VA Puget Sound Health Care System Deployment Health
















- Slides: 21

VA Puget Sound Health Care System Deployment Health Clinic Outreach Post-Combat Evaluations Follow-up Care 1/8/2022 * 1

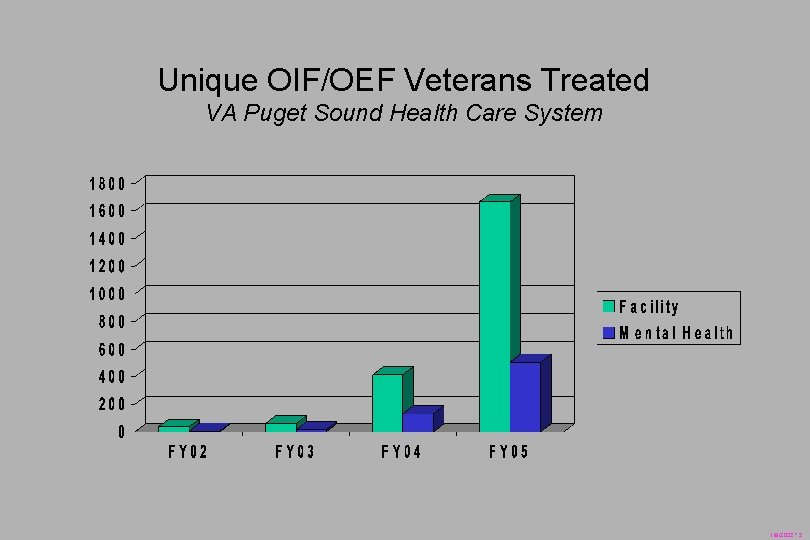
Unique OIF/OEF Veterans Treated VA Puget Sound Health Care System 1/8/2022 * 2

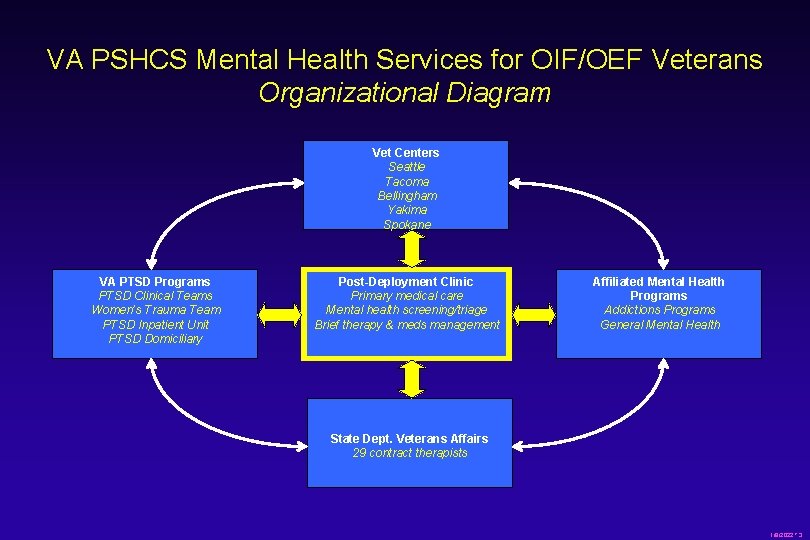
VA PSHCS Mental Health Services for OIF/OEF Veterans Organizational Diagram Vet Centers Seattle Tacoma Bellingham Yakima Spokane VA PTSD Programs PTSD Clinical Teams Women’s Trauma Team PTSD Inpatient Unit PTSD Domiciliary Post-Deployment Clinic Primary medical care Mental health screening/triage Brief therapy & meds management Affiliated Mental Health Programs Addictions Programs General Mental Health State Dept. Veterans Affairs 29 contract therapists 1/8/2022 * 3

Integrated Care for Combat Veterans Common Barriers to Treatment • • Lack of information on available services • • • Stigma against receiving care (mental or physical) Perceived/actual problems with access to services (dropped cases referred to specialty clinics) Lack of information on health risks Low priority of care compared to “getting back to normal life” 1/8/2022 * 4

