URINALYSIS AND BODY FLUIDS SEROUS FLUIDS Dr Essam

URINALYSIS AND BODY FLUIDS (SEROUS FLUIDS) Dr. Essam H. Jiffri 1

SEROUS FLUIDS The closed cavities of the body mammal; the pleural, pericardial, and peritoneal cavities are each liner by two membranes referred to as the serous membranes. 2
3

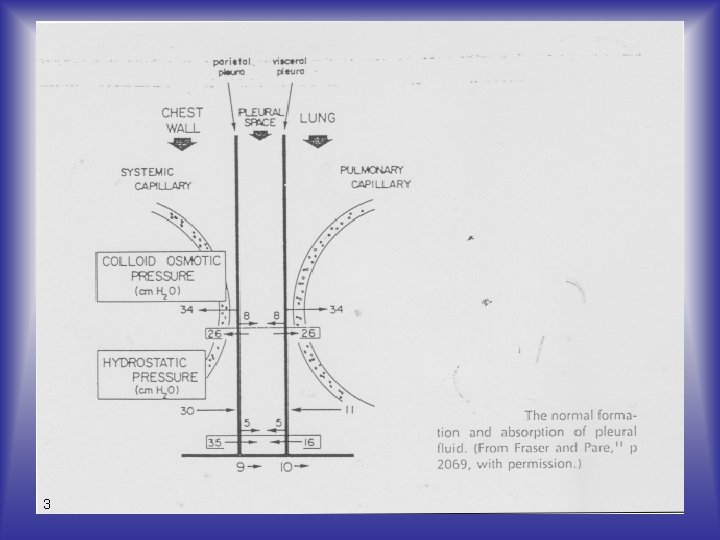
SEROUS FLUIDS One membrane lines the cavity wall (parietal membrane), and the other covers the organs within the cavity (visceral membrane). The fluid between the membranes which provides lubrication as the surfaces move against each other, is called serous fluid. 4

SEROUS FLUIDS Normally only a small amount of serous fluid is present because production and absorption take place at a constant rate. 5

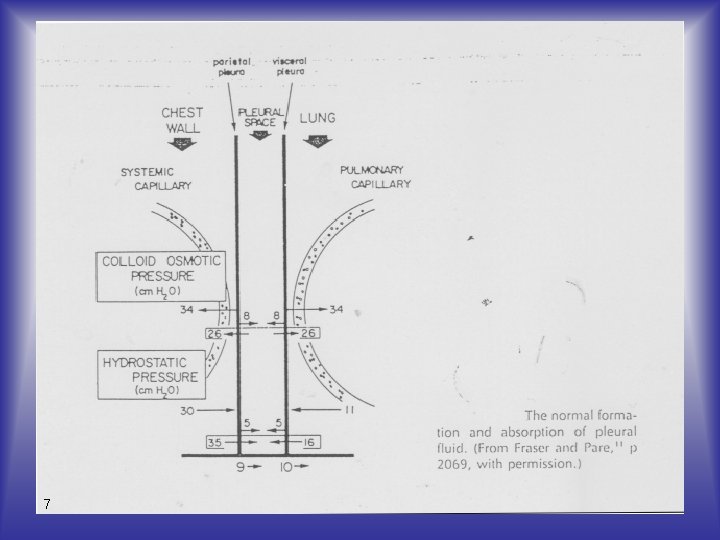
Formation Serous fluids are formed as ultrafiltrates of plasma, with no additional material contributed by the membrane cells. Production and reabsorption are subject to hydrostatic and colloidal (oncotic) pressures from the capillaries serving the cavities under normal conditions. 6
7

Formation The greater hydrostatic pressure in the systemic capillaries on the parietal side favors fluid production through the parietal membrane and reabsorption through the visceral membrane. 8

Formation Fluids for laboratory examination are collected by needle aspiration from the respective cavities. These aspiration procedures are referred to as: Ø thoracentesis (pleural) Ø pericardiocentesis(pericardial). Ø paracentesis (peritoneal). 9

Formation Abundant fluid is usually collected; therefore, suitable specimens are available for each section of the laboratory. An anti coagulated specimen is needed for cell counts, a sterile tube for culture. Large volumes of fluid should be prepared prior to microbiologic and cytologic examinations 10

General Laboratory Procedures Routine fluid examination including classification as a transudate or exudate, appearance, cell count, differential, chemistry and microbiology procedures is performed in the same manner on all serous fluids. 11

