Urinary Incontinence Mixed Urge Stress Jan BusbyWhitehead MD

Urinary Incontinence Mixed Urge Stress Jan Busby-Whitehead, MD Chief, Division of Geriatric Medicine University of North Carolina

Definition of Urinary Incontinence “ The involuntary loss of urine which is objectively demonstrable and a social or hygienic problem. ” * The International Continence Society University of North Carolina School of Medicine Center for Aging and Health
URINARY INCONTINENCE Common Treatable Significant Effect on Quality of Life (Qo. L) University of North Carolina School of Medicine Center for Aging and Health
Prevalence • Community: 17% older men, up to 30% older women • Hospital: up to 50% older men and women • LTCF: 50 -70% older men and women University of North Carolina School of Medicine Center for Aging and Health
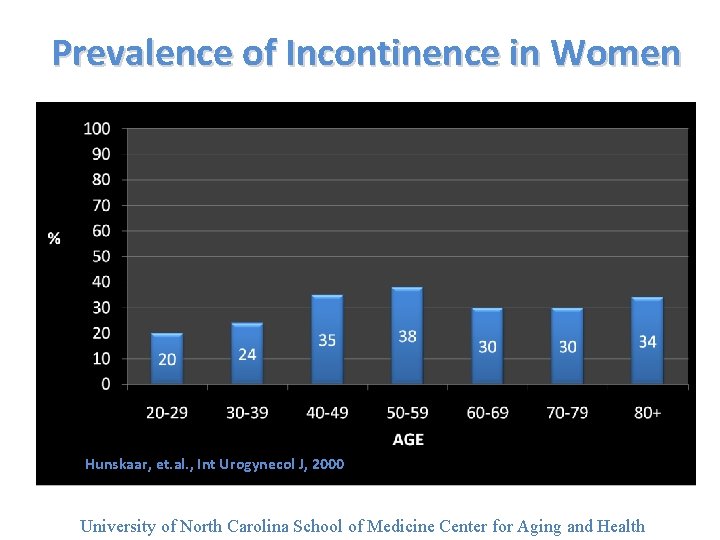
Prevalence of Incontinence in Women Hunskaar, et. al. , Int Urogynecol J, 2000 University of North Carolina School of Medicine Center for Aging and Health
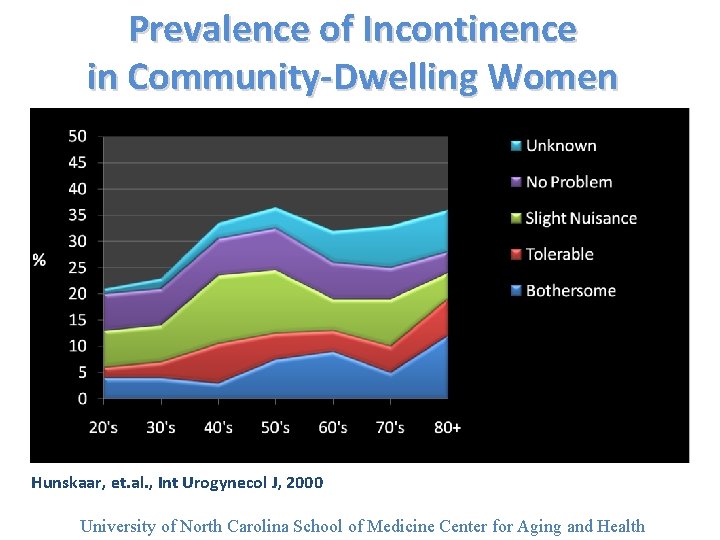
Prevalence of Incontinence in Community-Dwelling Women Hunskaar, et. al. , Int Urogynecol J, 2000 University of North Carolina School of Medicine Center for Aging and Health

