VARIOUS DRUGS USED IN PAEDIATRIC DENTISTRY By Jyoti

VARIOUS DRUGS USED IN PAEDIATRIC DENTISTRY By : Jyoti Verma JR III
INTRODUCTION “The adult may be treated as a child: the converse can lead to disaster. ” -Sir Lancelot Barrington A drug can be defined as any substance or product that is used or is intended to be used to modify or explore phsiological system or pathological states for the benefit of the recipient. (WHO, 1966) Antibiotics Nutrition Supplement s Analgesics Paediatric Drugs Medical Emergency Drugs Anaestheics Drugs for sedation

Drugs in pedodontic practice can be classified in following groups: • Drugs for infection control: Antibiotics. • Drugs for pain control: • Non steroidal anti-inflammatory drugs • Opioid analgesics. • Local anaesthetics. • Drugs for Conscious sedation • Drugs for General anaesthesia. • Miscellaneous drugs. • Drugs for medical emergencies. • Drugs as nutrition supplement.

Dose calculation in Paediatric dentistry practice: Age Body Weight Body Surface Area • Clark’s SA Rule • Young’s Rule • Clarke’s rule • Dilling’s Rule • Brunton’s Rule • Fried ‘s Rule • Cowling’s Rule • Starkenstein’s Rule In the calculation of dosages, weight has a more direct bearing on the dose than any other factor, especially in the calculation of pediatric doses. The rule governing calculation of pediatric doses for newborns and young infants with a normal lean body mass and normal body development is Clark's Rule. For toddlers use Fried’s Rule, and for older children Young’s Rule is used.

AGE Young’s rule (for 1 to 12 years): Paediatric dose = Age (in years) x adult dose age+12 Brunton’s Rule: Paediatric dose = age x adult dose 25 Dilling’s rule: Paediatric dose = age (in years) x adult dose 20 Fried's Rule (for Infants and Children up to 1 to 2 Years): Paediatric dose = age (in months) x adult dose 150 Cowling’s rule: Pediatric dose = age(at next birthday in years) x adult dose 24 Starkenstein’s Rule: Paediatric dose = age x adult dose 18

Clarke’s rule: Body Weight Paediatric dose = weight(in pounds) x adult dose 150 Body surface area (BSA) is determined from a west’s nomogram using the child's height and weight. Body surface area Paediatric dose = child’s body surface area x adult dose 1. 7 m 2 Clark’s SA Rule: Paediatric dose = Surface area of child x adult dose Surface area of adult

1) Drugs for infection control: Antimicrobial Agents Ø An antibiotic is a chemical substance produced by various species of micro organisms (bacteria, fungi, and actinomycets) that suppress the growth of other microorganisms and may eventually destroy them. ØMay be : Synthetic drugs Naturally obtained drugs ØChoice of an antimicrobial agent depends upon Patient Factors Organism related considerations Drug factors
Beta Lactem Antibiotics Tetracycline and chloramphenicol Anti. Fungal Agents An tim icro bia l. A gen ts Metronidazole Anti. Viral Agents

• A)Beta Lactam Antibiotics Penicillin and Cephalosporine Penicillins: (1941) Originally obtained from Penicillium notatum, now it is derived from P. chrysogenum. Inhibit the bacterial cell wall synthesis and are mainly active against the gram positive baceria. The commonly used agents are: Amoxicillin Extended spectrum aminopenicillin good oral absorption not interfered by food. Drug of choice in orodental infectionsand in the antibiotic prophylaxis. Ampicillin an aminopenicillin with spectrum similar to amoxicillin with an incomplete oral absorption as food interferes with it. This also frequently leads to diarrhea after oral administration.

