URINARY SYSTEM Medical ppt http hastaneciyiz blogspot com
URINARY SYSTEM Medical ppt http: //hastaneciyiz. blogspot. com

FUNCTIONS OF THE SYSTEM URINARY 1. 2. 3. 4. 5. 6. FILTERING OF BLOOD REGULATION OF BLOOD VOLUME REGULATION OF BLOOD SOLUTES RBC SYNTHESIS VITAMIN D SYNTHESIS GLUCONEOGENESIS

KIDNEY ANATOMY
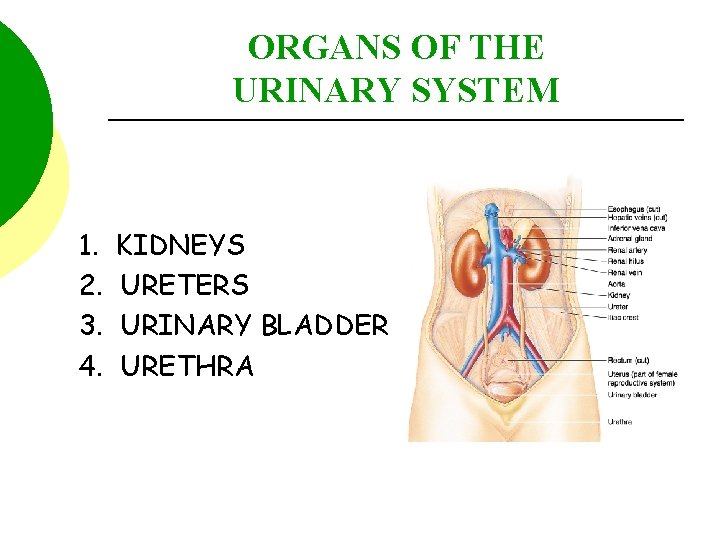
ORGANS OF THE URINARY SYSTEM 1. 2. 3. 4. KIDNEYS URETERS URINARY BLADDER URETHRA
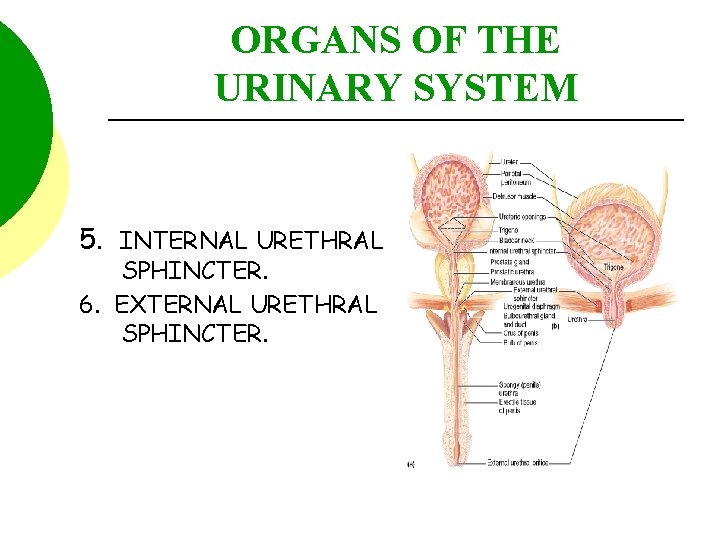
ORGANS OF THE URINARY SYSTEM 5. INTERNAL URETHRAL SPHINCTER. 6. EXTERNAL URETHRAL SPHINCTER.
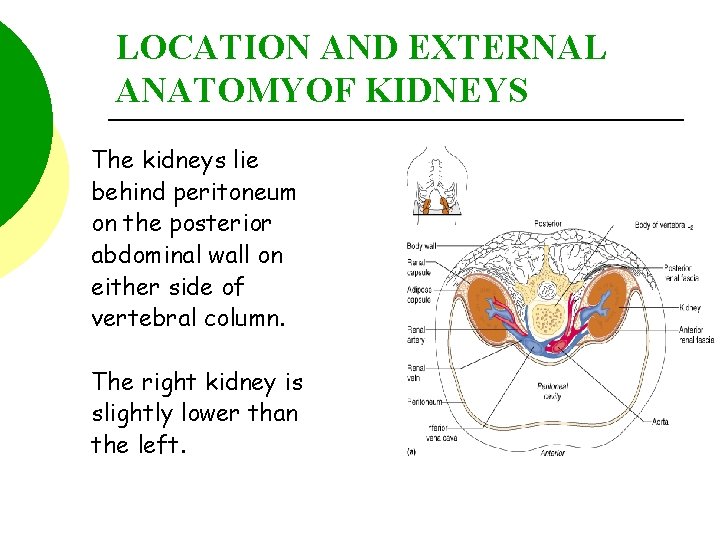
LOCATION AND EXTERNAL ANATOMYOF KIDNEYS The kidneys lie behind peritoneum on the posterior abdominal wall on either side of vertebral column. The right kidney is slightly lower than the left.

