Unit IV Alteration in Metabolism Nutrition and Elimination

Unit IV - Alteration in Metabolism, Nutrition and Elimination Part C Effects of Inflammatory Processes on Digestion

Assessment • Subjective – History – Life Style • Objective – Endoscopic and Radiographic Studies

Barium Swallow & Enema • Barium Swallow – Pre: NPO – What are we assessing for? – Post: What is your nursing care? • Barium Enema – Pre: NPO – What are we assessing for? – Post: What is your nursing care?

Endoscopy Care • Consent form • Pre-procedure care & instructions – Sedation • Post-procedure care – VS – Gag reflex

Care of the Adult with Specific Disorders • Peptic Ulcer Disease (PUD) • Gastric versus duodenal – Location • Acute versus chronic –Depends on degree/duration of mucosal involvement

Types of PUD • Acute – Superficial erosion – Minimal inflammation – Short duration, resolves quickly when cause is identified and removed

Types of PUD • Chronic – Muscular wall erosion with formation of fibrous tissue – Long duration—present continuously for many months or intermittently – Four times as common as acute erosion

Peptic Ulcer Disease Clinical Manifestations • Common—no pain or other symptoms – Due to lack of sensory pain fibers • If pain exists – Gastric ulcer pain • High in epigastrium • 1 to 2 hours after meals • Burning or gaseous pain

Peptic Ulcer Disease Clinical Manifestations Duodenal ulcer pain • • Mid-epigastric region beneath xiphoid process Back pain—if located posterior aspect 2 to 4 hours after meals Tendency to occur, then disappear, then occur again

Peptic Ulcer Disease Complications • Three major complications include – Hemorrhage – Perforation – Gastric outlet obstruction • All considered emergency situations

Peptic Ulcer Disease Hemorrhage • Most common complication of peptic ulcer disease • Develops from erosion of – Granulation tissue found at base of ulcer during healing – Ulcer through a major blood vessel

Peptic Ulcer Disease Perforation • Most lethal complication of peptic ulcer • Common in large penetrating duodenal ulcers that have not healed and are located on posterior mucosal wall • Perforated gastric ulcers often located on lesser curvature of stomach • Mortality rates higher with perforation of gastric ulcers

Peptic Ulcer Disease Perforation • When ulcer penetrates serosal surface with spillage of contents into peritoneal cavity • Size proportional to length of time ulcer existed • Large perforations: Immediate surgical closure
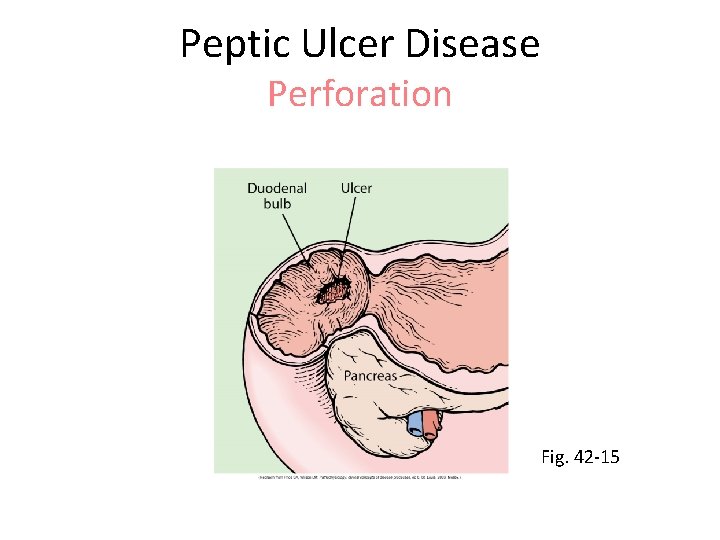
Peptic Ulcer Disease Perforation Fig. 42 -15

Peptic Ulcer Disease Perforation • Clinical manifestations – Sudden, dramatic onset – Severe upper abdominal pain spreads throughout abdomen – Possible shoulder pain – Rigid, boardlike abdominal muscles