Clavulanic acid It is a progressive beta lactamase inhibitor, with rapid oral absorption. Its combination reestablishes the activity of amoxicillin against resistant strains. Cephalosporins Group of semisynthetic antibiotic, having actions and properties similar to penicillins with a difference in spectrum. Cephalosporins used in pedodontic practice are: • Cephalexin: orally effective first generation cephalosporin active against most of penicillin sensitive organism, including beta lactamase producing Staph. • Cefadroxil: similar to cephalexin in spectrum and properties.
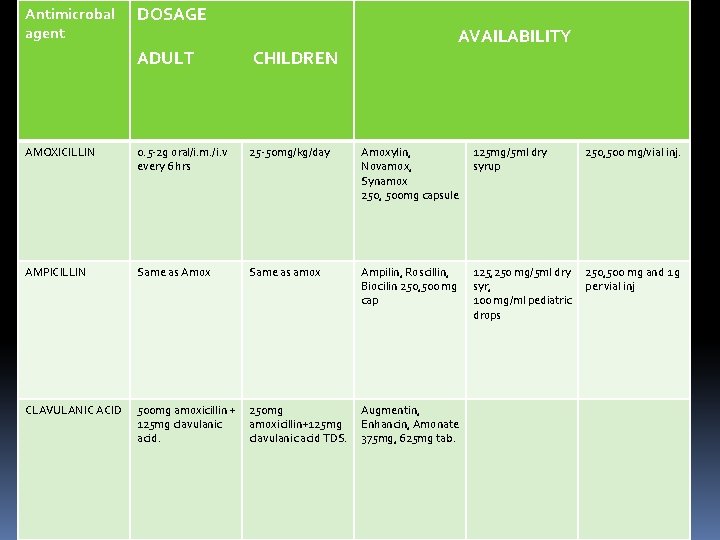
Antimicrobal agent DOSAGE ADULT CHILDREN AVAILABILITY AMOXICILLIN 0. 5 -2 g oral/i. m. /i. v every 6 hrs 25 -50 mg/kg/day Amoxylin, Novamox, Synamox 250, 500 mg capsule 125 mg/5 ml dry syrup 250, 500 mg/vial inj. AMPICILLIN Same as Amox Same as amox Ampilin, Roscillin, Biocilin 250, 500 mg cap 125, 250 mg/5 ml dry syr, 100 mg/ml pediatric drops 250, 500 mg and 1 g per vial inj CLAVULANIC ACID 500 mg amoxicillin + 125 mg clavulanic acid. 250 mg amoxicillin+125 mg clavulanic acid TDS. Augmentin, Enhancin, Amonate 375 mg, 625 mg tab.
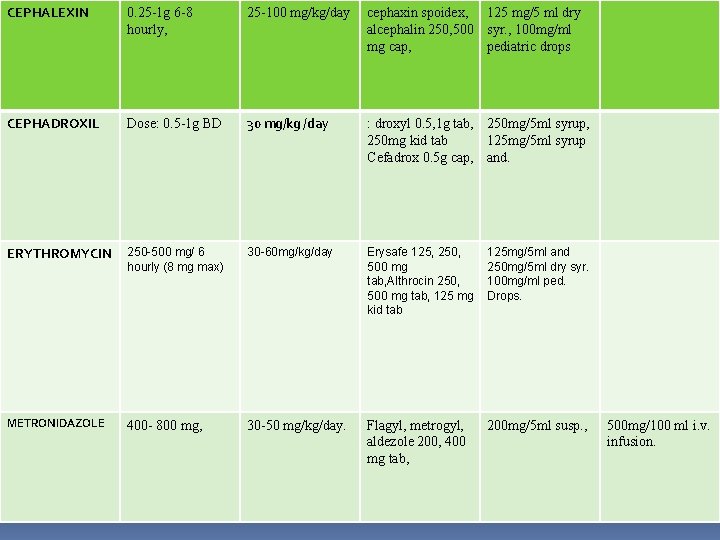
CEPHALEXIN 0. 25 -1 g 6 -8 hourly, 25 -100 mg/kg/day cephaxin spoidex, 125 mg/5 ml dry alcephalin 250, 500 syr. , 100 mg/ml mg cap, pediatric drops CEPHADROXIL Dose: 0. 5 -1 g BD 30 mg/kg /day : droxyl 0. 5, 1 g tab, 250 mg/5 ml syrup, 250 mg kid tab 125 mg/5 ml syrup Cefadrox 0. 5 g cap, and. ERYTHROMYCIN 250 -500 mg/ 6 hourly (8 mg max) 30 -60 mg/kg/day Erysafe 125, 250, 500 mg tab, Althrocin 250, 500 mg tab, 125 mg kid tab 125 mg/5 ml and 250 mg/5 ml dry syr. 100 mg/ml ped. Drops. METRONIDAZOLE 400 - 800 mg, 30 -50 mg/kg/day. Flagyl, metrogyl, aldezole 200, 400 mg tab, 200 mg/5 ml susp. , 500 mg/100 ml i. v. infusion.

Erythromycin: • Bacteriostatic at low but bactericidal at high concentration, • Antibacterial spectrum narrow, includes mostly gram positive and a few gram negative organism. • Acid labile, supplied in enteric coated tablet and taken empty stomach. • Indicated in patients allergic to penicillin. Metronidazole: • It is a nitroimidzole having a broad spectrum cidal activity against protozoa and many anaerobic bacteria. In pedodontic practice, it is indicated in anaerobic infections. • Adverseeffects : metallic taste, peripheral neuropathy thrombophlebitis of the injected vein.

Contraindication: blood dyscrasias, neurological disease first trimester of pregnancy Tetracycline : • broadspectrum, bacteriostatic antibiotics • chelating property, leading to deposition of calcium tetracycline chelate in developing teeth and bones. • strictly contraindicated in pregnancy and children below 6 years of age. • pregnancy to 5 months of extra uterine life, deciduous teeth are affected: brown discoloration and ill formed teeth. • 3 months of age to 5 years affect permanent anterior dentition. Repeated courses are damaging to teeth and bones.

Doxycycline and Minocycline are alternate drug to tetracycline ØHigh potency ØLess renal and vestibular toxicity, and diarrhea Chloramphenicol: • Broadspectrum, bacteriostatic antibiotics • Strictly contraindicated in pregnancy and in neonates. • It leads to “gray baby syndrome” in children.