EXTERNAL ANATOMY OF THE KIDNEY The covering of kidney consists of three layers. The inner layer, the renal capsule, the middle layer, the adipose capsule, and the outer, renal fascia.
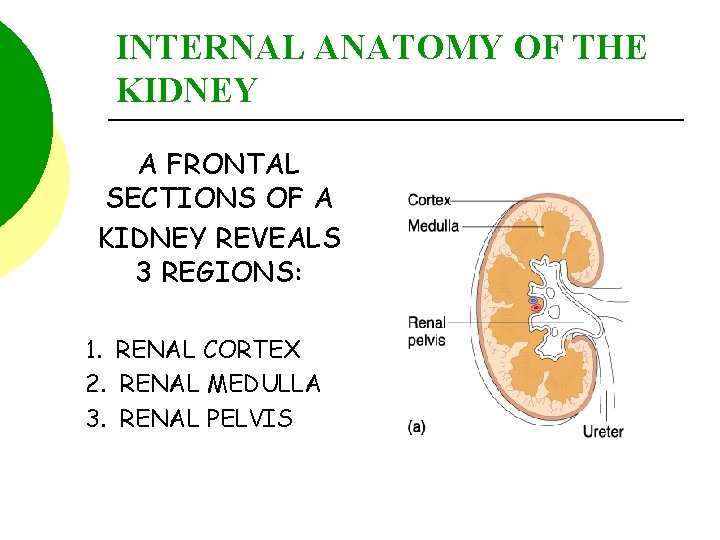
INTERNAL ANATOMY OF THE KIDNEY A FRONTAL SECTIONS OF A KIDNEY REVEALS 3 REGIONS: 1. RENAL CORTEX 2. RENAL MEDULLA 3. RENAL PELVIS
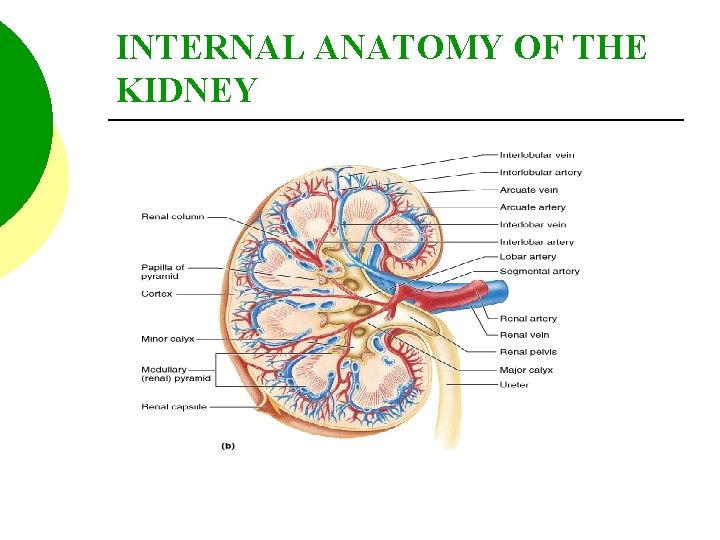
INTERNAL ANATOMY OF THE KIDNEY
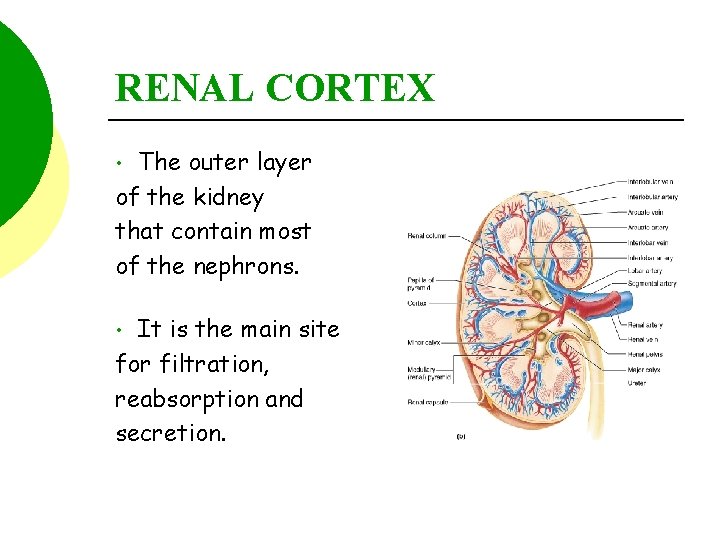
RENAL CORTEX The outer layer of the kidney that contain most of the nephrons. • It is the main site for filtration, reabsorption and secretion. •
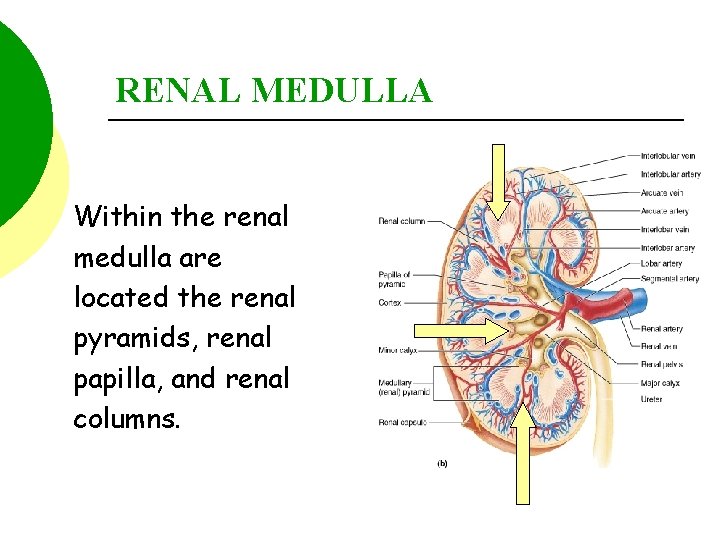
RENAL MEDULLA Within the renal medulla are located the renal pyramids, renal papilla, and renal columns.
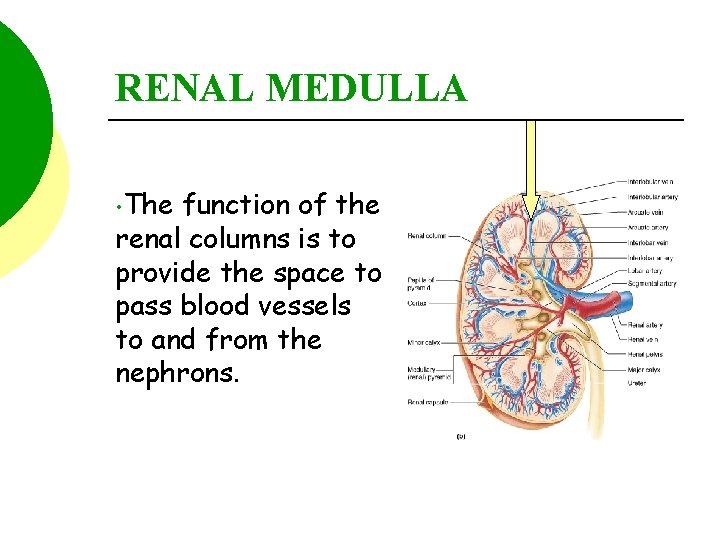
RENAL MEDULLA • The function of the renal columns is to provide the space to pass blood vessels to and from the nephrons.
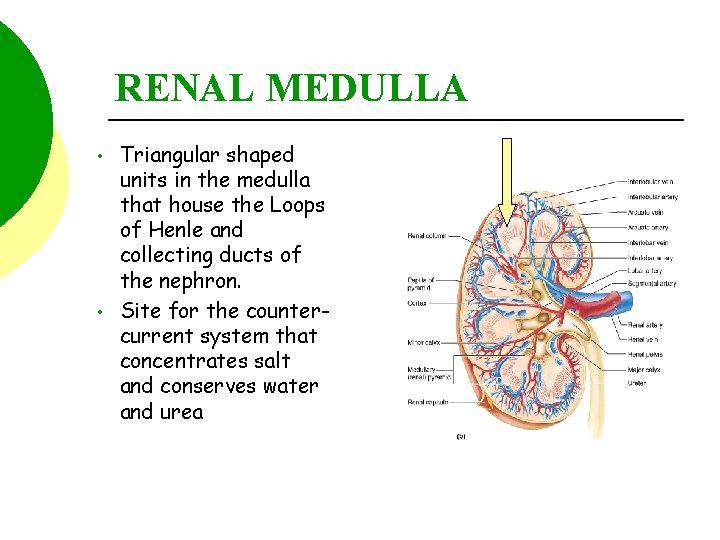
RENAL MEDULLA • • Triangular shaped units in the medulla that house the Loops of Henle and collecting ducts of the nephron. Site for the countercurrent system that concentrates salt and conserves water and urea
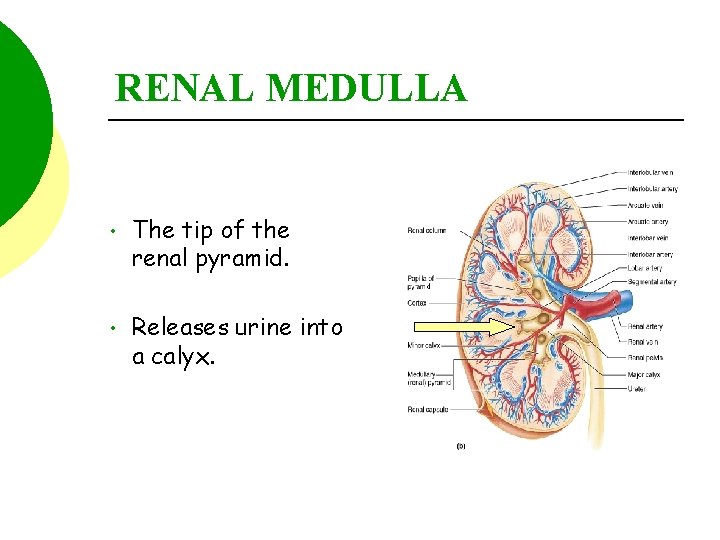
RENAL MEDULLA • The tip of the renal pyramid. • Releases urine into a calyx.
INTERNAL ANATOMY OF THE KIDNEY The nephrons of the kidneys produces urine. It flows from the renal papilla, to the minor calyce, to the major calyce, to the renal pelvis, and finally exits the kidney within the ureter.
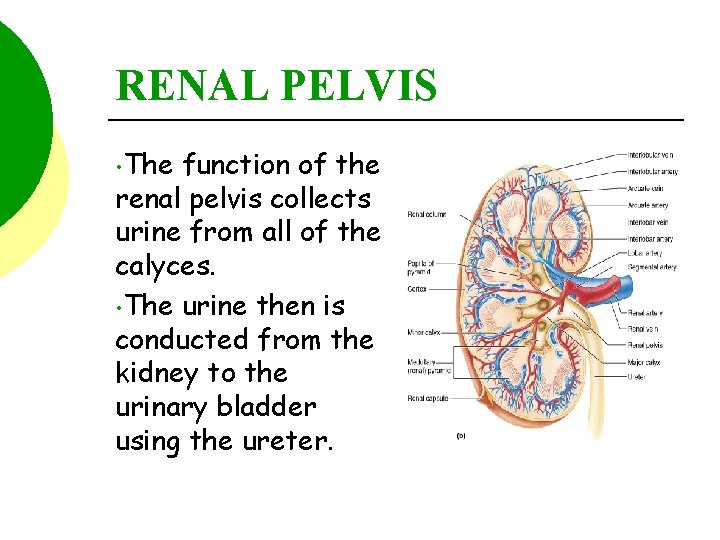
RENAL PELVIS • The function of the renal pelvis collects urine from all of the calyces. • The urine then is conducted from the kidney to the urinary bladder using the ureter.
INTERNAL ANATOMY OF THE KIDNEY Two major blood vessels are associated with the kidney. The renal artery, a branch of the abdominal aorta, and the renal vein, which empties into the inferior vena cava.
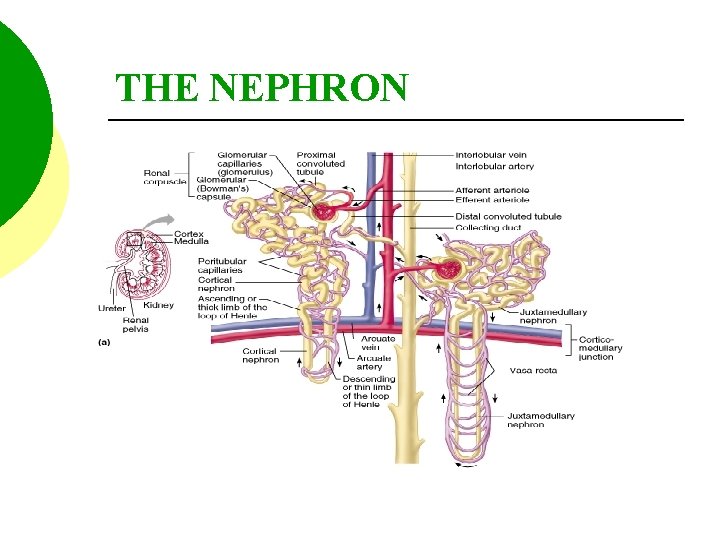
THE NEPHRON
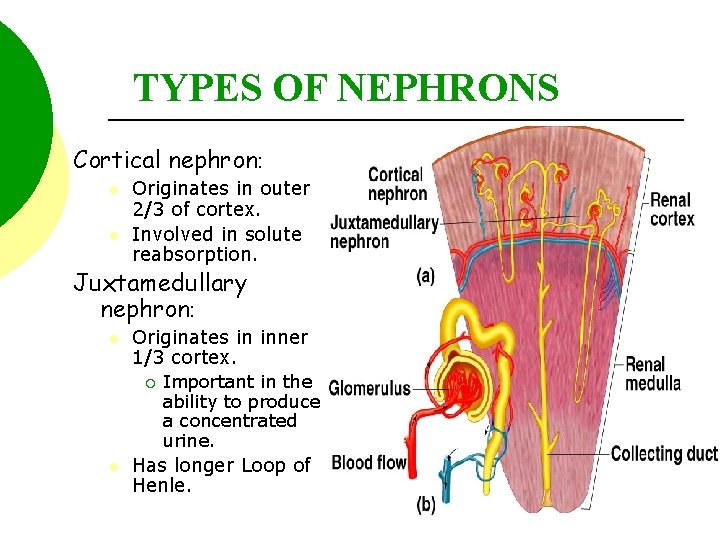
TYPES OF NEPHRONS Cortical nephron: l l Originates in outer 2/3 of cortex. Involved in solute reabsorption. Juxtamedullary nephron: l Originates in inner 1/3 cortex. ¡ l Important in the ability to produce a concentrated urine. Has longer Loop of Henle. Insert fig. 17. 6
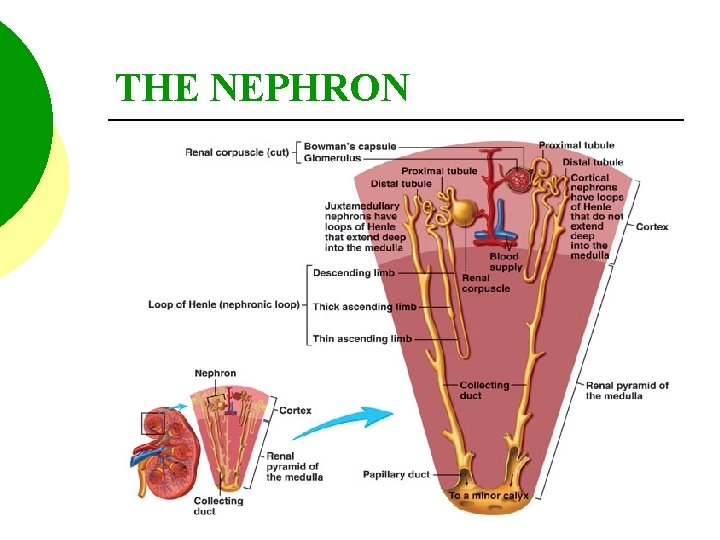
THE NEPHRON