General Laboratory Procedures Cell counts are usually performed manually using the Neubauer counting chamber. Differential counts are performed on (Wright stained smears). Any suspicious cells been on the differential should be referrer to the cytology laboratory or the pathologist. 12

Summary of Serous Fluid Testing Pleural Fluid Normal appearance: Clear, pale yellow Turbidity: White blood cells and microorganisms Blood: Traumatic injury, malignancy, traumatic tap Milky: Chylous or pseudochylous material Neutrophils: Bacterial infection Lymphocytes: Tuberculosis, malignancy Normal glucose: Parallels serum glucose Low glucose: Tuberculosis, rheumatoid inflammation, malignancy Low p. H: Tuberculosis, malignancy, esophageal rupture Elevated amylase: Pancreatitis 13

Summary of Serous Fluid Testing Pericardial Fluid Normal appearance: Clear, pale yellow Milky: Lymphatic drainage Turbidity: Infection, malignancy Blood: Tuberculosis, tumor, cardiac puncture Neutrophils: Bacterial endocarditis Low glucose: Bacterial infection, malignancy 14

Summary of Serous Fluid Testing Peritoneal Fluid Normal appearance: Clear, pale yellow Turbidity: Peritonitis, cirrhosis Blood: Trauma Neutrophils: Peritonitis Low glucose: Tubercular peritonitis, malignancy Elevated amylase: Pancreatitis, gastrointestinal perforation Elevated alkaline phosphatase: Intestinal perforation Elevated urea or creatinine: Ruptured bladder 15

TRANSUDATES AND EXUDATES Many pathologic conditions can cause a buildup (effusion) of serous fluid. A general classification of the cause of the effusion can be accomplished by separating the fluid into the category of transudate or exudate. 16

TRANSUDATES AND EXUDATES Exudates are produced by conditions that directly involve the membranes of the particular cavity, including infections, malignancies and from an inflammatory process. Transudates also can be thought of as resulting from a mechanical process, 17

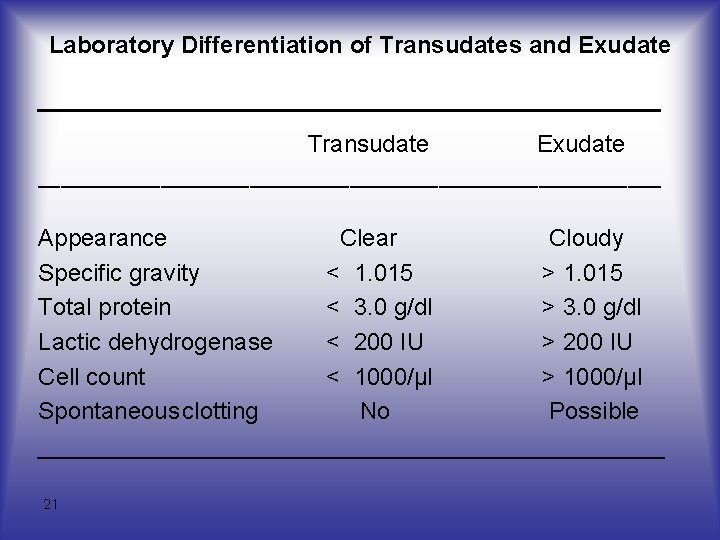
TRANSUDATES AND EXUDATES A variety of laboratory tests have been used to differentiate between transudates and exudates, including appearance, specific gravity, total protein, lactic dehydrogenase, cell counts, and spontaneous clotting. 18

TRANSUDATES AND EXUDATES As can be seen using these criteria, one would expect a transudate to be a clear fluid with a specific gravity less than 1. 015, protein less than 3. 0 g per dl, and a lactic dehydrogenase below 200 IU. 19

TRANSUDATES AND EXUDATES Traditionally, specific gravity and protein were considered to be the most valuable criteria for classification. In recent years, the lactic dehydrogenase has replaced the specific gravity. 20
Laboratory Differentiation of Transudates and Exudate __________________ Transudate Exudate ____________________________ Appearance Clear Cloudy Specific gravity < 1. 015 > 1. 015 Total protein < 3. 0 g/dl > 3. 0 g/dl Lactic dehydrogenase < 200 IU > 200 IU Cell count < 1000/µl > 1000/µl Spontaneous clotting No Possible ________________________ 21
- Slides: 21