Anti fungal agents: • The anti fungal agents are important in immune compromised patients, • children with rampant caries • angular chelitis • Drugs for oral candidiasis are: • Nystatin (mycostatin , 1 lac U /g oint. ) Ketoconazole (nizral, funginoc 2% oint) Anti viral agents: • The antiviral drugs are important due to a high prevalence of herpetic infections in children. • This is one of the most common infections transferred from children to the pedodontist. • Most common antiviral agent is Acyclovir (herpex 200 mg tab, 3% eye oint. , 5% skin cream
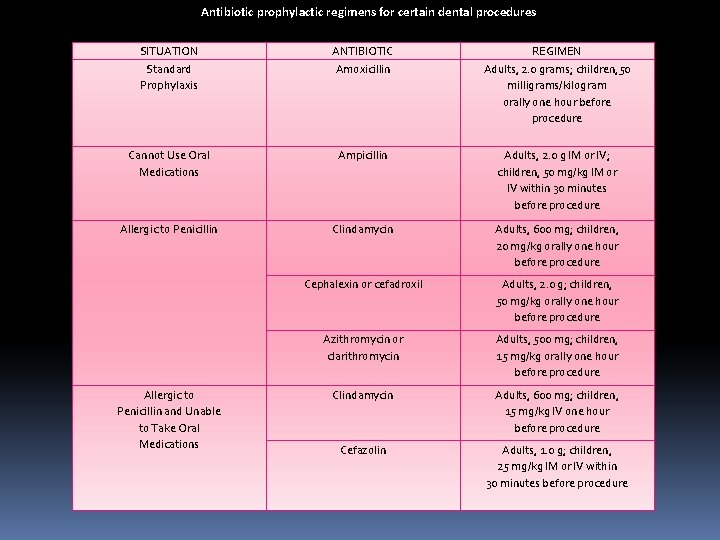
Antibiotic prophylactic regimens for certain dental procedures SITUATION Standard Prophylaxis ANTIBIOTIC Amoxicillin REGIMEN Adults, 2. 0 grams; children, 50 milligrams/kilogram orally one hour before procedure Cannot Use Oral Medications Ampicillin Adults, 2. 0 g IM or IV; children, 50 mg/kg IM or IV within 30 minutes before procedure Allergic to Penicillin Clindamycin Adults, 600 mg; children, 20 mg/kg orally one hour before procedure Cephalexin or cefadroxil Adults, 2. 0 g; children, 50 mg/kg orally one hour before procedure Azithromycin or clarithromycin Adults, 500 mg; children, 15 mg/kg orally one hour before procedure Clindamycin Adults, 600 mg; children, 15 mg/kg IV one hour before procedure Cefazolin Adults, 1. 0 g; children, 25 mg/kg IM or IV within 30 minutes before procedure Allergic to Penicillin and Unable to Take Oral Medications
Drugs for pain control v Analgesic is a drug that relieves pain by acting in the central nervous system or on peripheral pain mechanisms. v. Widely prescribed for pain relief, especially after a dental surgical procedures, pulpitis, gingival infections and periapical infections, dental extractions and teething. Non steroidal anti-inflammatory drugs Classified as Opioid analgesics

Non steroidal anti inflammatory drugs: (non narcotic or aspirin like and antipyretic analgesic) CLASSIFICATION A. Nonselective COX inhibitors (conventional NSAIDS) Salicylates Aspirin Pyrazolone derivatives Phenylbutazone, oxyphenbutazone Indole derivatives Indomethacin Propionic acid derivatives Ibuprofen, Naproxen, Ketoprofen, Fenoprofen, Flurbiprofen. Anthranilic acid derivative Mephenamic acid Aryl-acetic acid derivatives Diclofenac Oxicam derivatives Piroxicam, Tenoxicam Pyrrolo-pyrrole derivative Ketorolac.

B. Preferential COX-2 inhibitors : Nimesulide, Meloxicam, Nabumetone c. Selective COX-2 inhibitors : Celecoxib, Rofecoxib, Valdecoxib, Etoricoxib D. Analgesic - antipyretics with poor antiinflammatory: Paraaminophenol derivative Paracetamol (Acetaminophen) Pyrazolone derivatives Metamizol (Dipyrone), propiphenazone Benzoxazocine derivative Nefopam • NSAIDS are weaker analgesics but they do not depress the central nervous system and have no physical dependence.

