UPDATES IN ANTIBODY TESTING IN RHEUMATOLOGY BY DR

UPDATES IN ANTIBODY TESTING IN RHEUMATOLOGY BY DR. Mohamed Gamal MD

Historical

What are Antibodies and Antibodies are part of the immune Autoantibodies? system
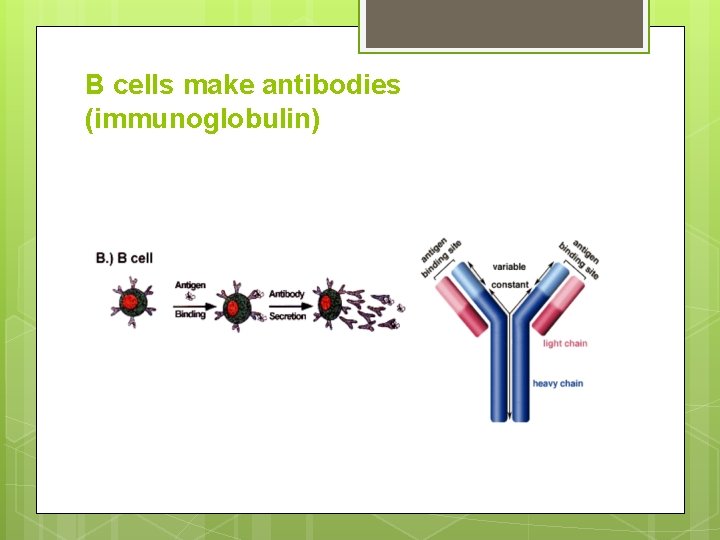
B cells make antibodies (immunoglobulin)

What are autoantibodies? Antibodies which instead of attaching to foreign antigens are directed against the host self-constituents Most autoantibodies are not thought to be the immediate cause of disease but are ‘biomarkers’ of pathology Close association between particular autoantibodies and certain diseases and clinical phenotypes Can discriminate subgroups of patients that differ in prognosis or response to therapy. Autoantibody levels may reflect disease activity

CHALLENGES OF AUTOANTIBODY TESTING The clinical information offered by autoantibody testing is invaluable for the diagnosis and management of SARDs limitations result from the complex analytical specificity of the tests and the need for high sensitivity. Methodological issues (such as source and preparation of antigen, coating systems and the use of different calibrators and calibration protocols )are critical variables that can affect autoantibody test results
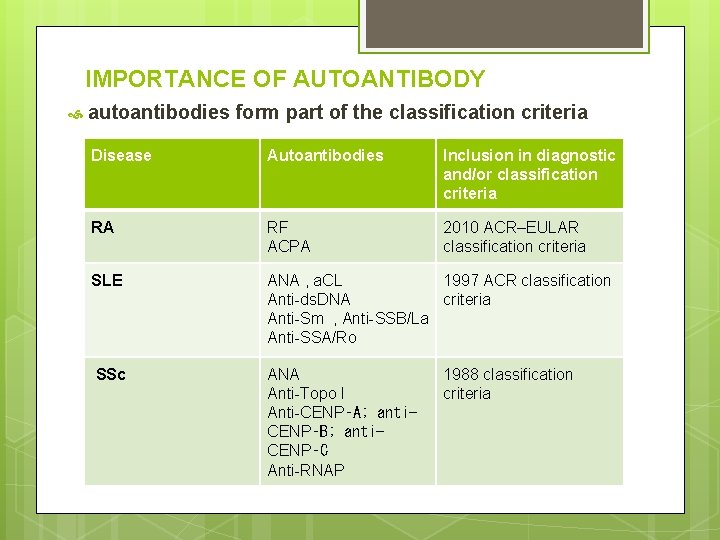
IMPORTANCE OF AUTOANTIBODY autoantibodies form part of the classification criteria Disease Autoantibodies Inclusion in diagnostic and/or classification criteria RA RF ACPA 2010 ACR–EULAR classification criteria SLE ANA , a. CL 1997 ACR classification Anti-ds. DNA criteria Anti-Sm , Anti-SSB/La Anti-SSA/Ro SSc ANA Anti-Topo I Anti-CENP‑A; anti. CENP‑B; anti. CENP‑C Anti-RNAP 1988 classification criteria

