ValueBased Care Introduction to ValueBased Care Lecture a

Value-Based Care Introduction to Value-Based Care Lecture a This material (Comp 23 Unit 1) was developed by Normandale Community College and the University of Alabama at Birmingham, funded by the Department of Health and Human Services, Office of the National Coordinator for Health Information Technology under Award Number 90 WT 0003/07. This work is licensed under the Creative Commons Attribution-Non. Commercial-Share. Alike 4. 0 International License. To view a copy of this license, visit http: //creativecommons. org/licenses/by-nc-sa/4. 0/.

Introduction to Value-Based Care Learning Objectives 1 • Describe in general terms the features of the fee-for-service health care system and outline why this payment model is changing • Describe the overall value and goals of value-based care from various stakeholder perspectives • Describe the recent history of the patient empowerment movement and explain why it is key in value-based care 2

Introduction to Value-Based Care Learning Objectives 2 • Name the key pieces of legislation and rule making that create, define, and regulate value-based care • Discuss why attention to improving quality is essential in value-based care • Discuss the types of health information technology that support value-based care 3
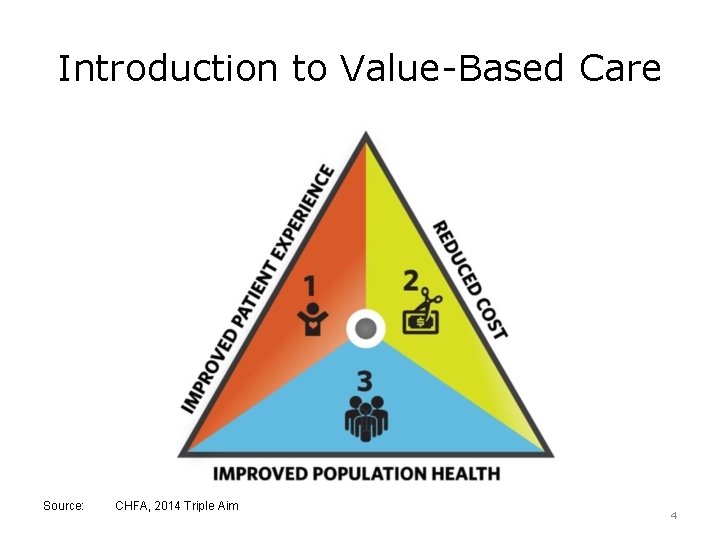
Introduction to Value-Based Care Source: CHFA, 2014 Triple Aim 4

Value in Health Care • Value – “health care outcomes per dollar spent” • Outcomes – Lower mortality and morbidity • Value in U. S. health care – Goal: people live longer, healthier lives for the right amount of money Source: Porter, 2010 5

