Vasectomy Male Sterilization Session V Practicing NoScalpel Vasectomy




















- Slides: 37

Vasectomy (Male Sterilization) Session V: Practicing No-Scalpel Vasectomy Session V, Slide #1

Session 5 Objectives By the end of this session, participants will be able to: 1. Describe how to prepare a client for no-scalpel vasectomy (NSV) 2. List the steps of NSV procedure in the correct sequence 3. Demonstrate the NSV procedure on the model 4. Demonstrate the NSV procedure on a client Session V, Slide #2

Client Preparation for NSV • • Screen for eligibility Informed consent Examination Preoperative instructions Session V, Slide #3

NSV Instruments and Supplies • Two unique instruments – Ringed clamp – Dissecting forceps • Other instruments – Sponge-holding forceps – Scissors – Gallipot • Supplies Ringed Clamp Dissecting Forceps Source Engender. Health 2013 Session V, Slide #4

NSV Procedure: Tasks • Preprocedure tasks—in the preprocedure area/room • Preoperative tasks—in the procedure area • Infiltration with local anesthetic • Delivery and occlusion of the vas • Postprocedure tasks Session V, Slide # 5

Preprocedure Steps • Greet and welcome the client. • Conduct the client evaluation (history and physical examination, review of client card/notes). • Verify informed consent. • Ensure that the client is aware of what will happen during NSV. • Ask the client to void his bladder and prepare for the procedure. • Ensure that the procedure area is set in readiness. Session V, Slide # 6

Preprocedure Steps in the Procedure Area • Assist the client onto the operation table/couch. • Set up instruments and supplies. • Examine the external genitalia. • Do a surgical scrub and put on a gown. • Communicate with the client. • Expose the operation site. • Assume appropriate positioning (on the client’s right side) Session V, Slide # 7

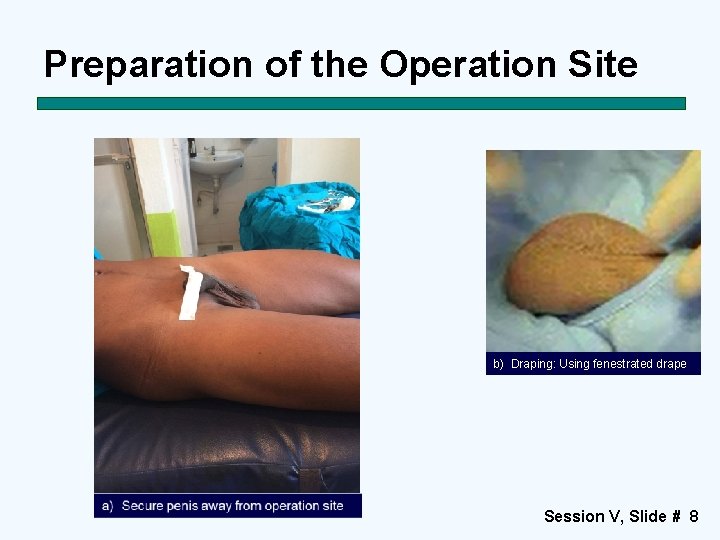
Preparation of the Operation Site b) Draping: Using fenestrated drape Session V, Slide # 8

Pain Management during and Immediately after NSV • • • Local anesthesia (1 or 2% lidocaine) 5 ml of 2% or 10 ml of 1% lidocaine solution Not exceeding maximum recommended dosage 4. 5 mg/kg Side effects and lidocaine toxicity are rare Recent advances—no-needle administration of local anesthetic – Pain-free – Lower dosage – Counseling, communication with client – Gentle surgical techniques • Use of analgesics in the immediate postoperative period • Scrotal support, rest Session V, Slide # 9

Infiltration with Local Anesthetic: Steps • Communicate with client. • Use 5 ml of 2% lidocaine or 10 ml of 1% lidocaine. • Use three-finger technique. • Raise a small wheal. • Secure the right vas and anesthetize. • Secure the left vas and anesthetize. • WAIT for 2 minutes for optimum anesthetic effect. Session V, Slide # 10

