Unit Seven Gastrointestinal Alterations Gastrointestinal Assessment and Diagnostic
























































- Slides: 57

Unit Seven Gastrointestinal Alterations Gastrointestinal Assessment and Diagnostic Procedures

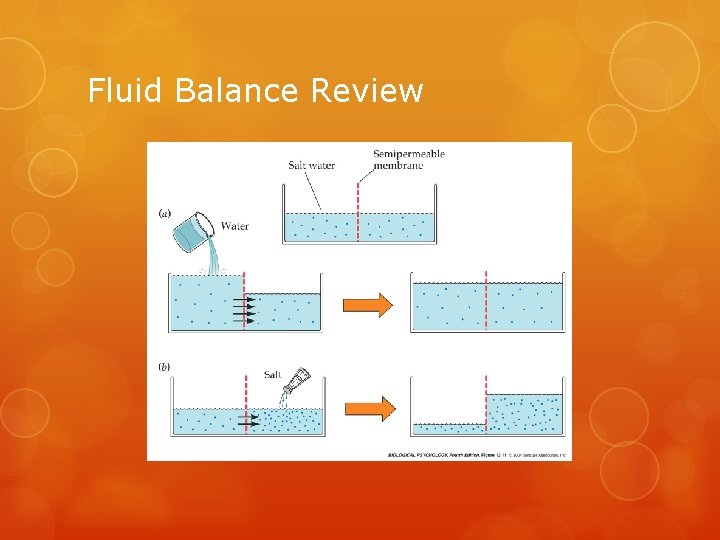
Fluid Balance Review

Objectives Identify the components of a gastrointestinal history. Describe inspection, palpation, percussion, and auscultation of the patient with gastrointestinal dysfunction. Delineate the clinical significance of selected laboratory tests used in the assessment of gastrointestinal disorders

Objectives Identity key diagnostic procedures used in assessment of the patient with gastrointestinal dysfunction. Discuss the nursing management of a patient undergoing a gastrointestinal diagnostic procedure.

GI Clinical Assessment & Diagnostic Procedures • Clinical Assessment – History • Present Illness/ Chief Complaint • General GI Status (previous GI studies/ procedures) • Personal and Social History – dietary habits, nutritional status, bowel characteristics, alcohol intake, laxative/ enema use • Family History – metabolic disorders, malabsorption syndromes, cancer

GI Clinical Assessment & Diagnostic Procedures Physical Examination Inspection – oral cavity, abd. skin & shape Jaundice, skin lesions Pink-purple striae (Cushing’s syndrome) Cullen’s sign – discolored umbilicus (intra-peritoneal hemorrhage), trauma Asymmetric distention (organ enlargement or mass) Visible hyperactive peristalsis (intestinal obstruction) Increased pulsation in epigastric area (AAA)

GI Clinical Assessment & Diagnostic Procedures Physical Examination Auscultation of 4 quadrants (Box 21 -1) Bowel sounds occur every 5 – 15 seconds Presence of bruits (partially obstructed artery) Hyperactive (hunger, gastroenteritis)High pitched may be signs of early bowel obstruction, intestinal air Hypoactive (peritonitis or ileus) Absent x 5 min (loss of motility – complete ileus) Percussion – to detect size & position of organs

GI Clinical Assessment & Diagnostic Procedures Physical Examination Palpation- palpate tender areas last Most useful in detecting abd. pathological conditions Light palpation assesses depth of skin & facia Deep palpation assesses the rectus abdominis muscle & is most helpful in detecting masses Normal findings: no areas of tenderness/ pain/ guarding, masses, or hardened areas Abnormal: rebound tenderness – pain increases with quick release of palpated area (inflamed peritoneum)

GI Clinical Assessment & Diagnostic Procedures Assessment Findings of Common Disorders Right Upper Quadrant (RUQ) Liver hepatitis Head of pancreas Acute hepatic congestion-hepatic flexure of colon, ascending and transverse colon Biliary stones, colic Acute cholecystitis Perforated peptic ulcer

GI Clinical Assessment & Diagnostic Procedures Assessment Findings of Common Disorders Right Lower Quadrant (RLQ) Appendicitis Perforated duodenal ulcer Cecal volvulus- cecum and appendix Strangulated hernia Right kidney Uterus if it is enlarged Right ovary and salpinx Right ureter and right spermatic cord

GI Clinical Assessment & Diagnostic Procedures Assessment Findings of Common Disorders Left Upper Quadrant (LUQ) Splenic trauma-splenic flexure of the colon Stomach Pancreatitis, body of the pancreas Left adrenal gland left kidney Pyloric obstruction Left lobe of the liver Portions of the transverse and descending colon

