US HEPATOBILIARY SYSTEM TECHNIQUE AND US IN HEPATOBILIARY

US HEPATOBILIARY SYSTEM TECHNIQUE AND US IN HEPATOBILIARY DISEASE พญ. เสาวลกษณ ชนมยน รงสแพทย โรงพยาบาลนาน

OUTLINE • Anatomy • US technique • Hepatobiliary tract disease( Liver, gallbladder and biliary tract )

ANATOMY
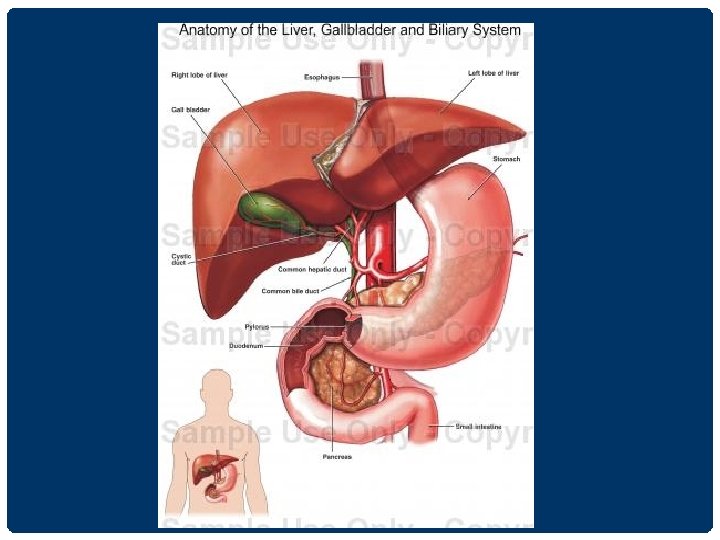
ทอทผาน เขา -ออก LIVER ม 4 ทอ ดงน. 1 Hepatic Vein 2. Portal Vein 3. Bile Duct 4. Hepatic Artery
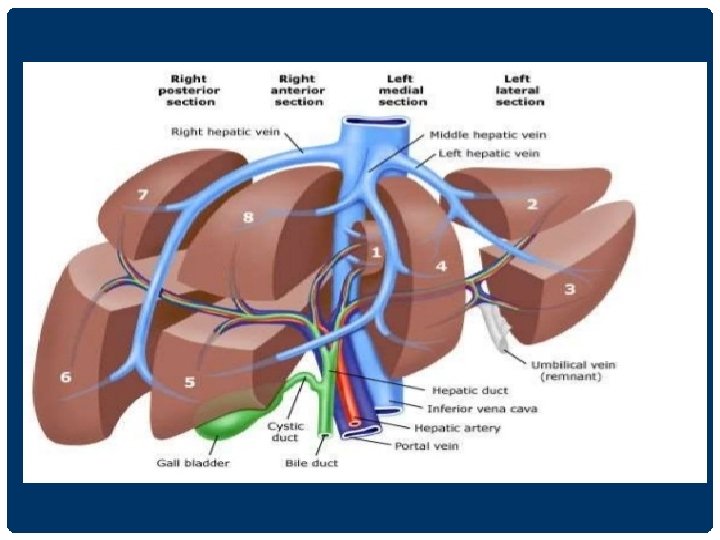
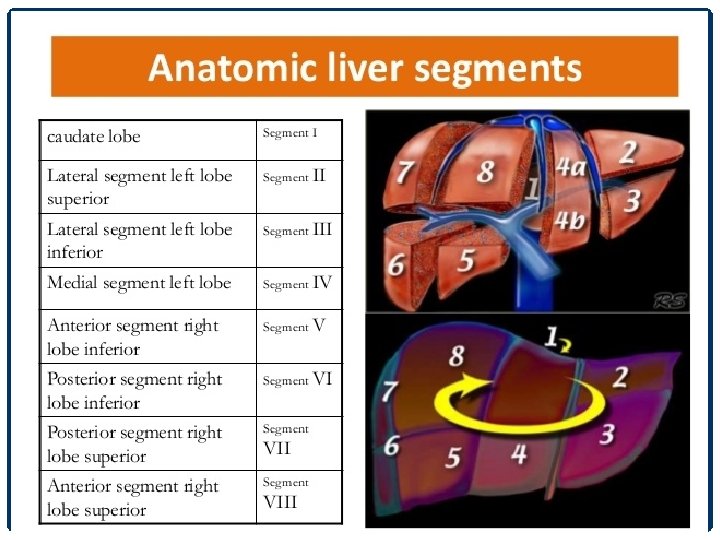

HEPATIC SEGMENTAL LANDMARKS
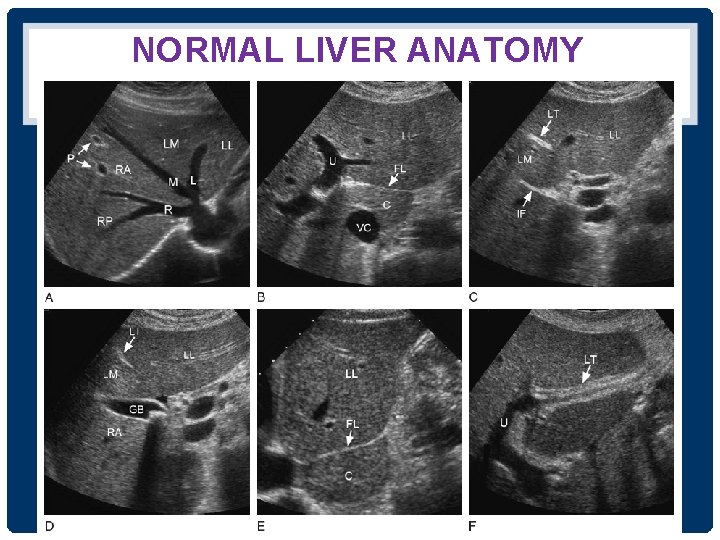
NORMAL LIVER ANATOMY
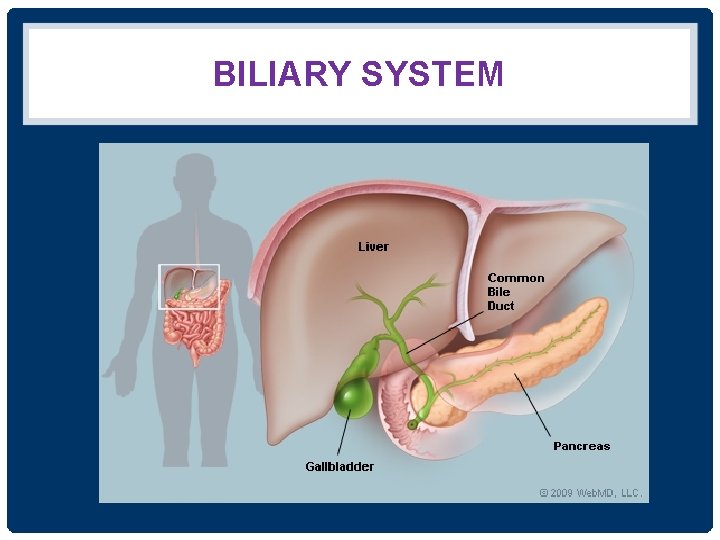
BILIARY SYSTEM

