Understanding the Basics of Therapeutic Exercise Chapter 12

Understanding the Basics of Therapeutic Exercise Chapter 12

Cryotherapy is cold/ice Cryotherapy cools through conduction 20 -30 minutes application Indications: acute injury, pain, swelling, muscle spasm, inflammation, recovery Contraindications: respiratory problems, open wounds, cardiac conditions, circulations or sensory deficits, increased blood pressure, advanced diabetes, peripheral vascular disease, infection Benefits of cryotherapy include: Decreased pain Decreased Swelling Vasoconstriction Decreased Spasm

Cryotherapy Types of Cryotherapy Ice Bag: 20 minute average Chemical Ice Pack: 20 minute average, use barrier Ice Bucket: 15 minute average, use a toe cover Cold Whirlpool: 50 -55 degrees, 10 -15 minutes Ice Massage: 7 -10 minutes Cold Spray 4 Stages of Cold Burning Aching Numbness

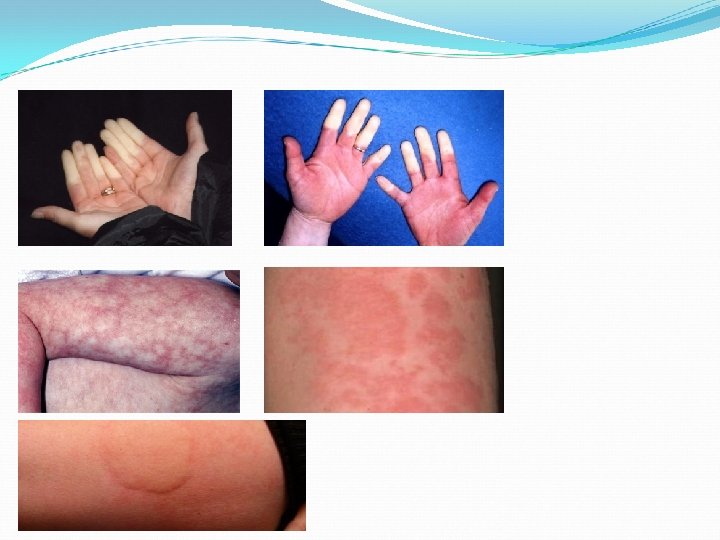
Cryotherapy Reactions Raynaud’s Phenomenon: A condition in which cold temperatures or strong emotions cause blood vessel spasms. This blocks blood flow to the fingers, toes, ears, and nose. First, the fingers, toes, ears, or nose to become white, then turn blue. When blood flow returns, the area becomes red and then later returns to normal color. The attacks may last from minutes to hours. Hunting Response: An unusual reaction of digital blood vessels exposed to cold(during hunting in wintertime); vasoconstriction is alternated with vasodilation in irregular repeated sequence. Intermittent supply of warm blood to cold exposed extremities. Mottling To mark with spots or blotches of different shades or colors. n. 1. A spot or blotch of color. 2. A variegated pattern, as on marble
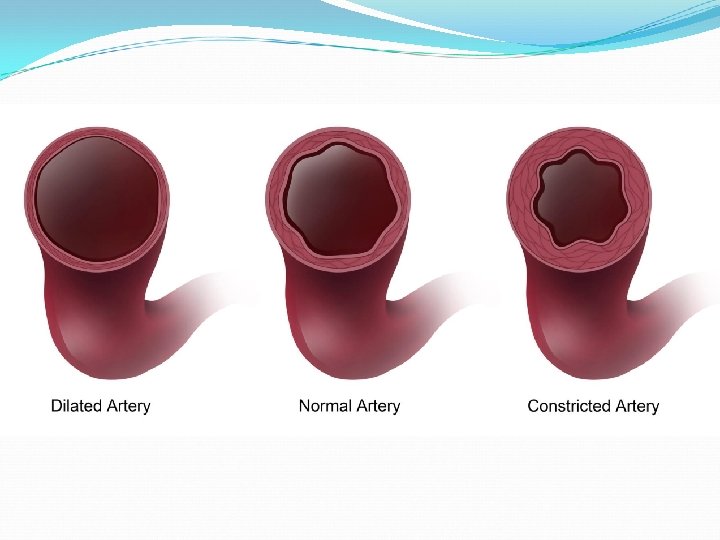