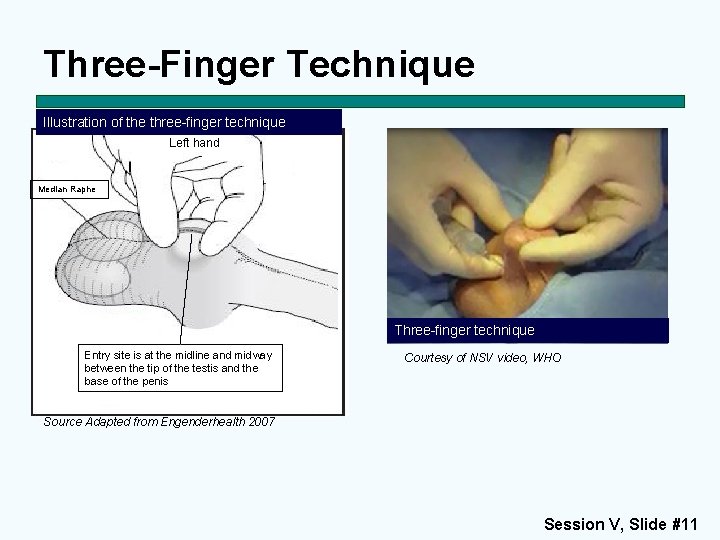
Three-Finger Technique Illustration of the three-finger technique Left hand Median Raphe Three-finger technique Entry site is at the midline and midway between the tip of the testis and the base of the penis Courtesy of NSV video, WHO Source Adapted from Engenderhealth 2007 Session V, Slide #11

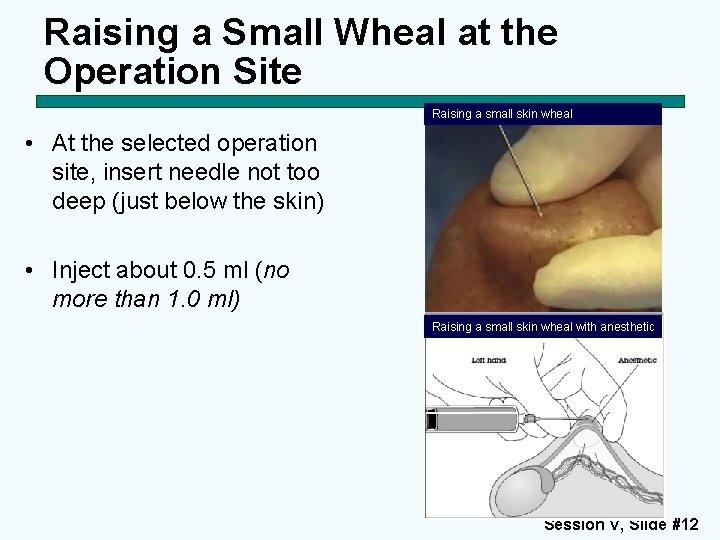
Raising a Small Wheal at the Operation Site Raising a small skin wheal • At the selected operation site, insert needle not too deep (just below the skin) • Inject about 0. 5 ml (no more than 1. 0 ml) Raising a small skin wheal with anesthetic Session V, Slide #12

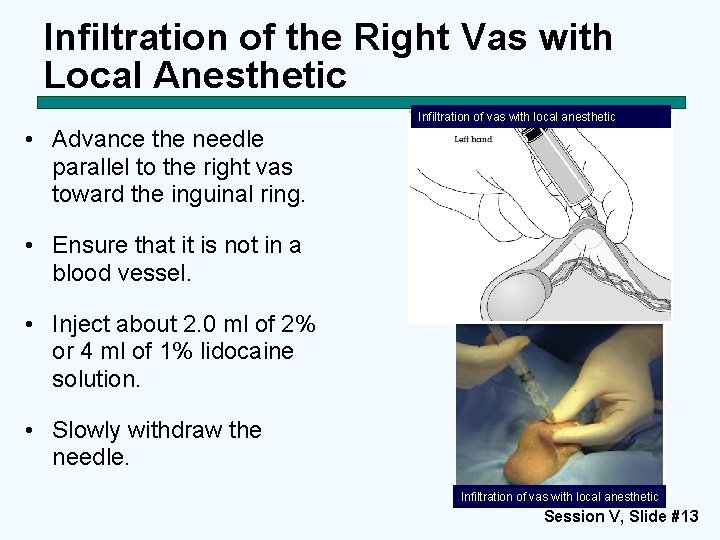
Infiltration of the Right Vas with Local Anesthetic Infiltration of vas with local anesthetic • Advance the needle parallel to the right vas toward the inguinal ring. • Ensure that it is not in a blood vessel. • Inject about 2. 0 ml of 2% or 4 ml of 1% lidocaine solution. • Slowly withdraw the needle. Infiltration of vas with local anesthetic Session V, Slide #13