THE NEPHRON STRUCTURES OF THE NEPHRON 1. BOWMAN’S CAPSULE 2. PROXIMAL CONVOLUTED TUBULE 3. LOOP OF HENLE A. DESCENDING LIMB B. ASCENDING LIMB 4. DISTAL CONVOLUTED TUBULE THESE EMPTY INTO THE COLLECTING DUCT OR TUBULES.


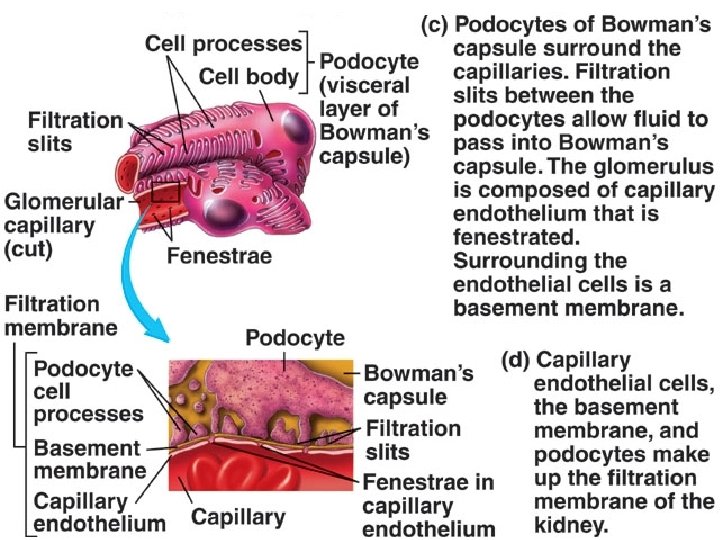

PROXIMAL CONVOLUTED TUBULE

PROXIMAL CONVOLUTED TUBULES Simple cuboidal epithelial cells with prominent brush borders of microvilli.
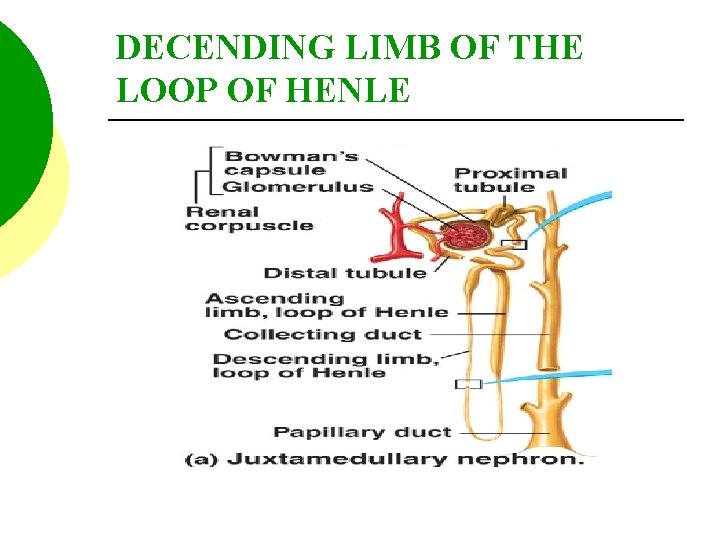
DECENDING LIMB OF THE LOOP OF HENLE
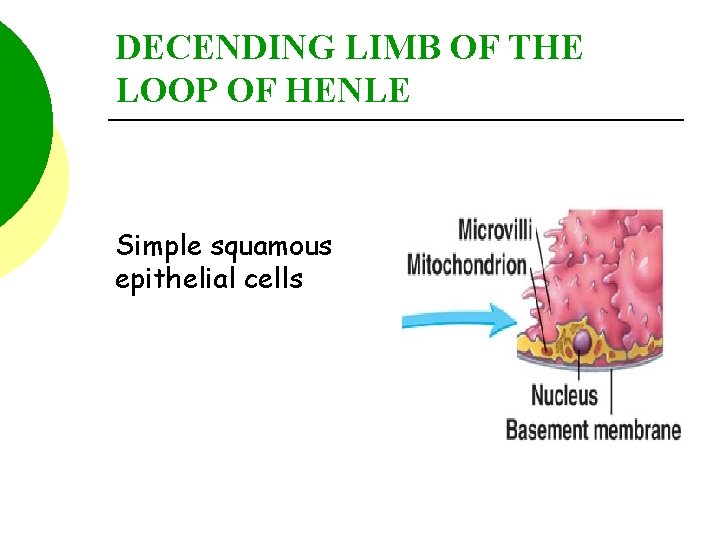
DECENDING LIMB OF THE LOOP OF HENLE Simple squamous epithelial cells
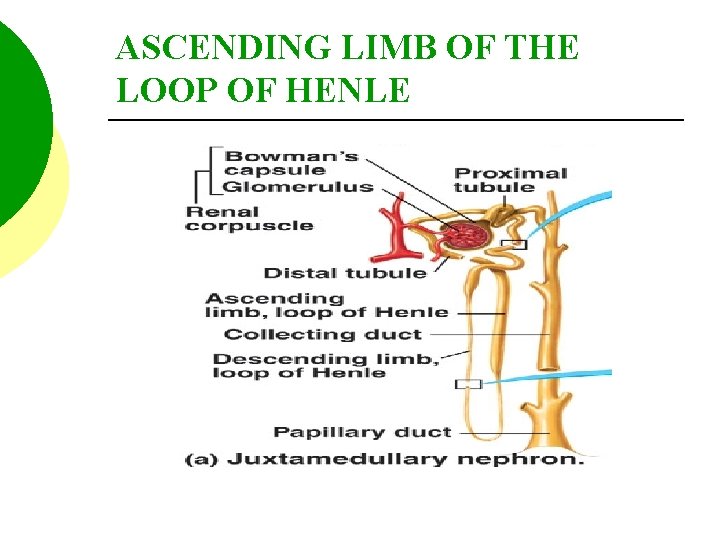
ASCENDING LIMB OF THE LOOP OF HENLE

ASCENDING LIMB OF THE LOOP OF HENLE Simple cuboidal epthelial to low columnar cells.
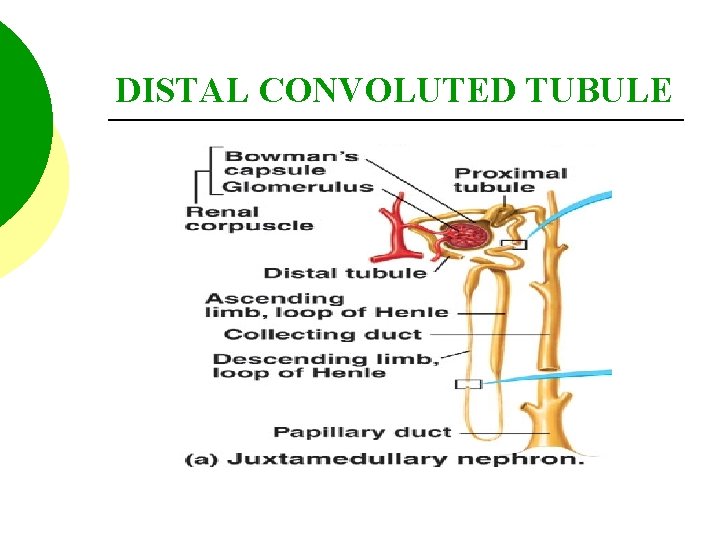
DISTAL CONVOLUTED TUBULE
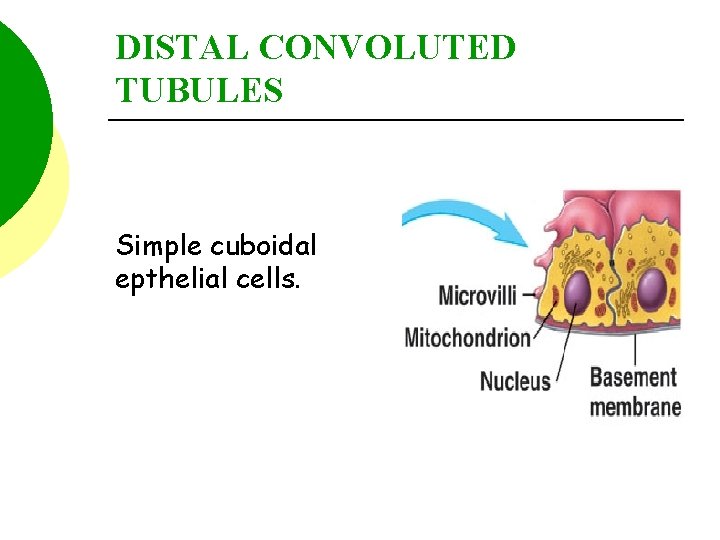
DISTAL CONVOLUTED TUBULES Simple cuboidal epthelial cells.

