Upper GI bleeding University of Jordan UPPER GI
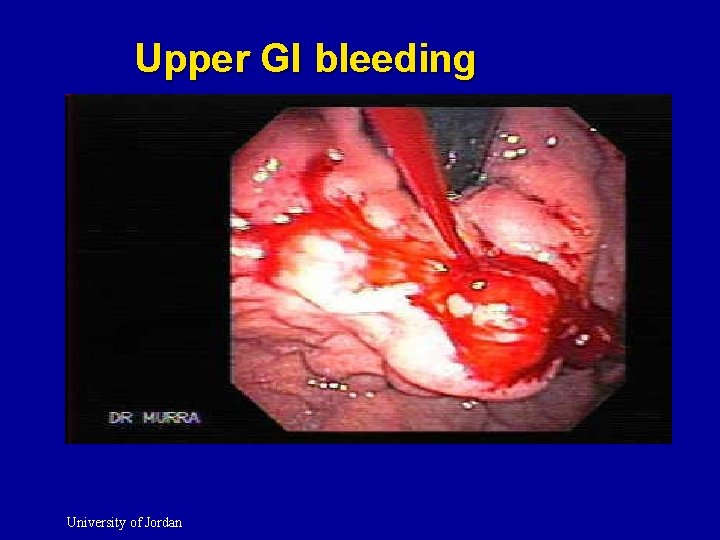
Upper GI bleeding University of Jordan

UPPER GI BLEEDING Signs and Symptoms l l l Hematemesis Melena Dizziness Abd. Pain and symptoms of Peptic ulcer disease Hx of NSAID’s use University of Jordan l l Pallor Hypotension Orthostasis Jaundice and other stigmatas of chronic liver diseases

UPPER GI BLEEDING CAUSES RARE CAUSES Unknown 5% Rare 5% GU 20% Varices 15% Mallory Weiss 5% Erosions 25% University of Jordan DU 25% Neoplasms GU AVM/Ectasia DU Dieulafoy’s Erosions Mallory Weiss Stoma ulcers Esophageal ulcers Varices Rare Deodenitis Unknown Hemobilia Aorto-enteric fistulas

UPPER GI BLEEDING Peptic Ulcer Disease l l l Defect in the GI mucosa extending through the muscularis mucosa. Decreasing incidence. Caused by imbalance between the aggressive and defensive factors. University of Jordan

UPPER GI BLEEDING Peptic Ulcer Disease l l Helicobacter Pylori NSAID’s Acid Hypersecretory state. Antral G cell Hyperplasia University of Jordan
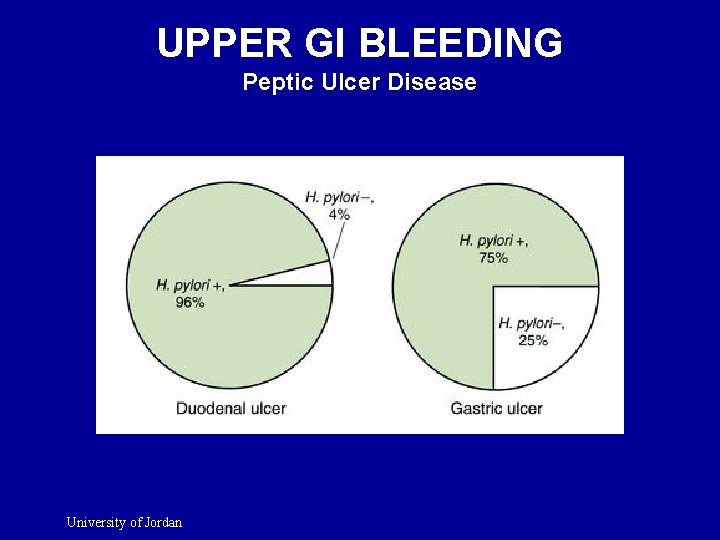
UPPER GI BLEEDING Peptic Ulcer Disease University of Jordan

