UNMET NEEDS OF PATIENTS WITH Hb DISORDERS THE

UNMET NEEDS OF PATIENTS WITH Hb DISORDERS THE THALASSAEMIA PERSPECTIVE GLOBALLY AND IN EUROPE December, 2020

About the Thalassaemia International Federation TIF Membership TODAY: 232 National Thalassaemia Associations from 62 countries EUR AMR Albania, Austria, Azerbaijan, Belgium, Bulgaria, Cyprus, Denmark, France, Germany, Greece, Ireland, Israel, Italy, Luxembourg, Malta, Netherlands, Portugal, Romania, Spain, Sweden, Turkey, UK Argentina, Canada, Trinidad & Tobago, USA Afghanistan, Bahrain, Egypt, Iran, Iraq, Jordan, Kuwait, Lebanon, Morocco, EMR Pakistan, Palestine, Saudi Arabia, Sudan, Syria, Tunisia, UAE, Yemen SEAR Vision: To strengthen research for better care & cure and to provide equal and timely access to quality health, social and other care for all patients with thalassaemia globally, in a truly patient-centred healthcare setting Mission: Development and implementation of national disease – specific control programmes within national healthcare systems based on universal coverage Working in official relations with the World Health Organization (WHO) since 1996 In special consultative status with the United Nations Economic and Social Council (ECOSOC) since 2017 Official Partners of the European Commission in the field of Health since 2018 Participatory status at the Council of Europe since 2019 PILLARS OF ACTIVITIES Bangladesh, India, Indonesia, Maldives, Myanmar, Nepal, Sri Lanka, Thailand Australia, Cambodia, China PDR (including Hong Kong SAR of China and Taiwan WPR Province of China), Malaysia, Philippines, Singapore, Taiwan, Vietnam AFR Algeria, Congo, Ghana, Mauritius, Nigeria, South Africa 2
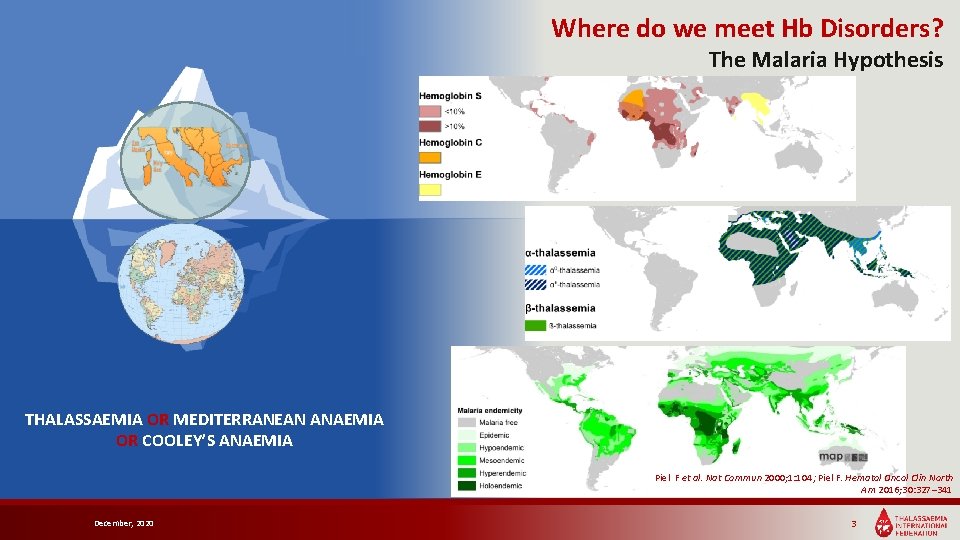
Where do we meet Hb Disorders? The Malaria Hypothesis THALASSAEMIA OR MEDITERRANEAN ANAEMIA OR COOLEY’S ANAEMIA Piel F et al. Nat Commun 2000; 1: 104; Piel F. Hematol Oncol Clin North Am 2016; 30: 327– 341 December, 2020 3
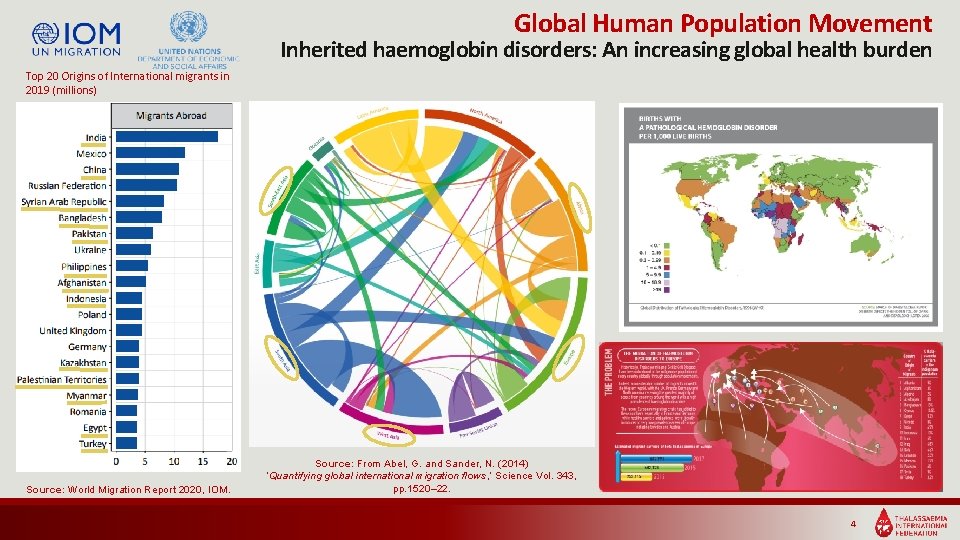