THE NEPHRON 1. Proximal convoluted tubule 1. 2. Descending limb of Loop of Henle 2. 3. 4. Ascending Limb of Loop of Henle Distal convoluted tubules 3. 4. Simple cuboidal epithelial cells with prominent brush borders of microvilli. Simple squamous epithelial cells Simple cuboidal to low columnar epithelial cells. Simple cuboidal epthelial cells.

THE NEPHRON BLOOD VESSELS OF THE NEPHRON 1. 2. 3. 4. 5. AFFERENT ARTERIOLE GLOMERULUS EFFERENT ARTERIOLE PERITUBULAR CAPILLARIES VASA RECTA
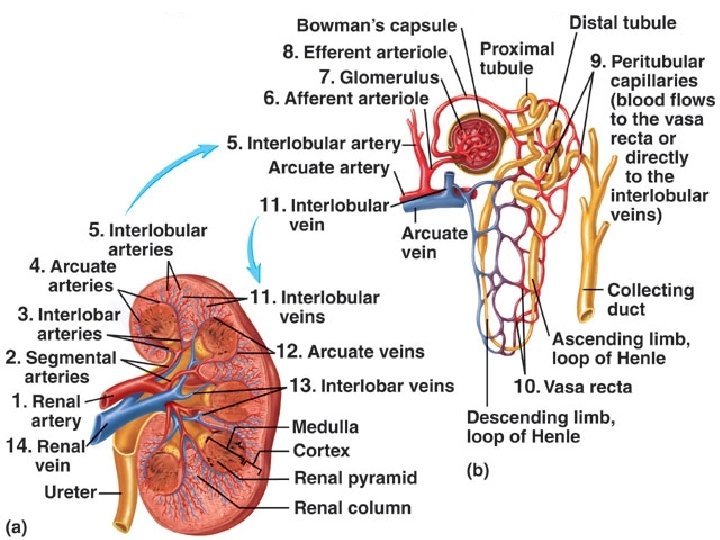

JUXTAGLOMERULAR APPARATUS THE JGA IS LOCATED WHERE THE INITIAL PORTION OF THE DISTAL CONVOLUTED TUBULE LIES AGAINST THE AFFERENT, AND SOMETIMES THE EFFERENT, ARTERIOLE.
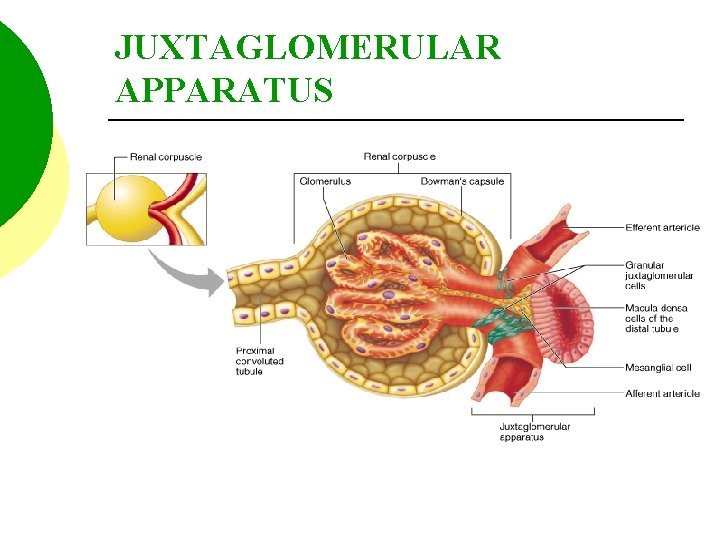
JUXTAGLOMERULAR APPARATUS

JUXTAGLOMERULAR APPARATUS SOME THE SMOOTH MUSCLE CELLS OF THE AFFERENT ARTERIOLES ENLARGE AND HAVE PROMINENT SECRETORY GRANULES CONTAINING RENIN. THESE CELLS ARE TERMED JG CELLS, AND THEY ACT AS BARORECEPTORS.

JUXTAGLOMERULAR APPARATUS THE CELLS OF THE DISTAL CONVOLUTED TUBULE WHICH CONTACT THE ARTERIOLES ARE TERMED THE MACULA DENSA. THESE CELLS DETECT CHANGES IN THE RATE AT WHICH URINE FLOW PAST THEM AND THE CONCENTRATION OF SOLUTES IN THE URINE.

JUXTAGLOMERULAR APPARATUS THE MACULA DENSA CELLS TRIGGER THE RELEASE OF LOCALLY ACTING CHEMICALS WHICH EITHER VASOCONSTRICT OR VASODILATE THE AFFERENT ARTERIOLE. THIS RESULTS IN A CHANGE THE GFR.

KIDNEY PHYSIOLOGY

KIDNEY PHYSIOLOGY URINE FORMATION AND THE SIMULTANEOUS ADJUSTMENT OF BLOOD COMPOSITION INVOLVES THREE MAJOR PROCESSES: 1. GLOMERULAR FILTRATION 2. TUBULAR REABSORPTION 3. SECRETION

KIDNEY PHYSIOLOGY

KIDNEY PHYSIOLOGY FILTRATION is the movement of substances from the glomerulus into the lumen of bowman’s capsule. This forms filtrate.

KIDNEY PHYSIOLOGY REABSORPTION is the movement of substances, solutes and water, across the walls of nephron into the capillaries associated with the nephron.

KIDNEY PHYSIOLOGY SECRETION is the movement of substances from the capillaries, associated with the nephron, across the walls of nephron into the filtrate with the nephron.

OSMOTIC EFFECTS Water serves as the universal solvent in which a variety of solutes are dissolved. Solutes can be classified as electrolytes and nonelectrolytes.

ELECTROLYTES Electrolytes have ionic bonds which allow the compounds to dissociate into ions in water. Because ions are charged particles, they can conduct an electrical current.

ELECTROLYTES Examples of electrolytes include inorganic salts, inorganic and organic acids and bases, and some proteins.

NONELECTROLYTES Nonelectrolytes have bonds, usually covalent bonds, that prevent them from dissociating in solution. Therefore, they have no electrical charge.

NONELECTROLYTES Examples of nonelectrolytes include glucose, lipids, creatinine, and urea.

OSMOTIC EFFECTS All dissolved solutes contribute to the osmotic activity of a fluid. However, electrolytes have greater power because each electrolyte molecule dissociates into at least 2 ions.

OSMOTIC EFFECTS Water moves according to osmotic gradients—from areas of lesser osmolality to areas of greater osmolality.

OSMOLALITY A solution’s osmolality is number of solute particles dissolved in one liter of water. Osmotic activity is determined only by the number of solute particles.

OSMOLALITY Ten sodium ions have the same osmotic activity as ten glucose molecules or ten amino acids in the same volume of solution.

OSMOLALITY Water moves according to osmotic gradients— from areas of lesser to higher osmolality.

GLOMERULAR FILTRATION “Urine” formation begins with glomerular filtration. It is a passive process in which fluids and solutes are forced through the glomerular membrane.

GLOMERULAR FILTRATION Substances which pass from the glomerulus into the nephron include: water, electrolytes, glucose, amino acids, vitamins, small proteins, creatinine, urate ions, and urea.

GLOMERULAR FILTRATION

GLOMERULAR FILTRATION The net filtration pressure (NFP) is responsible for filtrate formation. NFP=HPg- (OPg+ HPc)

GLOMERULAR FILTRATION Glomerular filtration rate, GFR, is the total amount of filtrate formed per minute by the kidneys. A normal GFR in both kidneys is 120 -125 ml/min or about 180 l/day

GLOMERULAR FILTRATION RATE FACTORS GOVERNING FILTRATION RATE ¡ ¡ ¡ Total surface area available for filtration. Filtration membrane permeability Net Filtration Pressure

GLOMERULAR FILTRATION GFR IS HELD RELATIVELY CONSTANT BY TWO IMPORTANT MECHANISMS THAT REGULATE RENAL BLOOD FLOW: 1. INSTRINICALLY BY RENAL AUTOREGULATION 2. EXTRINICALLY BY NEURAL AND HORMONAL CONTROLS

RENAL AUTOREGULATION OF GFR To maintain a stable GFR, the kidney regulates the diameter of the afferent arteriole. therefore, when B. P. decreases the vessel dilates, and when B. P. increases the vessel constricts. This results in a stable G. F. R.

RENAL AUTOREGULATION OF GFR THE KIDNEY USES TWO MECHANISMS TO PREFORM AUTOREGULATION: 1. MYOGENIC MECHANISM 2. TUBULOGLOMERULAR FEEDBACK

MYOGENIC MECHANISM The myogenic mechanism is based on the tendency of vascular smooth muscle to contract when stretched. If B. P. is elevated, the smooth muscle in the afferent arterioles are stretched. In response, the smooth muscle contracts, which narrows the arteriole’s lumen, and renal blood flow decreases, which reduces GFR to is previous level. This mechanism normalizes renal blood flow and GFR within seconds after blood pressure changes.

