Urinary System Ch 17 List the general functions





















- Slides: 32

Urinary System Ch 17

List the general functions of the organs of the urinary system. �Main function: Filter blood and remove salts and nitrogenous waste. �Maintains normal water and electrolyte concentration. �Regulates p. H and volume of body fluids. �Controls red blood cell production and blood pressure.

List the general functions of the organs of the urinary system. �Kidneys (2) – Remove substances from blood, form urine, and regulate RBC production. �Ureters (2) – Transport urine from kidneys to bladder. �Urinary bladder – Stores urine �Urethra – Conducts urine outside the body

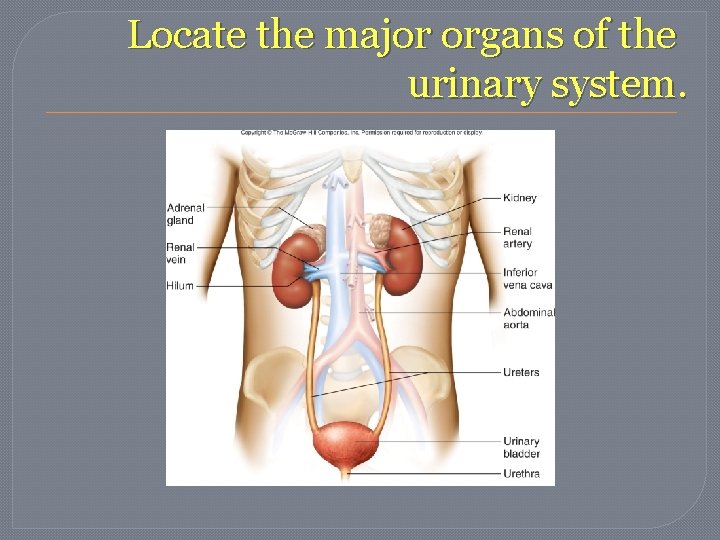
Locate the major organs of the urinary system.

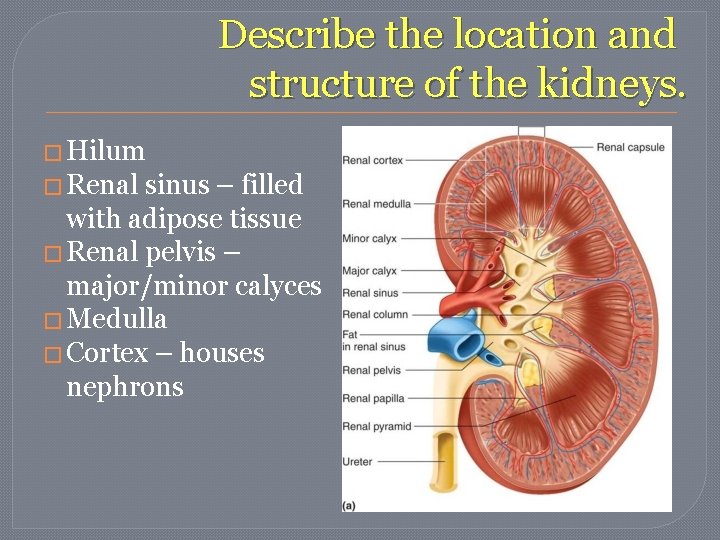
Describe the location and structure of the kidneys. �Location – either side of the vertebral column on posterior wall of the abdominal cavity �High – T 12 -L 3 ish Left is slightly higher than right. �Attached to inferior vena cava and abdominal aorta.

