VARICOSE VEINS Superficial Venous Insufficiency Ali SABBOUR Vascular

VARICOSE VEINS Superficial Venous Insufficiency Ali SABBOUR Vascular Surgery Department, Ain Shams University
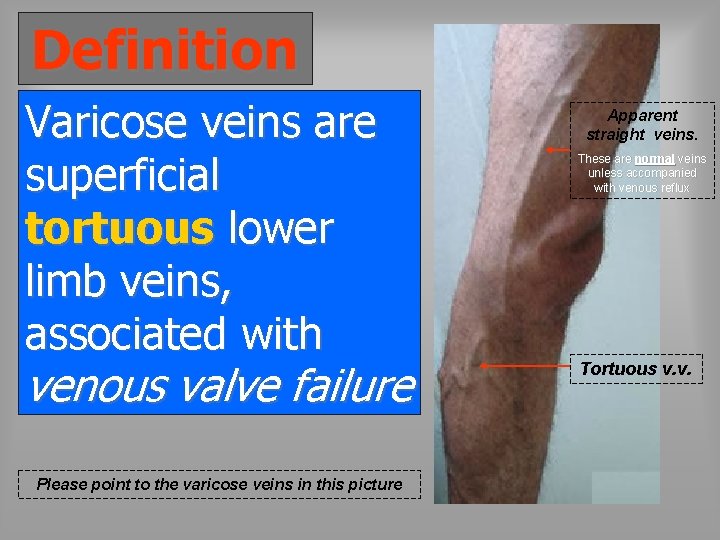
Definition Varicose veins are superficial tortuous lower limb veins, associated with venous valve failure Please point to the varicose veins in this picture Apparent straight veins. These are normal veins unless accompanied with venous reflux Tortuous v. v.

Etiology Varicose veins develop more often in people who stand more frequently during their work Their is a strong genetic predisposition. Hereditary mechanisms include a collagen defect in the venous wall and absent valve in the common femoral vein just proximal to the saph-fem. Junction.

