ValueBased Care Volume to Value Lecture b MACRA

Value-Based Care Volume to Value Lecture b – MACRA and Value-Based Payments This material (Comp 23 Unit 6) was developed by Normandale Community College, funded by the Department of Health and Human Services, Office of the National Coordinator for Health Information Technology under Award Number 90 WT 0003. This work is licensed under the Creative Commons Attribution-Noncommercial-Share Alike 4. 0 International License. To view a copy of this license, visit http: //creativecommons. org/licenses/by-nc-sa/4. 0/.

Volume to Value Learning Objectives 1 • Describe alternative payment models. • Discuss the changes in CMS payment models toward Value-Based Care incentive programs • Discuss how electronic information and data can support organizational readiness for these alternative payment models • Discuss how data acquired from electronic information systems can support alternative payment models 2

The Move to Value-Based Payment Models - Overview 3
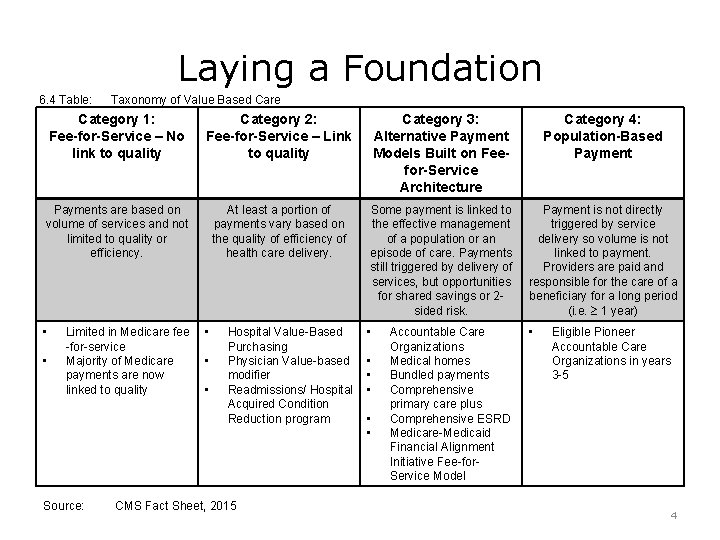
Laying a Foundation 6. 4 Table: Taxonomy of Value Based Care Category 1: Fee-for-Service – No link to quality Category 2: Fee-for-Service – Link to quality Category 3: Alternative Payment Models Built on Feefor-Service Architecture Category 4: Population-Based Payments are based on volume of services and not limited to quality or efficiency. At least a portion of payments vary based on the quality of efficiency of health care delivery. Some payment is linked to the effective management of a population or an episode of care. Payments still triggered by delivery of services, but opportunities for shared savings or 2 sided risk. Payment is not directly triggered by service delivery so volume is not linked to payment. Providers are paid and responsible for the care of a beneficiary for a long period (i. e. 1 year) • • Limited in Medicare fee -for-service Majority of Medicare payments are now linked to quality Source: • • • Hospital Value-Based Purchasing Physician Value-based modifier Readmissions/ Hospital Acquired Condition Reduction program CMS Fact Sheet, 2015 • • • Accountable Care Organizations Medical homes Bundled payments Comprehensive primary care plus Comprehensive ESRD Medicare-Medicaid Financial Alignment Initiative Fee-for. Service Model Eligible Pioneer Accountable Care Organizations in years 3 -5 4

The Medicare Access and CHIP Reauthorization Act (MACRA) • Legislation that changed three elements of the Medicare payment model – Ended the Sustainable Growth Rate (SGR) – Created a framework to reward value, not volume – Authorized the combination of existing quality reporting programs into one system 5

Sustainable Growth Rate (SGR) • This plan was enacted in 1997 to control Medicare spending. • It was supposed to make large cuts in Medicare’s fee schedules. However, every year but one (2002), the cuts were put off because there was no political will to reduce what providers got paid. Source: CMS, Office of the Actuary, 2012 6

SGR’s Transformation • By ending SGR, Congress eliminated a regulation that was not going to be implemented anyway • With MACRA, the plans to control cost shifted to incentive payment programs 7

Merit-Based Incentive Payment System (MIPS) • MIPS is a Category 2 payment model • MIPS was created by combining several other programs: – Physician Quality Report System (PQRS) – Value-Based Modifier (VBM) – Medicare Electronic Health Record (EHR) incentive program and meaningful use (MU) Source: Quality Payment Program, CMS 8

MIPS Drives EPs to APMs MIPS programs increase their impact on provider payments over a series of years. Image: Path to Value, CMS 9

