Urinary Incontinence in Women December 2017 Taken from

Urinary Incontinence in Women December 2017 Taken from NICE guidance 2015 Amy Micklethwaite GP Linthorpe surgery

Learning Objectives 1. To have an approach to a patient presenting with urge incontinence in line with nice guidance 2. To have an approach to a patient presenting with stress incontinence in line with nice guidance 3. To have an approach to a patient presenting with mixed incontinence in line with nice guidance 4. To know the 2 week rule criteria for referral in this presenting population 5. To have an idea of what is likely to happen once a patient has been referred, in order to give the patient further information.

Plan for the session 1. Boring slide bit- the NICE guidance 2. Break into groups- approach to a patient presenting with incontinence 3. Back together to discuss this 4. COFFEE aimed 3. 10 -3. 30 5. Cases & quizzes in groups 6. Back together to present our views 7. Feedback 8. Home 16. 30

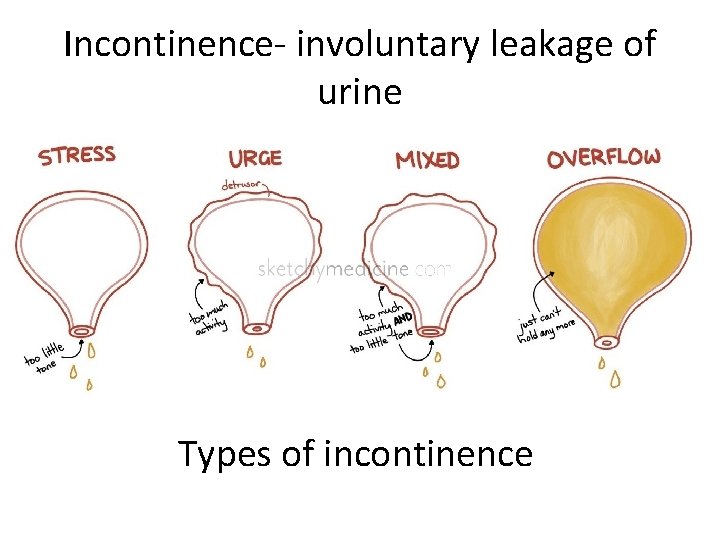
Incontinence- involuntary leakage of urine Types of incontinence
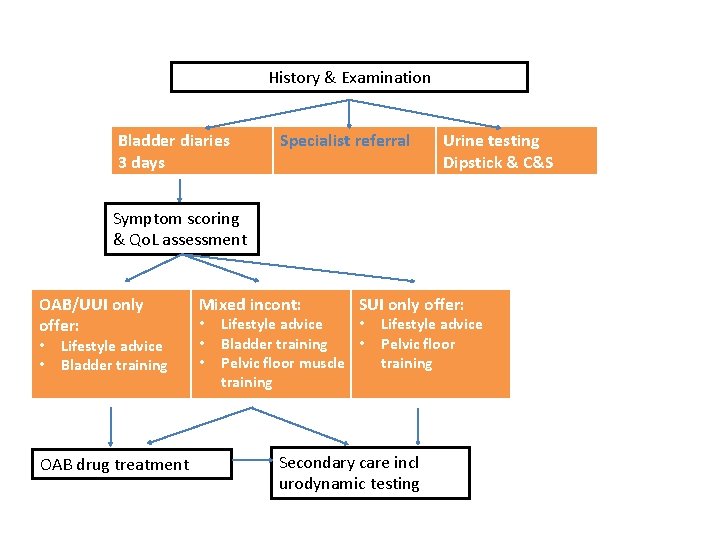
History & Examination Bladder diaries 3 days Specialist referral Urine testing Dipstick & C&S Symptom scoring & Qo. L assessment OAB/UUI only offer: • • Lifestyle advice Bladder training OAB drug treatment Mixed incont: • • • SUI only offer: Lifestyle advice • Bladder training • Pelvic floor muscle training Lifestyle advice Pelvic floor training Secondary care incl urodynamic testing

Specialist referral: 2 week rule Renal tract Cancer • >45 yrs with frank haematuria without UTI • >45 yrs with frank haematuria which recurs after UTI treatment. • >60 yrs with microscopic haematuria AND EITHER dysuria or raised WBC. • (Routine referral for >60 yrs with recurrent UTIs) Ovarian cancer • Ascites • Pelvic/abdominal mass • Check urgent Ca 125 (USS) especially if >50 yrs if frequent/persistant: – – – Bloating Early satiety/loss of appetite Pelvic/abdominal pain Increased urinary urge/frequency New IBS Consider if: • Unexplained weight loss • Fatigue • Bowel changes

