VASCULAR LESIONS OF HEAD NECK BED SORES Presenter
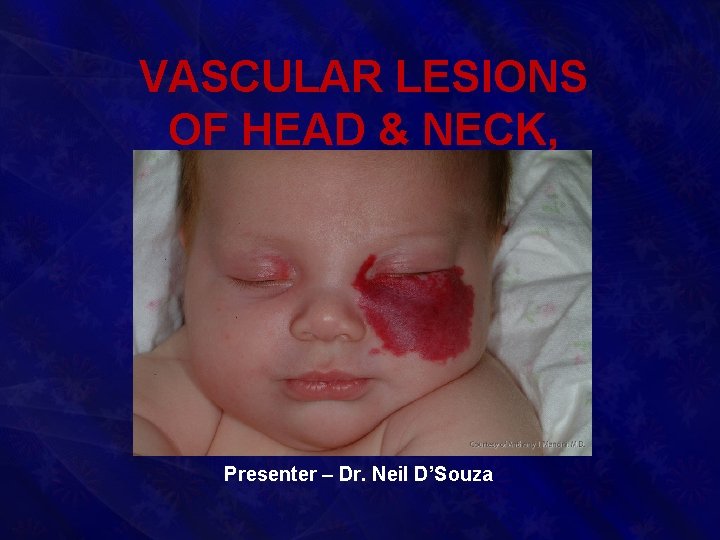
VASCULAR LESIONS OF HEAD & NECK, BED SORES Presenter – Dr. Neil D’Souza

HAEMANGIOMA

• Most common vascular tumour in children (in 10% of term deliveries) • Benign vascular endothelial tumour • Common in girls (3 : 1)
• Onset is few weeks after birth • Biphasic growth showing initial rapid growth with gradual involution over 5 -7 years • Shows cellular endothelial hyperplasia with increased mast cells
• Commonly seen in skin and subcutaneous tissue • Common in head and neck region (60%) • Can occur anywhere in the body like in liver, brain, lungs, other organs

• It grows rapidly in first year and 70% involutes in 7 years • Early proliferative lesion is bright red, irregular; deep lesion is bluish coloured • Involution causes colour fading, softness, shrinkage leaving crepe paper like area
• Head and neck haemangioma is associated with ocular and intracranial anomalies • Ulceration, bleeding, airway block and visual disturbances are common complications. • Platelet trapping and severe thrombocytopenia • Rare, but important life-threatening complication • Presents as ecchymosis, petechiae, intracranial haemorrhage, massive GI bleed

• Raised angiogenic (fibroblastic) growth factor which is secreted in patient’s urine is useful lab investigation

Classification • Capillary • Salmon patch (stork bite) • Strawberry haemangioma • Port-wine stain (naevus flammeus) • Cavernous

CAPILLARY HAEMANGIOMA

Salmon patch (stork bite)

• Presents at birth • Commonly occurs in the nape of the neck (50%), face, scalp and limbs • Usually involves a wide area of skin
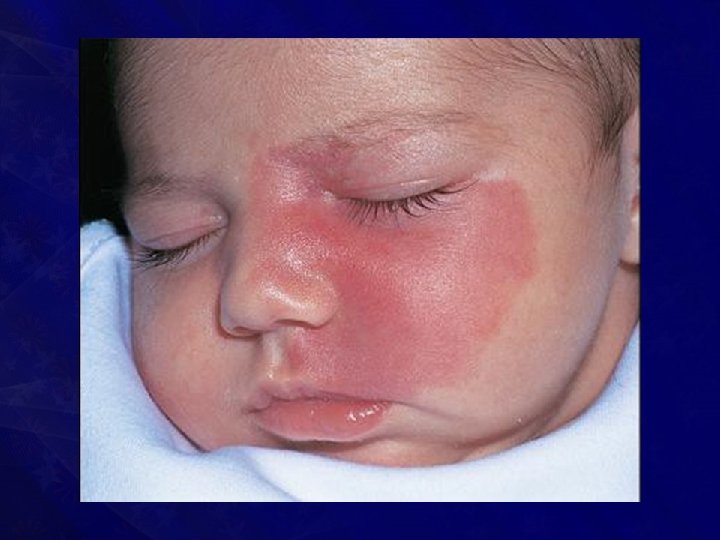
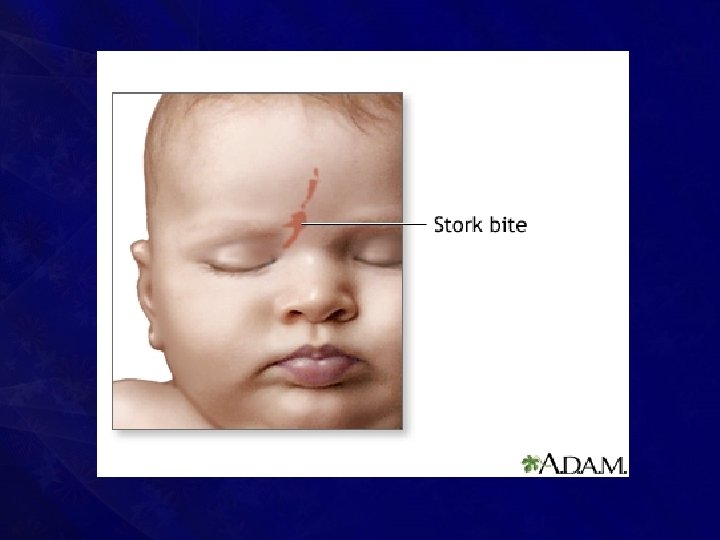

