Venous Thromboembolism Diagnosis and Managament R Cavalcanti and

Venous Thromboembolism: Diagnosis and Managament R. Cavalcanti and B. Laluck April, 2007

Learning objectives • Review factors affecting risk of VTE • Understand an approach to diagnosis of VTE • Review aspects of treatment of VTE

Outline • • • Cases Diagnostic algorithm Prophylaxis Type and duration of anticoagulation IVC filters

Case 1 • 68 F Post op day #2 after R TKR • Referred for fever + SOB • PMHx: HTN, osteoporosis, 40 pyr smoker • Meds: Alendronate, Atenolol/HCTZ, Dalteparin 5000, Moxifloxacin • Over 2 d has needed increasing O 2

Case 1 (cont) • OE: w w HR 110 RR 24 BP 90/50 SPO 2 90% on 50%FM T 38. 5 CVS N hs; JVP 4 -5 cm ASA Chest: Fine crackles over bases, long expiratory time • Inv: w CBC: 98 11. 7 318 w Lytes 138 104 3. 5 26 w ABG: 7. 43 34 65 23 on Fi. O 2 0. 5

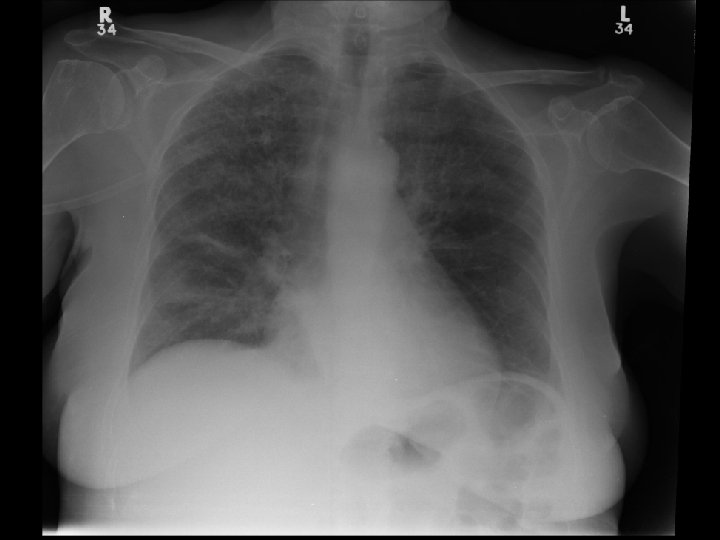

CT Angio Chest • No PE • Diffuse interstitial changes consistent with pulmonary edema • Left lower lobe opacity

Case 2 • 23 F presents with shortness of breath • OCP, smoker and recently flew in from Berlin • Now requires 2 L O 2 NP for Sp. O 2 96%

Case 3 • 83 F presenting with BRBPR w C-Scope: large rectal tumour w Unilateral R leg swelling • Doppler US LE: Positive for DVT • Management?

Tests for VTE • • • Wells score: D-dimers: Venous Doppler US CT Angio Chest VQ scan Conventional pulmonary angiography