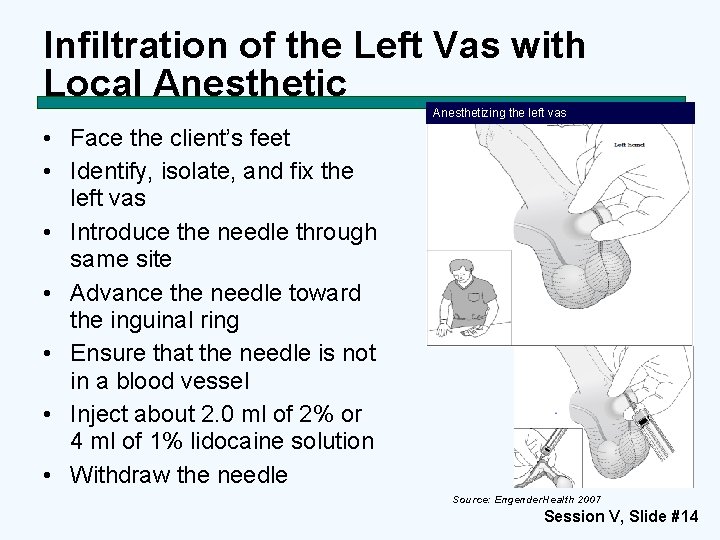
Infiltration of the Left Vas with Local Anesthetic Anesthetizing the left vas • Face the client’s feet • Identify, isolate, and fix the left vas • Introduce the needle through same site • Advance the needle toward the inguinal ring • Ensure that the needle is not in a blood vessel • Inject about 2. 0 ml of 2% or 4 ml of 1% lidocaine solution • Withdraw the needle Source: Engender. Health 2007 Session V, Slide #14

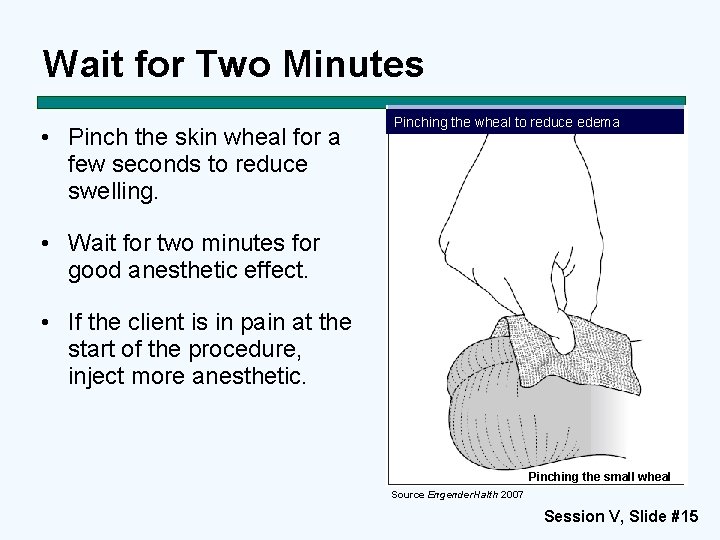
Wait for Two Minutes • Pinch the skin wheal for a few seconds to reduce swelling. Pinching the wheal to reduce edema • Wait for two minutes for good anesthetic effect. • If the client is in pain at the start of the procedure, inject more anesthetic. Pinching the small wheal Source Engender. Halth 2007 Session V, Slide #15

Delivering and Occluding the Vas • Secure the right vas (using the three-finger technique). • Grasp the right vas (using the ringed clamp forceps). • Puncture the skin (using the dissecting forceps). • Deliver the right vas. • Strip the sheath from the right vas. • Occlude vas by ligation and excision or by cautery. • Continue communicating with the client throughout the procedure. Session V, Slide #16

