Using PopulationBased Data to Estimate Treatment Gaps in

Using Population-Based Data to Estimate Treatment Gaps in Depression and the Impact of Physician Incentives Joseph H Puyat, MA (Psychology), MSc, Ph. D Centre for Health Evaluation & Outcome Sciences Providence Health Care 29 November 2016


Outline 1) Background 2) Gaps and variations in depression care 3) Impact of physician on depression care 4) Conclusions For more info: jpuyat@cheos. ubc. ca https: //www. researchgate. net/profile/Joseph_Puyat

What is Depression? • Mood Disorder • > 5 symptoms from the following Sleep changes Interest (loss of) Guilt (feelings of) Energy (lack of) Cognition (substantial changes in) Appetite (loss of) Psychomotor (irritability or depressed mood) Suicidality
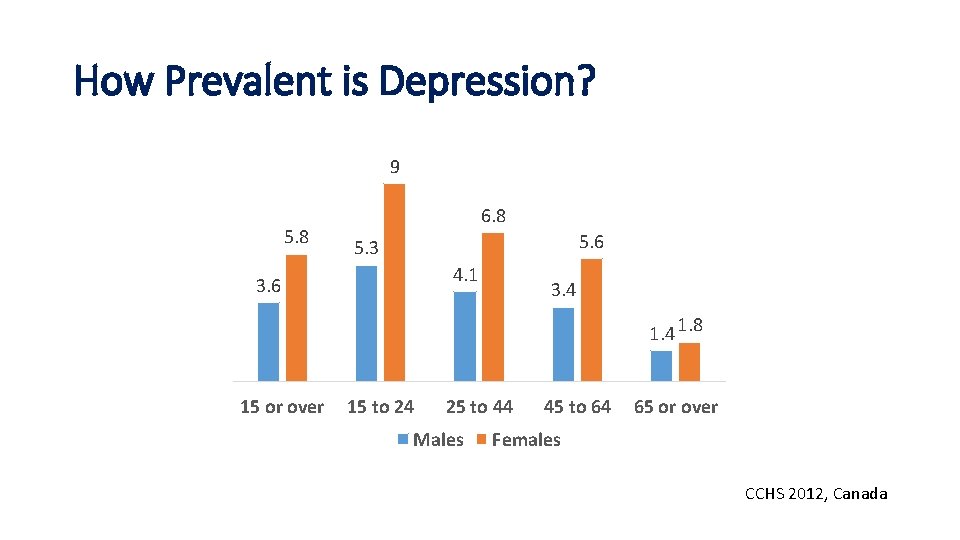
How Prevalent is Depression? 9 5. 8 6. 8 5. 6 5. 3 4. 1 3. 6 3. 4 1. 8 15 or over 15 to 24 25 to 44 Males 45 to 64 65 or over Females CCHS 2012, Canada
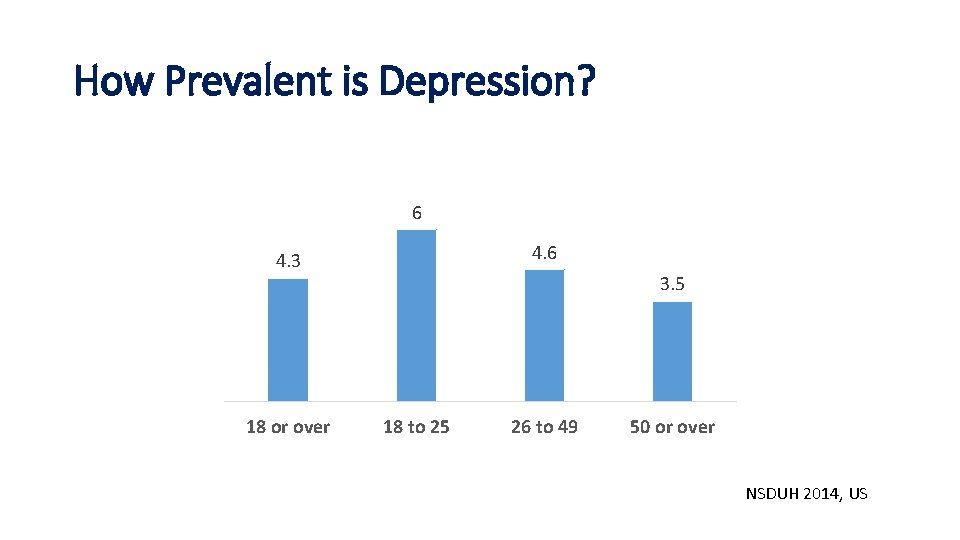
How Prevalent is Depression? 6 4. 3 18 or over 3. 5 18 to 25 26 to 49 50 or over NSDUH 2014, US

How is Depression Treated?