Peptic Ulcer Disease Perforation • Clinical manifestations (cont’d) – Shallow, rapid respirations – Bowel sounds absent – Nausea/vomiting – History reporting symptoms of indigestion or previous ulcer

Peptic Ulcer Disease Gastric Outlet Obstruction • Obstruction due to: – Edema – Inflammation – Pylorospasm – Fibrous scar tissue formation – All contribute to narrowing of pylorus

Peptic Ulcer Disease Obstruction • Clinical Manifestations: – Usually long hx of ulcer pain – Pain progresses to generalized upper abd. Discomfort. – Pain worsens toward end of days as stomach fills and dilates – Relief obtained by belching or vomiting – Vomiting is common

Peptic Ulcer Disease Obstruction • Constipation common (r/t dehydration, lack of roughage in diet. • Swelling in stomach & upper abdomen • Loud peristalsis • Visible peristaltic waves

Peptic Ulcer Disease Diagnostic Studies • • Endoscopy H. pylori Urea breath test Barium studies Gastric Analysis CBC Serum amylase Stool examination

Peptic Ulcer Disease Collaborative Care • Medical regimen consists of – Adequate rest – Dietary modification – Drug therapy – Elimination of smoking and alcohol – Long-term follow up care – Stress management

Nursing and Medical Management Modalities • Pharmacologic agents – Antacid – H 2 receptor antagonists – Acid secretion inhibitor – Motility agents

Stress-Related Mucosal Disease • Also called physiologic stress ulcer • Acute ulcers that develop after major physiologic insult – Trauma or surgery • Form of erosive gastritis • Prophylaxis with antisecretory agents
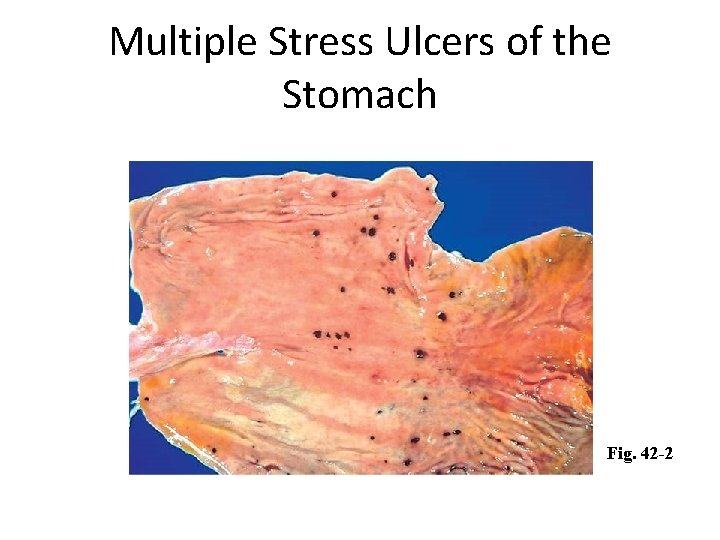
Multiple Stress Ulcers of the Stomach Fig. 42 -2

Medical Management Modalities • Surgical procedures – Gastric resection – Billroth I and Billroth II – Vagotomy

Surgical Procedures • Surgical procedures – Billroth I: Gastroduodenostomy • Partial gastrectomy with removal of distal 2/3 stomach and anastomosis of gastric stump to duodenum – Billroth II: Gastrojejunostomy • Partial gastrectomy with removal of distal 2/3 stomach and anastomosis of gastric stump to jejunum
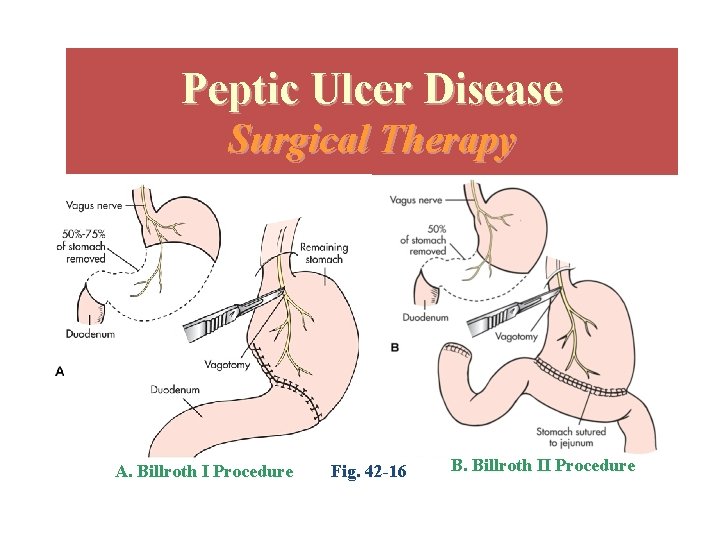
Peptic Ulcer Disease Surgical Therapy A. Billroth I Procedure Fig. 42 -16 B. Billroth II Procedure Copyright © 2007, 2004, 2000, Mosby, Inc. , an affiliate of Elsevier Inc. All Rights Reserved.

