Unit 10 Notes Blood Flow of Kidney Blood

Unit 10 Notes
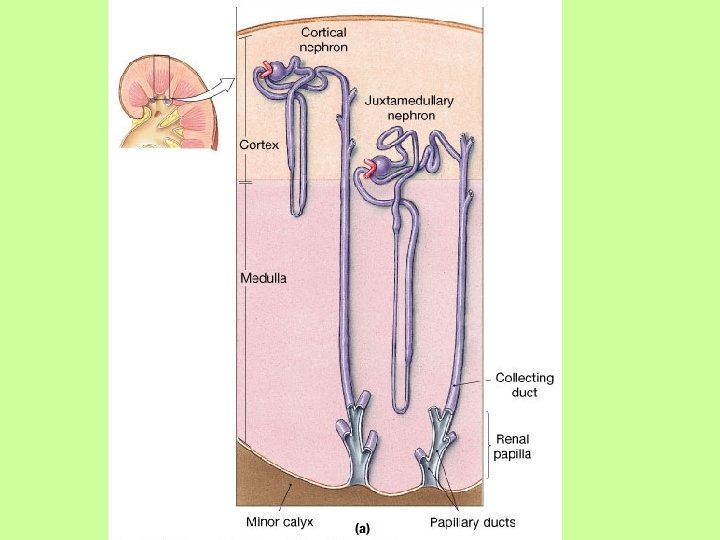
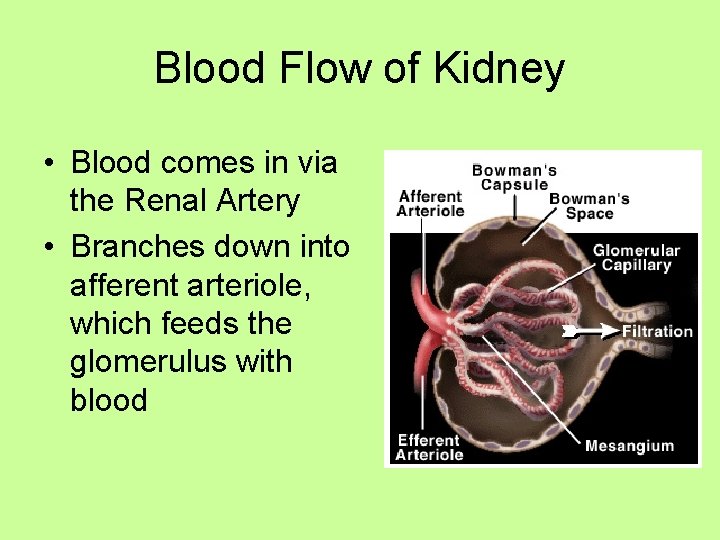
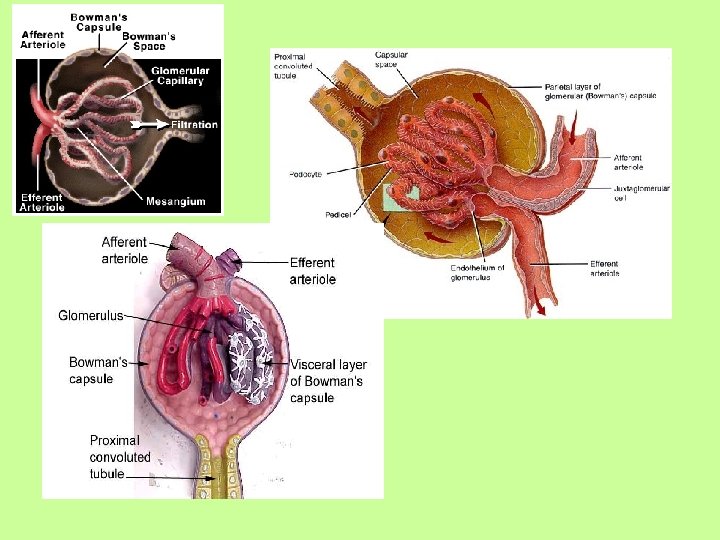
Blood Flow of Kidney • Blood comes in via the Renal Artery • Branches down into afferent arteriole, which feeds the glomerulus with blood
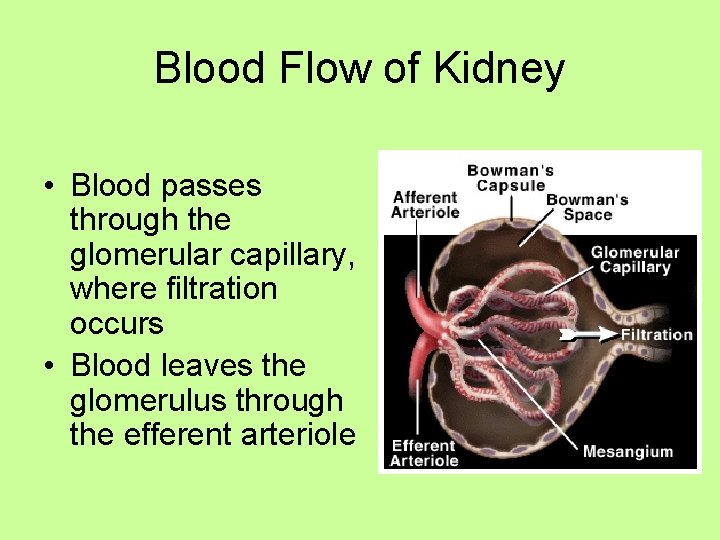
Blood Flow of Kidney • Blood passes through the glomerular capillary, where filtration occurs • Blood leaves the glomerulus through the efferent arteriole
