UOG Journal Club November 2017 Outcome of monochorionic

UOG Journal Club: November 2017 Outcome of monochorionic twin pregnancy with selective intrauterine growth restriction according to umbilical artery Doppler flow pattern of smaller twin: systematic review and meta-analysis D. Buca, G. Pagani, G. Rizzo, A. Familiari, M. E. Flacco, L. Manzoli, M. Liberati, F. Fanfani, G. Scambia and F. D’Antonio Volume 50, Issue 5, pages 559 -568 Journal Club slides prepared by Dr Yael Raz (UOG Editor for Trainees)

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Introduction Gratacós et al. 1 classification of s. IUGR in MC twins, based on umbilical artery (UA) Doppler flow pattern of the smaller twin : • Type I - persistently positive diastolic flow • Type II - persistently absent/reversed diastolic flow • Type III - intermittently absent/reversed diastolic flow Stated perinatal outcomes in the original series : - Type I s. IUGR showed the best outcome - Type II had the worst prognosis - Type III was characterized by an unpredictable clinical course. 1 Gratacós E, Lewi L, Muñoz B, Acosta-Rojas R, Hernandez-Andrade E, Martinez JM, Carreras E, Deprest J. A classification system for selective intrauterine growth restriction in monochorionic pregnancies according to umbilical artery Doppler flow in the smaller twin. Ultrasound Obstet Gynecol 2007; 30: 28– 34.

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Aim of the systemic review To explore the outcome in MC twin pregnancies affected by s. IUGR according to the UA Doppler flow pattern of the smaller twin.

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Methods – Study selection • Inclusion: studies reporting the prenatal diagnosis of s. IUGR in MC twins according to the classification of Gratacós et al. • Exclusion: - Cases with superimposed TTTS - Studies reporting only one type of s. IUGR - Studies from which the information regarding the type of s. IUGR could not be extrapolated - Studies including cases undergoing fetal therapy - Studies published before 2000

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Results - Study design 13 studies were included 610 MC twin pregnancies affected by s. IUGR: 39% – Type I 38. 2 % - Type II 22. 8% - Type III Mean gestational age at diagnosis: Type I - 26. 5 weeks Type II - 21. 1 weeks Type III - 20. 2 weeks
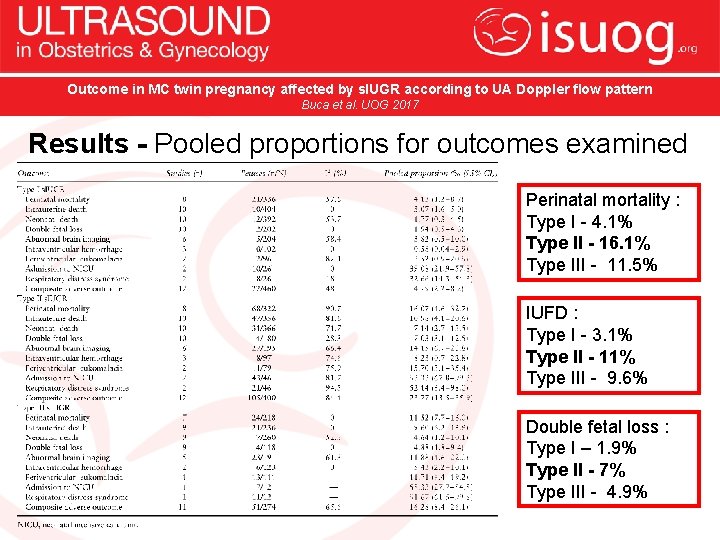
Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Results - Pooled proportions for outcomes examined Perinatal mortality : Type I - 4. 1% Type II - 16. 1% Type III - 11. 5% IUFD : Type I - 3. 1% Type II - 11% Type III - 9. 6% Double fetal loss : Type I – 1. 9% Type II - 7% Type III - 4. 9%
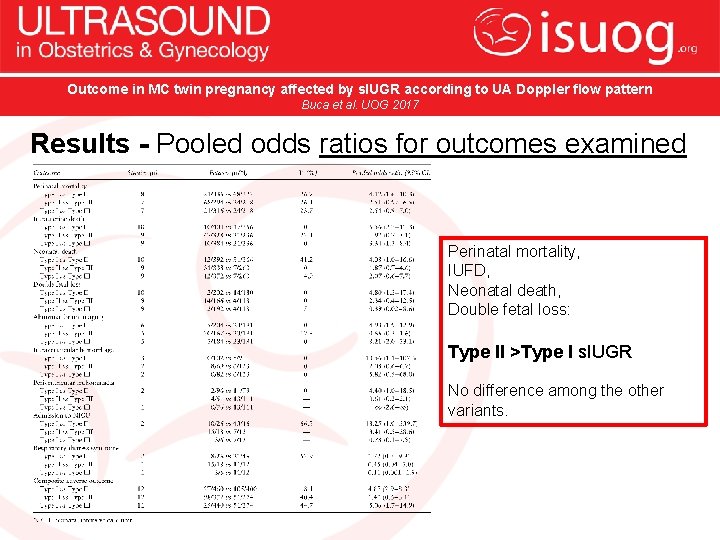