Specialist Referral – Symptomatic pelvic organ prolapse that is visible at or below the introitus. – A palpable bladder – Persistent bladder or urethral pain (refer urgently if cancer is suspected). – A pelvic mass that is clinically benign, such as uterine fibroids. – Associated faecal incontinence. – Suspected or known neurological disease. – A history of previous prolapse surgery, incontinence surgery, pelvic cancer surgery, or previous radiation therapy. – Recurrent urinary tract infection. – Microscopic (non-visible) haematuria in a woman who is <60 not fulfilling the 2 wk rule. • Refer to a renal physician if there is also proteinuria or raised serum creatinine levels. • Refer non-urgently to a urologist if there is no proteinuria and serum creatinine level is normal. – Suspected or known acute kidney injury (AKI) — refer to a nephrologist, urgent or same day referral may be required.
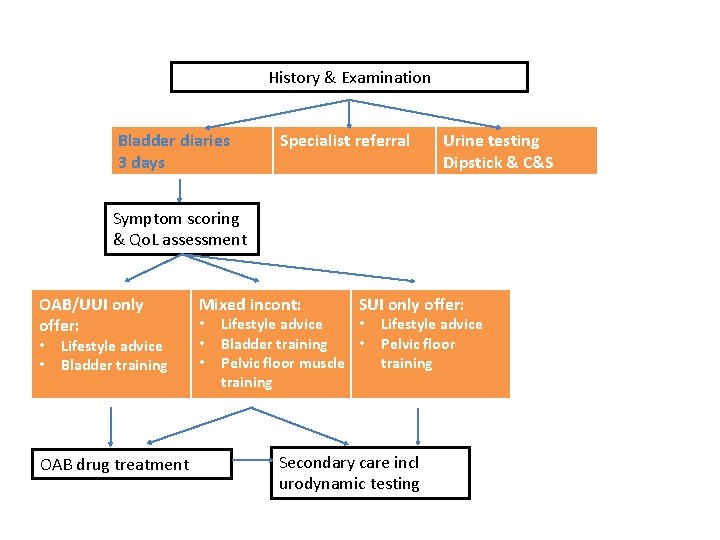
History & Examination Bladder diaries 3 days Specialist referral Urine testing Dipstick & C&S Symptom scoring & Qo. L assessment OAB/UUI only offer: • • Lifestyle advice Bladder training OAB drug treatment Mixed incont: • • • SUI only offer: Lifestyle advice • Bladder training • Pelvic floor muscle training Lifestyle advice Pelvic floor training Secondary care incl urodynamic testing
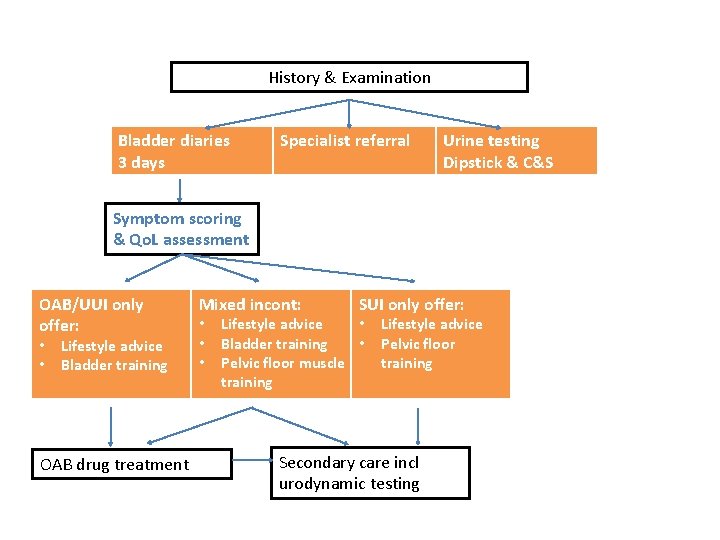
History & Examination Bladder diaries 3 days Specialist referral Urine testing Dipstick & C&S Symptom scoring & Qo. L assessment OAB/UUI only offer: • • Lifestyle advice Bladder training OAB drug treatment Mixed incont: • • • SUI only offer: Lifestyle advice • Bladder training • Pelvic floor muscle training Lifestyle advice Pelvic floor training Secondary care incl urodynamic testing
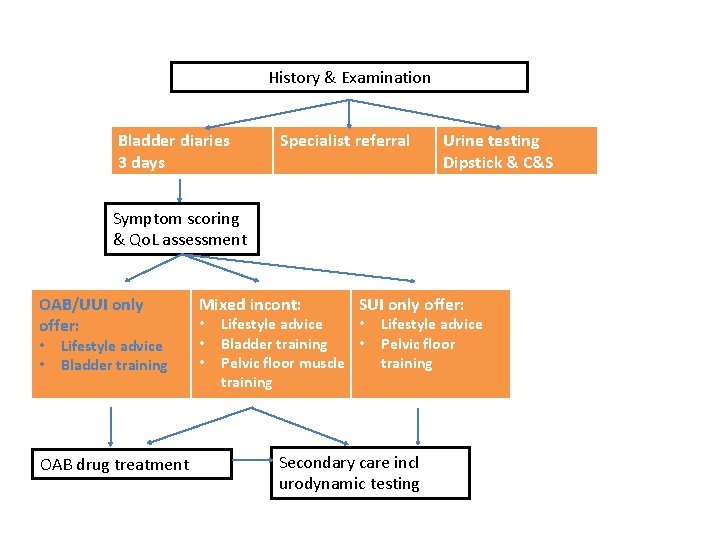
History & Examination Bladder diaries 3 days Specialist referral Urine testing Dipstick & C&S Symptom scoring & Qo. L assessment OAB/UUI only offer: • • Lifestyle advice Bladder training OAB drug treatment Mixed incont: • • • SUI only offer: Lifestyle advice • Bladder training • Pelvic floor muscle training Lifestyle advice Pelvic floor training Secondary care incl urodynamic testing