Estimating risk

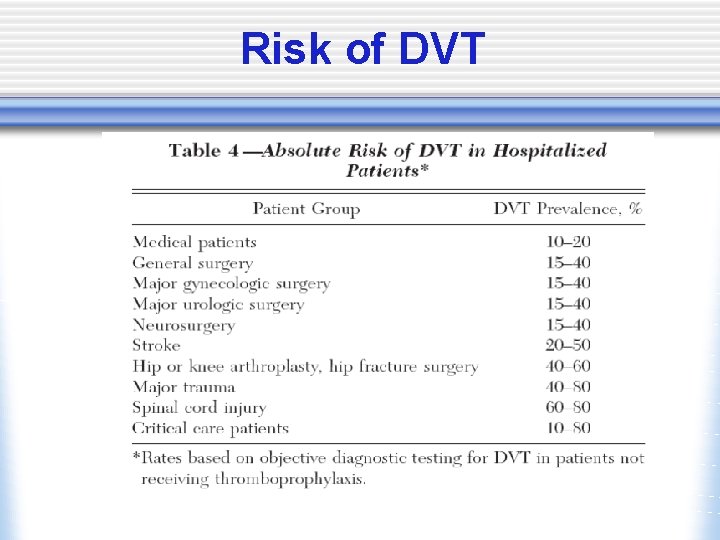
Risk of DVT

Wells Prediction Rule for Diagnosing Deep Venous Thrombosis: Clinical Evaluation Table for Predicting Pretest Probability of Deep Vein Thrombosis Clinical Characteristic Active cancer (treatment ongoing, within previous 6 months, or palliative) 1 Paralysis, paresis, or recent plaster immobilization of the lower extremities 1 Recently bedridden >3 days or major surgery within 12 weeks requiring general or regional anesthesia Localized tenderness along the distribution of the deep venous system Entire leg swollen Calf swelling 3 cm larger than asymptomatic side (10 cm below tibial tuberosity) Pitting edema confined to the symptomatic leg 1 Collateral superficial veins (nonvaricose) Alternative diagnosis at least as likely as deep venous thrombosis – 2 Score 1 1 1 Note: Clinical probability: low 0; intermediate 1– 2; high 3. In patients with symptoms in both legs, the more symptomatic leg is used. Reprinted from The Lancet, Vol 350, Wells PS, Anderson DR, Bormanis J, et al. Value of assessment of pretest probability of deep-vein thrombosis in clinical management, pp 1795– 1798, Copyright 2002, with permission from Elsevier.
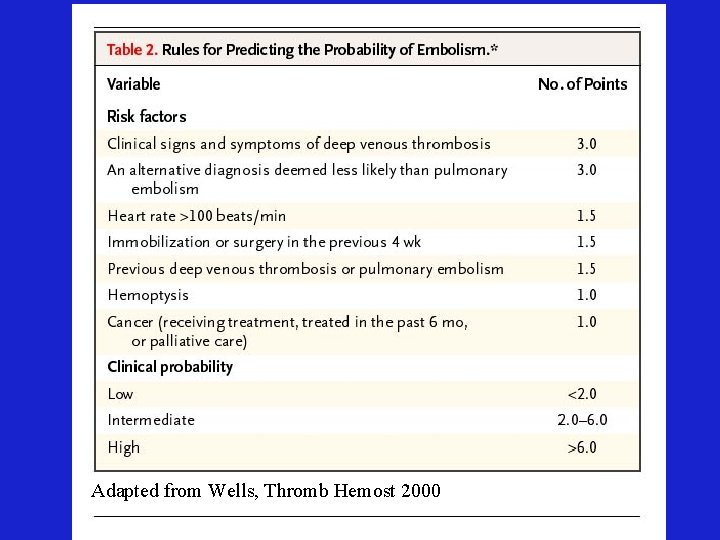
Adapted from Wells, Thromb Hemost 2000

Diagnostic approach

Diagnostic approach • Assess risk • D-dimer • Lung Imaging w CT angiography of Chest w VQ Scan • Leg imaging w CT venography w Venous doppler US

First step • Assess risk w Wells prediction rule § Validated in number of studies (17 DVT / 3 PE) § Induvidual features low predictive value § Works best for younger patients without comorbitidies or a history of VTE § Clinical judgement should be used in older patients with co-morbidities

D-dimer • Usefulness depends on number factors w Sensitivity (must be high or 3 rd generation) w Other reason for + § Any trauma, surgery enough to get blood to clot will elevate D-dimer w Probability of disease • When used alone w In patient’s with comorbidity, older age, longer duration of symptoms in low to moderate risk § Only 40 – 50% specificities

Wells + D-dimer • If you have a patient with low pretest probability of DVT / PE and a HIGH – sensitivity D-dimer is negative w 0. 5% incidence of in 3 months of DVT § No need for further imaging • If you have a patient with mod to high pretest probability of DVT / PE and a HIGH – sensitivity D-dimer is negative w 3. 5% and 21. 4% DVT risk within 3 months w Further imaging needed