GI Clinical Assessment & Diagnostic Procedures Assessment Findings of Common Disorders Left Lower Quadrant (LLQ) Ulcerative colitis Colonic diverticulitis Lower left pole of the kidney Sigmoid colon Portion of the descending colon Bladder if distended Ovary and salpinx Left ureter and left spermatic cord

GI Clinical Assessment& Diagnostic Procedures Laboratory Studies – no single study provides an overall picture of the various organs’ functioning GI tests (Table 21 -2)-culture, micro organisms, fat, occult blood, O&P, Common lab studies (Table 21 -3) Liver function. ALT, AST, LDH, SGOT, Bili(indirect and direct), Total Bili, urine bili. Serum proteins, (albumin, globulin, A/G ratio, transferrin, AFP, PT, PTT,

GI Clinical Assessment& Diagnostic Procedures Pancreatic studies (Table 21 -4) Serum & urine amylase Serum lipase Secretin test-hormone secreted by duodenum that stimulates HCO 3 secretion by the pancreas and bile secretion by the liver(decrease GI motility) Stool fat

GI Clinical Assessment & Diagnostic Procedures Abdominal Diagnostic Procedures Barium enema (lower GI)-colorectal lesions, diverticulitis, fistulas, inflammation, size length and patency NPO before Fluids & laxatives after

GI Clinical Assessment & Diagnostic Procedures Barium swallow (upper GI) Clear liquid & laxative the evening before NPO after midnight Cleansing enema on the morning of the test Fluids & mild laxative after

GI Clinical Assessment & Diagnostic Procedures Abdominal Diagnostic Procedures Endoscopy (EGD) Golytely prep NPO 4 -8 hours prior to test Monitor for indications of sepsis & hemorrhage Colonoscopy Anoscopy, proctosigmoidoscopy Ultrasound Barium must be cleared from GI tract Full bladder

GI Clinical Assessment & Diagnostic Procedures Flat plate of abdomen (KUB) CT Scan w or w/o contrast ERCP Biopsy MRI Liver Scan Paracentesis HIDA scan

Chapter 22 Gastrointestinal Disorders and Therapeutic Management

Objectives • Describe the etiology and pathophysiology of selected gastrointestinal disorders. • Identify the clinical manifestations of selected gastrointestinal disorders. • Explain the treatments of selected gastrointestinal disorders. • Discuss the nursing priorities for managing a patient with selected gastrointestinal disorders. • Outline the use and care of gastrointestinal tubes.

Acute Gastrointestinal Hemorrhage Description Medical emergency Results in almost 300, 000 hospital admissions/ year Mortality rate remains between 5% - 35%

Acute Gastrointestinal Hemorrhage Etiology Upper GI tract Peptic Ulcer Disease Stress Related Erosive Syndrome (SRES) Esophagogastric Varices Mallory-Weiss tear Esophagitis Lower GI tract Diverticulitis/diverticulosis Inflammatory Bowel Disease Trauma Colitis, infectious or radiation Bowel ischemia Hemorrhoids

Acute Gastrointestinal Hemorrhage Upper GI tract Peptic Ulcer Disease Gastric & duodenal ulcers (50%) of cases Results from breakdown of mucosal lining Leading cause of upper GI hemorrhage Main causes of mucosal breakdown or lack of protective mechanisms (mucosal lining, epithelial cells, prostaglandins and nitric oxide and HCO 3 secretion) NSAIDs H. pylori

Acute Gastrointestinal Hemorrhage Upper GI tract Stress Related Erosive Syndrome (SRES) Stress ulcers develop in response to severe stress in other organ systems Same pathophysiology of PUD Usually limited to the stomach Also results from breakdown of mucosal lining Main cause is increased acid production

Acute Gastrointestinal Hemorrhage Upper GI tract Esophageal Varices Engorged & distended blood vessels of the esophagus & proximal stomach Develop as a result of portal hypertension secondary to cirrhosis Are vulnerable to damage from gastric secretions May rupture, causing massive hemorrhage which occurs in 16% - 44% of cases

Acute Gastrointestinal Hemorrhage Pathophysiology Life-threatening disorder (review Fig 22 -2, p. 430) Characterized by acute, massive GI bleeding Results in hypovolemic shock, initiation of shock response, & development of MODS if left untreated

Acute Gastrointestinal Hemorrhage Assessment and Diagnosis Hematemesis (bright red or coffee ground emesis) Hematochezia (bright red stools) – lower GI Melena (black-tarry stools) – upper GI Laboratory Studies H & H (may not decrease for 72 hrs. after acute bleeding) Platelet count & PTT should also be obtained Diagnostic Procedures – endoscopy to ID source of bleeding (once pt. is hemodynamically stable)

