Ventilator Waveforms Basic Interpretation and Analysis Vivek Iyer

Ventilator Waveforms: Basic Interpretation and Analysis Vivek Iyer MD, MPH Steven Holets, RRT CCRA Rolf Hubmayr, MD Edited for ATS by: Cameron Dezfulian, MD

Outline of this presentation • Goal: – To provide an introduction to the concept of ventilator waveform analysis in an interactive fashion. • Content: – Outline of types of ventilatory waveforms. – Introduction to respiratory mechanics and the ‘Equation Of Motion’ for the respiratory system – Development of the concept of ventilator waveforms – Illustrations and videos of waveforms to illustrate their practical applications and usefulness.
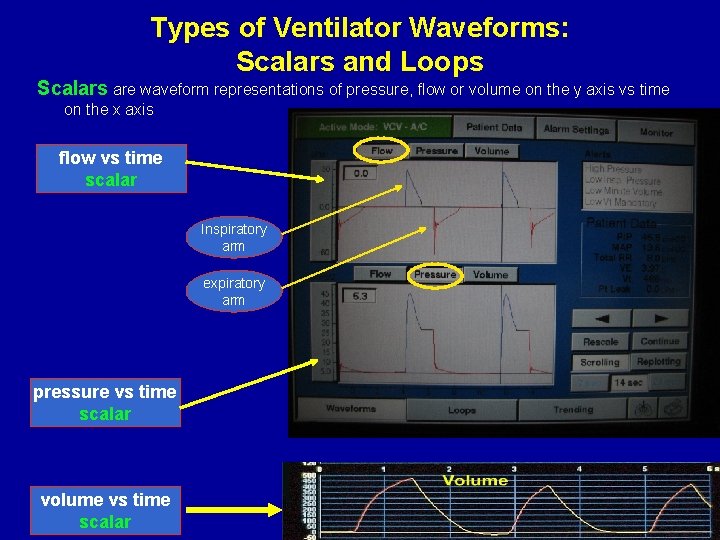
Types of Ventilator Waveforms: Scalars and Loops Scalars are waveform representations of pressure, flow or volume on the y axis vs time on the x axis flow vs time scalar Inspiratory arm expiratory arm pressure vs time scalar volume vs time scalar
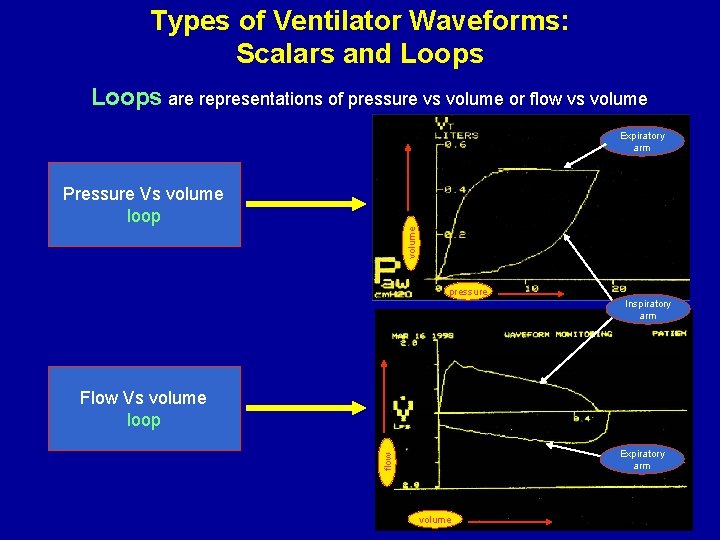
Types of Ventilator Waveforms: Scalars and Loops are representations of pressure vs volume or flow vs volume Expiratory arm volume Pressure Vs volume loop pressure Inspiratory arm Flow Vs volume loop flow Expiratory arm volume

Understanding the flow-time waveform • There are two components to the flow-time waveform – The inspiratory arm: • Active in nature • The character is determined by the ventilatory flow settings. – The expiratory arm: • Passive in nature • The character is determined mainly by elastic recoil of the patients lungs and airway resistance. • Also affected by patient respiratory effort (if any) • There are two commonly used types of flow patterns available on most ventilators – The ‘square wave’ or ‘constant flow’ pattern – The ‘ramp’ (decelerating) type pattern
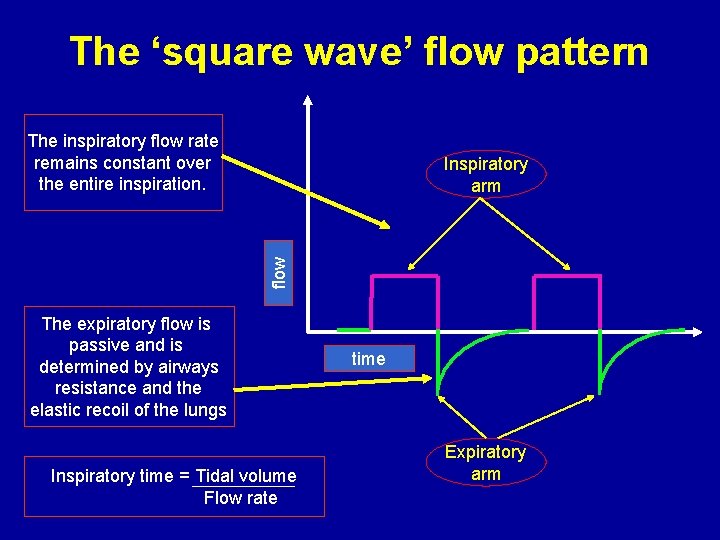
The ‘square wave’ flow pattern The inspiratory flow rate remains constant over the entire inspiration. flow Inspiratory arm The expiratory flow is passive and is determined by airways resistance and the elastic recoil of the lungs Inspiratory time = Tidal volume Flow rate time Expiratory arm
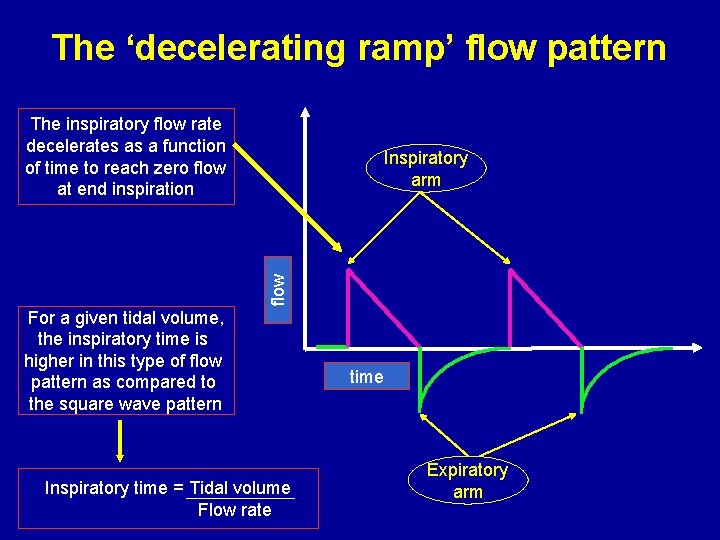
The ‘decelerating ramp’ flow pattern The inspiratory flow rate decelerates as a function of time to reach zero flow at end inspiration flow Inspiratory arm For a given tidal volume, the inspiratory time is higher in this type of flow pattern as compared to the square wave pattern Inspiratory time = Tidal volume Flow rate time Expiratory arm