Describe the location and structure of the kidneys. � Hilum � Renal sinus – filled with adipose tissue � Renal pelvis – major/minor calyces � Medulla � Cortex – houses nephrons

List the functions of the kidneys. �Maintain homeostasis • Removes wastes from blood and dilute with water and electrolytes to form urine. �Secretes hormone erythropoietin – regulate RBC production �Activates Vitamin D �Maintains blood volume and pressure (enzyme: renin)

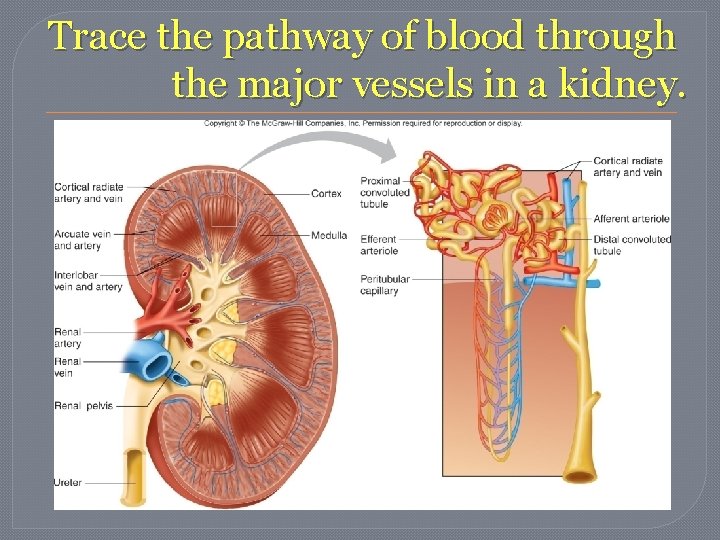
Trace the pathway of blood through the major vessels in a kidney. �abdominal aorta -> renal arteries -> (kidneys) interlobar arteries -> arcuate arteries -> interlobular arteries -> afferent arterioles-> (nephron glomerulus) -> efferent arteriole -> peritubular capillary system -> interlobular vein -> arcuate vein -> interlobar vein -> renal vein (exits kidney) -> inferior vena cava

Trace the pathway of blood through the major vessels in a kidney.

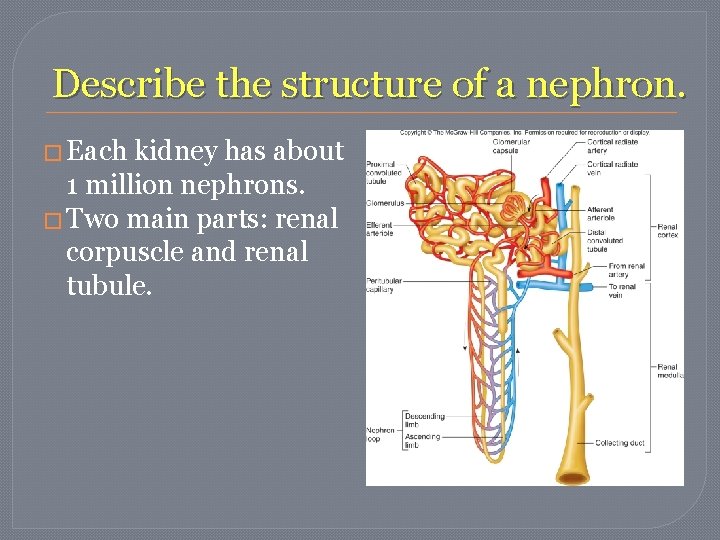
Describe the structure of a nephron. � Each kidney has about 1 million nephrons. � Two main parts: renal corpuscle and renal tubule.

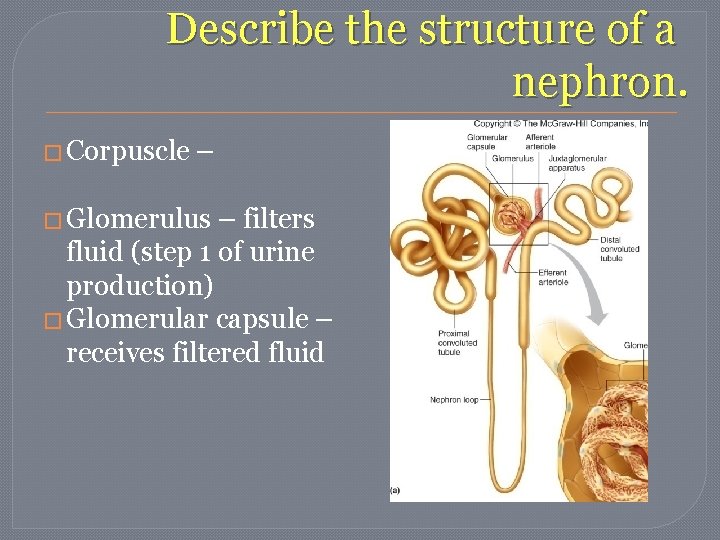
Describe the structure of a nephron. � Corpuscle – � Glomerulus – filters fluid (step 1 of urine production) � Glomerular capsule – receives filtered fluid