IMPORTANCE OF AUTOANTIBODY v Serum titers of some autoantibodies can also offer information on disease activity and/or the effect of immunosuppressive treatment v the involvement of particular tissues or organs v Ex. : levels of anti-doublestranded DNA (ds. DNA) antibodies with systemic lupus erythematosus Ex. : ACPA can be related to the prognosis of rheumatoid arthritis identifying subgroups of patients Ex. : anti-histone antibodies in drug induced lupus

IMPORTANCE OF AUTOANTIBODY v Autoantibody positivity may be the determining factor in starting primary prophylactic therapy, even in the absence of overt clinical signs, in order to reduce the risk to the patient v Ex. : anti-RNA polymerase III in systemic sclerosis evaluating the risk of developing specific complications Ex. : anti ribosomal p antibody in neuropsicatric lupus

Methods for detecting autoantibodies
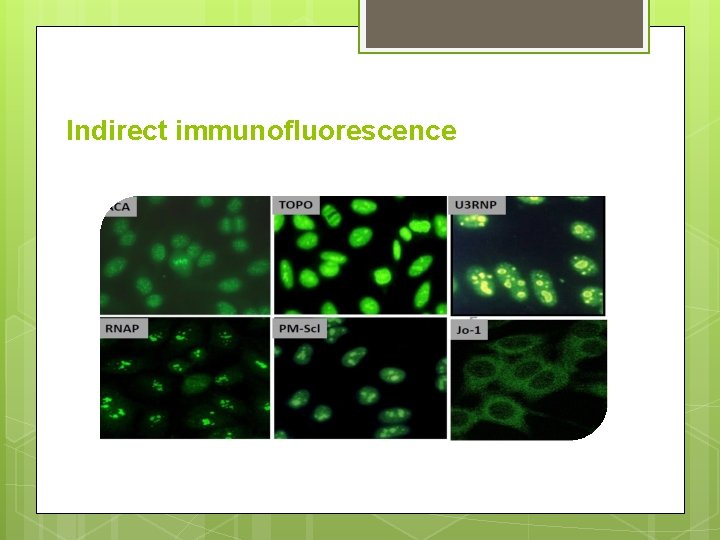
Indirect immunofluorescence

THE SPECTRUM OF AUTOIMMUNE CONNECTIVE TISSUE DISEASE
RHEUMATOID ARTHRITIS

RHEUMATOID ARTHRITIS RF ACCP AMCV

RHEUMATOID ARTHRITIS 14 -3 -3 eta — Serum 14 -3 -3 eta, an isoform of the 14 -3 -3 family of intracellular chaperonin proteins, have similar sensitivity and specificity to RF and ACPA in distinguishing patients with RA from osteoarthritis, other autoimmune disorders, and healthy controls. the addition of 14 -3 -3 eta testing resulted in a modest increase in positive testing in both early RA and established RA Its presence was also associated with more severe disease, although serum levels of 14 -3 -3 eta did not correlate with levels of acute phase markers or composite disease activity scores

RHEUMATOID ARTHRITIS Serum levels of 14 -3 -3 eta in inflammatory arthritis correlate with levels of matrix metalloproteinase (MMP)-1 and MMP-3, and the protein possesses ligand activity, preferentially activating cells of the innate immune system to activate proinflammatory cytokines, including interleukin (IL)-1, IL-6, and TNF-alpha, as well as factors involved in joint injury such as MMP-9 and Receptor Activator of Nuclear factor Kappa B ligand (RANKL)
DERMATOMYOSIT IS