Now let us try to understand the following in the next few slides • A basic ventilator circuit diagram • Airway pressures • The equation of motion for the respiratory system • The pressure-time waveform
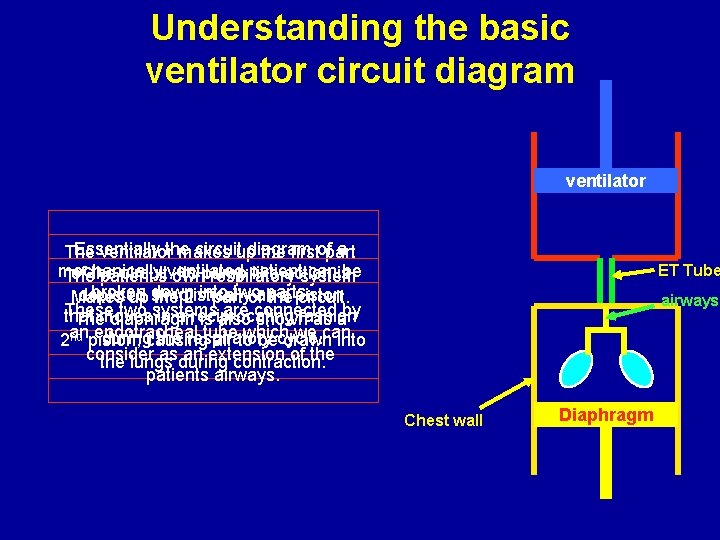
Understanding the basic ventilator circuit diagram ventilator Essentially circuitup diagram a The ventilatorthe makes the firstofpart mechanically patient canisbe of the circuit. ventilated Its pump like action The patient’s own respiratory system broken down two depicted a piston Makes up simplistically the 2 ndinto part ofasparts…. . the circuit. These two systems are connected that in a reciprocating fashion Themoves diaphragm is also shown as aby endotracheal tube which we can nd piston; duringcausing the respiratory 2 an air to becycle. drawn into consider as an extension of the lungs during contraction. patients airways. ET Tube airways Chest wall Diaphragm
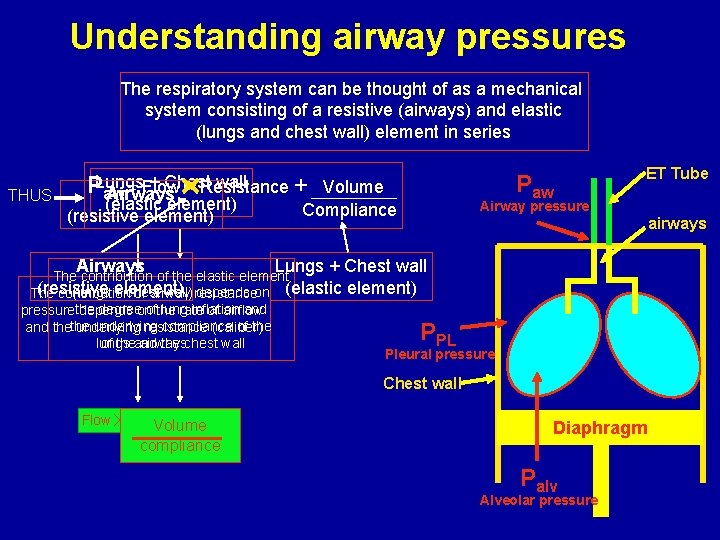
Understanding airway pressures The respiratory system can be thought of as a mechanical system consisting of a resistive (airways) and elastic (lungs and chest wall) element in series Airways ET Tube Paw Lungs + Chest wall P = Flow Resistance + Volume aw Airways THUS (elastic element) Compliance (resistive element) Airway pressure Lungs + Chest wall element) The contribution of the elastic element (resistive element) (lungs + chest wall) resistance depends on (elastic The contribution of airway degreeonofthe lung inflation and pressurethe depends rate of airflow underlying compliance of the and thethe underlying resistance (caliber) lungs the chest wall of theand airways PPL Pleural pressure Chest wall Flow resistance Volume compliance Diaphragm Palv Alveolar pressure airways
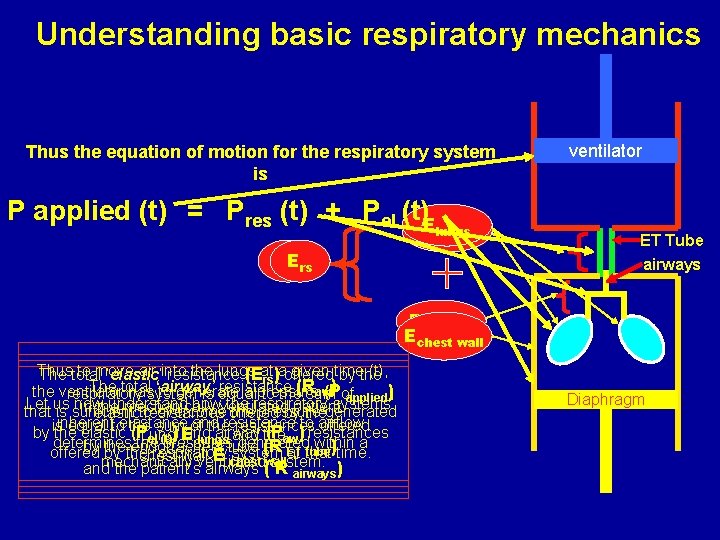
Understanding basic respiratory mechanics Thus the equation of motion for the respiratory system is P applied (t) = Pres (t) + Pel (t)E lungs RET tube Raw Ers ventilator ET Tube airways Rairways Echest wall Thus to move air into the lungs a given time (t), The total ‘elastic’ resistance (Eat rs) offered by the The total ‘airway’ resistance ) of aw the ventilator hassystem to generate a pressure (P respiratory is equal to the(R sum applied) Let us now understand how the respiratory systems’ in the mechanically ventilated patient that is sufficient overcome offered the pressure elasticto resistances by thegenerated inherent elastance and resistance to airflow is equal to the sum of the resistances offered by the elastic (PLung ) Eand airway ( P ) resistances and the el (t) aw lungs generated within a determines the pressures by the endotracheal tube (R ET tube)time. offered by the respiratory system at that chest wall E chest wall mechanically and the patient’sventilated airways (system. R airways) Diaphragm
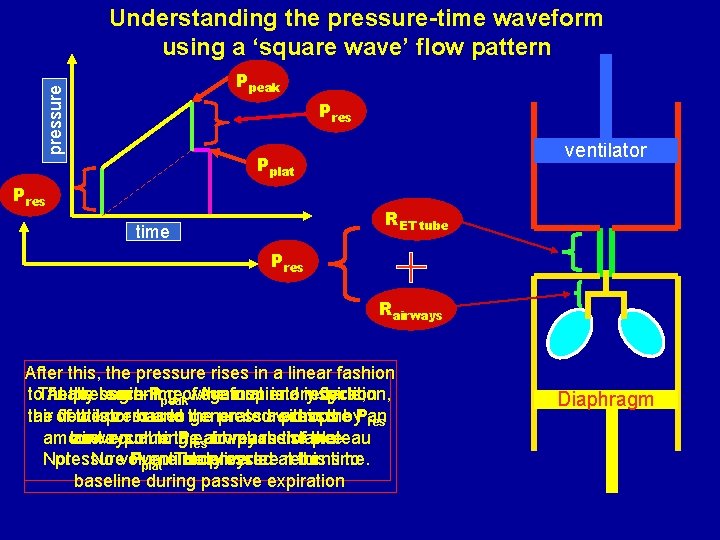
Understanding the pressure-time waveform using a ‘square wave’ flow pattern pressure Ppeak Pres ventilator Pplat Pres RET tube time Pres Rairways After this, the pressure rises in a linear fashion to. The finally reach Ppeakof. Again at end inspiration, At the pressure-time beginning waveform the inspiratory is a reflection cycle, air of flow zero and pressure drops by. Pan the ventilator theispressures has to the generated awithin pressure the res amount to airways overcome equal during to the Pres each airway to reach phase resistance. the of the plateau Note: pressure No volume Pventilatory is delivered pressure cycle. at returns this time. to plat. The baseline during passive expiration Diaphragm
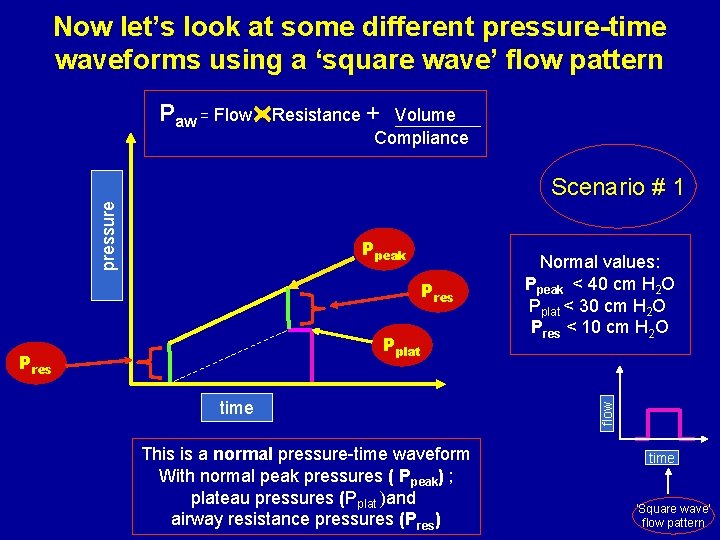
Now let’s look at some different pressure-time waveforms using a ‘square wave’ flow pattern Paw = Flow Resistance + Volume Compliance Ppeak Pres Pplat Pres time This is a normal pressure-time waveform With normal peak pressures ( Ppeak) ; plateau pressures (Pplat )and airway resistance pressures (Pres) Normal values: Ppeak < 40 cm H 2 O Pplat < 30 cm H 2 O Pres < 10 cm H 2 O flow pressure Scenario # 1 time ‘Square wave’ flow pattern
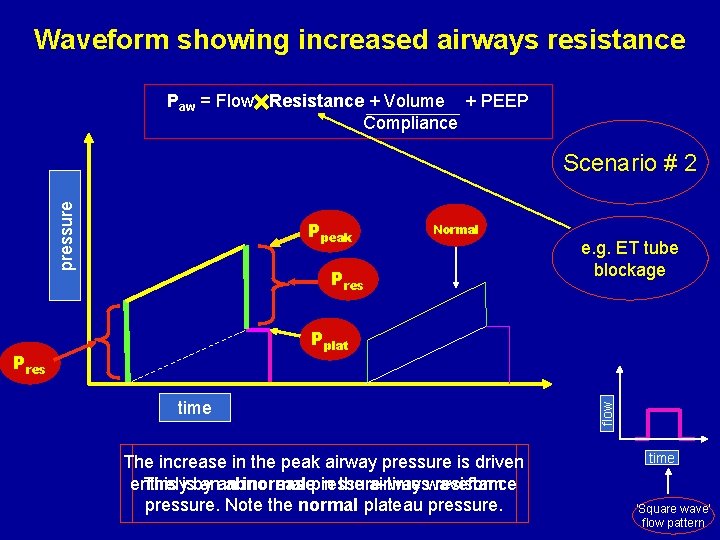
Waveform showing increased airways resistance Paw = Flow Resistance + Volume + PEEP Compliance pressure Scenario # 2 Ppeak Normal Pres e. g. ET tube blockage Pres time The increase in the peak airway pressure is driven entirely This isby anan abnormal increasepressure-time in the airwayswaveform resistance pressure. Note the normal plateau pressure. flow Pplat time ‘Square wave’ flow pattern
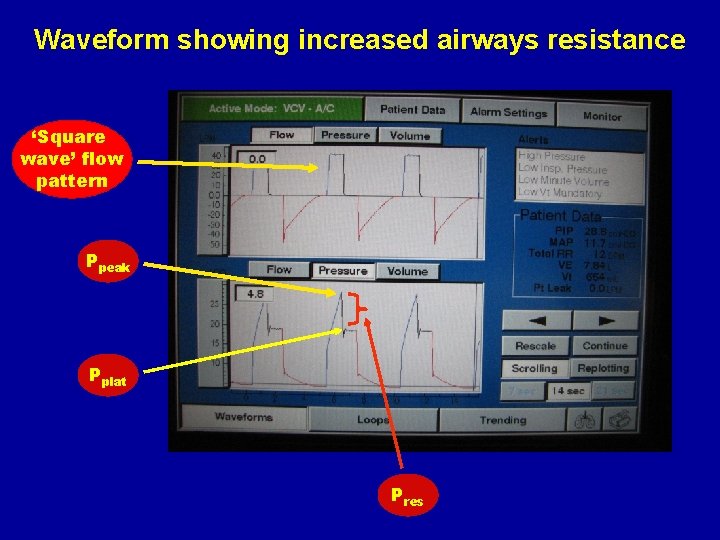
Waveform showing increased airways resistance ‘Square wave’ flow pattern Ppeak Pplat Pres
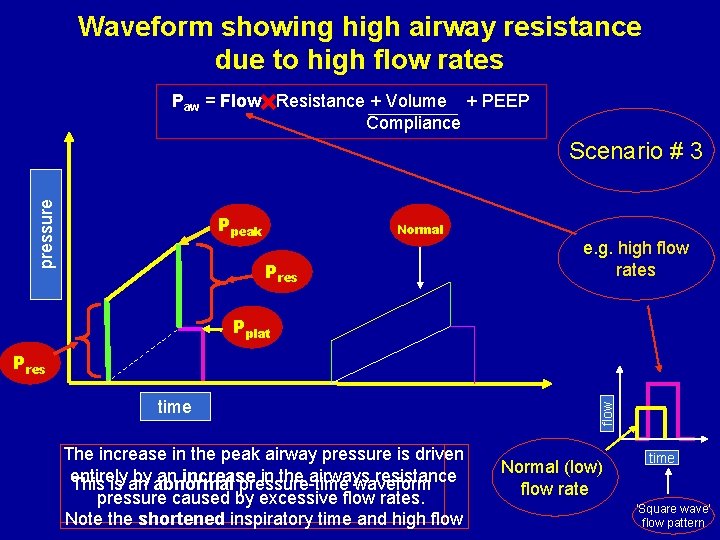
Waveform showing high airway resistance due to high flow rates Paw = Flow Resistance + Volume + PEEP Compliance pressure Scenario # 3 Ppeak Normal Pres e. g. high flow rates Pplat time The increase in the peak airway pressure is driven entirely by abnormal an increase in the airways resistance This is an pressure-time waveform pressure caused by excessive flow rates. Note the shortened inspiratory time and high flow Pres Normal (low) flow rate time ‘Square wave’ flow pattern
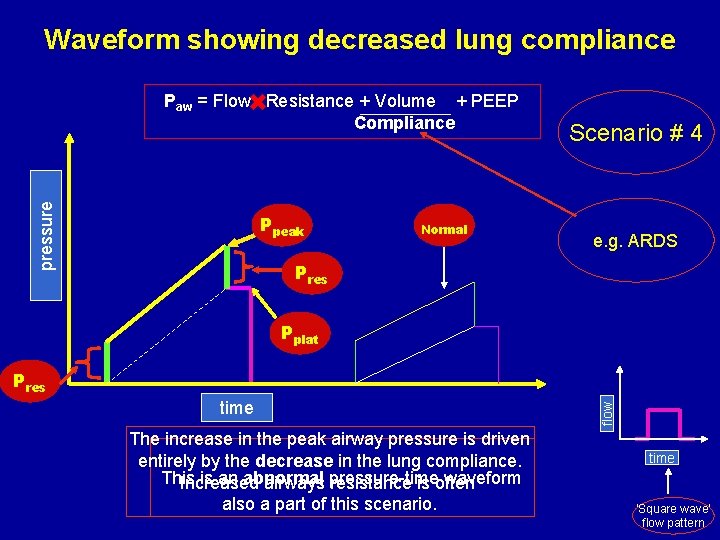
Waveform showing decreased lung compliance pressure Paw = Flow Resistance + Volume + PEEP Compliance Ppeak Normal Scenario # 4 e. g. ARDS Pres Pplat time The increase in the peak airway pressure is driven entirely by the decrease in the lung compliance. This is an abnormal waveform Increased airways pressure-time resistance is often also a part of this scenario. flow Pres time ‘Square wave’ flow pattern