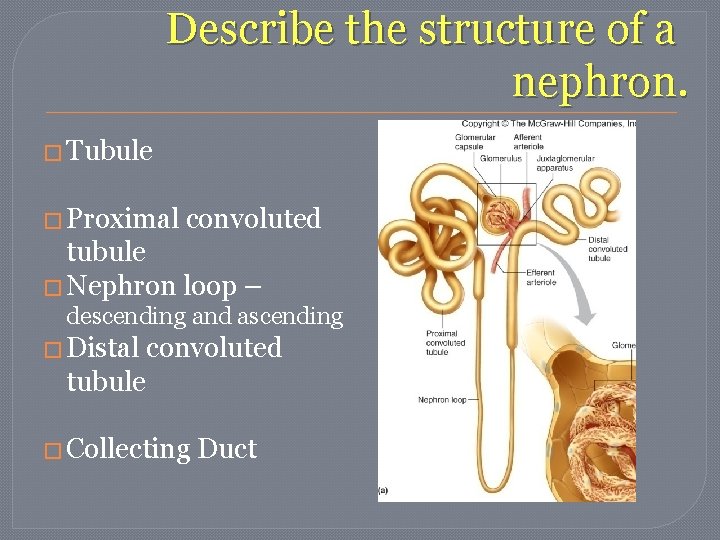
Describe the structure of a nephron. � Tubule � Proximal convoluted tubule � Nephron loop – descending and ascending � Distal convoluted tubule � Collecting Duct

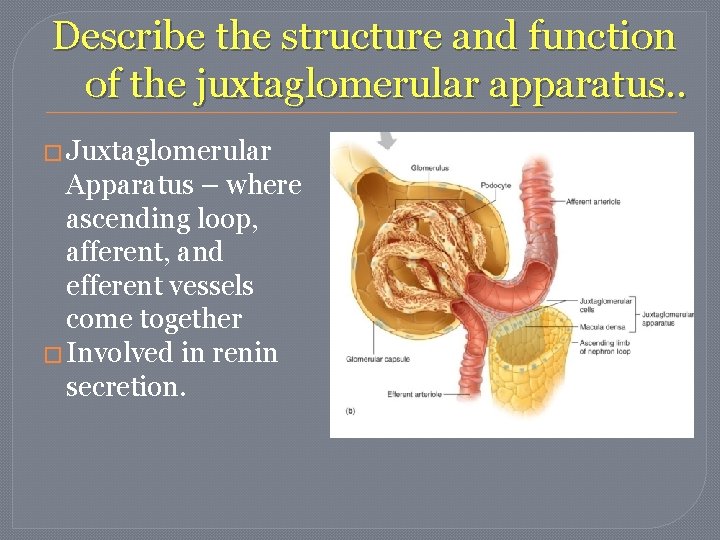
Describe the structure and function of the juxtaglomerular apparatus. . � Juxtaglomerular Apparatus – where ascending loop, afferent, and efferent vessels come together � Involved in renin secretion.

Urine Production �Urine formation happens through three processes: • Glomerular filtration • Tubular reabsorption • Tubular secretion �Amount of urine = amt. filtered-amt. reabsorbed + amt. secreted

Explain how glomerular filtrate is produced. �Glomerular capillaries in glomerulus filter water and other dissolved substances to create glomerular filtrate. �Glomerular filtrate moves to glomerular capsules.