• Caused by an area of persistent fetal dermal circulation • With age, it undergoes spontaneous regression and disappears completely (usually in one year) • Hence masterly inactivity is the treatment

Strawberry haemangioma

• May start at birth • If the child is normal at birth; between one to three weeks it may appear as a red mark which rapidly increases in size within 3 months to form strawberry/raspberry haemangioma
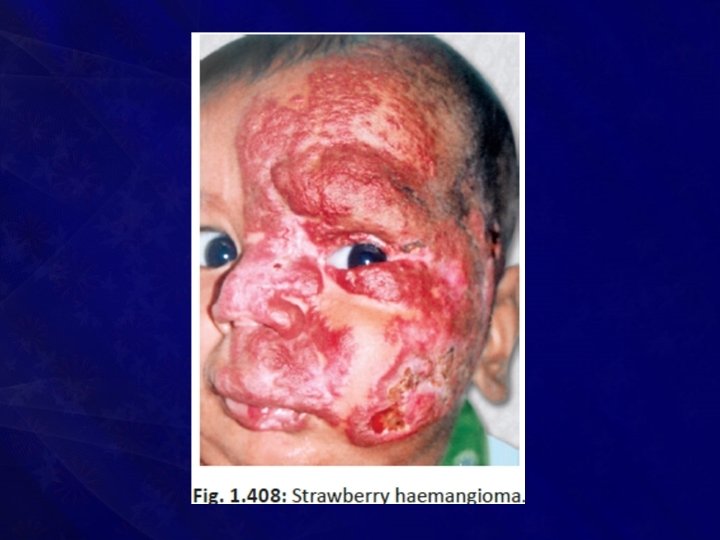

• Contains immature vasoformative tissues • There will eventually be intravascular thrombosis, fibrosis and mast cell infiltration • It is a true capillary haemangioma

• It is 20 times more common than port wine stain. • It is common in white girls • Male to female ratio is 1 : 3 • It is common in head and neck region.

• It is clinically compressible, warm with bluish surface. • Bleeding, ulceration can occur after minor trauma and also • It involves skin, subcutaneous tissues and often muscles

• After one year of age, it slowly begins to fade, and disappears completely in 7 -8 years (70% in 7 years) • It is the most common haemangioma

Port-wine stain (Naevus flammeus)

• It presents at birth and persists throughout life without change • Spontaneous regression will not occur • Due to defect in maturation of sympathetic innervation of skin causing localised vasodilatation of intradermal capillaries