Thermotherapy is heat Heat is transferred by circulation or conduction Physiological Response to heat: decrease spasm, decreased pain, vasodilation (increased blood flow), increased elasticity, increased swelling, decreased joint stiffness, increased temperature Indications: chronic inflammation, joint contracture, tight tissue, chronic pain, chronic muscle spasm Contraindications: acute injuries, decreased sensation, decreased circulation, tumors, open wounds, peripheral vascular disease Types of Heat: average treatment time 20 -30 minutes Moist Heat Pack Paraffin Wax Warm Whirlpool: 98 – 100 degrees Fluidotherapy

Ultrasound Use of sound waves generated through a transducer head to penetrate soft tissues. The difference between the two types of ultrasound therapy is the rate at which the sound waves penetrate the tissues Thermal ultrasound therapy: uses a more continuous transmission of sound waves. The sound waves cause microscopic vibrations in the deep tissue molecules, increasing heat and friction. The warming effect encourages healing in the soft tissues by increasing the metabolism at the level of the tissue cells Mechanical ultrasound therapy: uses pulses of sound waves to penetrate tissues. While this still has a minor warming effect on the tissues, it also causes expansion and contraction in the tiny gas bubbles of the soft tissues. This helps to decrease the inflammatory response, reducing tissue swelling and thus decreasing pain 1 MHz (deep) vs. 3 MHZ (shallow) 10%, 20%, 50%, 100% Indications: chronic inflammation, acute injuries (non-thermal), muscle strains, ligament sprains, bruises, muscle spasms, scar tissue, tightened soft tissue Contraindications: decreased circulation, decreased sensation, tumors, growth plates, not over heart, not over eyes, not over nerve plexus, NO thermal with acute injuries, pregnancy, not near spinal cord, vascular problems Physiological Response: Thermal = increases temperature, increased range of motion, increased elasticity, deeper penetration of hear Non-thermal = decreased chronic inflammation, helps with scar maturation
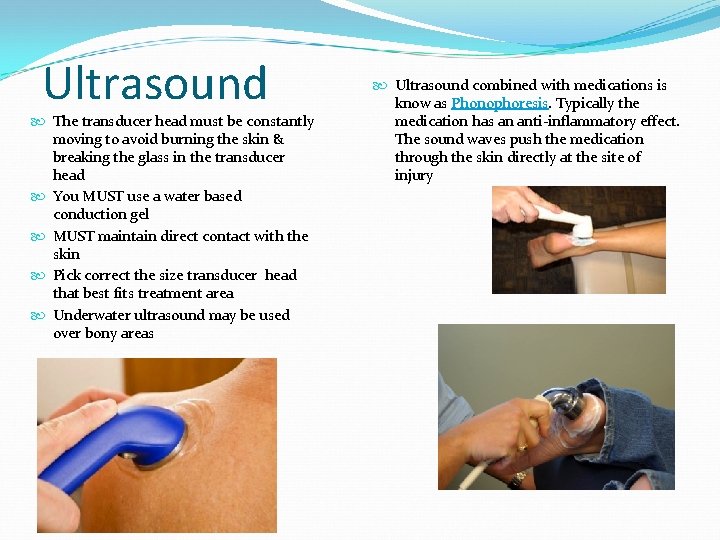
Ultrasound The transducer head must be constantly moving to avoid burning the skin & breaking the glass in the transducer head You MUST use a water based conduction gel MUST maintain direct contact with the skin Pick correct the size transducer head that best fits treatment area Underwater ultrasound may be used over bony areas Ultrasound combined with medications is know as Phonophoresis. Typically the medication has an anti-inflammatory effect. The sound waves push the medication through the skin directly at the site of injury

Electrical Stimulation Direct Current (continuous, uninterrupted) vs. Alternative (pulsed, interrupted) Usually combined with another modality Uses electricity: the flow of electrons between two points Treatment time is usually around 15 -20 minutes Place pads at least a pad length apart Physiological Response: decreased pain, decreased spasm, decreased swelling, increased muscle strength, muscle reeducation, increased circulation, stimulate body tissue to speed up healing Indications: pain, edema, muscle spasm, muscle weakness, muscle reeducation, to increase circulation Contraindications: pregnancy, unknown pain, pacemaker, infection, fracture, not over heart, not over eyes, not over carotid sinus, not over airway, open wound, tumors

Types of Electrical Stimulation Premodulated: 2 pads Interferential: 4 pads Microcurrent (low intensity) Russian: 2 pads across muscle TENS: Transcutaneous Electrical Nerve Stimulation

Gate Control Theory The gate control theory of pain asserts that nonpainful input closes the "gates" to painful input. Closing the “gates” prevents pain sensation from traveling to the central nervous system. Therefore, stimulation by non-painful input is able to suppress pain.