Reversible causes of UI D R I P - Delirium or Drugs - Restricted mobility - Infection, impaction - Polyuria University of North Carolina School of Medicine Center for Aging and Health
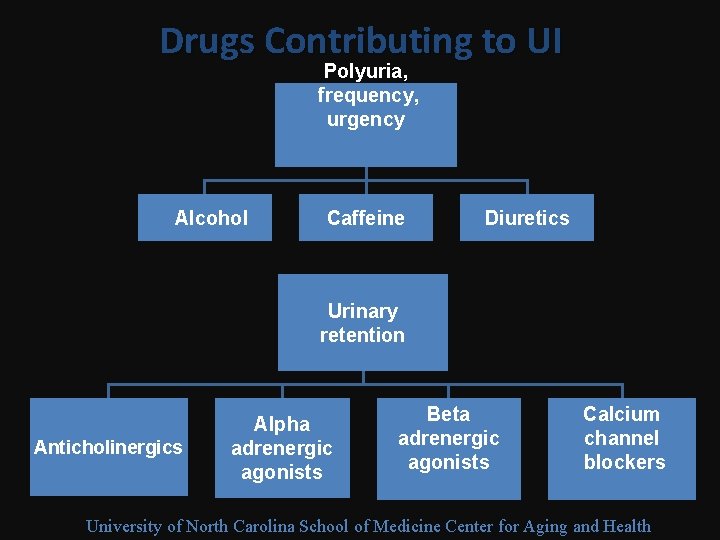
Drugs Contributing to UI Polyuria, frequency, urgency Alcohol Caffeine Diuretics Urinary retention Anticholinergics Alpha adrenergic agonists Beta adrenergic agonists Calcium channel blockers University of North Carolina School of Medicine Center for Aging and Health
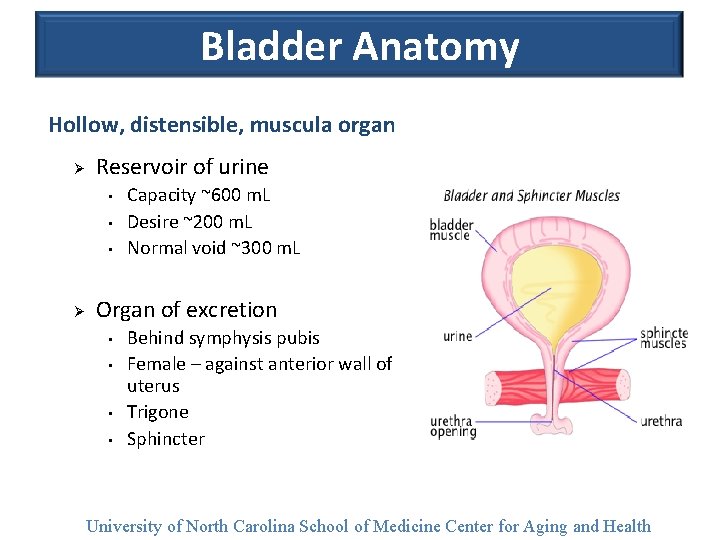
Bladder Anatomy Hollow, distensible, muscula organ Ø Reservoir of urine • • • Ø Capacity ~600 m. L Desire ~200 m. L Normal void ~300 m. L Organ of excretion • • Behind symphysis pubis Female – against anterior wall of uterus Trigone Sphincter University of North Carolina School of Medicine Center for Aging and Health
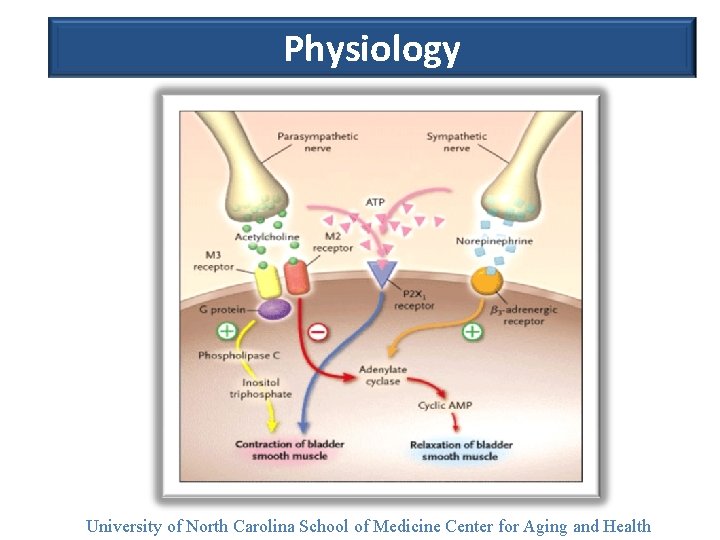
Physiology University of North Carolina School of Medicine Center for Aging and Health

