Venous Thromboembolism Anthony Battad CD MSc MPH FRCPC

Venous Thromboembolism Anthony Battad CD, MSc. , MPH, FRCPC Director // Directeur Ambulatory Care, St. Boniface Hospital // Soins ambulatoire, Hôpital St. Boniface Medical Director //Directeur médical Master of Physician Assistant Studies // Mâitre d’études assitants-médicine University of Manitoba // Université du Manitoba abattad@sbgh. mb. ca

Disclosure • Conference expenses paid for by University of Manitoba • No financial conflicts to disclose
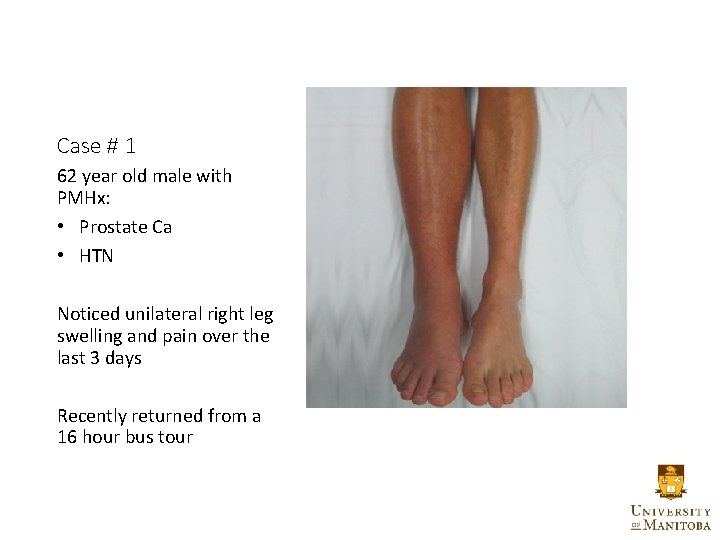
Case # 1 62 year old male with PMHx: • Prostate Ca • HTN Noticed unilateral right leg swelling and pain over the last 3 days Recently returned from a 16 hour bus tour
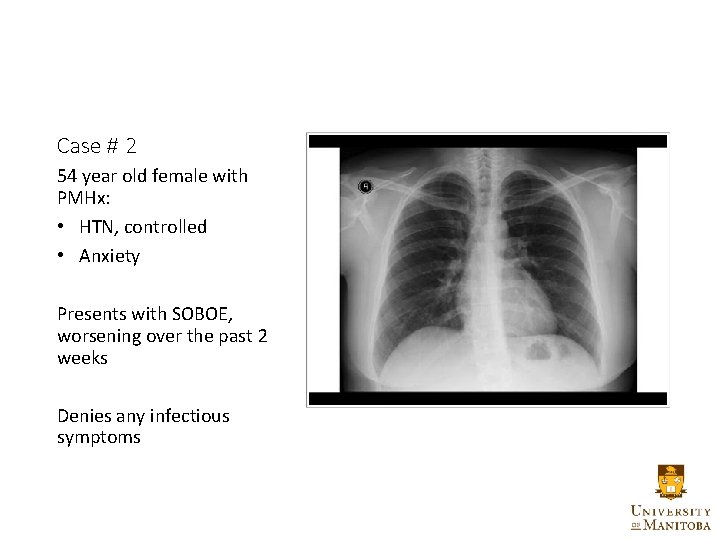
Case # 2 54 year old female with PMHx: • HTN, controlled • Anxiety Presents with SOBOE, worsening over the past 2 weeks Denies any infectious symptoms

Case # 3 28 year old male • In a walking cast for 2 weeks because of 3 o ankle sprain • Now has unilateral right swelling