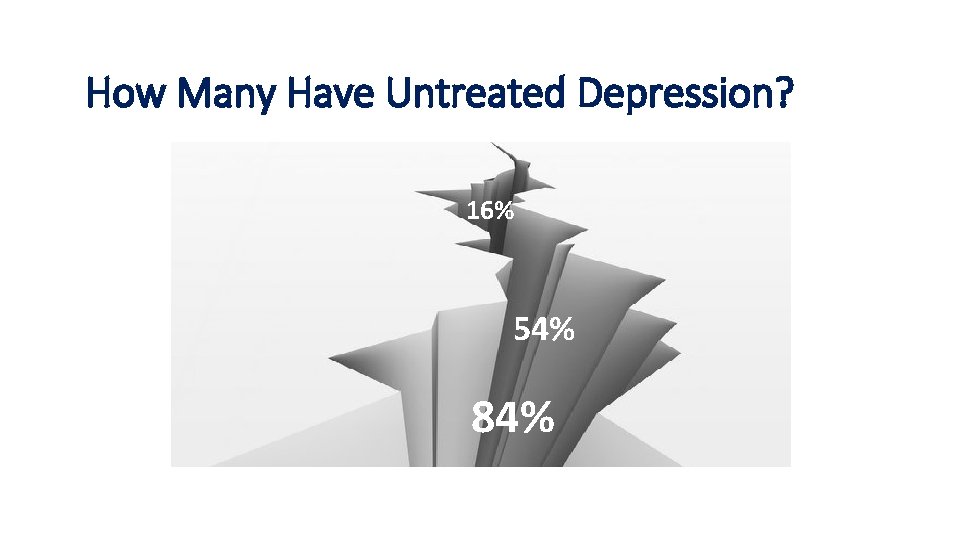
Treatment How Many. Gap Have Untreated Depression? 16% 54% 84%

So What? Global Burden of Disease Study Depression is the leading cause of disability worldwide (1990, 2000, 2010, 2020) Depression costs the economy CAD$32. 3 B/year

Data 1) 2) 3) 4) 5) Canadian Community Health Survey Medical Services Payment (MSP) Data Mental Health Services Data File Hospital Discharge Database Pharma. Net Database
![Treatment Gap [CATEGORY NAME] [VALUE] Treated [VALUE] Statistics Canada, CCHS 2012 Treatment Gap [CATEGORY NAME] [VALUE] Treated [VALUE] Statistics Canada, CCHS 2012](http://slidetodoc.com/presentation_image_h2/73820d9d2fa3dfde686b4a7a70caf033/image-11.jpg)
Treatment Gap [CATEGORY NAME] [VALUE] Treated [VALUE] Statistics Canada, CCHS 2012
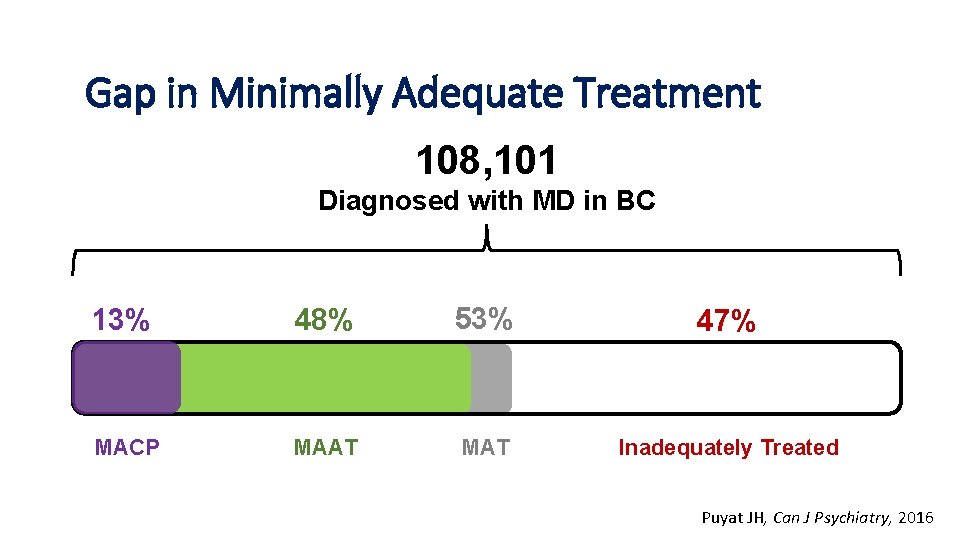