UPPER GI BLEEDING Gastric Ulcers University of Jordan
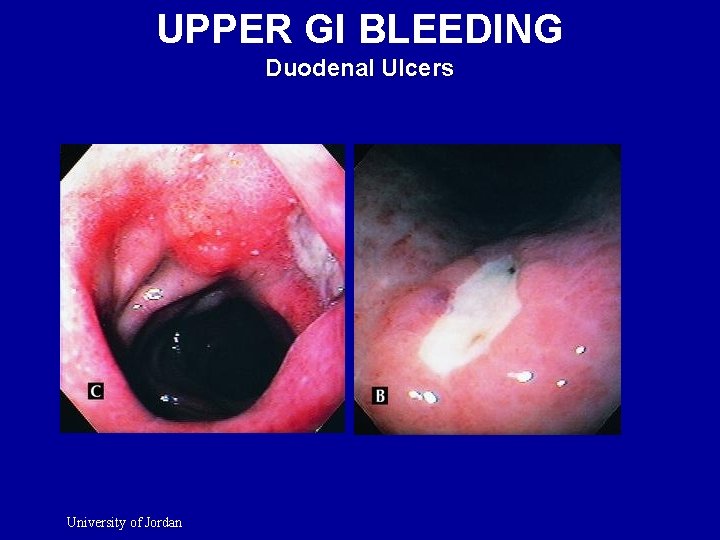
UPPER GI BLEEDING Duodenal Ulcers University of Jordan
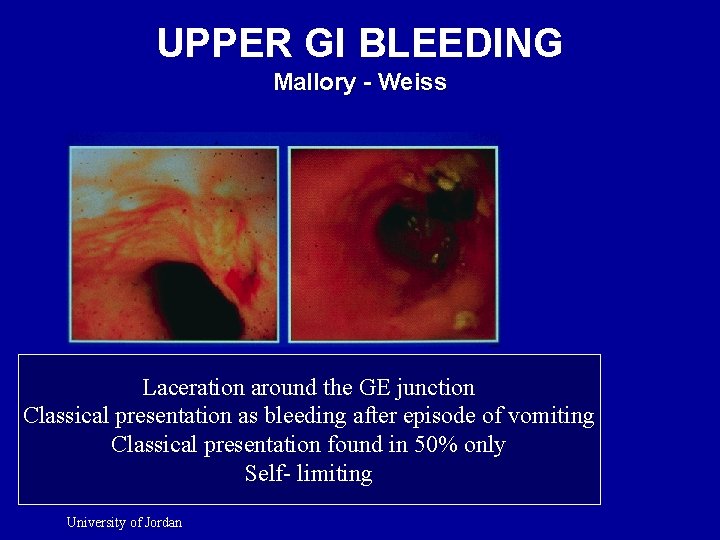
UPPER GI BLEEDING Mallory - Weiss Laceration around the GE junction Classical presentation as bleeding after episode of vomiting Classical presentation found in 50% only Self- limiting University of Jordan
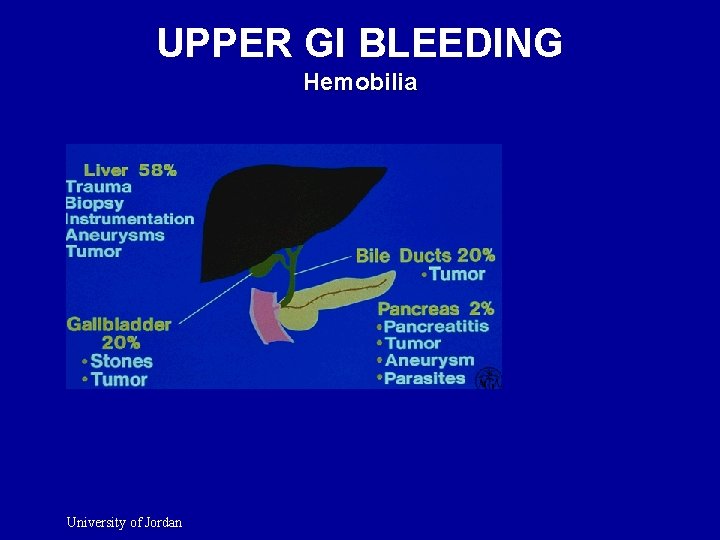
UPPER GI BLEEDING Hemobilia University of Jordan
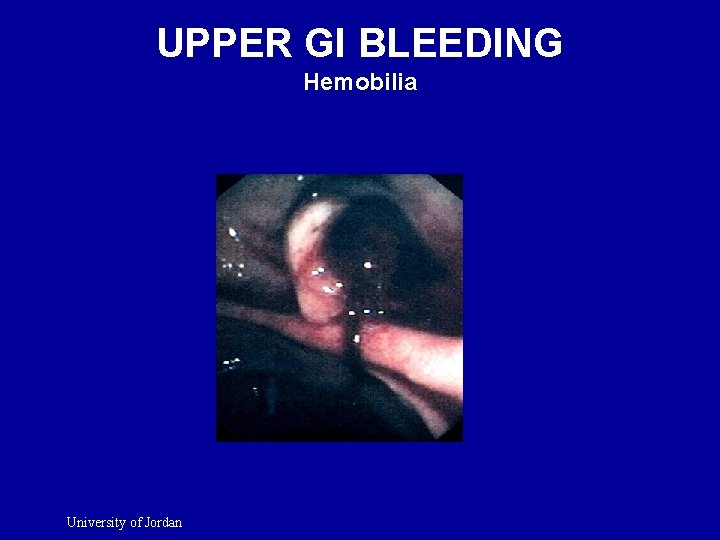
UPPER GI BLEEDING Hemobilia University of Jordan
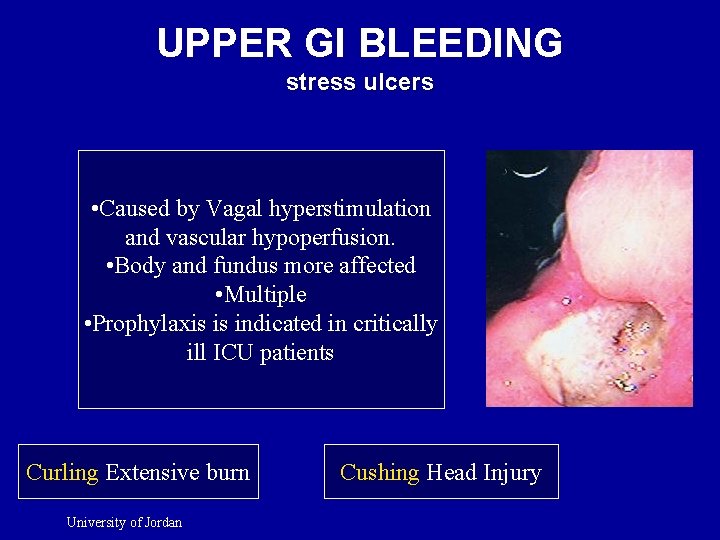
UPPER GI BLEEDING stress ulcers • Caused by Vagal hyperstimulation and vascular hypoperfusion. • Body and fundus more affected • Multiple • Prophylaxis is indicated in critically ill ICU patients Curling Extensive burn University of Jordan Cushing Head Injury