Objectives • Know the impact of VTE disease on health • Describe the pathogenesis of VTE (DVT and PE) • Recognize the risk factors for VTE • Name the signs and symptoms of DVT and PE • Identify the appropriate diagnosis and treatment of VTE
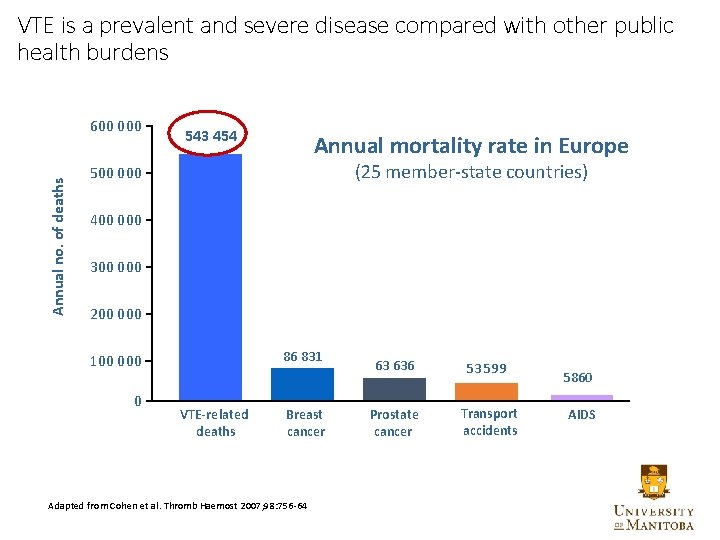
VTE is a prevalent and severe disease compared with other public health burdens Annual no. of deaths 600 000 543 454 Annual mortality rate in Europe (25 member-state countries) 500 000 400 000 300 000 200 000 86 831 100 0 VTE-related deaths Breast cancer Adapted from Cohen et al. Thromb Haemost 2007; 98: 756 -64 63 636 53 599 Prostate cancer Transport accidents 5860 AIDS
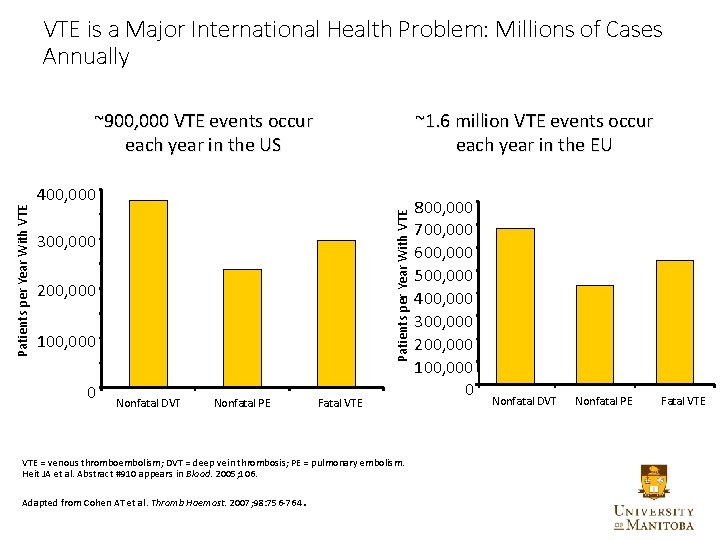
VTE is a Major International Health Problem: Millions of Cases Annually ~1. 6 million VTE events occur each year in the EU 400, 000 Patients per Year With VTE ~900, 000 VTE events occur each year in the US 300, 000 200, 000 100, 000 0 Nonfatal DVT Nonfatal PE Fatal VTE = venous thromboembolism; DVT = deep vein thrombosis; PE = pulmonary embolism. Heit JA et al. Abstract #910 appears in Blood. 2005; 106. Adapted from Cohen AT et al. Thromb Haemost. 2007; 98: 756 -764 . 800, 000 700, 000 600, 000 500, 000 400, 000 300, 000 200, 000 100, 000 0 Nonfatal DVT Nonfatal PE Fatal VTE