COMMON PROPERTIES OF ALL NSAIDS Analgesia Anaphylactoid reactions Antipyresis Antiinflammatory Renal effects Dysmenorrhoea Gastric mucosal damage Parturition Ductus arteriosus closure Antiplatelet aggregatory

Indications: • Mild to moderate pain • Fever • Inflammation • Dysmenorrhoea • Thromboembolism • Patent ductus arteriosus Contraindications: • Asthma. • Gastritis. • Pregnancy and lactating mothers. • Diabetics, Congestive heart failure, hypovolemia, hepatic cirrhosis, renal disease, those receiving diuretics and anti-hypertensives. Renal effects of NSAIDS leading to Na+ retention and oedema. • Chronic liver disease. • NSAIDS should be stopped one week before elective surgery.
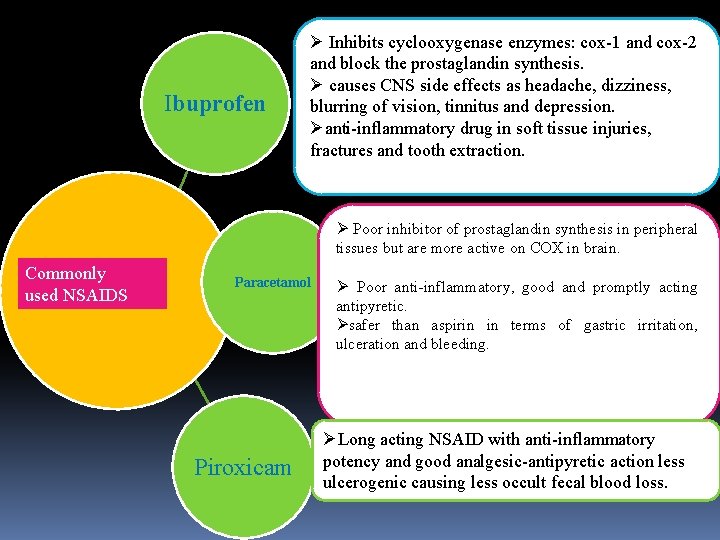
Ibuprofen Ø Inhibits cyclooxygenase enzymes: cox-1 and cox-2 and block the prostaglandin synthesis. Ø causes CNS side effects as headache, dizziness, blurring of vision, tinnitus and depression. Øanti-inflammatory drug in soft tissue injuries, fractures and tooth extraction. Ø Poor inhibitor of prostaglandin synthesis in peripheral tissues but are more active on COX in brain. Commonly used NSAIDS Paracetamol Piroxicam Ø Poor anti-inflammatory, good and promptly acting antipyretic. Øsafer than aspirin in terms of gastric irritation, ulceration and bleeding. ØLong acting NSAID with anti-inflammatory potency and good analgesic-antipyretic action less ulcerogenic causing less occult fecal blood loss.

Ibuprofen: Dose&Availability: Brufen, emflam, ibusynth, 200, 400, 600 mg tab Brufamol kid DT 200 mg Ibugesic 100 mg/5 ml susp. Paracetamol : Dose: Infants 50 mg, children (1 -3 years) 60 -80 mg, (4 -8 years) 240 -320 mg, (9 -12 years) 300600 mg Adult. Availability: Crocin, Metacin, Paracin 500 mg tab, 125 mg/5 ml syrup, 150 mg/ml paed. drops. Ultragin, Pyrigesic 500 mg tab, 125 mg/5 ml syrup. Neomal, Fevastin febrinil 300 mg/2 ml inj. Piroxicam: Dose: 20 mg BD for two days followed by 20 mg OD. Availability: Dolonex, Pirox 10, 20 mg cap, , 20 mg/ml inj. In 1 and 2 amps.
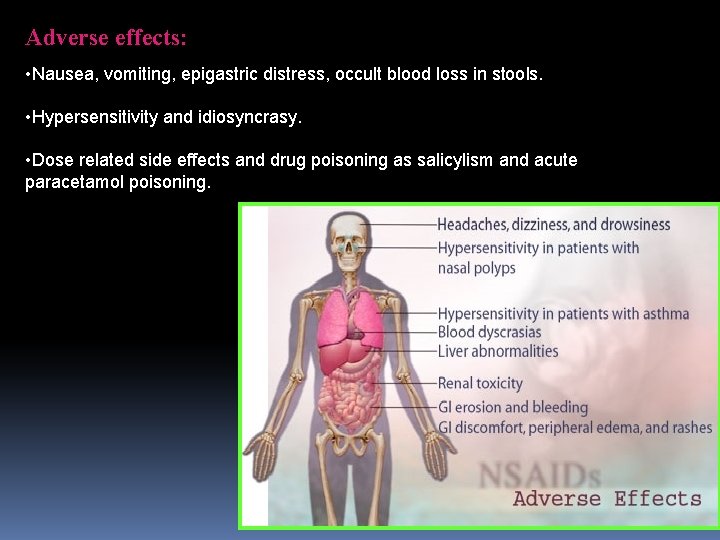
Adverse effects: • Nausea, vomiting, epigastric distress, occult blood loss in stools. • Hypersensitivity and idiosyncrasy. • Dose related side effects and drug poisoning as salicylism and acute paracetamol poisoning. acute

paracetampoisoning Serious toxicity can occur at >150 mg/kg and fatality is common with >250 mg/kg. Acute Paracetamol Poisoning: • Specially in small children(>150 mg/kg or >10 g in adult) Fatal at >250 mg/kg. • Nausea, vomiting, abdominal pain, • hepatic tenderness and leads to centrilobular hepatic necrosis, • renal tubular necrosis and hypoglycemia. • causes coma in 12 -18 hours and jaundice in 2 days. • Fulminating hepatic failure and death occurs if plasma levels are above 200 ug/ml at 4 hours and 30 ug/ml at 15 hours. • Paracetamol is not recommended in premature infants (<2 kg) for fear of hepatotoxicty.