UPPER GI BLEEDING ADVERSE PROGNOSTIC FACTORS n Diagnosis u u n n n Varices Malignancy Older age Severe initial bleeding Recurrence during hospitalization Coincidental diseases Endoscopic stigmata of recent bleeding Need for emergency surgery University of Jordan

UPPER GI BLEEDING MANAGEMENT Resuscitation Assessment History Physical Labs Endoscopy Bleeding Stops Bleeding continues Surgery or angiogram/ embolization University of Jordan

UPPER GI BLEEDING MANAGEMENT Most Have Rectal Exam Endoscopy University of Jordan

UPPER GI BLEEDING MANAGEMENT Most Have Rectal Exam Endoscopy University of Jordan

UPPER GI BLEEDING MANAGEMENT Most Have Rectal Exam Endoscopy University of Jordan

UPPER GI BLEEDING MANAGEMENT Most Have Rectal Exam Endoscopy University of Jordan

UPPER GI BLEEDING University of Jordan

UPPER GI BLEEDING MANAGEMENT: Proton Pump Inhibitors l l l 10 studies had been published on the use of PPIs for upper GI bleeding since 1990. Proven benefit in controlling bleeding when 80 mg bolus of Omeprazole followed by infusion for total of 160 mg/day. Preventing rebleeding when Omeprazole orally at 40 mg twice daily. University of Jordan

UPPER GI BLEEDING ESOPHAGEAL VARICEAL • Dilated tortuous veins of the lower and mid esophagus. • Secondary to portal HTN • 30% mortality after the first episode. • 60% Rebleeding rate University of Jordan
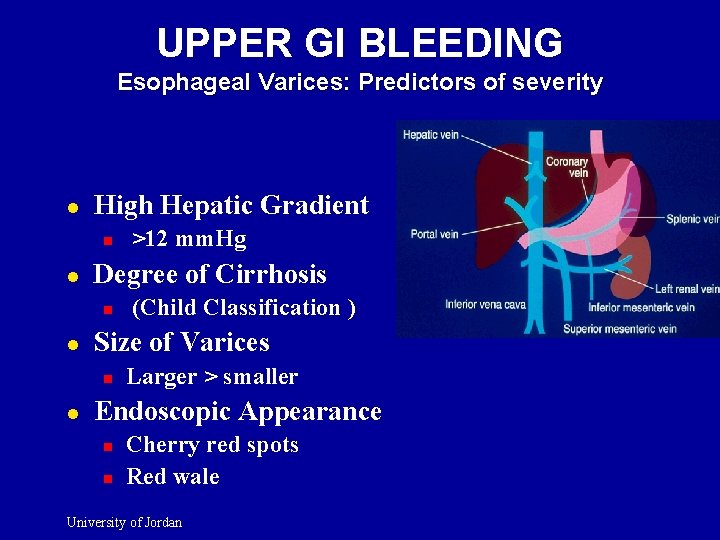
UPPER GI BLEEDING Esophageal Varices: Predictors of severity l High Hepatic Gradient n l Degree of Cirrhosis n l (Child Classification ) Size of Varices n l >12 mm. Hg Larger > smaller Endoscopic Appearance n n Cherry red spots Red wale University of Jordan
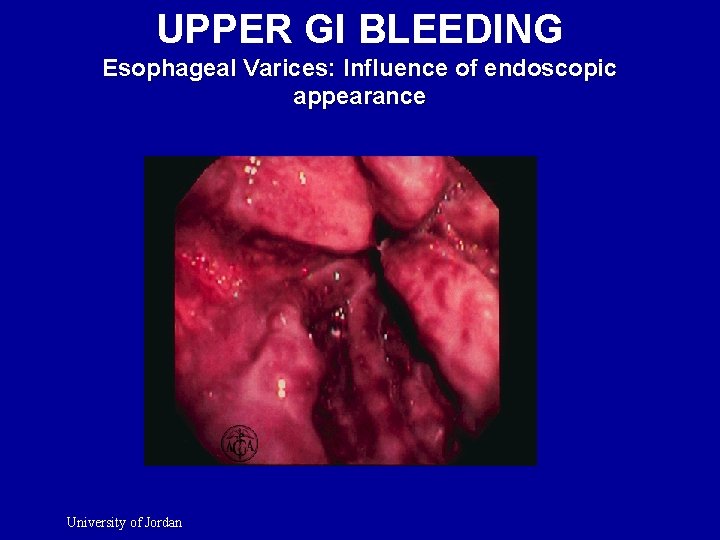
UPPER GI BLEEDING Esophageal Varices: Influence of endoscopic appearance University of Jordan

