Uveal Disorders By Ahmad Mostafa MD Professor of

Uveal Disorders By Ahmad Mostafa, MD Professor of Ophthalmology

► The following subjects will be discussed in the same order: 1. Anatomy of the uveal tract 2. Physiology of the pupil 3. Uveitis: a. Definition of uveitis b. Classification of uveitis c. Clinical features of uveitis d. Complications of uveitis e. Treatment of uveitis f. Specific uveitis syndromes

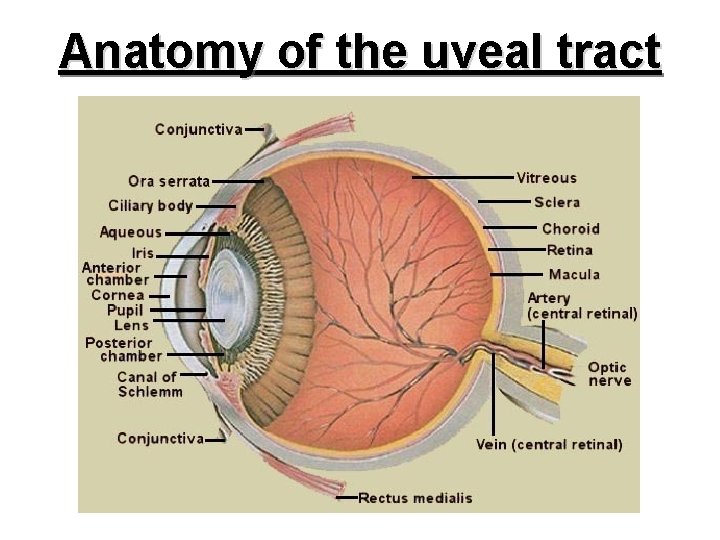
Anatomy of the uveal tract

Anatomy of the uveal tract • Anatomy of the iris a. Gross anatomy c. Blood supply • Anatomy of the ciliary body a. Gross anatomy c. Blood supply • b. Minute anatomy d. Nerve supply Anatomy of choroid a. Gross anatomy c. Blood supply b. Minute anatomy d. Nerve supply


Physiology of the pupil A. Normal Pupillary Reactions (A) Light reflex: reflex 1. 2. Direct Indirect (Consensual) (B) Near or Accommodation Reflex: - On fixing a near object, 3 associated actions occur: 1. 2. 3. Accomodation: Accomodation CB contraction Convergence: Convergence contraction of both medial recti Miosis: by contraction of sphincter pupillae muscle.

B. Abnormal Pupillary Reactions a. Argyll Robertson’s pupil b. Marcus-Gunn pupil C. Horner’s syndrome


Uveitis a. Definition of uveitis b. Classification of uveitis c. Clinical features of uveitis d. Complications of uveitis e. Treatment of uveitis f. Specific uveitis syndromes

Definition of Uveitis • Uveitis is an inflammation of the uveal tract • May be: iritis, iridocyclitis, Pars planitis, choroiditis, chorioretinitis.