Etiology §Women are affected more frequently than men §They often develop during pregnancy under the influence of oestrogen and progesterone causing smooth muscle vein wall relaxation.
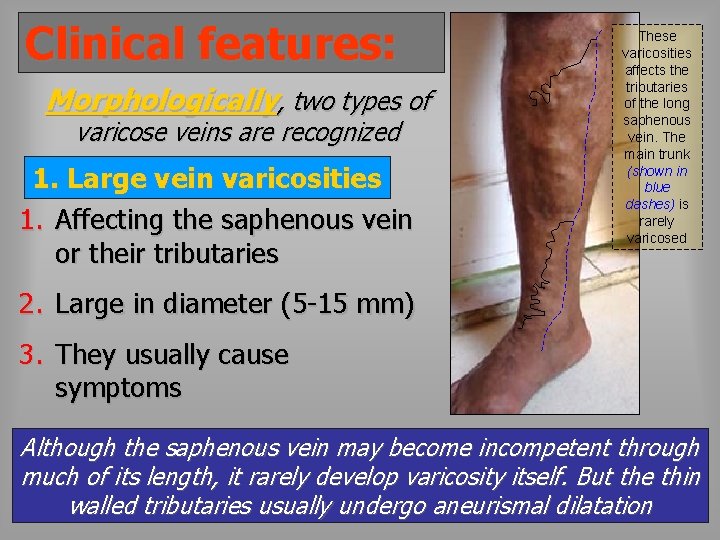
Clinical features: Morphologically, two types of varicose veins are recognized 1. Large vein varicosities 1. Affecting the saphenous vein or their tributaries These varicosities affects the tributaries of the long saphenous vein. The main trunk (shown in blue dashes) is rarely varicosed 2. Large in diameter (5 -15 mm) 3. They usually cause symptoms Although the saphenous vein may become incompetent through much of its length, it rarely develop varicosity itself. But the thin walled tributaries usually undergo aneurismal dilatation
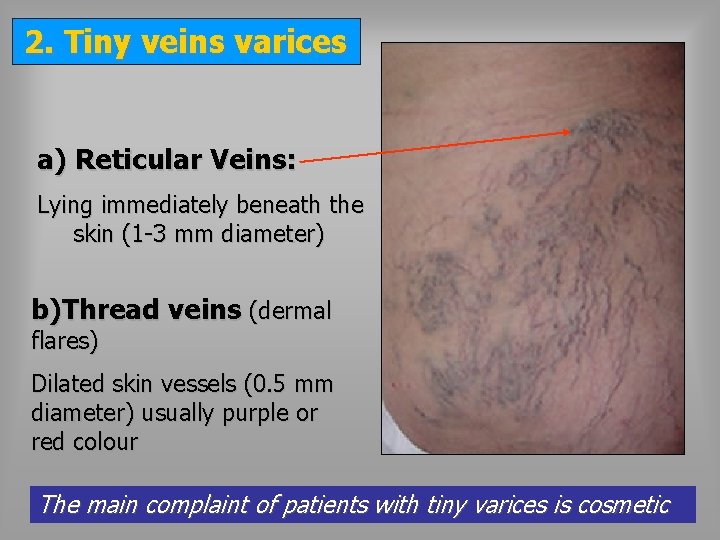
2. Tiny veins varices a) Reticular Veins: Lying immediately beneath the skin (1 -3 mm diameter) b)Thread veins (dermal flares) Dilated skin vessels (0. 5 mm diameter) usually purple or red colour The main complaint of patients with tiny varices is cosmetic
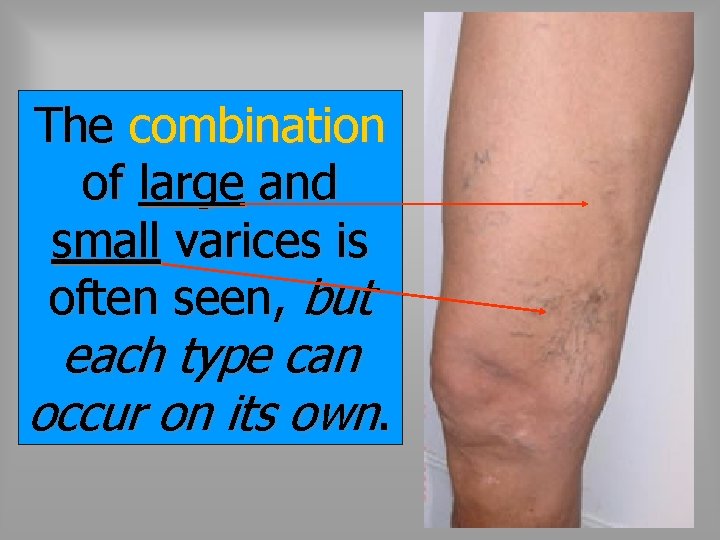
The combination of large and small varices is often seen, but each type can occur on its own.
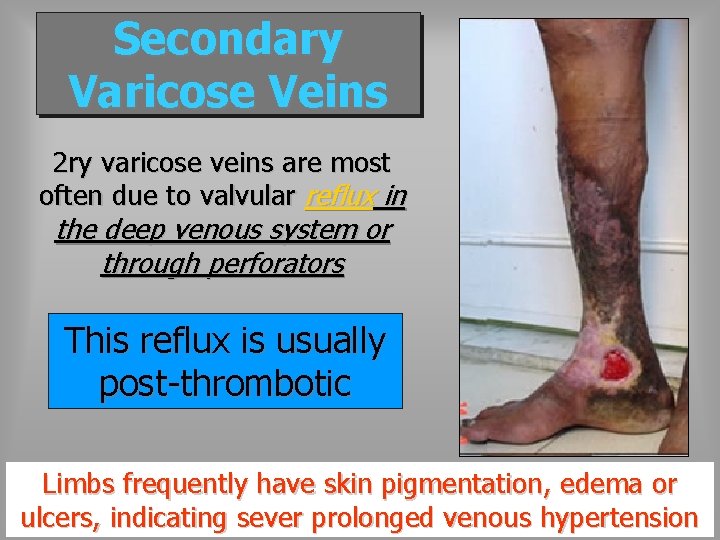
Secondary Varicose Veins 2 ry varicose veins are most often due to valvular reflux in the deep venous system or through perforators This reflux is usually post-thrombotic Limbs frequently have skin pigmentation, edema or ulcers, indicating sever prolonged venous hypertension