TECHNIQUE

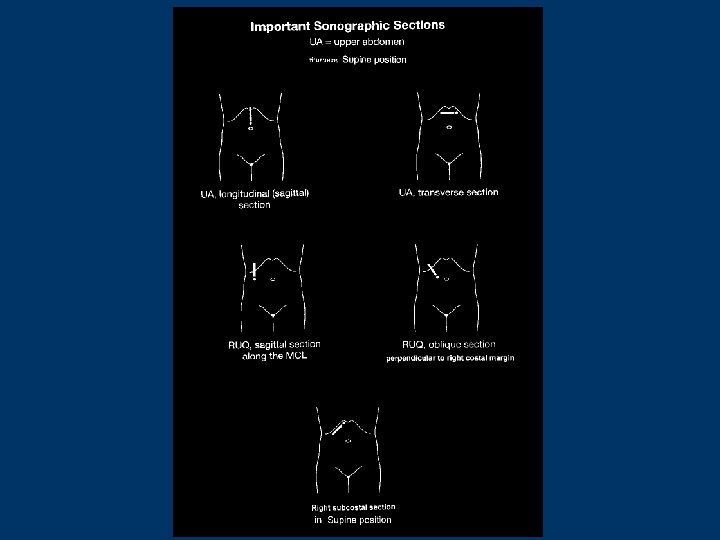
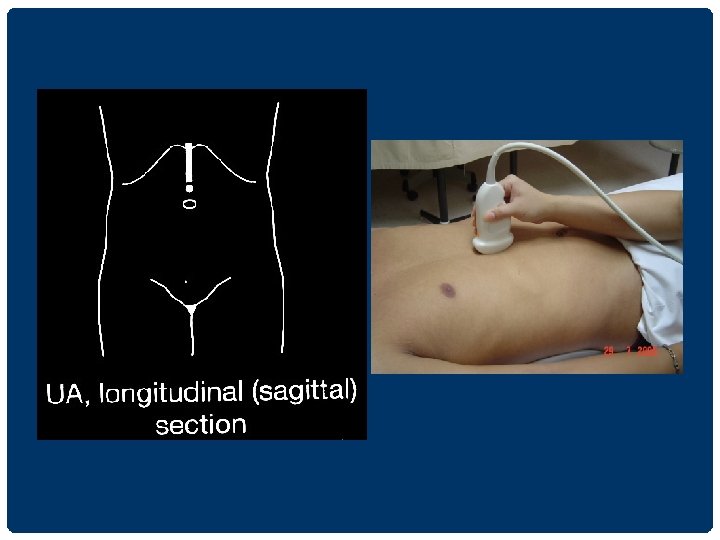
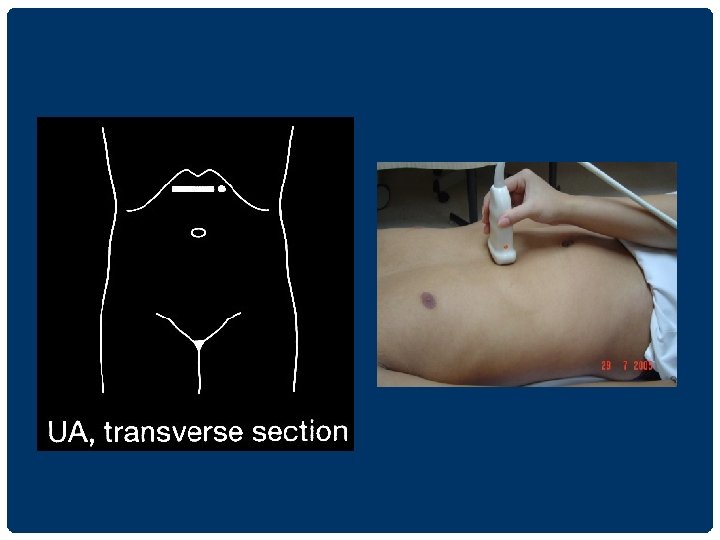
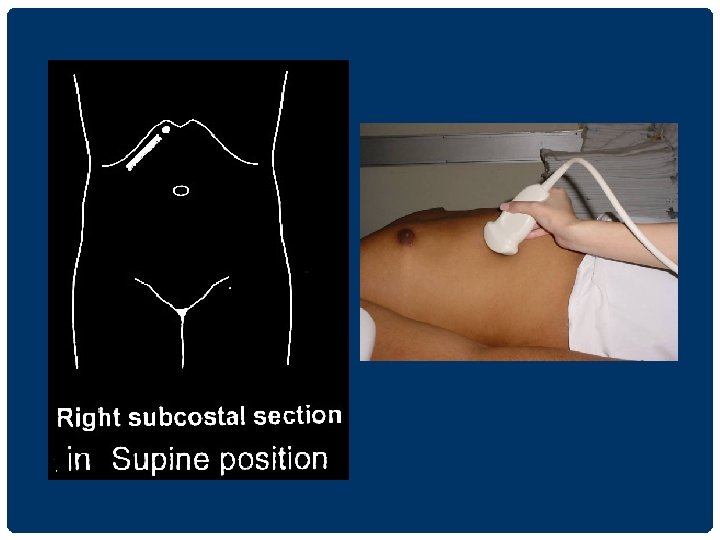
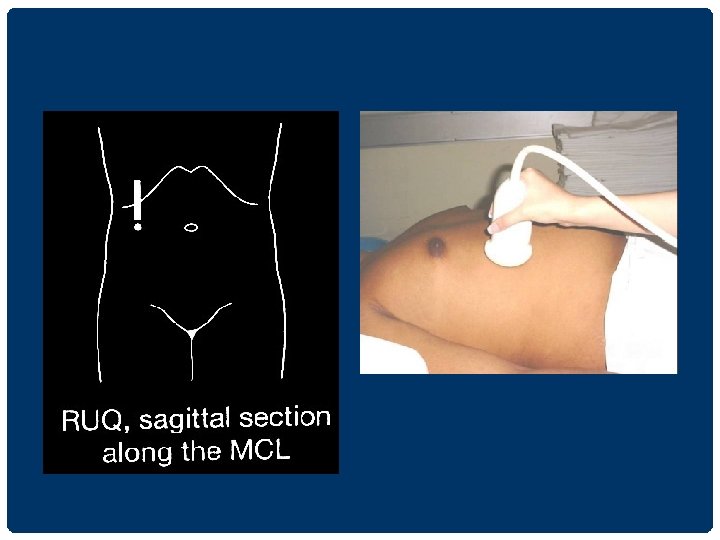
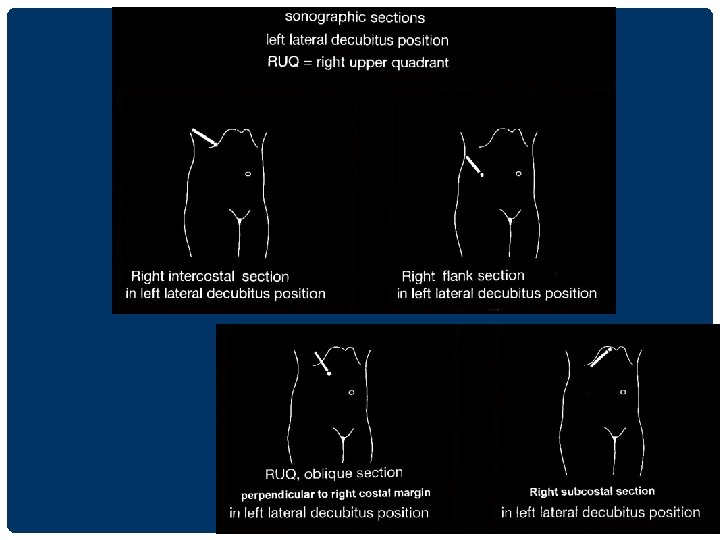
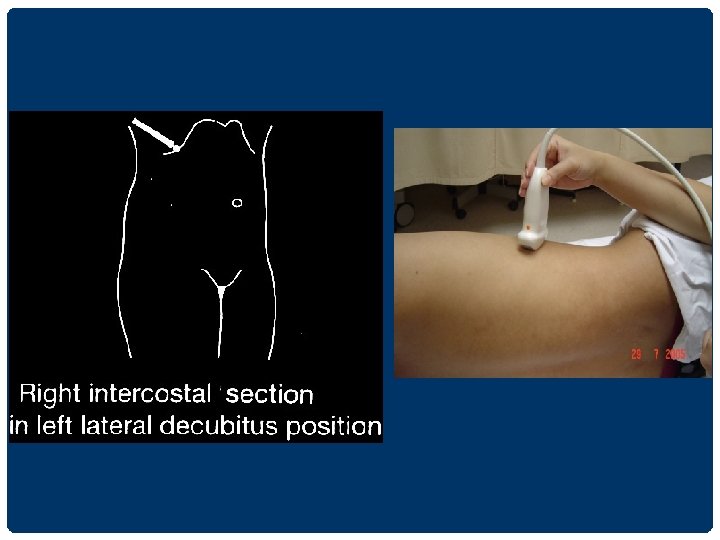
UPPER ABDOMINAL ULTRASONOGRAPHY 1. supine position นอนหงาย 2. left lateral decubitus position นอนตะแคง เอาดานซายลง 3. right lateral decubitus position นอนตะแคง เอาดานขวาลง
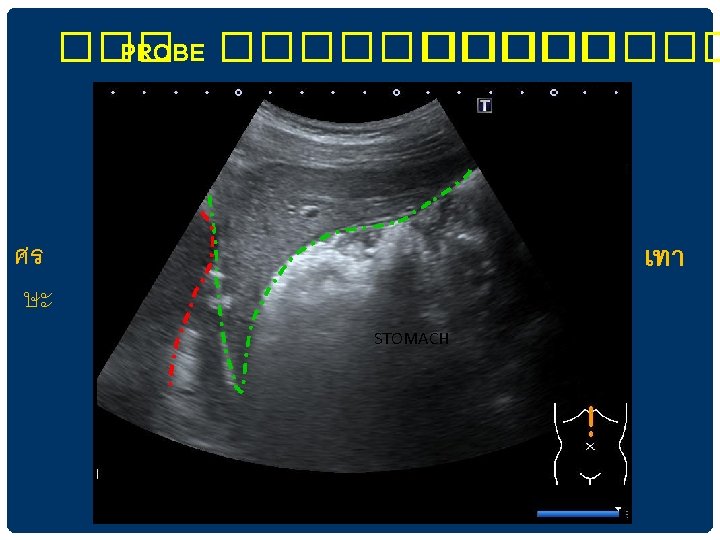
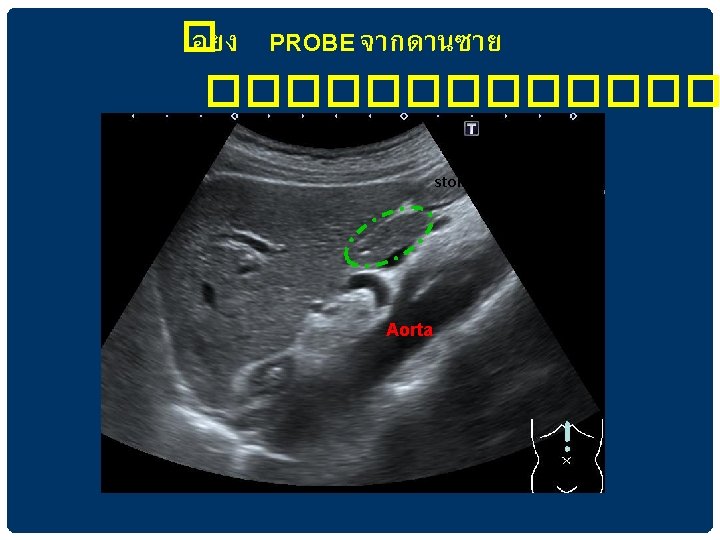
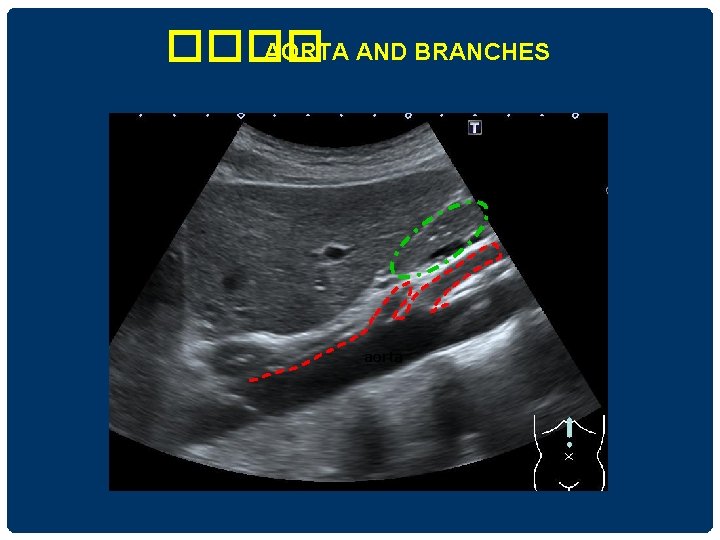
���� AORTA AND BRANCHES aorta
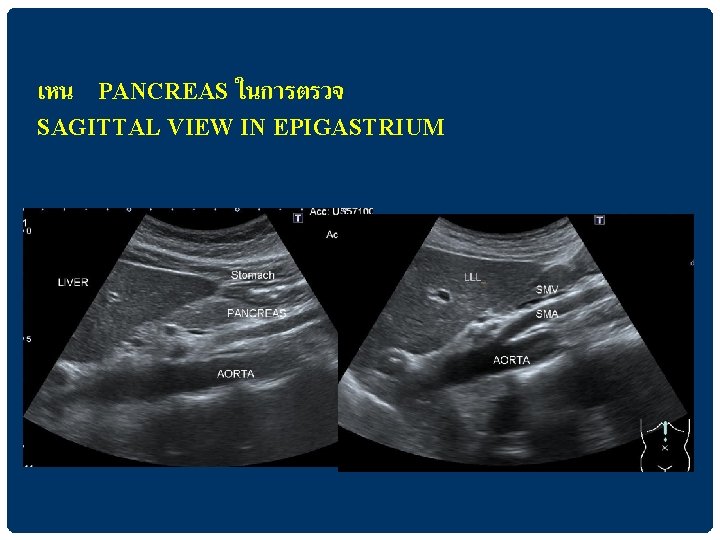
เหน PANCREAS ในการตรวจ SAGITTAL VIEW IN EPIGASTRIUM
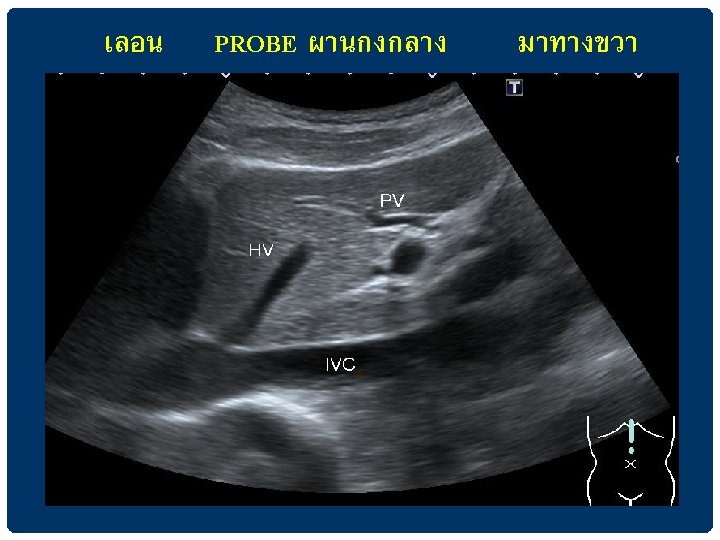
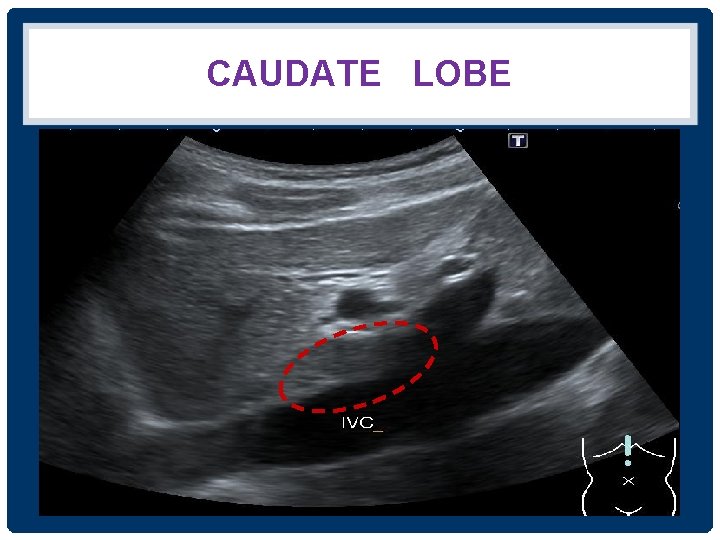
CAUDATE LOBE IVC
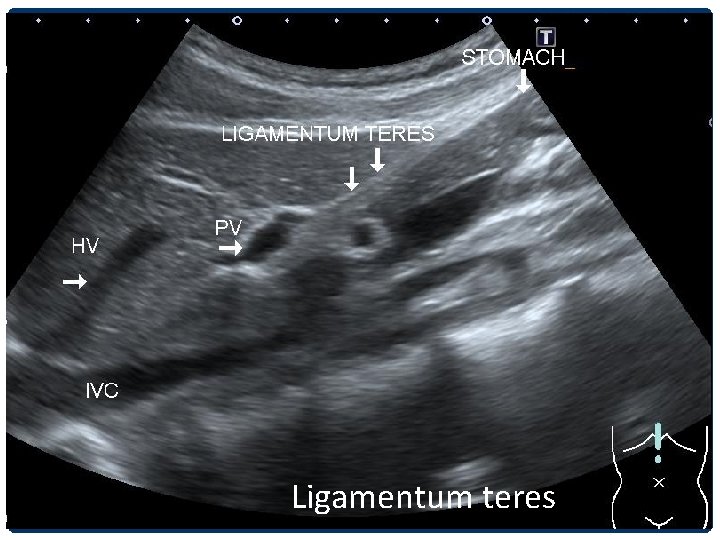
Ligamentum teres
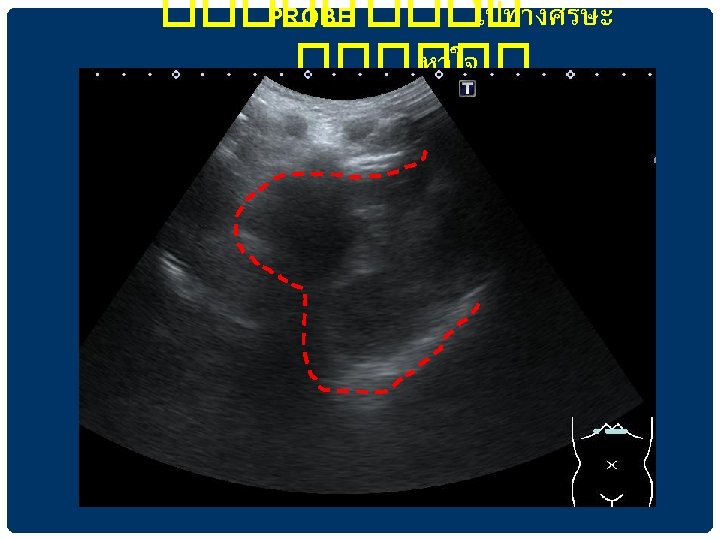
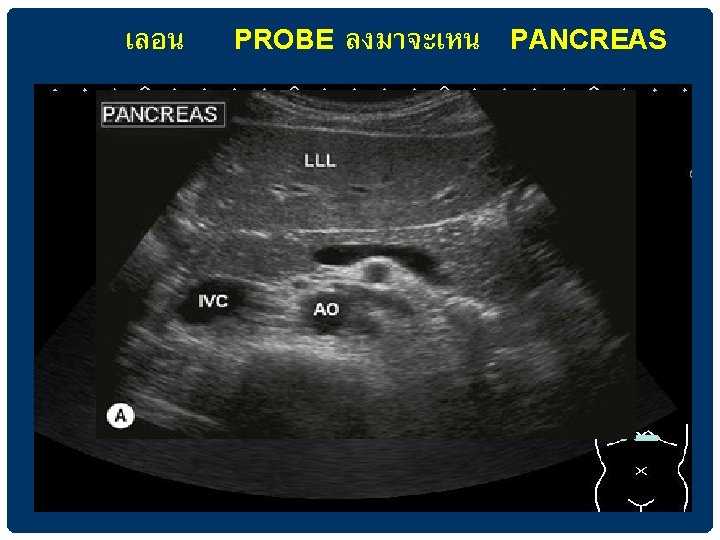
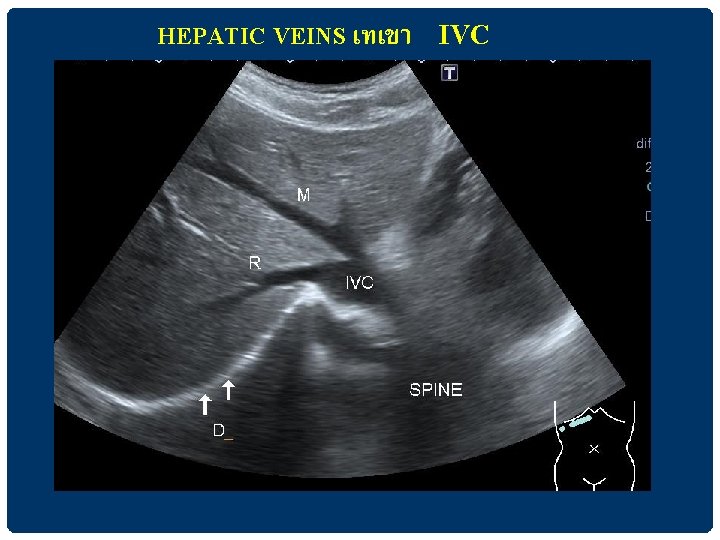
HEPATIC VEINS เทเขา IVC
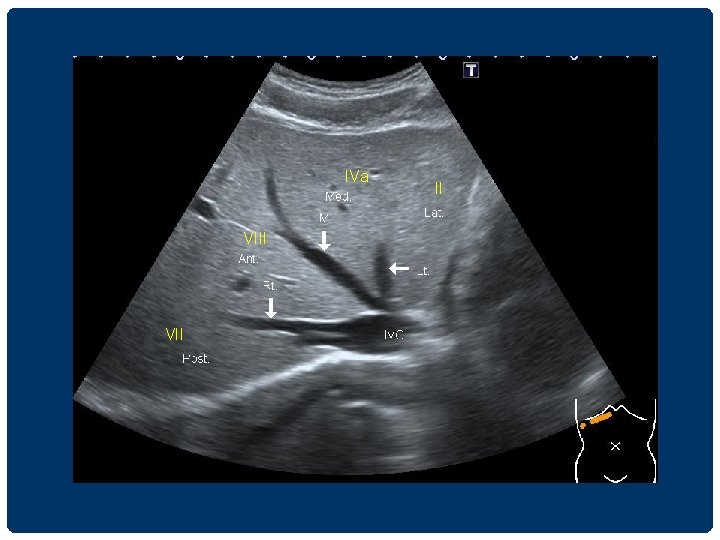
IVa VIII VII II
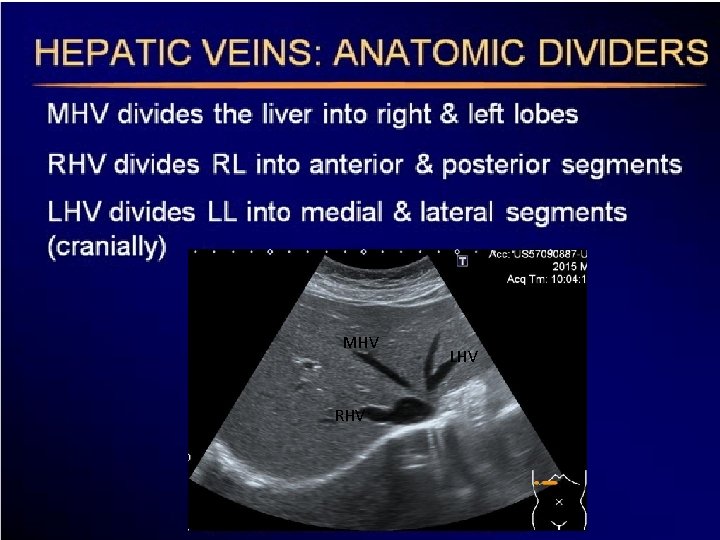
MHV RHV LHV
PORTAL VEIN • Periportal fibrofatty tissue produces brighter echoes around the portal veins • Normal size ไมควรเกน 13 mm ถามากกวานใหสงสยวามภาวะ portal hypertension
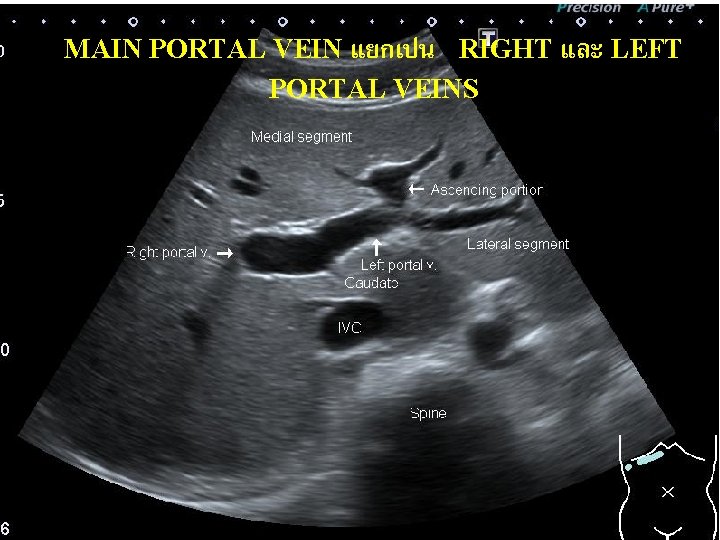
MAIN PORTAL VEIN แยกเปน RIGHT และ LEFT PORTAL VEINS
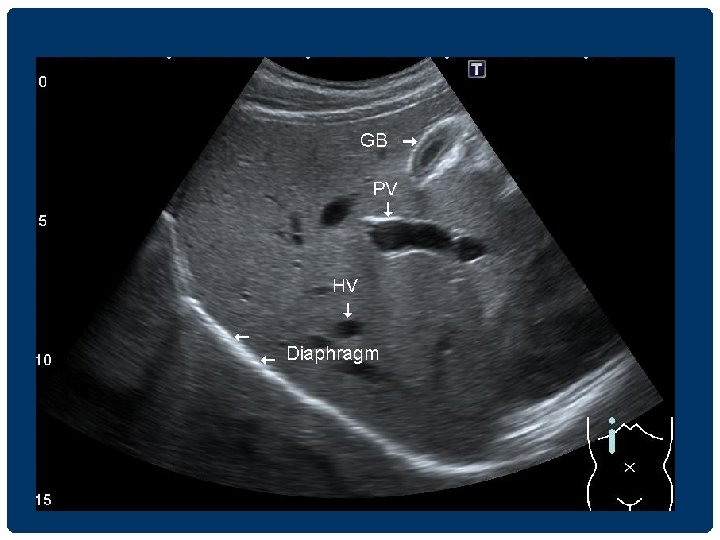
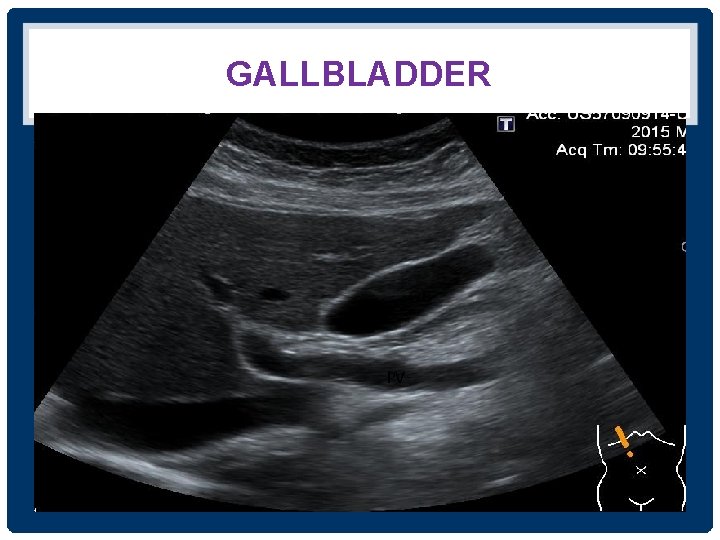
GALLBLADDER GB PV
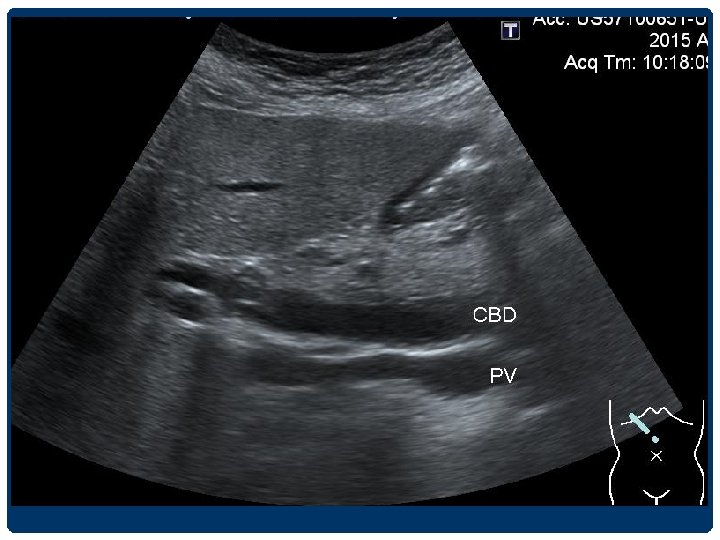
DILATED CBD
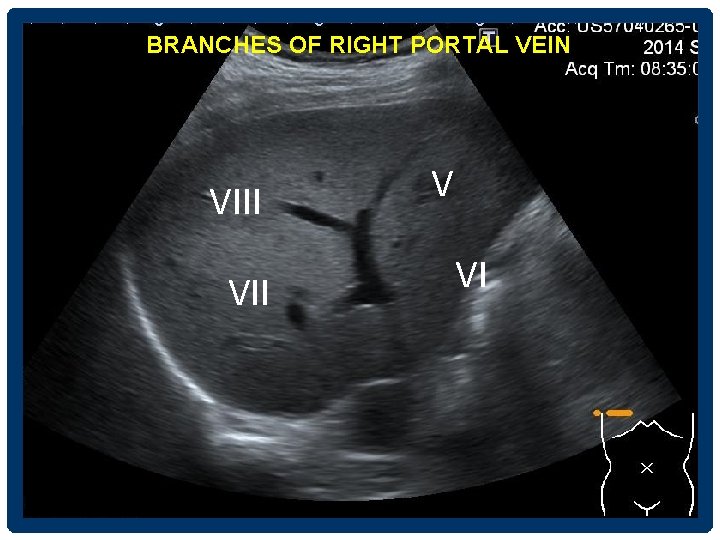
BRANCHES OF RIGHT PORTAL VEIN VIII V VI
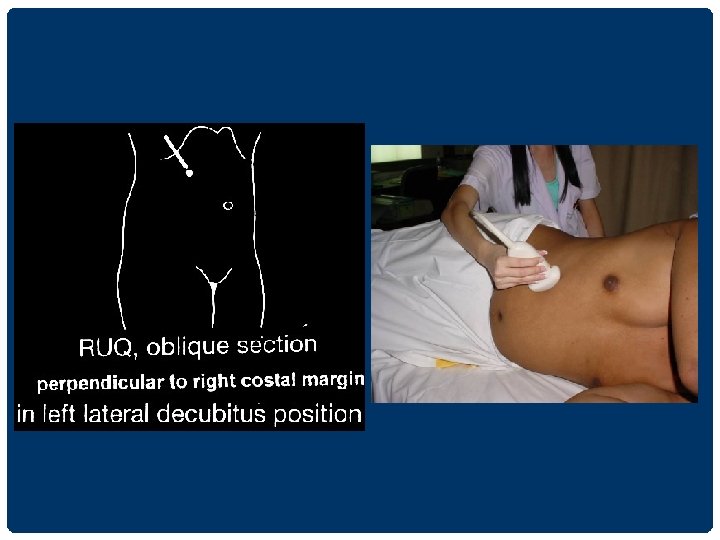