Goal of Therapeutic Exercise Return injured participant to pain-free functional activity Return the athlete to the same level they were prior to injury Components of a Rehabilitation Program Swelling Pain Modulation ROM & flexibility Strength, Power & Endurance Neuromuscular Control Balance Cardiovascular fitness Functional Progressions Functional Testing

Psychological Aspects Impact of sport or activity participation on self -identity and esteem. Who are they without the sport? Injury can be devastating Physical and emotional need to be met in order to progress Remember: Each person reacts differently to an injury… Know your athletes! Individualize your treatment.

Adjustment to Injury Stage model Kübler-Ross stages of grieving Denial and isolation Anger Bargaining Depression Acceptance Cognitive model Accounts for individual differences Personal and situational factors

Coping with Injury – Assistance Education Goal setting Helps guide and motivate Process Establish trust and respect Develop partnership Goals should be: Realistic, objective, measurable, and attainable Long-term and short-term

Mental Skills Training – Interventions · Relaxation – Reduces pain, anxiety, and tension – Slows breathing, lowers heart rate · Imagery – Mentally practice skills or processes · Positive self-talk – Redirect negative thoughts into positive task-oriented thoughts

ATC’s Role of the ATC Do not negate the individual's emotional responses to the process Provide positive encouragement Include the patient as an integral part of the rehab process. Give the athlete some control. Referral for psychological problems Establish a procedural plan General rule: any psychological difficulty that persists for more than a few days and interferes with the progress of rehabilitation should be referred Follow-up

Developing a Therapeutic Exercise Program Steps Assess the patient Current level of function and dysfunction Subjective and objective components of SOAP Interpret the assessment Identify § § Part factors outside normal limits Primary deficits Secondary problems of assessment component of SOAP Establish goals (Plan) Therapist and patient work together Long-term and Short-term Part of assessment component of SOAP

Developing a Therapeutic Exercise Program Develop and supervise the treatment plan Incorporate therapeutic exercise, modalities, and medication Four phases Inflammatory response, pain, swelling, and ecchymosis are controlled Regaining ROM Restoring muscle strength, endurance, and power Prepares the individual to return to activity and includes sportspecific skill training, regaining coordination, and improving cardiovascular conditioning Reassess the progress of the program Adjust as needed

Phase 1: Controlling Inflammation Goal Control swelling Limit hemorrhage, edema, effusion, muscle spasm, & pain Reduce length of immobilization If you limit the athlete’s pain they will be more actively involved in the rehabilitation process Treat acute symptoms PRICE Modality options Cryotherapy, intermittent compression, EMS Electrical therapy TENS

Protection Post Injury Depends on: Injury severity, structures damaged Philosophy of supervising health care provider Restricted activity “Relative rest” Detraining Can occur after only 1– 2 weeks of inactivity

Criteria for Progression to Phase 2 Control of inflammation Athlete should have minimal edema/ swelling, muscle spasm, and pain Working on Range of Motion (ROM) & joint flexibility

Phase 2: Restoration of Motion Focus: Restoring ROM and flexibility Maintaining general body strength Factors that limit joint motion Bony block Joint adhesions Muscle tightness Tight skin or inelastic dense scar tissue Swelling Pain Fat or other soft tissues that block normal motion

Restoration of Motion Passive ROM: the patient isn’t using an active muscle contraction to cause the motion Flexibility Agonists v. Antagonists Ballistic (movement) v. Static (no movement) PNF – Proprioceptive Neuromuscular Facilitation

Active Assisted and Active ROM Active Assisted ROM Working the limb through available pain-free motion with assistance will more quickly restore normal active ROM than working within limited voluntary motion Active ROM Enhances circulation Initiation of strength exercises before full AROM Should be relatively painless

Resisted ROM (RROM) · Static or dynamic · Static Measured with an isometric muscle contraction – Used during phases 1 and 2 in pain-free arc of motion – · Dynamic – Isotonic training Advantages – Disadvantages – Technique –

Criteria for Progression to Phase 3 Limited swelling & edema (if any) Inflammation and pain under control ROM within 80% of normal Pain free ROM Bilateral joint flexibility restored Cardiovascular endurance and general body strength maintained

Phase 3: Muscle Strength, Endurance & Power Focus: Restoring the function of the a body part to pre-injury status Techniques: Isometric Progressive Isokinetic Plyometric Resistance - Isotonic