Treatment : ØInduce vomiting and gastric lavage. ØActivated charcoal is given orally to cause further absorption. Ø N-acetyl cysteine 150 mg/kg infused i. v. over 15 min followed by same dose over next 20 hours. Alternatively 75 mg/kg orally may be given every 4 -6 hours for 2 -3 days. It replenishes the glutathione stores in liver and prevents the toxic N-acetyl-benzoquinone-imine from binding to other cellular constituents. Other NSAIDS: Frequently NSAIDS are cautiously used in children due to their hepatic and renal toxicity. Selective cox-2 inhibitors as rofecoxib and celecoxib have been found to interfere with bone maturation and hence are not of paediatric importance. Nimesulide considered safe for adult usage is not indicated in children due to their hepatotoxicity.

Opioid analgesics: ØOpium is a dark brown resinous material obtained from poppy (Papaver somniferum ØWith the advent of recent safer alternatives and the problems associated with the addiction and adverse effects of the opioids, their use has been limited to poorly localized visceral pain and very severe pain. ØClassification: Natural Opiate Semi synthetic Opiate Synthetic Opiate

• Natural opium alkaloids: Morphine, Codeine. • Semi synthetic opiates: Diacetylmorphine (Heroin), Pholcodiene. • Synthetic opioids: Pethidine, Fentanyl, Tramadol, methadone. Indications: • Dull, diffuse visceral pain. • Milder pain as tooth ache, not controlled by non steroidal anti-inflammatory drugs. • Surgical analgesia in obstetric, abdominal, lower limb and pelvic operations. • Preanaesthetic medication. • Balanced anaesthesia and neurolept analgesia. • Relief of anxiety and apprehension. • Analog-sedation in management of uncooperative children.

Contraindications: • Infants and elderly are more susceptible to the respiratory depressant action of morphine. • Patients with respiratory insufficiency. • Bronchial asthma. • Head injury. • Hypotensive states. • Undiagnosed acute abdominal pain. • Elderly males. • Hypothyroidism. • Unstable personalities.

Adverse effects: • Sedation, mental clouding, lethargy and even dysphoria. • Idiosyncrasy and allergy: urticaria itching and swelling of the lips. • Apnoea: may occur in new born when morphine is given to mother during labour. • Acute morphine poisoning at >250 mg • Tolerance and dependence. Opioid analgesics in Pedodontic practice: Tramadol Dose: 50 -100 mg oral/ i. m. / slow i. v. infusion 4 -6 hourly. 1 -2 mg/kg ( in children 4 to 16 years) Drug name: contramal, domadol, tramazac 50 mg cap and 50 mg/ml inj. In 1 and 2 ml amps. Fentanyl: In the past associated with neurolept anaesthesia in combination with Droperidol. Available as trofentyl 50 ug/ml , fentanyl citrate inj in 2 ml amp and 10 ml vial.