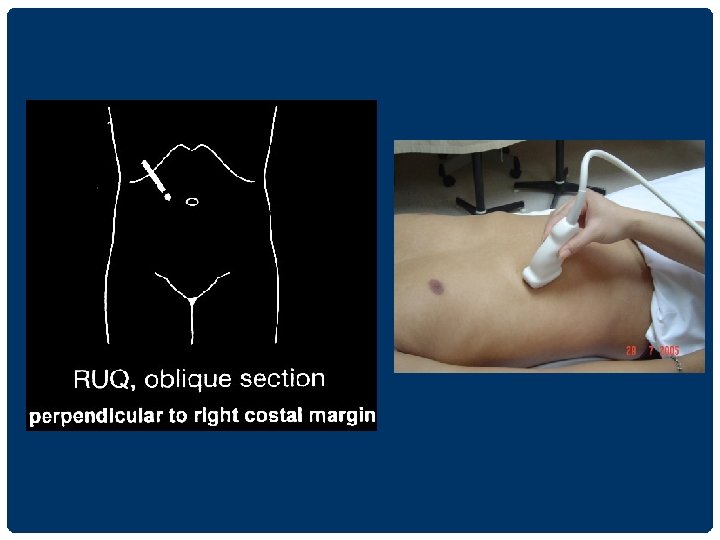
RIGHT SUBCOSTAL SECTION IN LEFT LATERAL DECUBITUS POSITION ��������� lesion ����������
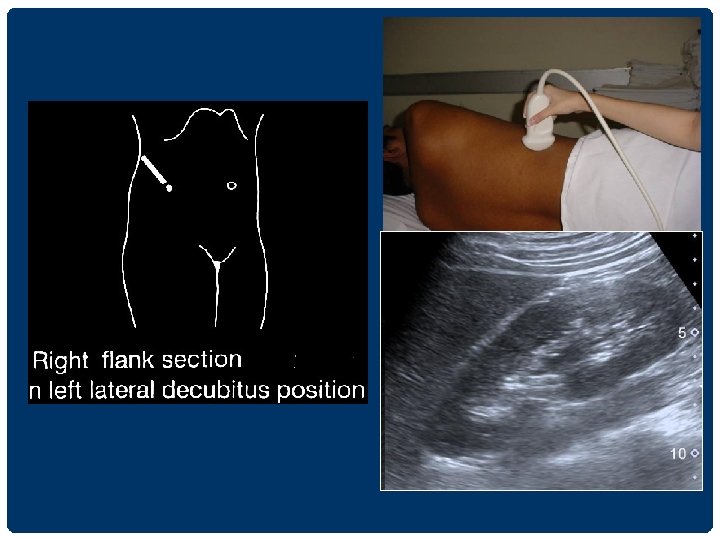
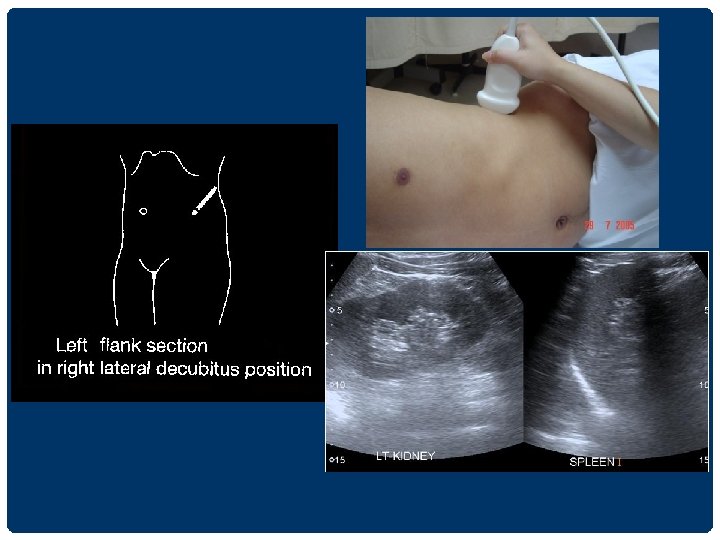