Phase 3: Developing Muscular Strength, Endurance, & Power Muscular strength Ability of a muscle or group of muscles to produce force in one maximal effort Concentric contraction Shortening; decreases joint angle Work to accelerate a limb Eccentric contraction Lengthening (elongate); increases joint angle Work to decelerate a limb and provide shock absorption

Open vs. Closed Kinetic Chain Exercises Closed kinetic chain (CKC) Distal segment of the extremity cannot move independently Weight bearing Example – Squats, leg press, or pushups Open kinetic chain (OKC) Distal segment of the extremity is free to move without causing motion at another joint Non–weight bearing Example – Leg extensions or bicep curls

Static Strength Isometric exercise Increase Static Strength Decrease muscle atrophy No joint movement Can be used during immobilization period Can decrease swelling by causing a muscle pumping action
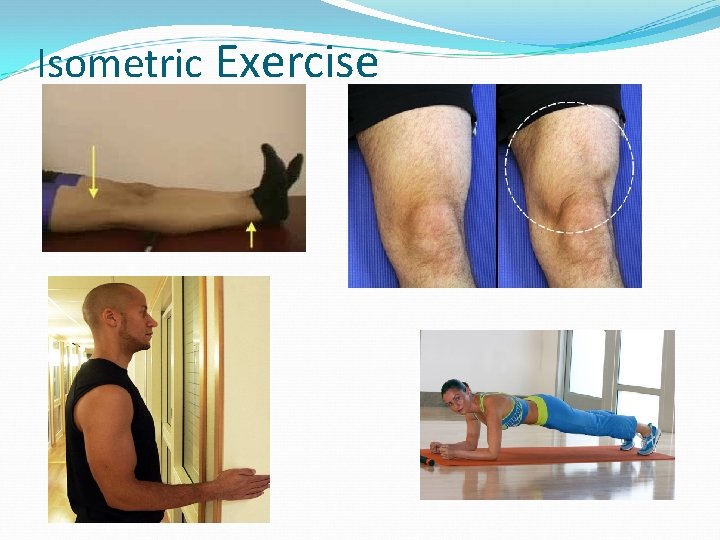
Isometric Exercise

Dynamic Strength Progressive Resistance - Isotonic exercise Variable speed/fixed resistance Advantages Permits exercise of multiple joints simultaneously Allows both eccentric & concentric contractions Permits weight-bearing, CKC exercises Disadvantage When a load is applied, the muscle can only move that load through the ROM with as much force as the muscle provides at its weakest point

Progressive Resistance Isotonic Exercise

Isokinetic Exercise Isokinetic exercise Fixed speed/variable resistance Biodex Ankle Biodex Knee Advantages 100% loading throughout ROM Pain disengages mechanism Disadvantages As muscle fatigues, resistance decreases Most machines only permit concentric contraction $$$$
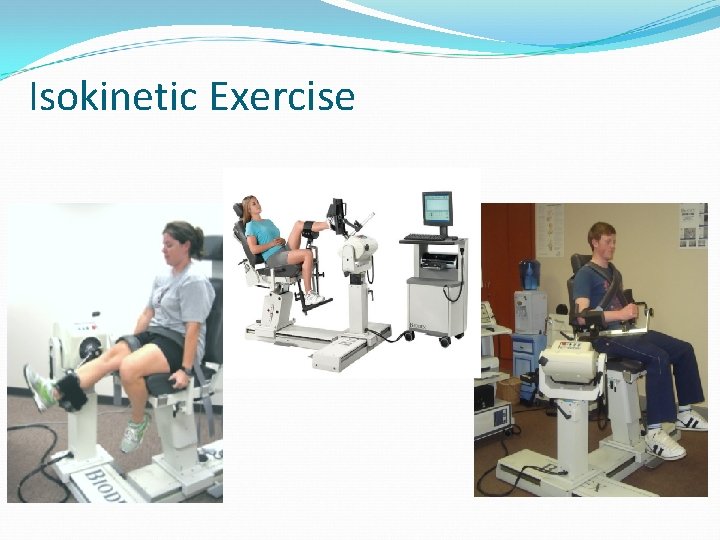
Isokinetic Exercise

Muscular Endurance and Power Muscular endurance Ability of muscle tissue to exert repetitive tension over an extended period Fatigue is related to endurance Relationship between strength and endurance Lifting low weights/faster velocity/more reps