Aging Changes • Decreased bladder capacity • Reduced voiding volume • Reduced flow rates • Increased urine production at night * Nordling, J Experimental Gerontology, 2002, 37: 991 University of North Carolina School of Medicine Center for Aging and Health
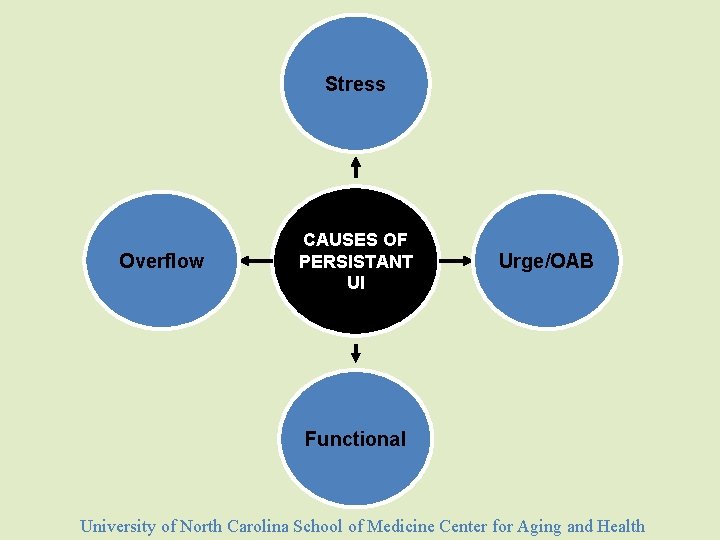
Stress Overflow CAUSES OF PERSISTANT UI Urge/OAB Functional University of North Carolina School of Medicine Center for Aging and Health
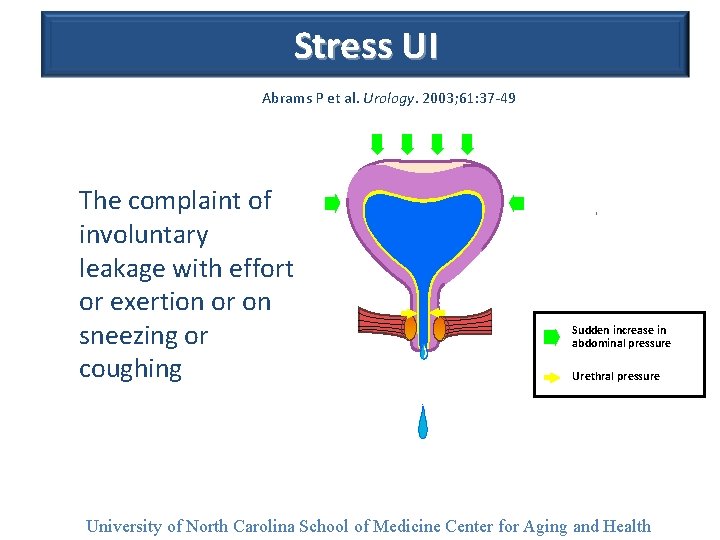
Stress UI Abrams P et al. Urology. 2003; 61: 37 -49. The complaint of involuntary leakage with effort or exertion or on sneezing or coughing Sudden increase in abdominal pressure Urethral pressure University of North Carolina School of Medicine Center for Aging and Health
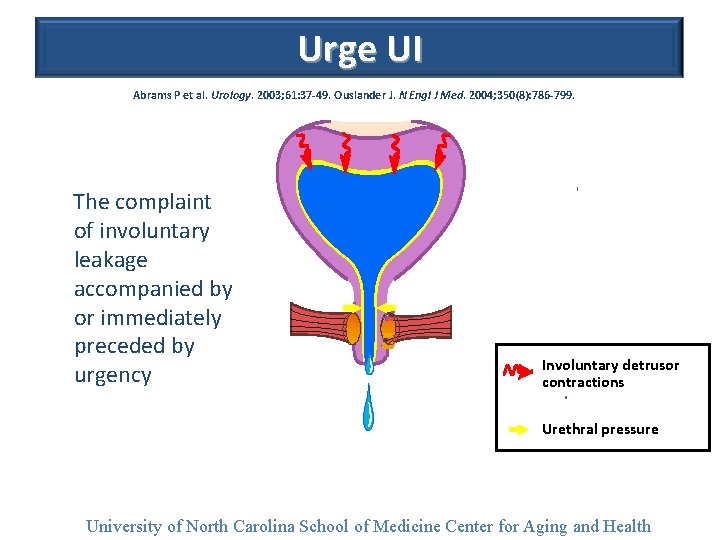
Urge UI Abrams P et al. Urology. 2003; 61: 37 -49. Ouslander J. N Engl J Med. 2004; 350(8): 786 -799. The complaint of involuntary leakage accompanied by or immediately preceded by urgency Involuntary detrusor contractions Urethral pressure University of North Carolina School of Medicine Center for Aging and Health