THE LIVER
LIVER Size - Right MCL วด craniocaudal direction ขนาดนอยกวา 15 cm - Indirect signs of hepatomegaly extension of the right lobe below the lower pole of the kidney rounding of the inferior tip of the liver extension of the left lobe into the LUQ above the spleen

LIVER ABNORMALITY Parenchymal disease -Fatty liver -Liver cirrhosis -Periductal fibrosis Liver mass /Focal lesion
LIVER PARENCHYMA - Homogeneous echogenicity โดยท echogenicity of the liver ≥ renal cortex, < renal capsule < spleen, < pancreas - Smooth surface - Visible tubular structuresare hepatic veins and portal veins - Hepatic veins ; thin wall IVC - Portal vein ; thick wall hepatic hilum - Bile duct parallel with portal vein seen at porta hepatis

DIFFUSE HEPATIC INHOMOGENEITY • COMMON -cirrhosis -metastasis -fatty infiltration • UNCOMMON -hepatocellular cancer -hepatic fibrosis -lymphoma

FATTY INFILTRATION • Intracellular deposition of triglycerides within hepatocytes • Causes – Alcoholic , Steroid , DM, Drug • NASH ( Nonalcoholic Steatohepatitis ) = Severe fatty liver with hepatomegaly with inflammation and fibrosis • Findings - Increased echogenicity of the liver, finer echotexture than normal liver • เทยบกบ kidney and pancreas

FATTY INFILTRATION • Sensitivity 60 -94 % Specificity 66 -95 % • Diffuse - Grading -mild = mildly increasing echogenicity -moderate = blurring of veins margins -severe = significant of posterior shadowing • Focal fatty infiltration
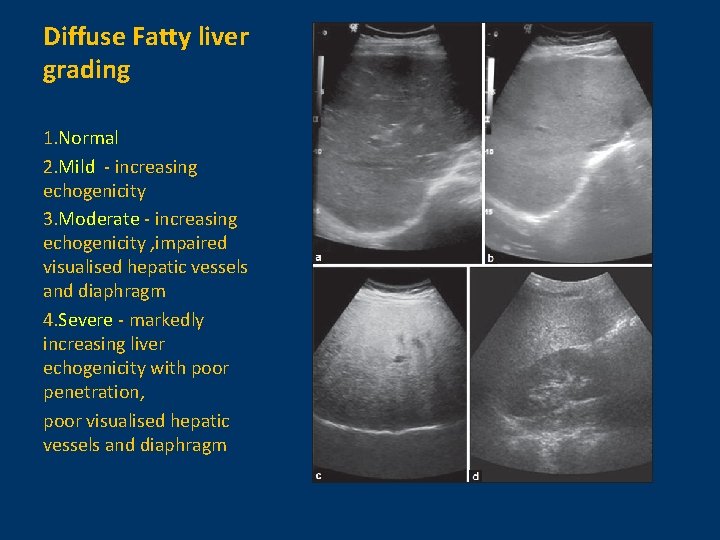
Diffuse Fatty liver grading 1. Normal 2. Mild - increasing echogenicity 3. Moderate - increasing echogenicity , impaired visualised hepatic vessels and diaphragm 4. Severe - markedly increasing liver echogenicity with poor penetration, poor visualised hepatic vessels and diaphragm

FOCAL FATTY SPARING FOCAL FATTY INFILTRATION Focal fatty sparing Focal fat infiltration • Diffuse fatty infiltration with FFS • Geographic hypoechoic area • Focal or nodular • Anterior aspect of LL (esp. medial segment), adjacent to the falciform ligament, anterior to the PV bifurcation • Atypical locations metastases or hemangioma • Usually located in front of the RPV or PV bifurcation or around the gallbladder • Lack of mass effect on hepatic vessels
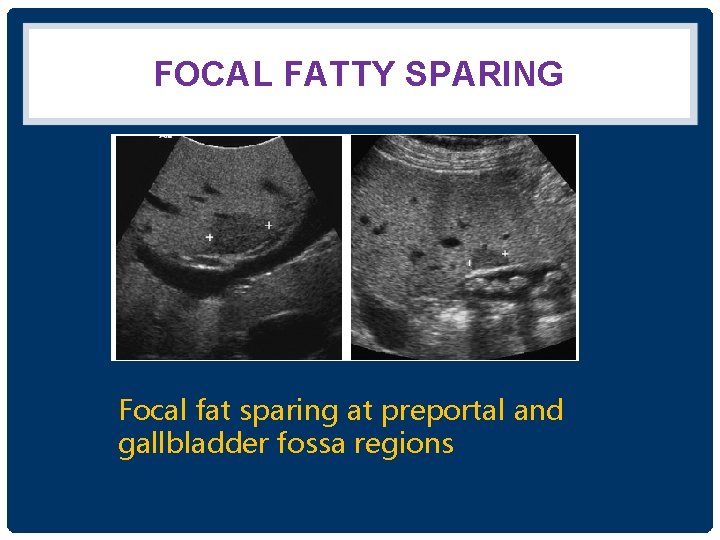
FOCAL FATTY SPARING Focal fat sparing at preportal and gallbladder fossa regions
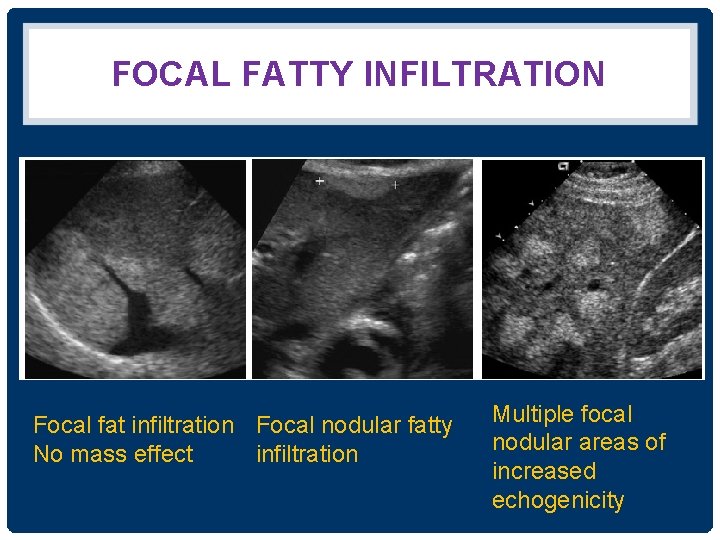
FOCAL FATTY INFILTRATION Focal fat infiltration Focal nodular fatty No mass effect infiltration Multiple focal nodular areas of increased echogenicity

CIRRHOSIS • US appearance • Surface nodularity reliable sign • Coarsening and nodularity of the liver parenchyma(RN/DN) • Segmental hypertrophy/atrophy • Hypertrophy of the caudate lobe and lateral segments of left lobe (S 2&3) • Atrophy of the posterior segments (S 6&7) of the right lobe • RL: LL(longitudinal ratio) < 1. 3 (normal =1. 44) • Signs of portal hypertension