Waveform showing decreased lung compliance ‘Square wave’ flow pattern Ppeak Pplat Pres
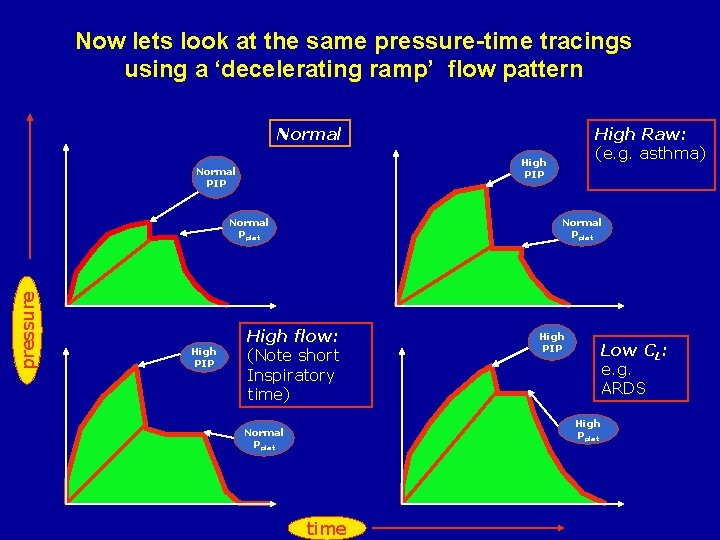
Now lets look at the same pressure-time tracings using a ‘decelerating ramp’ flow pattern Normal High PIP Normal PIP pressure Normal Pplat High PIP High Raw: (e. g. asthma) Normal Pplat High flow: (Note short Inspiratory time) High PIP Low CL: e. g. ARDS High Pplat Normal Pplat time

