Unhealthy Alcohol Use in People with HIV Infection





















- Slides: 26

Unhealthy Alcohol Use in People with HIV Infection: The Role of Pharmacotherapy Richard Saitz MD, MPH, FACP, FASAM Professor of Medicine & Epidemiology Boston University Schools of Medicine & Public Health Director, Clinical Addiction, Research and Education (CARE) Unit Boston Medical Center Supported by NIAAA U 24 AA 020801 01, U 01 AA 020802 01, U 01 AA 020793 01

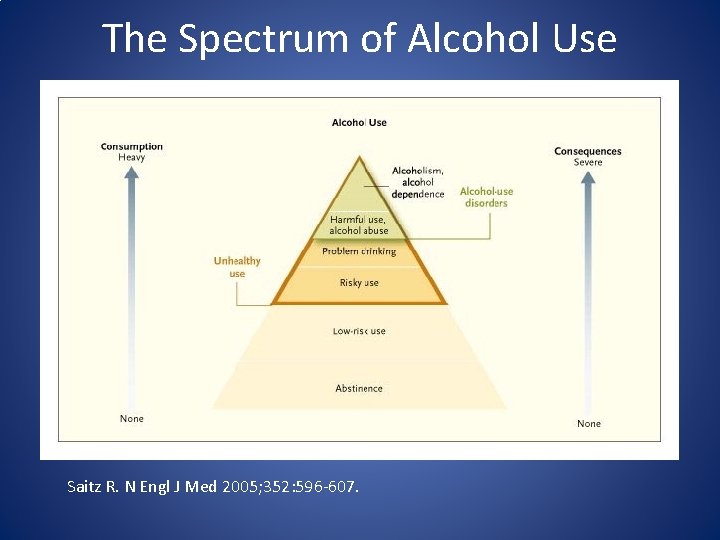
The Spectrum of Alcohol Use Saitz R. N Engl J Med 2005; 352: 596 -607.

Standard Drinks

Prevalence of Unhealthy Alcohol Use Among People With HIV Cost and Services Utilization Study (n=2864)* 8% HIV Research Network (n=951)† 11% Women’s Interagency HIV Study (n=2770)‡ 14 -24% (11 -year period) Veterans Aging Cohort Study (n=881)** 36% (AUDIT ≥ 8) * Galvan, Bing, Fleishman, et al. J Stud Alcohol. 2002; 63: 179 -186. † Chander, Josephs, Fleishman, et al. HIV Med. 2008; 9: 196 -202. ‡ Cook, Zhu, Belnap, et al. Am J Epidemiol. 2009; 169: 1025 -1032. ** Conigliaro, Gordon, Mc. Ginnis, Rabeneck, Justice. J AIDS. 2003; 33: 521 -525.

Alcohol and ART Non-adherence† • Meta-Analysis of 40 studies and over 25, 000 participants – Risky and dependent drinkers were less likely to be adherent than lower risk drinkers and abstainers (OR 0. 5) Alcohol Use and Risky Sex* • Meta-analysis (n=27 studies) found… – Any alcohol consumption (OR 1. 6) – Problematic drinking (OR 1. 7) – Alcohol use in sexual contexts (OR 2. 0) …significantly associated with unprotected sex among HIVinfected individuals †Hendershot, Stoner, Pantalone, Simoni. J AIDS. 2009. 52: 180 -202. * Shuper, Jonarchi, Irving, Rehm. AIDS Behav. 2009; 13: 1021 -1036.

Alcohol and HIV Disease Progression • Prospective study of 595 HIV+ adults with past or current ‘alcohol problems’ − Among patients not on ART, CD 4 counts averaged 48. 6 cells lower for those with heavy alcohol use v. abstinence (p=0. 03) Samet. JAIDS. 2007; 46: 194 -9.