UPPER GI BLEEDING Esophageal Varices: Management Assessment / Resuscitation Pharmacological Therapy • Somatostatin or Octreotide • Vassopressin and Nitroglycerine Endoscopy for diagnosis and therapy • Variceal Banding Balloon Temponade University of Jordan

Cirrhosis and Portal hypertension
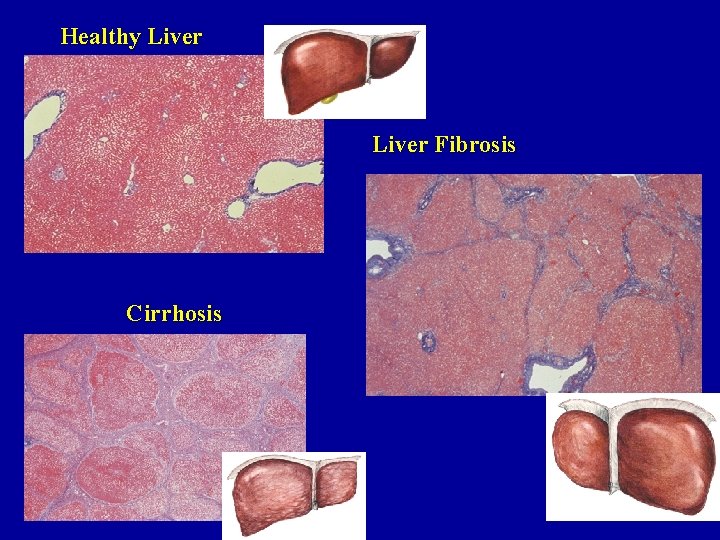
Healthy Liver Fibrosis Cirrhosis
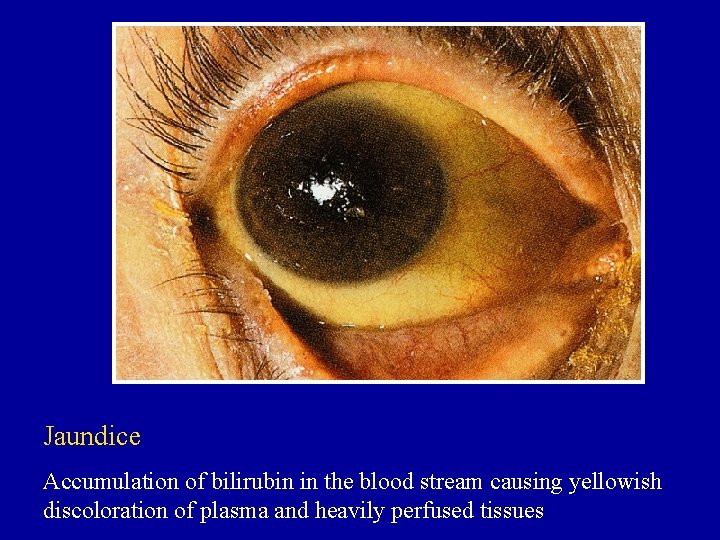
Jaundice Accumulation of bilirubin in the blood stream causing yellowish discoloration of plasma and heavily perfused tissues