Overactive bladder • Includes urinary urgency with or without urge incontinence, urinary frequency, and nocturia • Associated with involuntary contractions of the detrusor muscle University of North Carolina School of Medicine Center for Aging and Health
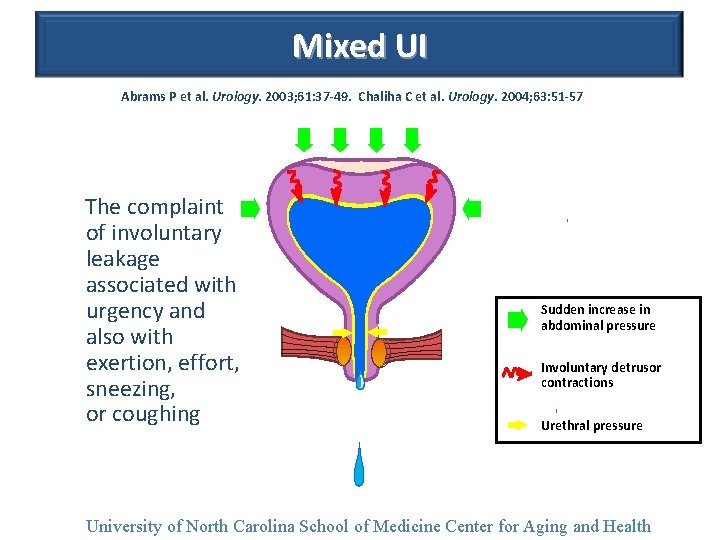
Mixed UI Abrams P et al. Urology. 2003; 61: 37 -49. Chaliha C et al. Urology. 2004; 63: 51 -57. The complaint of involuntary leakage associated with urgency and also with exertion, effort, sneezing, or coughing Sudden increase in abdominal pressure Involuntary detrusor contractions Urethral pressure University of North Carolina School of Medicine Center for Aging and Health
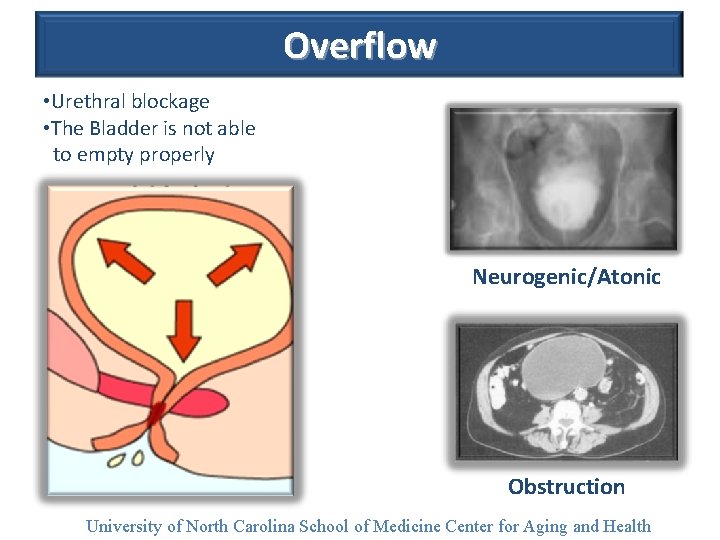
Overflow • Urethral blockage • The Bladder is not able to empty properly Neurogenic/Atonic Obstruction University of North Carolina School of Medicine Center for Aging and Health