Classification of Uveitis A. Anatomical Classification B. Clinical Classification C. Aetiological Classification D. Pathological Classification
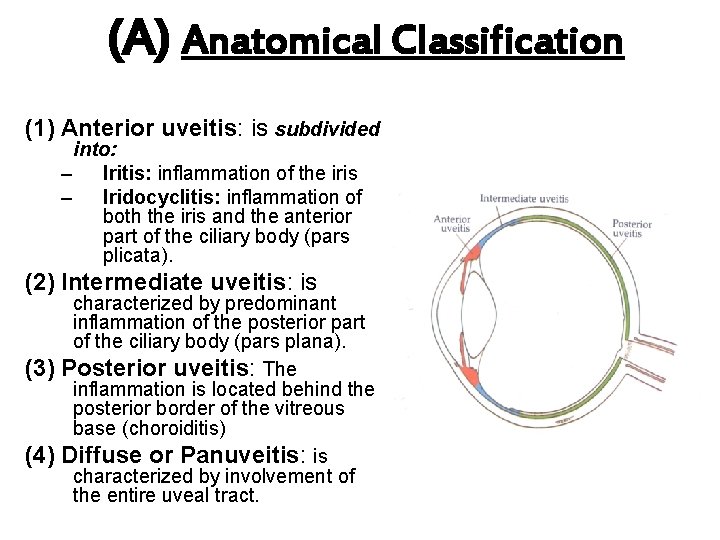
(A) Anatomical Classification (1) Anterior uveitis: is subdivided into: – Iritis: inflammation of the iris – Iridocyclitis: inflammation of both the iris and the anterior part of the ciliary body (pars plicata). (2) Intermediate uveitis: is (3) (4) characterized by predominant inflammation of the posterior part of the ciliary body (pars plana). Posterior uveitis: The inflammation is located behind the posterior border of the vitreous base (choroiditis) Diffuse or Panuveitis: is characterized by involvement of the entire uveal tract.

(B) Clinical Classification (1) Acute uveitis: with a sudden onset and duration of < 6 weeks (2) Chronic uveitis: with an insidious onset and lasts for months or years.

(C) Aetiological Classification a. Exogenous uveitis is caused by either external injury to the uvea or invasion of microaneurysms or other agents from outside. b. Endogenous uveitis is caused by microaneurysms or other agents from within the patient. - The following are the main types: 1. Associated with systemic diseases e. g. ankylosing spondylitis. 2. Infection which may be: • • Bacterial e. g. tuberculosis Viral e. g. herpes zoster Fungal e. g. candidiasis Parasitic e. g. toxoplasmosis & toxocariasis 3. Idiopathic non-specific uveitis entities which constitute about 25% of all cases of uveitis.

(D) Pathological Classification 1. Granulomatous uveitis e. g. sarcoidosis 2. Non-granulomatous uveitis

Clinical Picture of uveitis
Clinical picture of Uveitis • A. Clinical picture of anterior uveitis (iridocyclitis) • B. Clinical picture of intermediate uveitis (Pars planitis) • C. Clinical picture of posterior uveitis (choroiditis, chorioretinitis)

(a) Clinical Picture of Iridocyclitis

A. Symptoms ► In acute iridocyclitis, the main symptoms are: Pain redness Photophobia lacrimation Diminution of vision
Pain • Cause: Cause 1. Irritation of sensory nerves of the iris & CB ( iris is richly supplied by branches from ophthalmic division of 5 th nerve) 2. Spasm of sphincter pupillae m & ciliary m. • Type: - dull aching in character (Neuralgic pain) - Increase at night due to congestion of the head & neck area - Referred to the eyebrow (as headache) along branches of 5 th nerve.

Photophobia, Lacrimation & blepharospasm • Cause: Cause Reflex irritation of sensory nerve endings of 5 th CN.

Diminution of vision • Causes: 1. Aqueous & vitreous haze (turbidity) 2. Corneal edema & KPs 3. Ciliary spasm transient myopia (1 -2 D) 4. Toxic maculopathy (diffusion of prostaglandins into the posterior pole) 5. Secondary glaucoma (due to angle block)