OAB/UUI only offer: • Lifestyle advice • Bladder training 1. Lifestyle advice Reversible causes or contributing factors 2. Bladder training Minimum 6 weeks. Refer to incontinence service.
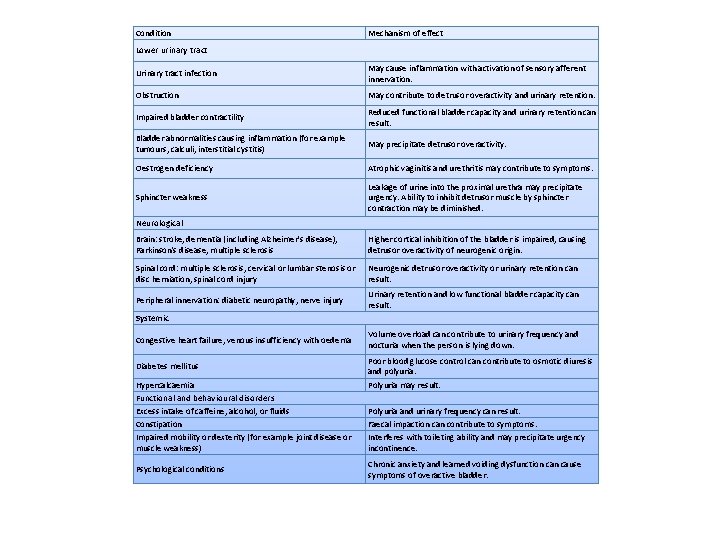
Condition Mechanism of effect Lower urinary tract Urinary tract infection May cause inflammation with activation of sensory afferent innervation. Obstruction May contribute to detrusor overactivity and urinary retention. Impaired bladder contractility Reduced functional bladder capacity and urinary retention can result. Bladder abnormalities causing inflammation (for example tumours, calculi, interstitial cystitis) May precipitate detrusor overactivity. Oestrogen deficiency Atrophic vaginitis and urethritis may contribute to symptoms. Sphincter weakness Leakage of urine into the proximal urethra may precipitate urgency. Ability to inhibit detrusor muscle by sphincter contraction may be diminished. Neurological Brain: stroke, dementia (including Alzheimer's disease), Parkinson's disease, multiple sclerosis Higher cortical inhibition of the bladder is impaired, causing detrusor overactivity of neurogenic origin. Spinal cord: multiple sclerosis, cervical or lumbar stenosis or disc herniation, spinal cord injury Neurogenic detrusor overactivity or urinary retention can result. Peripheral innervation: diabetic neuropathy, nerve injury Urinary retention and low functional bladder capacity can result. Systemic Congestive heart failure, venous insufficiency with oedema Diabetes mellitus Hypercalcaemia Functional and behavioural disorders Excess intake of caffeine, alcohol, or fluids Constipation Impaired mobility or dexterity (for example joint disease or muscle weakness) Psychological conditions Volume overload can contribute to urinary frequency and nocturia when the person is lying down. Poor blood glucose control can contribute to osmotic diuresis and polyuria. Polyuria may result. Polyuria and urinary frequency can result. Faecal impaction can contribute to symptoms. Interferes with toileting ability and may precipitate urgency incontinence. Chronic anxiety and learned voiding dysfunction cause symptoms of overactive bladder.