Local anaesthetics Ø Local anaesthesia has been defined as a loss of sensation in a circumscribed area of the body caused by a depression of excitation in nerve endings or an inhibition of the conduction process in peripheral nerves. Ø An important feature of local anaesthesia is that it produces this loss of sensation without inducing a loss of consciousness.
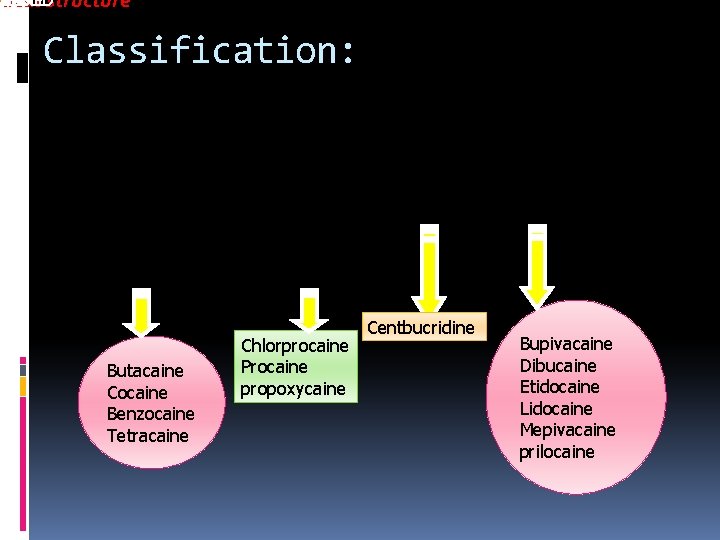
TER DES OLINE IC BAACIDstructure mical Classification: Butacaine Cocaine Benzocaine Tetracaine Chlorprocaine Procaine propoxycaine Centbucridine Bupivacaine Dibucaine Etidocaine Lidocaine Mepivacaine prilocaine
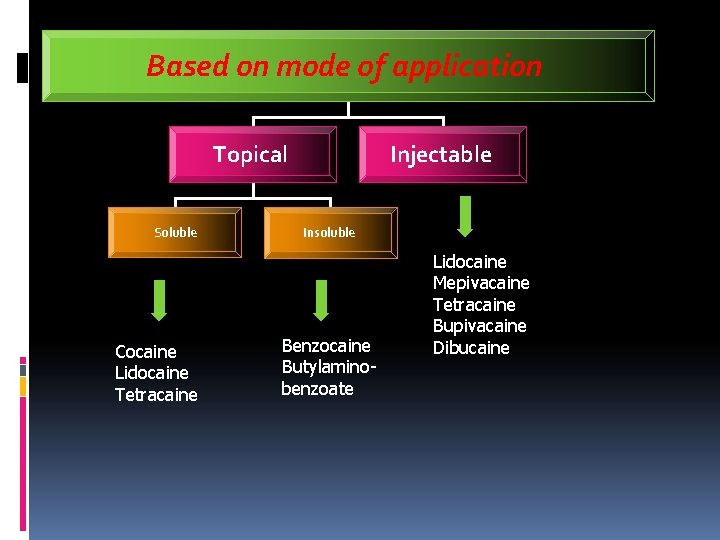
Based on mode of application Topical Soluble Cocaine Lidocaine Tetracaine Injectable Insoluble Benzocaine Butylaminobenzoate Lidocaine Mepivacaine Tetracaine Bupivacaine Dibucaine
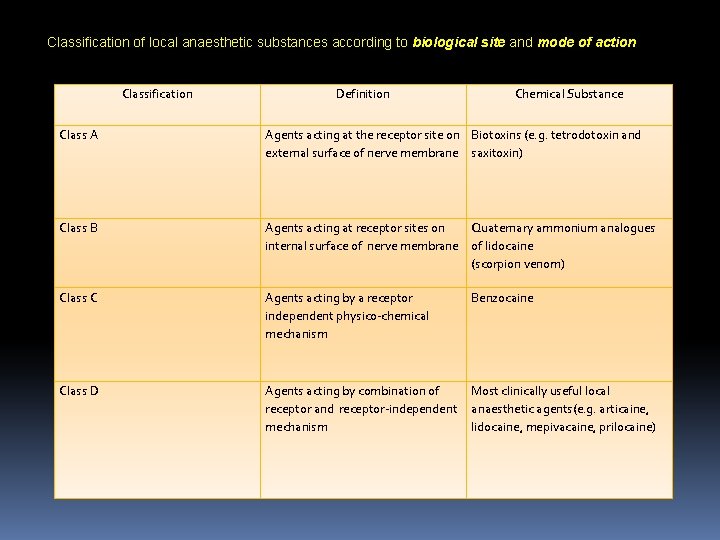
Classification of local anaesthetic substances according to biological site and mode of action Classification Definition Chemical Substance Class A Agents acting at the receptor site on Biotoxins (e. g. tetrodotoxin and external surface of nerve membrane saxitoxin) Class B Agents acting at receptor sites on Quaternary ammonium analogues internal surface of nerve membrane of lidocaine (scorpion venom) Class C Agents acting by a receptor independent physico-chemical mechanism Benzocaine Class D Agents acting by combination of receptor and receptor-independent mechanism Most clinically useful local anaesthetic agents(e. g. articaine, lidocaine, mepivacaine, prilocaine)

Composition Lignocaine hydrochloride- 24. 64 mg Adrenaline bitartrate - 0. 0125 mg Sodium chloride/modified Ringer’s solution 6 mg/ml Sodium metabisulfide - 0. 5 mg/ml Methyl paraben - 1 mg/ml Thymol - 1 mg/ml Water local anesthesia 12/4/2020 36
Clinical uses of local anaesthetics: The clinical uses of local anaesthetics in pedodontic practice may be divided into: 1. Surface anaesthesia. 2. Infiltration anaesthesia. 3. Field block 4. Nerve block 5. Intraligamentary. 6. Intra pulpal.

Local anaesthetic agents used in pedodontic practice are as follows: Lidocaine: • It is an amide type of agent having rapid onset of action and producing more profound anaesthesia. • Maximum recommended dose : 4. 4 mg/kg without adrenaline : 7 mg/kg with adrenaline • Duration of Pulpal anaesthesia : 60 min Soft tissue anaesthesia: 2 -3 hours.

Availability: • Xylocaine, Gesicain 4% topical solution, • 2% Lidocaine jelly, 5% ointment, • 1% and 2% injection(with or without adrenaline), 5% heavy for spinal anaesthesia and 100 mg/ml spray (10 mg per puff). Mepivacaine: • Mepivacaine 3% produces pulpal anaesthesia: 25 min and soft tissue anaesthsia : 90 min • It was a popular drug till lidocaine came to picture. • This drug requires additional caution when being administered to young children.