B. Signs • Eyelids • Conjunctiva • Cornea • AC • Iris • Pupil • CB • Lens • Vitreous • IOP

1. Eyelids • Lid edema & redness
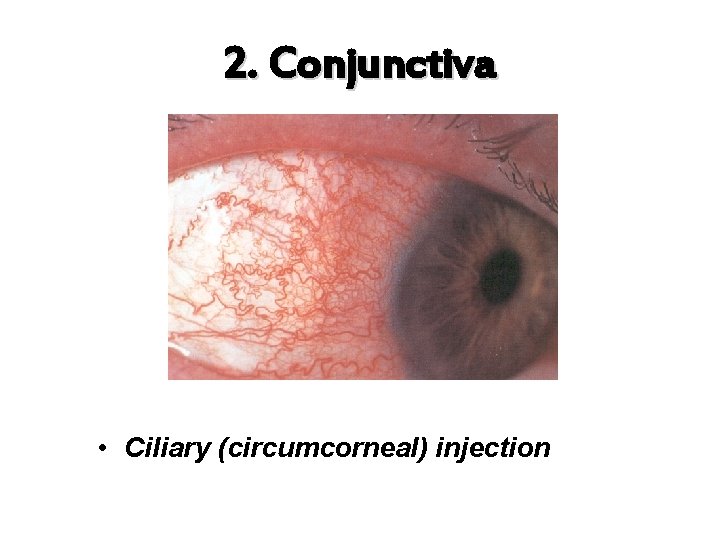
2. Conjunctiva • Ciliary (circumcorneal) injection
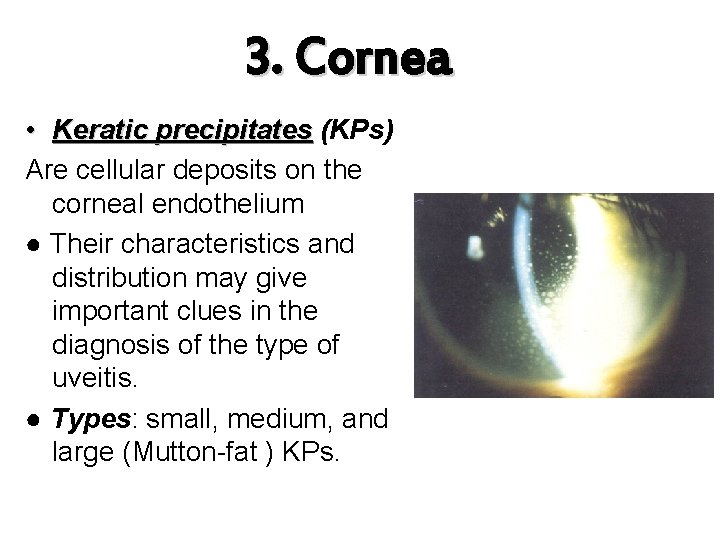
3. Cornea • Keratic precipitates (KPs) Are cellular deposits on the corneal endothelium ● Their characteristics and distribution may give important clues in the diagnosis of the type of uveitis. ● Types: small, medium, and large (Mutton-fat ) KPs.

4. Anterior Chamber a. Aqueous flare b. Aqueous cells c. Hypopyon d. Hyphema

a. Aqueous flare - It is the earliest sign of iritis - It is the result of leakage of proteins into the aqueous through the damaged iris blood vesselss. - it is not indicative of active inflammation, SO the presence of aqueous flare in the absence of aqueous cells is not an indication for activity of the disease or failure of treatment. - It is graded from 0 to +4

b. Aqueous cells ● Aqueous cells are signs of active inflammation. ● They are graded from + 1 to + 4 as follows: • • 5 – 10 cells grade + 1 11 – 20 cells grade + 2 21 – 50 cells grade + 3 > 50 cells grade + 4
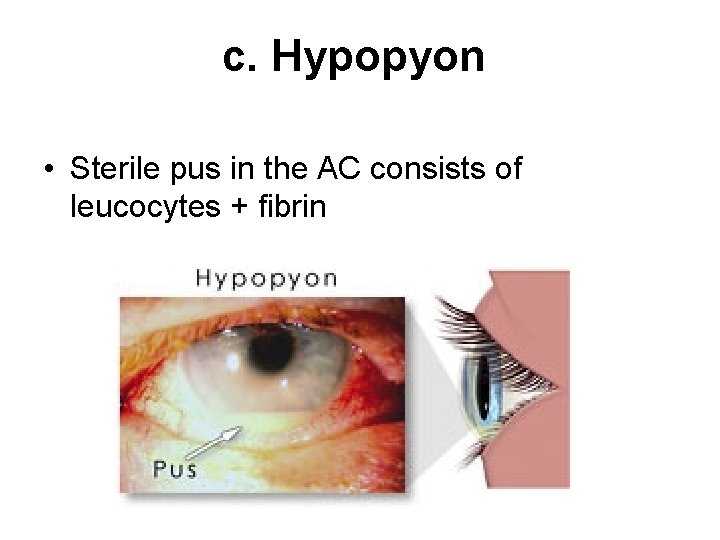
c. Hypopyon • Sterile pus in the AC consists of leucocytes + fibrin

