Ventilator associated Pneumonia Tobias Welte Department of Respiratory

Ventilator associated Pneumonia Tobias Welte Department of Respiratory Medicine and Intensive Care
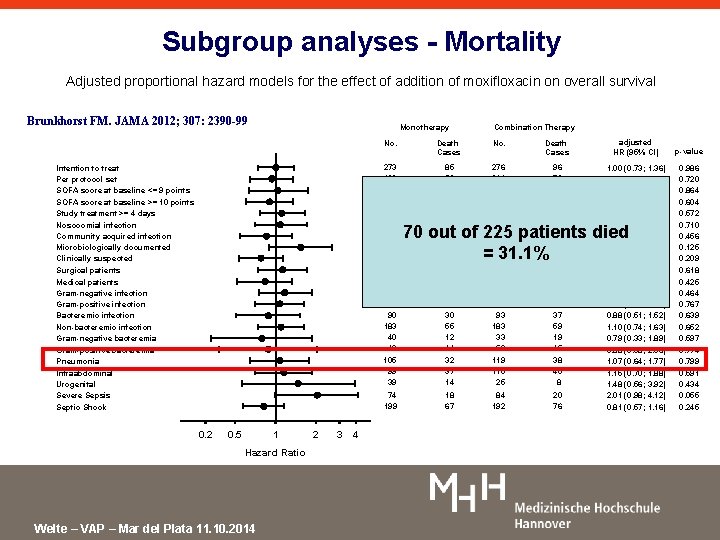
Subgroup analyses - Mortality Adjusted proportional hazard models for the effect of addition of moxifloxacin on overall survival Brunkhorst FM. JAMA 2012; 307: 2390 -99 Monotherapy B Intention to treat Per protocol set SOFA score at baseline <= 9 points SOFA score at baseline >= 10 points Study treatment >= 4 days Nosocomial infection Community acquired infection Microbiologically documented Clinically suspected Surgical patients Medical patients Gram-negative infection Gram-positive infection Bacteremic infection Non-bacteremic infection Gram-negative bacteremia Gram-positive bacteremia Pneumonia Intraabdominal Urogenital Severe Sepsis Septic Shock 0. 2 0. 5 1 Hazard Ratio Welte – VAP – Mar del Plata 11. 10. 2014 2 3 4 Combination Therapy No. Death Cases adjusted HR (95% CI) p-value 273 199 141 132 206 137 136 97 176 146 127 149 140 90 183 40 49 85 59 37 48 57 43 42 32 53 47 38 47 43 30 55 12 14 276 214 153 123 209 135 141 98 178 162 114 120 155 93 183 33 58 96 70 43 53 61 46 50 28 68 50 46 46 53 37 59 19 15 1. 00 (0. 73; 1. 36) 0. 94 (0. 65; 1. 35) 1. 05 (0. 63; 1. 74) 0. 90 (0. 60; 1. 34) 1. 12 (0. 76; 1. 66) 1. 09 (0. 70; 1. 69) 0. 84 (0. 54; 1. 32) 1. 54 (0. 89; 2. 66) 0. 78 (0. 53; 1. 15) 0. 986 0. 720 0. 864 0. 604 0. 572 0. 710 0. 456 0. 125 0. 209 1. 11 (0. 73; 1. 71) 0. 82 (0. 51; 1. 32) 1. 19 (0. 75; 1. 88) 1. 07 (0. 69; 1. 64) 0. 88 (0. 51; 1. 52) 0. 618 0. 425 0. 464 0. 767 0. 639 105 99 39 32 37 14 119 110 25 38 40 8 74 199 18 67 84 192 20 76 1. 10 (0. 74; 1. 63) 0. 79 (0. 33; 1. 89) 0. 88 (0. 38; 2. 06) 1. 07 (0. 64; 1. 77) 1. 15 (0. 70; 1. 88) 1. 48 (0. 56; 3. 92) 2. 01 (0. 98; 4. 12) 0. 81 (0. 57; 1. 16) 0. 652 0. 597 0. 774 0. 799 0. 591 0. 434 0. 055 0. 245 70 out of 225 patients died = 31. 1%

• Diagnostics Dalhoff K et al. Pneumologie 2012; 66: 707 -65 Dt. Ärzteblatt Int. 2013; 110 (38): 634 -40 1. Clinical diagnosis and differential diagnosis 2. Imaging procedures in the diagnostic work up 3. The role of scoring in the diagnostics and for risk assessment 4. The role of biomarkers in the diagnostics 5. The role of blood cultures in the diagnostics 6. The role of an antigen test in the diagnostics 7. What microbiological tests should be carried out? ? 8. Invasive or non invasive diadnostic techniques? 9. Standards in diagnostics 10. Mykological diagnostics Welte – VAP – Mar del Plata 11. 10. 2014

CDC and prevention national healthcare safety network clinical definition for VAP Klompas. Curr Opin Infect Dis 2012; 25: 176 -82 Patients must fulfil radiographic, systemic and pulmonary criteria: Two or more serial radiographic, systemic and pulmonary criteria New or progressive and peristent infiltrate Consolidation Cavitation One of the following Two of the following Fever (>38ºC or >100. 4ºF) New onset of purulent sputum or change in character of sputum or increased respiratory secretions or increased suctioning requirements Leukopenia (<400 WBC/µl) or leukocytosis (>12000 WBC/µl) New onset or worsening cough, or dypsnea, or tachypnea For adults ≥ 70 years old, altered mental status with no other recognised cause Rales or bronchial breath sounds Worsening gas exchange (eg oxygen desaturation, increased oxygen requirements, or increased ventilation demand) Welte – VAP – Mar del Plata 11. 10. 2014

Do we have an objective, independent and reliable surveillance system? Clinical signs for VAP are subjective and non-specific Initiatives intended to decrease the occurrence of nosocomial infection can artefactually lower VAP rates Bonten. Clin Infect Dis 2011; 52: 115 -21; Klompas. Curr Opin Infect Dis 2012; 25: 176 -82 Welte – VAP – Mar del Plata 11. 10. 2014

A comparison of VAP rates as identified according to intensivists vs infection control practitioners • Prospective comparison of 5 months of VAP surveillance by surgical intensivists vs infection preventionists in a surgical ICU using CDC definitions • Intensivists found much higher rates of VAP than infection preventionists (28. 5% vs 8. 3%; p<0. 001) • When compared with BAL, intensivist-VAP had 61% sensitivity and preventionist-VAP had 29% sensitivity Thomas et al. Am Surg 2011; 77: 998 -1002 Welte – VAP – Mar del Plata 11. 10. 2014