Peptic Ulcer Disease Surgical Therapy • Surgical therapies (cont’d) – Vagotomy • Severing of vagus nerve • Done in conjunction with gastrectomy – Pyloroplasty • • Surgical enlargement of pyloric sphincter Commonly done after vagotomy ↓ Gastric motility and gastric emptying If accompanying vagotomy, ↑gastric emptying

Peptic Ulcer Disease Postoperative Complications • Most common – Dumping syndrome – Postprandial hypoglycemia – Bile reflux gastritis

Peptic Ulcer Disease Postoperative Complications • Dumping syndrome – 33% to 50% of patients experience after surgery – Direct result of surgical removal of a large portion of stomach and pyloric sphincter – ↓ Ability of stomach to control amount of gastric chyme entering small intestine • Large bolus of hypertonic fluid enters intestine • ↑ Fluid drawn into bowel lumen

Peptic Ulcer Disease Postoperative Complications • Dumping syndrome (cont’d) – Occurs at end of meal or 15 to 30 minutes after eating – Symptoms include • Weakness, sweating, palpitations, dizziness, abdominal cramps, borborygmi, urge to defecate • Last no longer than an hour

Peptic Ulcer Disease Postoperative Complications • Postprandial hypoglycemia – Variant of dumping syndrome – Result of uncontrolled gastric emptying of a bolus of fluid high in carbohydrate into small intestine • ↑ Blood sugar • Release of excessive amounts of insulin into circulation

Peptic Ulcer Disease Postoperative Complications • Postprandial hypoglycemia (cont’d) – Secondary hypoglycemia occurs with symptoms ~2 hours after meals – Symptoms include sweating, weakness, mental confusion, palpitations, tachycardia and anxiety – When symptoms occur, immediate ingestion of sugared fluids or candy relieves symptoms

Peptic Ulcer Disease Postoperative Complications • Bile reflux gastritis – Surgery can result in reflux alkaline gastritis • Prolonged contact of bile causes damage to gastric mucosa • May result in back-diffusion of H+ ions through gastric mucosa • PUD may reoccur

Peptic Ulcer Disease Postoperative Complications • Bile reflux gastritis (cont’d) – Continuous epigastric distress that ↑ after meals – Administration of cholestyramine (Questran) relieves irritation – Aluminum hydroxide antacids also used

Care of the Adult with Specific Disorders • Crohn’s disease • Ulcerative colitis • Compare & contrast these conditions with respect to assessment and appropriate nursing interventions

Inflammatory Bowel Disease Description • Ulcerative colitis: inflammation and ulceration of the colon and rectum • Crohn’s disease: inflammation of segments of the GI tract

Comparison of Ulcerative Colitis & Crohn’s Disease • • Ulcerative Colits Bleeding common Malabsorption rare Fistulas rare Perforation common Surgery usually cures Location: Distal & spreads continuously up. Crohn’s Disease Bleeding rare Malabsorption common Fistulas common Perforation common Surgery: segmental resection • Location: Skips around • • •

Ulcerative Colitis Etiology and Pathophysiology • Diffuse inflammation beginning in the rectum and spreading up the colon in a continuous pattern – Inflammation and ulcerations occur in mucosa and submucosa • Multiple abscesses develop in the intestinal glands – Abscesses break through into the submucosa, leaving ulcerations