Global Human Population Movement Inherited haemoglobin disorders: An increasing global health burden Top 20 Origins of International migrants in 2019 (millions) Source: World Migration Report 2020, IOM. Source: From Abel, G. and Sander, N. (2014) ‘Quantifying global international migration flows, ’ Science Vol. 343, pp. 1520– 22. 4
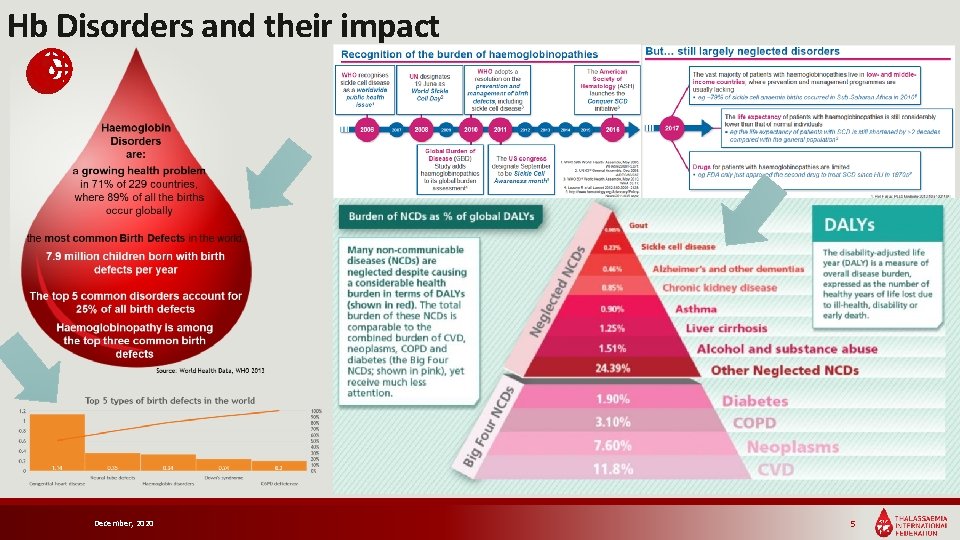
Hb Disorders and their impact December, 2020 5
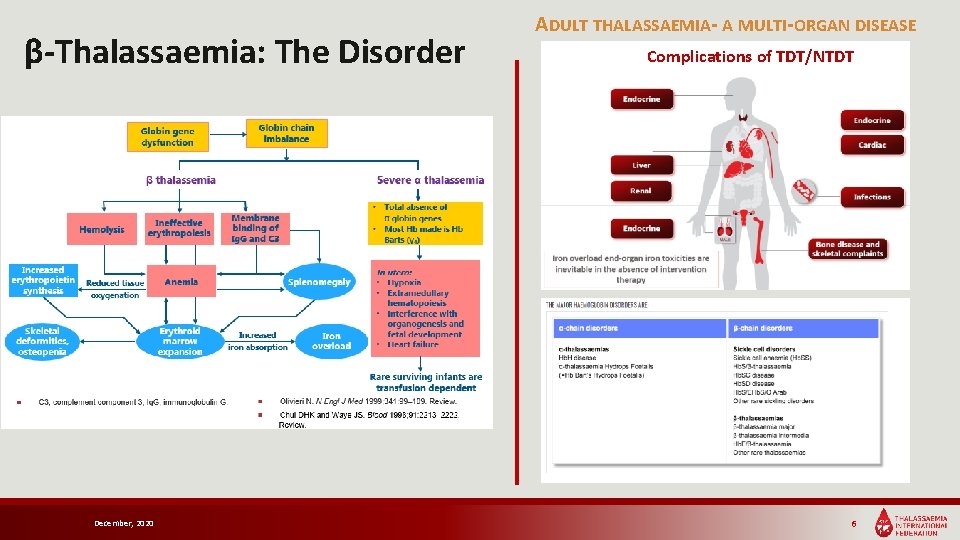
β-Thalassaemia: The Disorder December, 2020 ADULT THALASSAEMIA- A MULTI-ORGAN DISEASE Complications of TDT/NTDT 6

Can we effectively address the control of Hb disorders? ! S E Y The β-thal perspective Mediterranean countries supported by the UK & France (initially) have documented success. National Management Programmes EFFECTIVE PATIENT OUTCOMES December, 2020 National Prevention Strategies EFFECTIVE • • • SCREENING AWARENESS PRENATAL DIAGNOSIS/PRE-IMPLANTATION DIAGNOSIS REGISTRIES GUIDELINES CME REFERENCE CENTRES/NETWORKING TRANSFUSION POLICIES PUBLIC HEALTH AVAILABILITY OF AND ACCESSIBILITY TO DRUGS MONITORING DISEASE/TREATMENT Outside of a National Programme INEFFECTIVE Outside of a National Programme POOR TO NO BENEFIT 7
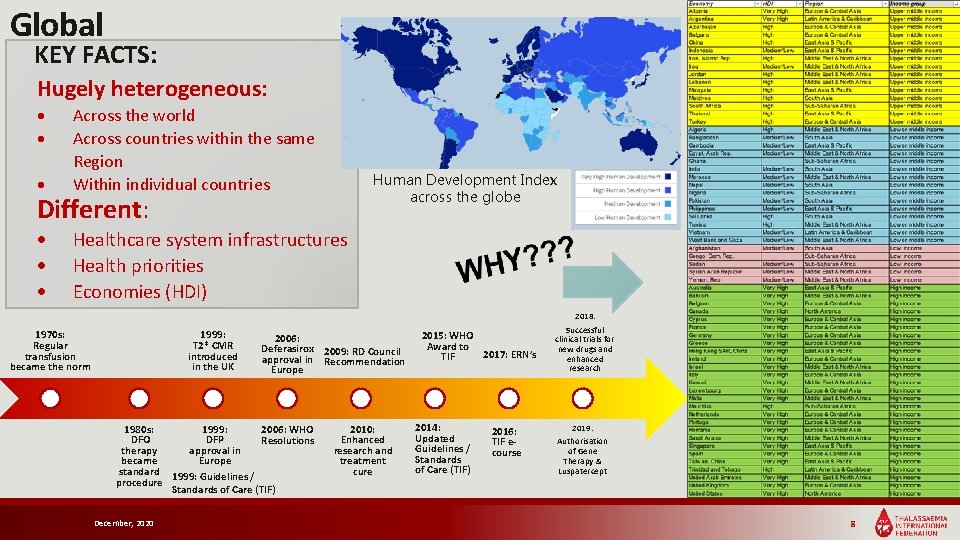
Global KEY FACTS: Hugely heterogeneous: Across the world Across countries within the same Region Within individual countries Healthcare system infrastructures Health priorities Economies (HDI) Human Development Index across the globe Different: 1970 s: Regular transfusion became the norm 1999: T 2* CMR introduced in the UK 2006: Deferasirox 2009: RD Council approval in Recommendation Europe 1980 s: 1999: 2006: WHO DFP Resolutions therapy approval in became Europe standard 1999: Guidelines / procedure Standards of Care (TIF) December, 2020 2010: Enhanced research and treatment cure 2015: WHO Award to 2017: ERN’s TIF 2014: Updated Guidelines / Standards of Care (TIF) 2016: TIF ecourse 2018: Successful clinical trials for new drugs and enhanced research 2019: Authorisation of Gene Therapy & Luspatercept 8