Now let us try to understand the practical aspects of ventilator waveform analysis in an interactive fashion.

Clinical applications of ventilator waveform analysis • Ventilator waveforms can be very useful in many different situations including: – – – Diagnosing a ventilator that is ‘alarming’ Detecting obstructive flow patterns on the ventilator Detecting air trapping and dynamic hyperinflation Detecting lung overdistention Detecting respiratory circuit secretion build-up Detecting patient-ventilator interactions • • Dyssynchrony Double triggering Wasted efforts Flow starvation

Some ventilators with waveform displays Puritan Bennett 840 Puritan Bennett 7200 Siemens Servo 300 A Bear 1000 series Dräger Evita XL Respironics Esprit
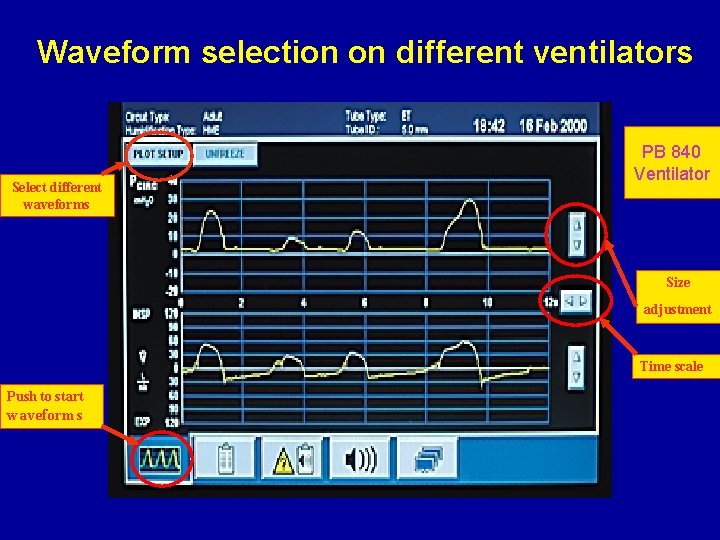
Waveform selection on different ventilators Select different waveforms PB 840 Ventilator Size adjustment Time scale Push to start waveforms
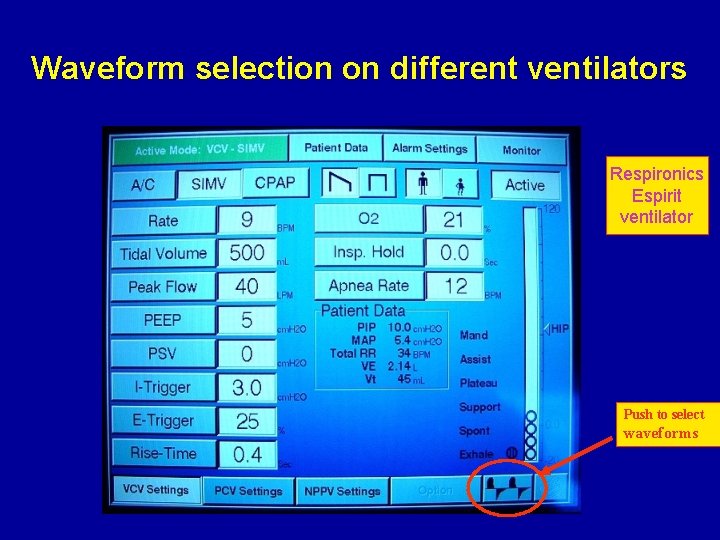
Waveform selection on different ventilators Respironics Espirit ventilator Push to select waveforms

Waveform selection on different ventilators Switch between waveforms Respironics Espirit ventilator Press to adjust size Switch between Loops and scalars
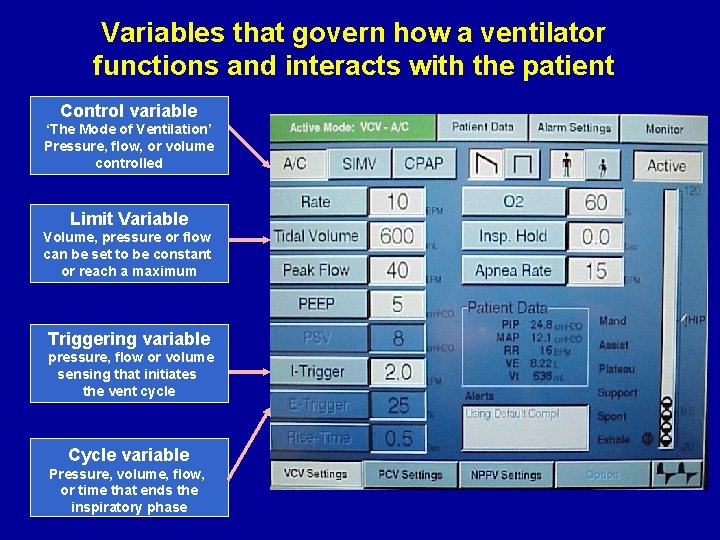

Variables that govern how a ventilator functions and interacts with the patient Control variable ‘The Mode of Ventilation’ Pressure, flow, or volume controlled Limit Variable Volume, pressure or flow can be set to be constant or reach a maximum Triggering variable pressure, flow or volume sensing that initiates the vent cycle Cycle variable Pressure, volume, flow, or time that ends the inspiratory phase