Incidence of VTE in Canada • ~ 45, 000 patients in Canada are affected by deep vein thrombosis (DVT) each year 1 • Among those who develop DVT 2: • One-third will have long term complications such as chronic lower leg edema, post-phlebitic syndrome, pain, pigment changes • One-third will develop a recurrent event within 10 years • Despite adequate therapy, 1% to 8% of patients in whom pulmonary embolism develops, will die 2 1. Thrombosis Canada, 2013, Clinical Guides, Venous Thromboembolism; http: //thrombosiscanada. ca/ 2. Scarvelis et al, CMAJ 2006; 175(9) 1087 -92
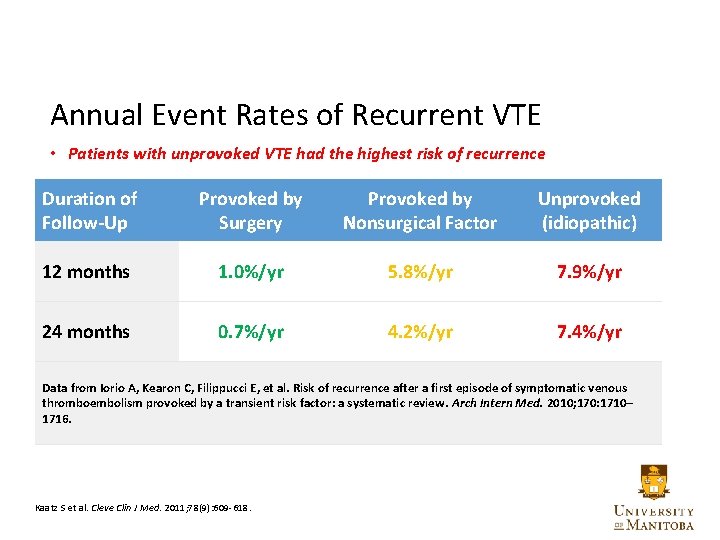
Annual Event Rates of Recurrent VTE • Patients with unprovoked VTE had the highest risk of recurrence Duration of Follow-Up Provoked by Surgery Provoked by Nonsurgical Factor Unprovoked (idiopathic) 12 months 1. 0%/yr 5. 8%/yr 7. 9%/yr 24 months 0. 7%/yr 4. 2%/yr 7. 4%/yr Data from Iorio A, Kearon C, Filippucci E, et al. Risk of recurrence after a first episode of symptomatic venous thromboembolism provoked by a transient risk factor: a systematic review. Arch Intern Med. 2010; 170: 1710– 1716. Kaatz S et al. Cleve Clin J Med. 2011; 78(9): 609 -618. 10

Pathophysiology of VTE Hypercoagulability Virchow’s Endothelial Injury Triad Stasis of Venous Blood Flow Adapted from Kyrle PA et al. Blood 2009; 114: 1138 -1139 11