Secondary Varicose Veins Rare causes of secondary varicosities aretriovenous fistulas (Parks-Weber syndrome) and venous malformation syndromes (Klippel-Trenaunay & Sturge-Weber) It is important to note that deep venous system hypoplasia or aplasia are common with venous malformation syndromes. Removal of the superficial varicose veins in these syndromes may lead to a disaster as they may by the only veins draining the limb

How does varicose veins cause symptoms?
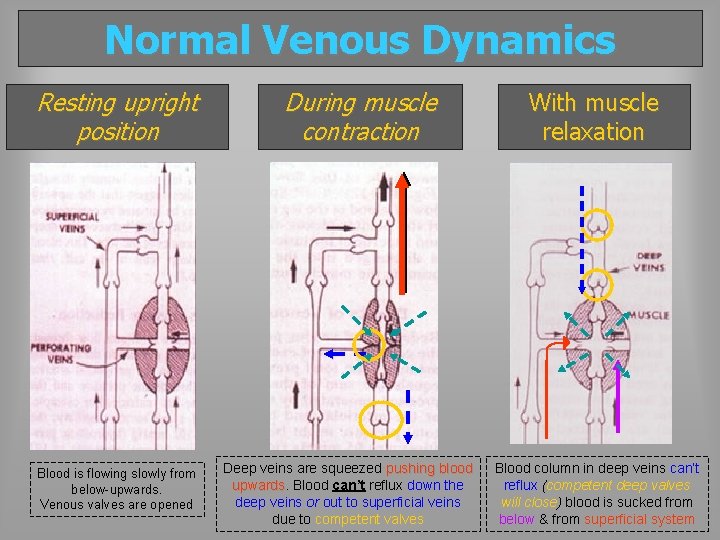
Normal Venous Dynamics Resting upright position Blood is flowing slowly from below-upwards. Venous valves are opened During muscle contraction Deep veins are squeezed pushing blood upwards Blood can’t reflux down the deep veins or out to superficial veins due to competent valves With muscle relaxation Blood column in deep veins can’t reflux (competent deep valves will close) blood is sucked from below & from superficial system
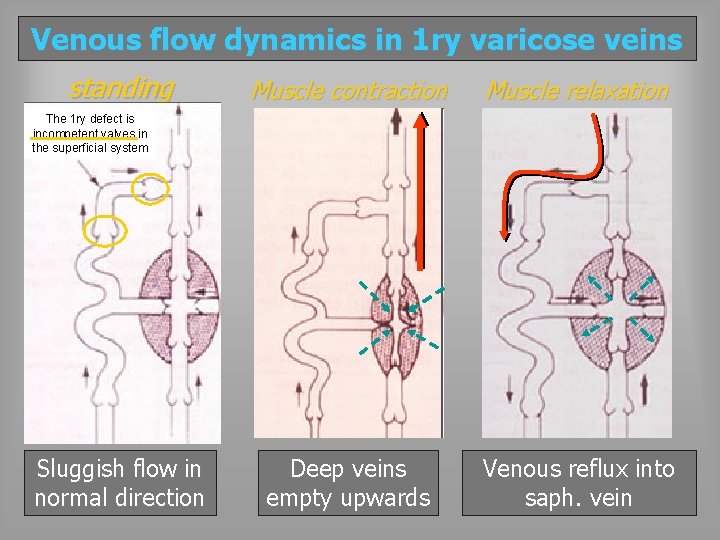
Venous flow dynamics in 1 ry varicose veins standing Muscle contraction Muscle relaxation Deep veins empty upwards Venous reflux into saph. vein The 1 ry defect is incompetent valves in the superficial system Sluggish flow in normal direction

So, varicose veins permit reverse flow through its incompetent valves This venous reflux add extra work on the veno-muscular pump, which should push this blood again to protect the microcirculation from venous hypertension. As long as the veno-muscular pump can cope with this extra work, the patient will remain asymptomatic. Symptoms and signs of CVI will only start when the pump fails to cope with this extra load.