Gap in Minimally Adequate Treatment Overall Results 108, 101 Diagnosed with MD in BC 13% 48% 53% 47% MACP MAAT MAT Inadequately Treated Puyat JH, Can J Psychiatry, 2016
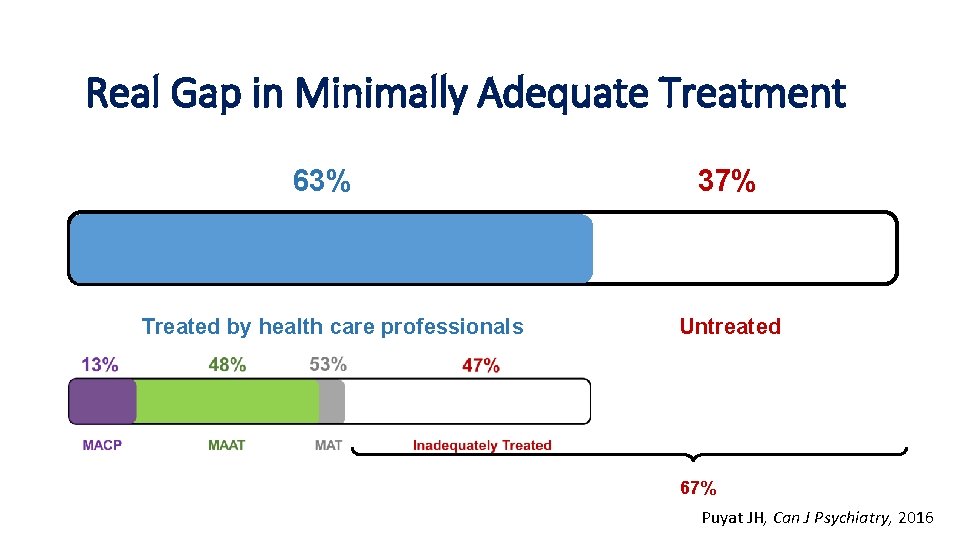
Overall Results Real Gap in Minimally Adequate Treatment 63% Treated by health care professionals 37% Untreated MAT 33% 67% Puyat JH, Can J Psychiatry, 2016
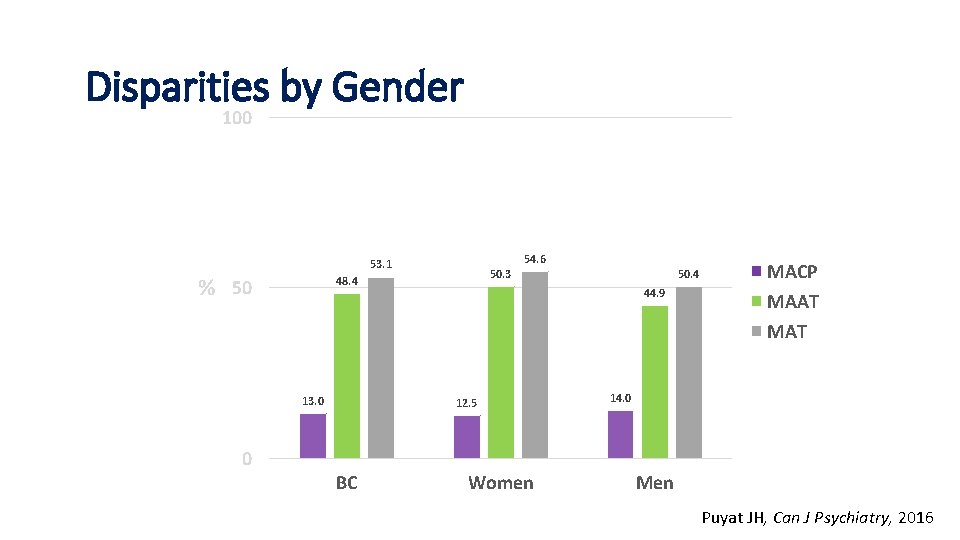
Sex and MAT Disparities by Gender 100 54. 6 53. 1 % 50 13. 0 50. 4 50. 3 48. 4 44. 9 12. 5 MACP MAAT MAT 14. 0 0 BC Women Men Puyat JH, Can J Psychiatry, 2016
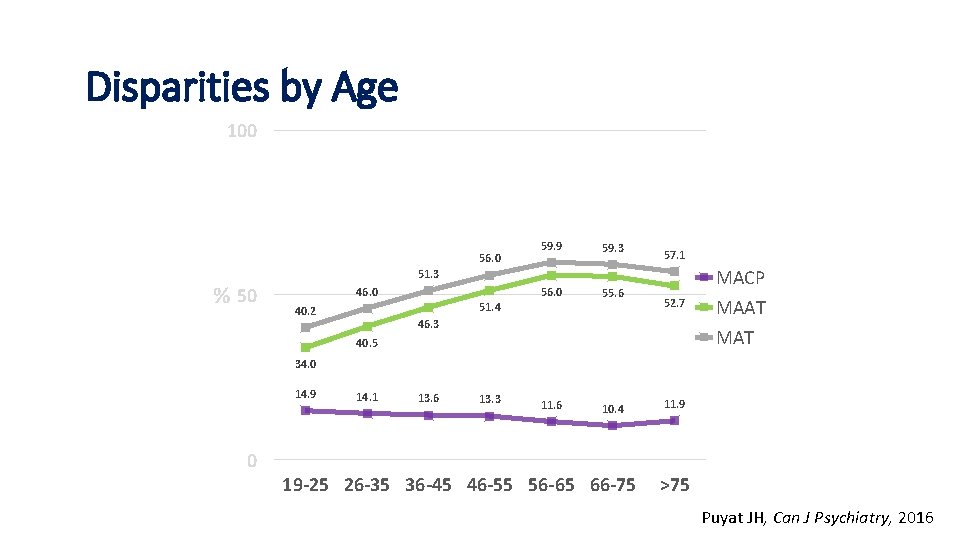
Age and MAT Disparities by Age 100 56. 0 % 50 59. 9 59. 3 57. 1 51. 3 46. 0 55. 6 11. 6 10. 4 51. 4 40. 2 52. 7 46. 3 40. 5 MACP MAAT MAT 34. 0 14. 9 14. 1 13. 6 13. 3 11. 9 0 19 -25 26 -35 36 -45 46 -55 56 -65 66 -75 >75 Puyat JH, Can J Psychiatry, 2016