SONOGRAPHIC SIGNS OF PORTAL HYPERTENSION • • • Ascitis Splenomegaly Portal vein enlargement >13 mm Portosystemic collateral Enlarged hepatic arteries Hepatofugal(reversed)portal flow
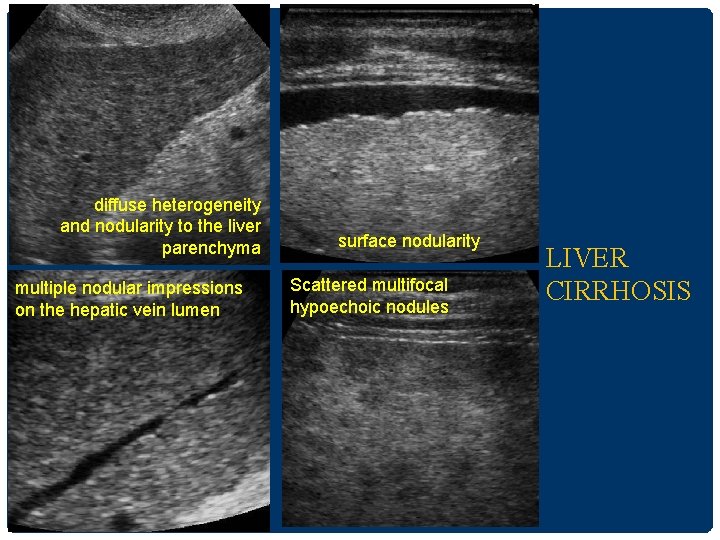
diffuse heterogeneity and nodularity to the liver parenchyma multiple nodular impressions on the hepatic vein lumen surface nodularity Scattered multifocal hypoechoic nodules LIVER CIRRHOSIS
LIVER ABNORMALITY Parenchymal disease -Fatty liver -Liver cirrhosis -Periductal fibrosis Liver mass /Focal lesion
ECHOGENICITY OF LIVER MASS /FOCAL LIVER LESION • Echogenic pattern - calcifications - anechogenic - hypoechogenic - isoechogenic - hyperechogenic - mixed echogenic • Outline - well defined / poor • Others - acoustic shadow - posterior enhancement - dilated bile duct
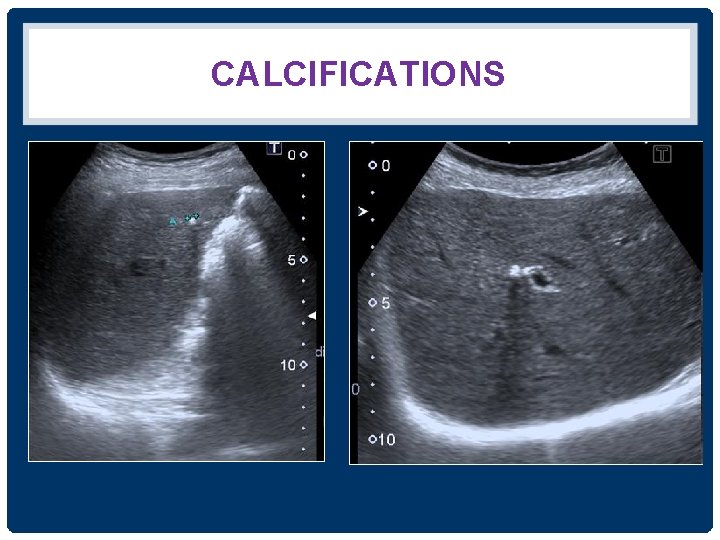
CALCIFICATIONS
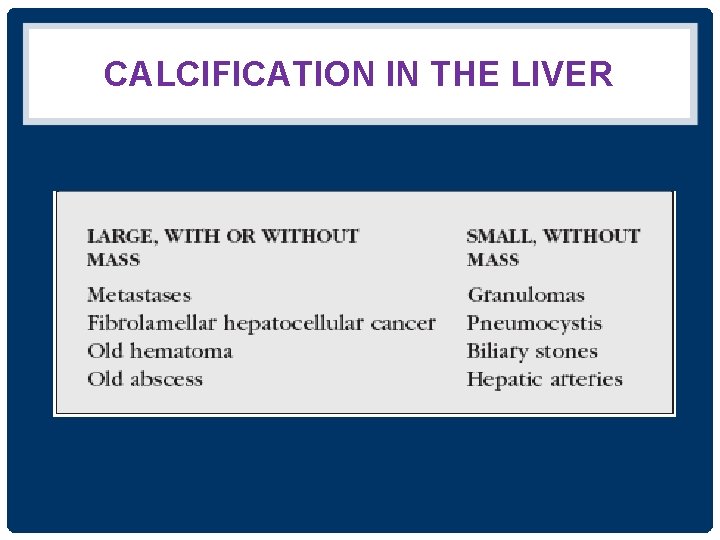
CALCIFICATION IN THE LIVER
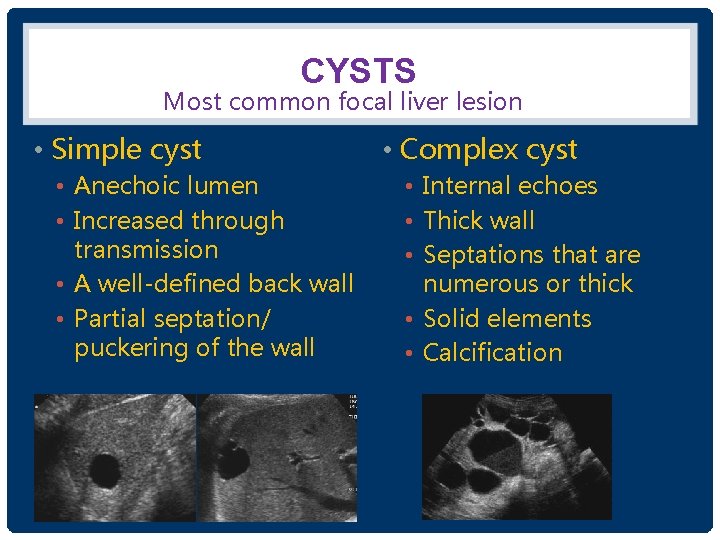
CYSTS Most common focal liver lesion • Simple cyst • Anechoic lumen • Increased through transmission • A well-defined back wall • Partial septation/ puckering of the wall • Complex cyst • Internal echoes • Thick wall • Septations that are numerous or thick • Solid elements • Calcification
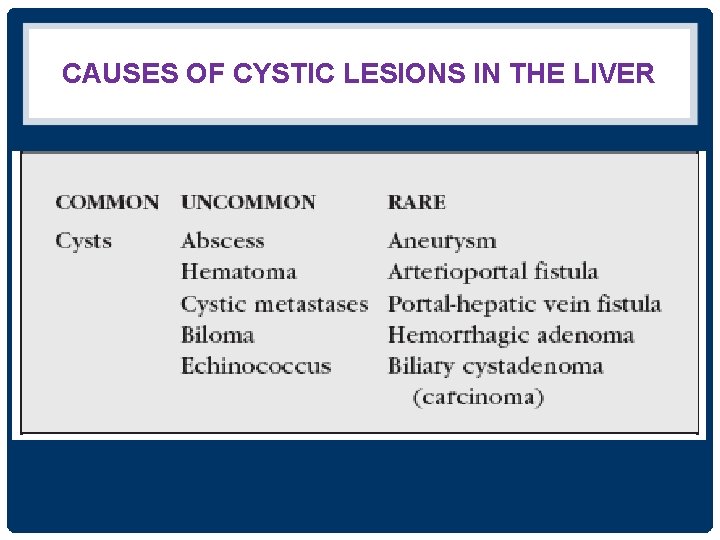
CAUSES OF CYSTIC LESIONS IN THE LIVER
LIVER ABSCESS • Complex fluid collections with a mixed echogenicity • May mimic solid hepatic masses • Thick-walled cystic lesions or cysts with fluid-fluid levels • Gas forming abscess • DDx: hematoma, hemorrhagic cyst, necrotic or hemorrhagic tumor
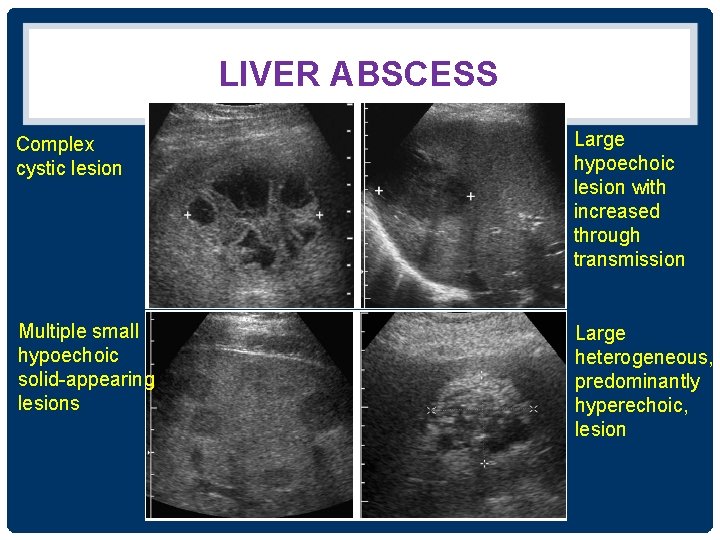
LIVER ABSCESS Complex cystic lesion Large hypoechoic lesion with increased through transmission Multiple small hypoechoic solid-appearing lesions Large heterogeneous, predominantly hyperechoic, lesion

HEMANGIOMA • Approximately 7% of adult, F>M, 10% are multiple Typical appearance (60 -70%) homogeneous round/lobulated hyperechoic mass usually less than 3 cm sharp&smooth margins calcification มได แต rare • Atypical hemangiomas • Hyperechoic periphery and a hypoechoic center “reverse target” appearance
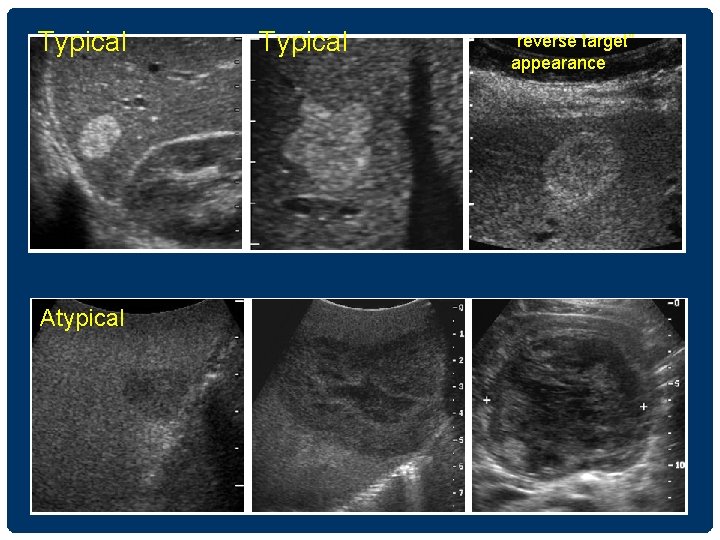
Typical Atypical Typical “reverse target” appearance

HEMANGIOMA • • Usually stable over time ~ 10% decrease in echogenicity ~ 5% regress partially or completely ~ 2% enlarge

DDX HYPERECHOIC MASSES • • Hemangioma Metastasis Hepatocellular cancer Focal fatty infiltration

HEPATOCELLULAR CARCINOMA • Strongly associated with chronic liver disease hepatitis B&C and cirrhosis • Growth pattern of HCC solitary, multifocal or diffuse and infiltrating • Typical a large dominant lesion with scattered smaller satellite lesions • Sonographic appearance non-specific • Venous invasion 30 -60% for the portal veins and 15% for the hepatic veins
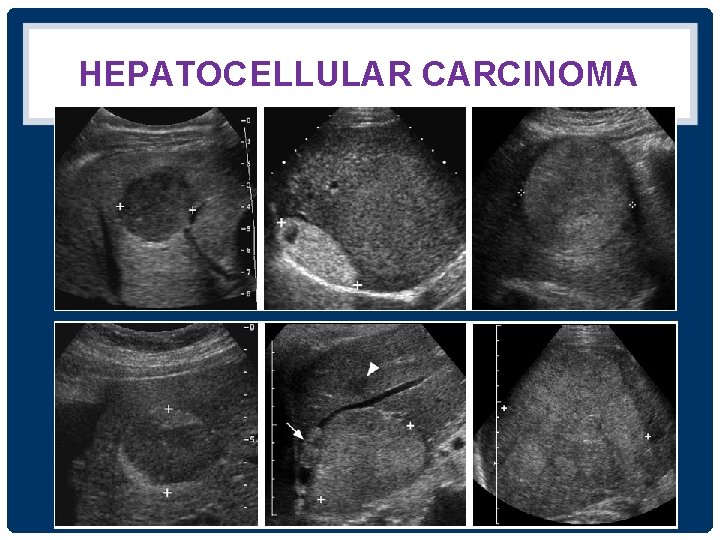
HEPATOCELLULAR CARCINOMA
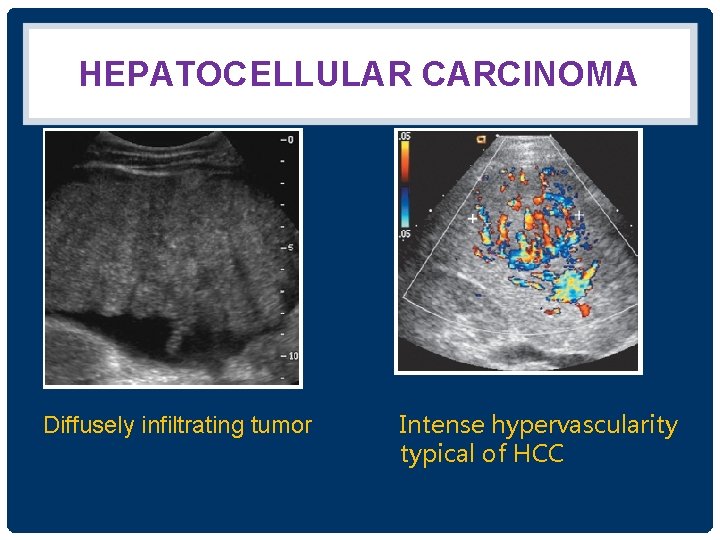
HEPATOCELLULAR CARCINOMA Diffusely infiltrating tumor Intense hypervascularity typical of HCC

