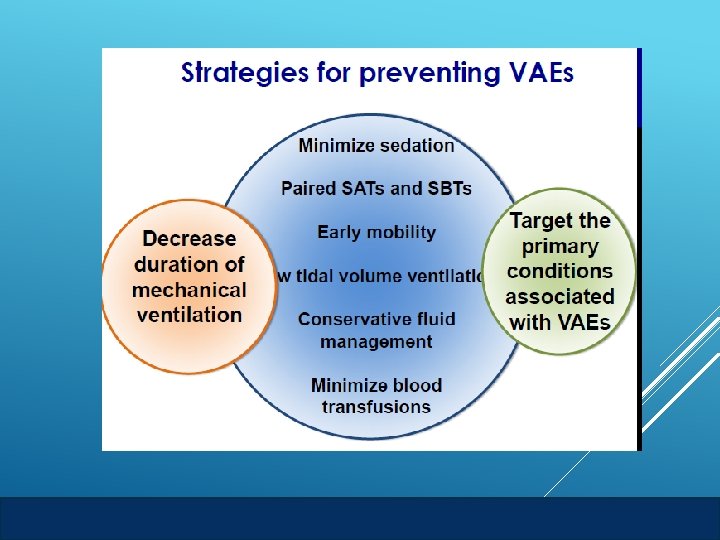
Prevent pneumonia by implementing HOB elevation Avoid pulmonary complications through fluid conservation Protect against atelectasis by managing sedation Combat acute lung injury by following a low tidal volume ventilation strategy VAE PREVENTION TECHNIQUES AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 22

Where to start? 1. Look at both process and outcome measures 2. Track your own performance over time 3. Do we see improvements? GETTING STARTED ON PREVENTION AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 23
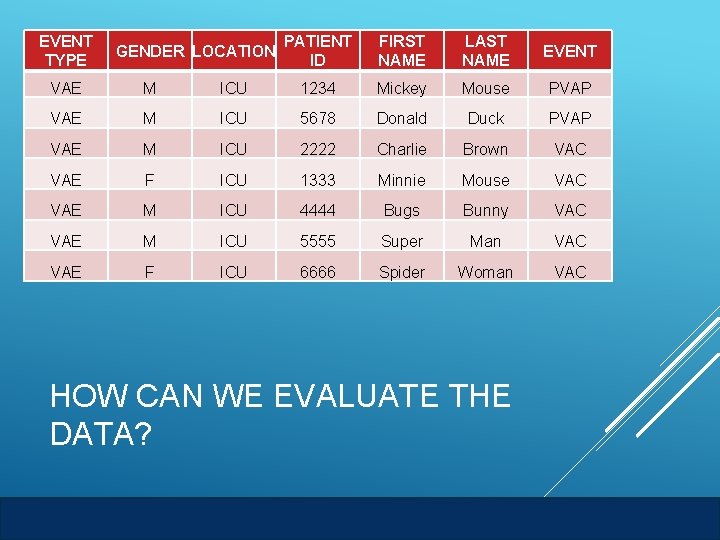
EVENT TYPE GENDER LOCATION PATIENT ID FIRST NAME LAST NAME EVENT VAE M ICU 1234 Mickey Mouse PVAP VAE M ICU 5678 Donald Duck PVAP VAE M ICU 2222 Charlie Brown VAC VAE F ICU 1333 Minnie Mouse VAC VAE M ICU 4444 Bugs Bunny VAC VAE M ICU 5555 Super Man VAC VAE F ICU 6666 Spider Woman VAC HOW CAN WE EVALUATE THE DATA? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 24

Review both individual cases and system level issues Develop a form to help analyze individual cases Do we have policies and procedures in place? Do we follow evidence-based guidelines? Are we consistent with our practices? HOW WILL I USE MY DATA TO DRIVE IMPROVEMENT? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 25

Patient develops a VAC Chronic ventilator dependency Ambulation protocols were not implemented Not monitored for dehydration Presence of sputum not documented Lack of communication between nursing and respiratory groups REVIEW ALL VAC CASES–CASE REVIEW 1 AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 26

Ms. X is a 76 -year-old woman, admitted to the ICU with septic shock requiring large volume fluid resuscitation Intubated and placed on ventilator Stable until day 6 when she has progressive oxygenation demands Increased demands last for 72 hours CASE REVIEW 2 AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 27