So what waveforms should I be observing and analyzing? Look at the waveforms that are varying based on the settings you have ordered
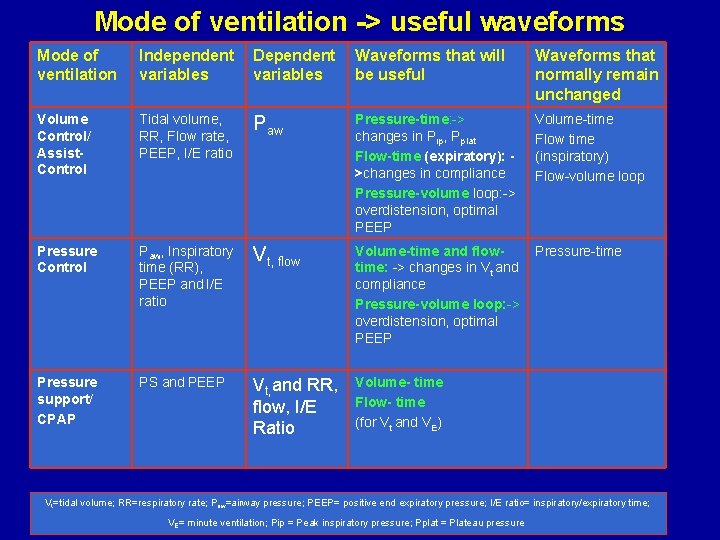
Mode of ventilation -> useful waveforms Mode of ventilation Independent variables Dependent variables Waveforms that will be useful Waveforms that normally remain unchanged Volume Control/ Assist. Control Tidal volume, RR, Flow rate, PEEP, I/E ratio Paw Pressure-time: -> changes in Pip, Pplat Flow-time (expiratory): >changes in compliance Pressure-volume loop: -> overdistension, optimal PEEP Volume-time Flow time (inspiratory) Flow-volume loop Pressure Control Paw, Inspiratory time (RR), PEEP and I/E ratio Vt, flow Volume-time and flowtime: -> changes in Vt and compliance Pressure-volume loop: -> overdistension, optimal PEEP Pressure-time Pressure support/ CPAP PS and PEEP Vt, and RR, flow, I/E Ratio Volume- time Flow- time (for Vt and VE) Vt=tidal volume; RR=respiratory rate; Paw=airway pressure; PEEP= positive end expiratory pressure; I/E ratio= inspiratory/expiratory time; VE= minute ventilation; Pip = Peak inspiratory pressure; Pplat = Plateau pressure

Waveforms to observe during volume assist control ventilation • Pressure-time waveform: – Affected by patient effort and changes in resistance and compliance • Flow-time waveform: – Expiratory flow is not fixed, waveform is dependent on elastic recoil pressure of respiratory system/patient effort – Therefore this scalar is nearly always of interest

Waveforms to observe during pressure targeted ventilation: PCV • Pressure-time waveform usually will not change • Flow-time and volume-time waveform will be affected by changes in compliance, resistance and the patient’s respiratory muscle strength (independent variables)

Now let us begin riding the ‘waves’ by looking at a few ventilator waveforms!
Basic ventilator waveforms Mode of ventilation: Assist/control – square wave flow – Airway pressures: dependent on lung compliance, tidal volume and flow (dependent variable) – Tidal volumes, respiratory rate: ventilator controlled – Flow pattern: ventilator controlled (square wave pattern) – Inspiratory time: ventilator controlled – Waveforms shown: flow-time and pressure-time
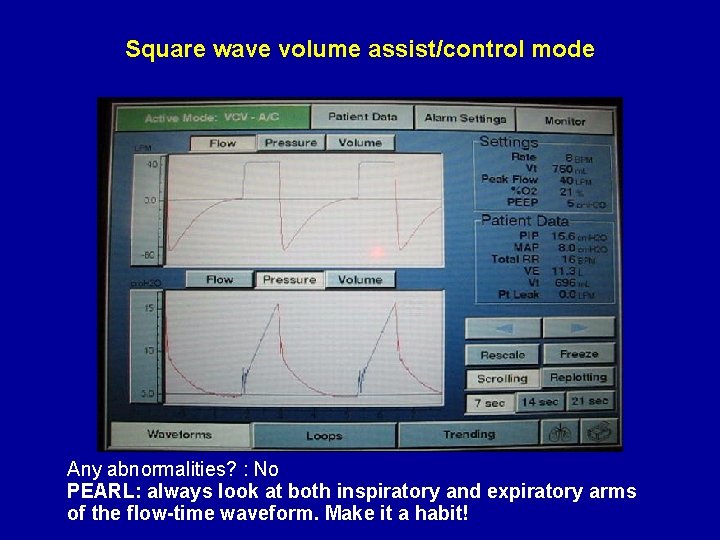
Square wave volume assist/control mode Any abnormalities? : No PEARL: always look at both inspiratory and expiratory arms of the flow-time waveform. Make it a habit!

Basic ventilator waveforms Mode of ventilation: Assist/control – decelerating flow pattern – Airway pressures: dependent on lung compliance, tidal volume and flow (dependent variable) – Tidal volumes, respiratory rate: ventilator controlled – Flow pattern: ventilator controlled (decelerating wave pattern) – Inspiratory time: ventilator controlled – Waveforms shown: flow-time and pressure-time
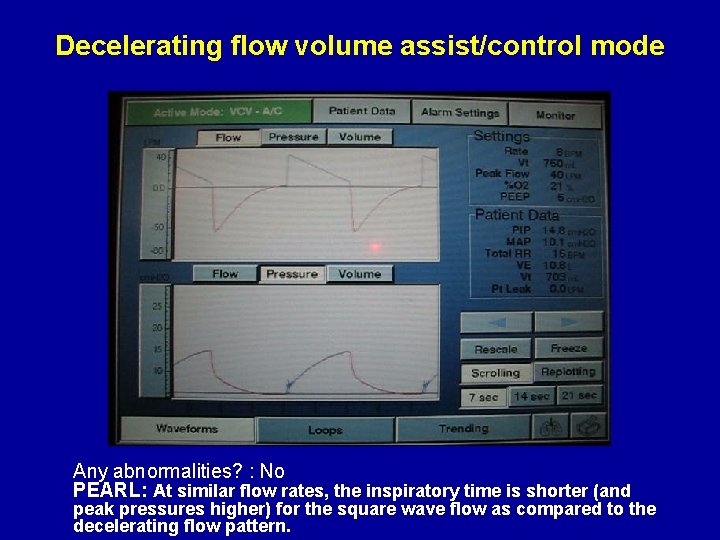
Decelerating flow volume assist/control mode Any abnormalities? : No PEARL: At similar flow rates, the inspiratory time is shorter (and peak pressures higher) for the square wave flow as compared to the decelerating flow pattern.
Basic ventilator waveforms Mode of ventilation: CPAP + PS – Airway pressures: patient controlled (indirectly through control of volume and flow) – Flow pattern: patient controlled – Inspiratory time, respiratory rate: patient controlled – Waveforms shown: flow-time and volume-time
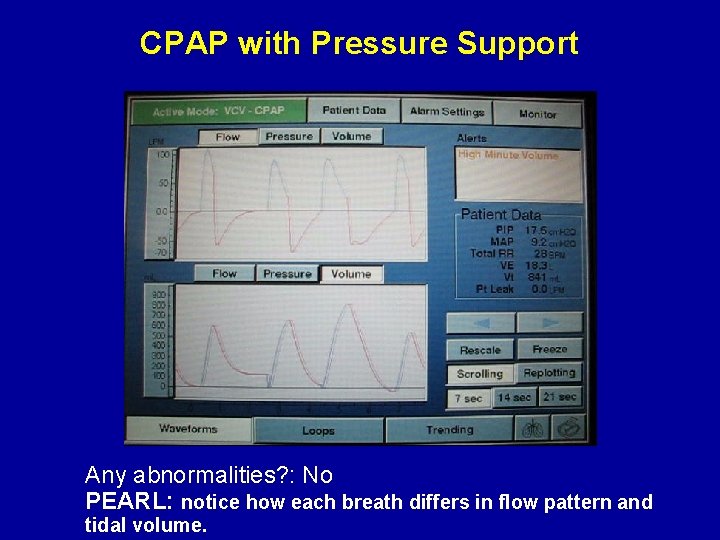
CPAP with Pressure Support Any abnormalities? : No PEARL: notice how each breath differs in flow pattern and tidal volume.