Ulcerative Colitis Etiology and Pathophysiology • Ulcerations destroy the mucosal epithelium, causing bleeding and diarrhea – Fluid and electrolyte losses – Protein loss – Pseudopolyps
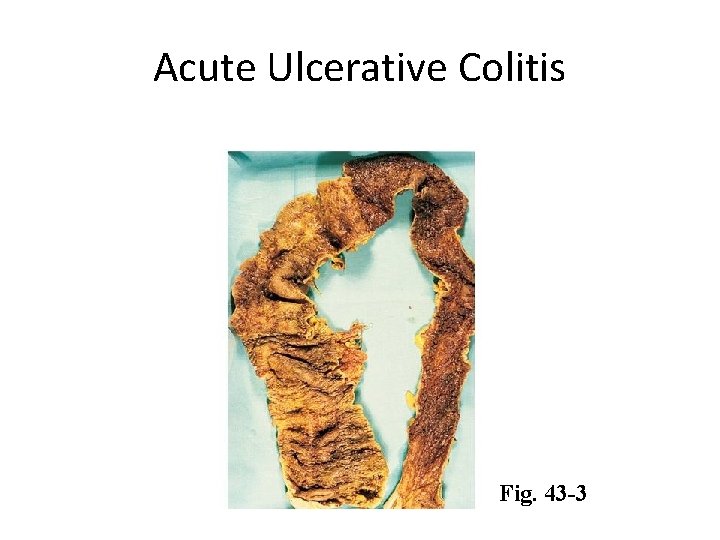
Acute Ulcerative Colitis Fig. 43 -3

Ulcerative Colitis Clinical Manifestations • Major symptoms – Bloody diarrhea – Abdominal pain • Other symptoms – Tenesmus – Rectal bleeding

Ulcerative Colitis Complications • Intestinal complications – Hemorrhage – Strictures – Perforation – Toxic megacolon • Dilation and paralysis of the colon • Associated with perforation

Crohn’s Disease Etiology and Pathophysiology • Inflammation involves all layers of the bowel wall • Skip lesions – Segments of normal bowel occurring between diseased portions • Ulcerations are deep and longitudinal • Ulcerations penetrate between islands of inflamed edematous mucosa, causing the classic cobblestone appearance

Crohn’s Disease Etiology and Pathophysiology • Narrowing of the lumen with stricture development – May cause bowel obstruction • Microscopic leaks can allow bowel contents into peritoneal cavity

Crohn’s Disease Etiology and Pathophysiology • Peritonitis may develop • Abscesses or fistula tracts that communicate with other loops of bowel, skin, bladder, rectum, or vagina may develop

Crohn’s Disease Etiology and Pathophysiology Fig. 43 -2

Crohn’s Disease Clinical Manifestations • Depend on the anatomic site of involvement, extent of the disease process, and presence/absence of complications • Main manifestations – Diarrhea (nonbloody) • Colicky abdominal pain • Other symptoms – Malabsorption – Nutritional deficiencies

Crohn’s Disease Complications • Intestinal – Strictures and obstruction from scar tissue – Fistulas – Peritonitis • Extraintestinal – – – Thromboembolism Arthritis Ankylosing spondylitis Osteoporosis Liver disease Skin lesions

Inflammatory Bowel Disease Collaborative Care • Goals of treatment – Rest the bowel – Control inflammation – Combat infection – Correct malnutrition – Alleviate stress – Symptomatic relief – Improve quality of life

Inflammatory Bowel Disease Collaborative Care • Drug therapy – Aminosalicylates – Antimicrobials – Corticosteroids – Immunosuppressants – Biologic therapy

Inflammatory Bowel Disease Collaborative Care • Drug therapy – Sulfasalazine (Azulfidine) • • Principal drug used Decreases GI inflammation Effective in achieving and maintaining remission Mild to moderately severe attacks

Inflammatory Bowel Disease Collaborative Care • Drug therapy (cont’d) – Antimicrobials • Prevent or treat secondary infection – Corticosteroids • Decrease inflammation • Used to achieve remission • Helpful for acute flareups **Aminosalicylates and corticosteroids are mainstays of treatment for ulcerative colitis