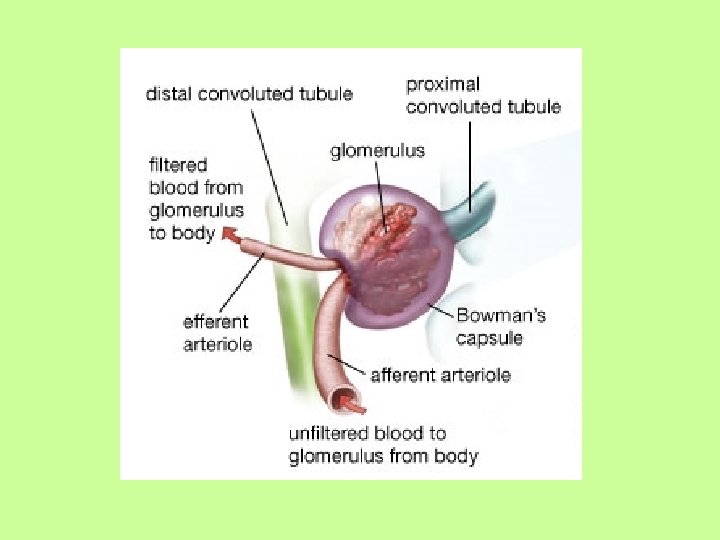
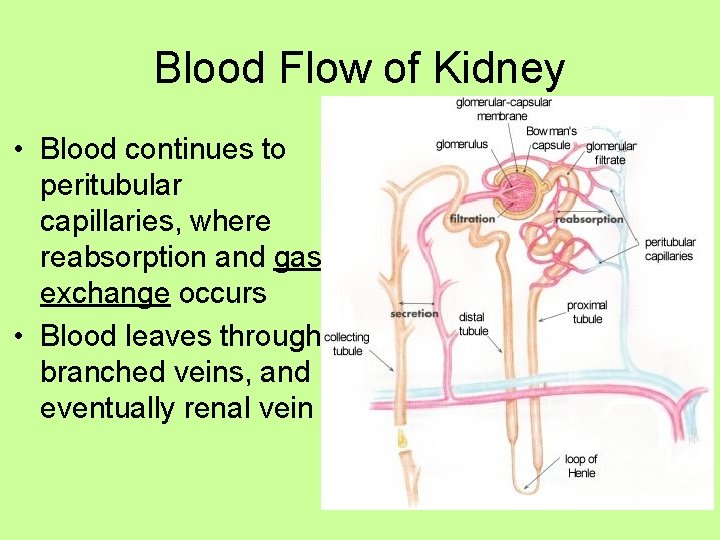
Blood Flow of Kidney • Blood continues to peritubular capillaries, where reabsorption and gas exchange occurs • Blood leaves through branched veins, and eventually renal vein
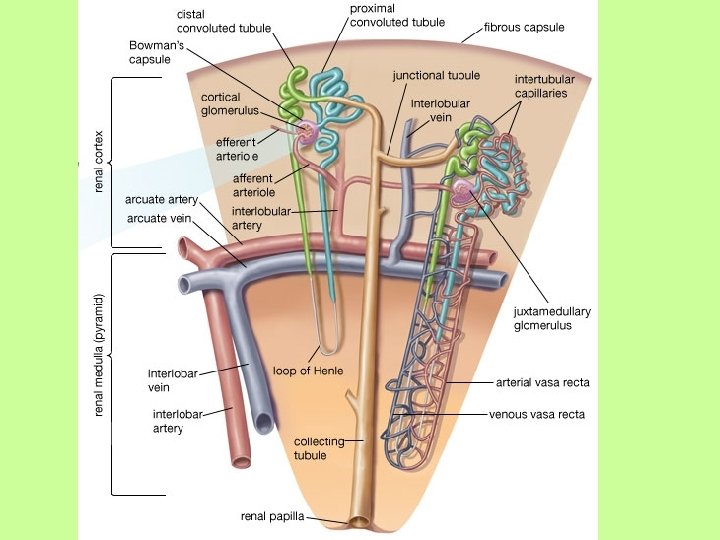
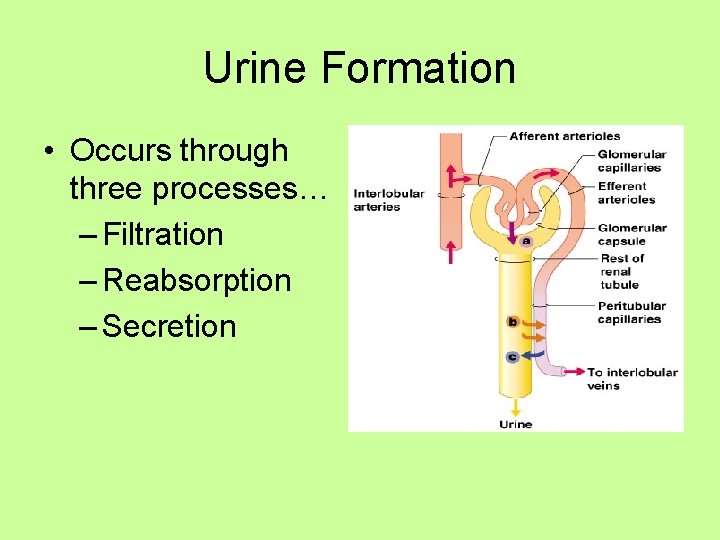
Urine Formation • Occurs through three processes… – Filtration – Reabsorption – Secretion