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Results - Pooled odds ratios for outcomes examined Perinatal mortality, IUFD, Neonatal death, Double fetal loss: Type II >Type I s. IUGR No difference among the other variants.
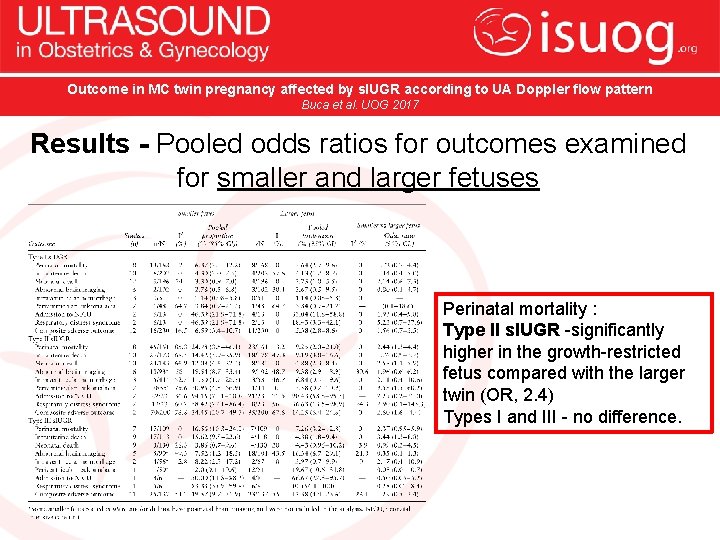

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Results - Pooled odds ratios for outcomes examined for smaller and larger fetuses Perinatal mortality : Type II s. IUGR -significantly higher in the growth-restricted fetus compared with the larger twin (OR, 2. 4) Types I and III - no difference.

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Results - Morbidity Abnormal postnatal brain imaging: • Twins affected by Type II (OR, 4. 9 ) or Type III (OR, 8. 2) s. IUGR had a significantly higher risk of compared with Type I s. IUGR. • No difference in the growth-restricted compared with the larger twin for all s. IUGR types. IVH and PVL: • Both were significantly higher in Type II compared with Type I s. IUGR, (OR, 10. 6 and 4. 4, respectively). • No increased risk in either IVH or PVL in Type II compared with Type III. NICU admission: • Risk was higher in Type II compared with Type I s. IUGR (OR, 18. 3). • No difference between Type II vs III and Type I vs III s. IUGR. • Not difference between the smaller and larger twins for all s. IUGR types.

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Results - Morbidity Composite adverse outcome: • Risk was higher in Type II (OR, 4. 9) and Type III (OR, 5. 1) compared with Type I s. IUGR. • No difference between Type II and Type III s. IUGR. Deterioration of fetal status: • Risk was higher in Type II compared with Type I (OR, 7. 2 ) and Type III (OR, 16. 1). • No difference in risk in Type I vs III s. IUGR. Mean gestational age at delivery: • Twin pregnancies affected by Type I s. IUGR were delivered at a significantly later gestational age than those with Type II (33. 7 vs 34. 3 weeks; MD, 2. 8 weeks) and Type III (33. 7 vs 30. 9 weeks; MD, 2. 1 weeks). • No difference in gestational age at delivery between Type II and Type III s. IUGR.

