Updates on Optic Neuritis Briar Sexton Neuroophthalmology Clinical

Updates on Optic Neuritis Briar Sexton Neuro-ophthalmology Clinical Day Friday, November 18, 2005
Introduction • • Optic neuritis Atypical optic neuritis Treatment of optic neuritis Optic neuritis and MS

Optic Neuritis: Epidemiology • Incidence: 1 -5 per 100 000 per year • Highest incidence in – Caucasians – Countries with high latitudes: genetics? – Springtime – Ages 20 -49 – Women
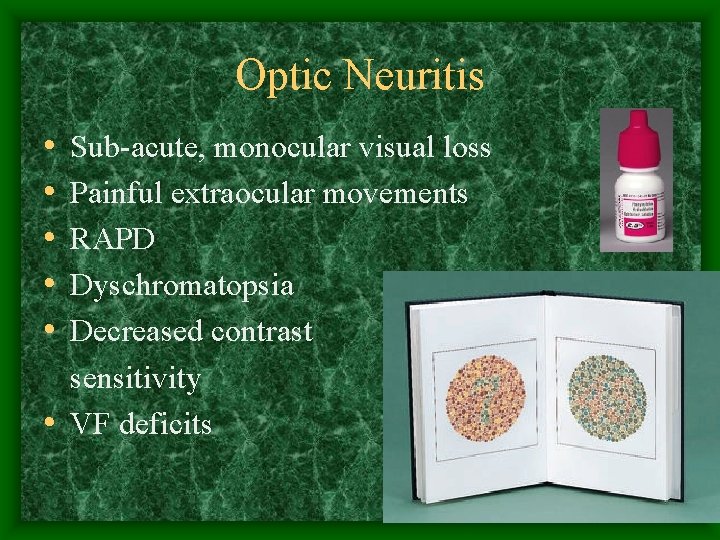
Optic Neuritis • • • Sub-acute, monocular visual loss Painful extraocular movements RAPD Dyschromatopsia Decreased contrast sensitivity • VF deficits
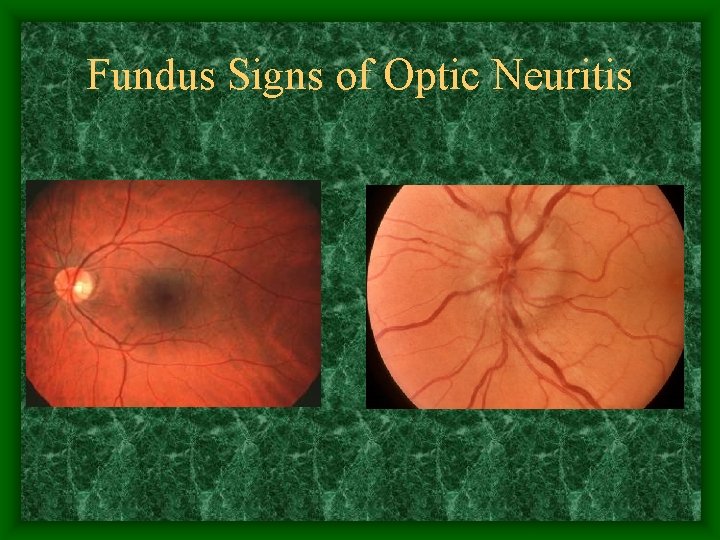
Fundus Signs of Optic Neuritis

Investigations Based on ONTT results for “typical” optic neuritis • Demyelination is the most common cause • No need for laboratory investigation – i. e. ESR, ANA • Need to do MRI of the brain – Assess MS risk