TUBULOGLOMERULAR FEEDBACK The macula densa cells of the juxtaglomerular apparatus respond to changes in the osmolarity and changes in flow rate of the filtrate at the junction of the D. C. T. and the ascending limb of the loop of Henle.

TUBULOGLOMERULAR FEEDBACK This results in the secretion of chemicals which produce local vasoconstriction of the afferent and efferent arterioles. Examples include nitric oxide, adenosine, endothelin, and prostaglandins. This mechanism operates more slowly than the myogenic mechanism.

EXTRINIC CONTROL OF GFR THE GFR CAN ALSO BE CONTROLLED EXTRINICALLY BY: 1. SYMPATHETIC NERVOUS SYSTEM 2. RENIN, ANGIOTENSION, ALDOSTERONE MECHANISM

TUBULAR REABSORPTION The proximal convoluted tubules are the most active in tubular reabsorption. All glucose, lactate, and amino acids are reabsorbed in this area.

TUBULAR REABSORPTION About 65% of sodium, 70% of water, are also reabsorbed 90% of bicarbonate ions, 50% of chloride ions, and 55% of potassium are reabsorbed in the proximal convoluted tubules.

TUBULAR REABSORPTION This large amount of tubular reabsorption associated with the pct, results in the GFR being reduced from 120 ml/min to about 40 ml/min.
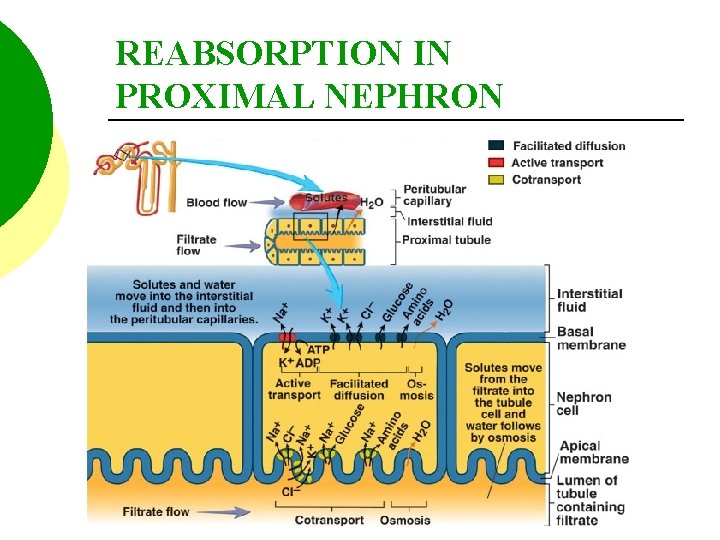
REABSORPTION IN PROXIMAL NEPHRON

TUBULAR REABSORPTION Tubular reabsorption from the loop of Henle results in 10% of water being reabsorbed from the descending limb, 30% of potassium ions, 20% of sodium, and 35% of chloride from the ascending limb.
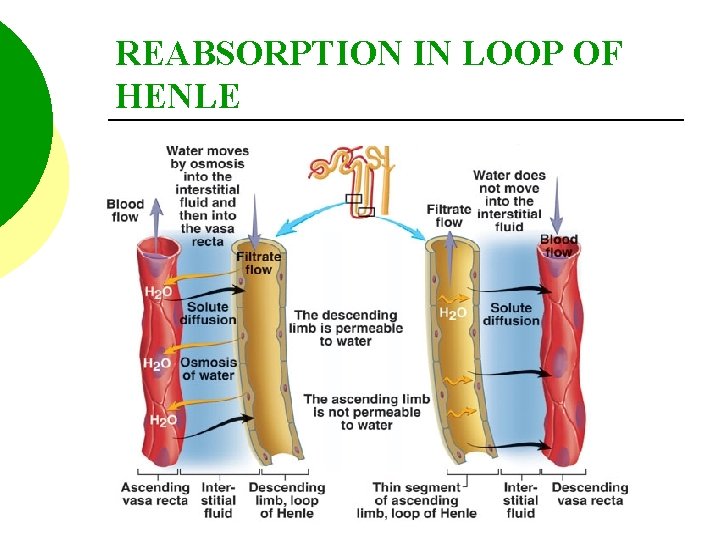
REABSORPTION IN LOOP OF HENLE

REABSORPTION IN LOOP OF HENLE

TUBULAR REABSORPTION Fluids enters the distal convoluted tubules at a rate of about 25 ml/min. because about 80% of the water in the filtrate has been reabsorbed.

TUBULAR REABSORPTION As fluid flows through the DCT, sodium and chloride are reabsorbed. By the time fluids reaches the end of the DCT, about 90% of the filtered solutes and water has been returned to the blood.

THE COUNTER CURRENT MECHANISM One of the functions of the kidneys is to regulate urine concentration and volume. The kidneys accomplish this by the countercurrent mechanism.

THE COUNTER CURRENT MECHANISM In the kidneys the countercurrent mechanism involves the interaction between the flow of filtrate through the loops of Henle, and the flow of blood through the adjacent vasa recta blood vessels.

THE COUNTER CURRENT MECHANISM The flow in these two structures is opposite in direction.
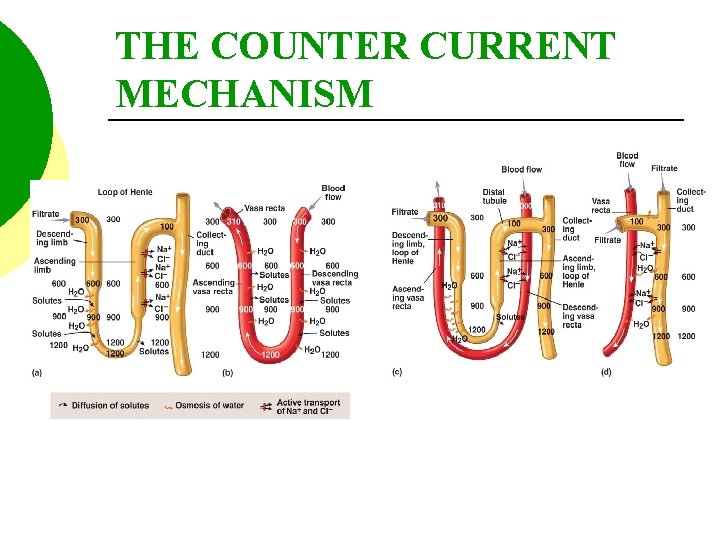
THE COUNTER CURRENT MECHANISM

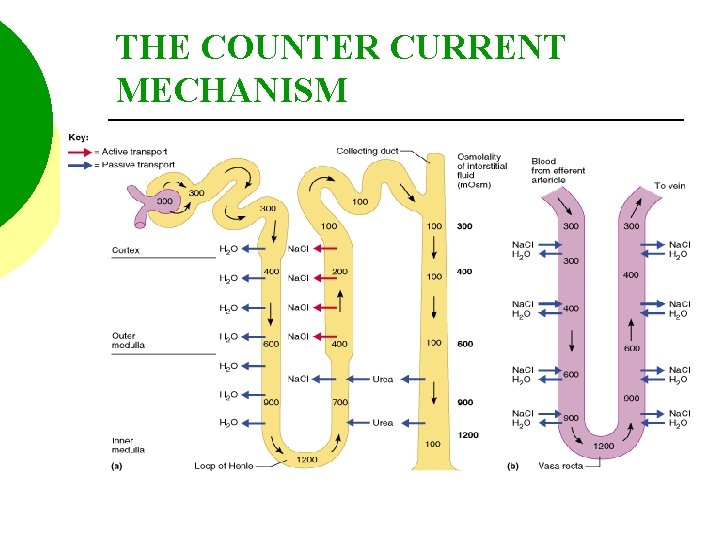
THE COUNTER CURRENT MECHANISM The Na. Cl concentration of the medulla acts as an osmotic force which “draws” water from the descending limb of the loop of Henle.

THE COUNTER CURRENT MECHANISM This is possible because the descending limb is lined with simple squamous epithelial cells, that are permeable to water, but, impermeable to Na. Cl and other solutes.

THE COUNTER CURRENT MECHANISM The movement of water causes the osmolarity of the filtrate to increase from 300 to 1, 200 m. OSM/L.
THE COUNTER CURRENT MECHANISM

THE COUNTER CURRENT MECHANISM The ascending limb of the loop of Henle reabsorbs chloride by active transport. In addition, as chloride moves from the filtrate it “pulls” sodium along into the medulla.

THE COUNTER CURRENT MECHANISM This is possible because the ascending limb is impermeable to water.

THE COUNTER CURRENT MECHANISM The movement of Na. Cl into the medulla decreases the osmolarity of the filtrate from 1, 200 to 100 m. Osm/L.

THE COUNTER CURRENT MECHANISM

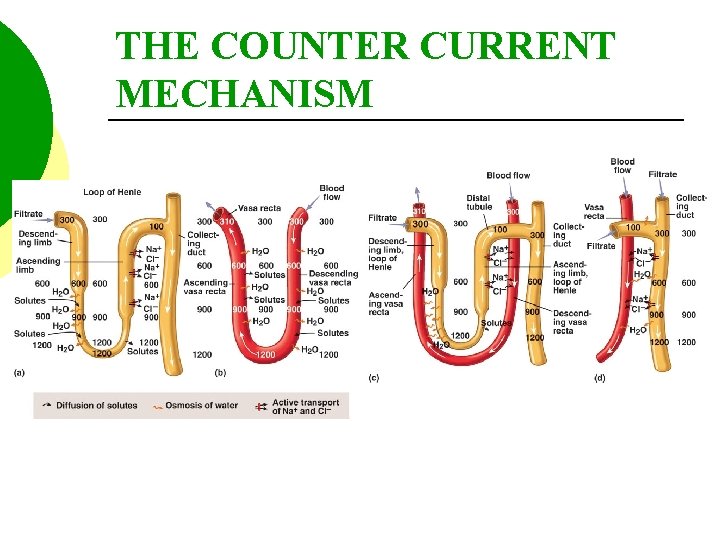
THE COUNTER CURRENT MECHANISM The hyperosmotic medulla also “pulls” water from the collecting ducts. This varies depending on the amount of ADH. As water moves from the collecting duct, urea follows.