Prevention and therapy of HAP using a bundle approach • Zack JE, et al. Effect of an educational program aimed at reducing the occurrence of ventilatorassociated pneumonia. Crit Care Med 2002; 30: 2407 -12. • Babcock HM, et al. An educational intervention to reduce ventilator-associated pneumonia in an integrated health system: a comparison of effects. Chest 2004; 125: 2224 -31. • Resar R, et al. Using a bundle approach to improve ventilator care processes and reduce ventilatorassociated pneumonia. Jt Comm J Qual Patient Saf 2005; 31: 243 -8. • Institute for Healthcare Improvement. Implement the ventilator bundle. Available at: http: //www. ihi. org. • Apisarnthanarak A, et al. Effectiveness of an educational program to reduce ventilator-associated pneumonia in a tertiary care center in Thailand: a 4 -year study. Clin Infect Dis 2007: 45: 704 -11. • Bird D, et al. Adherence to ventilator-associated pneumonia bundle and incidence of ventilatorassociated pneumonia in the surgical intensive care unit. Arch Surg 2010; 145: 465 -70. • De. Palo VA, et al. The Rhode Island ICU collaborative: a model for reducing central line-associated bloodstream infection and ventilator-associated pneumonia statewide. Qual Saf Health Care 2010; 19: 555 -61. • Berenholtz SM, et al. Collaborative cohort study of an intervention to reduce ventilator-associated pneumonia in the intensive care unit. Infect Control Hosp Epidemiol 2011; 32: 305 -14. • Anon. Five years without VAP? Two years without BSI? Hosp Peer Rev 2011; 36: 42 -6. Welte – VAP – Mar del Plata 11. 10. 2014
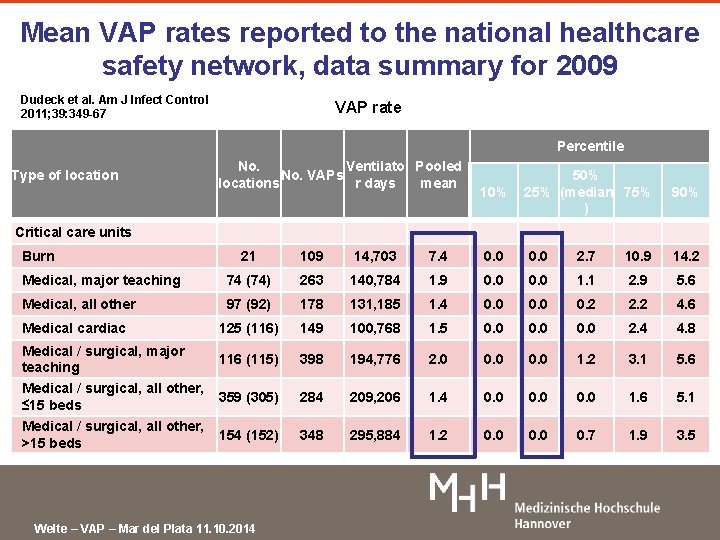
Mean VAP rates reported to the national healthcare safety network, data summary for 2009 Dudeck et al. Am J Infect Control 2011; 39: 349 -67 VAP rate Percentile Type of location No. Ventilato Pooled No. VAPs locations r days mean 10% 50% 25% (median 75% ) 90% Critical care units Burn 21 109 14, 703 7. 4 0. 0 2. 7 10. 9 14. 2 Medical, major teaching 74 (74) 263 140, 784 1. 9 0. 0 1. 1 2. 9 5. 6 Medical, all other 97 (92) 178 131, 185 1. 4 0. 0 0. 2 2. 2 4. 6 Medical cardiac 125 (116) 149 100, 768 1. 5 0. 0 2. 4 4. 8 Medical / surgical, major teaching 116 (115) 398 194, 776 2. 0 0. 0 1. 2 3. 1 5. 6 Medical / surgical, all other, ≤ 15 beds 359 (305) 284 209, 206 1. 4 0. 0 1. 6 5. 1 Medical / surgical, all other, >15 beds 154 (152) 348 295, 884 1. 2 0. 0 0. 7 1. 9 3. 5 Welte – VAP – Mar del Plata 11. 10. 2014

What is the clinical relevance of studies having demonstrated a VAP rate of zero? • None of them were rigorously evaluated and demonstrated a benefit using relevant endpoints such as: – – Antibiotic use Duration of mechanical ventilation Length of stay in the ICU and the hospital Overall mortality Bonten. Clin Infect Dis 2011; 52: 115 -21; Klompas. Curr Opin Infect Dis 2012; 25: 176 -82 Welte – VAP – Mar del Plata 11. 10. 2014

Blood Culture Diagnostics The Reality • Structured telephone interviews about blood culture diagnostics in Great Britain (Gb), France (F), Italien (I) and Germany (G) – 59 Intensivists – 79 Clinical mikrobiologists • Time from taking the blood cultures to inkubation of them in Gb 2, F 3, I 4, G 20 hours – If the microbiological lab was inhouse 2 h • Satisfaction with the quality of the blood cultures – Intensivists 62% – Mikrobiologists 47% Welte – VAP – Mar del Plata 11. 10. 2014 Schmitz RP et al. Crit Care 2013; 17 (5): R 248 1 9

PCR diagnostics in blood cultures • Septi. Fast®, Roche, Basel, Switzerland – Multiplex real-time PCR that simultaneously detects a pre-defined panel of the most important sepsis pathogens by species- or genus-specific fluorescent probes • Sepsi. Test. TM, Molzym, Bremen, Germany – Eubacterial and pan-fungal real-time PCR that is able to detect nearly all known bacterial and fungal pathogens by a 16 S and 18 S r. RNA gene-based universal PCR, followed by sequencing of the amplification product for species identification • VYOO®, SIRS Lab, Jena, Germany – Multiplex PCR that detects a predefined panel of the most important sepsis pathogens by microarray-based detection of target-specific amplicons • Plex-IDTM, Abbott, Wiesbaden, Germany – Eubacterial and pan-fungal PCR that is able to detect nearly all known bacterial and fungal pathogens by genome-specific targets followed by mass spectrometry for species identification PCR, polymerase chain reaction; r. RNA, ribosomal ribonucleic acid Welte – VAP – Mar del Plata 11. 10. 2014 Pletz MW et al. Intensive Care Med 2011; 37: 1069 -76 11