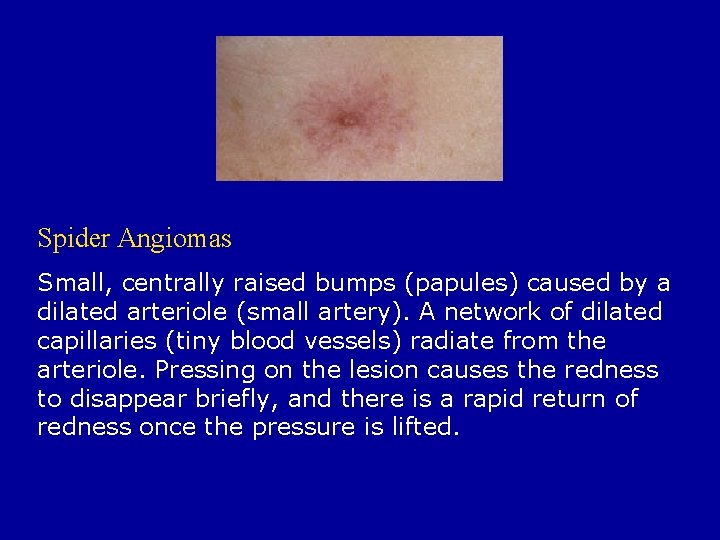
Spider Angiomas Small, centrally raised bumps (papules) caused by a dilated arteriole (small artery). A network of dilated capillaries (tiny blood vessels) radiate from the arteriole. Pressing on the lesion causes the redness to disappear briefly, and there is a rapid return of redness once the pressure is lifted.
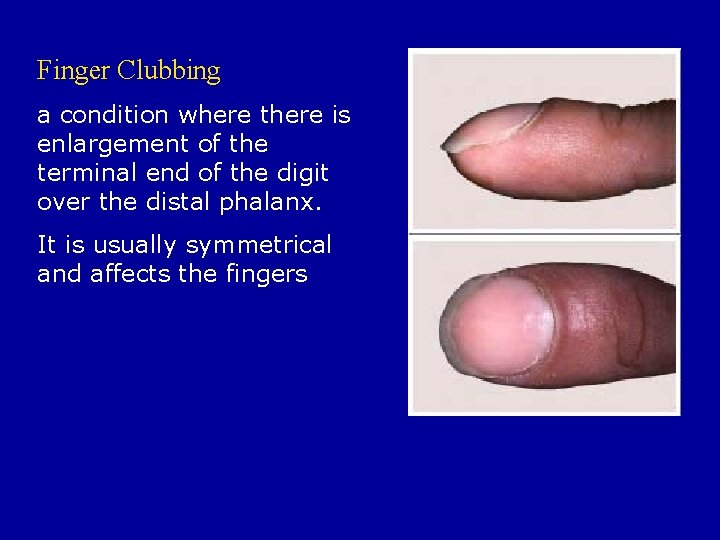
Finger Clubbing a condition where there is enlargement of the terminal end of the digit over the distal phalanx. It is usually symmetrical and affects the fingers

Gynecomastia Breast development in men
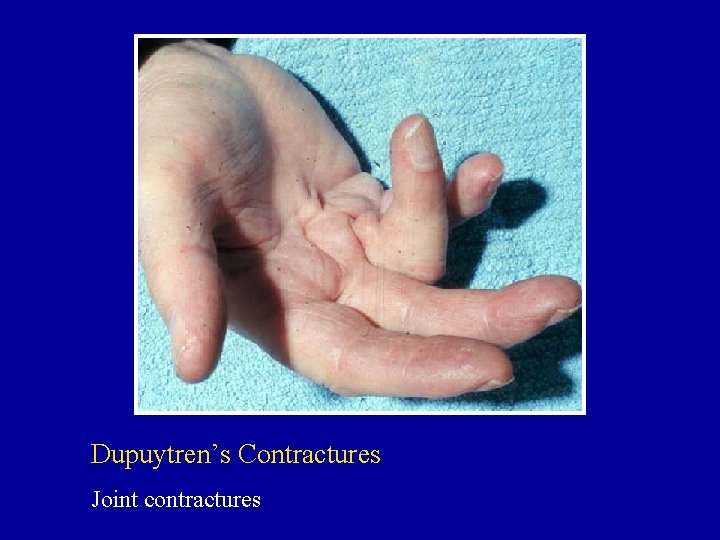
Dupuytren’s Contractures Joint contractures

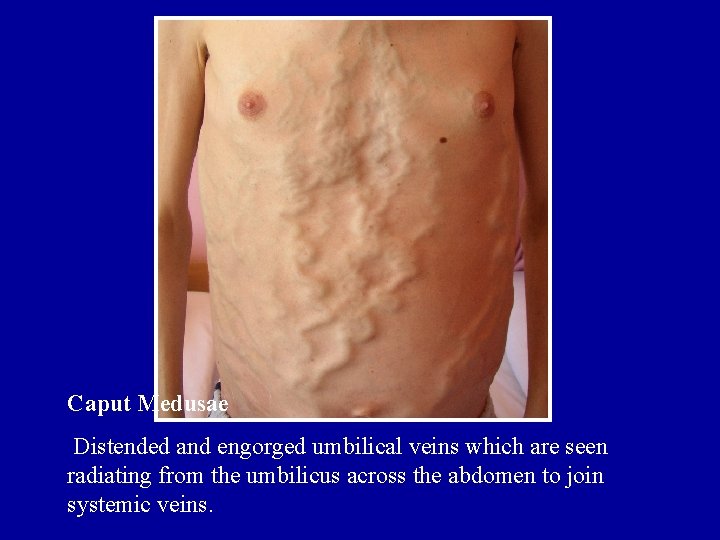
Caput Medusae Distended and engorged umbilical veins which are seen radiating from the umbilicus across the abdomen to join systemic veins.




