Universal Screening 101 Depression Anxiety Substance Use in

Universal Screening 101: Depression, Anxiety & Substance Use in Primary Care Transformation Collaborative of RI FEBRUAR Y 28, 2019 NELLY BUR DE TTE, PSYD 1

Objectives • Describe importance of screening and rates of depression, anxiety and substance use in primary care • Understand how to administer, score and interpret the following screening tools in primary care: • PHQ 9 (Depression) • GAD 7 (Anxiety) • CAGE-AID (Alcohol and Substance Use) 2

Depression in Primary Care • 18. 8 million adults • 9. 5% of the U. S. population aged 18 years and older in a given year. 3 • More than 80% of patients with depression have a medical comorbidity 5 • PCPs detect major depression in 1/3 - 1/2 of patients 5 • 570 -80% of antidepressants prescribed in primary care • Only 20 -40% showing substantial improvement over 12 months 5 3

PHQ 9 • Purpose: dual purpose 9 item depression scale that can establish provisional depression diagnosis and grade depressive symptom severity • Target Population: Adults age 18 and over • Evidence: Validated for measuring depression severity; detecting and monitoring depression in primary care settings 4 • Estimated Time: 2 -5 min • Administered by: Patient (self-report), Provider, Telephonically • Intended Settings: Primary Care 4

PHQ 9 Administration • Ask the first two questions and continue with remaining questions if score > 3 • Score > 3 = 83% sensitivity for major depression, 90% specificity 4 • High rates of false positives when lowering cutoff to 2 1 • Nine scored questions • Total 27 points • Each question having ranging from 0 -3 • All focusing on past 2 weeks • Tenth question focuses on ADLs and is not scored 5

PHQ 9 Administration 6

7

PHQ 9 Scoring and Plan 8
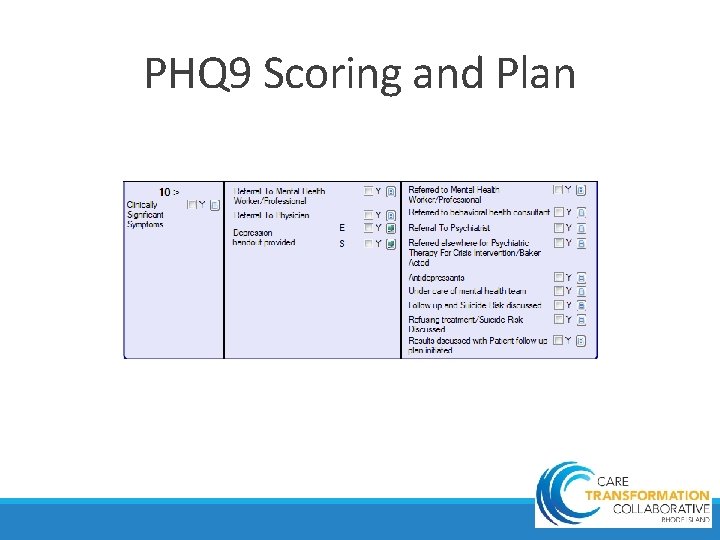

PHQ 9 Scoring and Plan 9

PHQ 9 Repeat 4 Administrations • Detecting depression and initiating treatment are NECESSARY but often INSUFFICIENT steps to improve outcomes in primary care • Monitoring clinical response to treatment is also CRITICAL. • 5 -point change correlates with a moderate effect size on multiple domains of health-related quality of life and functional status • Total score of <10 = partial response and <5 = remission 10

Anxiety in Primary Care • Occurs among 7 -8% primary care patients 8 and in general population 30% 9 • Predominant presentation includes headaches or GI distress, not worry 8 • Anxiety continues to be undertreated in primary care • Adequate pharmacotherapy received < 20% • Adequate psychotherapy received 14% • Both pharmacotherapy and psychotherapy received by 5% • TOTAL: Quarter of patients received adequate care 9 11

12

GAD 7 • Purpose : evaluate for presence and severity of anxiety in general practice, as well as monitoring change across time 7 • Target Population: Adults age 18 and over • Evidence 1: Panic Disorder Social Anxiety Disorder PTSD - Sensitivity: 74% Specificity: 81% Sensitivity: 72% Specificity: 80% Sensitivity: 66% Specificity: 81% • Estimated Time: 2 -5 minutes • Administered by: Self-Report • Intended Settings: Primary Care 13
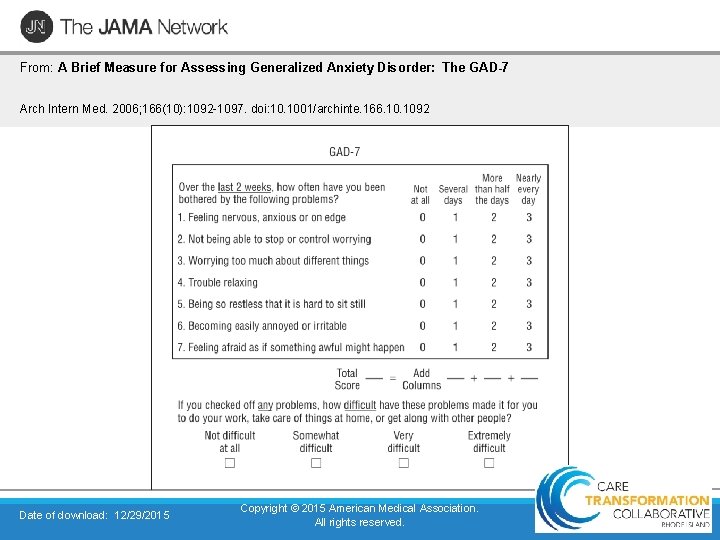

From: A Brief Measure for Assessing Generalized Anxiety Disorder: The GAD-7 Arch Intern Med. 2006; 166(10): 1092 -1097. doi: 10. 1001/archinte. 166. 1092 Date of download: 12/29/2015 Copyright © 2015 American Medical Association. All rights reserved.