• Presents as • Smooth, flat, reddish blue/intensely purple area • Eventually the surface becomes nodular and keratotic • Common in head, neck and face; • Often within the maxillary and mandibular dermatomes of 5 th cranial nerve
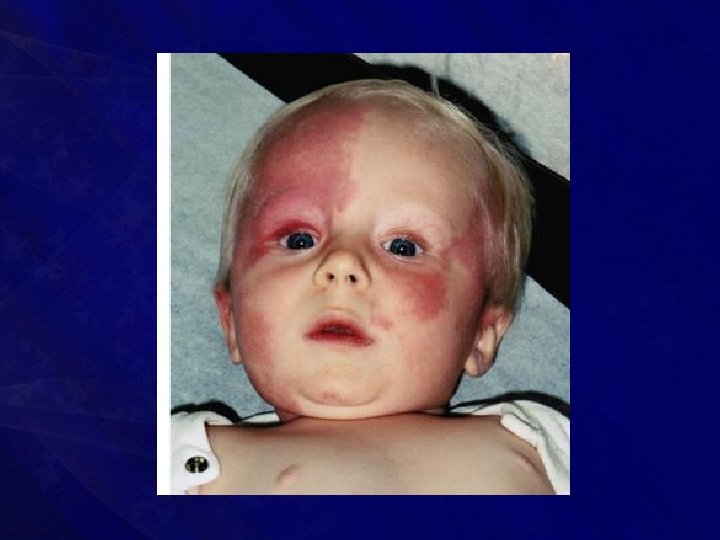
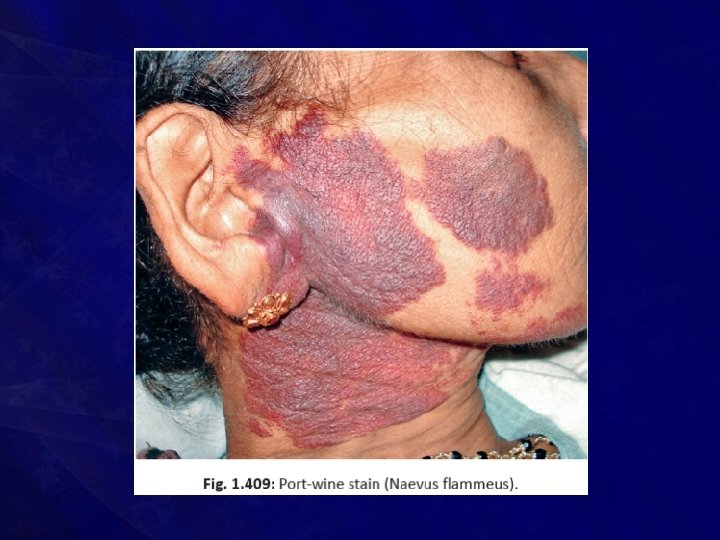

• It is actually a capillary malformation even though considered under haemangioma • It is often associated with • Sturge-Weber syndrome, • Klippel-Trenaunay-Weber syndrome and • Proteus syndrome

Treatment • Wait and watch policy commonly - allowed for spontaneous regression • Pulsed dye laser (diode laser) • Surgical excision and reconstruction • Sclerotherapy/ cryotherapy/ CO 2 snow therapy cause unpleasant scarring

• Indications for surgery or intervention • Uncontrolled growth • Functional impairment like vision or hearing • Accidental haemorrhage
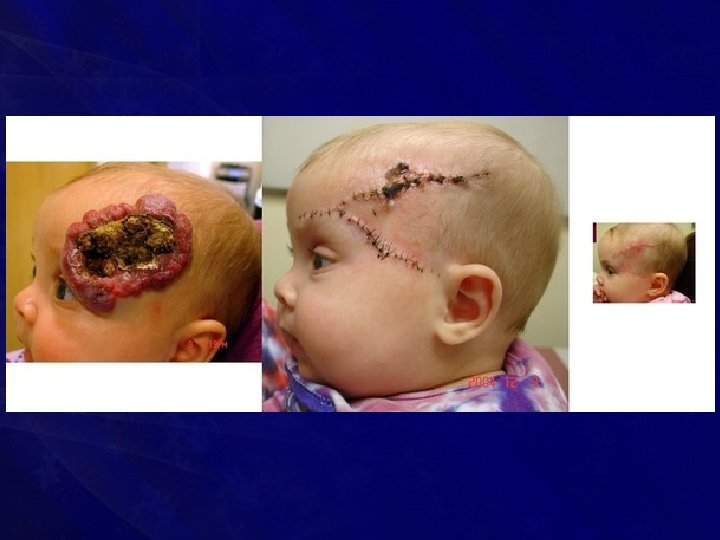