Acute Gastrointestinal Hemorrhage Medical Management Stabilization (crystalloids, blood, O 2, NG), H 2 antagonists, Proton pump inhibitors, airway protection, fluid resuscitation, address comorbities (coagulopathies) Vasopressin, octreotide, Gastric lavage Control Bleeding Peptic ulcer disease – endoscopic thermal therapy, injection (vasoconstriction), or mechanical (compression clips) SRES – intra-arterial infusion of vasopressin Esophegeal varices – band ligation or esophagogastric balloon, TIPS(transjugular intrahepatic portosystemic shunting

Acute Gastrointestinal Hemorrhage Surgical Intervention Peptic ulcer disease Vagotomy – vagus nerve to stomach is severed, reducing hydrochloric acid production Pyloroplasty – necessary to stimulate motility Esophegeal varices – shunt/ decompression procedure to divert portal blood flow away from liver & decompress portal system

Acute Gastrointestinal Hemorrhage Nursing Management Administering volume replacement – maintain two large bore IVs Provide comfort & emotional support Surveillance for complications Gastric perforation (surgical emergency) S&S: sudden, severe abd. Pain w/ rebound tenderness, rigidity, fever, tachycardia Patient & family education (alcoholism)

Acute Pancreatitis Description Acute inflammation of the pancreas(exocrine and endocrine dysfunction) 75% - 80% edematous interstitial pancreatitis (milder form) 15% develop severe, acute necrotizing pancr. Ranson’s Criteria to predict mortality (Box 22 -4 p. 434)) Admission At 48 hours

Acute Pancreatitis Etiology (Box 22 -5) Two most common causes Biliary Disease (gallstones) Alcoholism Other causes Surgical trauma Hypercalcemia Toxins & certain drugs Infections

Acute Pancreatitis Pathophysiology Normally inactive digestive enzymes become prematurely activated w/in the pancreas leading to autodigestion of pancreatic tissue Activation of trypsin, phospholipase A and lipase leading to leakage of fluid into interstitial space (edema & hypovolemia) Complications SIRS (Systemic Inflammatory Response) ↑WBC, temp, tachypnea tachy, acidosis (sepsis) MODS (Multi-Organ Dysfunction Syndrome) Death

Acute Pancreatitis • Assessment and Diagnosis – Clinical Manifestations (Box 22 -6) – Physical Examination – hypoactive BS, guarding, abd. tenderness, distension, & tympany, Gray-Turner’s or Cullens sign, palpable mass(cyst) – Laboratory Studies (Table 22 -2, p. 436) • Elevated serum amylase • Elevated serum lipase (more pancr. specific) • Leukocytosis, hypocalcemia, hypo-albuminemia, hyperbilirubinemia – Diagnostic Procedures • Abdominal CT scan w/ contrast, US, MRI, ERCP, KUB, Chest PA/LAT

Acute Pancreatitis Medical Management Systemic Complications (Box 22 -7 p. 437) Hypovolemia Shock/ Fluid Management Nutritional Support (enteral feedings/ TPN) Acute Respiratory Distress Syndrome (ARDS) Acute Renal Failure Local Complications Infected Pancreatic Necrosis (surgical debridement) Pancreatic Pseudocyst (drainage of fluid)

Acute Pancreatitis Nursing Management Provide pain relief and emotional support Morphine, relaxation-techniques, knee-chest position Surveillance for complications (Box 22 -7) Nursing Dx p. 437 Patient & family education Prevent recurrence Diet modification Supplemental pancreatic enzymes Alcoholism

Fulminant Hepatic Failure (FHF) Description Life-threatening(80% mortality) Severe, sudden liver dysfunction Hepatocellular necrosis Hepatic encephalopathy Mortality rate very high Liver transplantation is the definitive treatment

Fulminant Hepatic Failure (FHF) Etiology (Box 22 -11) Infections – Hepatitis, Herpes, Varicella Drugs – Tetracycline, Sulfa, Acetaminophen, Cocaine Toxins – Chlorinated hydrocarbons, Phosphorus Hypoperfusion – Obstruction, Ischemia Metabolic disorders – Heat Stroke, Wilson’s disease Surgery – Jejunoileal bypass, partial hepatectomy, transplant Other: Reye’s syndrome,

Fulminant Hepatic Failure (FHF) Pathophysiology Sudden onset of acute liver failure (1 -3 wks) Liver usually healthy before this illness Hepatic encephalopathy within 8 weeks Usually less than two weeks between liver failure and onset of encephalopathy Massive necrosis of hepatocytes

Fulminant Hepatic Failure (FHF) • Pathophysiology (cont’d) • Impaired bilirubin conjugation – Result: Jaundice • Decreased clotting factor production – Result: Bleeding • Depressed glucose synthesis – Result: Hypoglycemia • Decreased lactate clearance – Result: Metabolic Acidosis – Albumin synthesis, fluid and electrolyte imbalance – Acute portal hypertension