Explain factors that affect the rate of glomerular filtration and how the rate is regulated. �Pressure is created by hydrostatic pressure of blood. �Pressure is decreased by osmotic pressure of plasma and hydrostatic pressure inside glomerular capsule. �Net filtration pressure = blood’s H-S P – (plasma’s osmotic P + glom. caps’s H-S P)

Explain factors that affect the rate of glomerular filtration and how the rate is regulated. � Glomerular filtration rate (GFR) – commonly used to measure kidney function. � Affected by changes in diameter of afferent or efferent arterioles. � Can also change due to kidney stones, enlarged prostate gland, etc.

Explain factors that affect the rate of glomerular filtration and how the rate is regulated. �Filtration Rate Regulation • Most of the time, it’s constant. • Increases when body fluids are excessive • Decreases when body needs to conserve fluids �Controlled by sympathetic nervous system reflexes. �Can also be affected by renin counts.

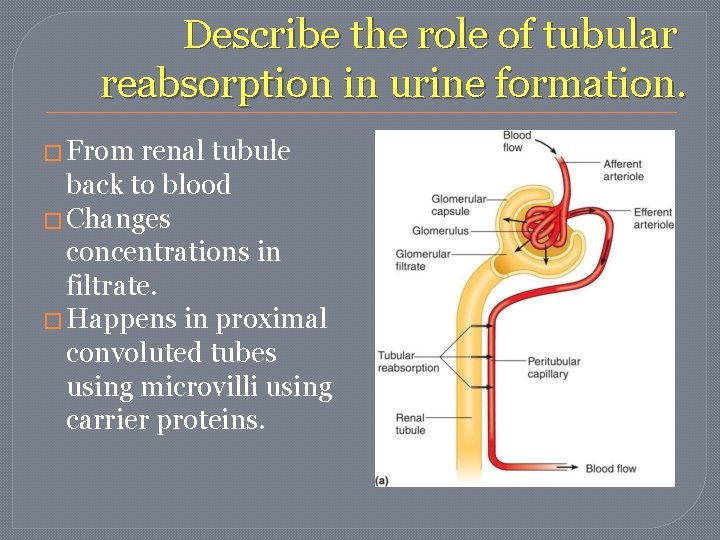
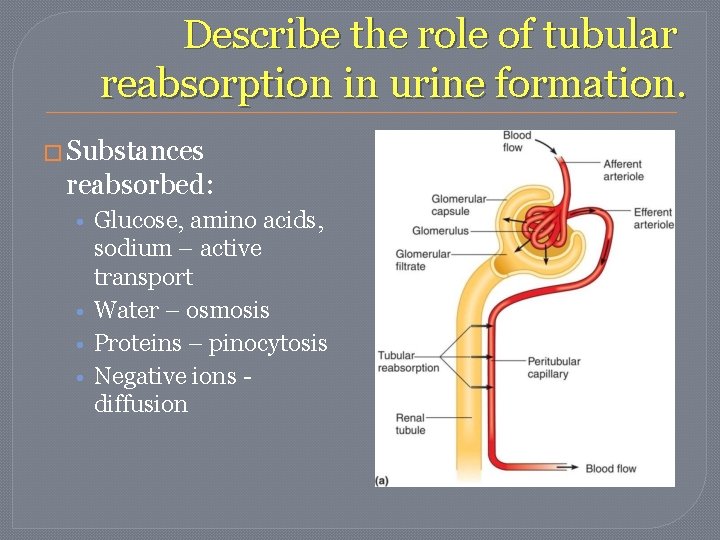
Describe the role of tubular reabsorption in urine formation. � From renal tubule back to blood � Changes concentrations in filtrate. � Happens in proximal convoluted tubes using microvilli using carrier proteins.