AUTOANTIBODIES IN MYOSITIS MSA (myositis ‘specific’ autoantibodies) Anti-t. RNAsynthetases(e. g. anti-Jo-1) Anti-Mi-2 Anti-signal recognition particle Anti-SAE Anti-TIF-1 g Anti-MDA 5 Anti-NXP 2 Anti-HMGCR Anti-EIF-3 Anti-MUP 44 • MAA (myositis associated autoantibodies) • Anti-PM-Scl • Anti-U 1 RNP • Anti-Ku • Anti-U 3 RNP
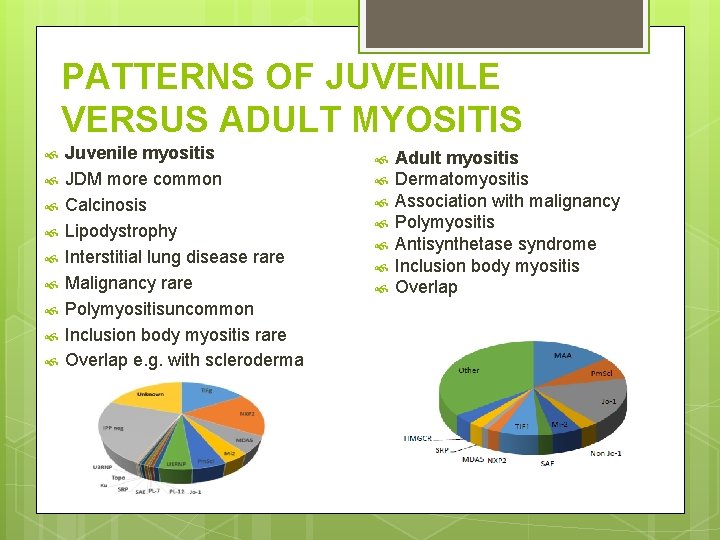
PATTERNS OF JUVENILE VERSUS ADULT MYOSITIS Juvenile myositis JDM more common Calcinosis Lipodystrophy Interstitial lung disease rare Malignancy rare Polymyositisuncommon Inclusion body myositis rare Overlap e. g. with scleroderma Adult myositis Dermatomyositis Association with malignancy Polymyositis Antisynthetase syndrome Inclusion body myositis Overlap

AUTOANTIBODIES IN JDM AND JUVENILE MYOSITIS OVERLAP Until recently less well characterized Myositis specific autoantibodies Myositis associated autoantibodies Anti-Mi-2 most frequently described Low frequency of anti-synthetase and anti-SRP Overlap syndromes with scleroderma/lupus Anti-Pm. Scl Anti-U 1 RNP New MSA in JDM Anti-TIF 1 g Anti-NXP 2 Anti-MDA 5
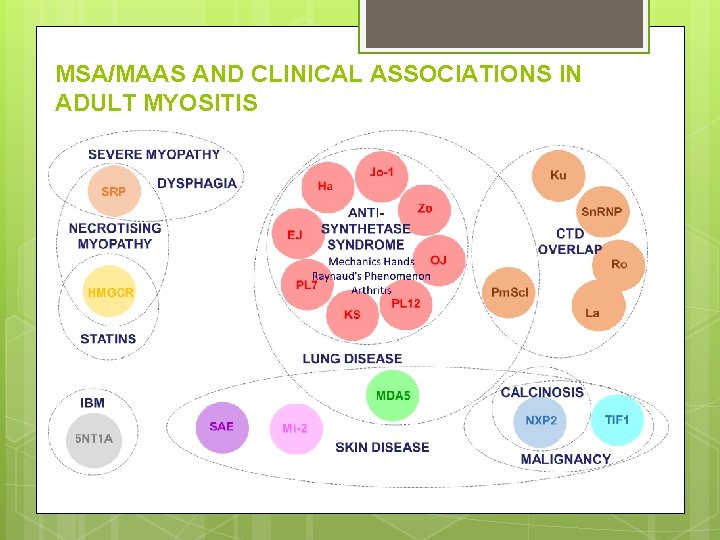
MSA/MAAS AND CLINICAL ASSOCIATIONS IN ADULT MYOSITIS

Anti-synthetase syndrome

MYOSITIS SPECIFIC ANTIBODIES Anti-SRP antibodies 5 percent exclusively occur in patients diagnosed with polymyositis Characterized by severe myopathy and aggressive disease typically show muscle fiber necrosis and endomysial fibrosis but show little or no inflammatory cell infiltrate high-dose glucocorticoids and immunosuppressive agents may be insufficient.

MYOSITIS SPECIFIC ANTIBODIES Anti-Mi-2 antibodies 7 percent of Caucasians and in about 30 percent of those from Central America Characterized by relatively acute onset of dermatomyositis a classic shawl or V sign, respond well to glucocorticoids

MYOSITIS SPECIFIC ANTIBODIES amyopathic dermatomyositis CADM-140 and anti-MDA-5 antibody first reported in Japanese patients strongly associated with rapidly progressive ILD, vasculopathy affecting the skin , a symmetric inflammatory polyarthropathy that was frequently indistinguishable from rheumatoid arthritis. responsive to immunosuppressive therapy.