Deployment Health Clinic Integrated Care for Combat Veterans “We recommend a comprehensive post-combat evaluation to establish a baseline snapshot of how you are functioning now” • Physical exam and mental health evaluation with attention to pertinent deployment experiences/environmental risks • Ongoing care to provide necessary treatment and monitoring for any emerging combat related conditions. • Education regarding available benefits/sources of support for the veteran and his/her family to ease transition 1/8/2022 * 5

Deployment Health Clinic The Deployment Health Clinic is dedicated to the care of veterans who are experiencing mental or physical health concerns related to a specific deployment (Gulf War I, Peace-Keeping Deployments, OIF/OEF) A philosophy of mind-body relationships is adopted in which medical and mental health concerns are presumed to interrelate 1/8/2022 * 6

VA Puget Sound Health Care System Deployment Health Clinic The purpose of the Deployment Health Clinic is to: • • Provide Outreach and Community Educational Services Address and support the veteran in all aspects of life which have been affected by their combat experience. • • Provide that support in an accessible and integrated format Provide support in an ongoing way for as long as it is needed 1/8/2022 * 7

VA Puget Sound Health Care System Deployment Health Clinic The objective of the Deployment Health Clinic is to: Provide the support necessary for the veteran and his/her family to readjust, recover and be optimally functioning in all realms as soon as possible after return from combat and for the long term. 1/8/2022 * 8

VA Puget Sound Health Care System Deployment Health Clinic • Staff Members » Primary Care Physician » Registered Nurse Practioner » Clinical Psychologist » Masters-level mental health counselor » Psychiatrist 1/8/2022 * 9

Integrated Care for Combat Veterans Primary Treatment Interventions • Deployment Health Clinic Services: » Integrated mental health and medical post combat care » Preventive/health promotion based care » Family involvement in care » Innovative psychiatric medication treatments (i. e. , prazosin) » Innovative Cognitive Behavioral Interventions (Brief Motivational Interviewing, BA, ACT, Mindfulness) » Referrals to inpatient/outpatient mental health services (PTSD, substance abuse, general mental health services) or specialty medical clinics within the VA Medical System 1/8/2022 * 10

VA Puget Sound Health Care System Deployment Health Clinic Post-combat care: Using the two years of post-combat priority eligibility proactively as a period for assessment, monitoring and utilization of appropriate services directed towards optimal recovery, rehabilitation and reintegration into post-combat, non-military life. 1/8/2022 * 11

Mental Health Problems and Clinical Services for OIF/OEF Veterans 1/8/2022 * 12

Common Post-Deployment Readjustment Reactions • Problems with finances, employment, and housing • Preoccupation with news about the war • Worry about friends still deployed overseas • Missed excitement of combat with urges to return • Adjustment to “civilian” norms • Altered schedule for sleeping and eating • Marital conflict and family reintegration problems 1/8/2022 * 13

Integrated Deployment Clinic Care Presenting Psychosocial Health Concerns • Redefined familial roles • Marital/parenting issues • Public Social Functioning • Occupational/financial concerns • Separation from military social support • Risk of re-deployment 1/8/2022 * 14

Common Mental Health Disorders • Anxiety disorders » Adjustment Disorder, Generalized Anxiety, Panic Disorders, PTSD (or PTSD-like syndromes) • Depressive Disorders » Adjustment Disorder, Dysthymia, Major Depressive Disorder • Substance Misuse, Abuse, and Dependency 1/8/2022 * 15

Mental Health Profiles of returning OIF/OEF Veterans Presenting to the Deployment Health Clinic (N = 128) • • Demographics: Mean age was 32. 2 years, 95. 3% were male, 72. 2% Caucasian, and 50. 8% were married. Measures » The PTSD Checklist Military Version (PCL-M) (Weathers, Huska, and Keane, 1991) » The PRIME-MD Patient Health Questionnaire (PHQ) (Spitzer, Kroenke, and Williams, 1999) t depression (major depressive disorder), t anxiety (any anxiety disorder except panic disorder) t alcohol misuse (abuse or dependence) » Barriers to Mental Health Care (Hoge et al. , 2004) 1/8/2022 * 16