• Feeding vessels may need to be ligated after wide exposure before achieving complete extirpation • Preoperative embolisation facilitates surgical excision and reduces the operative blood loss
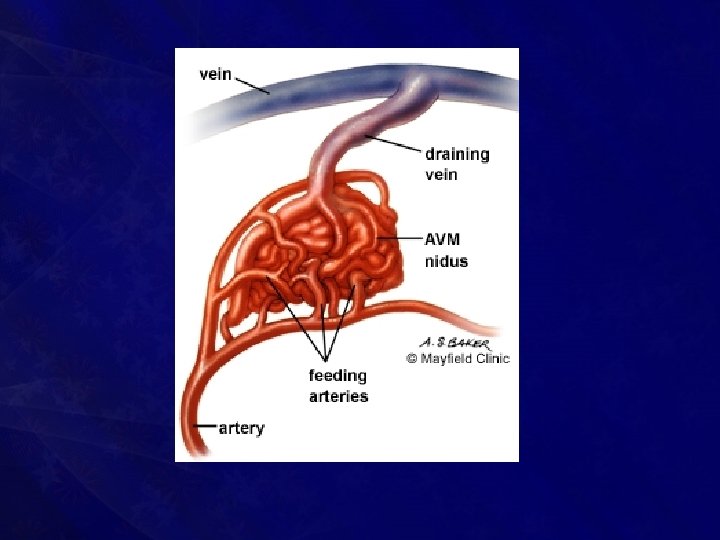
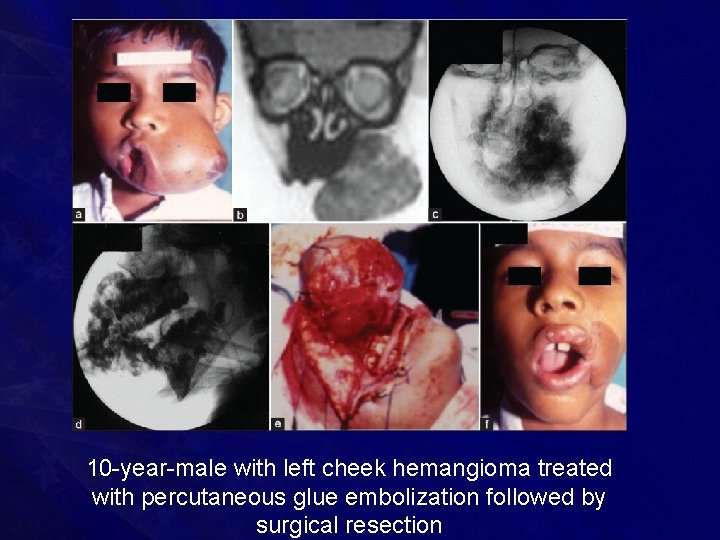
10 -year-male with left cheek hemangioma treated with percutaneous glue embolization followed by surgical resection

• Once embolisation is done, surgery should be done as early as possible otherwise recurrence occurs with enlarged collaterals • Materials used are—foam, plastic spheres, stainless/platinum steel coils, ethanol, polyvinyl alcohol foam of 1000 μmeters size, and rapidly polymerizing acrylic • Done with interventional radiology under. C-Arm guidance

• Rapidly growing haemangioma may need systemic/oral and intralesional steroid therapy • Antiangiogenic interferon 2 a may be useful • Life-threatening platelet trapping may be controlled by cyclophosphamide chemotherapy • Haemangioma with drug resistane can be treated with radiotherapy

CAVERNOUS HAEMANGIOMA

• Presents at birth • Gradually increases in size • Consists of a multiple venous channels • Often mixed with lymphatic component also
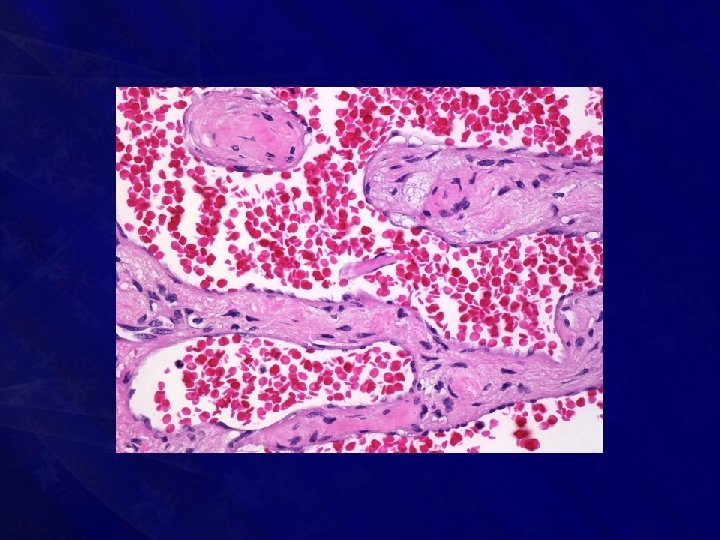