Filtration • Happens at glomerular capillaries • Includes… – Blood plasma without blood proteins or RBC’s • Water • Small Solutes • Blood pressure must be good for filtrate to pass through capillary walls! • Approx. 1 L of blood passes through kidney per minute… of this, about 120 -125 m. L is filtered out

Reabsorption • Most happens at Proximal Convoluted Tubule, but can happen all along renal tubule! • Reabsorbed back into Peritubular Capillaries • Mostly done by active transport (exception is water: passive transport) • Includes… – – Water Glucose Amino Acids Ions (H+, K+, Na+, Cl-, HCO 3 -) • Some of these substances will be left in the urine – if the body doesn’t need them to maintain homeostasis

Reabsorption • Nitrogen wastes tend NOT to be reabsorbed (or poorly if they are) – Urea: Formed by the liver (protein breakdown) – Uric Acid: Nucleic acids metabolized – Creatinine: Muscle metabolism • Also, excess water is not reabsorbed • All are found in high amounts in urine • Approx. 99% of filtrate is reabsorbed (taken back from filtrate to blood)

Secretion • Some substances are secreted by the Peritubular Capillaries back into the renal tube • Includes… – Creatinine – H+, K+ ions – Drugs • Any materials left move out the collecting duct, through the renal pelvis, and down the ureter to the bladder

• http: //www. argosymedical. com/Urinary/sa mples/animations/Urine%20 Formation/

• So, anything that’s left after filtration, absorption, and secreting by the kidney tubules is then called URINE.

Urine • Yellow in color • Color due to urochrome (pigment resulting from destroying hemoglobin); more solutes (less water/solvent) yields deeper color • Has an odor, but becomes more “ammonia” smelling if allowed to stand

Urine • p. H slightly acidic • More dense than distilled water (water + solutes) • Common solutes include H+ & K+ ions, urea, uric acid, creatinine, ammonia, and HCO 3 -

• Urine then continues down to URETERS
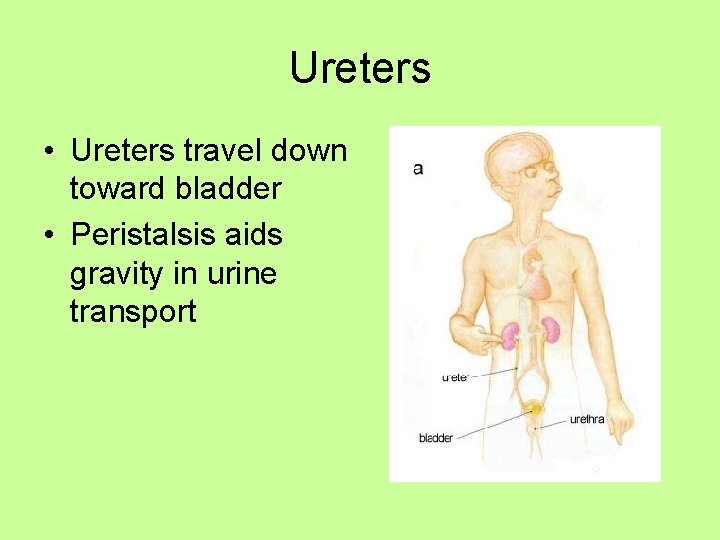
Ureters • Ureters travel down toward bladder • Peristalsis aids gravity in urine transport