PCR diagnostics in blood cultures Septifast® Bloos F et al. Intensive Care Med 2010; 36: 241 -7 PCR BC 61 microorganisms from 47 samples • 142 patients with severe sepsis and 63 surgical control individuals • Presence of microbial DNA was assessed by multiplex PCR (Septi. Fast®) on enrolment and each time a BC was obtained • Control individuals had ~4% positive PCRs and BCs • In severe sepsis, 34. 7% of PCRs were positive vs 16. 5% of BCs (p<0. 001) • 70. 3% of BCs had a corresponding PCR result, while only 21. 4% of PCR results were confirmed by BC • Patients with positive PCRs had higher SOFA scores (12 vs 9; p=0. 023) and a trend towards higher mortality (PCR negative 25. 3%; PCR positive 39. 1%; p=0. 115) Welte – VAP – Mar del Plata 11. 10. 2014 32 41 microorganisms from 39 samples 6 18 (7 not on PCR panel) 15 8 9 289 (75 not on PCR panel) Specimen 321 microorganisms from 135 samples

PCR diagnostics in blood cultures Vyoo ® Bloos F et al. PLo. S One 2012; 7: e 46003 • Observational study in a 50 -bed ICU • 311 concomitant blood cultures and blood for multiplex PCR (VYOO®) were obtained from patients with suspected sepsis (n = 245) – 14. 5% of blood cultures and 30. 1% of PCRs were positive – Median time to positivity was 24. 2 hours for the PCR and 68 hours for BC – In 34% of patients with positive PCRs, antimicrobial therapy was considered inadequate • 5 patients with VRE • 3 patients with multi-resistant Staphylococci • 4 patients with fungi Welte – VAP – Mar del Plata 11. 10. 2014 PCR Mi. Bi 85 18 227 97 not on target list 7 7 29 7 not on target list BC 10

PCR diagnostics in Sputum / BAL Jamal W et al. J Clin Microbiol 2014; 52: 2487 -92 Impact of the rapid multiplex PCR-based UPA in detecting aetiological pathogens and resistance markers in patients with NP • 49 patients with NP – 27 (55. 1%) and 4 (8. 2%) harboured multiple bacteria by UPA and conventional culture, respectively – A single pathogen was detected in 8 (16. 3%) and 4 (8. 2%) patients, respectively – 13 different genes were detected from 38 patients, including the erm. B gene (40. 8%), the bla. OXA-51 -like gene (28. 6%), the sul 1 (28. 6%) and int 1 (20. 4%) integrase genes, and the mec. A and bla. CTX-M genes (12. 3% each) – The time from sample testing to results was 4 hours by UPA vs 48– 96 hours by culture – Initial empirical treatment was changed within 5– 6 hours in 33 (67. 3%) patients based on the availability of UPA results Welte – VAP – Mar del Plata 11. 10. 2014 14
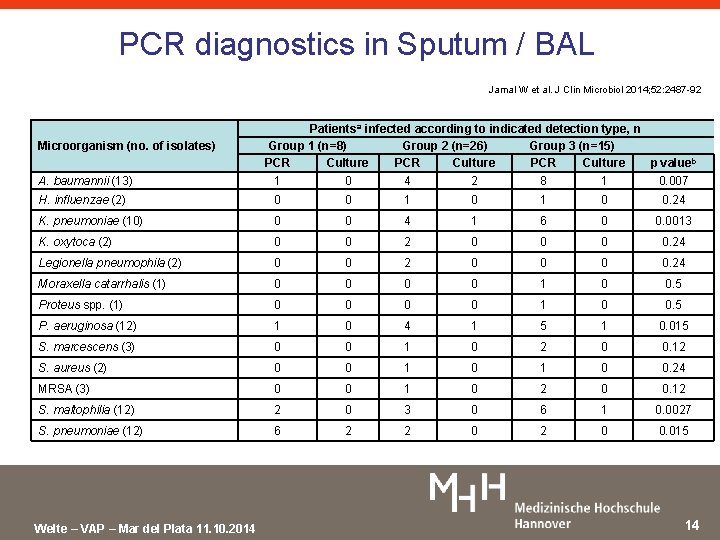
PCR diagnostics in Sputum / BAL Jamal W et al. J Clin Microbiol 2014; 52: 2487 -92 Microorganism (no. of isolates) A. baumannii (13) Patientsa infected according to indicated detection type, n Group 1 (n=8) Group 2 (n=26) Group 3 (n=15) PCR Culture p valueb 1 0 4 2 8 1 0. 007 H. influenzae (2) 0 0 1 0 0. 24 K. pneumoniae (10) 0 0 4 1 6 0 0. 0013 K. oxytoca (2) 0 0 2 0 0. 24 Legionella pneumophila (2) 0 0 2 0 0. 24 Moraxella catarrhalis (1) 0 0 1 0 0. 5 Proteus spp. (1) 0 0 1 0 0. 5 P. aeruginosa (12) 1 0 4 1 5 1 0. 015 S. marcescens (3) 0 0 1 0 2 0 0. 12 S. aureus (2) 0 0 1 0 0. 24 MRSA (3) 0 0 1 0 2 0 0. 12 S. maltophilia (12) 2 0 3 0 6 1 0. 0027 S. pneumoniae (12) 6 2 2 0 0. 015 Welte – VAP – Mar del Plata 11. 10. 2014 14
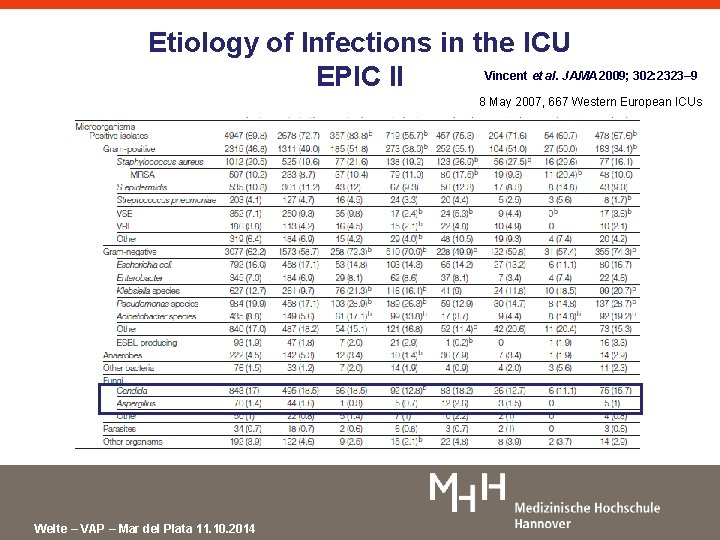
Etiology of Infections in the ICU Vincent et al. JAMA 2009; 302: 2323– 9 EPIC II 8 May 2007, 667 Western European ICUs Welte – VAP – Mar del Plata 11. 10. 2014