THE COUNTER CURRENT MECHANISM Thus, water is conserved, as well as, a certain amountof urea. The urea contributes to the high osmolarity of the medulla.

THE COUNTER CURRENT MECHANISM The vasta recta is composed of capillaries which surround the loop of henle. The vessels flow counter (opposite) to the loop of Henle and act as a counter current exchanger.

THE COUNTER CURRENT MECHANISM As blood flows through the vasa recta it picks up water and leaves behind Na. Cl.

THE COUNTER CURRENT MECHANISM Therefore, the vasa recta returns water back to the body and the Na. Cl maintains the hyperosmotic medulla.
THE COUNTER CURRENT MECHANISM

TUBULAR SECRETION Tubular secretion is the movement of chemicals from the blood into the nephron. This process can occur in the proximal or distal convoluted tubules.

TUBULAR SECRETION THIS PROCESS IS IMPORTANT FOR: 1. Disposing of substances which were not filtered. 2. Removal of excess K+. 3. Controlling blood ph. 4. Eliminating substances which have been reabsorbed.

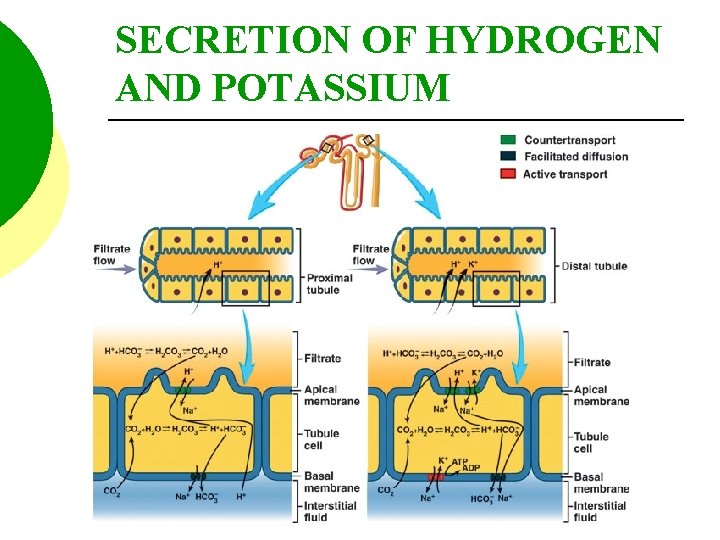
TUBULAR SECRETION Most secretion occurs within the PCT. Substances such as neurotransmitters, bile pigment, uric acid, penicillin, atropine, morphine, H+ , and ammonia are secreted.

TUBULAR SECRETION The DCT receives mainly K+ and H+ ions from the blood.
SECRETION OF HYDROGEN AND POTASSIUM
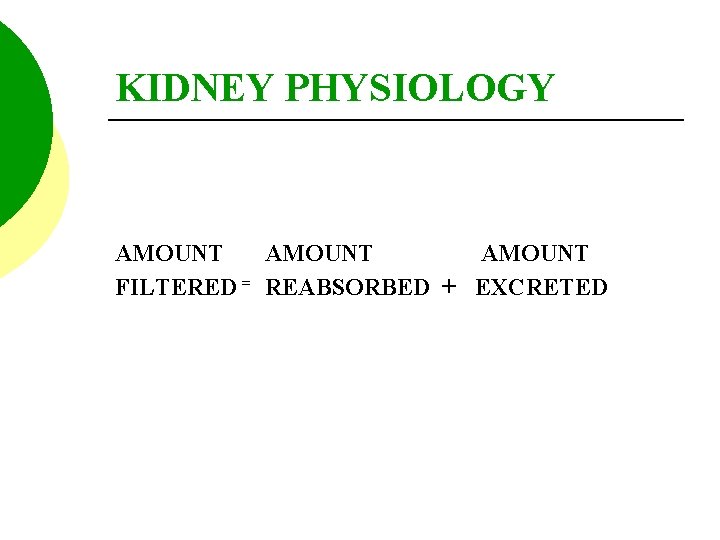

KIDNEY PHYSIOLOGY AMOUNT FILTERED = REABSORBED + EXCRETED

KIDNEY PHYSIOLOGY If the kidneys filters 16 grams of Na. Cl per day, and reabsorb 14 grams of Na. Cl per day, then 2 grams of Na. Cl would be excreted by the kidneys per day.

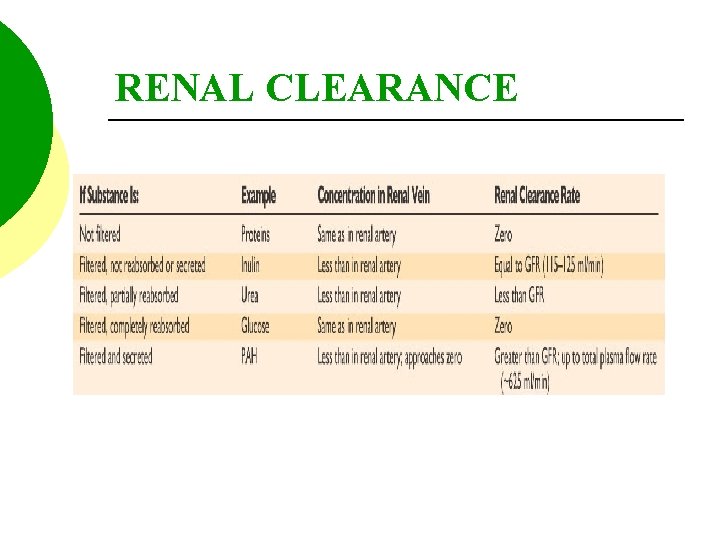
KIDNEY PHYSIOLOGY Renal clearance refers to the volume of plasma that is cleared of a particular substance in a given time, usually 1 minute.

KIDNEY PHYSIOLOGY RENAL CLEARANCE CAN BE CALCULATED USING: RC = UV/P U=CONCENTRATION OF SUBSTANCE IN URINE (mg/ml) V= FLOW RATE OF URINE FORMATION (ml/min) P=CONCENTRATION OF SUBSTANCE IN PLASMA (mg/ml)

RENAL CLEARANCE QUESTIONS: 1. If the renal clearance rate is = to GFR? 2. If the renal clearance rate is greater than GFR? 3. If the renal clearance rate is less than GFR?

RENAL CLEARANCE 1. All of the substance is filtered—inulin. 2. All of the substance is filtered and addition is secreted—PAH. 3. Some of the substance is reabsorbed— urea.
RENAL CLEARANCE

HORMONAL CONTROL OF THE KIDNEYS

ANTIDIURETIC HORMONE

HORMONAL CONTROL OF URINE CONCENTRATION One of the most important hormones in the control of urine concentration and volume is antidiuretic hormone, ADH.

ANTIDURETIC HORMONE Antiduretic hormone prevents wide variation in water balance, helping to avoid dehydration or edema.
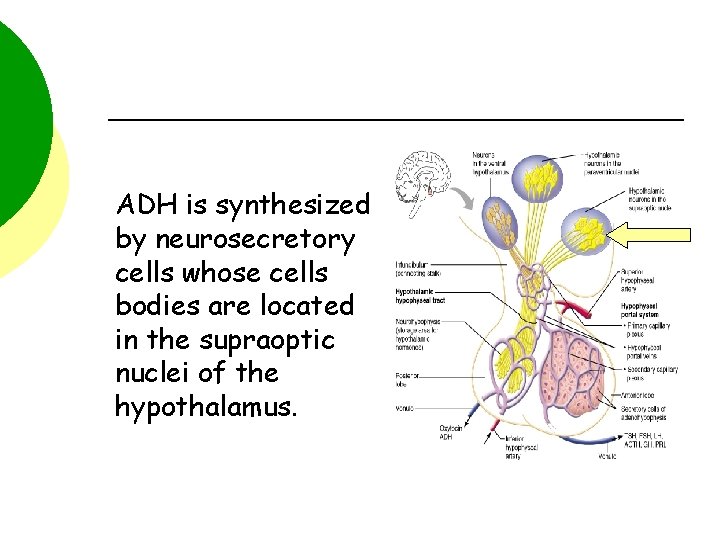
ADH is synthesized by neurosecretory cells whose cells bodies are located in the supraoptic nuclei of the hypothalamus.
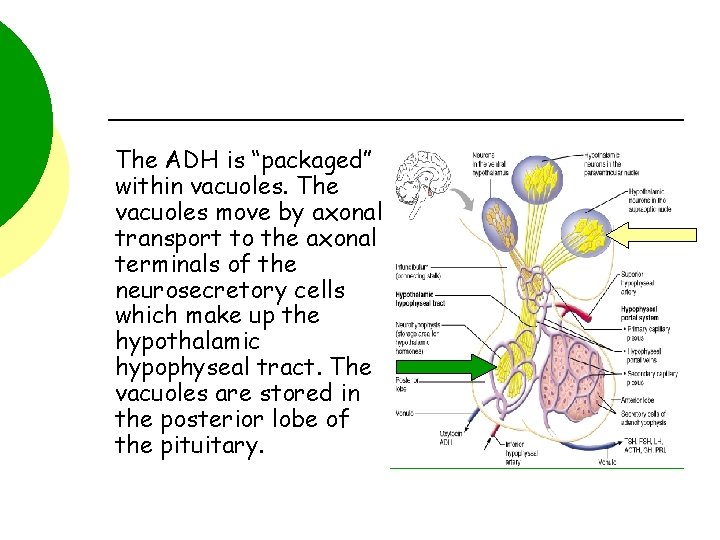
The ADH is “packaged” within vacuoles. The vacuoles move by axonal transport to the axonal terminals of the neurosecretory cells which make up the hypothalamic hypophyseal tract. The vacuoles are stored in the posterior lobe of the pituitary.