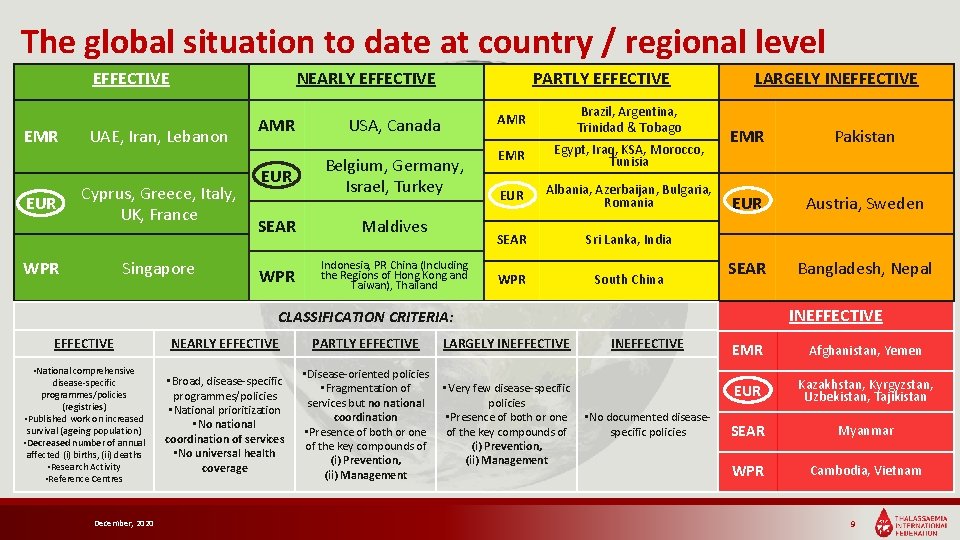
The global situation to date at country / regional level EFFECTIVE EMR EUR NEARLY EFFECTIVE UAE, Iran, Lebanon Cyprus, Greece, Italy, UK, France WPR Singapore AMR EUR PARTLY EFFECTIVE USA, Canada Belgium, Germany, Israel, Turkey SEAR Maldives WPR Indonesia, PR China (Including the Regions of Hong Kong and Taiwan), Thailand AMR Brazil, Argentina, Trinidad & Tobago EMR Egypt, Iraq, KSA, Morocco, Tunisia EUR Albania, Azerbaijan, Bulgaria, Romania SEAR Sri Lanka, India WPR South China LARGELY INEFFECTIVE EMR Pakistan EUR Austria, Sweden SEAR Bangladesh, Nepal INEFFECTIVE CLASSIFICATION CRITERIA: EFFECTIVE NEARLY EFFECTIVE PARTLY EFFECTIVE LARGELY INEFFECTIVE • National comprehensive disease-specific programmes/policies (registries) • Published work on increased survival (ageing population) • Decreased number of annual affected (i) births, (ii) deaths • Research Activity • Reference Centres • Broad, disease-specific programmes/policies • National prioritization • No national coordination of services • No universal health coverage • Disease-oriented policies • Fragmentation of services but no national coordination • Presence of both or one of the key compounds of (i) Prevention, (ii) Management • Very few disease-specific policies • Presence of both or one of the key compounds of (i) Prevention, (ii) Management December, 2020 INEFFECTIVE • No documented diseasespecific policies EMR Afghanistan, Yemen EUR Kazakhstan, Kyrgyzstan, Uzbekistan, Tajikistan SEAR Myanmar WPR Cambodia, Vietnam 9
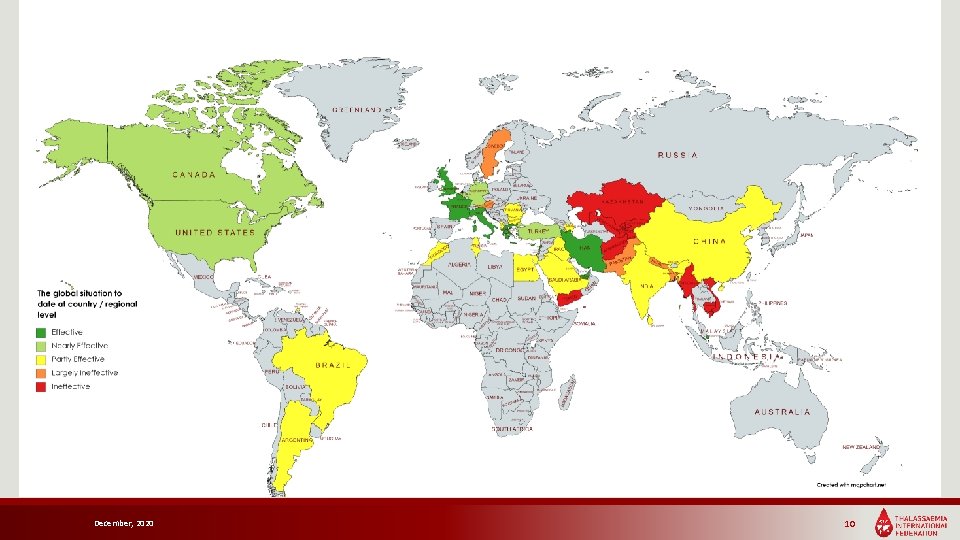
December, 2020 10

Unmet Policy-orientated Needs across the world – TIF’s perspective Global overview of common challenges § Confined number of national control strategies: ü well-coordinated prevention and management programmes ü disease-specific registries § Neglected work on epidemiological work (micromapping) December, 2020 Absence of sufficient and quality evidence to support policy-making, prioritization & global funding in countries