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Main findings • Type II s. IUGR is at a higher risk of perinatal mortality and morbidity, abnormal postnatal brain imaging and admission to NICU compared to Type I • The likelihood of an abnormal outcome is usually not significantly different between Types II and III. • Type III s. IUGR is affected by an unpredictable clinical course. • Pregnancies affected by Types II and III s. IUGR are delivered at a significantly earlier gestational age than those affected by Type I. • Pregnancies affected by Type II have a higher degree of BW discordance compared with Types I and III.

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Limitations • Small number of cases in some of the included studies. • Retrospective non-randomized design in some of the included studies. • Heterogeneity in prenatal management - data may be largely affected by the different protocols rather than the natural history of the condition. • Different periods of follow up. • Most of the observed outcomes were reported by only a limited proportion of the included studies preventing the stratification of the analysis according to different gestational ages at presentation of s. IUGR, type of UA flow abnormality (absent vs reversed end-diastolic flow) and different subtypes of neuromorbidity.

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Conclusions – Implications for clinical practice Type I s. IUGR: • Most likely represents the milder spectrum of growth restriction in MC twins. • The degree of unequal placental sharing between the twins is smaller than for the other types of s. IUGR, thus precluding a large discrepancy in fetal size. The relatively small number of arterioarterial anastomoses compared with the other s. IUGR types allows relative hemodynamic stability between the twins, which is reflected in the lower occurrence of perinatal death and postnatal brain damage • In the absence of Doppler abnormalities - follow up conservatively with weekly ultrasound scans.

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Conclusions – Implications for clinical practice Type II s. IUGR: • These pregnancies are affected commonly by severe discordance in fetal weight and by progressive abnormalities in arterial and venous Doppler, requiring delivery at an earlier gestational age. However, the latency between onset of UA flow anomalies and delivery is usually longer than that in singleton and dichorionic twin gestations. • The optimal prenatal management should be tailored according to the gestational age at diagnosis, the degree of fetal weight discordance and the severity of Doppler abnormalities. • Follow up with biweekly scans in the presence of absent or reversed end-diastolic flow in the UA, followed by delivery when venous Doppler abnormalities occur. (Confirmation in prospective trial is required. ) • Prenatal therapy (cord occlusion, laser coagulation of placental anastomoses) can be considered before viability. (Relatively high rate of cotwin loss or maternal complications, and is technically more difficult than when performed for TTTS).

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Conclusions – Implications for clinical practice Type III s. IUGR: • Type III s. IUGR is characterized by the presence of intermittent absent or reversed enddiastolic flow in the UA of the smaller twin, due to the peculiar vascular arrangement of Type III s. IUGR placentae, which show significantly more large arterioarterial anastomoses compared with uncomplicated Types I and II s. IUGR twins. • The clinical course of pregnancies with Type III s. IUGR is mainly determined by the magnitude and direction of blood exchange, which may lead to different clinical outcomes, even in twins showing the same degree of growth discrepancy. • Type III s. IUGR is affected by a high rate of unexpected fetal demise, even in the case of stable Doppler findings, thus questioning the actual role of Doppler ultrasound. • Management of Type III s. IUGR is arbitrary; several factors such as gestational age at diagnosis, degree of growth discordance and severity of Doppler anomalies may help the decision planning, but parents should be counseled about the unpredictable clinical course of these pregnancies. Fetal therapy may be considered before viability.

Outcome in MC twin pregnancy affected by s. IUGR according to UA Doppler flow pattern Buca et al. UOG 2017 Points for discussion • Is UA Doppler flow pattern also of value in MC twins without s. IUGR? • Is UA Doppler flow pattern also of value in MC twins with discordancy? • Can early changes in UA Doppler flow pattern predict the later occurrence of s. IUGR? • Can MC twins with Type III s. IUGR be better stratified by UA Doppler flow?
- Slides: 16