Physicians Quality Reporting System (PQRS) • PQRS: a program that uses negative payment adjustments to promote reporting of quality information by individual Eligible Professionals (EPs) and group practices • All EPs who bill Medicare Part B: ambulatory care affected. • EPs are penalized for not reporting after 2016 Source: CMS, November 12, 2016 10

PQRS Requires Reporting Must report measures from at least 3 of the 6 National Quality Strategy (NQS) domains Source: CMS, March 11, 2016 11

PQRS Reporting Options • EPs must report using one of four options • MU, through a staged implementation, increasingly allows providers to adopt to technology • The increasing use of CEHRT helps ease the burden of reporting 12

Considerations for Constructing Measures • Measure development is complex and highly charged • Patient population should be carefully considered when selecting a process or outcome to measure 13

Measure Harmonization • “Measurement mania” produced an overabundance of measures • Unintended consequences were a result • Measurement consolidation and harmonization produced alignment and simplification of measures. Sources: Health Leaders Media, January 7, 2016; CMS Press Release, February 16, 2016 14

Meaningful Use (MU) • Beginning in 2016, the MU program will see changes • ”Measuring clicks to focusing on care” • Moving forward from 2016, Certified Electronic Health Record Technology (CEHRT) continues to play a role Source: The CMS Blog, January, 2016 15

Health IT Supports Reporting and Measurement for APMs • Consistent adoption of Health IT practices supported by new implementation criteria, including: – Customization – Connectivity – Interoperability • Payment models supported through EHRs • Reporting burden eased through CEHRT 16

Value-Based Modifier • Part of the Affordable Care Act • Phase-in of VBM began in 2015, and would be complete by 2017. • Being rolled into MIPS • The EPs phase is determined by their group size. 17

QRUR Report Sample Sections 1 -3 Image: Fact Sheet: Computation of the 2016 Value Modifier September 2015 18
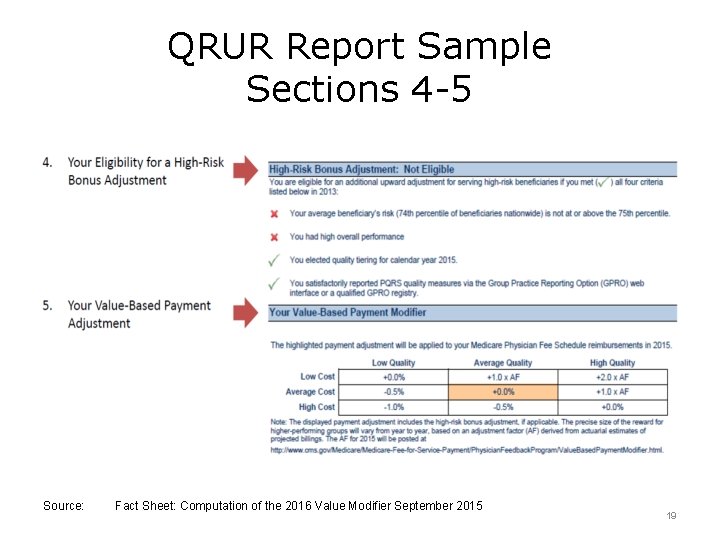

QRUR Report Sample Sections 4 -5 Source: Fact Sheet: Computation of the 2016 Value Modifier September 2015 19
Quality Measures for Hospitals • Readmissions Measures Through 2016 • Up to 3% reduction in total payments Image: Sample AMI hospital admission report, courtesy of Stratis Health Source: CMS, HRR program 20
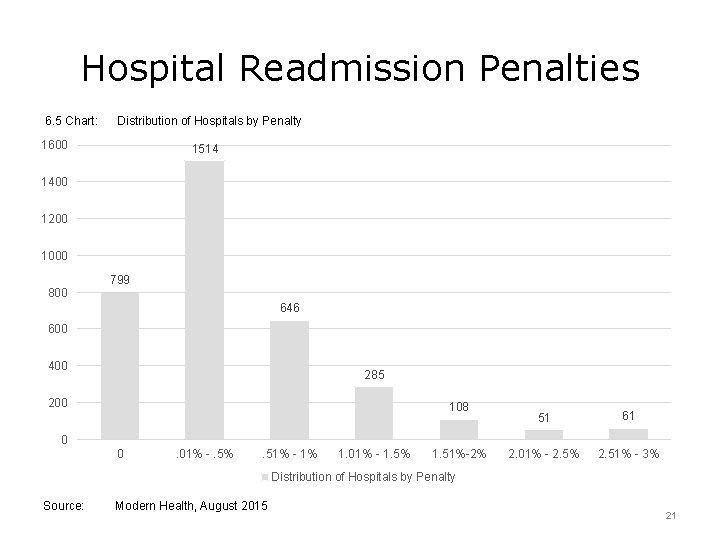
Hospital Readmission Penalties 6. 5 Chart: Distribution of Hospitals by Penalty 1600 1514 1400 1200 1000 800 799 646 600 400 285 200 108 51 61 2. 01% - 2. 5% 2. 51% - 3% 0 0 . 01% -. 5% . 51% - 1% 1. 01% - 1. 5% 1. 51%-2% Distribution of Hospitals by Penalty Source: Modern Health, August 2015 21