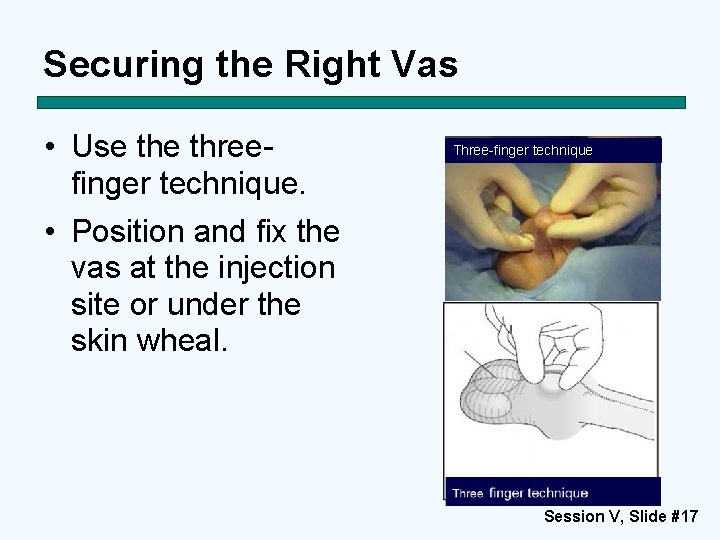
Securing the Right Vas • Use threefinger technique. • Position and fix the vas at the injection site or under the skin wheal. Three-finger technique Session V, Slide #17

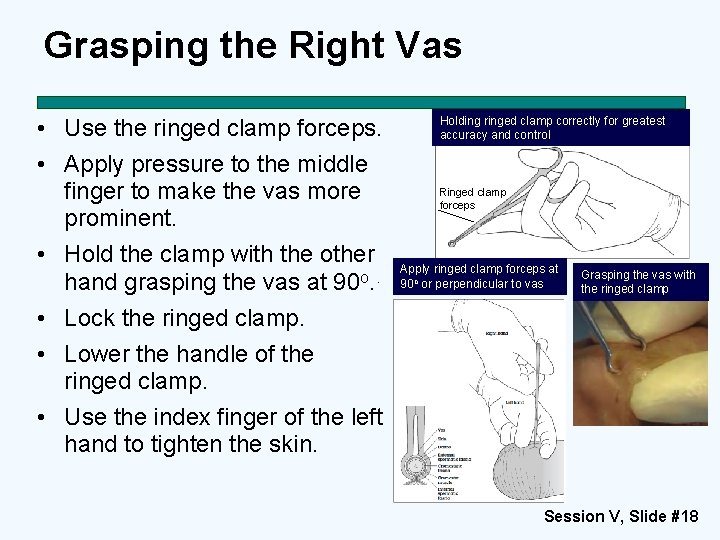
Grasping the Right Vas • Use the ringed clamp forceps. • Apply pressure to the middle finger to make the vas more prominent. • Hold the clamp with the other hand grasping the vas at 90 o. . • Lock the ringed clamp. • Lower the handle of the ringed clamp. • Use the index finger of the left hand to tighten the skin. Holding ringed clamp correctly for greatest accuracy and control Ringed clamp forceps Apply ringed clamp forceps at 90 o or perpendicular to vas Grasping the vas with the ringed clamp Session V, Slide #18

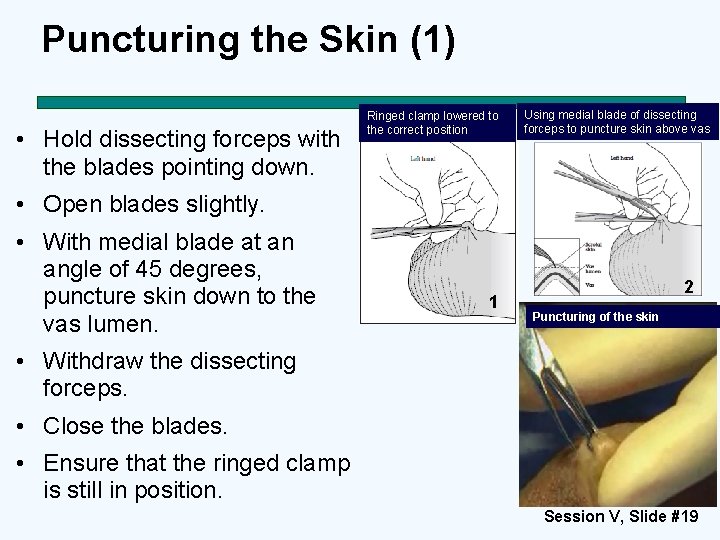
Puncturing the Skin (1) • Hold dissecting forceps with the blades pointing down. Ringed clamp lowered to the correct position Using medial blade of dissecting forceps to puncture skin above vas • Open blades slightly. • With medial blade at an angle of 45 degrees, puncture skin down to the vas lumen. 1 2 Puncturing of the skin • Withdraw the dissecting forceps. • Close the blades. • Ensure that the ringed clamp is still in position. Session V, Slide #19