Describe the role of tubular reabsorption in urine formation. � Substances reabsorbed: • Glucose, amino acids, sodium – active transport • Water – osmosis • Proteins – pinocytosis • Negative ions diffusion

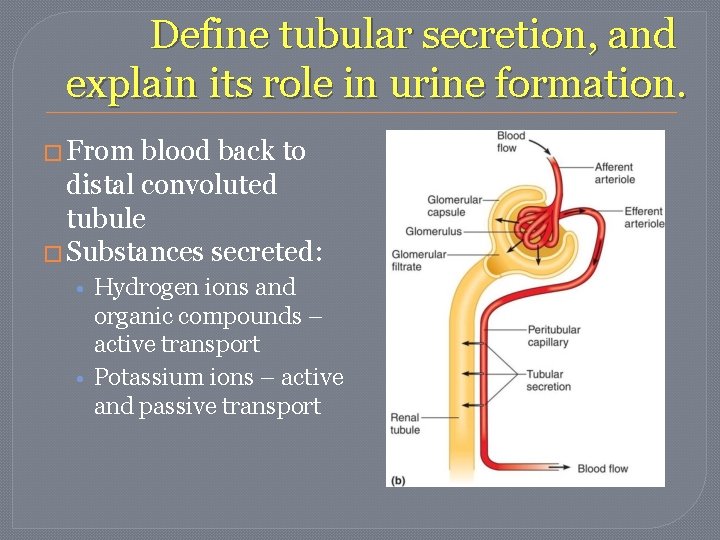
Define tubular secretion, and explain its role in urine formation. � From blood back to distal convoluted tubule � Substances secreted: • Hydrogen ions and organic compounds – active transport • Potassium ions – active and passive transport

Describe how urine concentrations are controlled. �Can be changed by presence of hormones • Aldosterone – secreted by adrenal glands (located posteriorly to kidneys); stimulates reabsorption of sodium and secretion of potassium. • ADH – secreted by neurons in hypothalamus; responds to decrease in water concentration or blood volume; causes water to be reabsorbed; negative feedback system. �Increased ADH=more water reabsorption �Decreased ADH=less water reabsorption

Describe normal urine composition. �Urea – made by amino acid catabolism; reflects amount of protein in diet; 20% leaves/80% reabsorbed �Uric acid – product of metabolism of nucleic acids; small amounts secreted into renal tubule and excreted in urine.

Describe normal urine composition. �Determined by the amount of water in diet and plasma. �Changes with changes in diet and metabolic activity.

Describe normal urine composition. �Should • • not have Glucose – sign of diabetes or large glucose intake. Proteins – may be there after strenuous exercise Ketones – after a prolonged fast Blood – sign of disease or disorder

Describe how urine is eliminated. �From collecting tubes in renal medulla �To ureter �To urinary bladder �To urethra

Describe how urine is eliminated. �Ureters - From renal pelvis to bottom of urinary bladder. �Three layers • Mucous coat – inside • Muscular coat – middle (smooth muscle) • Fibrous coat – connective tissue �Flap-like fold acts as valve allowing urine to enter bladder without backflow

Describe how urine is eliminated. �Urinary bladder – hollow, distendable, muscular organ �Stores urine and forces into urethra �Four layers • Mucous coat – inner layer (transitional epithelium) • Submucous coat • Muscular coat – smooth muscle fiber called detrusor muscle • Serous coat – outer layer

Describe how urine is eliminated. �Internal urethral sphincter • Sustained contraction keeps bladder from emptying • Detrusor muscle innervated with parasympathetic nerve fibers �External urethral sphincter • Voluntary skeletal muscle

Describe how urine is eliminated. �Micturition – Urination �Stimulated by distension of bladder triggering micturition reflex center • Controlled by pons and hypothalamus �Urge felt at about 150 m. L �Powerful contractions felt at 300 m. L �Pain felt at about 600 m. L

Describe how urine is eliminated. �Urethra – tube that conveys urine to outside �Female – 4 cm �Male – shared by urinary and reproductive system

Diagram Quiz � Kidneys � Nephron � Ureters � Urinary bladder � Urethra � Renal vein � Renal artery � Distal convoluted tube � Proximal convoluted tube loop � Glomerular capsule � Glomerulus � Renal cortex � Renal medullary