with > 80% Global Patient Population § Poor/weak healthcare/public health infrastructure § Other health-related priorities: Communicable diseases § Healthcare systems devoid of universal health coverage (many countries in transition stage) SGD UN 2030 → Goal 3 Consequently: § Confined reflection of the true and essential patient needs § Absence or limited work on the appropriate planning of medical/public health/ social services & programmes § Failure to accurately describe the contribution of Hb Disorders to the global/regional/national disease burden. 11
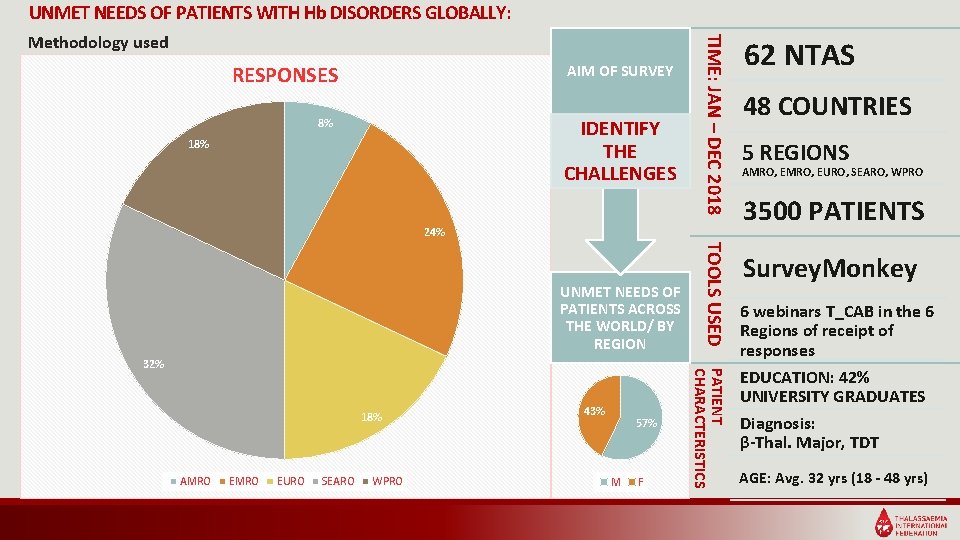
UNMET NEEDS OF PATIENTS WITH Hb DISORDERS GLOBALLY: AIM OF SURVEY RESPONSES IDENTIFY THE CHALLENGES 8% 18% TIME: JAN – DEC 2018 Methodology used 24% 18% AMRO EURO SEARO WPRO 43% 57% M F PATIENT CHARACTERISTICS 32% TOOLS USED UNMET NEEDS OF PATIENTS ACROSS THE WORLD/ BY REGION 62 NTAS 48 COUNTRIES 5 REGIONS AMRO, EURO, SEARO, WPRO 3500 PATIENTS Survey. Monkey 6 webinars T_CAB in the 6 Regions of receipt of responses EDUCATION: 42% UNIVERSITY GRADUATES Diagnosis: β-Thal. Major, TDT AGE: Avg. 32 yrs (18 - 48 yrs)
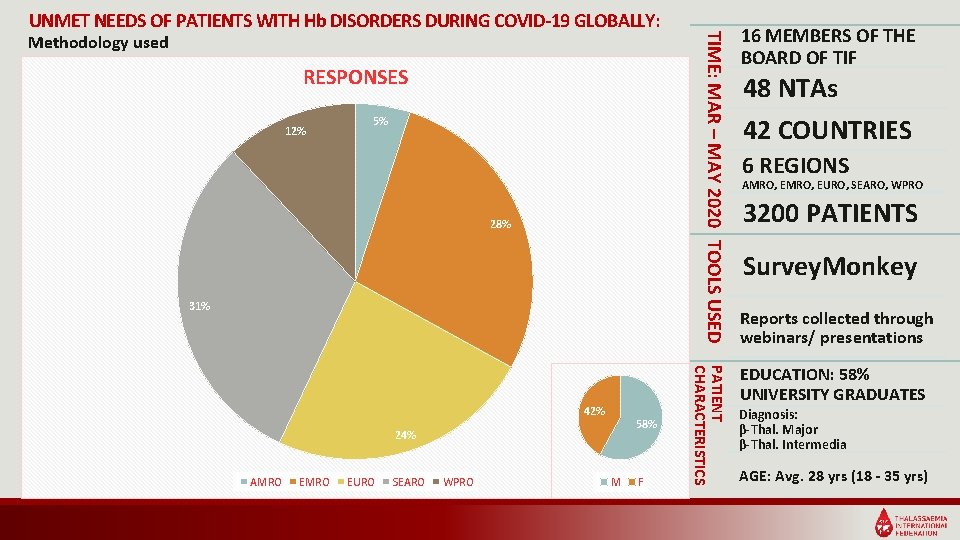
Methodology used RESPONSES 12% 5% 28% 31% 58% 24% AMRO EURO SEARO WPRO M F PATIENT CHARACTERISTICS 42% TIME: MAR – MAY 2020 TOOLS USED UNMET NEEDS OF PATIENTS WITH Hb DISORDERS DURING COVID-19 GLOBALLY: 16 MEMBERS OF THE BOARD OF TIF 48 NTAs 42 COUNTRIES 6 REGIONS AMRO, EURO, SEARO, WPRO 3200 PATIENTS Survey. Monkey Reports collected through webinars/ presentations EDUCATION: 58% UNIVERSITY GRADUATES Diagnosis: β-Thal. Major β-Thal. Intermedia AGE: Avg. 28 yrs (18 - 35 yrs)
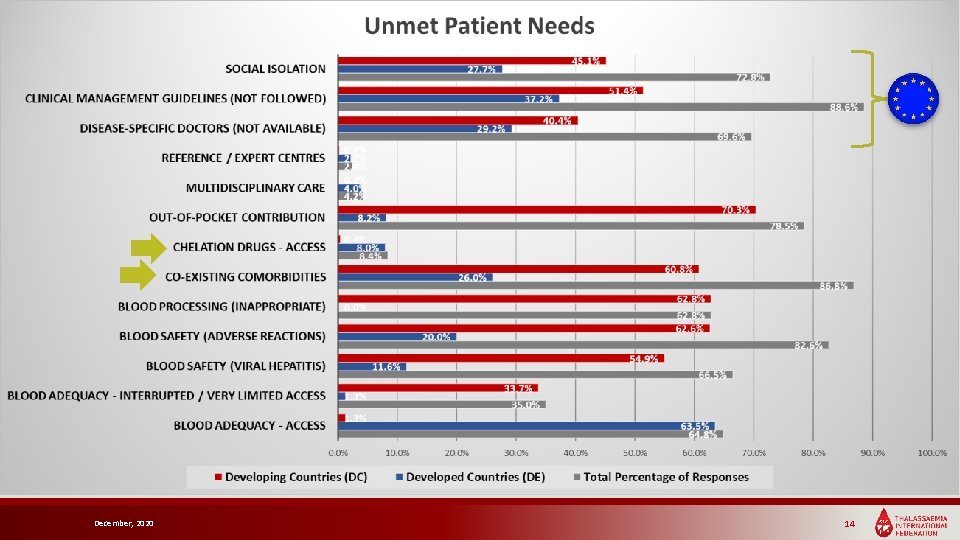
December, 2020 14
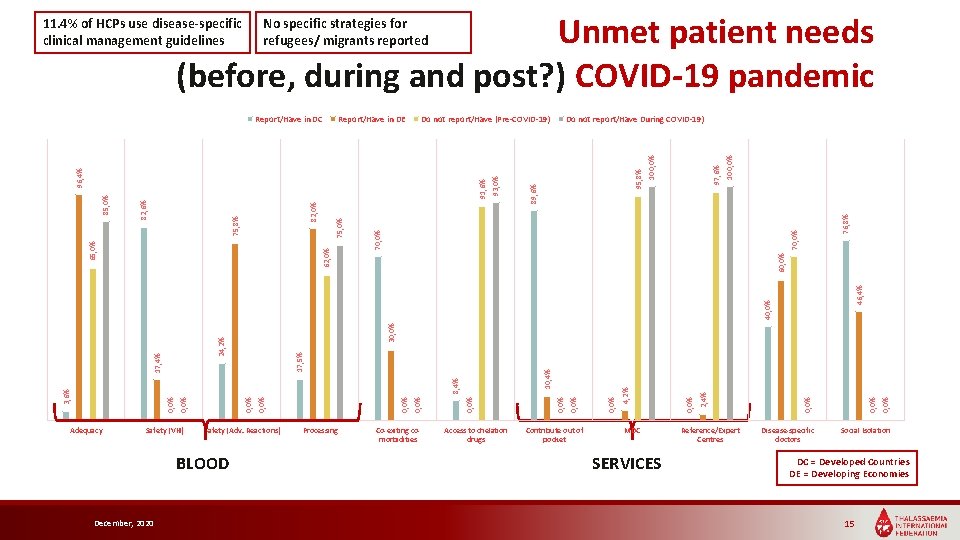