Puncturing the Skin (2) • The blades should be pointing downward and at a 45 -degree angle. • Insert both blades into the puncture site. • Gently open the blades to spread the tissues and widen the puncture opening. • Withdraw the dissecting forceps. • Keep the ringed clamp in position. Spreading the tissues Session V, Slide #20

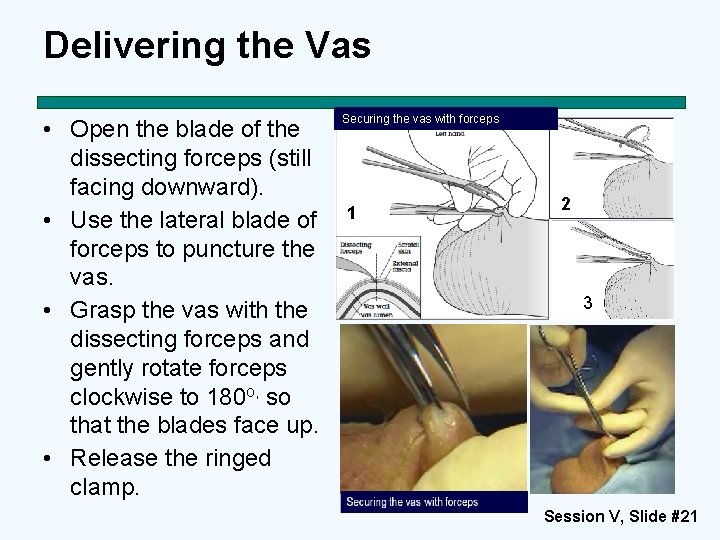
Delivering the Vas • Open the blade of the dissecting forceps (still facing downward). • Use the lateral blade of forceps to puncture the vas. • Grasp the vas with the dissecting forceps and gently rotate forceps clockwise to 180 o, so that the blades face up. • Release the ringed clamp. Securing the vas with forceps 1 2 3 Session V, Slide #21

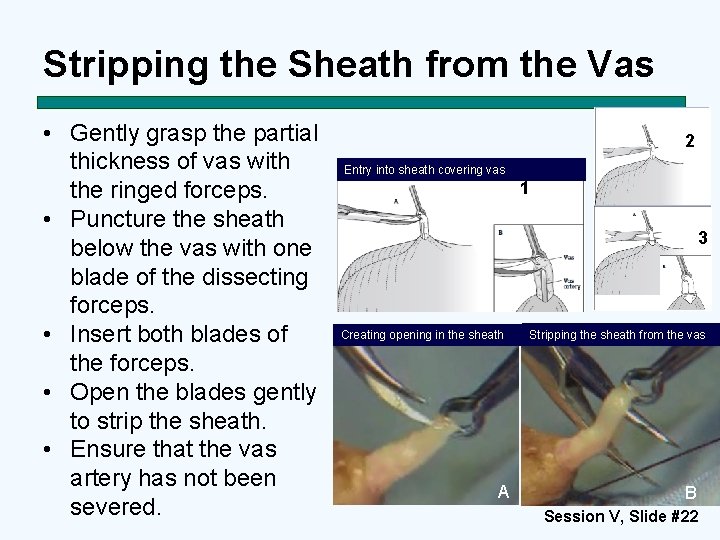
Stripping the Sheath from the Vas • Gently grasp the partial thickness of vas with the ringed forceps. • Puncture the sheath below the vas with one blade of the dissecting forceps. • Insert both blades of the forceps. • Open the blades gently to strip the sheath. • Ensure that the vas artery has not been severed. 2 Entry into sheath covering vas 1 3 Creating opening in the sheath A Stripping the sheath from the vas B Session V, Slide #22