• Urine then heads to the BLADDER
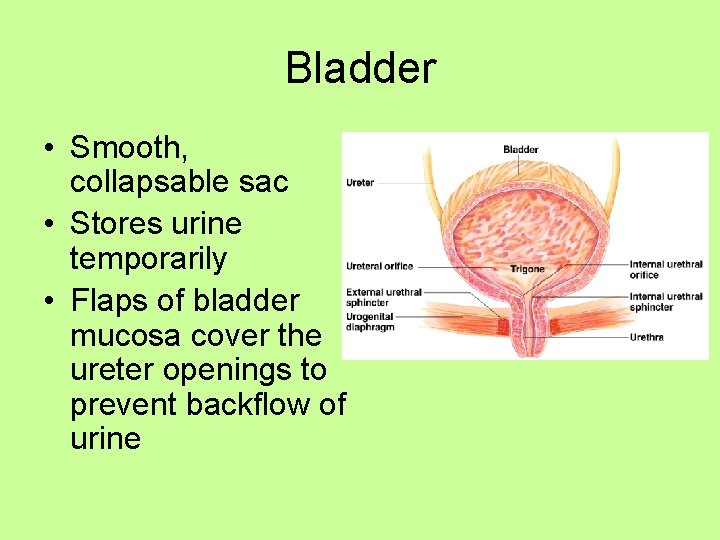
Bladder • Smooth, collapsable sac • Stores urine temporarily • Flaps of bladder mucosa cover the ureter openings to prevent backflow of urine
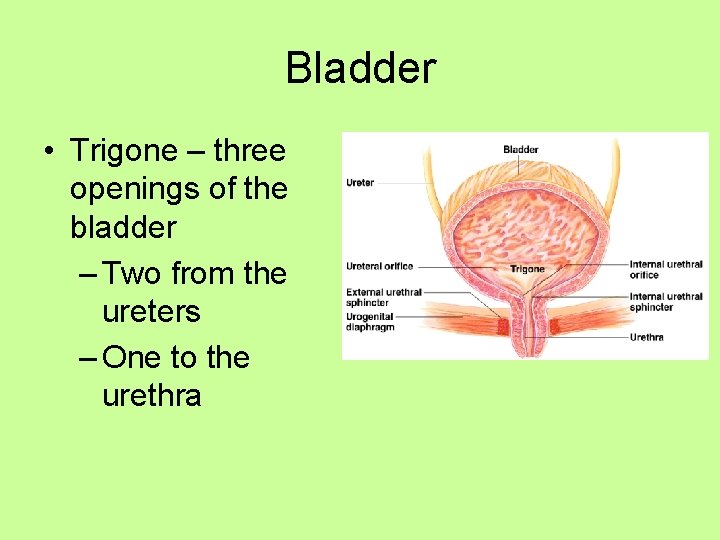
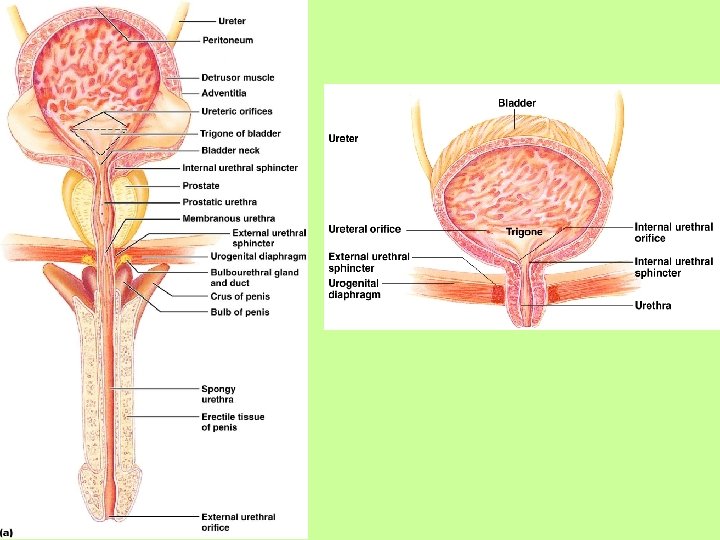
Bladder • Trigone – three openings of the bladder – Two from the ureters – One to the urethra
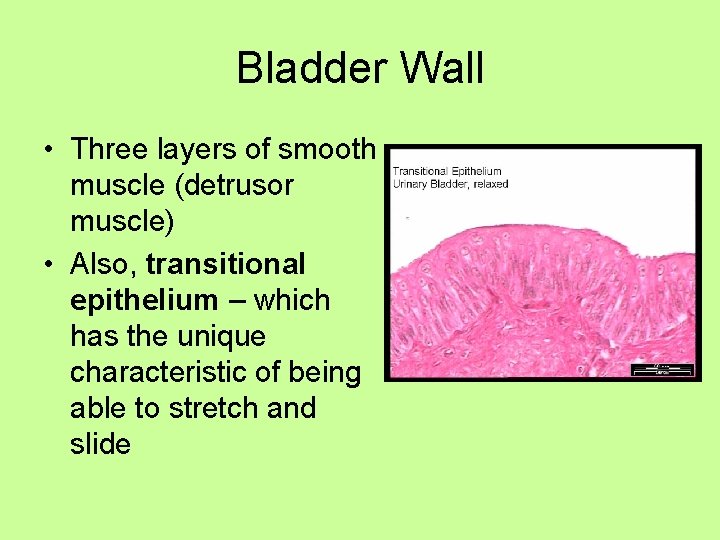
Bladder Wall • Three layers of smooth muscle (detrusor muscle) • Also, transitional epithelium – which has the unique characteristic of being able to stretch and slide
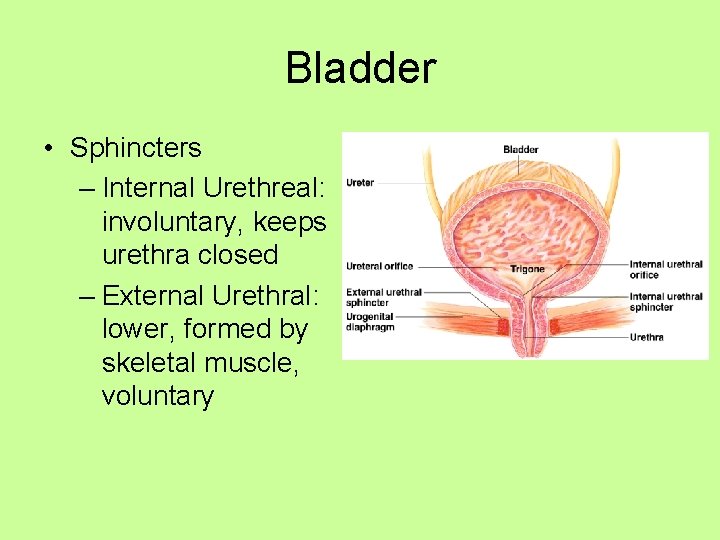
Bladder • Sphincters – Internal Urethreal: involuntary, keeps urethra closed – External Urethral: lower, formed by skeletal muscle, voluntary