Welte – VAP – Mar del Plata 11. 10. 2014
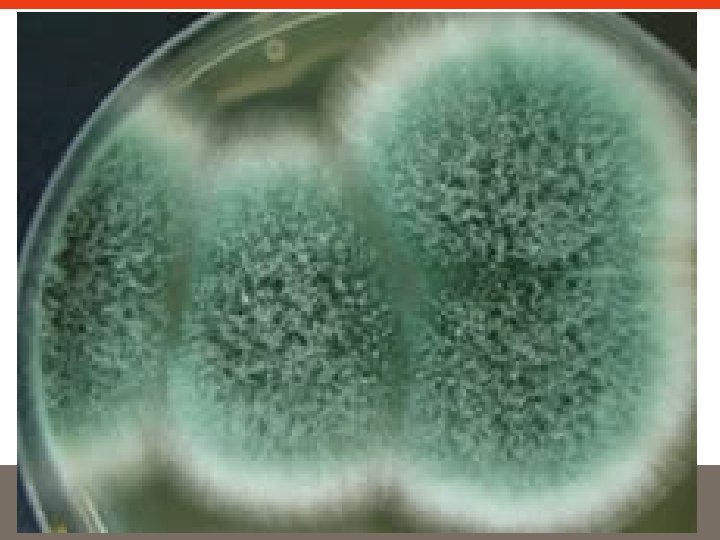
Welte – VAP – Mar del Plata 11. 10. 2014

Aspergillus: not only in neutropenic and immunosuppressed pts Meerssman, CID, 2007 Welte – VAP – Mar del Plata 11. 10. 2014
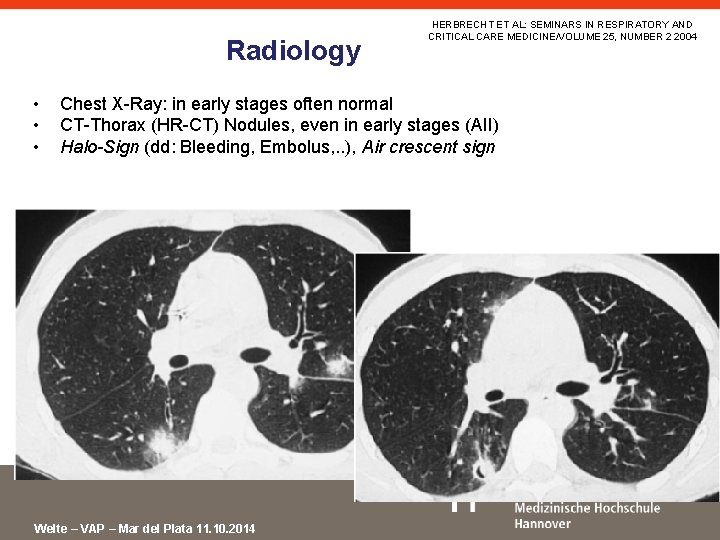
Radiology • • • HERBRECHT ET AL: SEMINARS IN RESPIRATORY AND CRITICAL CARE MEDICINE/VOLUME 25, NUMBER 2 2004 Chest X-Ray: in early stages often normal CT-Thorax (HR-CT) Nodules, even in early stages (AII) Halo-Sign (dd: Bleeding, Embolus, . . ), Air crescent sign Welte – VAP – Mar del Plata 11. 10. 2014
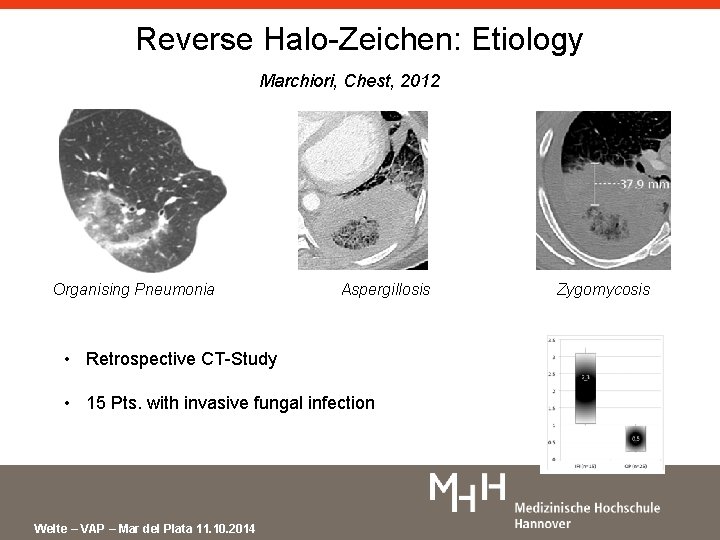
Reverse Halo-Zeichen: Etiology Marchiori, Chest, 2012 Organising Pneumonia Aspergillosis • Retrospective CT-Study • 15 Pts. with invasive fungal infection Welte – VAP – Mar del Plata 11. 10. 2014 Zygomycosis

Serology 1. Galaktomannan-Assay (Pastorex® Aspergillus) 1, 2 Specifity 90 -100%, Sensitivity 26 -76% 2. Galaktomannan ELISA (Platelia® Aspergillus) 3, 4 Specifity 80 -100%, Sensitivity 70 -90% (PPV 87, 5%) Galactomannan in neutropenic pts 2 x/week (AII), cave: Tazobactam or Amoxyclav. Negative predictive Value 95– 98% 3. Galaktomannan BAL Specifity 94– 100%, Sensitivity 76– 85% 5, 6, 7 4. G-Test: Beta-D-Glucan (Fungitec®G) Sensitivity+Specifity ? 1. Haynes K, Rogers TR (1994) Eur J Clin Microbiol Infect Dis 13: 670– 674 2. Machetti M, Feasi M, Mordini N, Van-Lint MT, Bacigalupo A, Latge JP, Sarfati J, Viscoli C (1998). Bone Marrow Transplant 21: 917– 921 3. Maertens J, Verhaegen J, Lagrou K, Van-Eldere J, Boogaerts M (2001). Blood 97: 1604– 1610 4. Sulahian A, Boutboul F, Ribaud P, Leblanc T, Lacroix C, Derouin F (2001). 91: 311– 338 5. Musher B, Fredricks D, Leisenring W et al. J Clin Microbiol 2004; 42: 5517– 5522. 6. Becker MJ, Lugtenburg EJ, Cornelissen JJBr J Haematol 2003; 121: 448– 457 7. Meersseman W, Lagrou K, Maertens J, Am J Respir Crit Care Med 2008; 177: 27– 34 Welte – VAP – Mar del Plata 11. 10. 2014
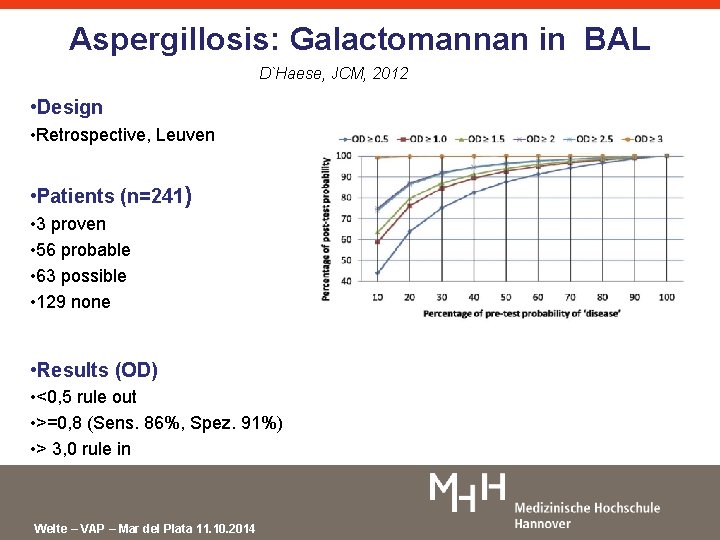
Aspergillosis: Galactomannan in BAL D`Haese, JCM, 2012 • Design • Retrospective, Leuven • Patients (n=241) • 3 proven • 56 probable • 63 possible • 129 none • Results (OD) • <0, 5 rule out • >=0, 8 (Sens. 86%, Spez. 91%) • > 3, 0 rule in Welte – VAP – Mar del Plata 11. 10. 2014