Lifestyle advice – Reducing caffeine intake — improve urgency and frequency – Fluid intake — avoid drinking excessive amounts or reduced amounts The recommended daily intake is six to eight glasses of water. Avoiding alcohol, citrus drinks, fizzy drinks. – Weight loss - if BMI >30 kg/m 2 – Smoking if appropriate —chronic cough may contribute to stress urinary incontinence
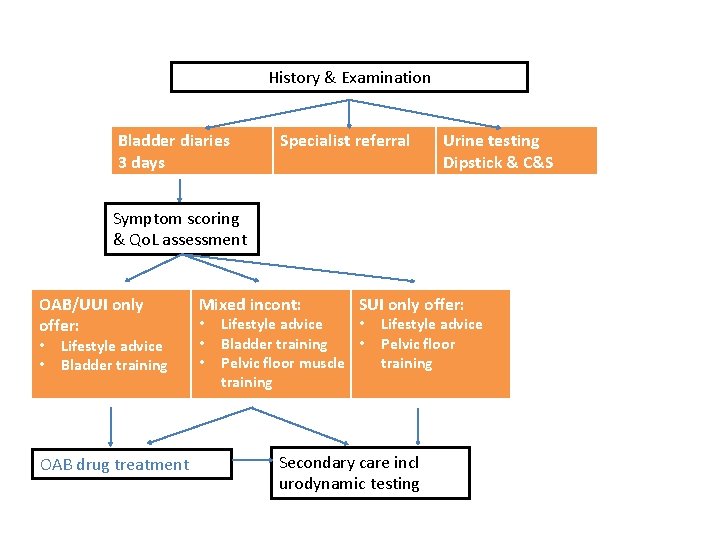
History & Examination Bladder diaries 3 days Specialist referral Urine testing Dipstick & C&S Symptom scoring & Qo. L assessment OAB/UUI only offer: • • Lifestyle advice Bladder training OAB drug treatment Mixed incont: • • • SUI only offer: Lifestyle advice • Bladder training • Pelvic floor muscle training Lifestyle advice Pelvic floor training Secondary care incl urodynamic testing

OAB drug treatment • Anticholinergic (antimuscarinic) Oxybutynin (immediate release) Tolterodine (immediate release) Darifenacin (once daily preparation) can be used first-line. – transdermal oxybutynin for women who are unable to take oral medication – DO NOT offer immediate release oxybutynin to frail older women due to the risk of impairment of daily functioning and delirium Mirabegron – Add in topical vaginal oestrogen if atrophy present – Consider adding desmopressin if troublesome nocturia

OAB drug treatment continued… • Counsel patients – Takes time to work – Side effects- anticholinergic load, dry mouth, constipation, retention if poor bladder emptying – May need to increase dose – Can stay on longterm • Review at 4 weeks: – If okay review at 12 weeks then annually (or 6 m or elderly – If not helping, try alternative antimuscarinic, consider mirabegron or referral
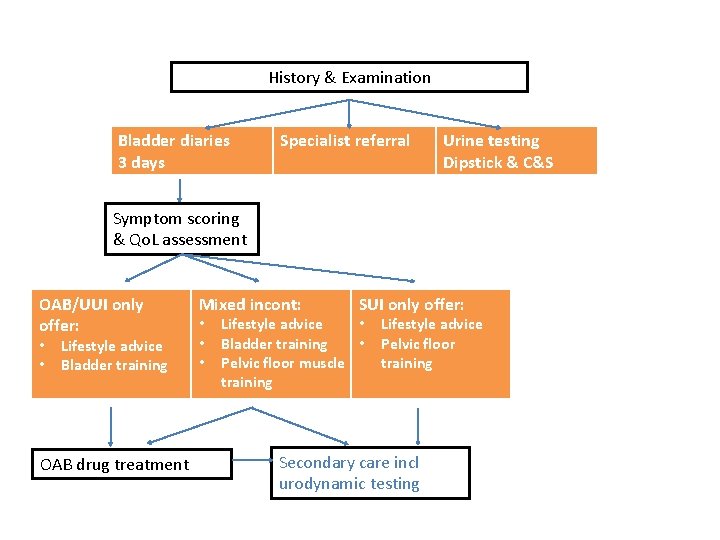
History & Examination Bladder diaries 3 days Specialist referral Urine testing Dipstick & C&S Symptom scoring & Qo. L assessment OAB/UUI only offer: • • Lifestyle advice Bladder training OAB drug treatment Mixed incont: • • • SUI only offer: Lifestyle advice • Bladder training • Pelvic floor muscle training Lifestyle advice Pelvic floor training Secondary care incl urodynamic testing