MYOSITIS SPECIFIC ANTIBODIES Anti-p 140 (anti-MJ) studied primarily in patients with juvenile dermatomyositis associated with calcinosis also described in adults with DM associated with interstitial lung disease anti-p 155/140 antibody, was detected in 7 of 52 patients (13 percent) with dermatomyositis but in none of the disease controls with polymyositis, SLE, SSc, or idiopathic interstitial pneumonia. Clinical associations include strong associations with adult and juvenile dermatomyositis, rather than polymyositis, and with cancer-associated myositis. Flagellate erythema and the conventional cutaneous DM findings of Gottron’s papules and a heliotrope eruption may be present.
ANCA ASSOCIATED VASCULITIS

IMPORTANCE OF ANCA SEROLOGY ANCA serologies are useful in distinguishing MPA from classic PAN. phenotypic differences among patients with CSS who are ANCA positive as opposed to ANCA negative. In patients with both ANCA and anti-GBM antibodies, ANCA antibodies were detected in earlier samples than anti-GBM antibodies, which suggest the possibility that the pulmonary or renal damage caused by ANCA may lead to secondary anti-GBM antibody formation.

Importance of ANCA serology Drug-induced ANCA-associated vasculitis : associated with previous treatment with antithyroid drugs , and less commonly with Hydralazine, and minocycline Most patients have MPO-ANCA, in very high titers. constitutional symptoms, arthralgias/arthritis, and cutaneous vasculitis. crescentic glomerulonephritis and alveolar hemorrhage, can also occur. the syndrome usually resolves with discontinuation of the inducing drugs , but severe cases may require treatment with corticosteroids and other immunosuppression.

CLINICAL APPLICATIONS Is a positive test result a "true positive"? Two types of ANCA assays are currently in wide use: ●Indirect immunofluorescence assay : more sensitive, used for screening ●Enzyme-linked immunosorbent assay (ELISA): more specific , used for confirmation.

CLINICAL APPLICATIONS Does a negative ANCA assay exclude an "ANCAassociated" vasculitis? up to 40 percent of patients with GPA , 30 percent of all MPA patients and 50 percent of those with Churg-Strauss syndrome (CSS) are ANCA negative ANCA status may change over time; ANCA negative patient with constitutional symptoms and pulmonary infiltrates may become PR 3 -ANCA positive upon the development of more generalized disease (eg, the occurrence of glomerulonephritis). A negative ANCA assay may therefore create a false sense of security.

CLINICAL APPLICATIONS ●Is the presence of a positive ANCA assay in and of itself sufficient to establish the diagnosis (i. e. , does it preclude the need for biopsy? ) many assays currently available are not sufficiently accurate and the potential toxicity of present therapies for ANCA-positive diseases is too great to rely upon serology alone. biopsy is required to document the presence or absence of a pauci-immune crescentic glomerulonephritis in ANCA-positive patients in whom the tissue diagnosis cannot be confirmed less invasively (eg, biopsy of a nasal lesion).

CLINICAL APPLICATIONS Does a rise in ANCA titers predict a disease flare? a controversial area , several rigorous studies have demonstrated that elevations in the titers of ANCA do not predict disease flares in a timely manner. the use of an elevation in ANCA titer as the sole parameter to justify immunosuppressive therapy cannot be endorsed. A reasonable recommendation is to closely follow patients with rising ANCA titers but not to alter their therapy unless there are clearcut clinical signs of active disease.

CLINICAL APPLICATIONS Does a persistently negative ANCA assure disease quiescence? If a patient was ANCA positive during a period of active disease, a persistently ANCA-negative status is consistent with, but not absolutely proof of, remission. This was illustrated in a report in which 37 of 100 patients with ANCA-associated vasculitis suffered flares during the period of observation. Of these, three (8 percent) were ANCA negative at the time of relapse.

CONCLUSION - Think before you request - Clinical impression hugely valuable in guiding Ix choice - Sensitive tests first… specific later to confirm diagnoses