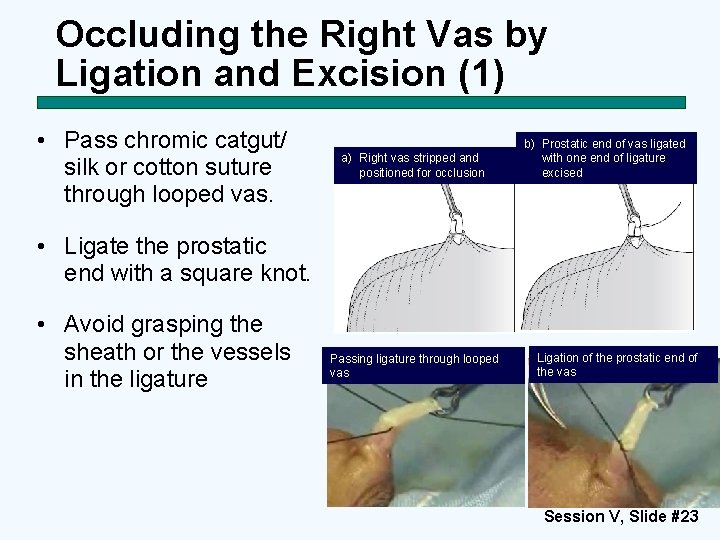
Occluding the Right Vas by Ligation and Excision (1) • Pass chromic catgut/ silk or cotton suture through looped vas. a) Right vas stripped and positioned for occlusion b) Prostatic end of vas ligated with one end of ligature excised • Ligate the prostatic end with a square knot. • Avoid grasping the sheath or the vessels in the ligature Passing ligature through looped vas Ligation of the prostatic end of the vas Session V, Slide #23

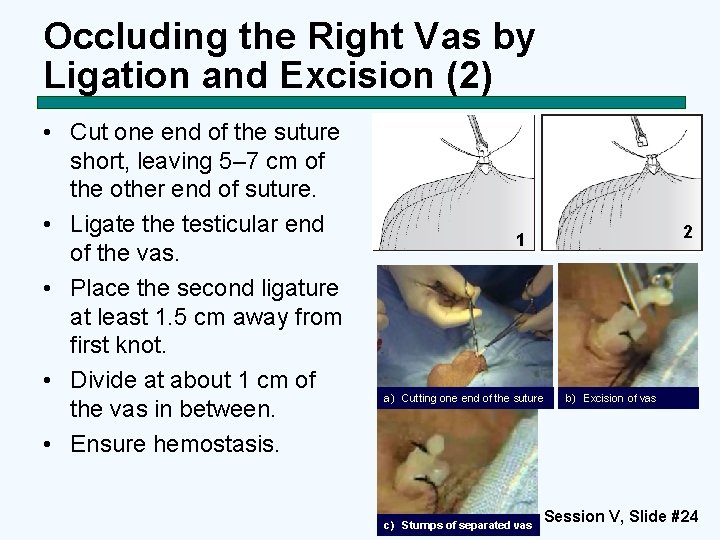
Occluding the Right Vas by Ligation and Excision (2) • Cut one end of the suture short, leaving 5– 7 cm of the other end of suture. • Ligate the testicular end of the vas. • Place the second ligature at least 1. 5 cm away from first knot. • Divide at about 1 cm of the vas in between. • Ensure hemostasis. 2 1 a) Cutting one end of the suture c) Stumps of separated vas b) Excision of vas Session V, Slide #24