Screening for Unhealthy Alcohol Use • Single question: How many times in the past year have you had X or more drinks in a day? (where X is 5 for men and 4 for women) A positive test is >1

AUDIT-C (Alcohol Use Disorders Identification Test-Consumption) Question 1: How often do you have a drink containing alcohol? (0) (1) (2) (3) (4) Never Monthly or less 2 to 4 times a month 2 to 3 times a week 4 or more times a week Question 2: How many drinks containing alcohol do you have on a typical day when you are drinking? (0) (1) (2) (3) (4) 1 or 2 3 or 4 5 or 6 7, 8, or 9 10 or more Question 3: How often do you have 4 or more (women) 5 or more (men) drinks on one occasion? (0) (1) (2) (3) (4) Never Less than monthly Monthly Weekly Daily or almost daily >3 in women, >4 in men is positive

Assessing Severity of Unhealthy Use • 10 item AUDIT* – 10 questions, each scored 0 -4 – ≥ 3 (women) ≥ 5 (men) = unhealthy use • NB ≥ 8 is “old” cutoff – ≥ 13 (women) or ≥ 15 (men) consistent with dependence • M. I. N. I. -International Neuropsychiatric Interview (MINI)** – Diagnosis of disorder (abuse/dependence) *http: //whqlibdoc. who. int/hq/2001/who_msd_msb_01. 6 a. pdf and Johnson et al Alcohol Clin Exp Res 2012. Adjust item 3 to 4 drinks for women, 5 for men. Can use 4/6 cutoffs if combined with single-item heavy drinking question [e. g. +score or heavy use]. **https: //medical-outcomes. com/ and Sheehan et al J. Clin Psychiatry, 1998; 59(suppl 20): 22 -33

Addressing Substance Use: Brief Intervention • 10 -15”, empathic • Feedback – Ask permission – Ask what patient thinks of it • Advice (clear) • Goal setting – Negotiate – Menu of options – Support self-efficacy • Follow-up “You are drinking more than is safe for your health. ” “My best medical advice is that you cut down or quit. ” “What do you think? Are you willing to consider making changes? ” Saitz R. N Engl J Med 2005; 352: 596 -607. Samet, Rollnick, Barnes. Arch Intern Med. 1996; 156: 2287 -2293 Boston University Alcohol Clinical Training Program http: //www. bu. edu/act/ and www. mdalcoholtraining. org

Rationale for Pharmacotherapy • Alcohol dependence is a chronic condition • Medications can target neurotransmitters involved in the reinforcing and anxiolytic effects of alcohol use • Beneficial in combination with non-pharmacologic therapy, including counseling and other behavioral therapies • Can reduce relapse and help maintain abstinence

Advantages of HIV care clinic for alcohol pharmacotherapy HIV clinics offer a potential opportunity for the integration of alcohol pharmacotherapy, given: – The long-term care of patients – The integration of a variety of specialty services (e. g. , psychiatric services) – Funding for prescription medications – Intensive case management models that promote outreach to and retention of patients who are often challenging to treat

Patient Selection for Pharmacotherapy • All people with alcohol dependence who are: – currently drinking – experiencing craving or at risk for return to drinking • Considerations – Specific medication contraindications – Alcohol withdrawal– most can safely cut down/quit without medication/inpatient stay – http: //pubs. niaaa. nih. gov/publications/arh 22 -1/05 -12. pdf – Consider risks (age, comorbidity, past seizures or delirium); reassess – Psychosocial support/therapy and follow-up • Primary care medical management* as effective as specialized behavioral therapy** *O’Malley SS et al. Arch Int Med 2003; 163: 1695 -1704. **Anton RF et al. JAMA 2006 May 3; 295: 2003 -17. *Latt NC, et al. Med J Australia 2002; 176: 530 -534.

Current Treatment Options FDA Approved Medications Under Investigation • Naltrexone • Ondansetron – Oral – Injectable • Acamprosate • Disulfiram – Early onset dependence • SSRIs – Late onset dependence – Anxiety/depression • Topiramate – Side effects/tolerability • Baclofen – No effect on liver