ANTIDURETIC HORMONE The chemical class of ADH is a protein

ANTIDURETIC HORMONE Solute concentrations in the blood are monitored by osmoreceptors in the hypothalamus. This is an example of humerol control.

ANTIDURETIC HORMONE When solute concentrations increase, thereby, increasing osmotic pressure, the receptors are stimulated.

ANTIDURETIC HORMONE The osmoreceptors, in turn, stimulate hypothalamic neurons in the supraoptic nucleus, which synthesize ADH.
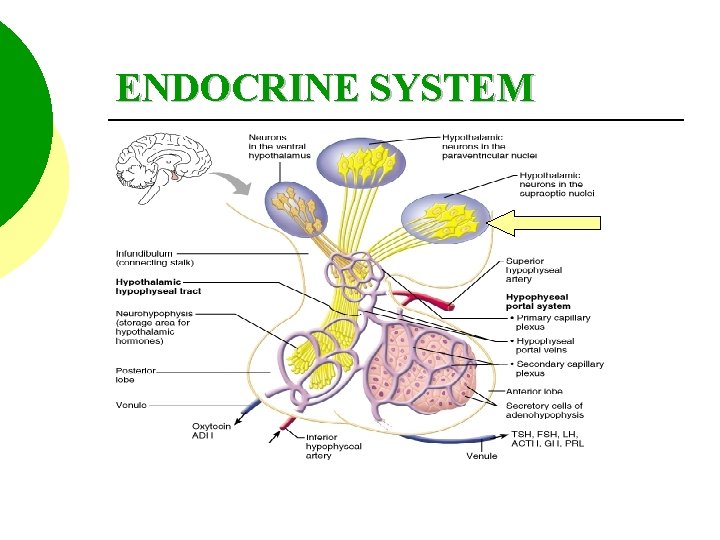
ENDOCRINE SYSTEM

ANTIDURETIC HORMONE Nerve action potentials trigger the release of ADH from the axonal terminals in the posterior lobe of the pituitary.
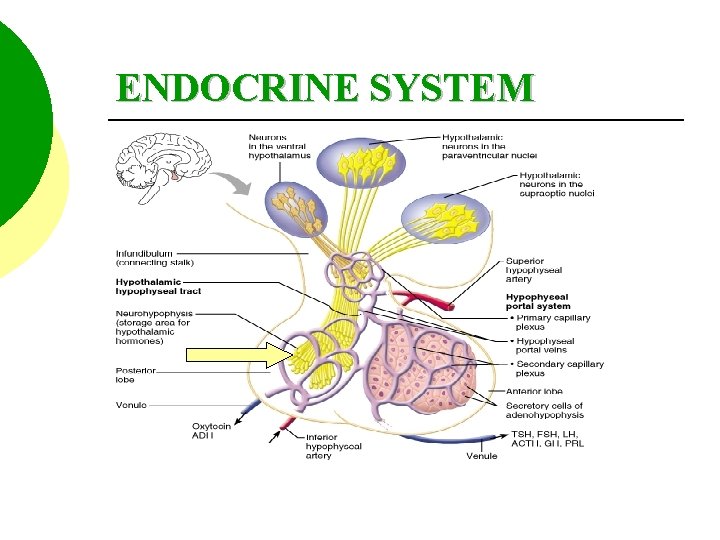
ENDOCRINE SYSTEM
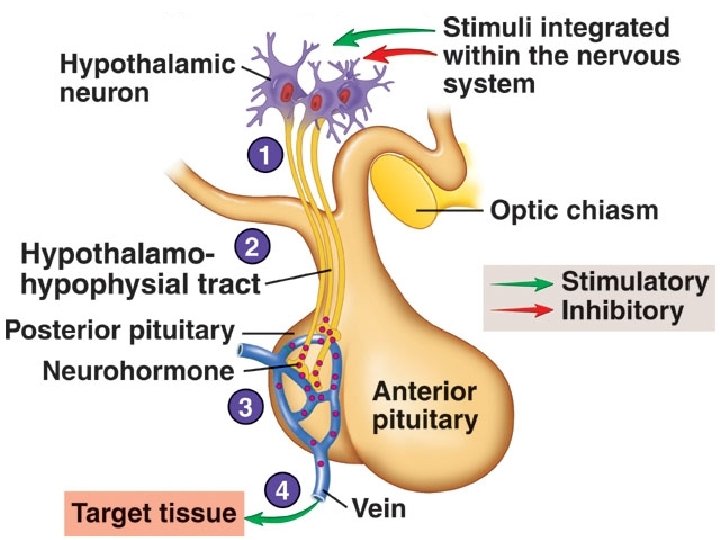

ANTIDURETIC HORMONE ADH travels through the systemic circulation to the distal convoluted tubules of the nephron and the collecting ducts.

ANTIDURETIC HORMONE ADH causes water to be reabsorbed from the D. C. T. and the collecting ducts into the capillaries which surround the nephron.

ANTIDURETIC HORMONE THE RESULTS OF ADH: 1. 2. 3. 4. A decrease in osmolality An increase in blood volume A decrease in urine output An increase in the concentration of the urine.
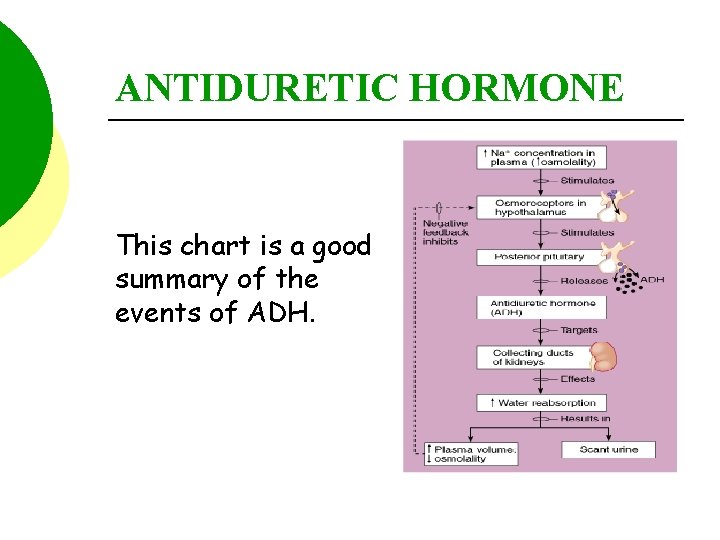
ANTIDURETIC HORMONE This chart is a good summary of the events of ADH.

ANTIDURETIC HORMONE ADH is regulated by negative feedback; when solute concentrations are reduced to normal levels the amount of ADH is reduced.

ANTIDURETIC HORMONE PATHOLOGY 1. Hypersecretion can produce SIADH. 2. Hyposecretion can produce diabetes insipidus.
ALDOSTERONE

ALDOSTERONE Aldosterone’s function is to help maintain Na+ ion balance, and indirectly water balance and K+, within the fluid compartments of the body.

ALDOSTERONE The chemical class of aldosterone is steroid

ALDOSTERONE A decrease in blood pressure
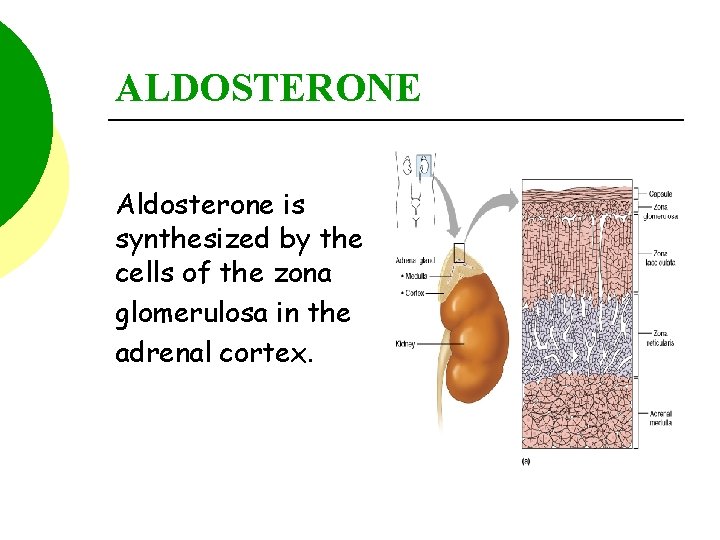
ALDOSTERONE Aldosterone is synthesized by the cells of the zona glomerulosa in the adrenal cortex.

ALDOSTERONE Aldosternone targets the D. C. T. of the nephron.

ALDOSTERONE EFFECTS OF ALDOSTERONE: 1. REABSORPTION OF Na+ IONS. 2. WATER IS REABSORB USING THE SAME TRANSPORT MECHANISM. 3. K+ IONS ARE SECRETION INTO THE DCT FROM THE CAPILLARIES.

ALDOSTERONE Aldosterone secretion is controlled by negative Feedback.

ALDOSTERONE PATHOLOGY: 1. Hypersecretion can produce aldosteronism. 2. Hyposecretion can produce addison disease.