Patient has a VAC No fever No increased white blood cell count No new antibiotics Diagnosis: Pulmonary edema Opportunities for improvement? CASE REVIEW 2 – OUTCOMES AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 28

In an example ICU, many VAEs are PVAPs Evaluation Head of bed monitoring Suctioning frequency SATs Endotracheal tubes with subglottic suctioning CASE REVIEW 3 AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 29

Analysis Quarter 4 VACs 16 0 1: 20 VACs IVACs PVAPs Most are other healthcareacquired infections CASE REVIEW 3 – OUTCOMES AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 30

• Hardwire ambulation protocols • Ensure documentation of secretions • Work collaboratively with respiratory therapists to identify subtle changes • Daily huddles OPPORTUNITIES FOR IMPROVEMENT AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 31

Surveillance is a critical component of every quality improvement effort; you cannot prevent it if you cannot measure it. KNOW YOUR DATA AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 32

VAEs are associated with increased mortality and ICU and hospital LOS In randomized controlled trials, VAP interventions have been shown to improve objective outcomes, such as duration of MV, ICU or hospital LOS, mortality, and costs The existing VAP prevention literature is the best available guide to improving outcomes for ventilated patients It is important to continue monitoring the processes of care and the outcomes for mechanically ventilated patients Always give feedback to providers and assess the potential for preventable events THE BOTTOM LINE AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 33

RT’s stepping up and taking an active roll Properly assessing and identifying patients at risk for retained secretions Providing Patient Education Ensuring proper follow-up after discharge Assessment of needs at discharge Effective Communication with: Discharge Planner Nursing Physician PT / OT Homecare /transitional care RT DME companies / vendors ROLE OF RESPIRATORY THERAPY IN READMISSIONS AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 34

I HAD TO……… AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 35

QUESTIONS? AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 36

1. Klompas M, Kleinman K, Murphy MV. Descriptive epidemiology and attributable morbidity of ventilator-associated events. Infect Control Hosp Epidemiol. 2014 May; 35(5): 502 -10. PMID: 24709718. 2. Klompas M, Khan Y, Kleinman K, et al. Multicenter evaluation of a novel paradigm for complications of mechanical ventilation. PLo. S One. 2011 Mar 22; 6(3): e 18062. PMID: 21445364. 3. Klompas M, Magill S, Robicsek A, et al. Objective surveillance definitions for ventilator-associated pneumonia. Crit Care Med. 2012 Dec; 40(12): 3154 -61. PMID: 22990454. Klompas M. Interobserver variability in ventilator-associated pneumonia surveillance. Am J Infect Control. 2010 Apr; 38(3): 237 -9. PMID: 20171757. 5. Rogers E. Diffusion of innovation, 5 th ed. New York, NY: Simon and Schuster; 2003. REFERENCES AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 37

6. Magill S, Gross C, Edwards JR. Characteristics of ventilator-associated events reported to the National Healthcare Safety Network in 2013. Oral abstract presented at the meeting of IDWeek, Philadelphia, PA, October 2014. 7. Klompas M. Complications of mechanical ventilation – the CDC’s new surveillance paradigm. N Engl J Med. 2013 Apr 18; 368(16): 1472 -5. PMID: 23594002. 8. Muscedere J, Sinuff T, Heyland DK, et al. The clinical impact and preventability of ventilator-associated conditions in critically ill patients who are mechanically ventilated. Chest. 2013 Nov; 144(5): 1453 -60. PMID: 24030318. 9. Klompas M, Branson R, Eichenwald EC, et al. Strategies to preventilatorassociated pneumonia in acute care hospitals: 2014 update. Infect Control Hosp Epidemiol. 2014 Aug; 35(8): 915 -36. PMID: 25026607. 10. Klompas M, Speck K, Howell MD, et al. Reappraisal of routine oral care with chlorhexidine gluconate for patients receiving mechanical ventilation: systematic review and meta-analysis. JAMA Intern Med. 2014 May; 174(5): 751 -61. PMID: 24663255. REFERENCES AHRQ Safety Program for Mechanically Ventilated Patients VAE Surveillance 38
- Slides: 38