SYSTEMIC LUPUS ERYTHEMATOSU S

Systemic Lupus Erythematosus more than 110 different types of autoantibodies have been identified in SLE specific for SLE: Anti-native-DNA (up to 90% of patients) anti-Sm anti-ribosomal-RNP and antibody to proliferating cell nuclear antigen (anti-PCNA) SLE is characterized by a heterogeneous and polyclonal antibody response, and the usual case of SLE has an average of three different circulating antibodies present simultaneously, including antibody to native DNA (ds. DNA), chromatin. Sm antigen, U I n. RNP, SS-A/RO, SS-B/La, and several other nonhistone protein or nonhistone protein-RNA complexes
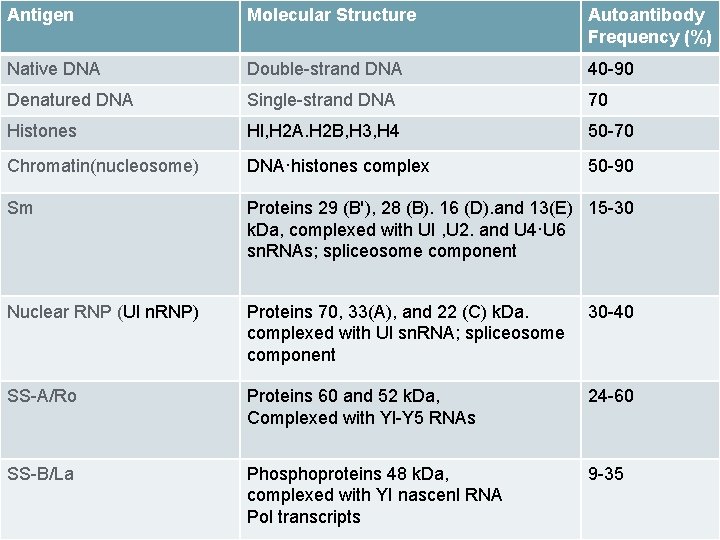
Antigen Molecular Structure Autoantibody Frequency (%) Native DNA Double-strand DNA 40 -90 Denatured DNA Single-strand DNA 70 Histones Hl, H 2 A. H 2 B, H 3, H 4 50 -70 Chromatin(nucleosome) DNA·histones complex 50 -90 Sm Proteins 29 (B'), 28 (B). 16 (D). and 13(E) 15 -30 k. Da, complexed with UI , U 2. and U 4·U 6 sn. RNAs; spliceosome component Nuclear RNP (Ul n. RNP) Proteins 70, 33(A), and 22 (C) k. Da. complexed with Ul sn. RNA; spliceosome component 30 -40 SS-A/Ro Proteins 60 and 52 k. Da, Complexed with Yl-Y 5 RNAs 24 -60 SS-B/La Phosphoproteins 48 k. Da, complexed with YI nascenl RNA Pol transcripts 9 -35
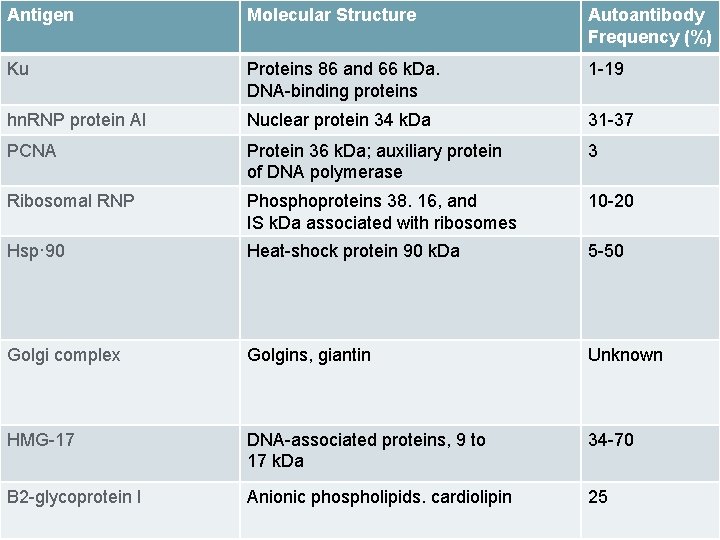
Antigen Molecular Structure Autoantibody Frequency (%) Ku Proteins 86 and 66 k. Da. DNA-binding proteins 1 -19 hn. RNP protein Al Nuclear protein 34 k. Da 31 -37 PCNA Protein 36 k. Da; auxiliary protein of DNA polymerase 3 Ribosomal RNP Phosphoproteins 38. 16, and IS k. Da associated with ribosomes 10 -20 Hsp· 90 Heat-shock protein 90 k. Da 5 -50 Golgi complex Golgins, giantin Unknown HMG-17 DNA-associated proteins, 9 to 17 k. Da 34 -70 B 2 -glycoprotein I Anionic phospholipids. cardiolipin 25