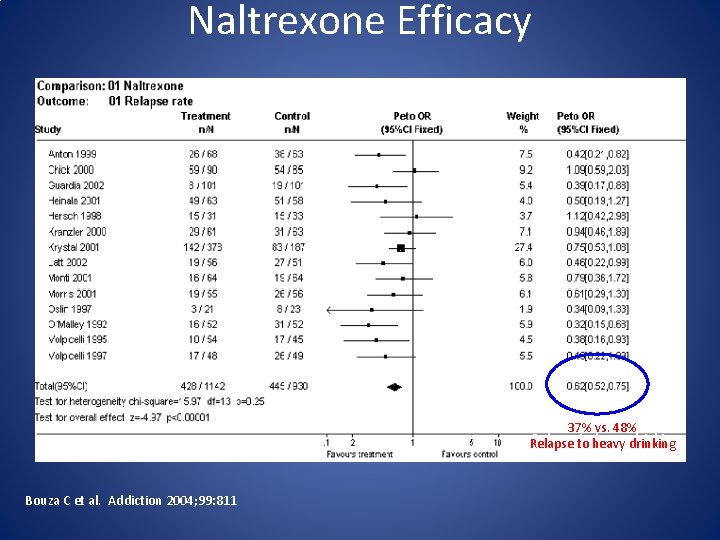
Naltrexone Efficacy 37%vs. 48% Relapse to to heavy drinking Relapse Bouza C et al. Addiction 2004; 99: 811

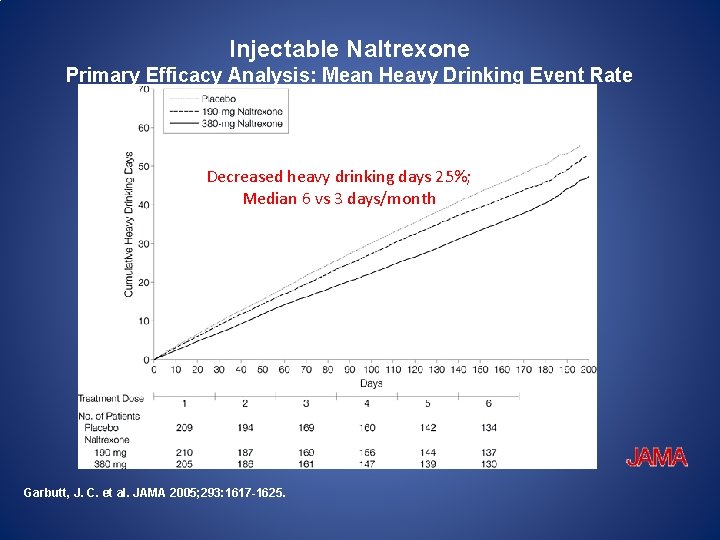
Injectable Naltrexone Primary Efficacy Analysis: Mean Heavy Drinking Event Rate Decreased heavydrinking days 25%; Decreased heavy days 25%; Median 66 vsvs 3 3 days/month Median Garbutt, J. C. et al. JAMA 2005; 293: 1617 -1625.

Prescribing Naltrexone 12. 5 mg/d-->25 mg/d-->50 mg/d (100 mg) or 380 mg IM per month • Main contraindication: opiates • Main side effects: nausea, dizziness • Monitor LFTs post medication initiation • No known drug interactions with antiretroviral therapy

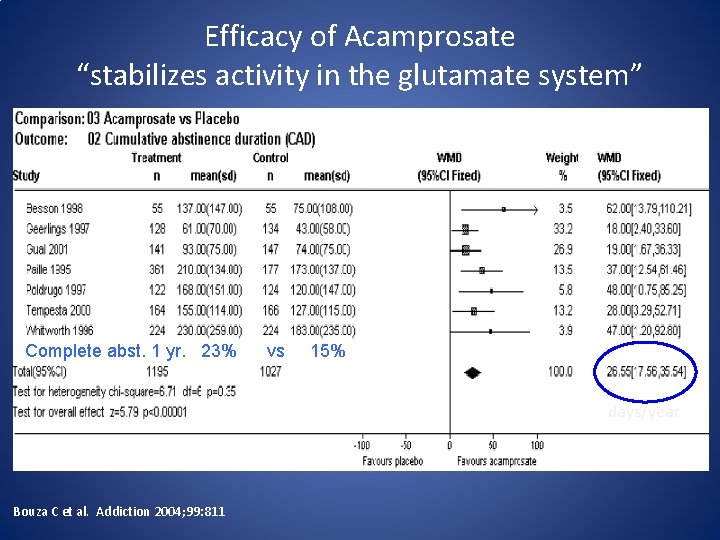
Efficacy of Acamprosate “stabilizes activity in the glutamate system” Complete abst. 1 yr. 23% vs 15% days/year Bouza C et al. Addiction 2004; 99: 811