Management of patients with venous disease The 1 st question: Is the patient’s complaint related to a venous disease? Patients may complain of symptoms unrelated to a preexisting asymptomatic venous condition e. g. lower limb pain due to osteoarthritis coexisting with asymptomatic reticular veins
Clinical presentation of varicose veins Apart from cosmetic disfigurement, varicose veins can present with the classical clinical picture of CVI depending on the severity and duration of venous hypertension Common Rare §Postural discomfort, relieved by leg elevation §Ankle pigmentation §Mild oedema §Venous ulcer §Night cramps §Lipodermatosclerosis §Itching & eczema
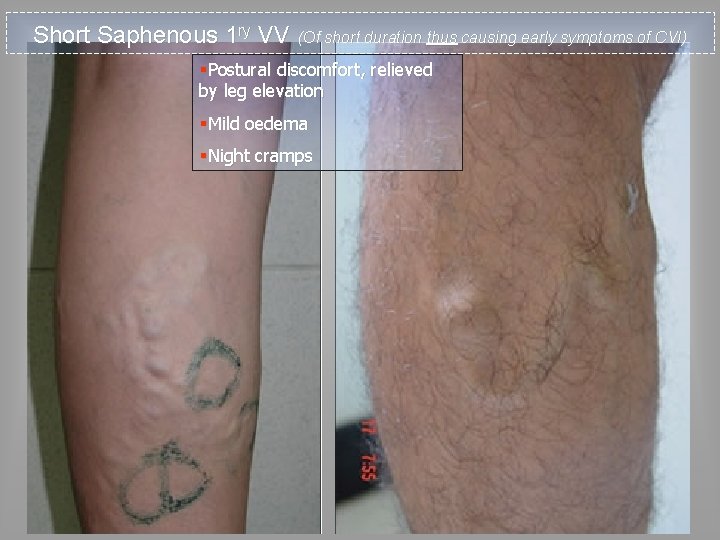
Short Saphenous 1 ry VV (Of short duration thus causing early symptoms of CVI) §Postural discomfort, relieved by leg elevation §Mild oedema §Night cramps
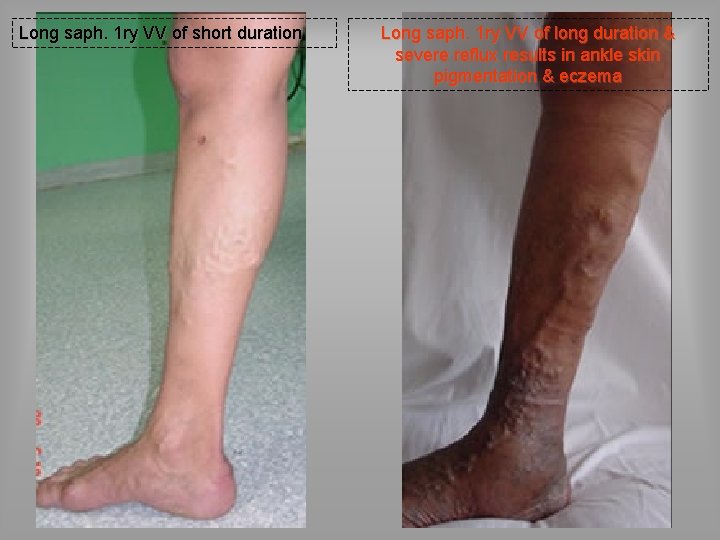
Long saph. 1 ry VV of short duration Long saph. 1 ry VV of long duration & severe reflux results in ankle skin pigmentation & eczema
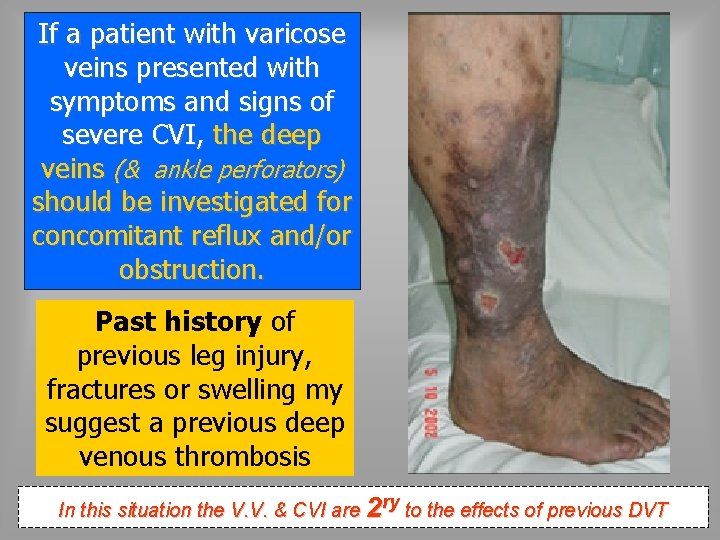
If a patient with varicose veins presented with symptoms and signs of severe CVI, the deep veins (& ankle perforators) should be investigated for concomitant reflux and/or obstruction. Past history of previous leg injury, fractures or swelling my suggest a previous deep venous thrombosis In this situation the V. V. & CVI are 2 ry to the effects of previous DVT