Combat Exposure • Event (Percentage) » stationed close to enemy lines (87. 0%), » faced an extreme threat to their personal safety (86. 9%) » received incoming fire from mortars, rockets, or artillery (74. 2%). » one or more firefight (59. 8%) » mines or booby traps (55. 2%) » sniper or sapper fire (51. 2%). » witnessed an accidental death (31. 7%) » took care of someone who’s life wasn’t saved (28. 8%) » were responsible for someone else’s death (11. 2%) » observed the death of a close friend (10. 1%) 1/8/2022 * 17

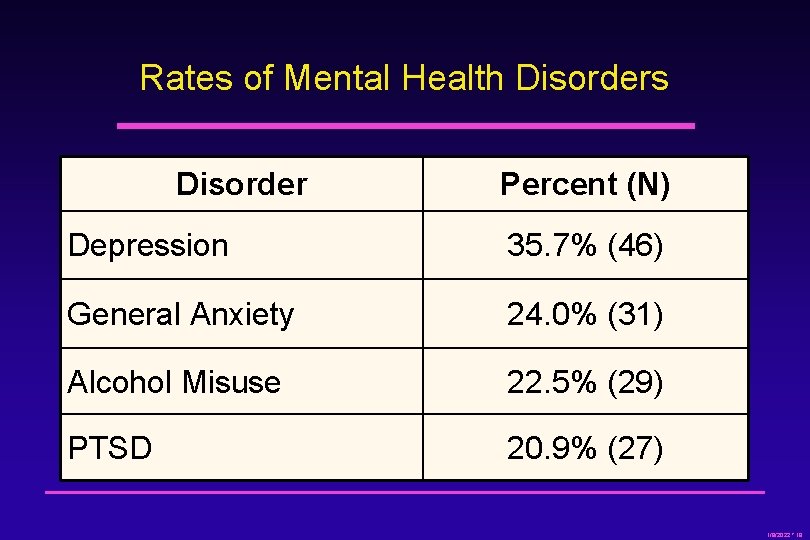
Rates of Mental Health Disorders Disorder Percent (N) Depression 35. 7% (46) General Anxiety 24. 0% (31) Alcohol Misuse 22. 5% (29) PTSD 20. 9% (27) 1/8/2022 * 18

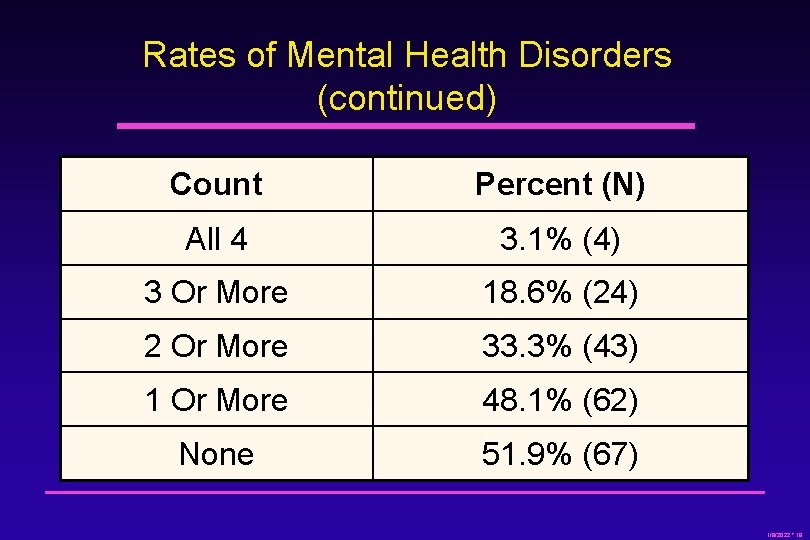
Rates of Mental Health Disorders (continued) Count Percent (N) All 4 3. 1% (4) 3 Or More 18. 6% (24) 2 Or More 33. 3% (43) 1 Or More 48. 1% (62) None 51. 9% (67) 1/8/2022 * 19

Barriers to Receiving Mental Health Care • The most frequently cited barriers to accessing mental health services: » financial (35. 4%) » fear of being perceived as weak (30. 8%) » fear of being treated differently by unit leadership or employers (26. 2%). 1/8/2022 * 20

Deployment Health Clinic Integrated Care for Combat Veterans Question: Does routine delivery of mental health assessment/ treatment in the primary care setting reduce stigma, improve satisfaction with care, and/or increase utilization of mental health services among soldiers returning from OIF/OEF? 1/8/2022 * 21