Unmet patient needs (before, during and post? ) COVID-19 pandemic No specific strategies for refugees/ migrants reported Adequacy Safety (VH) Safety (Adv. Reactions) BLOOD December, 2020 Processing Co-exiting comorbidities Access to chelation drugs Contribute out of pocket MDC SERVICES Reference/Expert Centres Disease-specific doctors 0, 0% 2, 4% 0, 0% 4, 2% 0, 0% 0, 0% 0, 0% 3, 6% 8, 4% 10, 4% 17, 5% 17, 4% 24, 2% 30, 0% 46, 4% 60, 0% 76, 8% 100, 0% 97, 6% 100, 0% 91, 6% 70, 0% 62, 0% 75, 0% 82, 0% 75, 8% 82, 6% 85, 0% 65, 0% Do not report/Have During COVID-19) 95, 8% Do not report/Have (Pre-COVID-19) 89, 6% Report/Have in DE 96, 4% Report/Have in DC 93, 0% 11. 4% of HCPs use disease-specific clinical management guidelines Social Isolation DC = Developed Countries DE = Developing Economies 15

Hb Disorders Unmet needs of patients in EUROPE HUMAN/PATIENTS’ RIGHTS FULLY RESPECTED (EU and extended) ü Universally Covered Healthcare Systems (UHC) ü Quality of HC services safeguarded (Directives, Regulations, Recommendations) ü Strong Medicinal Regulatory Agency – EMA (safe/effective medicines, including ATMPs) ü Regulated Medical/ Nursing/ Scientific professions ü Strong Research activity/ clinical trials ü Work and specific policies focused on Rare Diseases since 1999 § § Cross border Directive European Reference Networks e. g. EUROBLOODNET recognition ü STRONG PATIENTS’ VOICE AND INVOLVEMENT (EC, EMA, ERNS, EHA, EASL) December, 2020 Dörrbecker, M. D. (2015). European migrant crisis. Wikipedia. https: //en. wi kipedia. org/ wiki/Europea n_migrant_cr isis#/media/F ile: Map_of_t he_European _Migrant_Cri sis_2015. png BUT NO POLICIES FOR IMMIGRANT POPULATION 16
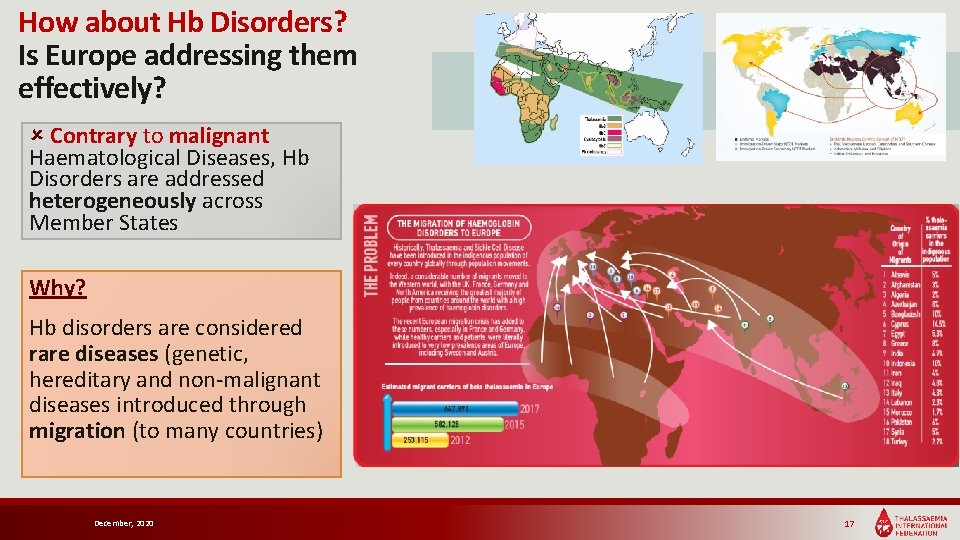
How about Hb Disorders? Is Europe addressing them effectively? Contrary to malignant Haematological Diseases, Hb Disorders are addressed heterogeneously across Member States Why? Hb disorders are considered rare diseases (genetic, hereditary and non-malignant diseases introduced through migration (to many countries) December, 2020 17
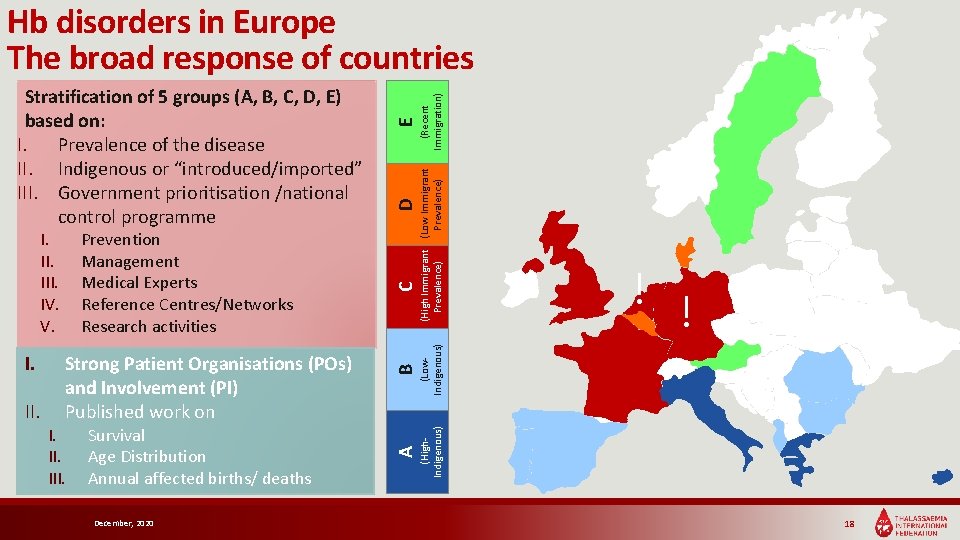