Basic ventilator waveforms Mode of ventilation: pressure control ventilation (PCV) – – – Airway pressures: ventilator controlled Respiratory rate: ventilator controlled Tidal Volumes: dependent variable (lung compliance) Flow rates: ventilator controlled (decelerating in this instance) Waveforms shown: flow-time and volume-time
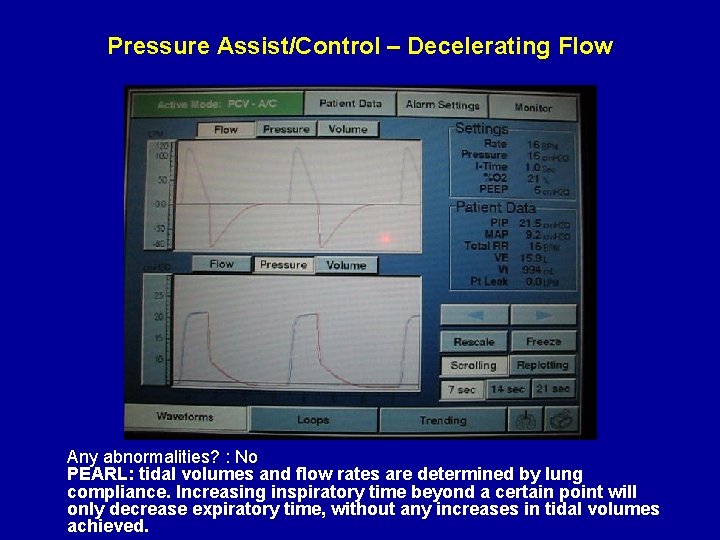
Pressure Assist/Control – Decelerating Flow Any abnormalities? : No PEARL: tidal volumes and flow rates are determined by lung compliance. Increasing inspiratory time beyond a certain point will only decrease expiratory time, without any increases in tidal volumes achieved.

Let us now shift gears and see how waveforms can help us recognize some common ventilator related problems! Common problems that can be diagnosed by analyzing Ventilator waveforms Abnormal ventilatory Parameters/lung mechanics E. g. . Overdistension, Auto PEEP COPD Patient-ventilator Interactions E. g. flow starvation, Double triggering, Wasted efforts Active expiration Ventilatory circuit related problems E. g. auto cycling and Secretion build up in the Ventilatory circuit
Now let us learn to recognize Lung overdistension and the development of Auto PEEP Abnormal ventilatory Parameters/lung mechanics E. g. . Overdistension, Auto PEEP COPD Patient-ventilator Interactions E. g. flow starvation, Double triggering, Wasted efforts Active expiration Ventilatory circuit related problems E. g. auto cycling and Secretion build up in the Ventilatory circuit

Let us briefly revisit the flow-time waveform • As previously noted, the flow-time waveform has both an inspiratory and an expiratory arm. • The expiratory arm is passive in nature and its character is determined by: – the elastic recoil of the lungs – the airways resistance – and any respiratory muscle effort made by the patient during expiration (due to patient-ventilator interaction/dys=synchrony) • The expiratory arm can be thought of in some ways as passive bedside spirometry. • It should always be looked at as part of any waveform analysis and can be diagnostic of various conditions like COPD, auto-PEEP, wasted efforts, overdistention etc.

Recognizing Lung Overdistension
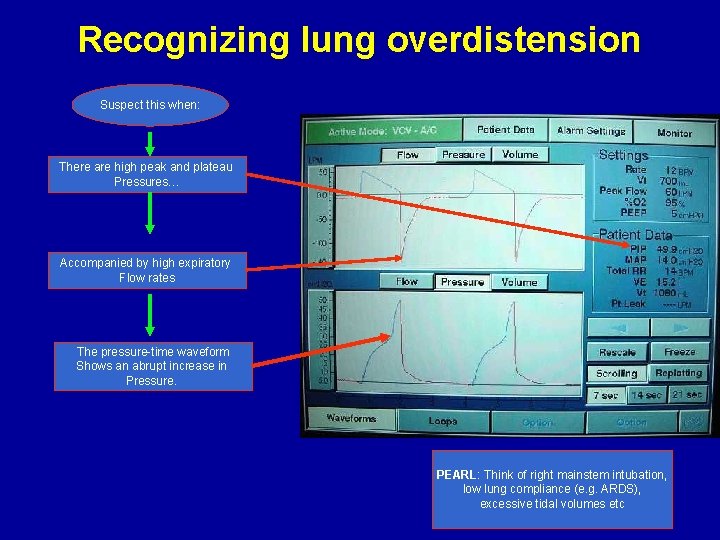
Recognizing lung overdistension Suspect this when: There are high peak and plateau Pressures… Accompanied by high expiratory Flow rates The pressure-time waveform Shows an abrupt increase in Pressure. PEARL: Think of right mainstem intubation, low lung compliance (e. g. ARDS), excessive tidal volumes etc
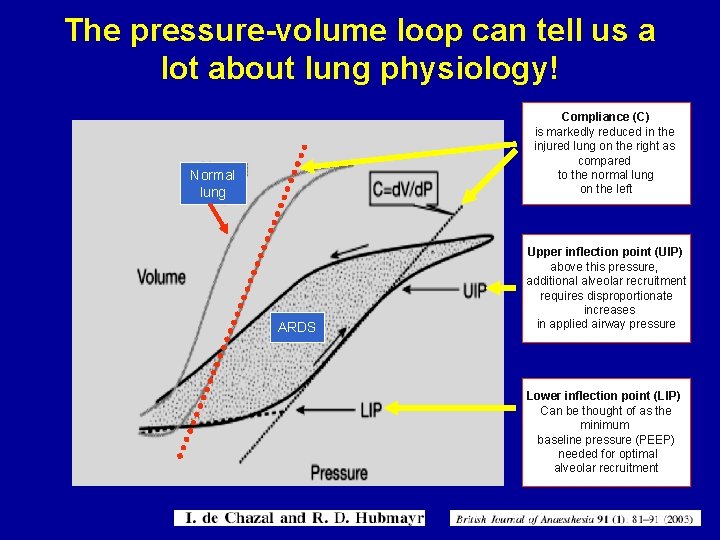
The pressure-volume loop can tell us a lot about lung physiology! Compliance (C) is markedly reduced in the injured lung on the right as compared to the normal lung on the left Normal lung ARDS Upper inflection point (UIP) above this pressure, additional alveolar recruitment requires disproportionate increases in applied airway pressure Lower inflection point (LIP) Can be thought of as the minimum baseline pressure (PEEP) needed for optimal alveolar recruitment
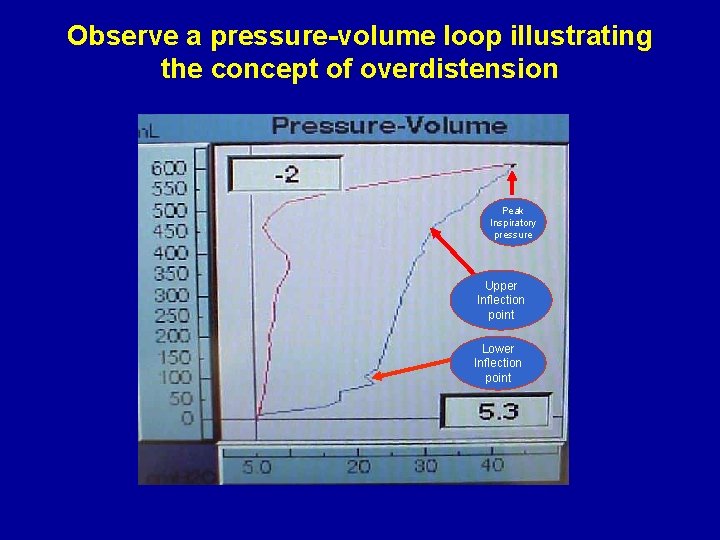
Observe a pressure-volume loop illustrating the concept of overdistension Peak Inspiratory pressure Upper Inflection point Lower Inflection point
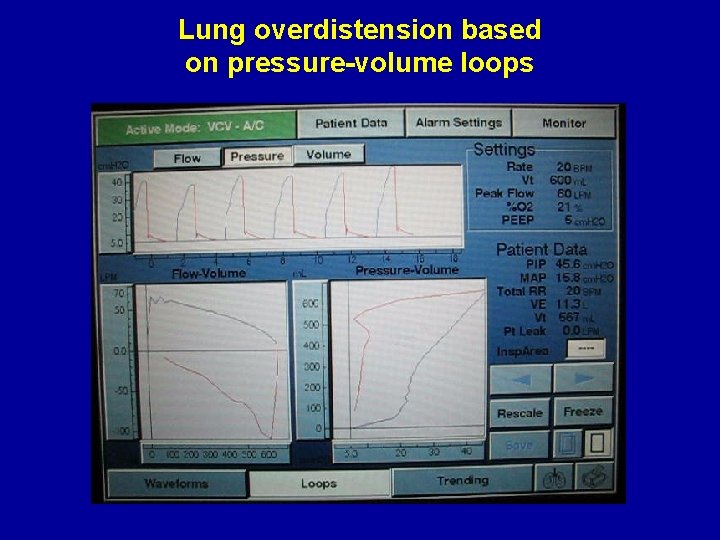
Lung overdistension based on pressure-volume loops