• http: //highered. mcgrawhill. com/sites/0072495855/student_view 0/ chapter 27/animation__micturition_reflex. ht ml

• Urine then exits the body through the URETHRA

Urethra • Thin-walled tube that carries urine from the bladder to the outside of the body by peristalsis • Length – Females – 3– 4 cm (1 inch), along wall of vagina – Males – 20 cm (8 inches), through prostate & penis • Function – Females – only carries urine – Males – carries urine and is a passageway for sperm cells

Facts to know about Urinary System… • Each kidney has over ONE MILLION nephrons • It takes about four minutes for all of your blood to be filtered through a kidney • A moderately full bladder holds about 500 m. L of urine, but it can hold up to 1 liter • In 24 hours, kidneys filter out 150 -180 liters of blood plasma, but only produce about 1 -1. 8 liters of urine

Remember some of the functions of kidneys… • 1. Excretion of nitrogen-containing wastes (which we discussed last class!) • 2. Maintaining water balance • 3. Regulate blood pressure • 4. Ensuring proper blood p. H • We’ve talked about number 1, but we will discuss 2 through 4 today!

Maintaining Water Balance • Normal amount of water in the human body – Young adult females – 50% – Young adult males – 60% – Babies – 75% – Old age – 45% • Water is necessary for many body functions and levels must be maintained

Maintaining Water Balance • Intracellular Fluid – 2/3 of body fluid, found in cells • Extracellular Fluid – 1/3 of body fluid, found outside cells – Includes blood plasma, cerebrospinal fluid, tissue fluid, and others • Ions (Electrolytes) are dissolved in much of this fluid

Maintaining Water Balance • Changes in electrolyte balance causes water to move in and out of the cells – Alters blood volume and blood pressure – Can impair the activity of cells