METASTASES • 98% multiple • Usually involve both lobes of the liver • Variety of sonographic appearance • สวนใหญจะเหนเปน “target appearance” echogenic/isoechoic center and a hypoechoic halo • Others: hypo/hyperechoic nodule, calcified metastases, cystic metastasis, diffuse heterogeneous
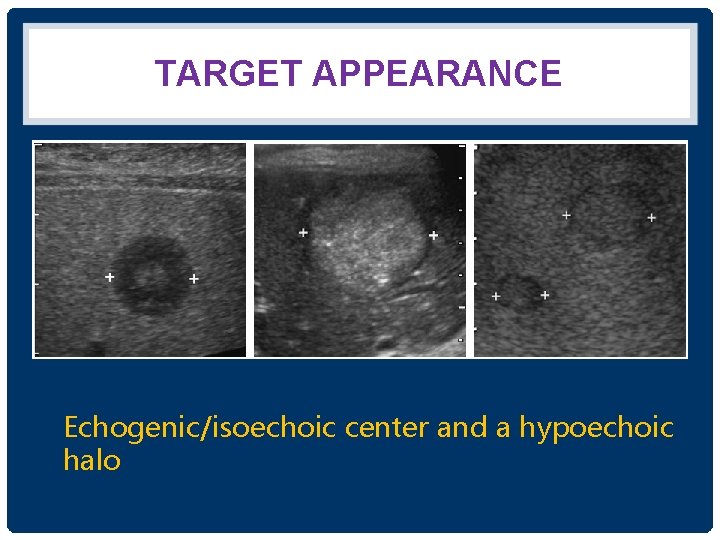
TARGET APPEARANCE Echogenic/isoechoic center and a hypoechoic halo

HEPATIC TARGET LESIONS
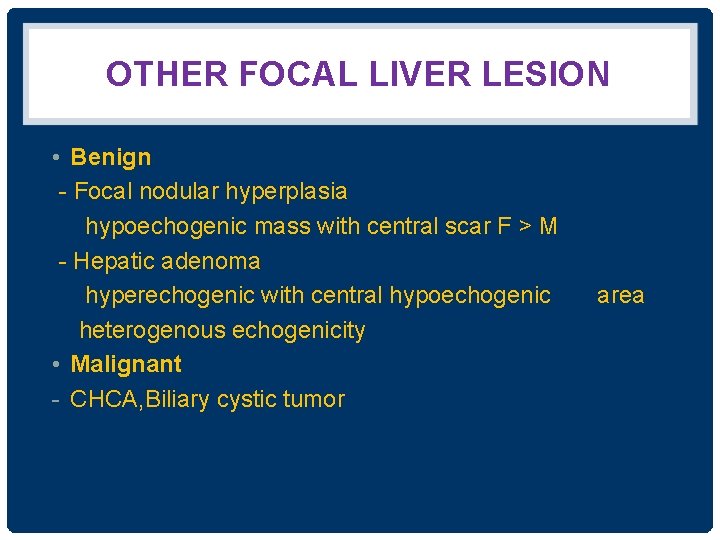
OTHER FOCAL LIVER LESION • Benign - Focal nodular hyperplasia hypoechogenic mass with central scar F > M - Hepatic adenoma hyperechogenic with central hypoechogenic heterogenous echogenicity • Malignant - CHCA, Biliary cystic tumor area

GALLBLADDER
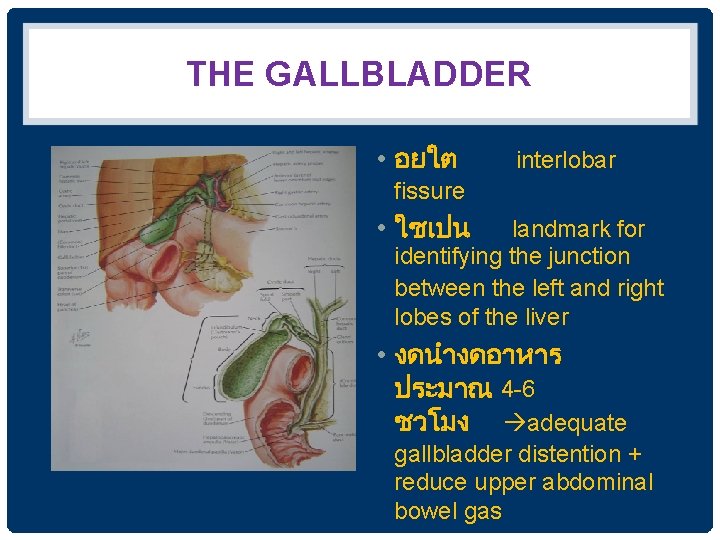
THE GALLBLADDER • อยใต interlobar fissure • ใชเปน landmark for identifying the junction between the left and right lobes of the liver • งดนำงดอาหาร ประมาณ 4 -6 ชวโมง adequate gallbladder distention + reduce upper abdominal bowel gas
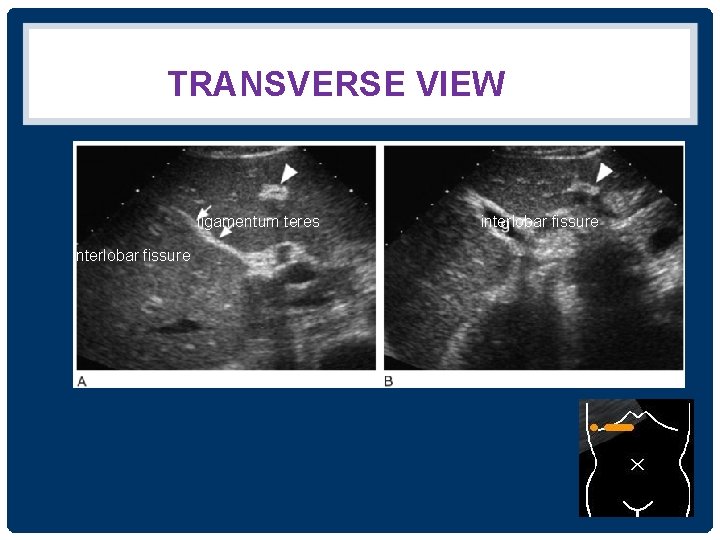
TRANSVERSE VIEW ligamentum teres interlobar fissure
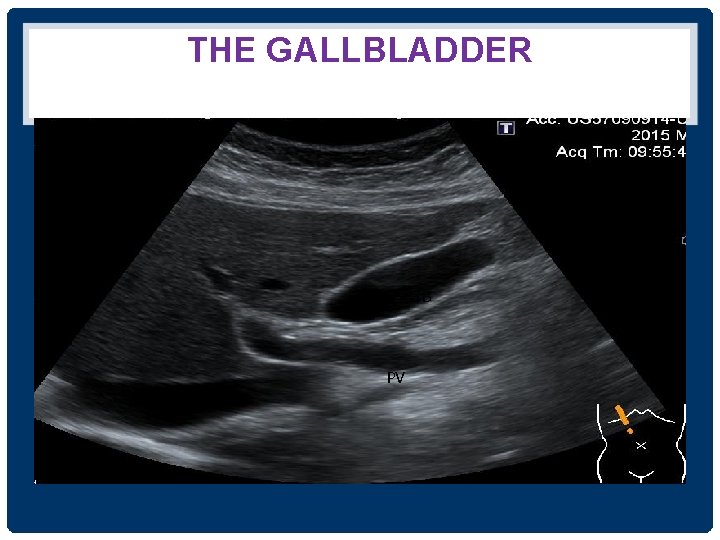
THE GALLBLADDER GB PV

CHARACTERISTICS OF THE NORMAL GALLBLADDER
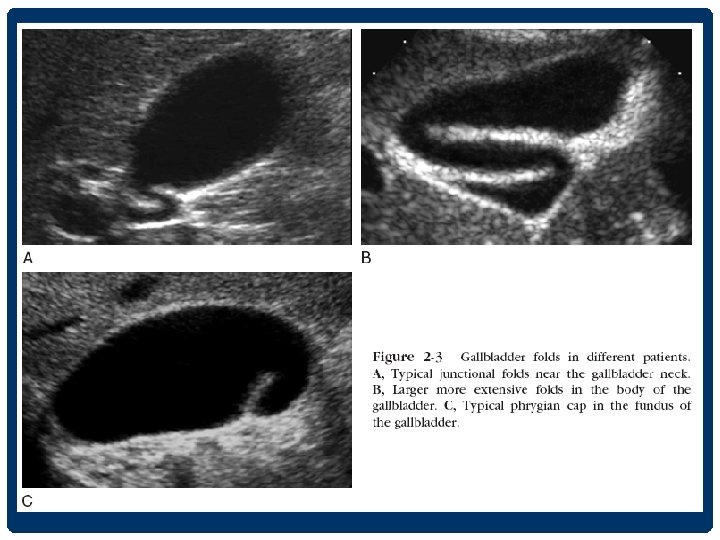

GALLBLADDER PATHOLOGY • stones • biliary sludge/ microlithiasis • polyp • contracted gallbladder • porcelain gallbladder • gallbladder wall thickening • acute cholecystitis • Chronic cholecystitis • Hyperplastic cholecystitis • carcinoma of gallbladder
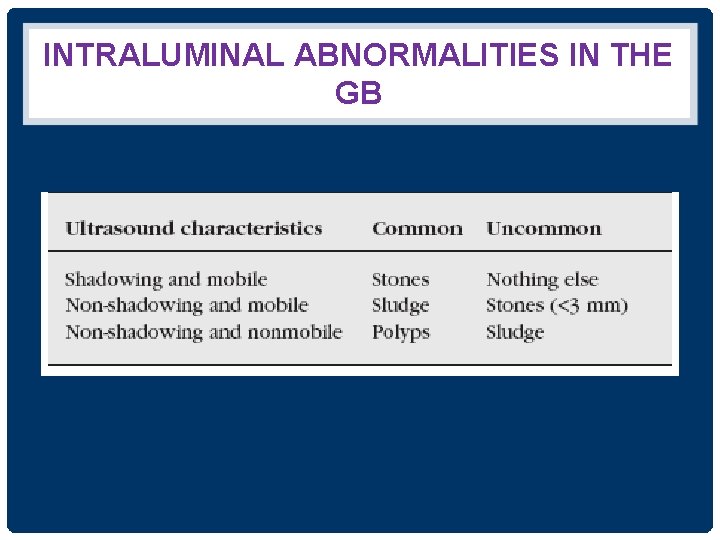

INTRALUMINAL ABNORMALITIES IN THE GB
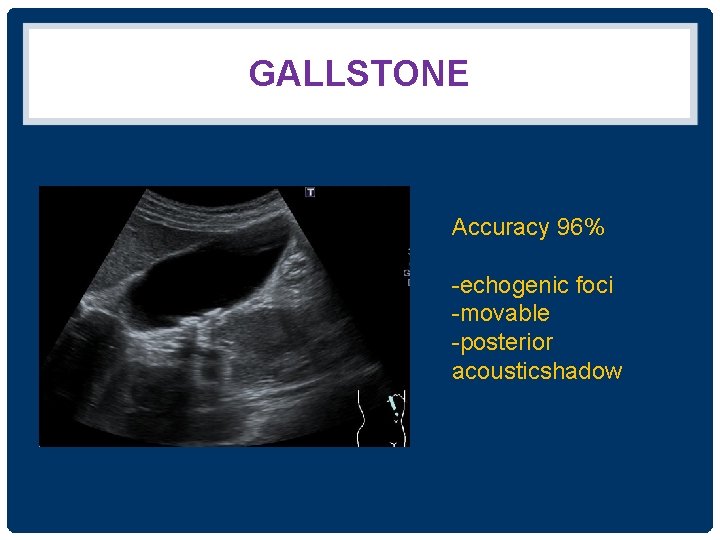
GALLSTONE Accuracy 96% -echogenic foci -movable -posterior acousticshadow
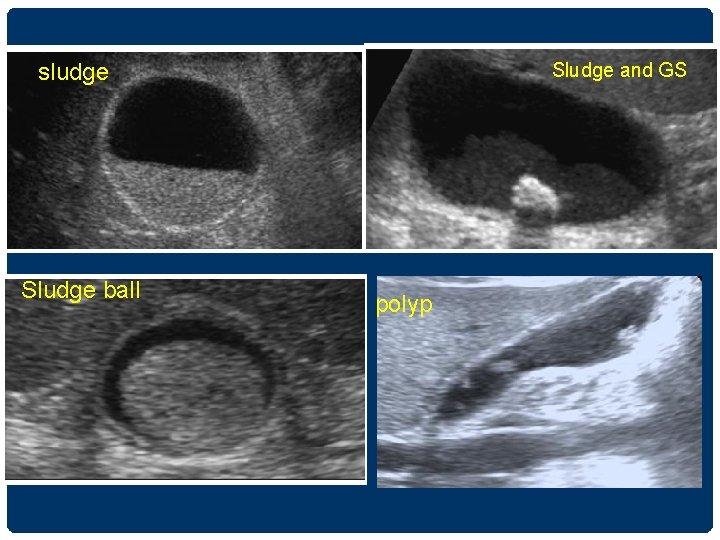
sludge Sludge ball Sludge and GS polyp
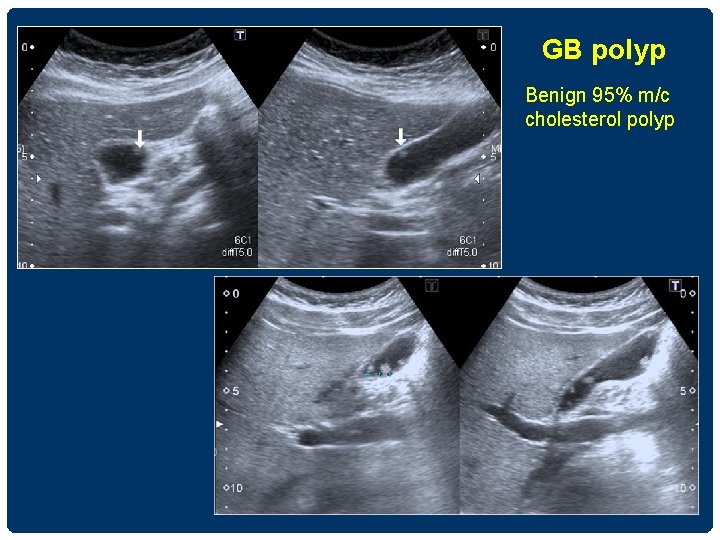
GB polyp Benign 95% m/c cholesterol polyp