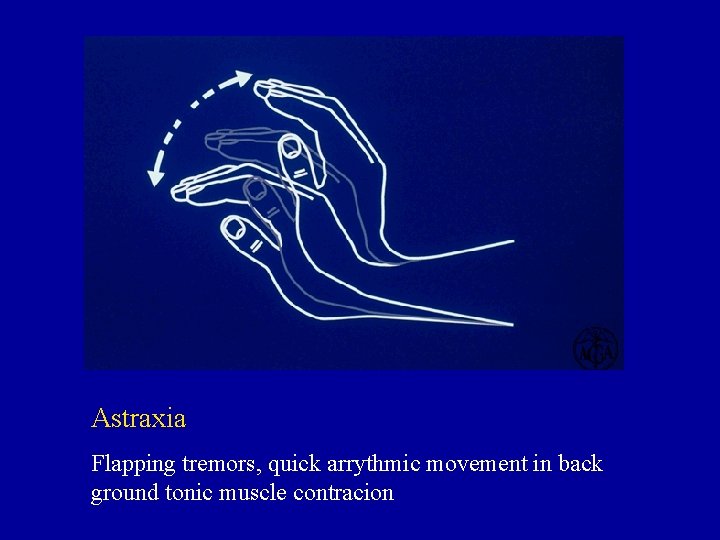
Astraxia Flapping tremors, quick arrythmic movement in back ground tonic muscle contracion


Hepatitis A-E Viruses An Overview
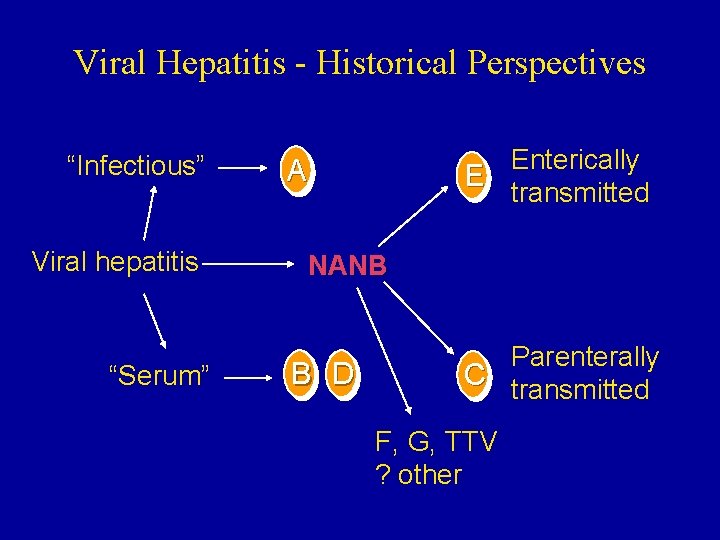
Viral Hepatitis - Historical Perspectives “Infectious” Viral hepatitis “Serum” Enterically E transmitted A NANB B D Parenterally C transmitted F, G, TTV ? other

Type of Hepatitis A Source of virus Route of transmission Chronic infection Prevention B C D E feces blood/ blood-derived body fluids feces fecal-oral percutaneous permucosal fecal-oral no yes pre/postexposure immunization yes blood donor pre/postscreening; exposure risk behavior immunization; modification risk behavior modification no ensure safe drinking water
Hepatitis A Virus

Hepatitis A - Clinical Features n n Incubation period: Jaundice by age group: n Complications: n Chronic sequelae: Average 30 days Range 15 -50 days <6 yrs, <10% 6 -14 yrs, 40%-50% >14 yrs, 70%-80% Fulminant hepatitis Cholestatic hepatitis Relapsing hepatitis None
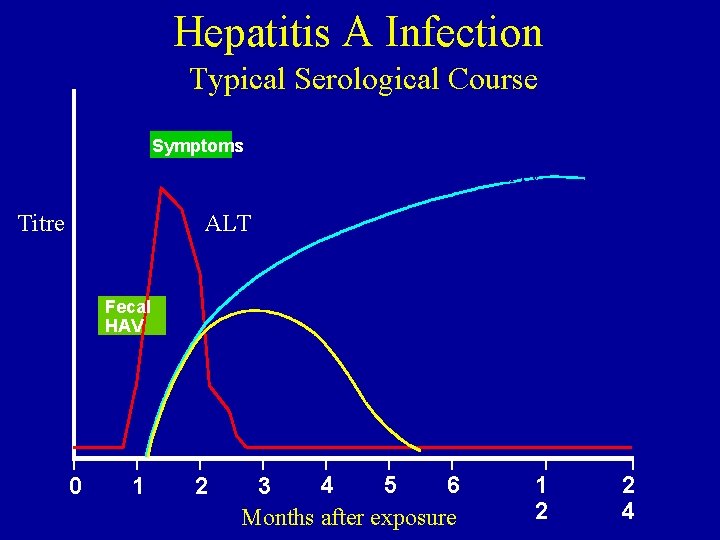
Hepatitis A Infection Typical Serological Course Total anti. HAV Symptoms Titre ALT Fecal HAV 0 1 Ig. M anti-HAV 2 4 5 6 3 Months after exposure 1 2 2 4

Hepatitis A Virus Transmission l l l Close personal contact (e. g. , household contact, sex contact, child day care centers) Contaminated food, water (e. g. , infected food handlers, raw shellfish) Blood exposure (rare) (e. g. , injecting drug use, transfusion)