Functional Incontinence • Immobility • Diminished vision • Aphasia • Environment • Psychological University of North Carolina School of Medicine Center for Aging and Health

Clinical Questions ? How do you evaluate for incontinence? ? Are behavioral techniques effective? For which patients? ? What drug treatments are useful and how do you use them? University of North Carolina School of Medicine Center for Aging and Health

Office Evaluation of UI • Identify presence of UI • Assess for reversible causes and treat • If UI persistent, determine type and initiate treatment • Identify patient who needs further evaluation and referral University of North Carolina School of Medicine Center for Aging and Health

Basic Evaluation of UI • History: Bladder diary • Physical examination, especially Genitourinary and Neurological • Bladder stress test • Postvoid residual • Urinalysis, urine culture if indicated • BUN, creatinine, fasting glucose University of North Carolina School of Medicine Center for Aging and Health

Referral Criteria ü Recurrent urinary tract infections ü Hematuria ü Elevated postvoid residual or other evidence of possible obstruction ü Recent gynecological or urological surgery or pelvic radiation ü Failed treatment of stress or urge UI University of North Carolina School of Medicine Center for Aging and Health

Cystometry • Gold standard for diagnosis • New definition for detrusor overactivity: Any rise in detrusor pressure during filling cystometry associated with symptoms and not related to abnormal bladder compliance • Provocative stimuli • Ambulatory monitoring University of North Carolina School of Medicine Center for Aging and Health

Treatment Options • Behavioral • Pharmacological • Functional Electrical Stimulation • Surgery University of North Carolina School of Medicine Center for Aging and Health

Are behavioral techniques effective? For whom? • Behavioral techniques are effective for treatment of stress and urge UI, and overactive bladder, but generally do not cure • Behavioral techniques are effective in community dwelling men and women • Behavioral techniques are most appropriate for cognitively intact, motivated persons University of North Carolina School of Medicine Center for Aging and Health
Behavioral Treatments for UI BEHAVIORAL TREATMENTS FOR UI Self management techniques Timed or scheduled voiding Pelvic floor muscle exercise with or without biofeedback University of North Carolina School of Medicine Center for Aging and Health

Self Management • Fluid Intake – Don’t reduce amount – Do not drink fluids 2 hr before bedtime – Avoid: caffeine, alcohol, nicotine University of North Carolina School of Medicine Center for Aging and Health

Scheduled Voiding • Scheduled voiding with systematic delay of voiding – Schedule based on time interval pt can manage in daytime – Void at scheduled time even if urge not present; suppress urge if not time with “Quick Kegels” – Increase voiding interval by 30 min each week until continent for up to 4 hr University of North Carolina School of Medicine Center for Aging and Health

Pelvic Muscle Exercises • Isolation of the pelvic muscles • Avoidance of abdominal, buttock or thigh muscle contractions • Moderate repetitions of strongest contraction possible • Ability to hold contraction 10 seconds, repeat in groups of 10 -30 TID University of North Carolina School of Medicine Center for Aging and Health
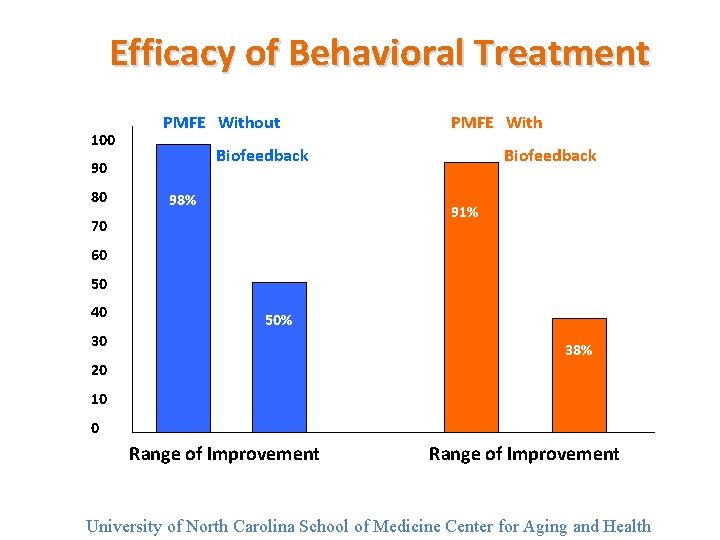
Efficacy of Behavioral Treatment 100 PMFE Without Biofeedback 90 80 PMFE With 98% Biofeedback 91% 70 60 50 40 50% 30 38% 20 10 0 Range of Improvement University of North Carolina School of Medicine Center for Aging and Health