Drugs for conscious sedation: Drugs for Oral concious sedation • Hydroxyzine • Promethazine • Chloral hydrate • Meperdine • Diazepam • Triazolam • Chlorpromazine Drugs for intramuscular sedation • Ketamine • Midazolam Drugs for Intravenous sedation Midazolam
Hydroxyzine H 1 antihistaminic drug which is mildly sedative along with antiemetic and anticholinergic action. Promethazine It is also a H 1 antihistaminic with properties and limitations similar to hydroxyzine. potentiates narcotic and central nervous system depressants. Dose: 25 -50 mg oral, i. m. (1 mg/kg). Dose: 25 -50 mg oral/i. m. Availability: phenergan 10, 25 mg tab, 10 mg/5 ml syr, 6 mg/ml drops, 25 mg/ml inj.

• It is the oldest synthetic hypnotic used since 1869. • It is used for all levels of anxiety, has a wide range of safety. Chloralhydrate it isrecommended an opioid derivative producing • • Not in children below 6 analog-sedation. years of age. • Best used in combination with promethazine and hydroxyzine for short procedures and chloral hydrate for longer procedure. • It has poor oral absorption and respiratory depression. Contraindicated in chronic obstructive pulmonary disease and liver dysfunction. Meperdine • Agitation is common in post operative period and has no analgesia. • Dose: adults: 1 g, children: 0. 25 -0. 5 g. Availability: Tricloryl 0. 5 g/5 ml elixir • Dose: 2 -4 mg/ kg every 3 hours. • It has an anti convulsant activity and good oral absorption. Triazolam • Availability: Demerol 50 mg/5 ml • It has a rapid elimination with safety levels not fully established.

• moderate anxiety particularly in children with cerebral palsy, mental Diazapam • retardation and age less than 6 years. • not effective in severe anxiety and multiple doses are required for sedation. • Dose: 0. 120. 8 mg/kg in 3 with or 4 meperdine divided doses. • used in combination and or promethazine. Chlorpromazin e Though useful in 5 mg/5 ml severe behavior problems, it is unpredictable and less studied. • • Availability: valium: elixir, 2, 5, 10, 15 mg tablets. . • Dose: 2 -3 mg/kg. availability: Thorazine 10 mg/ml syrup, 10, 25, 50, 100, 200 mg tablets.

Drugs for intramuscular sedation: Ketamine: • Potent analgesic and a potential for oral use. • Its safety for oral route has not yet been established • Dose: 1 -4 mg/kg. Availability: ketamin, ketlar 10 mg and 50 mg/ml inj. Midazolam: • Hypnotic benzodiazepine with anticonvulsant and muscle relaxant properties. Rapid onset of action, causes anterograde amnesia and is anxiolytic. Dose: 0. 07 -0. 08 mg/kg. • Availability: inj. Midaz, benzosed 1 mg/ml in 2 ml and 10 ml vial, 5 mg/ml in 1 ml vial. Drugs for intravenous sedation: Midazolam

General Anaesthetic agents: a) Inhalational anaesthetics. b) Intravenous anesthetics. ØA combination of inhalation and intravenous anesthetics, often with opioids added for pain relief and neuromuscular blockers for muscle paralysis, is called balanced anesthesia.

Inhalation anesthetics: Halothane causes unconsciousness but provides little pain relief; often administeredwith analgesics. Nitrous oxide Used with other drugs as thiopental to produce surgical anesthesia. The fastest induction and recovery time. Has a pleasant smell and is therefore often the anesthetic of choice when mask induction is used with children. Safest inhalation anesthetic because it does not slow respiration or blood flow to the brain. relatively weak anesthetic, not suited for major surgery. It may be toxic to the liver in adults. may be used alone for dental anesthesia, should not be used as a primary agent in more extensive procedures.
Enflurane Isoflurane Less potent, but produces a rapid onset of anesthesia and possibly a faster recovery. works quickly Not toxic to the liver but can induce irregular heart rhythms Not used in patients with kidney failure. Sevoflurane can be administered through a mask since it does not irritate the airway. On the other hand, sevoflurane can cause renal damage. Desflurane • a secondgeneration version of isoflurane, • irritating to the airway and therefore cannot be used for mask (inhalation) inductions, especially not in children.

ravenous anesthetics ØKetamine, ØThiopental (a barbiturate), ØMethohexital (Brevital), ØEtomidate, ØPropofol (Diprivan),

Ketamine Ø produces a different set of reactions from other intravenous anesthetics. ØResembles phencyclidine, which is a street drug that may cause hallucinations. ØBecause patients who have been anesthetized with ketamine often have sensory illusions and vivid dreams during post-operative recovery, ketamine is not often given to adult patients. Ø It is, however, useful in anesthetizing children, patients in shock, and trauma casualties in war zones where anesthesia equipment may be difficult to obtain.