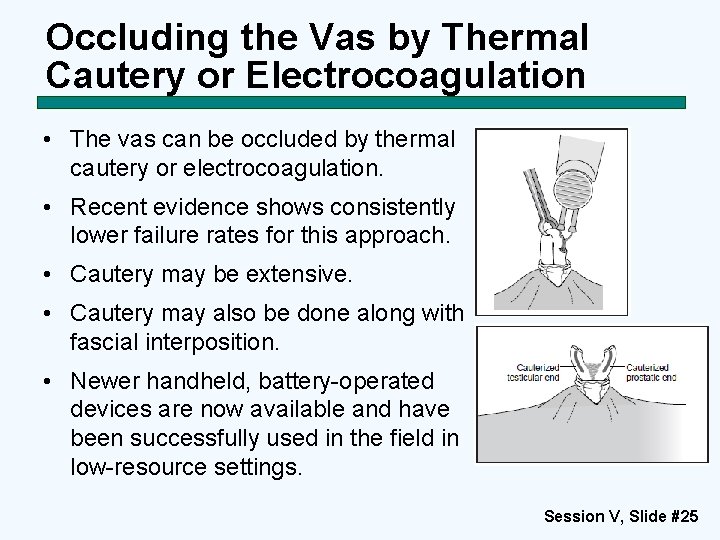
Occluding the Vas by Thermal Cautery or Electrocoagulation • The vas can be occluded by thermal cautery or electrocoagulation. • Recent evidence shows consistently lower failure rates for this approach. • Cautery may be extensive. • Cautery may also be done along with fascial interposition. • Newer handheld, battery-operated devices are now available and have been successfully used in the field in low-resource settings. Session V, Slide #25

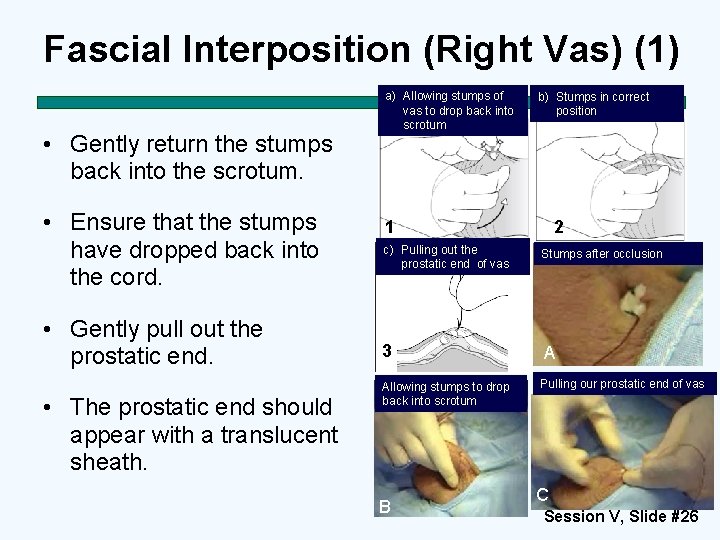
Fascial Interposition (Right Vas) (1) • Gently return the stumps back into the scrotum. • Ensure that the stumps have dropped back into the cord. • Gently pull out the prostatic end. • The prostatic end should appear with a translucent sheath. a) Allowing stumps of vas to drop back into scrotum b) Stumps in correct position 1 2 c) Pulling out the prostatic end of vas Stumps after occlusion 3 A Allowing stumps to drop back into scrotum Pulling our prostatic end of vas B C Session V, Slide #26

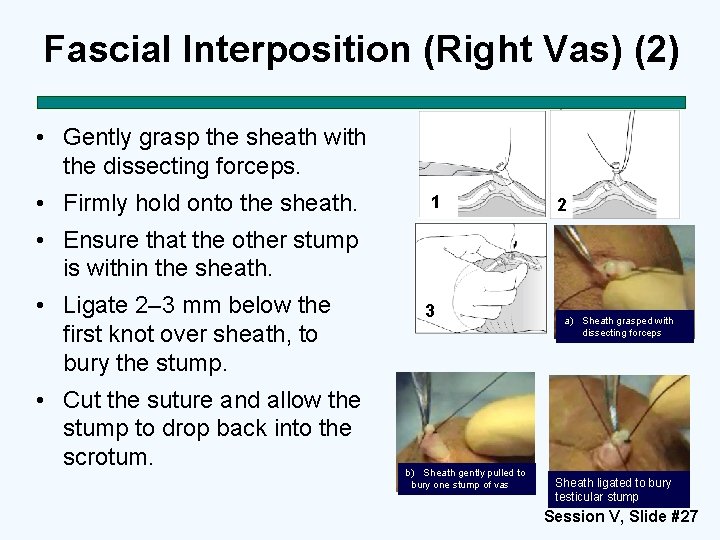
Fascial Interposition (Right Vas) (2) • Gently grasp the sheath with the dissecting forceps. • Firmly hold onto the sheath. 1 2 • Ensure that the other stump is within the sheath. • Ligate 2– 3 mm below the first knot over sheath, to bury the stump. • Cut the suture and allow the stump to drop back into the scrotum. 3 b) Sheath gently pulled to bury one stump of vas a) Sheath grasped with dissecting forceps Sheath ligated to bury testicular stump Session V, Slide #27