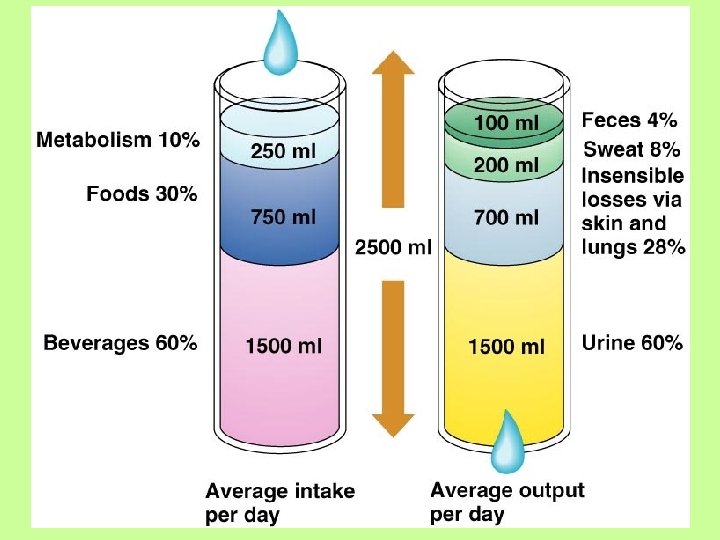
Maintaining Water Balance • Water intake must equal water output (about 2500 m. L / 2. 5 L every day) • Sources for water intake – Ingested foods and fluids – Water produced from metabolic processes • Sources for water output – – Vaporization out of the lungs Lost in perspiration Leaves the body in the feces Urine production

Maintaining Water Balance • How does your body know that it is lacking water? • How does it fix the problem? ? ? • And how do your kidneys regulate your blood pressure at the same time?

Way #1: ADH • • Water loss leads to low blood pressure …which leads to low filtrate production …which leads to unusual composition of blood …which causes your hypothalamus to say, “hey, something’s wrong!” The hypothalamus then sends out a nerve signal to the pituitary gland …which releases ADH (antidiuretic hormone) …which stimulates the kidney’s collecting ducts to reabsorb more water … which causes blood pressure and volume to rise! (more filtrate will be produced!)

Way #2: Renin-Angiotensin Mechanism • Water loss leads to low blood pressure • …which will stimulate the release of renin (an enzyme) • …which will speed up the production of angiotensin (a hormone) • …which will cause vasoconstriction (higher blood pressure!)

Way #2: Renin-Angiotensin Mechanism • Angiotensin will also stimulate the production of aldosterone • Aldosterone acts on the distal convoluted tubules • …and stimulates them to reabsorb more Na+ and water • …which increases blood pressure and volume!

Maintaining Blood p. H • p. H is the measure of the concentration of H+ ions – More H+, more acidic – p. H level 0 -7: acidic – p. H level 7 -14: basic – p. H level at 7: neutral

Maintaining Blood p. H • Blood p. H must remain between 7. 35 and 7. 45 to maintain homeostasis – Alkalosis – p. H above 7. 45 – Acidosis – p. H below 7. 35 (while not “acidic”, it still has more H+ than normal!)