GALLBLADDER POLYP Benign • size 5 mm-benign 5 -10 mm FU • pedunculated • m/c multiple • stable size Malignant • size >10 mm(3788%) • sessile • single • increasing in size

ACUTE CHOLECYSTITIS • GB wall thickening > 3 mm • GB enlargement • Pericholecystitic fluid • +/- Gall stone • US Murphy’s sign positive
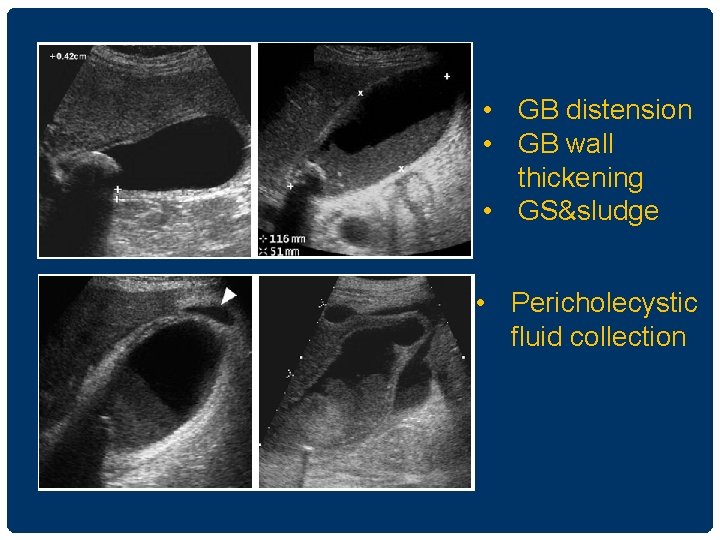
• GB distension • GB wall thickening • GS&sludge • Pericholecystic fluid collection

GB WALL THICKENING Biliary cause • Cholecystitis • Adenomyomatosis • Cancer • AID cholangiopathy • Sclerosing cholangitis Non biliary cause • Hepatitis • Pancreatitis • Heart failure • Cirrhosis • Hypoproteinemia • Lymphatic obstruction • Portal hypertension

OTHER GALLBLADDER DISEASE • Adenomyomatosis - Intramural diverticular diffuse or focal thickening GB wall • Carcinoma GB - Focal or diffuse thickenedwall - Polypoid maa - GB mass

BILIARY SYSTEM

THE BILE DUCT • Intrahepatic bile duct • จะวงขนานไปกบ portal veins & hepatic arteries • anterior to the adjacent portal veins • IHD สวนใหญจะตรวจไมพบใน US หรอถาพบกมกจะมขนาดไมเกน 2 mm

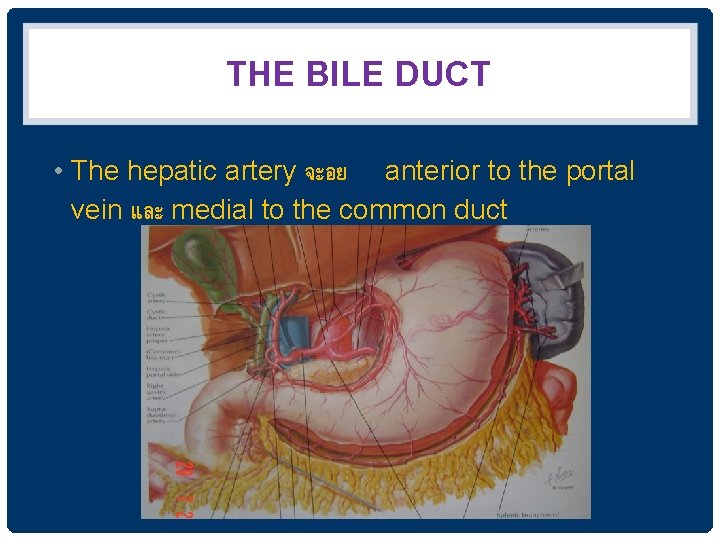
THE BILE DUCT • The hepatic artery จะอย anterior to the portal vein และ medial to the common duct
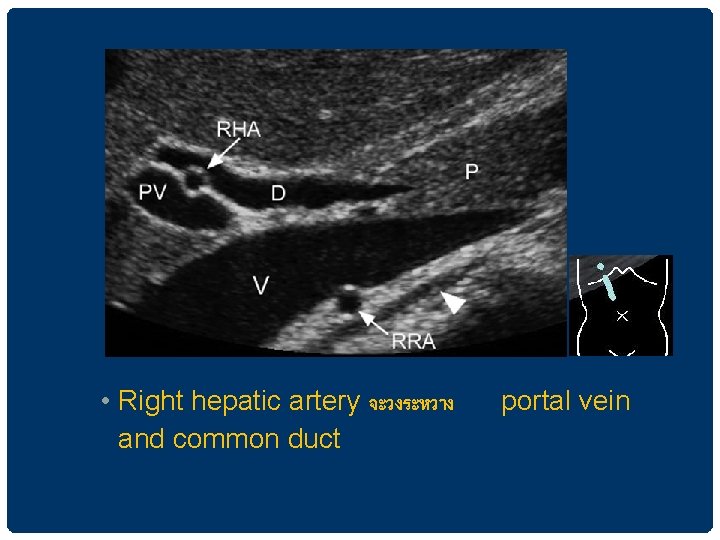
• Right hepatic artery จะวงระหวาง and common duct portal vein

BILIARY DILATATION Intrahepatic duct -larger than 2 mm diameter -more than 40% diameter of the adjacent portal vein
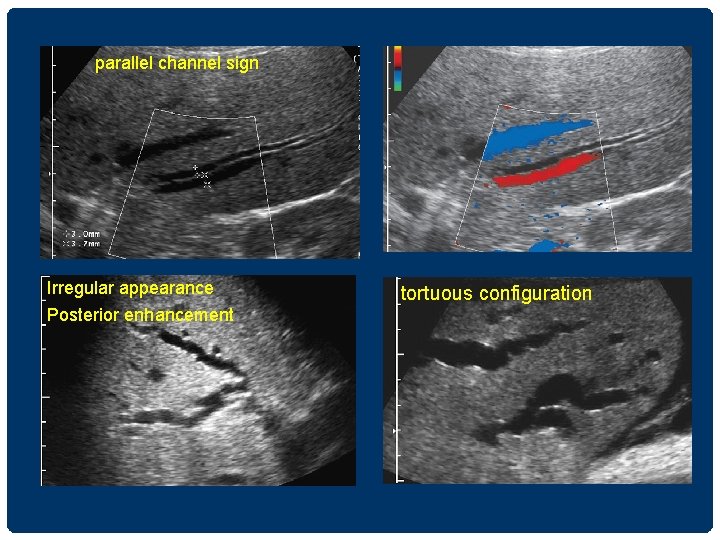
parallel channel sign Irregular appearance Posterior enhancement tortuous configuration

BILIARY DILATATION Extrahepatic duct - CHD 4 -5 mm - CBD วดจากขอบดานในของดานหนงไปอกดานหน ง 4 -6 mm 6 -7 mm equivocal >8 mm indicate ductal dilatation • Elderly patients and in postcholecystectomy patients อาจพบ common duct dilatation ไดถง 9 -10 mm • Acute, intermittent, and partial obstruction
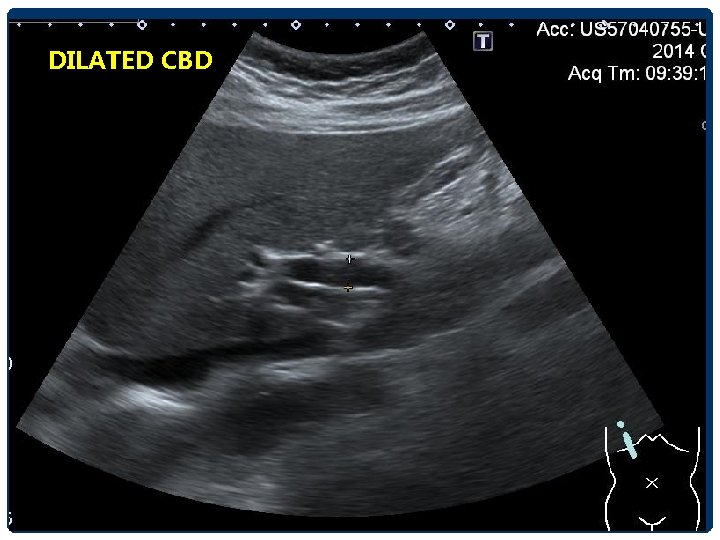
DILATED CBD
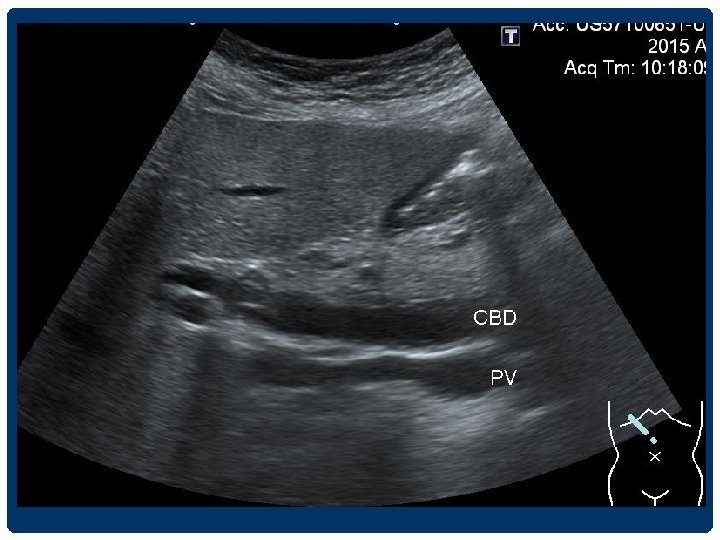