Atypical Optic Neuritis • Atypical symptoms – Unusual tempo of onset – Absence of pain – Co-morbidity • Atypical signs – – Progressive decline in vision > 2/52 Severe/hemorrhagic disc edema Uveitis: vitritis, retinitis, choroiditis Persistent ON sheath enhancement on MRI
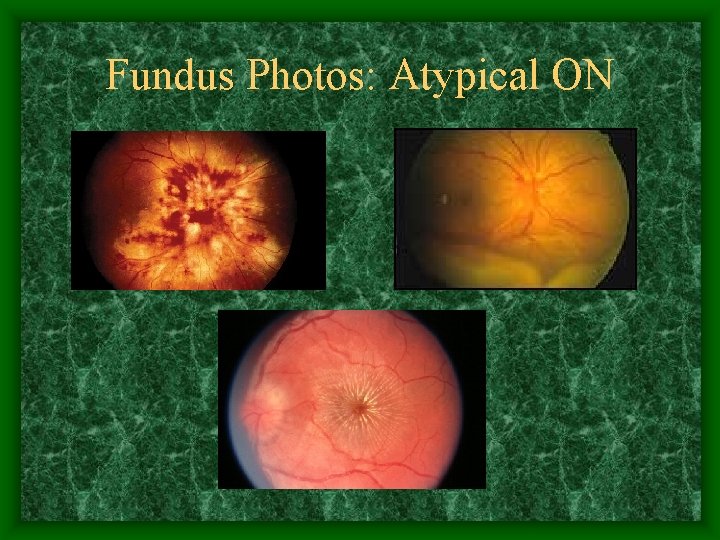
Fundus Photos: Atypical ON

Corticosteroid Dependent Optic Neuritis • Another atypical optic neuritis – Response to steroids – Vision falls with taper – Requires investigation
Atypical Optic Neuritis: Work-up • Laboratory investigations – CBC, ESR, ANA, MHA-ATP, ACE – Lyme, Baronella, TB skin test • CXR • Consider LP • Make sure MRI images optic nerve/orbits

Visual Fields • Central scotomas • Paracentral scotomas • Altitudinal defects

Neuroimaging • MRI – FLAIR sequencing – Gadolinium enhancement • Optic nerve sheath enhancement with gad • Periventricular white matter lesions on FLAIR
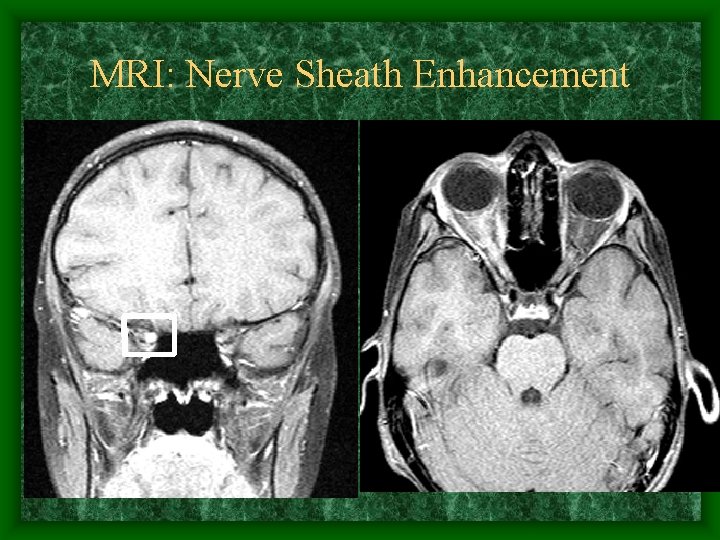
MRI: Nerve Sheath Enhancement •
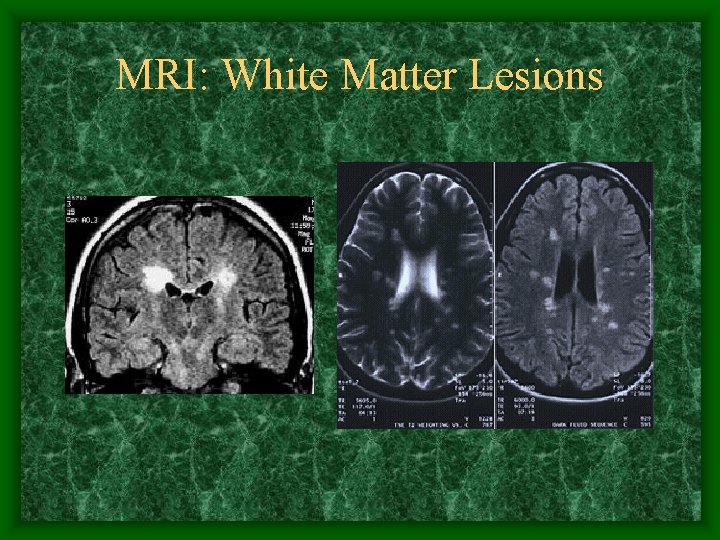
MRI: White Matter Lesions
The Optic Neuritis Treatment Trial (ONTT) • Objective: to evaluate the role of corticosteroids in the treatment of unilateral optic neuritis • Inclusion criteria: unilateral optic neuritis