ESTROGEN

ESTROGEN Estrogen is a female sex hormone produced by the ovaries.

ESTROGEN EFFECTS OF ESTROGEN: 1. Reabsorption of Na+ ions. 2. Water is reabsorb using the same transport mechanism. 3. Ca 2+ deposition into bone.

CORTISOL

CORTISOL Cortisol is a hormone produced by the cortex of the adrenal gland. It helps in the conversion of lipids and proteins to form glucose (gluconeogensis).

CORTISOL EFFECTS OF CORTISOL: 1. Reabsorption of Na+ ions. 2. Water is reabsorb using the same transport mechanism. 3. Can cause edema.
BONE CALCIUM REGULATION

CALCITONIN Calcitonin is a hormone produced by the thyroid gland in response to high levels of Ca 2+ ions in the blood.

CALCITONIN EFFECTS OF CALCITONIN: 1. Ca 2+ ion deposition into bone. 2. Inhibit osteoclasts.

CALCITONIN Calcium

PARATHYROID HORMONE Parathyroid hormone is produced by the parathyroid gland in response to low levels of Ca 2+ ions in the blood.

PARATHYROID HORMONE EFFECTS OF PTH: 1. Causes the break down of the inorganic matrix of bone, releasing Ca 2+ ions. 2. Increase absorption of Ca 2+ ions. 3. Reabsorption of Ca 2+ ions from the DCT.
PARATHYROID HORMONE Calcium

ACID BASE BALANCE BLOOD p. H REGULATED BY: 1. KIDNEYS 2. LUNGS 3. BUFFERS IN BLOOD

KIDNEY REGULATION The kidney can regulate p. H by retaining or excreting hydrogen or bicarbonate ions.
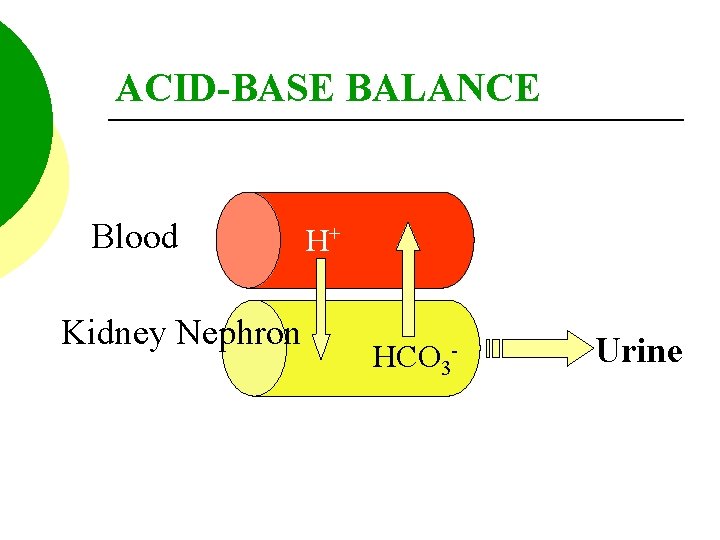
ACID-BASE BALANCE Blood Kidney Nephron H+ HCO 3 - Urine

RESPIRATORY REGULATION The respiratory system regulates p. H by regulating the amount of carbon dioxide in the blood.

CARBON DIOXIDE and p. H CO 2 + H 2 O H 2 CO 3 H+ + HCO 3 - Carbonic Acid

RESPIRATORY REGULATION If the p. H is low, the respiratory rate will be decreased, and if the p. H is high, the respiratory rate will be increased.

DISEASES and ABNORMALITIES ASSOCIATED WITH THE URINARY SYSTEM

ACIDOSIS 1. p. H below 7. 35 2. Depresses the nervous system.

ALKALOSIS 1. p. H above 7. 45. 2. Overexcites the nervous system.

RESPIRATORY ACIDOSIS Any condition that impairs breathing can cause respiratory acidosis. This can result in an increase in the amount of carbon dioxide in the blood and a reduction in the p. H.

RESPIRATORY ALKALOSIS Any condition that leads to hyperventilation cause respiratory alkalosis. This can result in an decrease in the amount of carbon dioxide in the blood and a increase in the p. H.

METABOLIC ACIDOSIS Metabolic acidosis is caused by excess acids in the blood. This can be the result of renal disease, diabetes mellitus, or a decrease in the number of bicarbonate ions in the blood.

METABOLIC ALKALOSIS Metabolic alkalosis is caused by a reduction in the amount of acid in the blood. This can be the result of vomiting, diuretics, or excessive bicarbonate ions in the blood.

SODIUM FUNCTIONS: 1. Attracts water into the ECF. 2. Nerve impulses. 3. Muscle contraction.

HYPERNATREMIA EXCESS SODIUM: 1. 2. 3. 4. Hypertension Muscle twitching Mental confusion Coma

HYPONATREMIA DEFICIENCY OF SODIUM: 1. Hypotension 2. Tachycardia 3. Muscle weakness

POTASSIUM FUNCTIONS: 1. Attracts water into the ICF. 2. Nerve impulse 3. Muscle contractions

HYPERKALEMIA EXCESS POTASSIUM: 1. Can lead to a cardiac arrhythmia 2. Elevated t waves 3. Muscle weakness

HYPOKALEMIA DEFICIENCY OF POTASSIUM: 1. Can lead to cardiac arrhythmia. 2. Depressed (flatened) t waves 3. Muscle weakness

CALCIUM FUNCTIONS: 1. Matrix of bones and teeth 2. Nerve impulse 3. Muscle contraction

HYPERCALCEMIA EXCESS CALCIUM: 1. Excess in calcium in blood 2. Kidney stones 3. Cardiac arrhythmia

HYPOCALCEMIA DEFICIENCY OF CALCIUM: 1. Tetany 2. Weak heart muscle contractions. 3. Increased clotting time.

URINARY DISEASES RENAL CALCULI (KIDNEY STONES) 1. Caused by the crystallization of Ca 2+ and Mg 2+ salts in the renal pelvis. 2. If the stone travel down the ureter, the patient will be in pain.

URINARY DISEASES CYSTITIS 1. Caused by bacteria, usually E. coli, Klebsiella, or Proteus. 2. Leads to inflammation, fever, increased urgency and frequency of urination and pain.

URINARY DISEASES GLOMERULONEPHRITIS: 1. Caused by inflammation of the glomerulus due to streptococcal antibody complexes. 2. Inflammation of the glomerulus leads to faulty filtration.

URINARY DISEASES INCONTINENCE: 1. Caused by loss of the ability to control voluntary micturition due to age, emotional disorders, pregnancy, or damage to the nervous system. 2. Leads to wet clothing.

URINARY DISEASES GOUT: 1. Caused by a increased blood level of uric acid. This leads to inflammation of the soft tissue associated with joints. 2. Decreased and painful movement.

ALDOSTERONISM EXCESS ALDOSTERONE: 1. Elevated sodium levels 2. Depressed potassium levels 3. Hypertension

ADDISON’S DISEASE DEFICIENCY OF ALDOSTERONE: 1. Hypotension 2. Low blood glucose levels. 3. Color of skin.

CUSHING’S SYNDROME EXCESSIVE GLUCOCORTICOIDS: 1. Hyperglycemia 2. Fat accumulation

DIABETES MELLITUS HYPOSECRETION OR ACTIVITY OF INSULIN: 1. 2. 3. 4. 5. Hyperglycemia Polyurea Thirst Body burns fat-ketones Vascular problems

INSULIN Cell Glucose Blood

DIABETES INSIPIDUS HYPOSECRETION OF ADH: 1. Increased urine volume. 2. Polyurea
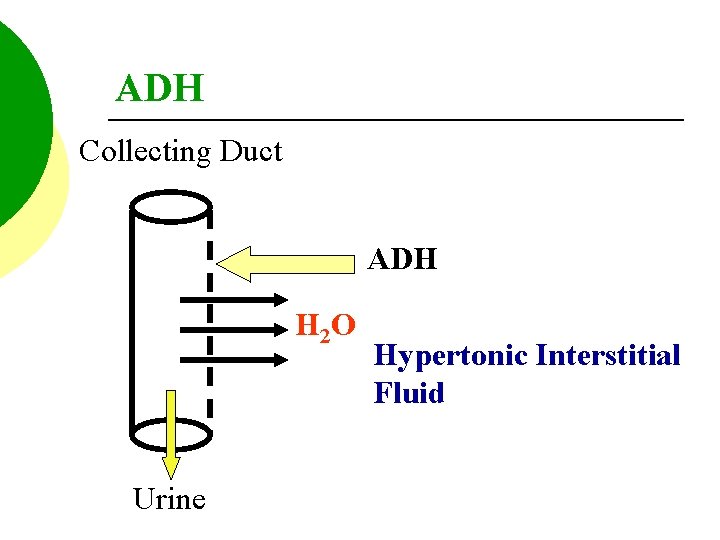
ADH Collecting Duct ADH H 2 O Urine Hypertonic Interstitial Fluid

DIALYSIS THERAPY Dialysis is a process that artificially removes metabolic wastes from the blood in order to compensate for kidney (renal) failure. Kidney failure results in the rapid accumulation of nitrogen waste (urea, etc. ). Uremia and ion disturbances can also occur. This condition cause acidosis, labored breathing, convulsions, coma and death.

DIALYSIS THERAPY The most common form of dialysisis hemodialysis which uses a machine to transfer patient’s blood through a semipermeable tube that is permeable only to selected substances. The dialysis machine contains an appropriate dialysis fluid that produces a diffusion gradient.

DIALYSIS THERAPY This gradient allows abnormal substances to diffuse from the patient’s blood and produce a “cleaning” effect. Medical ppt http: //hastaneciyiz. blogspot. com
- Slides: 187