GAD 7 Scoring and Plan • Cognitive-behavioral and SSRI/SNRI agents are effective in reducing symptoms in up to 50% of patients 8 • If a 50% or more decrease in treatment does not occur within 3 months of treatment, different or adjunctive treatment should be offered 8 15

Substance Use in Primary Care 6 • 22. 5 million persons older than 12 years meet criteria for substance abuse or dependence • < 20% of PCPs described themselves as very prepared to identify alcoholism or illegal drug use • More than 50% of patients with substance use disorders said their PCP did nothing to address their substance abuse. 16

CAGE-AID • Purpose: Assesses likelihood and severity of alcohol and drug use; modified from CAGE • Target Population: Adults aged 18 years and older • Evidence: One or more yes responses has sensitivity of 0. 79 and specificity of 0. 77; Two of more yes responses has sensitivity of 0. 70 and 0. 85. 2 • Estimated Time: 1 minute • Length: 4 yes/no questions • Intended Settings: Primary care 17

CAGE AID 18
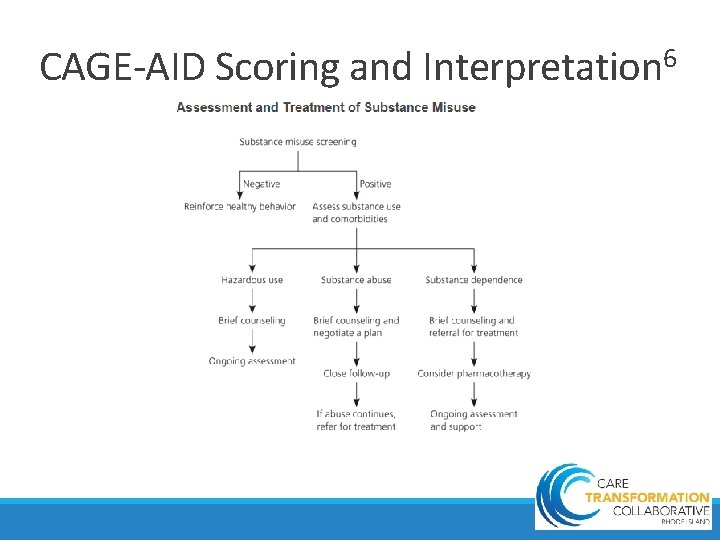
CAGE-AID Scoring and 6 Interpretation 19

Resources • PHQ and GAD Language Translation Options http: //www. phqscreeners. com • IMPACT for Depression, Evidence-Based Collaborative Care in Primary Care Setting http: //impact-uw. org/ 20

Final Thoughts • Screening for behavioral health does NOT equate to a behavioral health diagnosis. • Workflows should be in place to connect patients with positive screens to IBH providers for treatment. • Not “One and Done”; follow-up screenings should measure progress and allow for evidence to make changes to treatment options 21

References 1. Arroll, B. , Goodyear-Smith, F. , Crengle, S. , Gunn, J. , Kerse, N. , Fishman, T. , Falloon, K. , Hatcher, S. (2010). Validation of PHQ-2 and PHQ-9 to Screen for Major Depression in Primary Care Population. Annals of Family Medicine, 8 (4): 348 -353. 2. Brown, R. L. and Rounds, L. A. (1995). Conjoint screening questionnaires for alcohol and other drug abuse: criterion validity in a primary care practice. Wisconsin Medical Journal, 94(3): 135 -40. 3. Egede, L. E. (2007). Failure to Recognize Depression in Primary Care: Issues and Challenges. Journal of General Internal Medicine, 22(5), 701– 703. 4. Kroenke K, Spitzer R. (2002). The PHQ-9: A New Depression Diagnostic and Severity Measure. Psychiatry Annals. 32: 509 -515. 5. Mitchell J, Trangle M, Degnan B, Gabert T, Haight B, Kessler D, Mack N, Mallen E, Novak H, Rossmiller D, Setterlund L, Somers K, Valentino N, Vincent S. Institute for Clinical Systems Improvement. Adult Depression in Primary Care. Updated September 2013. 6. Shapiro, B. , Coffa, D. , Mc. Cance-Katz, E. F. (2013). A primary care approach to substance misuse. American Family Physician. 88 (2): 113 -21. 7. Spitzer RL, Kroenke K, Williams JW, Löwe B. (2006). A Brief Measure for Assessing Generalized Anxiety Disorder: The GAD-7. Archives Internal Medicine. 166(10): 1092 -1097. 8. Stein, M. B and Sareen, J. (2015). Generalized Anxiety Disorder. New England Journal of Medicine. 373(21): 2059 -2068. 9. Weisberg, R. B. , Beard, C. , Moitra, E. , Dyck, I. , Keller, M. B. (2014). Adequacy of Treatment Received by Primary Care Patients with Anxiety Disorders. Depression Anxiety. 31 (5): 443 -450. 22
- Slides: 22