The ONTT: Methods • Randomization to one of 3 groups 1. IV steroids: 250 mg methylprednisolone qid x 3 days, oral prednisone (1 mg/kg) x 11 days 2. Oral steroids: prednisone 1 mg/kg/day x 14 days 3. Oral placebo: 14 days

ONTT: Results • IV steroids – More rapid recovery but same endpoint – Protective v. placebo at 2 years, not 3 • Oral prednisone – Higher rate of new ON attacks at 1 year – Highest rate of relapse at 5 years
The ONTT and Oral Prednisone • Routing vs. Dose? – Probably dose: Greater CD 4 than CD 8 effect
Prognosis • Natural history: worsening over days to weeks followed by spontaneous recovery – 79% of patients begin to recover by 3/52 – 93% of patients show improvement by 5/52 • Ongoing clinical improvement to 1 year • VEP latency improves to 2 years
Prognosis • Severity of initial visual loss is related to final visual outcome • Most recover well – 74% ≥ 20/20 – 92% ≥ 20/40
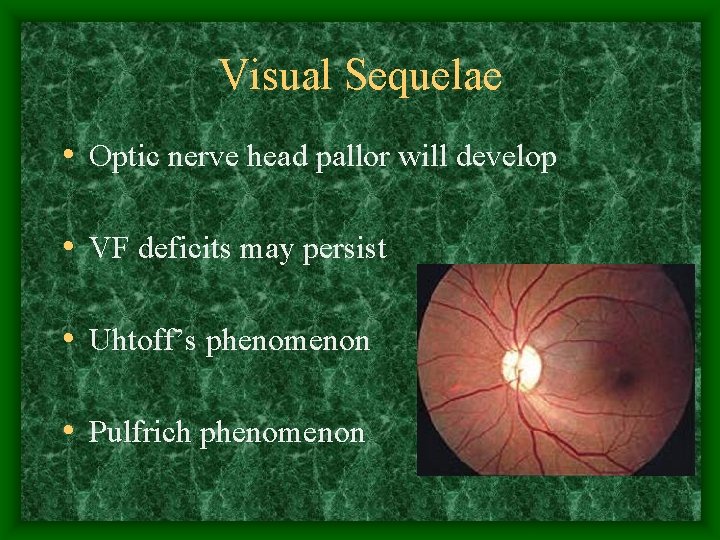
Visual Sequelae • Optic nerve head pallor will develop • VF deficits may persist • Uhtoff’s phenomenon • Pulfrich phenomenon

Optic Neuritis Recurrence From the ONTT • 35% of patients experienced recurrence in the previously affected eye or an attack in the fellow eye at 10 years • Recurrence rate was double in those with CDMS • Recurrence rate highest in the oral steroid group
Sub-clinical Optic Neuritis • Not all optic neuritis attacks are clinically evident • Sisto et al 2005 – VEP abnormalities in 54. 4% of CD-MS patients asymptomatic for visual impairment • Vidovic et al 2005 – 70% of visually asymptomatic MS patients had GVF defects consistent with optic neuritis

Optic Neuritis and MS • Clinical diagnosis – 2 demyelinating attacks separated in time and space – Sequential optic neuritis in one eye than the other meets the criteria – Discrete attacks in the same eye meets the criteria • Radiologic: Mac Donald Criteria

Optic Neuritis and MS • Lessell et al. 1988: 58% of optic neuritis at 15 years in initially isolated cases • 38 -50% of all CDMS develops optic neuritis at some point

Radiologic Predictors of MS 10 year ONTT data • White matter lesions on MRI – Risk is 22% if no baseline brain lesions – Risk is 56% if ≥ 1 baseline lesion – Risk increases with increasing lesions

Clinical Predictors of MS ONTT 10 year data • Low risk if no MRI lesions and – Male gender – Optic disc swelling • No CDMS in subset with above and one of • No pain • Severe disc edema • Peripapillary hemorrhages • Retinal exudates

Managing Optic Neuritis and MS • Positive MRI – Consider immunomodulatory therapy ie interferon or glatiramer acetate • Patients should be seen by neurology
CHAMPS Study • Effect of Interferon B 1 a treatment in patients with optic neuritis and MRI changes compatible with MS – Significantly less CDMS – Less progression of MRI lesions
Conclusions • Patients must be investigated for demyelination • Remember the atypical optic neuritis
- Slides: 30