Miscellaneous Drugs • A)Drugs for medical emergencies: • The use of pharmacological measures for behavior management and the uncooperative nature of substantial majority of the patients, puts the pedodontic practice at a greater risk. • These drugs can prove to be life-saving when a situation arises. • A practice requires a complete set of emergency drugs which are as follows:
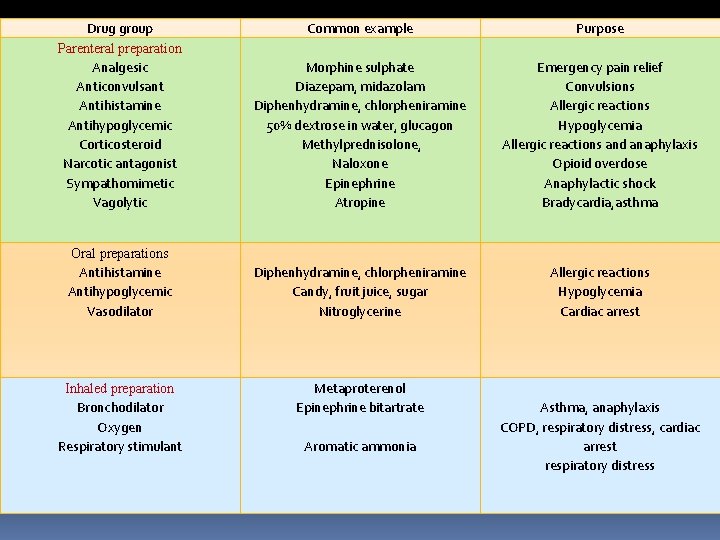
Drug group Parenteral preparation Analgesic Anticonvulsant Antihistamine Antihypoglycemic Corticosteroid Narcotic antagonist Sympathomimetic Vagolytic Common example Purpose Morphine sulphate Diazepam, midazolam Diphenhydramine, chlorpheniramine 50% dextrose in water, glucagon Methylprednisolone, Naloxone Epinephrine Atropine Emergency pain relief Convulsions Allergic reactions Hypoglycemia Allergic reactions and anaphylaxis Opioid overdose Anaphylactic shock Bradycardia, asthma Oral preparations Antihistamine Antihypoglycemic Vasodilator Diphenhydramine, chlorpheniramine Candy, fruit juice, sugar Nitroglycerine Allergic reactions Hypoglycemia Cardiac arrest Inhaled preparation Bronchodilator Oxygen Respiratory stimulant Metaproterenol Epinephrine bitartrate Aromatic ammonia Asthma, anaphylaxis COPD, respiratory distress, cardiac arrest respiratory distress

B) Nutritional supplements v. Mineral supplements i. Calcium glubionate: • • • indicated in deficient serum calcium levels. Dose : 800 -1200 mg/day. Available as calcium Sandoz, oscal syr 1. 8 g/5 ml. ii. Calcium lactate: • indicated in deficient serum calcium levels. • Dose: 400 -500 mg/day in 3 -6 divided doses. • Available: tablets 325, 500 mg. iii. Ferrous sulphate: • indicated in iron deficiency anaemia, for prophylaxis and in preterm infants (not before 2 months of age).

Dose: For iron deficiency anaemia- 6 mg elemental iron/kg/day in three divided doses. For prophylaxis- 1 -2 mg/kg/day in 2 -3 divided doses. Availability: Durovit, Fezocar drops, Syrup iberol, syr fezocar, cap Elferri-TR, 150 mg tab, pediatric drops 75 mg (15 mg iron)/0. 6 ml in 50 ml, 125 mg (25 mg iron)/1 ml in 50 ml, 45 mg(15 mg iron)/0. 6 ml in 60 ml.

v Vitamin supplements: Vitamin B-complex: i. these formulations comprise of water soluble vitamin B 1, B 2, B 3, B 6, B 12 and indicated along with antibiotics, prohylactically in Ariboflavinosis, and malnutrition. i. Individual preparations of each vitamin are also available for selected deficiencies. ii. Vitamin D: indicated to prevent or treat rickets. Dose: 10 mcg/day, 400 IU/24 hour Availability: calciferol, ergocalciferol liq. 8000 IU/ml in 60 ml.

References: • Tripathi KD. Essentials of medical pharmacology. • Stewart RE, Barber TK, Troutman KC, Wei SHY. Pediatric dentistry: scientific foundations and clinical practice. • Mcdonald RE, Avery DA, Dean JA. Dentistry for the child and adolescent. 2004, ed 8 • Malamed SF. Sedation: a guide to patient management. 1982 ed 4, • American academy of pediatric dentistry council on clinical affairs. Guidline on appropriate use of antibiotic therapy for pediatric dental patients. Pediatr dent. 20052006; 27 • Stephen HY Wei. Pediatric dentistry: total patient care. • Committee on nutrition, American academy of pediatrics: policy statement on calcium requirements of infants, children and adolescents. Pediatrics 1999; 104(5): 1152 -57.

Thank you
- Slides: 56