Value-Based Model for Home Health • 6 -year test in nine states • Medicare incentives • Measurement based Source: CMS, March 30, 2016 Image: CMS, December 17, 2015 22

How VBM Programs Affect the Value of Care • Fee-for-service hasn’t supported value • Value-based payment models increase potential for lower costs and higher value 23

Volume to Value Lecture b - Summary • Legislation supports the move to VBP • New payment models require reporting on quality measures • Reporting and measurement through CEHRT requires Health IT 24

Volume to Value Lecture b - References 1 References 2016 Physicianl Quality Reporting System (PQRS) List of Eligible Professionals (November 12, 2015). Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov Better Care. Smarter Spending. Healthier People: Paying Providers for Value, Not Volume (January 26, 2015). CMS Fact Sheet. Retrieved from htpps: //www. cms. gov CMS and major commercial health plans, in concert with physician groups and other stakeholders, announce alignment and simplification of quality measures. [Press Release] (February 16, 2016). Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov Donald Berwick on Better Care as a Route to Financial Success (January 7, 2016). Health. Leaders Media. Retrieved from http: //healthleadersmedia. com EHR Incentive Programs (n. d. ). Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov/ Estimated Sustainable Growth Rate and Conversion Factor, for Medicare Payments to Physicians in 2013. (November, 2012). Centers for Medicare and Medicaid Services, Office of the Actuary. Retrieved from: https: //www. cms. gov/ 25

Volume to Value Lecture b - References 2 References Home Health Value-Based Purchasing Model (March 30, 2016). Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov Medicare Access and Chip Reauthorization Act of 2015 Quality Payment Program (April 27, 2016). Notice of Proposed Rule Making. Department of Health & Human Services and Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov Medicare and Medicaid Programs; CY 2016 Home Health Prospective Payment System Rate Update; Home Health Value-Based Purchasing Model; and Home Health Quality Reporting Requirements. (November 5, 2015). Department of Health and Human Services and Centers for Medicare and Medicaid Services. Retrieved from: https: //www. federalregister. gov/ Quality Payment Program: Delivery System Reform, Medicare Payment Reform & MACRA: The Merit-Based Incentive Payment System (MIPS) & Alternative Payment Models (APMs). [web article] (n. d. ) Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov Rice, S. Most hospitals face 30 -day readmissions penalty in fiscal 2016. [Blog] (August 3, 2015). Modern Healthcare Retrieved from http: //www. modernhealthcare. com 26

Volume to Value Lecture b - References 3 References Slavitt, A. and De. Salvo, K. EHR Incentive Programs: Where We Go Next. (January 19, 2016). The CMS Blog. The Hospital Readmission Reduction (HRR) Program (n. d. ). Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov The Merit-Based Incentive Payment System (MIPS) & Alternative Payment Models (APMs). Centers for Medicare and Medicaid Services Retrieved from https: //www. cms. gov Tables, Charts and Figures 6. 4 Table: Payment Taxonomy Framework. CMS Fact Sheet, January 26, 2015. 6. 5 Chart: Distribution of Hospitals by Penalty. Rice, S. (August 3, 2015). Modern Healthcare Retrieved from http: //www. modernhealthcare. com 27

Volume to Value Lecture b - References 4 Images Slide 3: Word Cloud created for use in lecture, CC BY-NC-SA 4. 0 Slide 9: The Medicare Access & Chip Reauthorization Act of 2015: Path to Value (n. d. ). Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov/ Slide 11: 2016 Physician Quality Reporting System (PQRS): Implementation Guide (March 11, 2016). Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov Slide 18 and 19: Fact Sheet: Computation of the 2016 Value Modifier (September 2015). Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov Slide 20: Sample AMI hospital admission report, courtesy Stratis Health CC BY-NC-SA 4. 0 Slide 21: Rice, S. (August 3, 2015). Modern Healthcare Retrieved from http: //www. modernhealthcare. com Slide 22: Home Health Value-Based Purchasing, Home Health Agency Registration [Power. Point presentation] (December 17, 2015). Centers for Medicare and Medicaid Services. Retrieved from: https: //www. cms. gov 28

Volume to Value Lecture b This material was developed by Normandale Community College funded by the Department of Health and Human Services, Office of the National Coordinator for Health Information Technology under Award Number 90 WT 0003. 29
- Slides: 29