• Therapy – – – Dalhoff K et al. Pneumologie 2012; 66: 707 -65 Dt. Ärzteblatt Int. 2013; 110 (38): 634 -40 When should the antibiotic therapy starts? Calculated therapy in patients without risk for MDR pathogens Calculated Therapie in patients with risk for MDR pathogens Combination therapy Early stop of therapy Evaluation of treatment success Deescalation therapy Duration of treatment Treatment failure Ventilator Tracheobronchitis Inhaled antibiotic therapy Targeted therapy for special therapies Welte – VAP – Mar del Plata 11. 10. 2014

Welte – VAP – Mar del Plata 11. 10. 2014
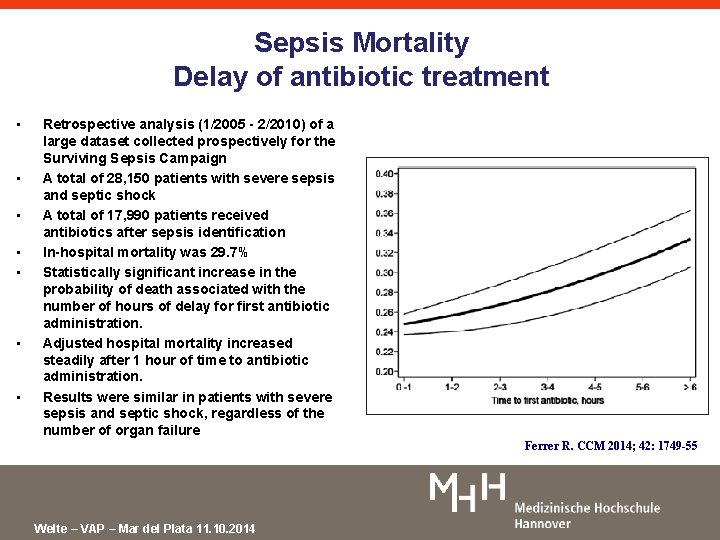
Sepsis Mortality Delay of antibiotic treatment • • Retrospective analysis (1/2005 - 2/2010) of a large dataset collected prospectively for the Surviving Sepsis Campaign A total of 28, 150 patients with severe sepsis and septic shock A total of 17, 990 patients received antibiotics after sepsis identification In-hospital mortality was 29. 7% Statistically significant increase in the probability of death associated with the number of hours of delay for first antibiotic administration. Adjusted hospital mortality increased steadily after 1 hour of time to antibiotic administration. Results were similar in patients with severe sepsis and septic shock, regardless of the number of organ failure Ferrer R. CCM 2014; 42: 1749 -55 Welte – VAP – Mar del Plata 11. 10. 2014
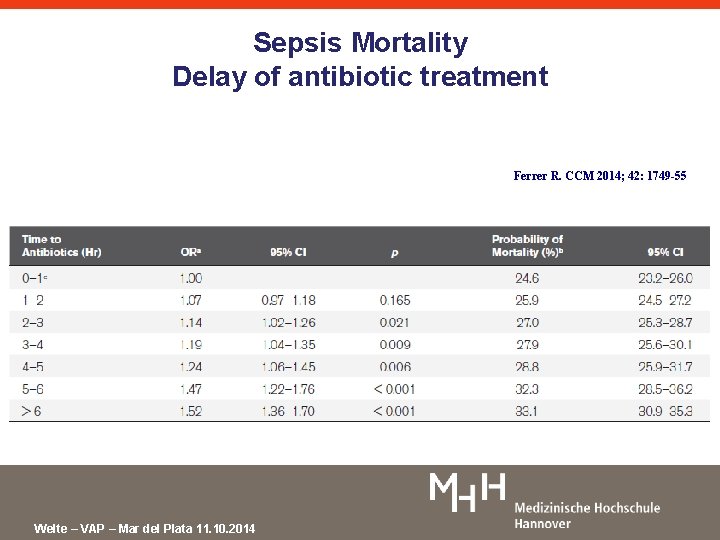
Sepsis Mortality Delay of antibiotic treatment Ferrer R. CCM 2014; 42: 1749 -55 Welte – VAP – Mar del Plata 11. 10. 2014
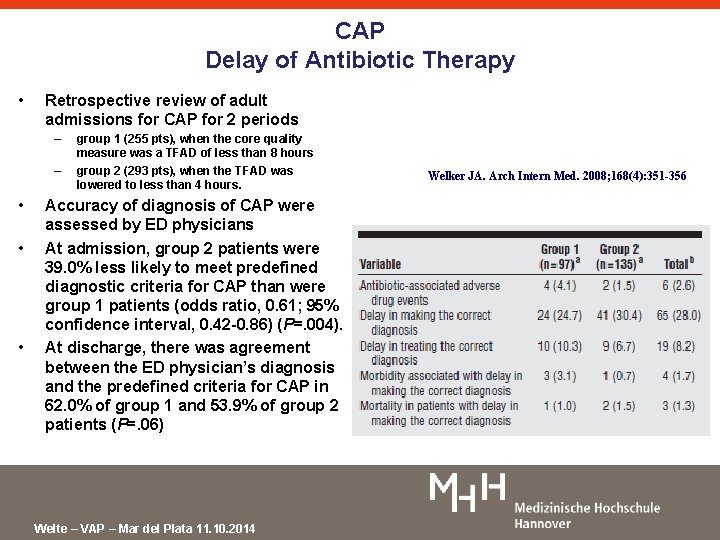