Patients with severe venous obstruction may develop bursting calf pain during walking, due to the very high venous pressure This is described as venous claudication
On examination, §Superficial venous reflux can be detected by the tourniquet or “Trendelenburg” test §Varicose veins crossing the inguinal ligament or over the abdomen are suggestive of underlying deep venous obstruction §Abdominal examination may occasionally reveal an abdominal neoplasm causing venous obstruction §Venous & arterial disease of the lower limbs may coexist. Peripheral pulses should be checked in elderly patients with ulcers
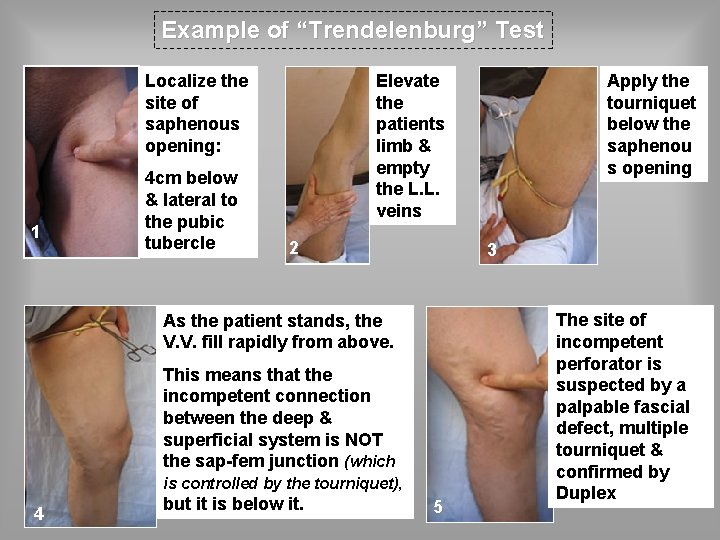
Example of “Trendelenburg” Test Localize the site of saphenous opening: 1 4 cm below & lateral to the pubic tubercle 2 3 As the patient stands, the V. V. fill rapidly from above. This means that the incompetent connection between the deep & superficial system is NOT the sap-fem junction (which is controlled by the tourniquet), 4 Apply the tourniquet below the saphenou s opening Elevate the patients limb & empty the L. L. veins but it is below it. 5 The site of incompetent perforator is suspected by a palpable fascial defect, multiple tourniquet & confirmed by Duplex
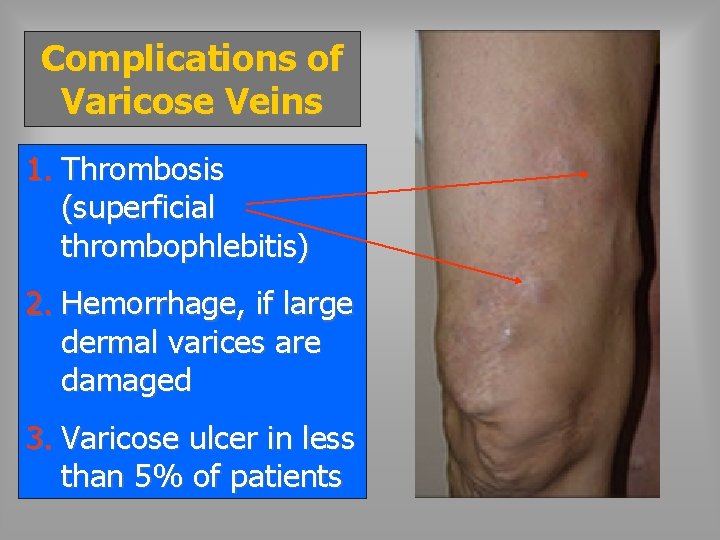
Complications of Varicose Veins 1. Thrombosis (superficial thrombophlebitis) 2. Hemorrhage, if large dermal varices are damaged 3. Varicose ulcer in less than 5% of patients