Recognizing Auto-PEEP
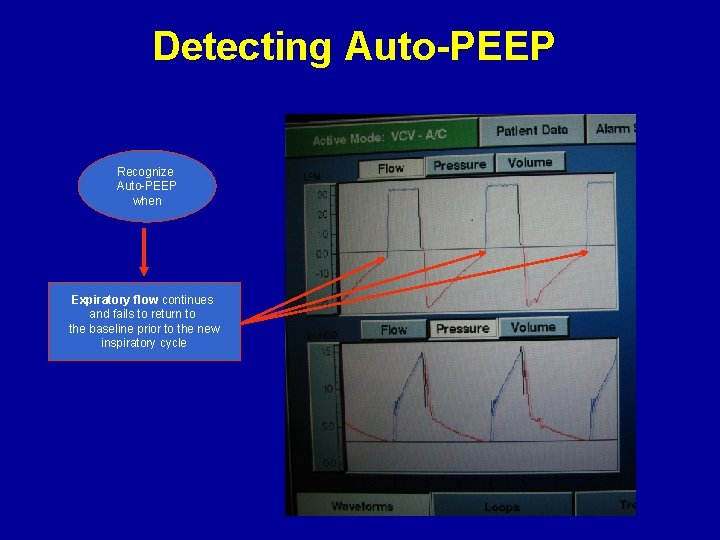
Detecting Auto-PEEP Recognize Auto-PEEP when Expiratory flow continues and fails to return to the baseline prior to the new inspiratory cycle

The development of auto- PEEP over several breaths in a simulation Notice how the expiratory flow fails to return to the baseline causing progressive air trapping Also notice how the progressive air trapping causes a gradual increase in airway pressures due to decreasing compliance

Development of auto-PEEP Notice how the expiratory flow fails to return to the baseline causing progressive air trapping Click here to watch video Also notice how the progressive air trapping causes a gradual increase in airway pressures because of decreasing compliance
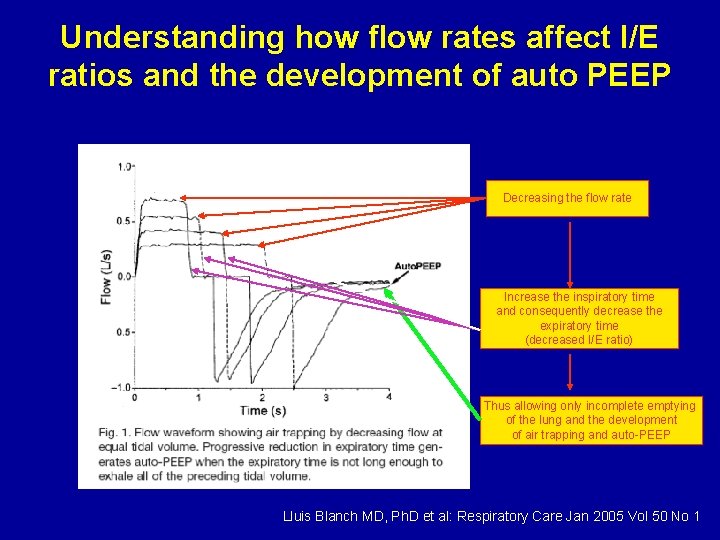
Understanding how flow rates affect I/E ratios and the development of auto PEEP Decreasing the flow rate Increase the inspiratory time and consequently decrease the expiratory time (decreased I/E ratio) Thus allowing only incomplete emptying of the lung and the development of air trapping and auto-PEEP Lluis Blanch MD, Ph. D et al: Respiratory Care Jan 2005 Vol 50 No 1

Understanding how inspiratory time affect I/E ratios and the development of auto-PEEP • In a similar fashion, an increase in inspiratory time can also cause a decrease in the I: E ratio and favor the development of auto-PEEP by not allowing enough time for complete lung emptying between breaths. • Watch in the next video how auto-PEEP develops in a patient on Pressure control ventilation at a RR of 20, just by increasing the inspiratory time from 0. 85 sec to 1. 0 sec (no auto-PEEP develops) and then to 1. 5 sec (development of auto PEEP)
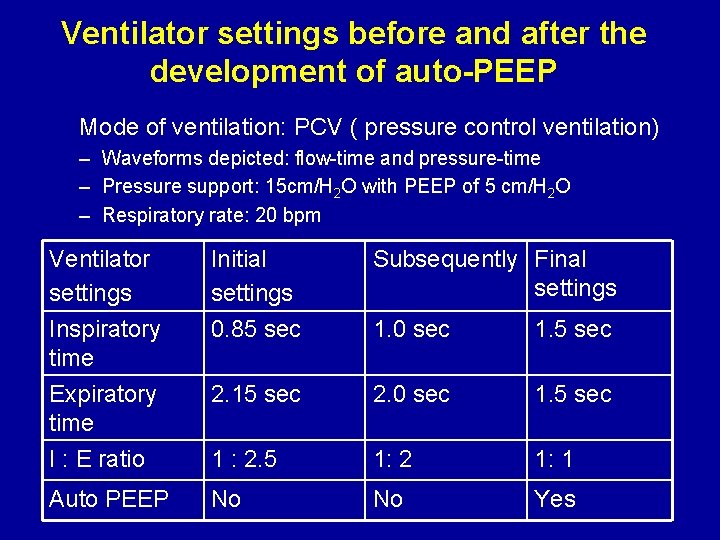

Ventilator settings before and after the development of auto-PEEP Mode of ventilation: PCV ( pressure control ventilation) – Waveforms depicted: flow-time and pressure-time – Pressure support: 15 cm/H 2 O with PEEP of 5 cm/H 2 O – Respiratory rate: 20 bpm Ventilator settings Inspiratory time Initial settings 0. 85 sec Subsequently Final settings 1. 0 sec 1. 5 sec Expiratory time I : E ratio 2. 15 sec 2. 0 sec 1. 5 sec 1 : 2. 5 1: 2 1: 1 Auto PEEP No No Yes

Development of auto-PEEP with inadequate expiratory time Click here to watch video

Recognizing Expiratory Flow Limitation (e. g. COPD, asthma)