Maintaining Blood p. H • Many metabolic processes will produce acids to throw off this balance! – Lactic Acid in your muscles – Fatty Acids – Carbonic Acid (formed by CO 2 and H 2 O mixing in your blood!) • Your kidneys help your body to maintain its optimal p. H by controlling H+ and HCO 3 absorption & secretion
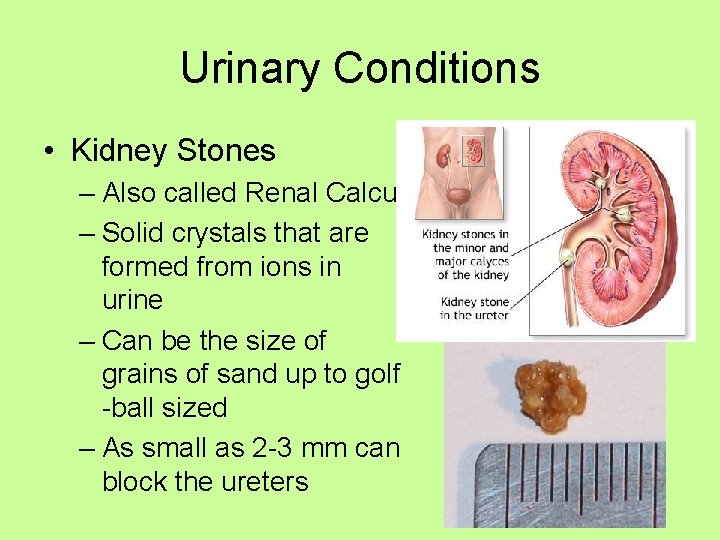
Urinary Conditions • Kidney Stones – Also called Renal Calculi – Solid crystals that are formed from ions in urine – Can be the size of grains of sand up to golf -ball sized – As small as 2 -3 mm can block the ureters
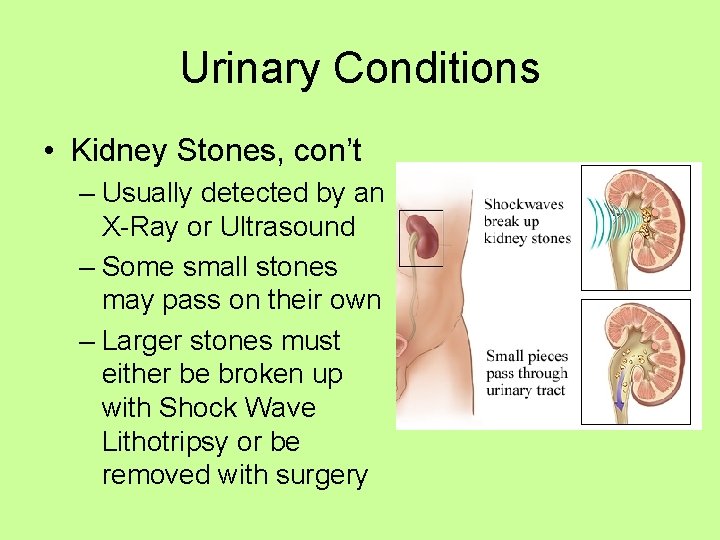
Urinary Conditions • Kidney Stones, con’t – Usually detected by an X-Ray or Ultrasound – Some small stones may pass on their own – Larger stones must either be broken up with Shock Wave Lithotripsy or be removed with surgery
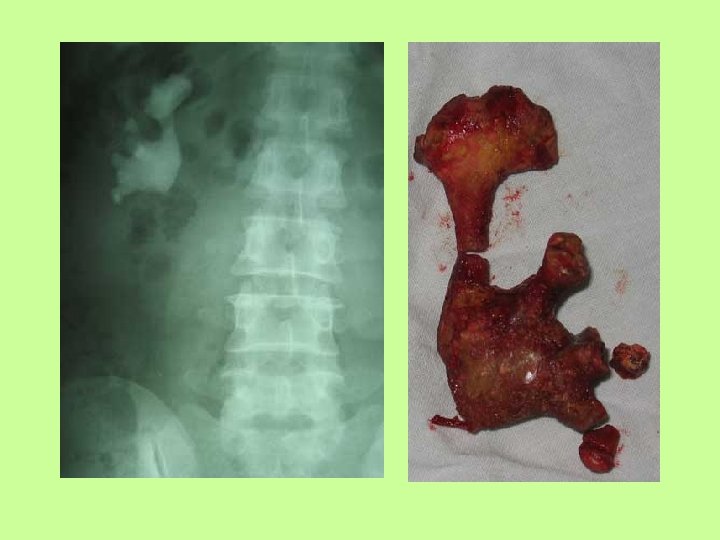

• FYI: Stones can look different depending on what ions precipitated out! • http: //www. herringlab. com/photos/

http: //www. youtube. com/watch? v=ODL 3 e. EZ CY 8 M&feature=related http: //www. youtube. com/watch? v=48 AWCO CG 5 ug&feature=fvw

Urinary Conditions • Urinary Incontinence (UI) – Involuntary leakage of urine – Different Types…

• Stress UI – Due to insufficient strength of pelvic floor muscles – In men, is common following removal of the prostate – In women, is common as a result of pregnancy and childbirth • Urge UI – Involuntary loss of urine due to random spasms of the bladder muscles – Can be due to damage of nerves

• Functional UI – A person knows they need to go, but cannot make it to the bathroom in time, usually due to some issue with thinking, moving, or communicating • Overflow UI – Because of weak bladder muscles or some sort of nervous system condition, the bladder is never completely emptied – This causes the person to “dribble” out urine

Urinary Conditions • Urinary Tract Infection – Caused by a bacteria that has entered through the urethra and multiplied in the urine – UTI’s are more common in those who are sexually active, and those with anatomical malformations of the urinary tract – Females are more prone than males to UTI’s because the urethra is much shorter and closer to the anus than in males – Usually treated with antibiotics

Old Wives’ Tale? ? ? • Some say that cranberry juice can lower the rate of UTI’s because certain components of the juice can prevent the adherence of certain pathogens to the epithelium of the urinary bladder

Renal Failure • Decreased rate of glomerular filtration • Can be caused by injury or by disease (including high blood pressure and diabetes) • Can be detected by elevated fluid and ion levels in the blood • Nitrogen wastes (such as urea) remain in the blood • Can lead to cardiovascular disease • If situation is bad enough, it can lead to the need for dialysis or a kidney transplant