Randomized Trials of Behavioral Treatment for Stress UI • 24 RCTs, but only 11 of high quality • Pelvic floor exercises were effective (up to 75%)in reducing symptoms of stress UI • Limited evidence for high vs low intensity • Benefits of adding biofeedback unclear * Berghmans et al. Br J Urol 1998: 82: 181 -191 University of North Carolina School of Medicine Center for Aging and Health

Behavioral Treatment for Urge/OAB • Bladder training – Initial approach – 3 RCT: 47 -90% cure rate with 6 mo f/u – Recurrence in 43 -58% after 2 -3 yr – 35% fewer UI episodes vs controls: Cochrane Review 2004 University of North Carolina School of Medicine Center for Aging and Health

Limitations of Behavioral Treatment Studies • Studies varied in – types of UI – characteristics of subjects – intervention strategies – outcome measures used – duration of follow-up • Few studies compared the efficacy of PFME performed with and without biofeedback University of North Carolina School of Medicine Center for Aging and Health

NIH Treatment Trial Kincade, Dougherty, Busby-Whitehead Purpose: • Compare pelvic floor muscle exercises alone to PFME plus biofeedback in women with stress and mixed urge and stress UI • Design – 315 women randomized to 3 groups, including an attention control group – Followup up at 2 weeks, 6 months, 1 year University of North Carolina School of Medicine Center for Aging and Health

Drug Treatment for UI: What Works • Stress UI – Alpha adrenergic agents? – Estrogen? – Combination therapy? University of North Carolina School of Medicine Center for Aging and Health

Alpha Adrenergic Drugs • Phenylpropanoloamine – – – • Once a first line drug 8 randomized controlled trials Study duration: 2 -6 weeks % cure: 0 -14 % side effects: 5 -33% WITHDRAWN FROM MARKET due to report of hemorrhagic stroke University of North Carolina School of Medicine Center for Aging and Health

Duloxetine (Cymbalta) • FDA application for stress UI withdrawn • Warning for liver dysfunction, alcohol University of North Carolina School of Medicine Center for Aging and Health

Estrogen • Combined study with Phenylpropanolamine suggested improvement in combination • Improves urogenital atrophy • Heart and Estrogen/Progestin Replacement Study 2001: 4 yr, randomized trial, 2763 postmenopausal women <80 given combined HRT or placebo for ischemic heart disease. – 55% had >1 episode UI/week – HRT group had worsening stress and urge UI sx University of North Carolina School of Medicine Center for Aging and Health

Drug Treatment of Overactive Bladder • Anticholinergic Drugs are mainstay – Oxybutynin IR 2. 5 -5 mg bid-qid – Ditropan XL 5 -20 mg daily – Oxytrol patch TDS 3. 9 mg 2 x/wk – Tolterodine tartrate IR 1 -2 mg bid – Detrol LA 2 -4 mg daily New Drugs: – Trospium chloride (Sanctura) 20 mg bid – Darifenicin (Enablex) 7. 5 -15 mg daily – Solefenicin (Vesicare) 5 -10 mg daily University of North Carolina School of Medicine Center for Aging and Health