What is Value-Based Care (VBC)? • “High value, cost-conscious care that aims to assess the benefits, harms and cost of interventions and consequently to provide care that adds value. ” • A set of initiatives, at the federal, state, and private levels to address the problem of value in the U. S. health care system Source: Owens et al, 2011 6
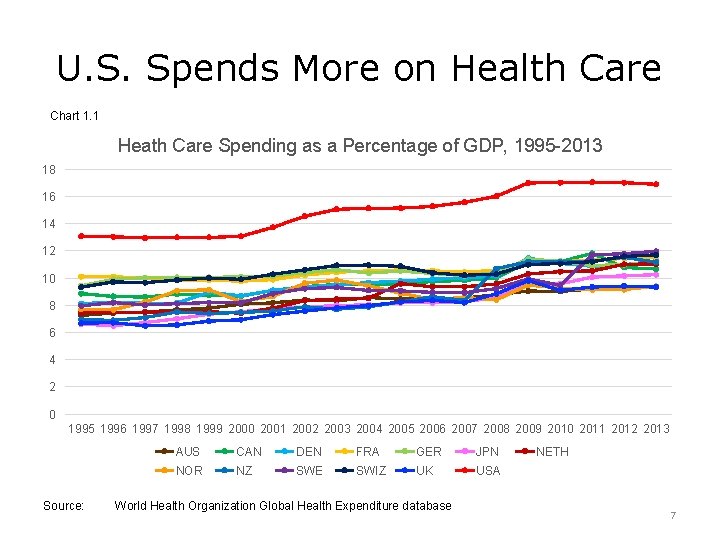
U. S. Spends More on Health Care Chart 1. 1 Heath Care Spending as a Percentage of GDP, 1995 -2013 18 16 14 12 10 8 6 4 2 0 1995 1996 1997 1998 1999 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 2013 Source: AUS CAN DEN FRA GER JPN NOR NZ SWE SWIZ UK USA World Health Organization Global Health Expenditure database NETH 7
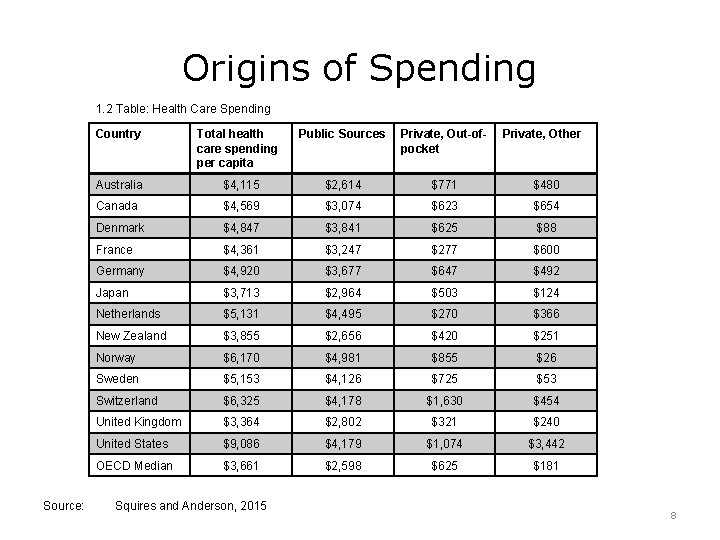
Origins of Spending 1. 2 Table: Health Care Spending Source: Country Total health care spending per capita Public Sources Private, Out-ofpocket Australia $4, 115 $2, 614 $771 $480 Canada $4, 569 $3, 074 $623 $654 Denmark $4, 847 $3, 841 $625 $88 France $4, 361 $3, 247 $277 $600 Germany $4, 920 $3, 677 $647 $492 Japan $3, 713 $2, 964 $503 $124 Netherlands $5, 131 $4, 495 $270 $366 New Zealand $3, 855 $2, 656 $420 $251 Norway $6, 170 $4, 981 $855 $26 Sweden $5, 153 $4, 126 $725 $53 Switzerland $6, 325 $4, 178 $1, 630 $454 United Kingdom $3, 364 $2, 802 $321 $240 United States $9, 086 $4, 179 $1, 074 $3, 442 OECD Median $3, 661 $2, 598 $625 $181 Squires and Anderson, 2015 Private, Other 8