Dialysis • Provides an artificial replacement for lost kidney function for people with renal failure • Utilizes the principles of diffusion, where substances in water tend to move from areas of higher concentration to lower concentrations • Blood flows by one side of a semi-permeable membrane, and a special fluid flows by the opposite side • Small solutes (such as ions and nitrogen wastes) are removed, but larger solutes (such as RBC’s and large proteins) remain in the blood
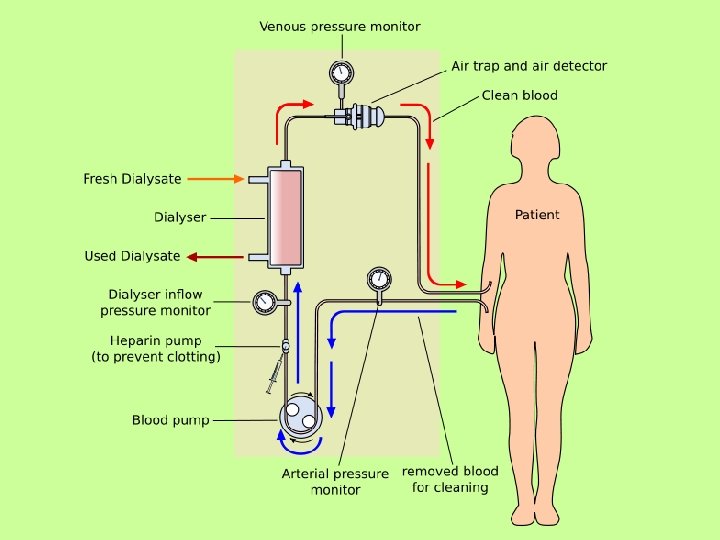

• http: //www. youtube. com/watch? v=jp. Qtn. V C 47 i. I&feature=related • http: //www. youtube. com/watch? v=E 8 Uj-C 1 -Hy. U • http: //www. youtube. com/watch? v=WZos. H ub 0 MOQ&feature=related

• Dr. Willem Kolff, a Dutch physician, constructed the first working dialyzer in 1943 during the Nazi occupation of the Netherlands. Due to the scarcity of available resources, Kolff had to improvise and built the initial machine using sausage skins, drink cans, a washing machine, and various other items that were available at the time. Over the following two years, Kolff treated 16 patients that suffering from acute kidney failure using his machine, but the results proved unsuccessful. Then in 1945, a 67 year old woman in uremic coma regained consciousness following 11 hours of haemodialysis with the dialyzer, and lived for another 7 years before passing away of an unrelated condition. This was the first patient to ever be successfully treated with dialysis.

• http: //www. youtube. com/watch? v=w. BBl. Jh 1 v. IZc • http: //www. youtube. com/user/UCLAHealth #p/u/80/2 fj. Vz 3 k. Vna. A
Urinalysis • Urinalysis is a diagnostic physical, chemical, and microscopic examination of a urine sample (specimen) • Specimens can be obtained by normal emptying of the bladder (voiding) or by a hospital procedure called catheterization

Purposes of Urinalysis • General evaluation of health • Diagnosis of metabolic, systemic, or endocrine disorders • Diagnosis of diseases or disorders of the kidneys or urinary tract • Monitoring of patients with diabetes • Testing for pregnancy • Screening for drug abuse

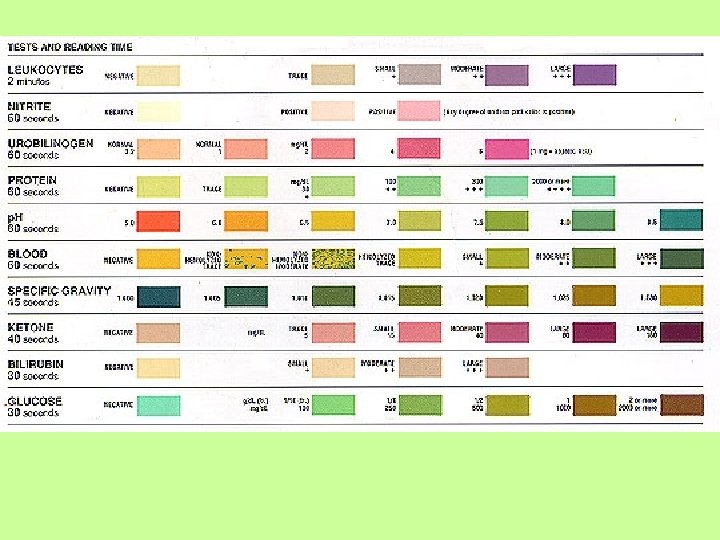
Urinalysis • Dipsticks are thin strips of plastic that change color in the presence of specific substances… can be used to measure… • Specific gravity (density) • Acidity of the urine (p. H) • The presence of blood, proteins, or sugars • Substances produced during the breakdown of fatty acids (ketones)

- Slides: 64