VTE: Clot Formation Within the Venous Circulation 1 Deep vein thrombosis (DVT) Migration Embolus 2 Pulmonary embolism (PE) Thrombus Tapson VF. N Engl J Med. 2008; 358: 1037 -1052. Image adapted from Tapson VF. 12
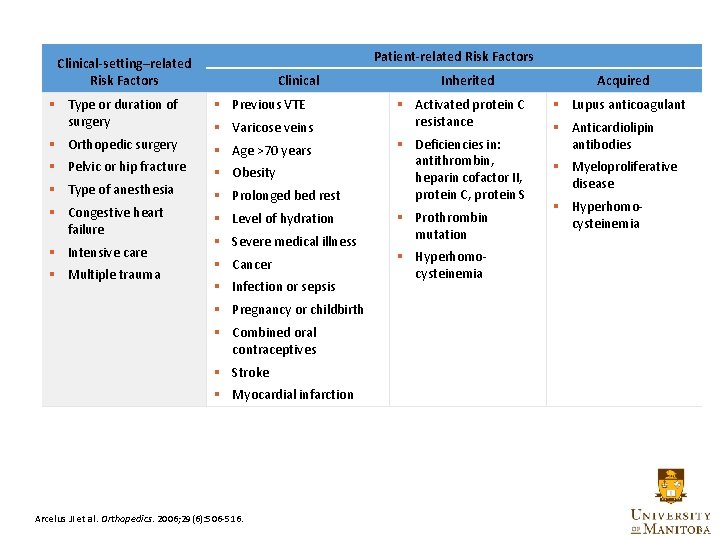
Patient-related Risk Factors Clinical-setting–related Risk Factors Clinical § Type or duration of surgery § Previous VTE § Orthopedic surgery § Age >70 years § Pelvic or hip fracture § Type of anesthesia § Congestive heart failure § Intensive care § Multiple trauma § Varicose veins § Obesity § Prolonged bed rest § Level of hydration § Severe medical illness § Cancer § Infection or sepsis Inherited § Activated protein C resistance § Deficiencies in: antithrombin, heparin cofactor II, protein C, protein S § Prothrombin mutation Acquired § Lupus anticoagulant § Anticardiolipin antibodies § Myeloproliferative disease § Hyperhomo- cysteinemia § Pregnancy or childbirth § Combined oral contraceptives § Stroke § Myocardial infarction Arcelus JI et al. Orthopedics. 2006; 29(6): 506 -516. 13
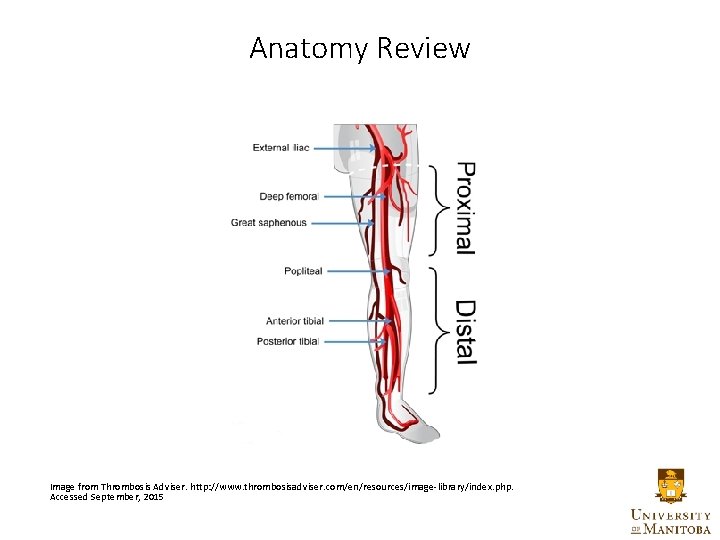
Anatomy Review Image from Thrombosis Adviser. http: //www. thrombosisadviser. com/en/resources/image-library/index. php. Accessed September, 2015

Proximal vs. Distal DVT Proximal DVT • > 90% of acute PE due to proximal DVT • Iliac, femoral, and popliteal veins • Associated with chronic risk factors: • Active malignancy, CHF, age > 75, chronic respiratory disese • ~ 50% untreated DVT PE within 3 months • Higher 3 month mortality than distal DVT Distal DVT • Small veins of the calf • Associated with transient risk factors: • Recent surgery • Immobilization • Travel • 25% - 33% of untreated and symptomatic distal DVT extend proximally • Proximal extensions treated as if they originated in proximal vein

Upper Extremity DVT • 4% to 11% of all DVT 1 • Risk Factors • CVL placement • Malignancy • Hospitalization • Less incidence of pain • Less likely to have PE at time of diagnosis • Rates of recurrent VTE and death similar to lower extremity VTE 1. Muñoz FJ et al. Chest. 2008; 133(1): 143 -148. http: //dx. doi. org/10. 1378/chest. 07 -1432 2. Joffe HV et al. Circulation. 2004; 110: 1605 -1611. 3. Mai C, Hunt D. Am J Med. 2011; 124(5): 402 -407.