Global Patterns of Hepatitis A Virus Transmission Disease Peak Age Endemicity Rate of Infection High Transmission Patterns Low to High Early childhood Person to person; outbreaks uncommon Moderate High Late childhood/ young adults Person to person; food and waterborne outbreaks Low Very low Young adults Person to person; food and waterborne outbreaks Very low Adults Travelers; outbreaks uncommon

Laboratory Diagnosis l l Acute infection is diagnosed by the detection of HAV-Ig. M in serum by EIA. Past Infection i. e. immunity is determined by the detection of HAV-Ig. G by EIA.
Hepatitis B Virus

Hepatitis B - Clinical Features § Incubation period: § Clinical illness (jaundice): § Acute case-fatality rate: § Chronic infection: § Premature mortality from chronic liver disease: Average 60 -90 days Range 45 -180 days <5 yrs, <10% 5 yrs, 30%-50% 0. 5%-1% <5 yrs, 30%-90% 5 yrs, 2%-10% 15%-25%

Spectrum of Chronic Hepatitis B Diseases 1. Chronic Persistent asymptomatic Hepatitis 2. Chronic Active Hepatitis symptomatic exacerbations hepatitis 3. Cirrhosis of Liver 4. Hepatocellular Carcinoma - of

Acute Hepatitis B Virus Infection with Recovery. Typical Serologic Course Symptoms HBe. Ag anti-HBe Total anti-HBc Titre HBs. Ag 0 4 8 anti-HBs Ig. M anti-HBc 12 16 20 24 28 32 36 Weeks after Exposure 52 100
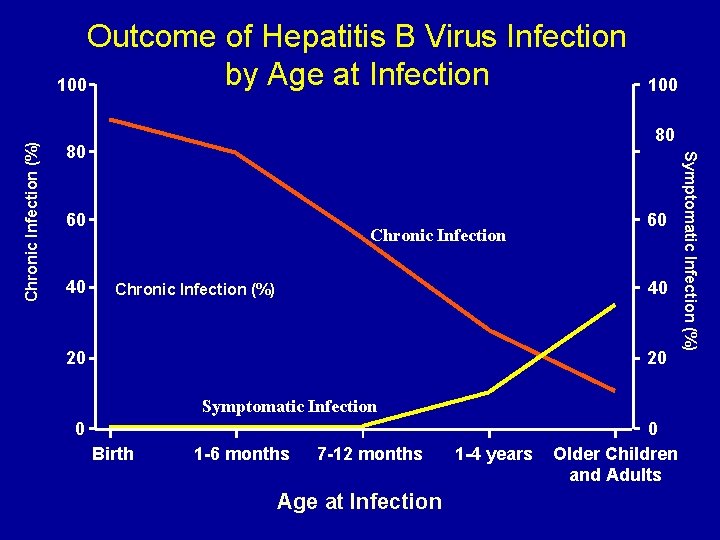
80 80 60 40 100 Chronic Infection 60 40 Chronic Infection (%) 20 20 Symptomatic Infection 0 Birth 1 -6 months 7 -12 months Age at Infection 1 -4 years 0 Older Children and Adults Symptomatic Infection (%) Chronic Infection (%) Outcome of Hepatitis B Virus Infection by Age at Infection 100
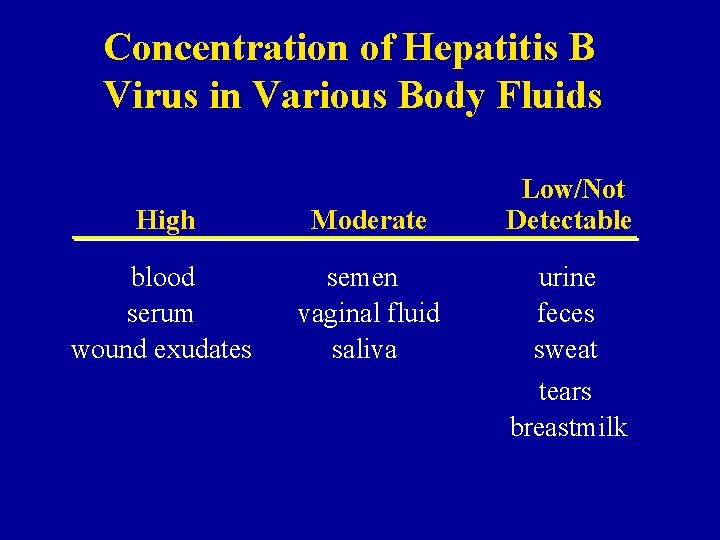
Concentration of Hepatitis B Virus in Various Body Fluids High Moderate blood serum wound exudates semen vaginal fluid saliva Low/Not Detectable urine feces sweat tears breastmilk

Hepatitis B Virus Modes of Transmission § Sexual - sex workers and homosexuals are particular at risk. § Parenteral - IVDA, Health Workers are at increased risk. § Perinatal - Mothers who are HBe. Ag positive are much more likely to transmit to their offspring than those who are not. Perinatal transmission is the main means of transmission in high prevalence populations.