Muscarinic Receptors • M 1 – Brain (cortex, hippocampus), salivary • glands, sympathetic ganglia • M 2 – Heart, hindbrain, smooth muscle (80% of detrusor) • M 3 – Smooth muscle (20% of detrusor), salivary glands, brain, eye (lens, iris) • M 4 – Brain (forebrain, striatum) • M 5 – Brain (substantia nigra), eye University of North Carolina School of Medicine Center for Aging and Health
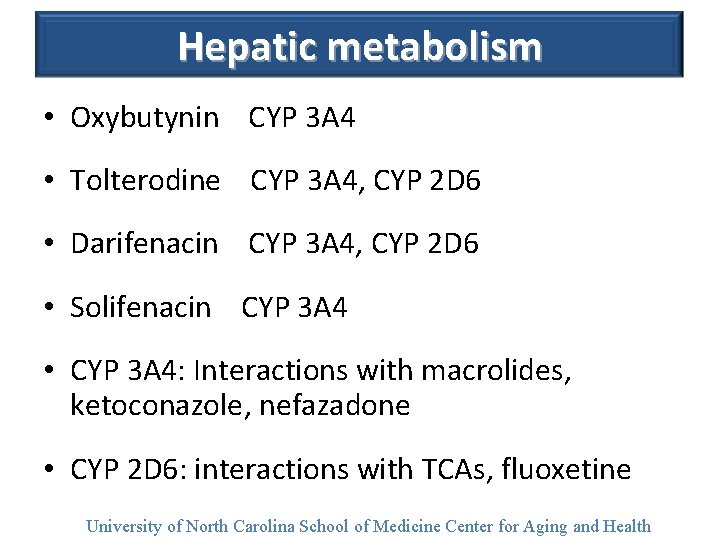

Hepatic metabolism • Oxybutynin CYP 3 A 4 • Tolterodine CYP 3 A 4, CYP 2 D 6 • Darifenacin CYP 3 A 4, CYP 2 D 6 • Solifenacin CYP 3 A 4 • CYP 3 A 4: Interactions with macrolides, ketoconazole, nefazadone • CYP 2 D 6: interactions with TCAs, fluoxetine University of North Carolina School of Medicine Center for Aging and Health

Behavioral vs Drug Rx for Urge UI in Older Women • Randomized, controlled trial by Burgio et al JAMA 1998; 280; 1995 -2000 • 197 women aged 55 -92 • 8 weeks of BFB, 8 weeks of oxybutynin • 2. 5 to 5 mg qd to tid, or placebo control • All 3 groups reduced UI frequency • Effectiveness: BFB>drug>placebo University of North Carolina School of Medicine Center for Aging and Health
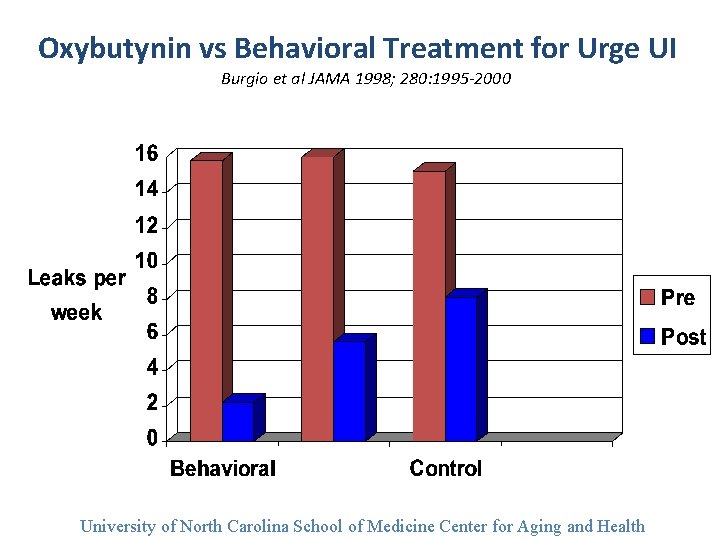
Oxybutynin vs Behavioral Treatment for Urge UI Burgio et al JAMA 1998; 280: 1995 -2000 University of North Carolina School of Medicine Center for Aging and Health

Oxybutynin • Both anticholinergic and smooth muscle relaxant properties • 6/7 RCTs show benefit • 15 -58% greater reduction in urge UI than placebo • Dose: 2. 5 -5 mg qd-qid, 20 mg/d maximum University of North Carolina School of Medicine Center for Aging and Health

Oxybutynin Controlled Release • Once daily dosing • RCT showed rate of daytime continence similar to that for immediate release (53 vs 58%) • Lower rate of dry mouth than immediate release form University of North Carolina School of Medicine Center for Aging and Health

Tolterodine tartrate • Pure muscarinic receptor antagonist • Dry mouth most common side effect • 3 RCT compared tolterodine (2 mg bid) to oxybutynin (5 mg tid): Equally effective and superior to placebo • Decreased urge U(I in study of 293 pts: 47% tolterodine, 71% oxybutynin, 19% placebo, dry mouth 86% oxybutynin, 50% tolerodine University of North Carolina School of Medicine Center for Aging and Health