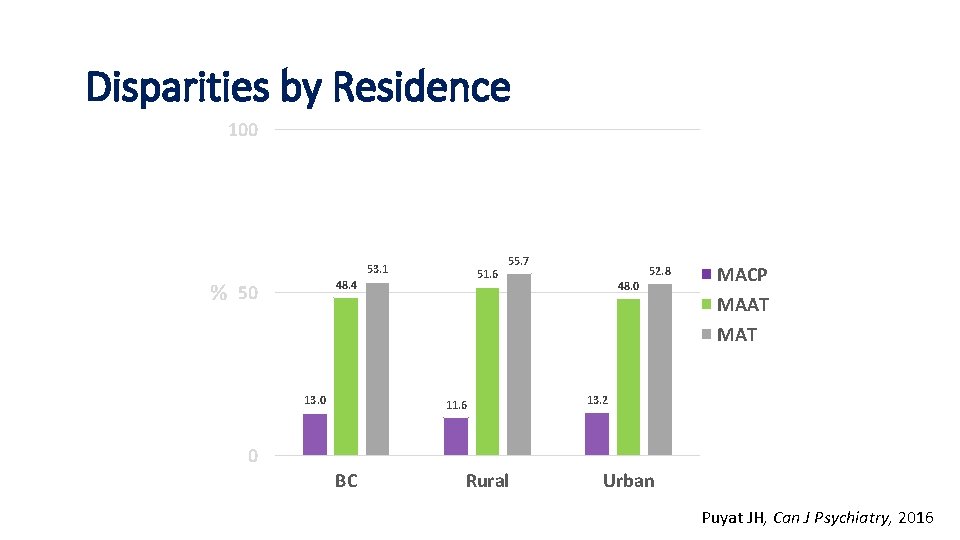
Location andby. MAT Disparities Residence 100 53. 1 51. 6 48. 4 % 50 13. 0 55. 7 11. 6 52. 8 48. 0 MACP MAAT MAT 13. 2 0 BC Rural Urban Puyat JH, Can J Psychiatry, 2016

http: //evidencenetwork. ca/archives/4970 What the rest of Canada can learn from BC “Provinces have been attempting ambitious and far-reaching reforms with new impetus over the last decade. Ontario, Quebec and Alberta have largely embraced structural reform, changing how services are delivered, creating community health clinics or family health teams with other allied health professionals like nurse practitioners, and putting doctors on salary or other payments models rather than traditional fee-for-service payments… British Columbia, has chosen a different route, opting to focus on operational reforms rather than structural reforms, through an active dialogue with physicians, patients, and other stakeholders to better align physician reimbursement with the provision of care to patients with complex health conditions and by supporting family doctors (also called General Practitioners or GPs) to feel better equipped both clinically and practically to do their job. ” BC Mental Health Initiatives (2008) 1) Mental Health Incentives • MH Planning Fee ($100/yr) • Increased billable counselling sessions from 4 to 8 per year ($53. 31 – $79. 97) • Up to 5 tel/email follow-up fees/18 months ($15) • Up to conferencing fees ($40/15 min) • CDM fee if patient has CPC ($120/year) 2) Training modules (diagnosing and managing mental disorders) • $2, 900 compensation • By 11/2012, 42% enrolled, 67 of whom completed the program.