Clinical Presentation: Signs and Symptoms 1 -4 DVT • • • Pain Swelling Tenderness Discoloration Pitting edema Left image from National Blood Clot Alliance. http: //www. stoptheclot. org/learn_more/learn_thrombosis. htm. Accessed September 2015. Right image from University of Maryland Medical Center. http: //www. umm. edu/patiented/articles/000583. htm. Accessed September, 2015 1. 2. 3. 4. PE • • • Shortness of breath Cough Chest pain Tachycardia Hypotension Low-grade fever Image from Medic Scientist. http: //medicscientist. com/chest-pain-differentialdiagnosis. Accessed September, 2015. Moll S. Arterioscler Thromb Vasc Biol. 2008; 28(3): 373 -379. Pai M et al. http: //www. uptodate. com/contents/deep-vein-thrombosis-dvt-beyond-the-basics Accessed September 2015 Thompson et al. http: //www. uptodate. com/contents/pulmonary-embolism-beyond-the-basics Accessed September 2015 Goldhaber SZ. Pulmonary Embolism. In: Bonow RO, Mann DL, Zipes DP, Libby P, Braunwald E, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine, 9 th ed. Philadelphia, PA: Elsevier, 2012. 17
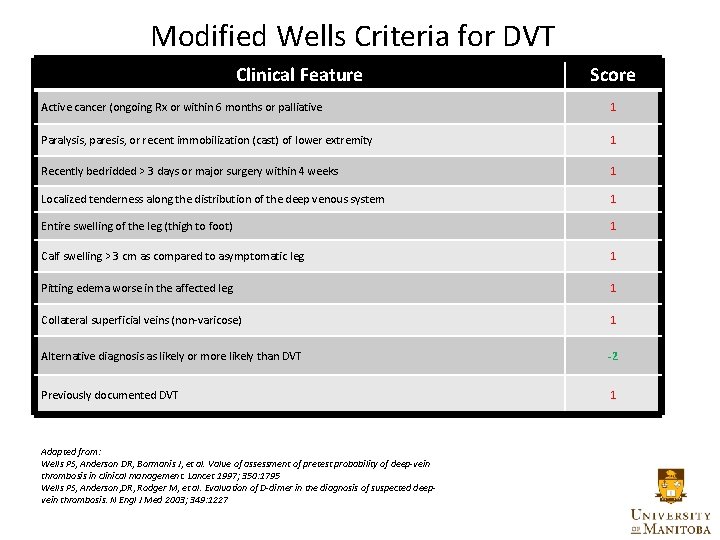
Modified Wells Criteria for DVT Clinical Feature Score Active cancer (ongoing Rx or within 6 months or palliative 1 Paralysis, paresis, or recent immobilization (cast) of lower extremity 1 Recently bedridded > 3 days or major surgery within 4 weeks 1 Localized tenderness along the distribution of the deep venous system 1 Entire swelling of the leg (thigh to foot) 1 Calf swelling > 3 cm as compared to asymptomatic leg 1 Pitting edema worse in the affected leg 1 Collateral superficial veins (non-varicose) 1 Alternative diagnosis as likely or more likely than DVT -2 Previously documented DVT 1 Adapted from: Wells PS, Anderson DR, Bormanis J, et al. Value of assessment of pretest probability of deep-vein thrombosis in clinical management. Lancet 1997; 350: 1795 Wells PS, Anderson, DR, Rodger M, et al. Evaluation of D-dimer in the diagnosis of suspected deepvein thrombosis. N Engl J Med 2003; 349: 1227

