Unnecessary complications of an unnecessary procedure Albert J

Unnecessary complications of an unnecessary procedure Albert J Mifsud

Mr Travers* • 56 year old civil engineer working in various locations in central Europe for previous 5 years • presented to his general practitioner with symptoms of bladder outflow obstruction • Prostate specific antigen (PSA) performed: 4. 9 ng/ml • Referred to urology clinic in local DGH * fictitious name

Initial presentation: April 12 • Presented to his general practitioner with symptoms of bladder outflow obstruction • Prostate Specific Antigen (PSA) performed: 4. 9 ng/ml • Referred to urology clinic in local DGH • Returned to Romania

Urology Clinic, July 2012 • Symptoms – urinary frequency (increasing over several months) – reduced flow (increasing over years) – some perineal discomfort (new) • On examination – apyrexial – Sl. tender mildly uniformly enlarged prostate

Investigations • MSU (microscopy) – 35 WBCs – No growth • PSA – 4. 8 ng/ml • In view of persistently elevated PSA, listed for prostate biopsy

Prostate biopsy: November 12 • Pre-assessment – penicillin allergy documented • 5 th November (09: 30 hrs) : biopsy performed under LA – Ciprofloxacin 500 mg commenced 2 hrs prior to biopsy – Prescription for Ciprofloxacin 500 mg bd 3 days issued


Do you agree with this course of action? Co-ordinator prompts • Should investigation and treatment for prostatitis been undertaken (avoid as outside scope of this topic)? • Is ciprofloxacin an appropriate agent to be used for prophylaxis for TRUS (avoid as outside scope of this topic)?

Post-biopsy course • Circa 18 hrs post biopsy (03: 00 hrs, 6 th Nov) – developed rigors – felt unwell – temp: 39. 8 o. C – pulse rate: 110 bpm – bp: 135/70 mm. Hg • Admitted under urology team (04: 00 hrs) – diagnosis of sepsis post TRUS biopsy + SIRS

What would you do now? Co-ordinator prompts (1) • Further history – Elucidation of nature of allergy – Nature of symptoms (with respect to prostatitis) • Investigations – Routine – Blood culture / rpt. MSU

• • Co-ordinator prompts (2) Severity assessment Assessment of need for supportive care Antibiotics: Discussion around nature of allergy and antibiotics advised / contraindicated

Initial management • Blood cultures collected • Treatment decision: – ‘IV antibiotics: Tigecycline as allergic to Amoxil’ – 100 mg loading dose (within 30 mins), 50 mg bd • FBC, U&E, CRP: largely normal

Do you agree with this approach? • September 2010: US FDA safety communication • April 2011: UK MHRA safety warning • (I have written a briefing note previously, but should be checked)

Progress, 6 th November • 15: 20 hrs, while on Tigecycline: – further rigors • microbiology contacted. Notes state – repeat blood / urine cultures – single dose of gentamicin (600 mg) • later (untimed): – temp 40. 8 o. C – haematuria

7 th November • 01: 00 hrs – temp 38. 2 o. C; pulse rate 112 bpm; – BP 79/47 mm. Hg – urinary retention (catheterised) – resuscitation with fluids – reviewed by ITU team • 13: 00 hrs – Blood cultures: Gram negative rods

8 th November • Progress: – Pyrexia, tachycardia settled – Hypotension persisted (80 -100 mg. Hg systolic) • Blood culture result: – E. coli – ESBL pattern, S gent, imipenem, tigecycline • Microbiologist advice (telephone) : – continue tigecycline 48 hrs, switch to imipenem if no improvement

Do you agree with this approach?

th 9 – th 18 November • Initial improvement, but interspersed with hypotensive periods • Microbiology advice (telephone) 9 th Nov: – Continue gent (but incorrect info provided) – Switch to imipenem, ‘with caution’ due to allergy • However, tigecycline continued • Eventual improvement: discharged (18/11) after 12 d course of tigecycline
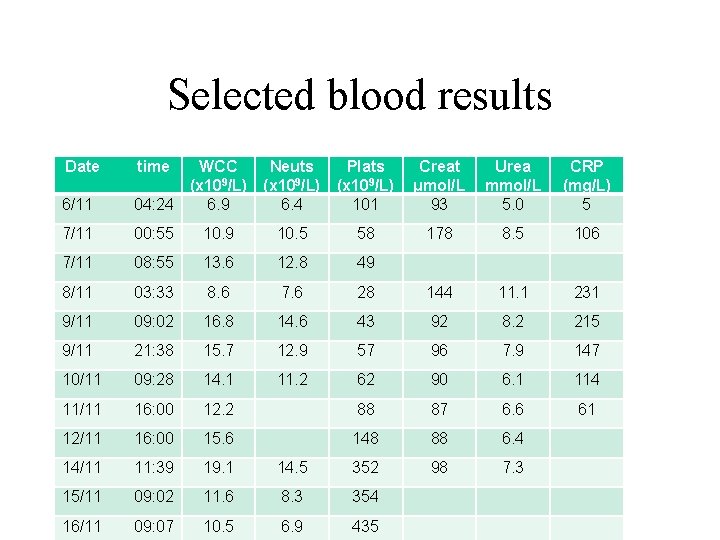
Selected blood results Date time 6/11 WCC (x 109/L) 04: 24 6. 9 Neuts (x 109/L) 6. 4 Plats (x 109/L) 101 Creat μmol/L 93 Urea mmol/L 5. 0 CRP (mg/L) 5 7/11 00: 55 10. 9 10. 5 58 178 8. 5 106 7/11 08: 55 13. 6 12. 8 49 8/11 03: 33 8. 6 7. 6 28 144 11. 1 231 9/11 09: 02 16. 8 14. 6 43 92 8. 2 215 9/11 21: 38 15. 7 12. 9 57 96 7. 9 147 10/11 09: 28 14. 1 11. 2 62 90 6. 1 114 11/11 16: 00 12. 2 88 87 6. 6 61 12/11 16: 00 15. 6 148 88 6. 4 14/11 11: 39 19. 1 14. 5 352 98 7. 3 15/11 09: 02 11. 6 8. 3 354 16/11 09: 07 10. 5 6. 9 435

Relapse, December 2012 • 1 st December (i. e. 8 days later) presented with 2 day history of dysuria, frequency and shivering. • On examination: temp 37. 8 o. C, tachycardic (120 bpm) but normotensive (115/70 mm. Hg) • Drug chart: ‘ penicillin headache’ • Re-started on tigecycline

What would you do now? Co-ordinator prompts • Meets SIRS / Sepsis criteria? • Further investigations / considerations? • Antibiotic choices?

Progress nd (2 day) • Next day developed pyrexia (38. 4 o. C), but remained haemodynamically stable • Discussed with microbiology (telephone): gentamicin advised • Remained pyrexial: MI scan showed multiple abscesses within prostate • Blood cultures, urine from 2/12: coliform with sens pattern as previously • Microbiologist advised gent +

Subsequent progress • Rapid recovery ensued over next 24 hrs • Microbiologist advice (telephone): ‘only option is full 14 day course of gentamicin plus metronidazole’. • Meticulous monitoring of gentamicin levels with Hartford nomogram undertaken.

Outcome • Presented to GP 1 wk later with unsteadiness • Diagnosis of vestibular failure due to gentamicin made.

Lessons learnt Co-ordinator prompts: • Importance of investigating claimed allergies • True risks of use of penicillins and betalactams in such patients • Alternatives in apparently-true Type I hypersensitivity
- Slides: 25