II. I. III. Survival Age Distribution Annual affected births/ deaths December, 2020 (High Immigrant (Low Immigrant Prevalence) E D C ! (Low. Indigenous) Strong Patient Organisations (POs) and Involvement (PI) Published work on ! (High. Indigenous) I. Prevention Management Medical Experts Reference Centres/Networks Research activities B I. III. IV. V. A Stratification of 5 groups (A, B, C, D, E) based on: I. Prevalence of the disease II. Indigenous or “introduced/imported” III. Government prioritisation /national control programme (Recent Immigration) Hb disorders in Europe The broad response of countries 18
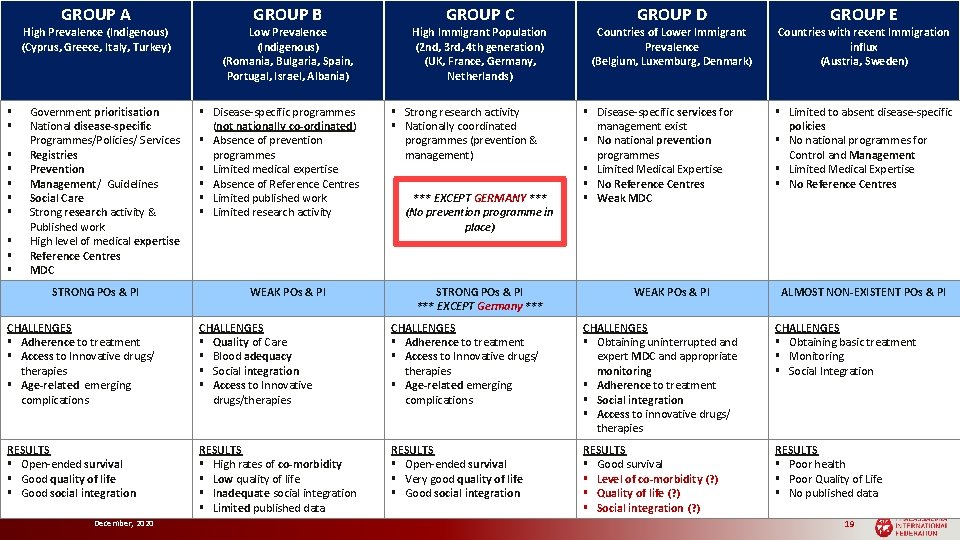
GROUP A High Prevalence (Indigenous) (Cyprus, Greece, Italy, Turkey) § § § § § Government prioritisation National disease-specific Programmes/Policies/ Services Registries Prevention Management/ Guidelines Social Care Strong research activity & Published work High level of medical expertise Reference Centres MDC STRONG POs & PI GROUP B Low Prevalence (Indigenous) (Romania, Bulgaria, Spain, Portugal, Israel, Albania) § Disease-specific programmes (not nationally co-ordinated) § Absence of prevention programmes § Limited medical expertise § Absence of Reference Centres § Limited published work § Limited research activity WEAK POs & PI GROUP C High Immigrant Population (2 nd, 3 rd, 4 th generation) (UK, France, Germany, Netherlands) § Strong research activity § Nationally coordinated programmes (prevention & management) *** EXCEPT GERMANY *** (No prevention programme in place) STRONG POs & PI *** EXCEPT Germany *** GROUP D Countries of Lower Immigrant Prevalence (Belgium, Luxemburg, Denmark) § Disease-specific services for management exist § No national prevention programmes § Limited Medical Expertise § No Reference Centres § Weak MDC WEAK POs & PI GROUP E Countries with recent Immigration influx (Austria, Sweden) § Limited to absent disease-specific policies § No national programmes for Control and Management § Limited Medical Expertise § No Reference Centres ALMOST NON-EXISTENT POs & PI CHALLENGES § Adherence to treatment § Access to Innovative drugs/ therapies § Age-related emerging complications CHALLENGES § Quality of Care § Blood adequacy § Social