d. Hyphema • a. b. c. d. May occur in some cases of severe iritis or iridocyclitis e. g. : Traumatic Herpetic Diabetic Gonococcal

5. Iris • Loss of iris pattern • Is muddy in color due to: loss of iris pattern, accumulation of exudates on its surface, and altered its color (yelloishbrown)
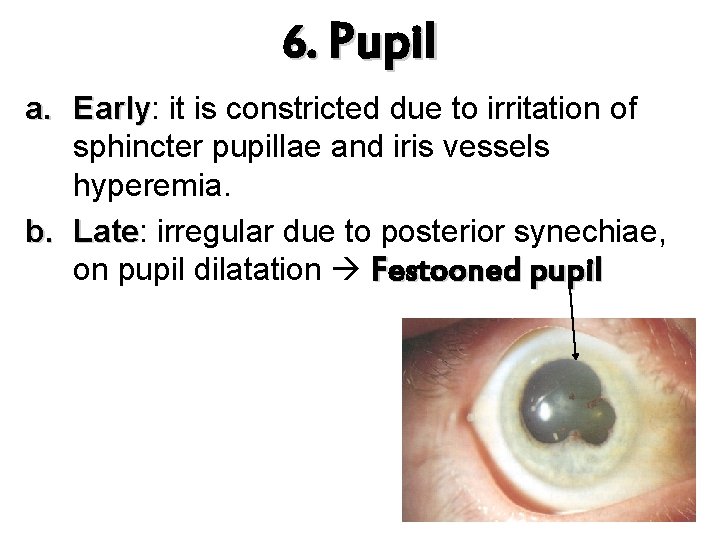
6. Pupil a. Early: Early it is constricted due to irritation of sphincter pupillae and iris vessels hyperemia. b. Late: Late irregular due to posterior synechiae, on pupil dilatation Festooned pupil

7. Ciliary Body • Is tender if palpated through the lids • Transient myopia due to spasm of ciliary muscles

8. Lens • Lenticular precipitates (cataract later on)

9. Vitreous • Anterior vitreous cells & turbidity in the retrolental space and anterior 1/3 of the vitreous

10. IOP • May be high (2 ry glaucoma) due to angle block (plasmoid aqueous) • May be low from suppression of aqueous secretion by chronically inflammed ciliary body

(b) Clinical Picture of intermediate uveitis

• (A) Symptoms: ● Are usually floaters ● Some patients may present with impairment of visual acuity due to cystoid macular edema (CME). (B) Signs: are bilateral in 80% of cases but frequently asymmetrical: ► Intermediate uveitis is characterized by: 1. Minimal or absent anterior uveitis: – KPs are small & few in number – Few, if any, cells in the AC 2. Vitritis: cellular infiltration of the vitreous (cells, snowballs & PVD).

"Snowball" vitritis in pars planitis 3. Snowbanking is the hallmark of pars planitis, it consists of grey-white opacities involving inferior pars plana. Inferior peripheral "snowbanking" in pars planitis

4. No focal inflammatory lesions in the fundus. ● Complications 1. Cystoid macular edema (CME): is the most common cause of impairment of vision in intermediate uveitis. 2. Cataract (uncommon) 3. Cyclitic membrane formation (rare) 4. Tractional RD (rare).
- Slides: 42