SYSTEMIC SCLEROSIS Antigen ANA staining pattern Scl-70 (topoisomerase. Speckled 1) Approximate frequency Clinical associations in all patients (percent) Organ involvement 10 to 40 dc. SSc Lung fibrosis, isolated pulmonary hypertension less likely lc. SSc Pulmonary hypertension, esophageal disease, "protection" from lung fibrosis and renal disease dc. SSc Renal, skin, malignancy Centromere (kinetochore) RNA polymerase III Fine speckled nucleolar 4 to 25 15 to 40
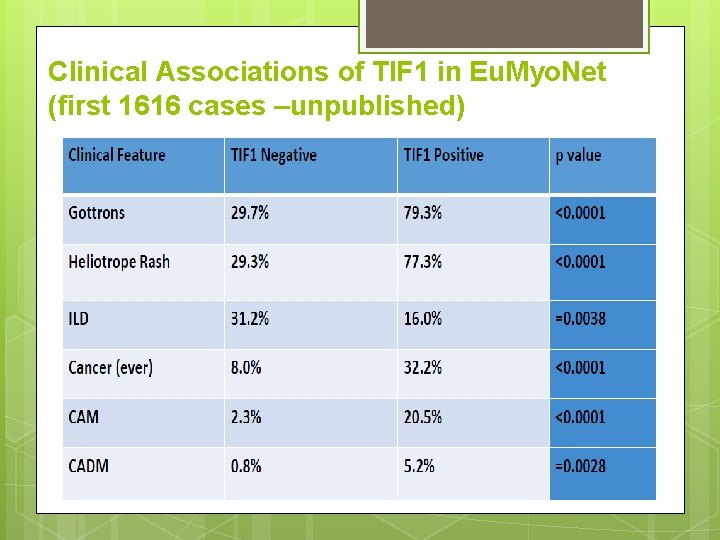
Clinical Associations of TIF 1 in Eu. Myo. Net (first 1616 cases –unpublished)
ANTIBODIES AND AUTOANTIBODIES
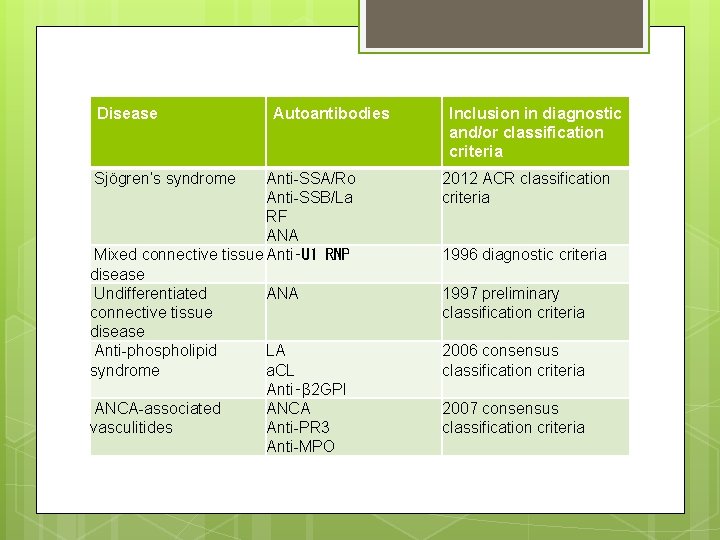
Disease Sjögren’s syndrome Autoantibodies Anti-SSA/Ro Anti-SSB/La RF ANA Mixed connective tissue Anti‑U 1 RNP disease Undifferentiated ANA connective tissue disease Anti-phospholipid LA syndrome a. CL Anti‑β 2 GPI ANCA-associated ANCA vasculitides Anti-PR 3 Anti-MPO Inclusion in diagnostic and/or classification criteria 2012 ACR classification criteria 1996 diagnostic criteria 1997 preliminary classification criteria 2006 consensus classification criteria 2007 consensus classification criteria

ANALYTICAL ISSUES IN AUTOANTIBODY STANDARDIZATION Pre-analytical issues Analytical issues Patient identification Assay variability Post-analytical issues Sample collection parameters Antigen characteristics Reporting of the results Sample storage and handling Immobilization of antigen Units of measurement Transport conditions Calibration and standardization Setting of the cutoff: analysis of distributions among systems Patient factors (physiological healthy subjects matched for sex and age, and among variables, pathological states) Detection systems pathological controls (including infectious diseases, samples with paraproteins or hypergammaglobulinemia) Interpretation and categorization; for example, “negative”, “borderline”, “positive”, “strong positive” Interpretation of new assays in comparison with older ones (for example, controimmunoelectrophoresis versus ELISA, chemiluminescence versus ELISA, determination of the range of sensitivity)
- Slides: 45