integration § Access to Innovative drugs/therapies CHALLENGES § Adherence to treatment § Access to Innovative drugs/ therapies § Age-related emerging complications CHALLENGES § Obtaining uninterrupted and expert MDC and appropriate monitoring § Adherence to treatment § Social integration § Access to innovative drugs/ therapies CHALLENGES § Obtaining basic treatment § Monitoring § Social Integration RESULTS § Open-ended survival § Good quality of life § Good social integration RESULTS § High rates of co-morbidity § Low quality of life § Inadequate social integration § Limited published data RESULTS § Open-ended survival § Very good quality of life § Good social integration RESULTS § Good survival § Level of co-morbidity (? ) § Quality of life (? ) § Social integration (? ) RESULTS § Poor health § Poor Quality of Life § No published data December, 2020 19
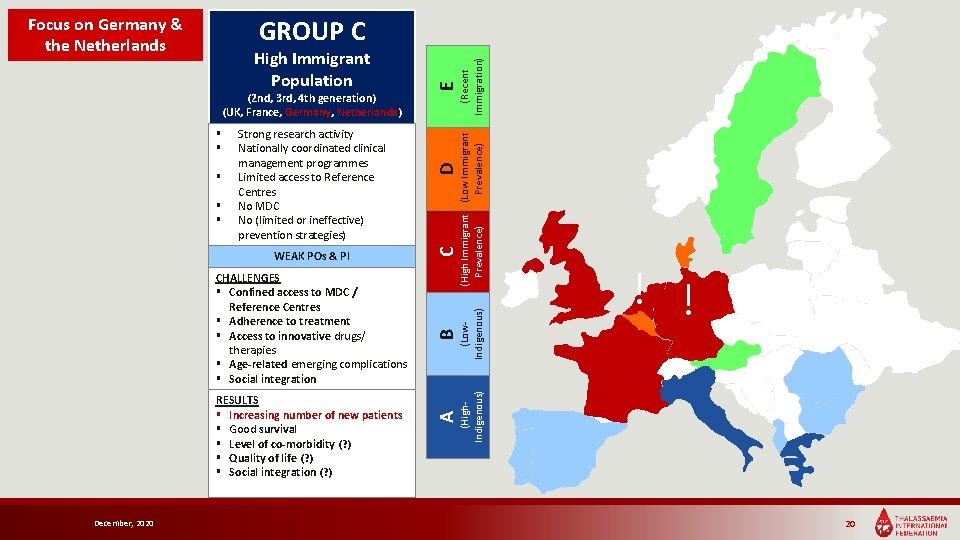
Focus on Germany & the Netherlands RESULTS § Increasing number of new patients § Good survival § Level of co-morbidity (? ) § Quality of life (? ) § Social integration (? ) December, 2020 E (High Immigrant (Low Immigrant Prevalence) CHALLENGES § Confined access to MDC / Reference Centres § Adherence to treatment § Access to innovative drugs/ therapies § Age-related emerging complications § Social integration (Low. Indigenous) WEAK POs & PI ! ! (High. Indigenous) § § D § Strong research activity Nationally coordinated clinical management programmes Limited access to Reference Centres No MDC No (limited or ineffective) prevention strategies) C § § B (2 nd, 3 rd, 4 th generation) (UK, France, Germany, Netherlands) A High Immigrant Population (Recent Immigration) GROUP C 20

European countries need to improve or build new Hb disease-specific policies: 1. Need to recognize the cost-effectiveness of developing National Strategies for the Prevention and Management of Hb Disorders 2. Development of National Registries to better plan the disease specific services 3. Identify and extend medical expertise through