CAP Delay of Antibiotic Therapy • Retrospective review of adult admissions for CAP for 2 periods – – • • • group 1 (255 pts), when the core quality measure was a TFAD of less than 8 hours group 2 (293 pts), when the TFAD was lowered to less than 4 hours. Accuracy of diagnosis of CAP were assessed by ED physicians At admission, group 2 patients were 39. 0% less likely to meet predefined diagnostic criteria for CAP than were group 1 patients (odds ratio, 0. 61; 95% confidence interval, 0. 42 -0. 86) (P=. 004). At discharge, there was agreement between the ED physician’s diagnosis and the predefined criteria for CAP in 62. 0% of group 1 and 53. 9% of group 2 patients (P=. 06) Welte – VAP – Mar del Plata 11. 10. 2014 Welker JA. Arch Intern Med. 2008; 168(4): 351 -356

Lancet Infect Dis 2012; 12: 774– 80 • Pre-/post study in a surgical ICU in the US – Aggressive therapy (01. 09. 2008 -31. 08. 2009) • If an infection was suspected antibiotic treatment was initiated immediately – Conservative therapy (01 -09. 2009 -31. 08. 2010) • Initiation of an antibiotic therapy only, when an infection has been confirmed by diagnostic results Welte – VAP – Mar del Plata 11. 10. 2014 4

Standard Treatment gram positive infections • S. pneumoniae – Beta-Laktam-Macrolid combination therapy • A and B-Streptococci – Penicillin-/Clindamycin combination therapy • Staph. Aureus – Sensibel: Oxacillin or 1. Gen. Cephalosporin – MRSA: Vancomycin/Linezolid/Daptomycin/Rifampicin • Enterococci – E. faecalis: Ampicillin or Ampicillin/Inhibitor Combination – E. faecium: Vancomycin/Linezolid Welte – VAP – Mar del Plata 11. 10. 2014

Standard Treatment gram negatives • E. coli/Enterobakteriacae – Ampicillin/Inhibitor Combinations – 2. and 3. Generation Cephalosporines – Ertapenem • Pseudomoas aeruginosa/Acinetobacter – Piperacillin/Tazobaktam – 4. Generation Cephalosporines – Carbapenemes • St. maltophilia – Fluorquinolones – Cotrimoxazol Welte – VAP – Mar del Plata 11. 10. 2014

FM Brunkhorst, M Oppert, G Marx and coauthors Effect of Empirical Treatment With Moxifloxacin and Meropenem vs Meropenem on Sepsis-Related Organ Dysfunction in Patients With Severe Sepsis: A Randomized Controlled Trial Published online May 21, 2012 Welte – VAP – Mar del Plata 11. 10. 2014
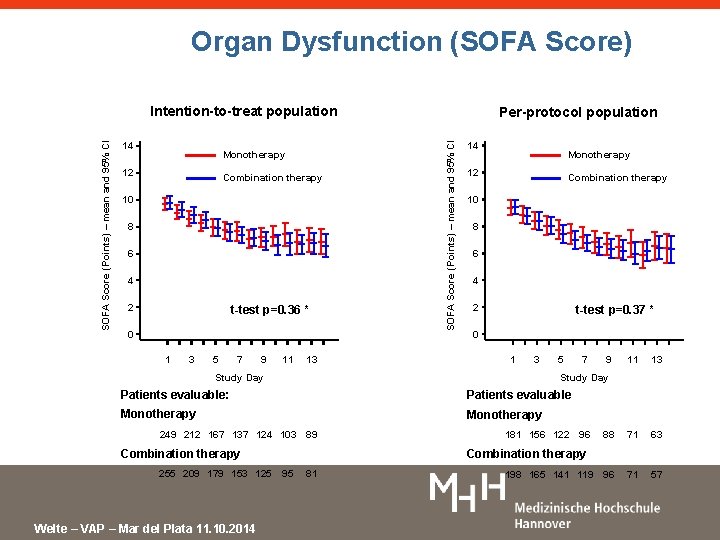
Organ Dysfunction (SOFA Score) 14 Monotherapy 12 Combination therapy 10 8 6 4 2 t-test p=0. 36 * 0 1 3 5 7 9 11 13 Per-protocol population SOFA Score (Points) – mean and 95% CI Intention-to-treat population 14 Monotherapy 12 Combination therapy 10 8 6 4 2 t-test p=0. 37 * 0 1 3 Study Day 5 Patients evaluable Monotherapy 249 212 167 137 124 103 89 Combination therapy Welte – VAP – Mar del Plata 11. 10. 2014 9 11 13 88 71 63 96 71 57 Study Day Patients evaluable: 255 209 179 153 125 7 181 156 122 96 Combination therapy 95 81 198 165 141 119
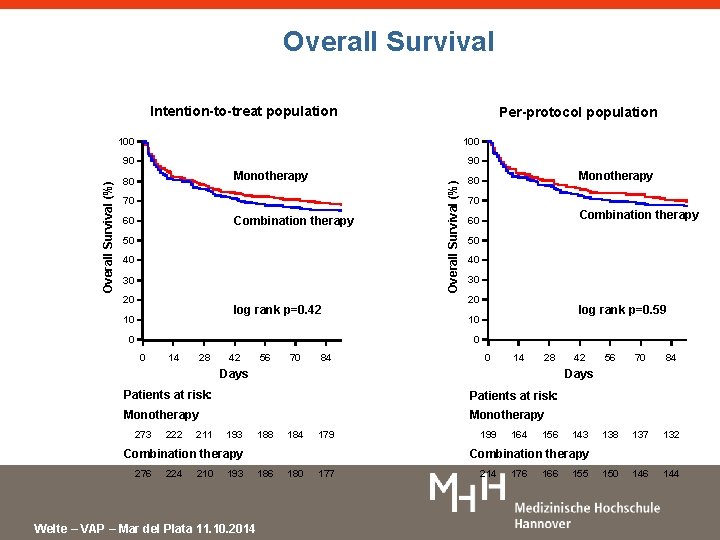
Overall Survival Intention-to-treat population Per-protocol population 100 90 Monotherapy 80 70 Combination therapy 60 50 40 30 20 log rank p=0. 42 10 Overall Survival (%) 90 Monotherapy 80 70 Combination therapy 60 50 40 30 20 log rank p=0. 59 10 0 14 28 42 56 70 84 0 14 28 Days Patients at risk: Monotherapy 222 211 193 188 184 179 Combination therapy 276 224 210 193 Welte – VAP – Mar del Plata 11. 10. 2014 56 70 84 138 137 132 150 146 144 Days Patients at risk: 273 42 199 164 156 143 Combination therapy 186 180 177 214 176 166 155
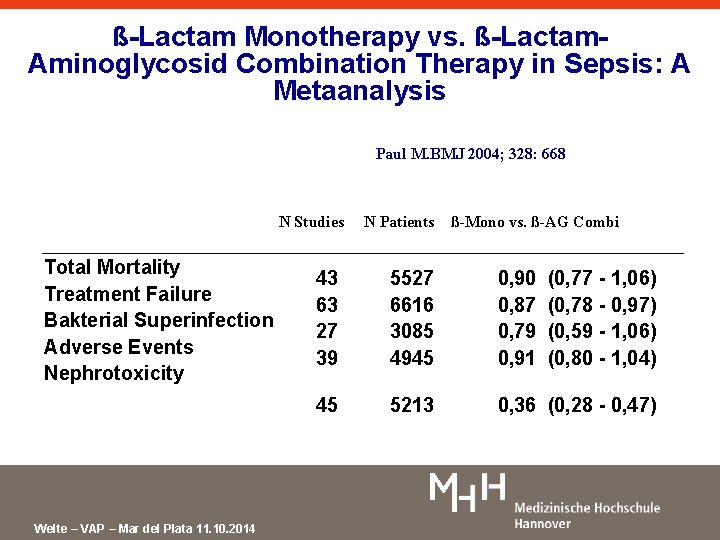
ß-Lactam Monotherapy vs. ß-Lactam. Aminoglycosid Combination Therapy in Sepsis: A Metaanalysis Paul M. BMJ 2004; 328: 668 N Studies Total Mortality Treatment Failure Bakterial Superinfection Adverse Events Nephrotoxicity Welte – VAP – Mar del Plata 11. 10. 2014 N Patients ß-Mono vs. ß-AG Combi 43 63 27 39 5527 6616 3085 4945 0, 90 0, 87 0, 79 0, 91 (0, 77 - 1, 06) (0, 78 - 0, 97) (0, 59 - 1, 06) (0, 80 - 1, 04) 45 5213 0, 36 (0, 28 - 0, 47)