Fulminant Hepatic Failure (FHF) Pathophysiology (cont’d) Other complications Cerebral edema/ ICP (changes in blood-brain barrier Cardiac dysrhythmias due electrolyte imbalance and acidosis Acute respiratory failure and ALI Acute renal failure Sepsis or circulatory failure (<CPP)

Fulminant Hepatic Failure (FHF) Assessment and Diagnosis Early recognition is important Coma grade (staging) – (Box 22 -12) Lab studies Serum bilirubin, liver enzymes (AST/SGOT, ALT/SGPT), alkaline phosphatase, serum ammonia, serum albumin Coagulation studies PT and INR, Coag. factors p. H

Fulminant Hepatic Failure (FHF) • Assessment and Diagnosis/ Signs & Sx • Headache, personality changes • Hyperventilation • Jaundice • Palmer erythema • Spider nevi, bruises • Edema • Asterixis or “liver flaps”

Fulminant Hepatic Failure (FHF) Medical Management Remove or decrease nitrogenous waste intestine/ ammonia levels Neomycin Lactulose Prevent bleeding Fluid resuscitation, CVP monitoring, ICP High risk for GI bleeding Stress ulcer prophylaxis in large

Fulminant Hepatic Failure (FHF) Medical Management (cont’d) Treat Acute Bleeding Fluid resuscitation Vitamin K Fresh Frozen Plasma (FFP) Coagulation factor replacement Blood transfusions Platelets

Fulminant Hepatic Failure (FHF) Medical Management (cont’d) Multi system organ involvement Brain: Cerebral edema (Mannitol) Kidneys: Renal failure Lungs: CV: Respiratory failure Hemodynamic instability Liver Transplantation Only definitive treatment

Fulminant Hepatic Failure (FHF) • Nursing Management • Protecting the patient from injury (severe agitation) • Provide comfort & emotional support (elevate HOB) • Surveillance for complications – Infection – Bleeding – Respiratory failure – Neurologic assessment q 1 hr. • Patient education – Transplant

GI Therapeutic Management Gastrointestinal Intubation Nasogastric suction tubes Long intestinal tubes Feeding Tubes Esophagogastric balloon tamponade tubes Transjugular Intrahepatic Portosystemic Shunt (TIPS)

GI Intubation Nasogastric suction tubes Remove fluid regurgitated into the stomach, prevent swallowed air, decompress bowel, reduce aspiration risk Nursing Management Prevent complications (nares ulceration, esophageal erosion Airway, aspiration, fluid/ electrolyte loss Irrigate q 4 hrs. w/ NS, ensure Salem air vent is patent Oral & nares care

GI Intubation Long Intestinal Tubes Types of weighted-tip, intestinal tubes Miller-Abbott/ Cantor (rarely used d/t mercury) Anderson Treat obstructions Contraindications: paralytic ileus, severe mech. Obstruction Nursing Management – observe for balloon malf.

GI Intubation Feeding Tubes Small diameter (8 – 12 Fr), inserted orally or nasally so tip ends up in stomach or duodenum X-ray to verify placement & mark at mouth/ nares Nursing Management Prevention of complications Monitor feeding tolerance Maintain patency

GI Intubation Esophagogastric balloon tamponade tubes Temp. tx to stop GI bleeding (80 -90% effective) Types (Figure 22 -5) Sengstaken-Blakemore tube – 3 lumens Linton tube – 3 lumens Minnesota tube – 4 lumens Nursing Management Monitor for rebleeding Observe for complications (pulmonary aspiration)

GI Therapeutic Management Transjugular Intrahepatic Portosystemic Shunt (TIPS) Interventional radiology procedure to decrease portal hypertension Angiographic catheter inserted into interior jugular vein to middle or right hepatic vein to place stent Used in: Pts. w. / portal HTN + active bleeding or poor liver reserve Transplant patients Pts. w/ other operative risks

GI Therapeutic Management Surgery Types Esophagectomy (cancer) Pancreaticoduodenectomy “Whipple Procedure” (cancer) Preoperative Care – thorough physical status eval. Surgical Considerations Esophageal resection to stomach Do not manipulate NG (damage to anastomosis)

GI Therapeutic Management Surgery (cont’d) Complications & Medical Management Pulmonary Complications Anastomatic Leak DVT/ PE Bleeding Postoperative Care Optimize oxygenation & ventilation Provide comfort & emotional support

GI Therapeutic Management Liver Transplant Indications and Selection (Box 22 -16 & 22 -17) Surgical Procedure Stage 1: Recipient hepatectomy (most difficult) Stage 2: Vascular anastomosis Suprahepatic inferior vena cava Infrahepatic vena cava Hepatic artery Portal vein Stage 3: Biliary anastomosis

GI Therapeutic Management Liver Transplant (cont’d) Postoperative Collaborative Management Reestablish normal body temperature Hemodynamic stabilization Maintenance of adequate oxygenation & ventilation Neurologic assessment Reduce infection risk