OBJECT Study Appel et al Mayo Clin Proc 2001: 76 • Compared efficacy and tolerability of extended release oxybutynin and tolterodine tartrate • 12 weeks • Prospective randomized, double-blind, parallel group study • 276 women and 56 men • Oxybutynin more effective for weekly urge UI, total incontinence, and urinary frequency University of North Carolina School of Medicine Center for Aging and Health

Trospium • Dose 20 mg bid • Renal metabolism • Nonselective for muscarinic receptors • Effective for detrusor overactivity in placebocontrolled double-blind studies: • Trospium 20 mg bid vs tolterodine 2 mg bid in 232 pts reduced voiding frequency and number of UI episodes • Dry mouth 7% and 9% respectively University of North Carolina School of Medicine Center for Aging and Health

Darifenicin • Dose 7. 5 to 15 mg daily • Selective M 3 receptor antagonist • Several RCTs • Mundy et al 2001 Randomized double-blind trial compared darifenacin 15 mg and 30 mg to oxybutynin 5 mg tid in 25 pts , similar efficacy • Side effects: Dry mouth, constipation(<2%) University of North Carolina School of Medicine Center for Aging and Health

Solefenacin • Dose 5 to 10 mg daily • Long acting muscarinic receptor antagonist, selective for M 3 • Undergoes hepatic metabolism involving cytochrom P 450 • Several multinational trials with over 800 pts, vs placebo, showed efficacy low side effects (2% dry mouth) University of North Carolina School of Medicine Center for Aging and Health
Urinary retention Gastric retention Cardiac arrhythmias Contraindications for Anticholinergics Bladder outlet obstruction Narrow angle glaucoma University of North Carolina School of Medicine Center for Aging and Health

Desmopressin • Decreases urine production • Helps nocturia • Dose: 20 -40 mcg intranasal spray q hs • Double-blind crossover trial showed decreased nighttime voids vs placebo, 1. 9 vs 2. 6 • Contraindications: CHF, HTN, ASCVD University of North Carolina School of Medicine Center for Aging and Health

Functional Electrical Stimulation • Frequency of 10 -50 Hertz for 15 -20 minutes daily • RCT: 50% cured after 8 weeks compared to sham controls • 52 -77% symptomatic improvement in short-term studies, non RCT • Implantable electrodes at S 2 -3, 76% improvement for refractory urge UI x 18 mo • BUT 33% required surgical revision University of North Carolina School of Medicine Center for Aging and Health

Surgery for Urge/OAB • If behavioral and pharmacological treatments don’t work • Augmentation enterocystoplasty • One series of 267 patients had a 93% continence rate with 3 yr f/u • Complications: urinary retention, stones, small bowel obstruction, reservoir rupture University of North Carolina School of Medicine Center for Aging and Health

Treatment of Overflow UI Due to Mild BPH • Alpha adrenergic antagonists – – Possibly relaxes prostate smooth muscle and stroma and urethra smooth muscle to increase urine flow Tamsulosin, doxazosin, terazosin Tamsulosin trials: 53 weeks, 31% and 36% improvement in maximal flow rate with 0. 4 mg and 0. 8 mg/day vs 21% placebo Uroselective alfuzosin in late stage clinical trials University of North Carolina School of Medicine Center for Aging and Health

Drug Treatment of Mild BPH • Type II 5 alpha reductase inhibitor – – Results in atrophy of the prostatic glandular epithelium due to decreased synthesis of dihydrotestosterone Slow onset, 20 -30% reduction in prostate volume and LUTS over time Side effects: Ejaculatory dysfunction (8%), loss of libido (10%), erectile dysfunction (16%) Finasteride , Dutasteride University of North Carolina School of Medicine Center for Aging and Health

Summary • Behavioral treatment is effective for treating stress and urge UI and OAB • Drugs are effective for treating urge UI and OAB and mild BPH • New selective agents for urge and OAB based on new understanding of bladder and urethral function • Caution needed in dosing, especially in older patients University of North Carolina School of Medicine Center for Aging and Health
- Slides: 57