Inflammatory Bowel Disease Collaborative Care • Drug therapy (cont’d) – Immunosuppressants • Suppress immune response • Most useful in those who do not respond to aminosalicylates, antimicrobials, or corticosteroids • Requires regular CBC monitoring

Inflammatory Bowel Disease Collaborative Care • Drug therapy (cont’d) – Biologic therapies • Inhibit tumor necrosis factor • Induce and maintain remission – Antidiarrheals • ↓ GI motility – Hematinics and vitamins • Correct iron deficiency • Promote healing

Inflammatory Bowel Disease Collaborative Care • Surgical therapy – Procedures for chronic ulcerative colitis • Total colectomy with rectal mucosal stripping and ileoanal reservoir • Total protocolectomy with continent ileostomy (Kock pouch) • Total protocolectomy with permanent ileostomy

Inflammatory Bowel Disease Collaborative Care • Surgical therapy (cont’d) – Total colectomy with rectal mucosal stripping and ileoanal reservoir • • Combination of two procedures 8 to 12 weeks apart Adaptation over 3 to 6 months Able to control defecation at anal sphincter
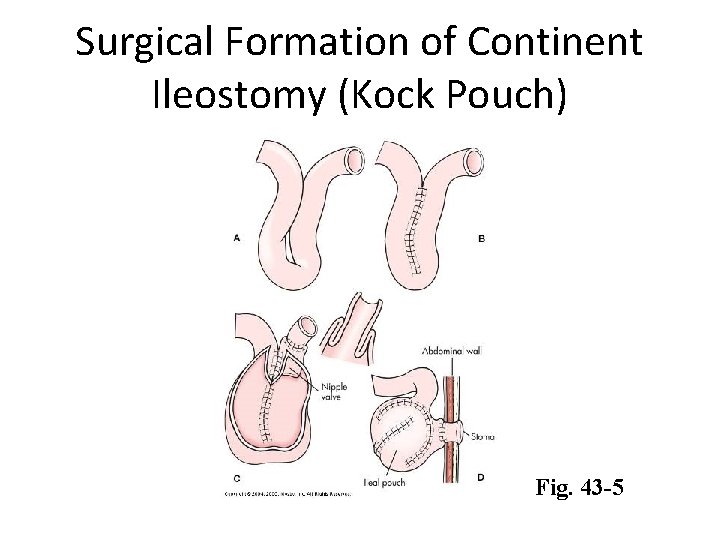
Surgical Formation of Continent Ileostomy (Kock Pouch) Fig. 43 -5

Inflammatory Bowel Disease Collaborative Care • Crohn’s disease: Surgical therapy – 75% will require surgery – Surgery produces remission, but high recurrence rate

Inflammatory Bowel Disease Collaborative Care • Surgical therapy: Postoperative care • Ileostomy, Monitoring of : – Stoma viability – Mucocutaneous juncture – Peristomal skin integrity • Enterostomal therapy nurse should help with problems • Output may be as high as 1500 to 2000 ml per 24 hours • Observe for hemorrhage, abdominal abscess, small bowel obstruction, dehydration

Inflammatory Bowel Disease Collaborative Care • Nutritional therapy – Dietary consultant – Provide adequate nutrition without exacerbating symptoms – Correct and prevent malnutrition – Replace fluid and electrolyte losses – Prevent weight loss

Inflammatory Bowel Disease Collaborative Care • Nutritional therapy – High-calorie – High-protein – Low-residue diet – Vitamin and iron supplements – Elemental diet – Parenteral nutrition

Inflammatory Bowel Disease Nursing Management • Teaching – Importance of rest and diet management – Perianal care – Action and side effects of drugs – Symptoms of recurrence – When to seek medical care – Use of diversional activities to reduce stress

Evaluations • • Effectiveness of care Home management Community support Family support

New surgery option • Ileoanal Reservoir (Pouch) – www. j-pouch. org/Whatis. html – www. trueguts. com
- Slides: 65