Mono- vs. Combination Therapy for VAP • Randomised controlled trial in 740 pts – Mechanical ventilated – VAP suspected after 4 days in the ICU – Pts. with known Pseudomonas or MRSA excluded • Meropenem 1 g tid + Ciprofloxacin 400 mg bid • vs. Meropenem alone • Outcome Parameters: – No difference in 28 -day mortality (RR 1. 05, p=0. 74) Welte – VAP – Mar del Plata 11. 10. 2014 Heyland D. CCM 2008; 36: 737 -44
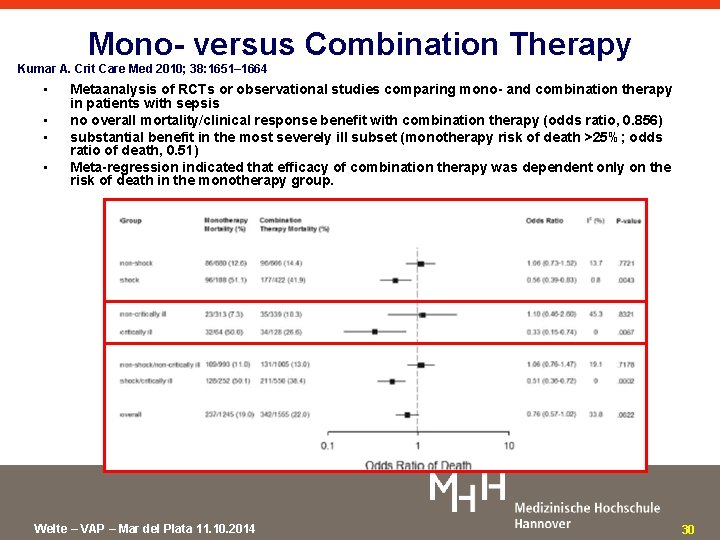
Mono- versus Combination Therapy Kumar A. Crit Care Med 2010; 38: 1651– 1664 • • Metaanalysis of RCTs or observational studies comparing mono- and combination therapy in patients with sepsis no overall mortality/clinical response benefit with combination therapy (odds ratio, 0. 856) substantial benefit in the most severely ill subset (monotherapy risk of death >25%; odds ratio of death, 0. 51) Meta-regression indicated that efficacy of combination therapy was dependent only on the risk of death in the monotherapy group. Welte – VAP – Mar del Plata 11. 10. 2014 30

Pseudomoas aeruginosa Combination Therapy • If combination therapy is required then combine with – + Aminoglycosid • Gentamycin/Tobramycin 6 mg/kg BW per day as a single dosage (Through Level < 2 mg/L) • Amikacin 20 -25 (-30) mg/kg KG BW per day as a single dosage – + Fluorquinolones • Ciprofloxacin (800 -1200 mg tgl. ) • Levofloxacin (1000 mg tgl. ) Welte – VAP – Mar del Plata 11. 10. 2014

Antibiotics Pharmacokinetics in severly ill patients • Charakteristic of severly ill patients – High Cardiac Index – Increased distribution volume – Altered plasma protein binding Welte – VAP – Mar del Plata 11. 10. 2014