Diagnosis l l l l A battery of serological tests are used for the diagnosis of acute and chronic hepatitis B infection. HBs. Ag - used as a general marker of infection. HBs. Ab - used to document recovery and/or immunity to HBV infection. anti-HBc Ig. M - marker of acute infection. anti-HBc. Ig. G - past or chronic infection. HBe. Ag - indicates active replication of virus and therefore infectiveness. Anti-Hbe - virus no longer replicating. However, the patient can still be positive for HBs. Ag which is made by integrated HBV-DNA - indicates active replication of virus, more accurate than HBe. Ag especially in cases of escape mutants. Used mainly for monitoring response to therapy.

Prevention l l l Vaccination - highly effective recombinant vaccines are now available. Vaccine can be given to those who are at increased risk of HBV infection such as health care workers. It is also given routinely to neonates as universal vaccination in many countries. Hepatitis B Immunoglobulin - HBIG may be used to protect persons who are exposed to hepatitis B. It is particular efficacious within 48 hours of the incident. It may also be given to neonates who are at increased risk of contracting hepatitis B i. e. whose mothers are HBs. Ag and HBe. Ag positive. Other measures - screening of blood donors, blood and body fluid precautions.

Hepatitis C Virus capsid envelop e protein c 22 protease/helica se 33 c RNA- RNA polymerase dependent c-100 5’ 3’ cor E 1 e E 2 hypervariable region NS 2 NS 3 NS 4 NS 5

Hepatitis C - Clinical Features Incubation period: Average 6 -7 wks Range 2 -26 wks Clinical illness (jaundice): 30 -40% (20 -30%) Chronic hepatitis: 70% Persistent infection: Immunity: 85 -100% No protective antibody response identified

Chronic Hepatitis C Infection l l The spectrum of chronic hepatitis C infection is essentially the same as chronic hepatitis B infection. All the manifestations of chronic hepatitis B infection may be seen, albeit with a lower frequency i. e. chronic persistent hepatitis, chronic active hepatitis, cirrhosis, and hepatocellular carcinoma.

Risk Factors Associated with Transmission of HCV § Transfusion or transplant from infected donor § Injecting drug use § Hemodialysis (yrs on treatment) § Accidental injuries with needles/sharps § Sexual/household exposure to anti-HCVpositive contact § Multiple sex partners § Birth to HCV-infected mother

Laboratory Diagnosis l l l HCV antibody - generally used to diagnose hepatitis C infection. Not useful in the acute phase as it takes at least 4 weeks after infection before antibody appears. HCV-RNA - various techniques are available e. g. PCR and branched DNA. May be used to diagnose HCV infection in the acute phase. However, its main use is in monitoring the response to antiviral therapy. HCV-antigen - an EIA for HCV antigen is available. It is used in the same capacity as HCV-RNA tests but is much easier to carry out.

Prevention of Hepatitis C § Screening of blood, organ, tissue donors § High-risk behavior modification § Blood and body fluid precautions
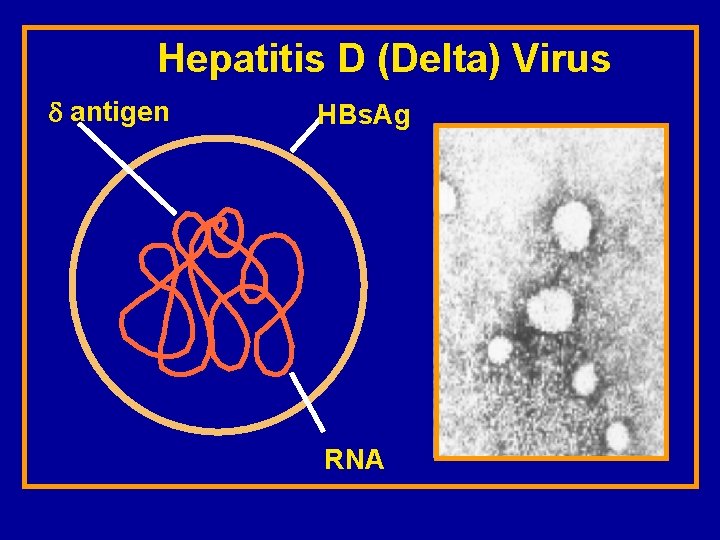
Hepatitis D (Delta) Virus antigen HBs. Ag RNA

Hepatitis D - Clinical Features § Coinfection – severe acute disease. – low risk of chronic infection. § Superinfection – usually develop chronic HDV infection. – high risk of severe chronic liver disease. – may present as an acute hepatitis.

Hepatitis D Virus Modes of Transmission § Percutanous exposures § injecting drug use § Permucosal exposures § sex contact
Hepatitis E Virus

Hepatitis E - Clinical Features n Incubation period: n Case-fatality rate: Average 40 days Range 15 -60 days Overall, 1%-3% Pregnant women, 15%-25% n Illness severity: Increased with age n Chronic sequelae: None identified
- Slides: 69