So, in symptomatic patients, we should answer two questions: 1. Where are the sites of venous reflux (causing retrograde filling of veins) ? 2. What is the condition of the deep system? Investigations of venous disease Role of Doppler, duplex, plethismography & venography

So, in symptomatic patients, we should answer two questions: 1. Where are the sites of venous reflux (causing retrograde filling of veins) ? The 1 st question can be answered : Clinically Investigations Inspection: Pocket Doppler Saphena-varix & blow-outs Duplex Examination Palpation: Saph-fem thrill & fascial defects Tourniquet tests:

2 - What is the condition of the deep system? The 2 nd question can be answered : Clinically Inspection: Veins crossing inguinal ligament (suspect underlying iliac vein thrombosis) Severe pigmentation & ulceration (suspect concomitant deep venous insufficiency) Perthy’s Test: (Inaccurate) Investigations Duplex: is now the standard in evaluating the deep system patency & reflux ( non invasive, dynamic study & can be repeated) Venography: invasive, static study, less commonly used (ascending venography for deep v. patency & descending venography for deep v. reflux Plethysmography: can give a GLOBAL evaluation of deep v. patency & reflux without localizing the site of obstruction or reflux. Used mainly in academic studies

Treatment The aim of treatment in symptomatic varicose veins is to overcome venous congestion. Improving the muscle pump by regular exercise can overcome mild venous hypertension
Compression stockings §Compression stockings supports varicose veins abolishing the effect of venous reflux §They are especially suitable to control deep venous reflux and secondary varicose veins §They are available in three grades of compression

Injection-Compression Sclerotherapy §Cosmetic for reticular veins §To obliterate localized bunch filling via a single perforator §For residual varices after surgery Should be given in an empty vein and compressed immediately after

Drugs There is nothing called venotonic drug, however, some drugs act on the microcirculation modulating the altered capillary permeability

Surgery for Varicose Veins Operative treatment of v. v. has changed over the years from radical to selective surgery, with the development of one day or even outpatient surgical techniques High ligation of the saphenous vein with division of ALL the groin tributaries, with or without saphenous vein striping in the thigh is classically done for documented saphenofemoral reflux Recurrence rates are higher with ligation alone. This is the reason we usually strip the long saphenous in the thigh Vein stripping below the knee is not needed (it is not varicosed, not connected to perforators and may cause saphenous nerve injury)
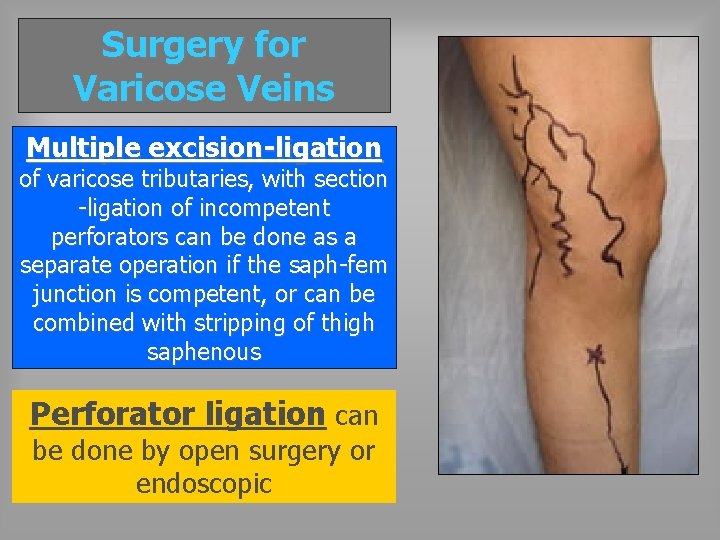
Surgery for Varicose Veins Multiple excision-ligation of varicose tributaries, with section -ligation of incompetent perforators can be done as a separate operation if the saph-fem junction is competent, or can be combined with stripping of thigh saphenous Perforator ligation can be done by open surgery or endoscopic

Surgery for Varicose Veins Short saphenous disconnection from the popliteal vein & stripping Is indicated in patients with saphpop reflux & 1 ry V. V. of the short saphenous system
- Slides: 32