Recognizing prolonged expiration (air trapping) Recognize Airway obstruction when Expiratory flow quickly tapers off and then enters a prolonged low-flow state without returning to baseline (auto- PEEP) This is classic for the flow limitation and decreased lung elastance characteristic of COPD or status asthmaticus
Let us now move forward and Learn about diagnosing patient-ventilator Interactions by analyzing ventilator waveforms Abnormal ventilatory Parameters/lung mechanics E. g. . Overdistension, Auto PEEP COPD Patient-ventilator Interactions E. g. flow starvation, Double triggering, Wasted efforts Active expiration Ventilatory circuit related problems E. g. auto cycling and secretion build up in the Ventilatory circuit

Recognizing: Wasted efforts Double triggering Flow starvation Active expiration

Recognizing ineffective/wasted patient effort Patient inspiratory effort fails to trigger vent cycle resulting in a wasted effort Results in fatigue, tachycardia, Increased metabolic needs, Fever etc
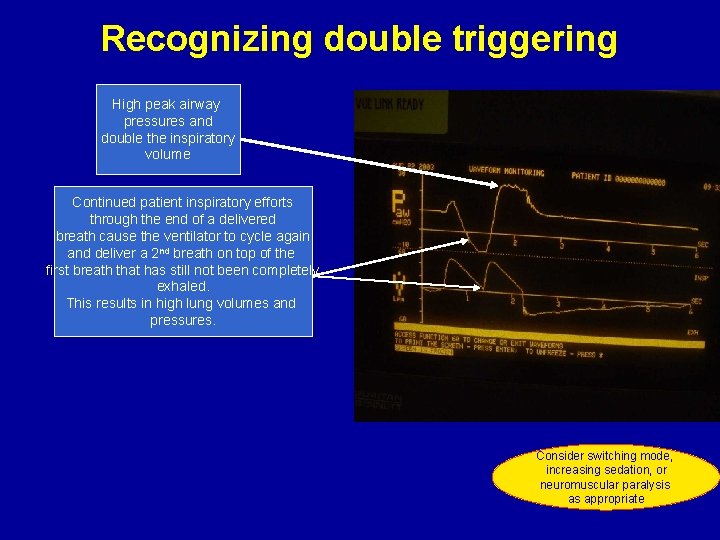
Recognizing double triggering High peak airway pressures and double the inspiratory volume Continued patient inspiratory efforts through the end of a delivered breath cause the ventilator to cycle again and deliver a 2 nd breath on top of the first breath that has still not been completely exhaled. This results in high lung volumes and pressures. Consider switching mode, increasing sedation, or neuromuscular paralysis as appropriate
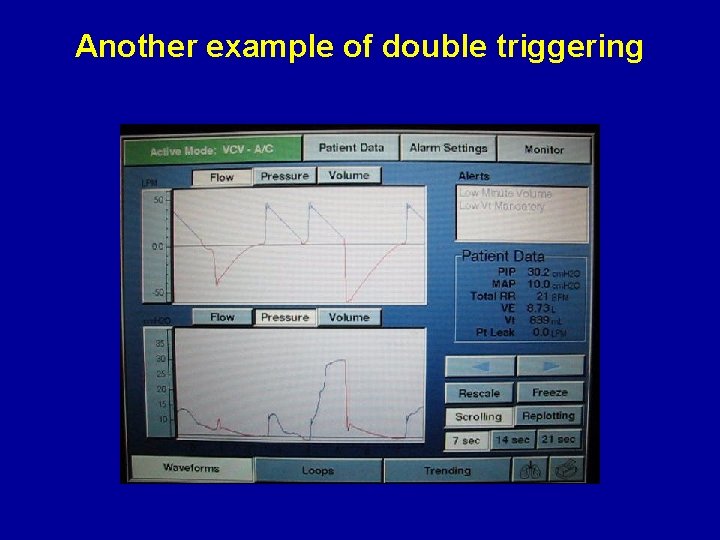
Another example of double triggering

Recognizing flow starvation Look at the pressure-time waveform If you see this kind of scooping or distortion instead of a smooth rise in the pressure curve…. Diagnose flow starvation in the setting of patient discomfort, fatigue, dyspnea etc on the vent

Recognizing active expiration Look at the flow-time & pressure-time Waveform In this situation, the patient is making active expiratory efforts during the inspiratory phase of the ventilator delivered breath cycle Notice how the expiratory flow and the pressure rise dramatically as a result of the opposing forces at work
Lastly let us learn to recognize Ventilatory circuit related problems by analyzing ventilatory waveforms Abnormal ventilatory Parameters/lung mechanics E. g. . Overdistension, Auto PEEP COPD Patient-ventilator Interactions E. g. flow starvation, Double triggering, Wasted efforts Ventilatory circuit related problems E. g. auto cycling and secretion build up in the Ventilatory circuit

Recognizing Airway Secretions & Ventilator Auto-Cycling

Recognizing airway or tubing secretions Normal flow-volume loop Flow volume loop showing a ‘saw tooth’ pattern typical of retained secretions
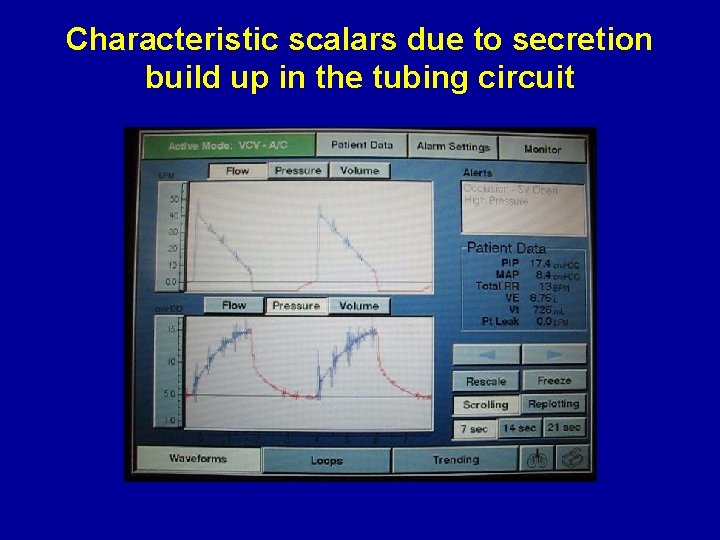
Characteristic scalars due to secretion build up in the tubing circuit

Recognizing ventilator auto-cycling • Think about auto-cycling when the respiratory rate increases suddenly without any patient input and if the exhaled tidal volume and minute ventilation suddenly decrease. • Typically occurs because of a leak anywhere in the system starting from the ventilator right up to the patients lungs – e. g. leaks in the circuit, ET tube cuff leak, lungs (pneumothorax) • May also result from condensate in the circuit • The exhaled tidal volume will be lower than the set parameters and this may set off a ventilator alarm for low exhaled tidal volume, low minute ventilation, circuit disconnect or rapid respiratory rate.

Waveform video showing the ventilator ‘auto cycling’ Click here to watch video

Take home points • Ventilator waveform analysis is a very integral and important component in the management of a mechanically ventilated patient. • Develop a habit of looking at the right waveform for the given mode that the patient is being ventilated on. • Always look at the inspiratory and expiratory components of the flow-time waveform. • Don’t hesitate to change the scale or speed of the waveform to aid in your interpretation.

Additional links • Follow these links for more waveform videos: – Auto-PEEP http: //www. youtube. com/watch? v=30 jd. Xd 7 TS 84 – Autocycling http: //www. youtube. com/user/dakaufman 123#p/a/u/0/ CPOsp 8 WJSr. A – Excessive airway secretions: http: //www. youtube. com/user/dakaufman 123#p/a/u/1/ F 93 m. PDMtl 8 I – Flow starvation http: //www. youtube. com/user/dakaufman 123#p/a/u/2/ Zoy. Fcv. Nq. Vq 0
- Slides: 72