Occluding the Left Vas by Ligation and Excision and Fascial Interposition • Fix the left vas. • Use the ringed clamp to secure the vas. • Use the dissecting forceps to open the skin and sheath. • Isolate the left vas and deliver the vas from the scrotum through the same opening (following earlier described steps). • Strip the sheath from the vas. • Ligate the prostatic and testicular ends. • Excise no more than 1 cm of vas. • Perform fascial interposition. Session V, Slide #28

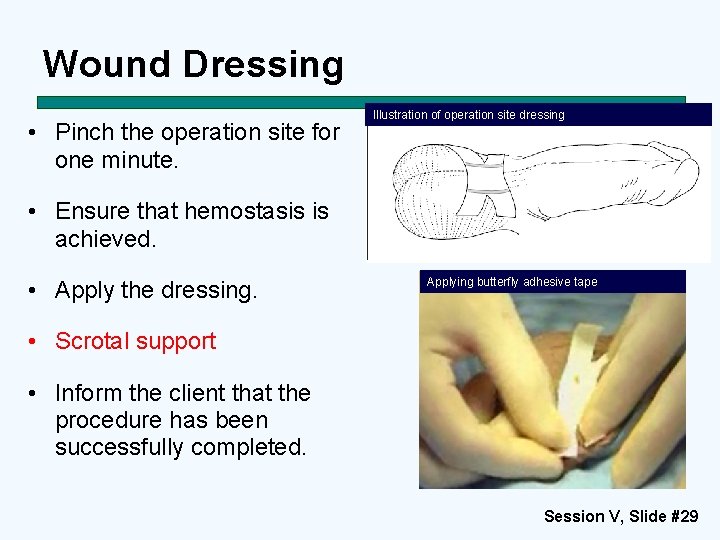
Wound Dressing • Pinch the operation site for one minute. Illustration of operation site dressing • Ensure that hemostasis is achieved. • Apply the dressing. Applying butterfly adhesive tape • Scrotal support • Inform the client that the procedure has been successfully completed. Session V, Slide #29

Postprocedural Tasks • • • Waste disposal Decontamination of instruments Hand hygiene Observation of the client Recording of the procedure Discharge of client with instructions Session V, Slide #30

Roles and Responsibilities of the NSV Team Members • Team consists of the surgeon and the assistant • Surgeon – Reviews history – Verifies informed consent – Performs procedure – Communicates with client • Assistant – Assists in preparation for the procedure – Assists with the surgery – Observes client – Communicates with client Session V, Slide #31

NSV Procedure Video • Purpose of video: demonstrate how to perform NSV • NSV procedure is done by Prof. Li • Introduction to video • Covers on ligation on right vas. . • Discussion… Session V, Slide #32

Demonstration of NSV Procedure • • Demonstration on model Improvised scrotal model Observe and follow steps in learning guide Note points for discussion at end of demonstration Session V, Slide #33

Model Practice • Models – Scrotal model – Improvised model • Instruments and supplies • Care of the scrotal model • Competency-based checklists – Learning guide – Observation checklist • Access to NSV video Session V, Slide #34

Improvised Model for NSV Procedure Practicing the three-finger technique Improvised NSV model Line represents the median raphe Photo Credits: Kaza Ram; Session V, Slide #35

Evaluation of Skills on Models • Trainer(s) will assess newly acquired skills using observation checklists. • All steps must be performed correctly in the proper sequence. • Trainees who master NSV steps on the model will move to supervised clinical practice sessions. Session V, Slide #36

Supervised Clinical Practice on Clients and Evaluation of Skills • Practice will take place in the clinical area. • Clients’ rights: Client consent is needed to observe. • Ensure privacy when discussing clients or the experience. • Demonstrate the procedure. • Perform first case, with assistance from trainer. • Practice under supervision. • Receive evaluation. Session V, Slide #37