established educational activities, collaboration with TIF expert centres/ participating ERNs 4. Utilise the Cross Border Healthcare national legislation 5. Support the revision of EU directives Blood needs at national and EU levels are increasing ü Medical/community needs in BT (transfusion-dependent patients) ü Increasing numbers due to migration (absent / inadequate blood products) December, 2020 6. i) Strengthen education of patients on their disease and its management ii) Better relations between patients and treating physicians iii) More active and productive involvement of patients ALLTOGETHER IMPROVING ADHERENCE 7. Strengthen social and other care of patients across their life spectrum (education, profession, having a family, integrate fully into society) 8. i) Strengthen HTA and similar/ relevant tools & encourage Patient Involvement, to support evaluation of cost and access to innovation ii) Create cost models for the various components of the disease, treatment and care, dedicate special national funds for innovative therapies across the European Union Countries iii) Network of Countries / Alliance of countries for achieving increased negotiating power and better prices 9. Southern European Countries need to be protected and supported from health-related challenges that are linked to migration / Promotion of disease specific policies (THALIA) 21

“NEW” / RECENT MIGRATION WAVES ACROSS EUROPE (incl. TO SOUTH MEDITERRANEAN, CENTRAL, WEST AND NORTHERN EUROPE) S! IPLE MULT ENGE L L A H C Mainly from displaced population No policies/ decisions/ commitments on the National or EU level addressing Hb disoders No education/ awareness campaign Unidentified: Carriers/Groups Undiagnosed: Patients/ parents of children seeking blood transfusion and chelation Pregnant women visiting gynecologists at late stages for late intervention NUMBERS UNKNOWN ONLY ESTIMATED ARE ON CARRIER RATE (ALSO ESTIMATE) OF COUNTRY OF BIRTH December, 2020 22

THANK YOU FOR YOUR ATTENTION December, 2020 23
- Slides: 23