• Sites : • • Head & neck Limbs, Tongue, Liver and other internal organs

• Large or multiple cavernous haemangiomas can cause congestive heart failure (hyperdynamic) due to shunting of large quantity of blood • Cavernous haemangioma with dyschondroplasia is called as Maffucci syndrome

Clinical Features • • • Non-pulsatile swelling Smooth Soft Well localised Warm Fluctuant Compressible Bluish surface Non-transilluminant
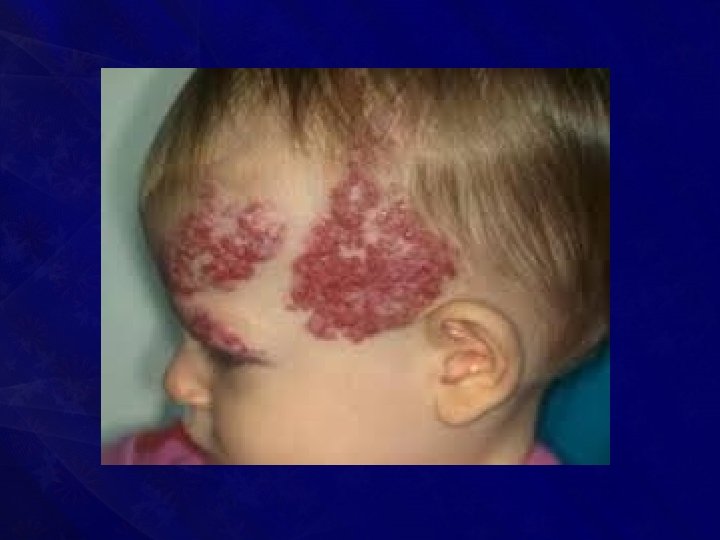

• Usually nontender unless it gets infected or undergoes thrombosis or causes haemorrhage

Differential Diagnosis • Lymphangioma: it is brilliantly transilluminant unless it is infected or fibrosed • Lipoma • Cold abscess • Lymph cyst
Complications • • Haemorrhage DIC Thrombosis Infection and septicaemia Ulceration Erosion into the adjacent bone High output cardiac failure

Investigations • Ultrasound with doppler • Angiogram to find out feeding vessel • Platelet count • MRI/MR angiogram to see feeding vessels and deeper extension

Treatment • Sclerosant therapy: • Initial first line of therapy • Causes aseptic thrombosis and fibrosis • Sodium tetradecyl sulphate/ hypertonic saline are used • Often multiple injections are needed to achieve complete required effect • Later excision of the lesion is done


• Ligation of feeding artery and at a later stage excision is done once haemangioma shrinks • Therapeutic embolisation • If small and located in accessible area, excision is the initial therapy • Laser ablation-Diode pulsed/ CO 2 / Nd: YAG laser

CIRSOID ANEURYSM

• Rare variant of capillary haemangioma occurring in the skin, beneath which abnormal artery communicates with the distended veins • Commonly seen in superficial temporal artery and its branches

• Often the underlying bone gets thinned out due to pressure • Occasionally extends into the cranial cavity • Ulceration is the eventual problem which will lead to uncontrollable haemorrhage