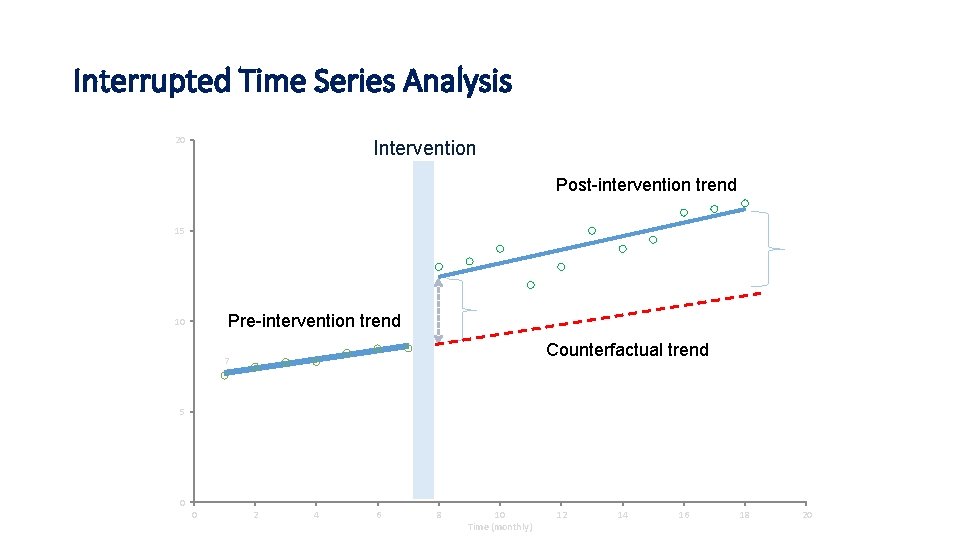
Interrupted Time Series Analysis 20 Intervention Post-intervention trend 15 Pre-intervention trend 10 Counterfactual trend 7 5 0 0 2 4 6 8 10 Time (monthly) 12 14 16 18 20
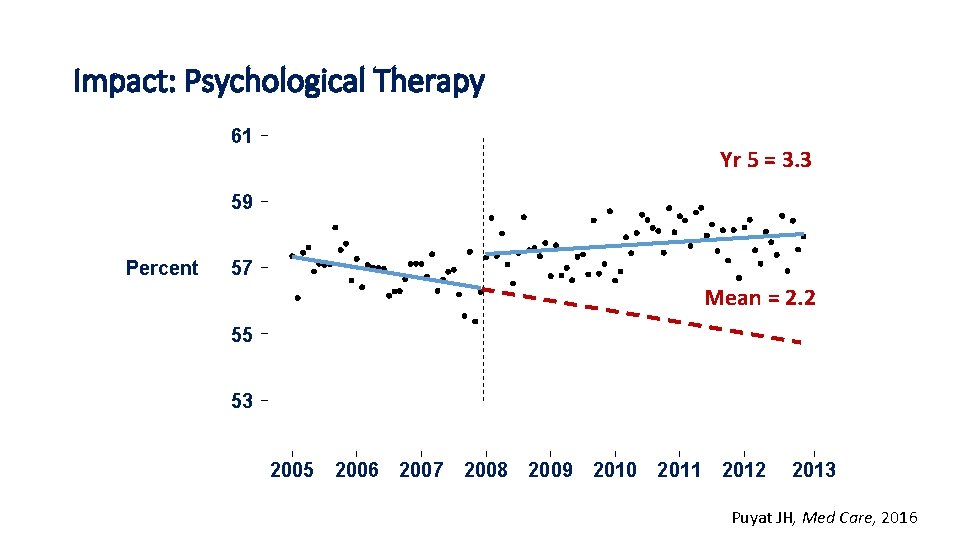
Impact: Psychological Therapy 61 Yr 5 = 3. 3 59 Percent 57 Mean = 2. 2 55 53 2005 2006 2007 2008 2009 2010 2011 2012 2013 Puyat JH, Med Care, 2016
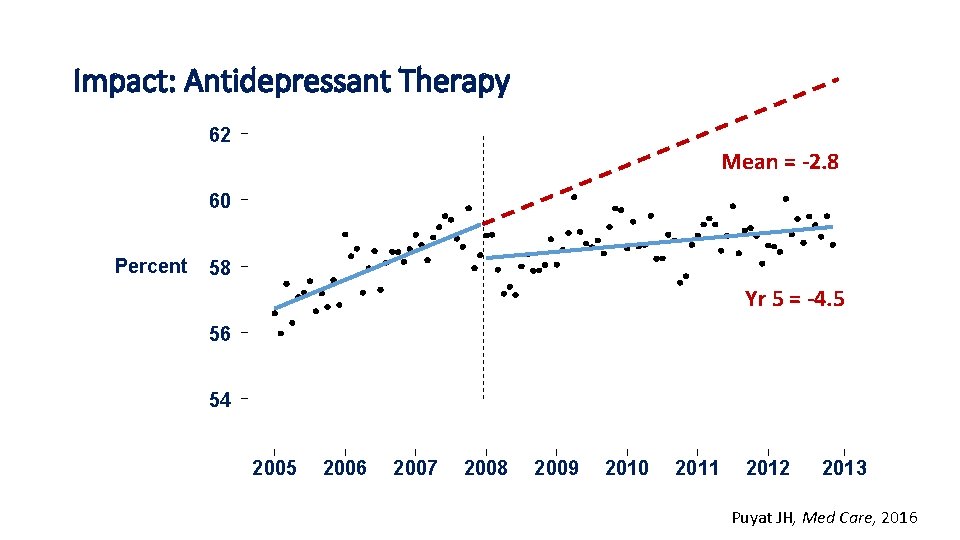
Impact: Antidepressant Therapy 62 Mean = -2. 8 60 Percent 58 Yr 5 = -4. 5 56 54 2005 2006 2007 2008 2009 2010 2011 2012 2013 Puyat JH, Med Care, 2016
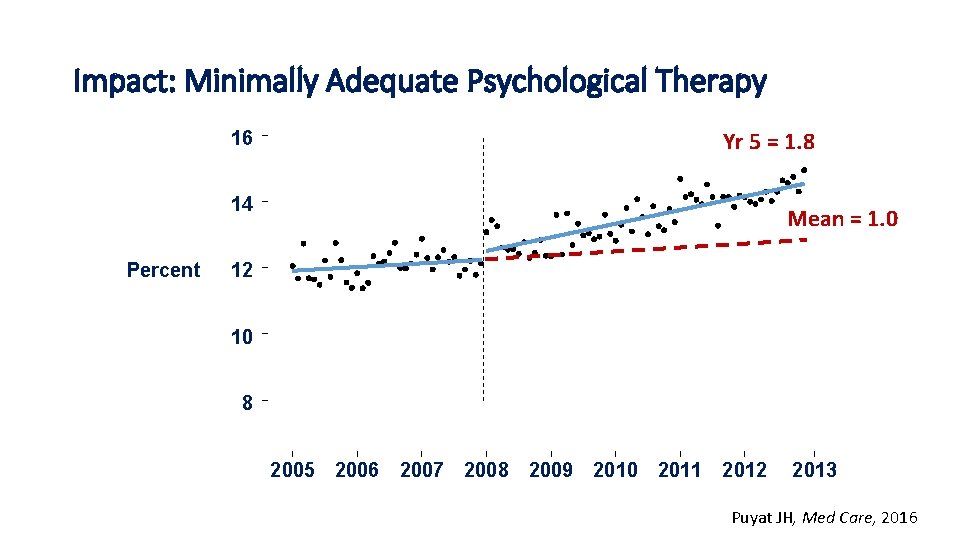
Impact: Minimally Adequate Psychological Therapy Yr 5 = 1. 8 16 14 Percent Mean = 1. 0 12 10 8 2005 2006 2007 2008 2009 2010 2011 2012 2013 Puyat JH, Med Care, 2016