Prescribing Acamprosate 666 mg tid • Main contraindication: renal insufficiency • Main side effect: diarrhea • No known drug interactions with antiretroviral therapy

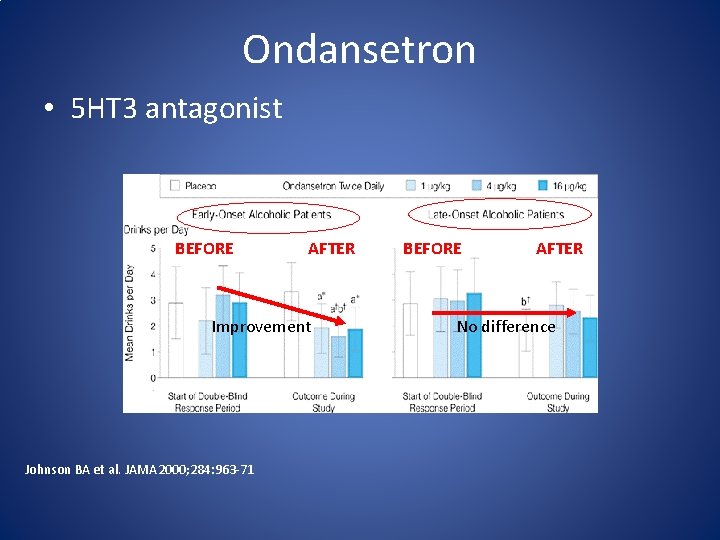
Ondansetron • 5 HT 3 antagonist BEFORE AFTER Improvement Johnson BA et al. JAMA 2000; 284: 963 -71 BEFORE AFTER No difference

Prescribing Ondansetron: 4µg/kg twice daily • Much lower (e. g. 0. 3 mg) than doses for FDA approved indications • For early onset (<age 25) alcohol dependence • Main contraindications: QT prolongation • May have interactions with ART • Main side effects: constipation, headaches, sedation

Disulfiram: works when monitored Randomized studies Author, Yr Follow-up Disulfiram Abstinence Gerrein, 1973 85%, 39% Monitored Unmonitored 40% 7% Azrin, 1976 90% Monitored Unmonitored 90 -98% 55% Azrin, 1982 100% Monitored Unmonitored 73%* 47* Liebson, 1978 78% Monitored Unmonitored 98% 79% Length of follow-up: Gerrein 1973: 8 weeks; Azrin 1976: 2 years, Azrin 1982: 6 months; Liebson 1978: 6 months. *Thirty-day abstinence at 6 months.

Prescribing Disulfiram 250 mg/d-->500 mg/d • Main contraindications: recent alcohol use, cognitive impairment, risk of harm from disulfiram--ethanol reaction, drug interactions, rubber, nickel or cobalt allergy • No known drug interactions with antiretroviral therapy – BUT ritonavir liquid and tipranavir caps contain alcohol • Main side effects: hepatitis, neuropathy

Prescribing Tips • Duration of treatment – Most studies 3 -4 months, treatment up to one year, maybe more • Frequency of follow-up – Check LFTs after initiation of naltrexone or disulfiram – Use local clinic resources (nursing) to call patients and discuss adherence to medications and side effects OR have patient return to clinic to discuss • Providing Support – Brief advice can be provided to encourage drinking reduction by physicians, nurses, social workers, counselors – http: //pubs. niaaa. nih. gov/publications/Practitioner/Clinicians. Guide 2005/clinicia ns_guide 19 b_support_p. htm (Google NIAAA Clinicians Guide)

Other Tips • Abstinence desirable but not required for initiation (except disulfiram) • Remind patients that even if they continue to drink alcohol, they should still take their HIV medications and their alcohol medication (unless on disulfiram). • Refer patients to on-line resources (http: //rethinkingdrinking. niaaa. nih. gov/)

Summary • Alcohol use among people with HIV is associated with HIV disease progression, worse medication adherence and increased HIV transmission risk behaviors • Screening and brief intervention for unhealthy alcohol use is a critical component of HIV primary care • Use of pharmacotherapy in persons with alcohol dependence may decrease craving and reduce heavy drinking/promote abstinence