Clinical Features • Pulsatile swelling in relation to superficial temporal artery • Warm, • Compressible, • With arterialisation of adjacent veins and • With bone thinning (due to erosion) • It feels like a ‘pulsating bag of worms’
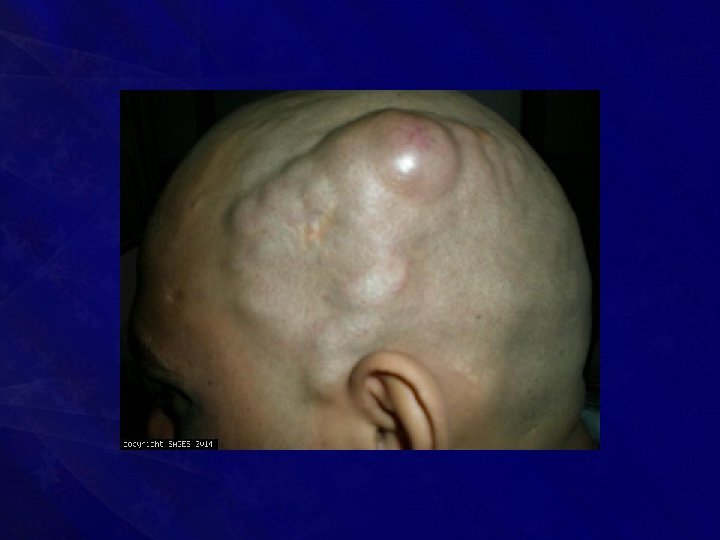

Investigations • USG with Doppler study • CT scan • Angiogram • X-ray of the part

Treatment • Ligation of feeding artery and excision of lesion, often requires preliminary ligation of external carotid artery • Intracranial extension requires formal neurosurgical approach
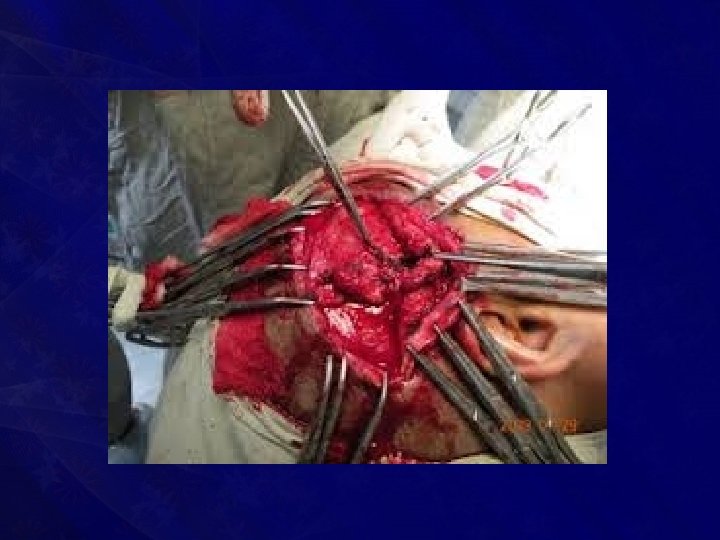

BEDSORES

• A bedsore is a trophic ulcer with bone as the base • It is gangrene caused by local pressure • It is a nonmobile, deep, punched out ulcer

• Sites of bedsore • • • Occiput Heel Sacrum Ischium Scapula
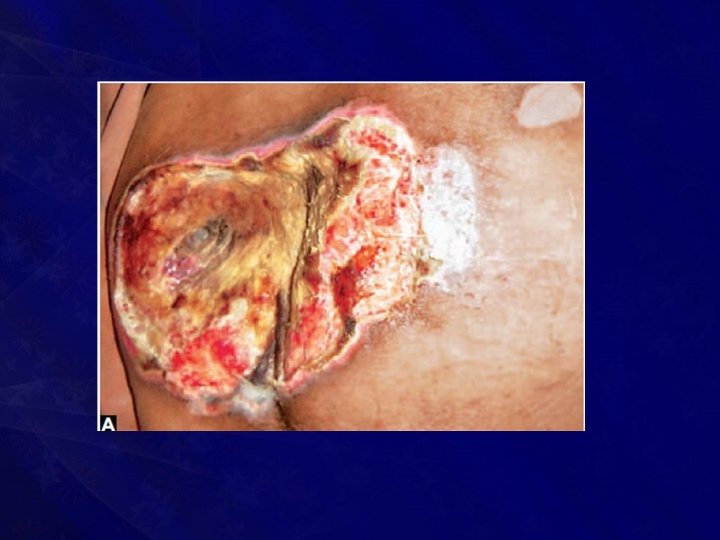