CHOLEDOCHOLITHIASIS/STONE • Most common causes of biliary obstruction • Intrahepatic duct stones less common than CBD stones • Gall stone --- 15% ass. with CBD stone • CBD stone ---95% ass. With GS
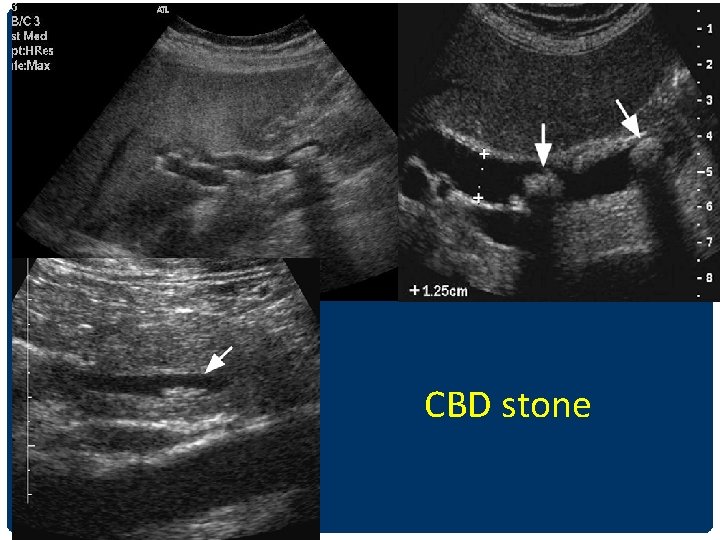
CBD stone
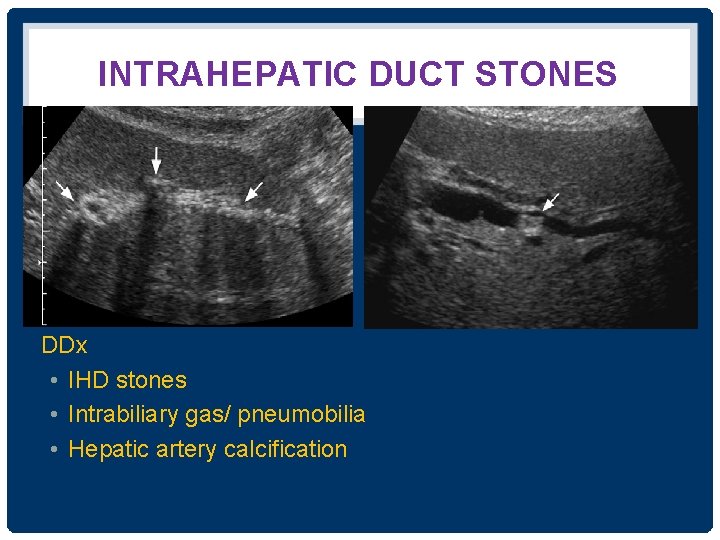
INTRAHEPATIC DUCT STONES DDx • IHD stones • Intrabiliary gas/ pneumobilia • Hepatic artery calcification
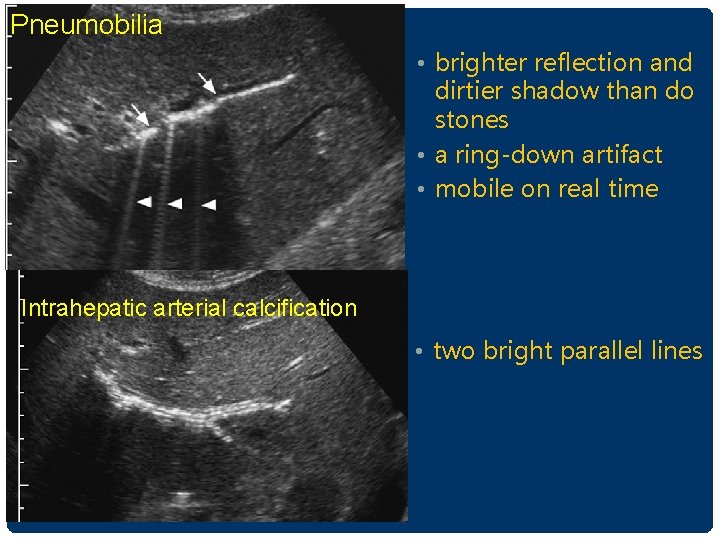
Pneumobilia • brighter reflection and dirtier shadow than do stones • a ring-down artifact • mobile on real time Intrahepatic arterial calcification • two bright parallel lines
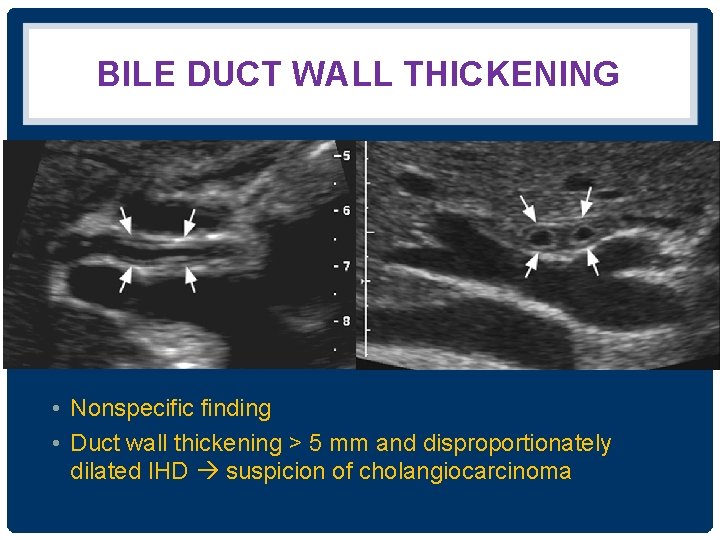
BILE DUCT WALL THICKENING • Nonspecific finding • Duct wall thickening > 5 mm and disproportionately dilated IHD suspicion of cholangiocarcinoma

CAUSES OF BILE DUCT WALL THICKENING Risk factor of CHCA > 5 mm and disproportionately dilated IHD Risk factor of CHCA
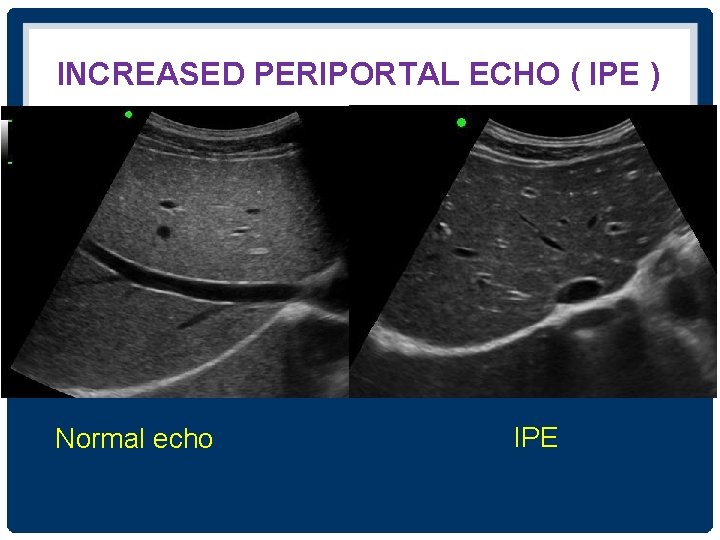
INCREASED PERIPORTAL ECHO ( IPE ) Normal echo IPE
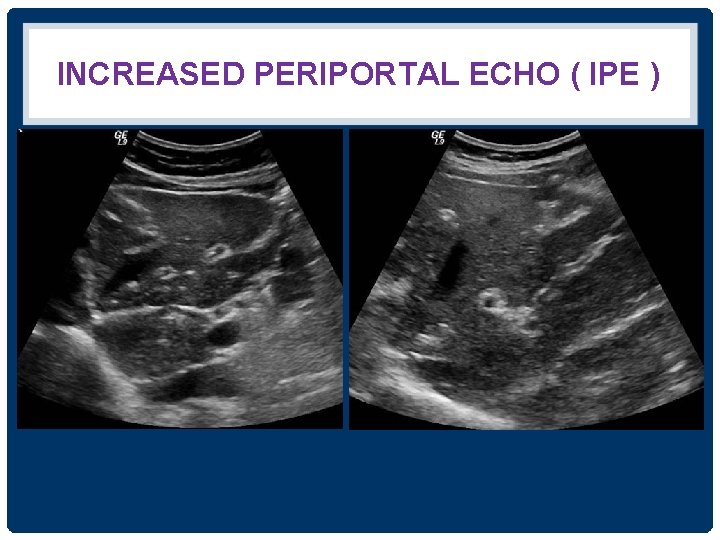
INCREASED PERIPORTAL ECHO ( IPE )
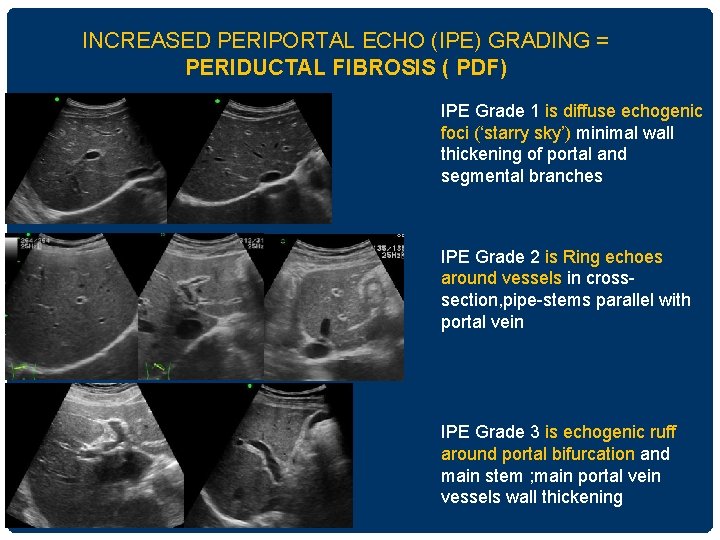
INCREASED PERIPORTAL ECHO (IPE) GRADING = PERIDUCTAL FIBROSIS ( PDF) IPE Grade 1 is diffuse echogenic foci (‘starry sky’) minimal wall thickening of portal and segmental branches IPE Grade 2 is Ring echoes around vessels in crosssection, pipe-stems parallel with portal vein IPE Grade 3 is echogenic ruff around portal bifurcation and main stem ; main portal vein vessels wall thickening
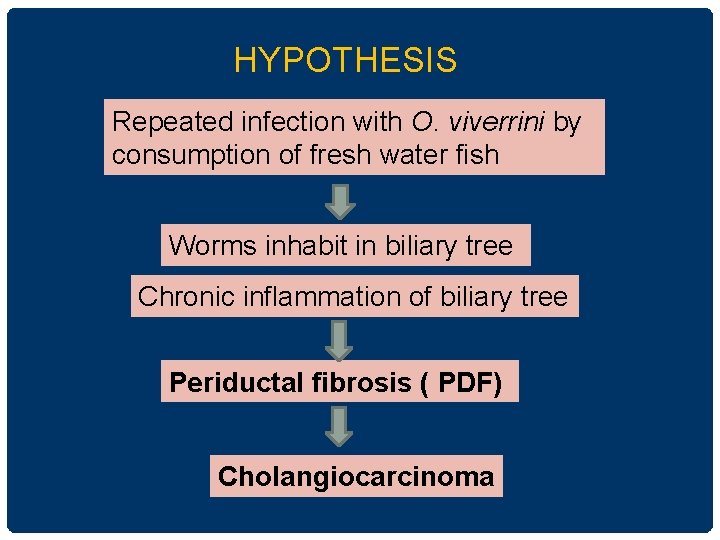
HYPOTHESIS Repeated infection with O. viverrini by consumption of fresh water fish Worms inhabit in biliary tree Chronic inflammation of biliary tree Periductal fibrosis ( PDF) Cholangiocarcinoma
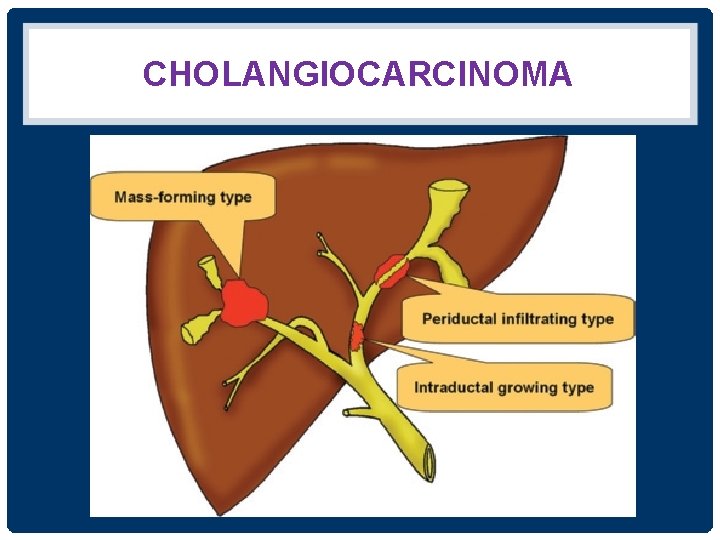
CHOLANGIOCARCINOMA

ULTRASONOGRAPHIC PATTERN OF CHCA • 1. Parenchymal mass • 2. Dilatation of bile duct without mass • 3. Parenchymal mass with dilated duct • 4. Dilatation of bile duct with intraluminal mass
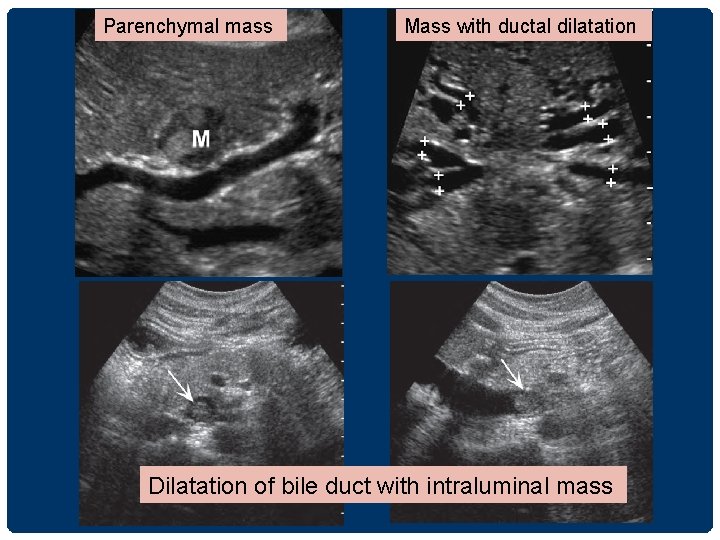
Parenchymal mass Mass with ductal dilatation Dilatation of bile duct with intraluminal mass

TAKE HOME POINT • Review anatomy • Middle hepatic vein is landmark for right and left lobe liver • CBD and all bile duct runs parallel to portal vein • Comparing echo pattern, liver echo > renal cortex • Normal tubular structures visible in liver parenchyma are portal vein, hepatic vein

TAKE HOME POINT • Cholangiocarcinoma have non-specific sonographic feature • Important in surveillance US 1. abnormal echo mass lesion 2. dilatation of IHD or EHD • PDF has protential to be sonographic sign to closely follow up in a risk group of CCA surveillance

THANK YOU
- Slides: 118