Antibiotics Pharmacokinetics in severly ill patients • Consequences – Dosage of antibiotics at the highest approved level (and above) – Take pentrtaion properties into the tissue were the infection is suspected, into account – Combination therapy for MDR pathogenes Welte – VAP – Mar del Plata 11. 10. 2014
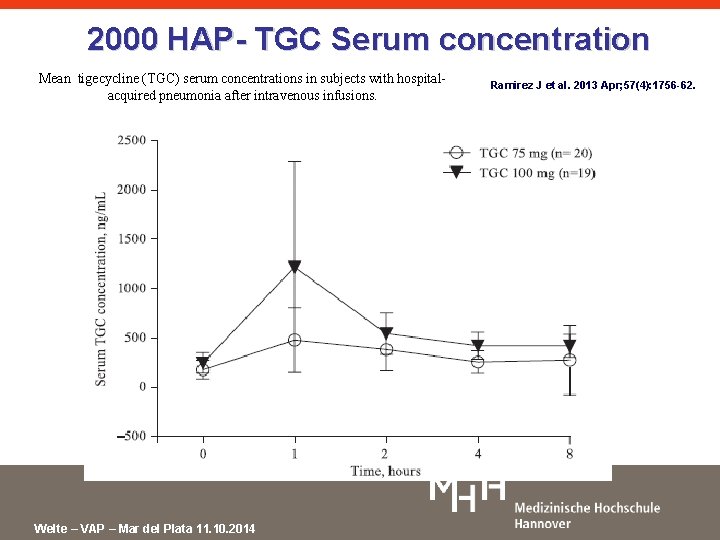
2000 HAP- TGC Serum concentration Mean tigecycline (TGC) serum concentrations in subjects with hospitalacquired pneumonia after intravenous infusions. Welte – VAP – Mar del Plata 11. 10. 2014 Ramirez J et al. 2013 Apr; 57(4): 1756 -62.
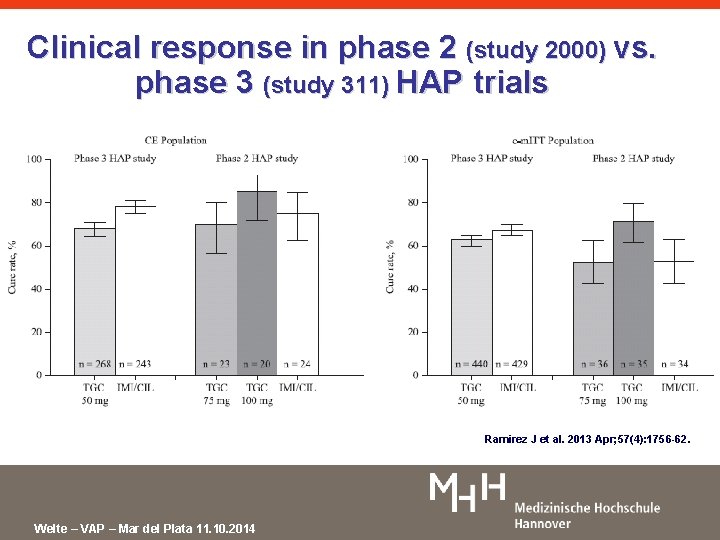
Clinical response in phase 2 (study 2000) vs. phase 3 (study 311) HAP trials Ramirez J et al. 2013 Apr; 57(4): 1756 -62. Welte – VAP – Mar del Plata 11. 10. 2014
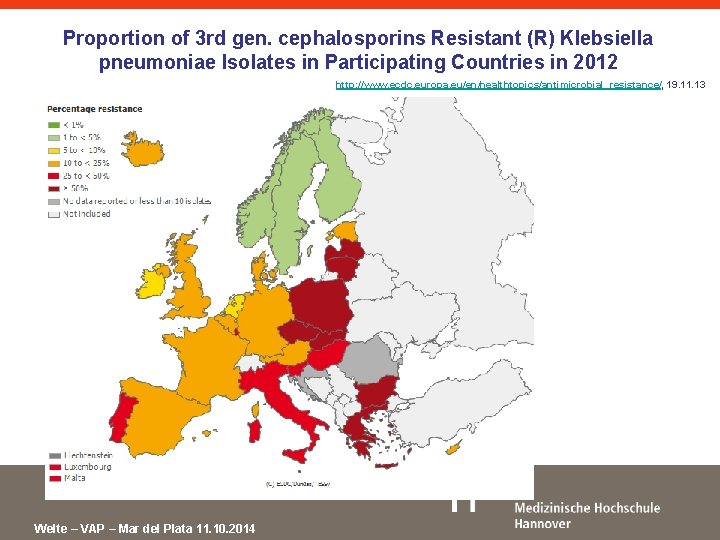
Proportion of 3 rd gen. cephalosporins Resistant (R) Klebsiella pneumoniae Isolates in Participating Countries in 2012 http: //www. ecdc. europa. eu/en/healthtopics/antimicrobial_resistance/, 19. 11. 13 Welte – VAP – Mar del Plata 11. 10. 2014

ESBL Treatment • Carbapenems, Carbapenems …. . Welte – VAP – Mar del Plata 11. 10. 2014
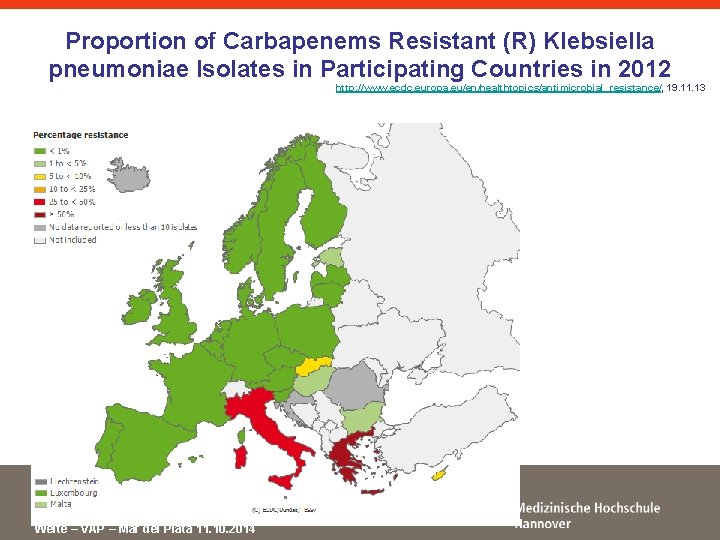
Proportion of Carbapenems Resistant (R) Klebsiella pneumoniae Isolates in Participating Countries in 2012 http: //www. ecdc. europa. eu/en/healthtopics/antimicrobial_resistance/, 19. 11. 13 Welte – VAP – Mar del Plata 11. 10. 2014

Revival of „old“ drugs Tigecyclin Ramirez J et al. 2013 Apr; 57(4): 1756 -62. • Phase II-Study in patients with hospital acquired pneumonia – Tigecyclin 75 mg twice daily – Tigecyclin 100 mg twice daily – Imipenem/Cilastatin 1 g three times a day • Primary Endpoint: Advers Events – No significant difference between the groups • Secondary Endpoint: Clinical Cure – Both tigecyclin groups were non inferior to Imipenem/Cilastatin – High dose tigecyclin was in trend more effective than low dose tigecyclin and imipenem/cilastatin Welte – VAP – Mar del Plata 11. 10. 2014 10

Revival of „old“ drugs Colistin • Combination Therapy (? ) with – Colistin • 9 Mill. E Loading Dose • 4. 5 Mill E twice daily as maintenance therapy • + inhaled colistin ? ? ? Welte – VAP – Mar del Plata 11. 10. 2014

Welte – VAP – Mar del Plata 11. 10. 2014
- Slides: 48