Cross-National Comparisons “Cross-national comparisons show that if the U. S. health care system performed like systems in other Western democracies, individuals would live longer lives and spend less, and the United States could provide universal access to care. ” Source: Blumenthal D. , March 03, 2016 9
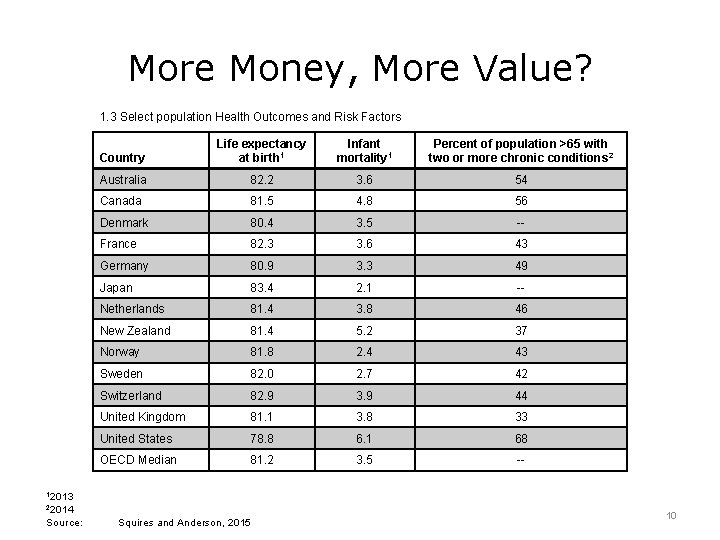
More Money, More Value? 1. 3 Select population Health Outcomes and Risk Factors Country Life expectancy at birth 1 Infant mortality 1 Percent of population >65 with two or more chronic conditions 2 Australia 82. 2 3. 6 54 Canada 81. 5 4. 8 56 Denmark 80. 4 3. 5 -- France 82. 3 3. 6 43 Germany 80. 9 3. 3 49 Japan 83. 4 2. 1 -- Netherlands 81. 4 3. 8 46 New Zealand 81. 4 5. 2 37 Norway 81. 8 2. 4 43 Sweden 82. 0 2. 7 42 Switzerland 82. 9 3. 9 44 United Kingdom 81. 1 3. 8 33 United States 78. 8 6. 1 68 OECD Median 81. 2 3. 5 -- 12013 22014 Source: Squires and Anderson, 2015 10
One Possible Culprit: Fee-for-Service (FFS) 11

Benefits of the Fee-for-Service Model • Fee-for-service pays health care providers for activity, creating an incentive to work hard • The more you do, the more you’re paid • There is no incentive under Fee-for. Service for providers to withhold health care 12

Drawbacks of the Fee-for-Service Model • Fee-for-Service can result in unnecessary tests, procedures, visits, etc. , because the provider is paid based on activity • The biggest problem from a value perspective is that traditional Fee-for. Service is not linked to outcomes: the provider is paid whether or not your health improves 13

Broad Strategy to Increase Value • Volume to Value – Rewards for achieving health outcomes • Pay for Performance – Incentives for desirable behavior 14

Leadership for the Pay for Performance Strategy • Center for Medicare and Medicaid Services (CMS) sums up the strategy as moving away from rewarding volume in order to improve care quality and reduce costs. • Reward value and care coordination rather than volume and care duplication Source: CMS. GOV 2015 Fact Sheet 15

What Supports the Move to VBC? • Quality Measurement • Reporting of performance to metrics • Incentive or penalty 16

Health IT for VBC • Electronic Health Record data • Improving outcomes using analytics • Clinical decision support 17

Laws That Support the Transition – HITECH and ACA 1. 4 Table: Laws that Support the Transition to VBC Legislation Year Passed Purpose HITECH 2009 Over 95% of hospitals are meaningful users. Over 80% of officebased MDs using EHRs. Technology base for VBC firmly in place ACA PPACA Obamacare 2010 to increase the quality and affordability of health insurance, lower the uninsured rate and reduce the costs of health care MACRA 2015 Ending the SGR. Combining existing quality reporting programs into one new system. Details of MIPS and APMs Source: MIPS and (October 2015). APMs, cms. gov 18
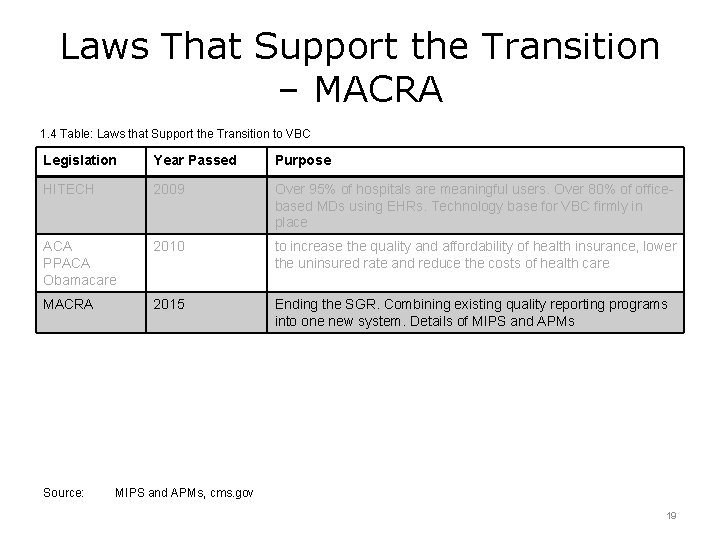