Modified Wells Scoring • 2 or greater DVT likely • 1 or less DVT unlikely • Modified Wells score takes into account D-Dimer • (eg) if DVT unlikely (score 1 or less), negative D-Dimer rules out DVT
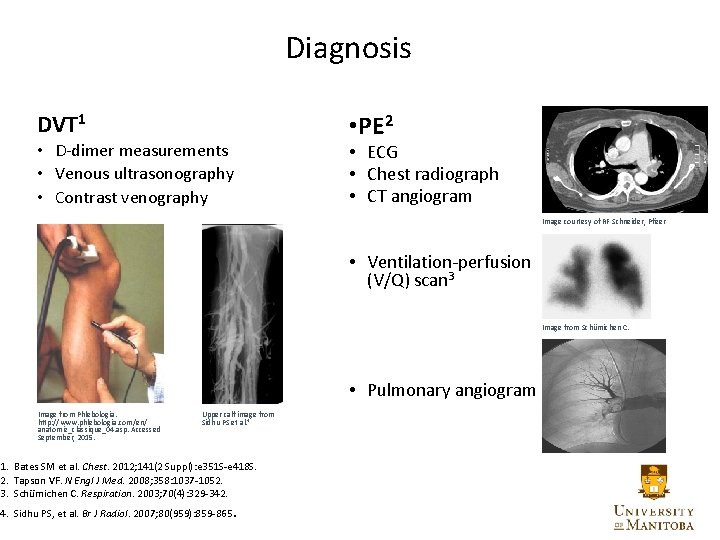
Diagnosis DVT 1 • D-dimer measurements • Venous ultrasonography • Contrast venography • PE 2 • ECG • Chest radiograph • CT angiogram Image courtesy of RF Schneider, Pfizer • Ventilation-perfusion (V/Q) scan 3 Image from Schümichen C. • Pulmonary angiogram Image from Phlebologia. http: //www. phlebologia. com/en/ anatomie_classique_04. asp. Accessed September, 2015. Upper calf image from Sidhu PS et al. 4 1. Bates SM et al. Chest. 2012; 141(2 Suppl): e 351 S-e 418 S. 2. Tapson VF. N Engl J Med. 2008; 358: 1037 -1052. 3. Schümichen C. Respiration. 2003; 70(4): 329 -342. 4. Sidhu PS, et al. Br J Radiol. 2007; 80(959): 859 -865. 20

Phases of Anticoagulation Treatment for VTE Initial 1 (0 to ~7 days) Risk of Recurrent VTE Parenteral Long-term (~7 days to ~3 months) Extended (~3 months to indefinite) Vitamin K antagonist (VKA) or other agent† Treatment Secondary prevention Time since starting treatment Start of treatment and secondary prevention 2 1. Kearon C et al. Chest. 2012; 141(2 Suppl): e 419 s-e 494 s. 2. Kearon C. J Thromb Haemost. 2012; 10: 507 -511. Completion of treatment 21

Phases of Anticoagulation Treatment for VTE Initial 1 (0 to ~7 days) Long-term (~7 days to ~3 months) Extended (~3 months to indefinite) Risk of Recurrent VTE NOAC/DOAC or Vitamin K Antagonist Treatment Secondary prevention Time since starting treatment Start of treatment and secondary prevention 2 1. Kearon C et al. Chest. 2012; 141(2 Suppl): e 419 s-e 494 s. 2. Kearon C. J Thromb Haemost. 2012; 10: 507 -511. Completion of treatment 22

Treatment Rationale • Do not delay treatment while waiting for diagnostics • Prevent clot extension • Prevent the development of PE • Reduce the risk of recurrence • Limit the development of late complications
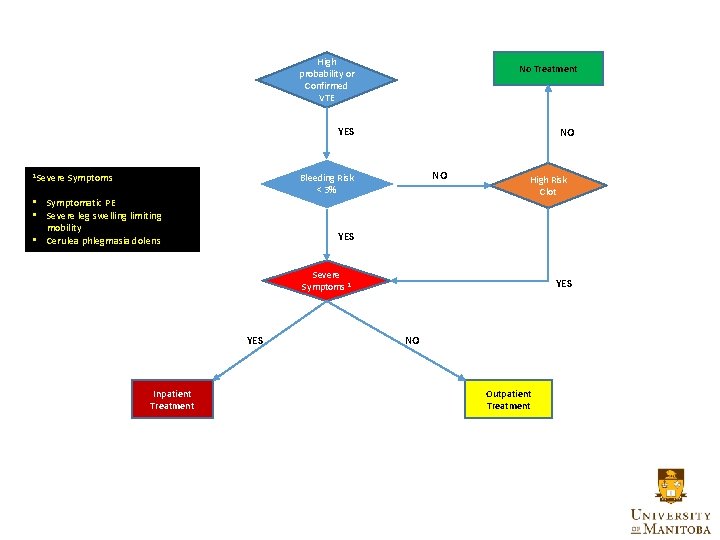
High probability or Confirmed VTE No Treatment YES 1 Severe Symptoms NO NO Bleeding Risk < 3% • Symptomatic PE • Severe leg swelling limiting mobility • Cerulea phlegmasia dolens High Risk Clot YES Severe Symptoms 1 YES Inpatient Treatment YES NO Outpatient Treatment