Leg Ultrasound performance depends on symptoms • NO SYMPTOMS • Proximal DVT w positive test rules in w negative test DOESN’T rule-out w sensitivity 60% w specificity 90 -95% • SYMPTOMS PRESENT • Proximal DVT w positive test rules in w negative test rules out sensitivity 90 -95% specificity 95% • Distal DVT w positive test rules in w negative test DOESN’T rule out w sensitivity 60%; w specificity 90 -95%

PIOPED II • CT Angio chest w Sn 83% w Sp 96% • CT Angio chest + CT Venography w Sn 90% w Sp 95%
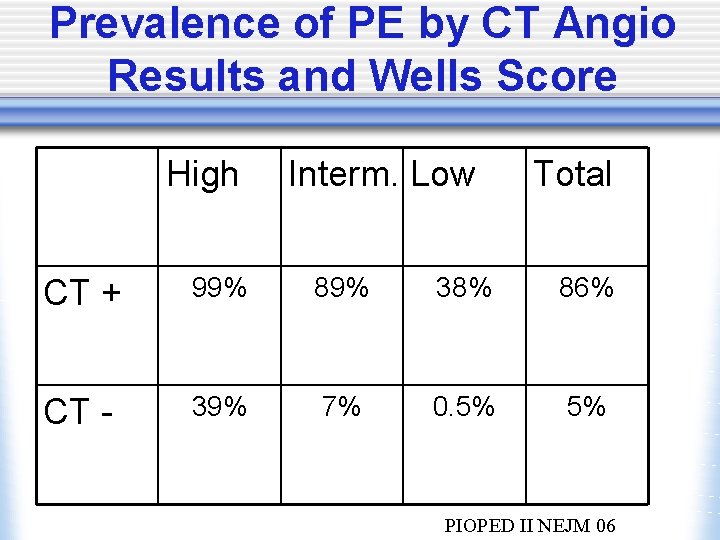
Prevalence of PE by CT Angio Results and Wells Score High Interm. Low Total CT + 99% 89% 38% 86% CT - 39% 7% 0. 5% 5% PIOPED II NEJM 06

Controversy • Are the next generation multidetector CTs better • To what level does the study see clots (segmental, subsegmental? ) • What should come first w Leg doppler vs CTA? • In a patient with a high pretest probability for PE w Is CTA sufficiently sensitive?

VTE Prophylaxis Treating medical and surgical patients at high risk of developing DVT

VTE Prophylaxis - non pharmacological • Mobilization w If possible • Graduated compression stockings (GCS) w TEDS • Intermittent pneumatic compression (IPC) w For surgical patients

VTE Prophylaxis - Rx • Low dose unfractionated heparin (LDUH) w 5000 u sc q 12 h or q 8 h • Low molecular weight heparin intermediate dose (LMWH) w Enoxaparin 30 mg bid or 40 mg od w Dalteparin 5000 u od • Fondaparinux 2. 5 mg sc od

VTE Treatment

VTE Treatment - Rx • High dose unfractionated heparin (UFH) w IV Titrated drip • Low molecular weight heparin treatment dose (LMWH) w Enoxaparin w Tinzaparin w Dalteparin and others • Fondaparinux • Coumadin (INR 2 – 3) w With at least 4 -5 days of heparin • Direct thrombin inhibitors w For patients with HIT (done via hematology)

VTE Treatment • Heparin vs LMWH w Safety and efficacy w Multiple studies § LMWH superior for treatment • Less mortality and major bleeding • Magnitude not very large § LMWH at least as effective as UFH

VTE Treatment • Outpatient vs Inpatient Treatment w Number of studies w Likely that LMWH at home is as least as safe as inpatient treatment for DVT § In appropriately chosen patients with required supports in place

VTE Treatment duration • If OR is only RF - reversible w Recommeded duration 3 months • If ongoing RF w At least 6 months • For ongoing malignancy w LMWH (CLOT trial)

IVC Filters • Limited evidence: no RCTs • Retrievable filters are available w Can be removed up to 6 weeks w Recent case series: 91% retrievable w Risk of migration • Can be adjunctives in patients with existing recent DVT in which anticoagulation contraindicated
- Slides: 34