Laws That Support the Transition – MACRA 1. 4 Table: Laws that Support the Transition to VBC Legislation Year Passed Purpose HITECH 2009 Over 95% of hospitals are meaningful users. Over 80% of officebased MDs using EHRs. Technology base for VBC firmly in place ACA PPACA Obamacare 2010 to increase the quality and affordability of health insurance, lower the uninsured rate and reduce the costs of health care MACRA 2015 Ending the SGR. Combining existing quality reporting programs into one new system. Details of MIPS and APMs Source: MIPS and APMs, cms. gov 19

Merit-Based Incentive Payment System • Developed by CMS • Combines several programs 1. Meaningful Use 2. Value-Based Modifier 3. Physician Quality Reporting System 4. Clinical practice improvement activities • Adopted by private insurers 20

Alternative Payment Models (APMs) • Medical homes – Responsibility for a population of patients – Incentivized for care coordination • Bundled payments – Fixed price for all care related a procedure • Capitated payments 21

Accountable Care Organizations • An Accountable Care Organization (ACO) is a group of providers that are jointly responsible for the health care spending and quality of a particular population of patients • In 2015, there were 400 ACOs serving 7. 2 million beneficiaries Source: Abrams et al. , 2015
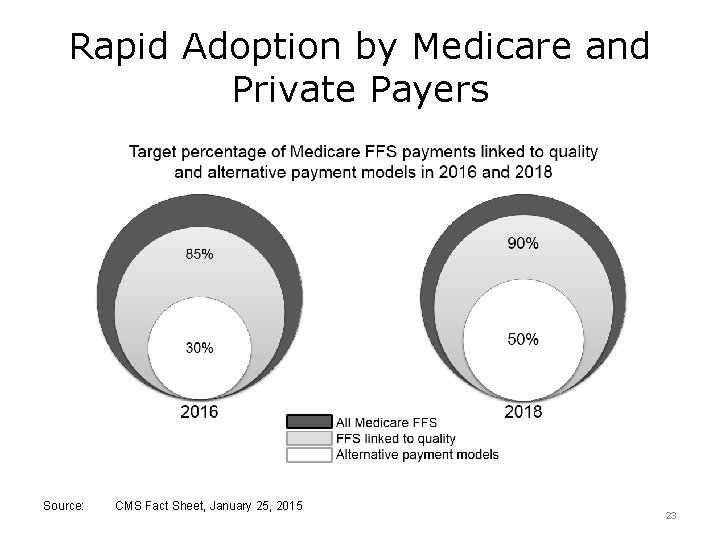
Rapid Adoption by Medicare and Private Payers Source: CMS Fact Sheet, January 25, 2015 23

Key Supporting Elements for Value-Based Care • • Care Coordination Population Health Focus Analytics and Monitoring Quality Improvement Care Management Fiscal Management Patient Engagement
The Patient as a Consumer Source: Patient as Consumer infographic 25

Patient Engagement • Past – Directive – Patients do what physician tells them to do • Present – Partnership – Patients as partners, being active in their care 26

Achieving High-Value Health Care • Ambitious goals 27

Examples of Organizations Delivering High-Value Care Three standouts 1. Northwest Family Physicians, MN – Small, privately-owned clinic 2. Montefiore Health System, NY – Large health system 3. South. Central Foundation, AK – Health system for native people of Alaska 28