• Predisposed to by five factors: • • • Pressure Injury Anaemia Malnutrition and Moisture
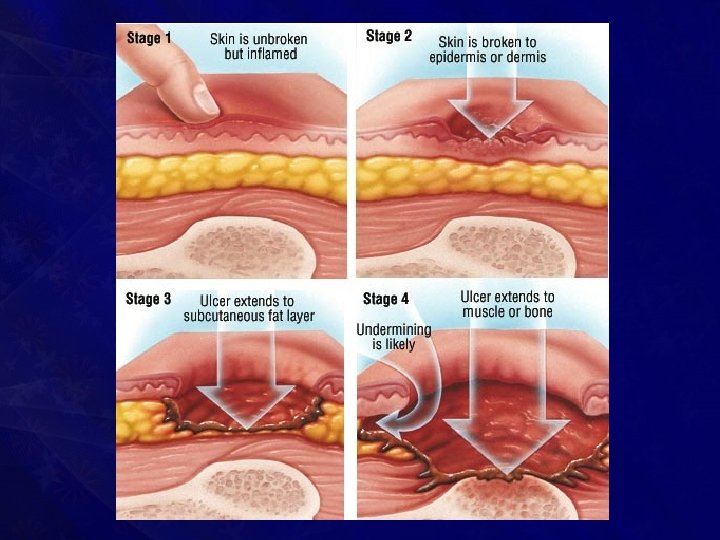

• It is common in • • • Old bedridden patients Tetanus Diabetic Paraplegic Comatose Patients with orthopaedic and head injuries

Treatment • Prevention • • Frequent change of position Use of water bed, ripple bed is advised Moisture has to be avoided Soaking by urine, sweat, pus, and faeces has to be taken care of
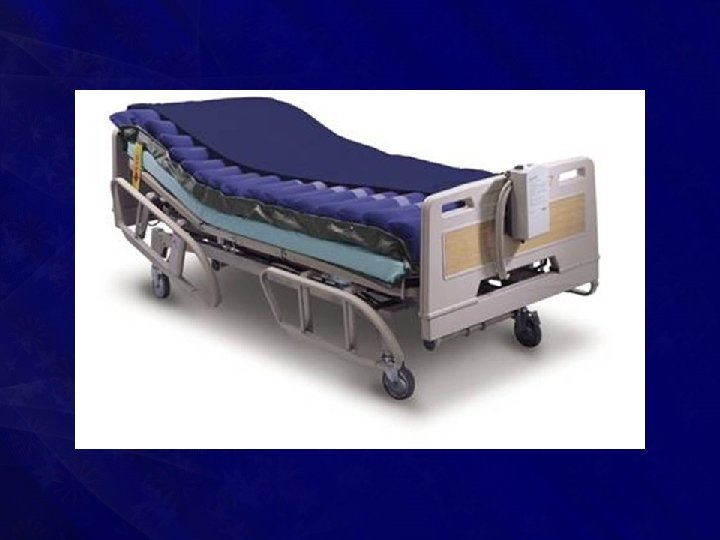

• Treatment • Excision of dead tissue followed by skin grafting or local rotation flaps may have to be done • Good nursing care, regular dressing, good nutrition • Antibiotics • Blood transfusion • Rehabilitation
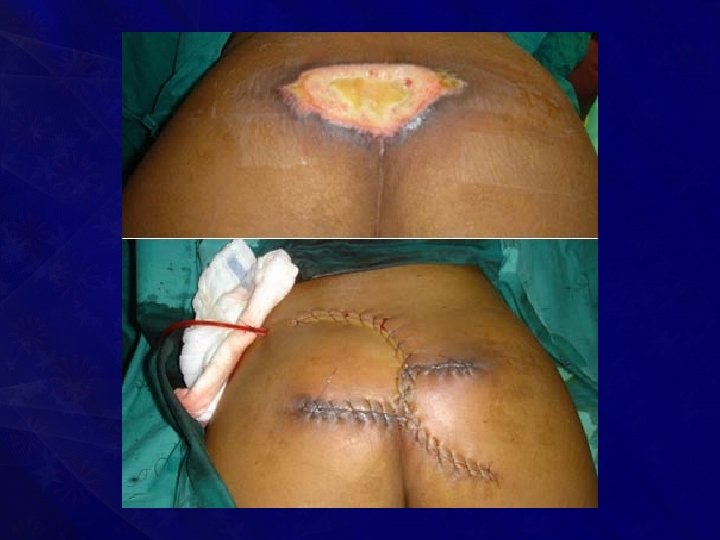

Thank You
- Slides: 71