HAS-BLED Score Courtesy of mayoclinic. org, Accessed October, 2015

Inpatient Treatment • Unfractionated heparin • Fallen out of favour – reserved for patients with decreased renal function • Low molecular weight heparin (LMWH) • Dalteparin • Fondiparinox – synthetic Xa inhibitor • Used in patients with HIT (heparin induced thrombocytopenia) • If using warfarin, start at the same time and overlap for 2 days of therapeutic INR (2 – 3)

Outpatient Treatment • LMWH plus warfarin • Overlap 2 days within therapeutic INR range (2 -3) • New Oral Anticoagulants (NOAC) • Dabigatran – direct thrombin inhibitor • Rivoroxiban – Xa inhibitor • Apixiban – Xa inhibitor • Avoid NOACs in patients with impaired renal function (e. GFR < 30)

A Few Words About NOACs n i r a f r a w , l a. v y o r a p d • Rapid onset and offset • Expensive p o t a r e s fo u use in patients with poor • No monitoring • r. Can’t a i o r f e d renal function it e r • Reliable and predictable c v t o r n p e r p pharmakokinetics • No “anti-dote” r a u e c b gincidence. Vof. ERmajor bleeding n i • Less s U (compared. NEto warfarin) ld u o • w Non-inferior to warfarin • Advantages • Disadvantages

Duration of Treatment • 1 st provoked DVT – 3 months • 2 nd provoked DVT – 6 months • 1 st unprovoked DVT – 3 -6 months (depending on risk of bleeding) • 2 nd unprovoked DVT – indefinite • Documented PE treated for 6 months • 2 nd PE – indefinite anticoagulation
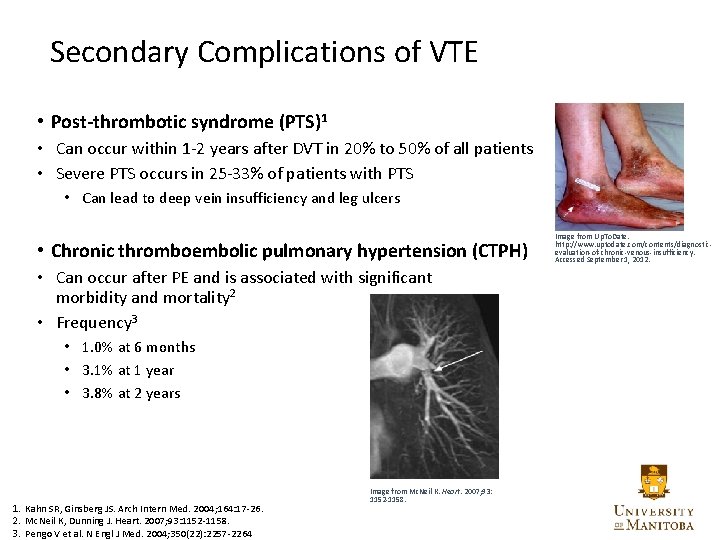
Secondary Complications of VTE • Post-thrombotic syndrome (PTS)1 • Can occur within 1 -2 years after DVT in 20% to 50% of all patients • Severe PTS occurs in 25 -33% of patients with PTS • Can lead to deep vein insufficiency and leg ulcers • Chronic thromboembolic pulmonary hypertension (CTPH) Image from Up. To. Date. http: //www. uptodate. com/contents/diagnosticevaluation-of-chronic-venous-insufficiency. Accessed September 1, 2012. • Can occur after PE and is associated with significant morbidity and mortality 2 • Frequency 3 • 1. 0% at 6 months • 3. 1% at 1 year • 3. 8% at 2 years 1. Kahn SR, Ginsberg JS. Arch Intern Med. 2004; 164: 17 -26. 2. Mc. Neil K, Dunning J. Heart. 2007; 93: 1152 -1158. 3. Pengo V et al. N Engl J Med. 2004; 350(22): 2257 -2264 Image from Mc. Neil K. Heart. 2007; 93: 1152 -1158. 30