Organizations Share Characteristics • Shared characteristics – Importance of primary and preventive care – Focus on keeping people out of hospital – Emphasis on innovation and change – Focus on quality measures – Electronic health record systems 29

Introduction to Value-Based Care Summary • Terms and features of the fee-for-service health care system and why this payment model is changing. • Overall value and goals of value-based care from various stakeholder perspectives. • The key pieces of legislation that create, define, and regulate value-based care. • The recent history of the patient empowerment movement and why it is key in value-based care. 30

Introduction to Value-Based Care Lecture a – References 1 References Accountable Care Organizations. (January 26, 2015). Retrieved from: The Centers for Medicare and Medicaid Services (CMS): https: //www. cms. gov/ Better Care. Smarter Spending. Healthier People: Paying Providers for Value, Not Volume. (2015). CMS 2015 Fact Sheet, press@cms. hhs. gov. Retrieved from: CMS: https: //www. cms. gov/ Blumenthal, D. (March 03, 2016). Better Health Care: A Way Forward. JAMA. doi: 10. 1001 Owens D. K. , Qaseem A. , Chou R. , Shekelle P. , (2011). High-Value, Cost-Conscious Health Care: Concepts for Clinicians to Evaluate the Benefits, Harms, and Costs of Medical Interventions. Ann Intern Med. (for the Clinical Guidelines Committee of the American College of Physicians). 154: 174 -180. doi: 10. 7326/0003 -4819 -154 -3201102010 -00007 Porter, M. E. (December 23, 2010). What Is Value in Health Care? N Engl J Med, 363: 2477 -2481 DOI: 10. 1056/NEJMp 1011024 Squires, D. and Anderson, C. (October 2015). U. S. Health Care from a Global Perspective: Spending, Use of Services, Prices, and Health in 13 Countries. The Commonwealth Fund. Retrieved from The Commonwealth Fund: www. commonwealthfund. org/ 31

Introduction to Value-Based Care Lecture a – References 2 References The Merit-Based Incentive Payment System (MIPS) & Alternative Payment Models (APMs). (n. d. ). The Centers for Medicare and Medicaid Services. Retrieved from: CMS: https: //www. cms. gov/ Unger, L. (March 16, 2015). Uninsured rates drop dramatically under Obamacare. U. S. A Today. Retrieved from: http: //www. usatoday. com/ Charts, Tables, Figures 1. 1 Chart: Health expenditure, total (% of GDP). World Health Organization Global Health Expenditure database. Retrieved from: http: //www. data. worldbank. org 1. 2 Table: Health Care Spending 2013. (October 2015). Squires, D. and Anderson, C. 1. 3 Table: Select Population Health Outcomes and Risk Factors. (October 2015). Squires, D. and Anderson, C. 1. 4 Table: Laws that support the transition to VBC compiled from The Merit-Based Incentive Payment System (MIPS) & Alternative Payment Models (APMs). (n. d. ) The Centers for Medicare and Medicaid Services. 32

Introduction to Value-Based Care Lecture a – References 3 Images Slide 4: From Fragmentation to Integration: A Triple Aim Imperative [Online image]. (2014). CFHA 16 th Annual Conference. Retrieved from: http: www/chfa. net/ Slide 11: Fee for Service Process Flow, created for use in program. Slide 23: CMS’s targeted adoption goals for APMs (2015). Centers for Medicare and Medicaid Services. Retrieved April 21, 2015 from CMS: https: //www. cms. gov/ Slide 25: Patient as Consumer, created for use in program. Slide 27: Cost and Care, created for use in program. 33

Introduction to Value-Based Care Lecture a This material (Comp 23 Unit 1) was developed by Normandale Community College and the University of Alabama at Birmingham, funded by the Department of Health and Human Services, Office of the National Coordinator for Health Information Technology under Award Number 90 WT 0003/07. 34
- Slides: 34