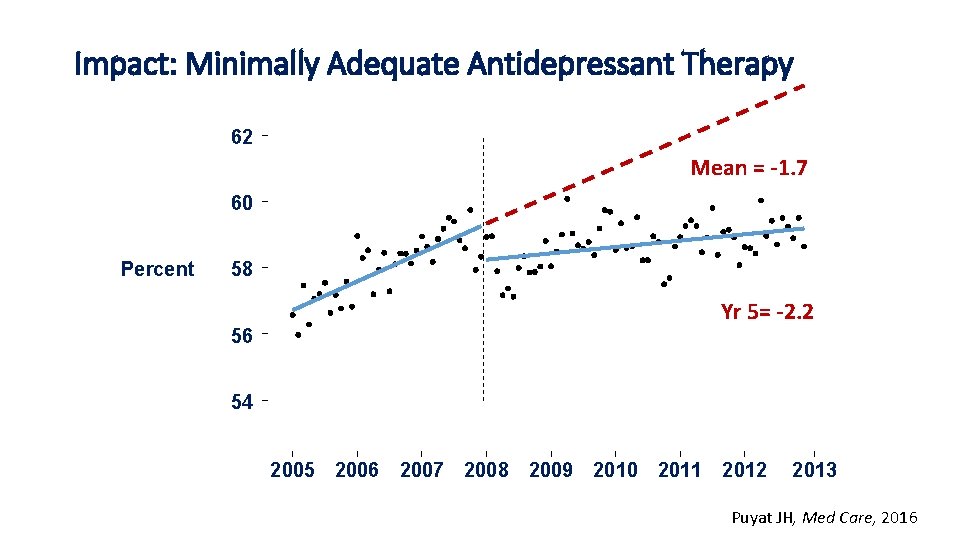
Impact: Minimally Adequate Antidepressant Therapy 62 Mean = -1. 7 60 Percent 58 Yr 5= -2. 2 56 54 2005 2006 2007 2008 2009 2010 2011 2012 2013 Puyat JH, Med Care, 2016
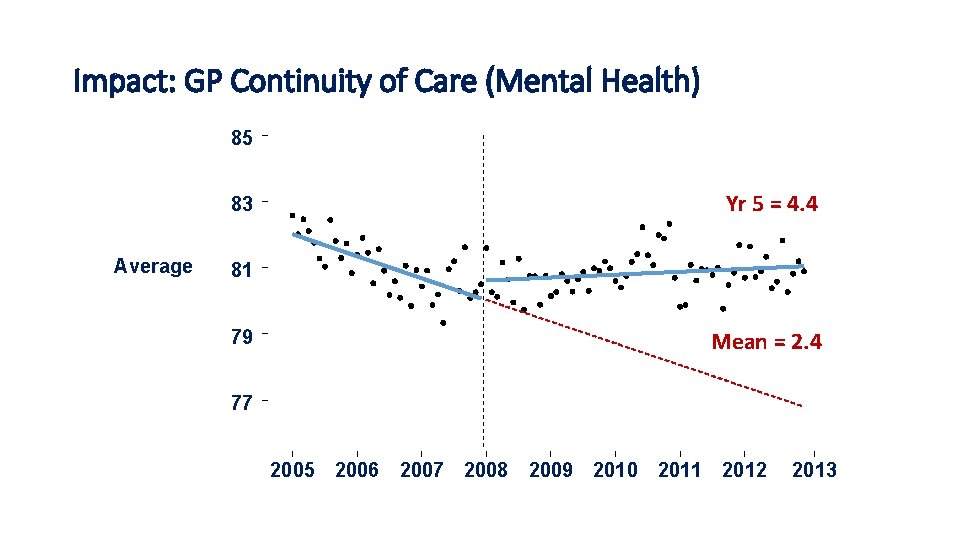
Impact: GP Continuity of Care (Mental Health) 85 Yr 5 = 4. 4 83 Average 81 79 Mean = 2. 4 77 2005 2006 2007 2008 2009 2010 2011 2012 2013

Summary • Reliable data are available and can be used to estimate gaps in treatment and examine the impact of policies • Gaps and disparities in depression care and treatment adequacy continue to persist • Physician incentives can influence depression care patterns, but the overall impact is modest

Implications • Improve mental health services to everyone in general • Examine how younger adults and men access mental health care • Accelerate efforts to promote team-based approaches to mental health service delivery and not rely mainly on operational reforms • Expand public coverage for psychological therapies

Thank You! References 1. Puyat JH, Kazanjian A, Wong H, Goldner EM. Is the Road to Mental Health Paved With Good Incentives? Estimating the Population Impact of Physician Incentives on Mental Health Care Using Linked Administrative Data. Medical Care. 2016 Sep 14; 2. Puyat JH, Kazanjian A, Goldner EM, Wong H. How Often Do Individuals with Major Depression Receive Minimally Adequate Treatment? A Population-Based, Data Linkage Study. Canadian Journal of Psychiatry. 2016 Jul 1; 61(7): 394– 404.
- Slides: 26