Malignancy Screening • Age appropriate screening acceptable • Multi-phase CT of chest, abdomen, pelvis

Back to the cases
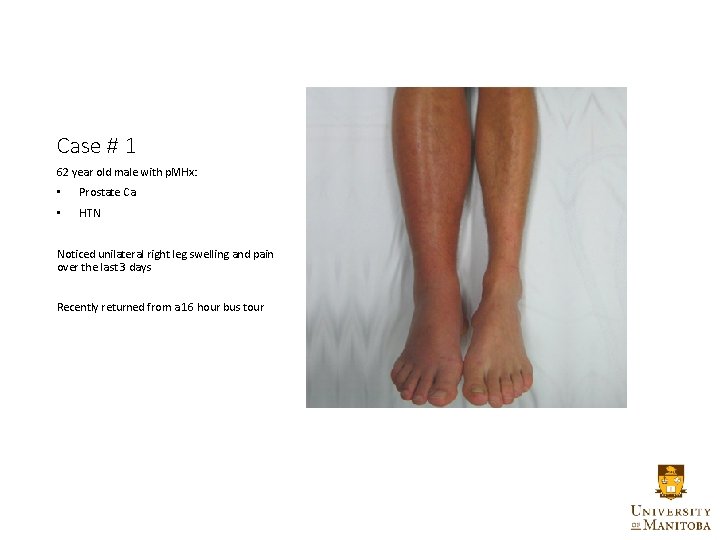
Case # 1 62 year old male with p. MHx: • Prostate Ca • HTN Noticed unilateral right leg swelling and pain over the last 3 days Recently returned from a 16 hour bus tour
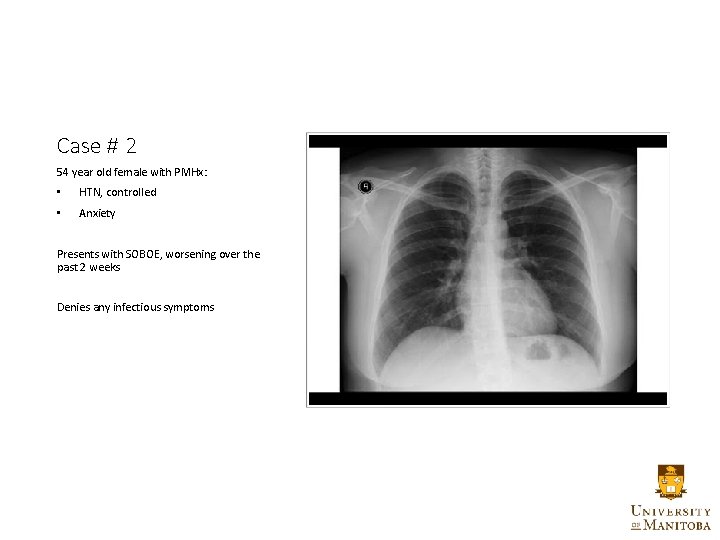
Case # 2 54 year old female with PMHx: • HTN, controlled • Anxiety Presents with SOBOE, worsening over the past 2 weeks Denies any infectious symptoms

Case # 3 28 year old male • In a walking cast for 2 weeks because of 3 o ankle sprain • Now has unilateral right swelling

Thank you. abattad@sbgh. mb. ca
- Slides: 36