Secondary care incl urodynamic testing If conservative treatments fail or if the woman wants further management, consider referring to urology/gynae for: Intermittant self catheterisation Botulinum toxin A Percutaneous sacral nerve stimulation Percutaneous posterior tibial nerve stimulation if the woman does not want botulinum toxin A or sacral nerve stimulation – Augmentation cystoplasty – Urinary diversion – –
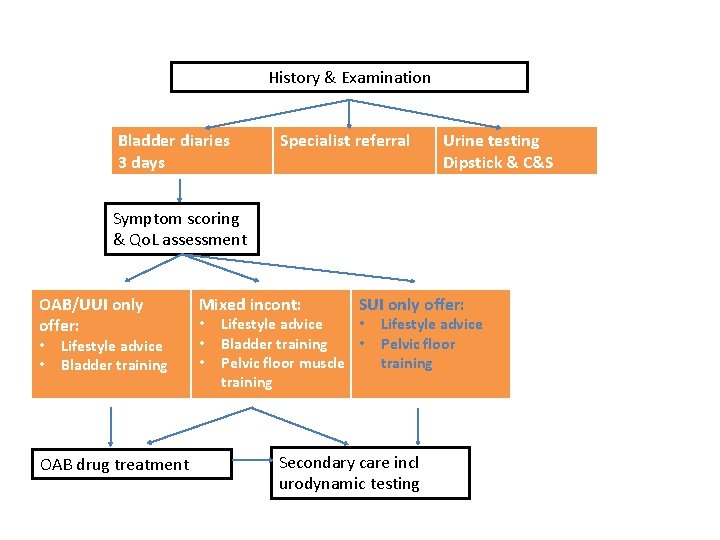
History & Examination Bladder diaries 3 days Specialist referral Urine testing Dipstick & C&S Symptom scoring & Qo. L assessment OAB/UUI only offer: • • Lifestyle advice Bladder training OAB drug treatment Mixed incont: • • • SUI only offer: Lifestyle advice • Bladder training • Pelvic floor muscle training Lifestyle advice Pelvic floor training Secondary care incl urodynamic testing


SUI only offer: ● Lifestyle advice ● Pelvic floor training 1. Lifestyle advice – Caffeine – Fluid intake – Weight loss – Smoking if this is appropriate — eg chronic cough which may contribute to stress urinary incontinence Give advice on reversible causes or contributing factors- as before

Lifestyle advice- self help info – NHS Choices provides online information for people with urinary incontinence. – The Bladder and Bowel Foundation has a helpline (telephone 01536 533 255) and provides a range of resources on their website (www. bladderandbowelfoundation. org).

2. Pelvic floor training • Offer referral for a programme of supervised pelvic floor muscle training (PFMT) – continence nurses locally – Should last at least 3 months – >8 pelvic floor muscle contractions >3 x/day. – Patient info at www. csp. org. uk (pdf) Pads & toileting aids should only be offered whilst awaiting treatment, if all treatment failed or severe cognitive or mobility impairment.
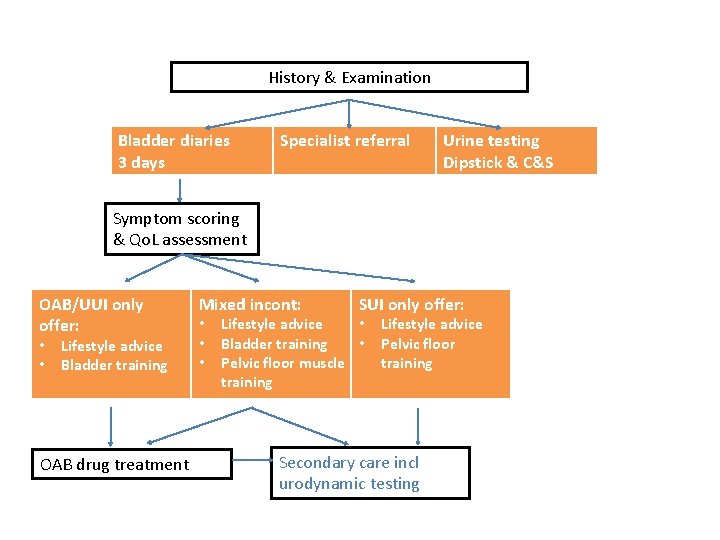
History & Examination Bladder diaries 3 days Specialist referral Urine testing Dipstick & C&S Symptom scoring & Qo. L assessment OAB/UUI only offer: • • Lifestyle advice Bladder training OAB drug treatment Mixed incont: • • • SUI only offer: Lifestyle advice • Bladder training • Pelvic floor muscle training Lifestyle advice Pelvic floor training Secondary care incl urodynamic testing

Secondary care • If conservative treatments fail or if the woman wants further management, consider: – Referring to gynae/urology • Treatment options in secondary care include – – – synthetic mid-urethral tape, colposuspension, autologous rectus fascial sling, intramural urethral bulking agents, or an artificial urinary sphincter. – Offer duloxetine as a second-line treatment, but only if the woman prefers drug to surgical treatment or is not suitable for surgical treatment.

References • http: //cks. nice. org. uk/incontinence-urinary-inwomen
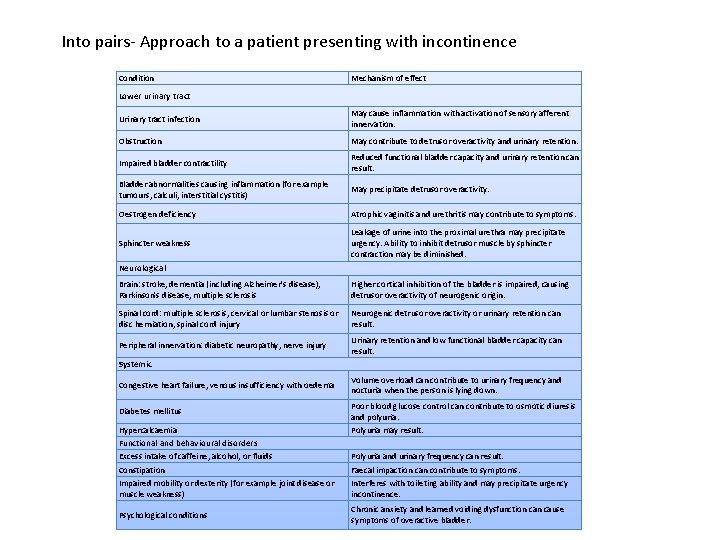
Into pairs- Approach to a patient presenting with incontinence Condition Mechanism of effect Lower urinary tract Urinary tract infection May cause inflammation with activation of sensory afferent innervation. Obstruction May contribute to detrusor overactivity and urinary retention. Impaired bladder contractility Reduced functional bladder capacity and urinary retention can result. Bladder abnormalities causing inflammation (for example tumours, calculi, interstitial cystitis) May precipitate detrusor overactivity. Oestrogen deficiency Atrophic vaginitis and urethritis may contribute to symptoms. Sphincter weakness Leakage of urine into the proximal urethra may precipitate urgency. Ability to inhibit detrusor muscle by sphincter contraction may be diminished. Neurological Brain: stroke, dementia (including Alzheimer's disease), Parkinson's disease, multiple sclerosis Higher cortical inhibition of the bladder is impaired, causing detrusor overactivity of neurogenic origin. Spinal cord: multiple sclerosis, cervical or lumbar stenosis or disc herniation, spinal cord injury Neurogenic detrusor overactivity or urinary retention can result. Peripheral innervation: diabetic neuropathy, nerve injury Urinary retention and low functional bladder capacity can result. Systemic Congestive heart failure, venous insufficiency with oedema Diabetes mellitus Hypercalcaemia Functional and behavioural disorders Excess intake of caffeine, alcohol, or fluids Constipation Impaired mobility or dexterity (for example joint disease or muscle weakness) Psychological conditions Volume overload can contribute to urinary frequency and nocturia when the person is lying down. Poor blood glucose control can contribute to osmotic diuresis and polyuria. Polyuria may result. Polyuria and urinary frequency can result. Faecal impaction can contribute to symptoms. Interferes with toileting ability and may precipitate urgency incontinence. Chronic anxiety and learned voiding dysfunction cause symptoms of overactive bladder.
- Slides: 29