Muscular Endurance and Power Muscular power Ability of muscle to produce force in a given time Started when at least 80% of strength Weight training at higher contractile velocities Use of Plyometric exercises Explosive exercise: quick concentric contraction followed by an eccentric contraction Caution: injury potential

Plyometric Exercise

Functional Application of Exercise Overload principle physiologic improvements occur only when an individual physically demands more of the muscles than is normally required (based on SAID) SAID principle: Specific Adaptations to Imposed Demands. the body responds to a given demand with a specific and predictable adaptation achieved by manipulating intensity, duration, frequency, specificity, speed, and progression

Functional Application of Exercise Intensity—reflects both the caloric cost of the work and the specific energy systems activated Strength gains depend primarily on intensity of overload, not the specific training method Daily Adjustable Progressive Resistance Exercise objective method of increasing resistance as the individual’s strength increases or decreases Effective, but not advised in early phases of rehabilitation may not be appropriate for chronic injuries or early postoperative rehabilitation; high weights can potentially cause a breakdown of the supporting soft tissue structures and exacerbate the condition

Functional Application of Exercise Strength: weight/ reps Early phases high-repetition, low-weight exercise may be more productive can stimulate blood flow and limit tissue damage Endurance: reps/ weight Endurance begin with 2– 3 sets of 10 reps, progressing to 5 sets of 10 reps, as tolerated when able to perform 50 reps, 1 pound may be added, and exercise reduced to 3 sets of 10 reps exercises should be performed slowly, concentrating on proper technique

Functional Application of Exercise Duration The length of a single exercise session Minimum: 20 minutes in absence of pain, swelling, or muscle soreness Frequency Number of exercise sessions per day or week 3– 4 times per week Twice per day may be appropriate Do not work the same muscle groups on successive days

Functional Application of Exercise Speed Rate at which the exercise is performed Initially, slow, deliberate movements Eventually, vary speeds Progression Objective improvement should occur each day Orderly progression with ever-increasing demands as healing process allows

Criteria for Progression to Phase 4 Bilateral ROM and flexibility restored Muscular strength, endurance, and power equal or near equal to those of the unaffected limb Cardiovascular endurance and general body strength at or better than the pre-injury level Sport-specific functional patterns completed using mild-to-moderate resistance Individual psychologically ready to return to protected activity

Phase 4: Return to Sport Activity Focus Correct any biomechanical inefficiencies in motion Restore coordination and muscle strength, endurance, and power in sport-specific skills

Phase 4: Return to Sport Activity Coordination Body’s ability to execute smooth, fluid, accurate, and controlled movements Categories Gross movement Fine movement Direct link with proprioception Improving coordination

Regaining Proprioception Injury can interrupt the neuromuscular feedback mechanisms to the CNS Restoration of feedback is necessary to promote dynamic joint and functional stability to prevent re-injury Mind’s attempt to teach the body conscious control of a specific movement Exercises Specific to type of activity Functional Strengthening exercises are essential Progression: slow-speed to high-speed, low-force to high-force, and controlled to uncontrolled activities

Proprioception and Kinesthesia Proprioception – sensation of joint position Kinesthesia – sensation of joint movement Balance – postural stability Information is sent from sensory receptors to CNS relative to tissue deformation Without balance training the athlete is predisposed to re-injury

Components of Phase 4 Cardiovascular endurance Body’s ability to sustain sub-maximal exercise over an extended period Detraining occurs within 1– 2 weeks Cardiovascular level impacts fatigue ACSM recommends Activity 3– 5 days per week 20 minutes Intensity of 60– 90% of maximal heart rate (HR max)

Components of Phase 4 Functional Progressions: gradually progressive activities designed to prepare an athlete for return to a specific sports Sport-specific conditioning Exercise should progress to the load and speed expected for the individual’s sport Exercises must be coupled with functional training Broken down into component parts Advance if activity doesn’t produce pain or swelling & athlete can perform without deficit Progress to position specific

Functional Progressions Assist the athlete in achieving normal pain free range of motion, restore adequate strength levels & regaining neuromuscular control throughout the entire rehabilitation program Example of lower extremity progression Walking Jogging Track , Walking Curves Jogging Full Track Run Track, Jog Curves Run Full Track Run for Fitness Lunges Sprints Acceleration/Deceleration Run Shuffle slide to Shuffle run Carioca

Functional Testing Uses functional progression drills for the purpose of assessing the athlete’s ability to perform a specific activity Performance of a single maximal effort to give some idea of how close the athlete is to a full return to activity Examples: agility runs such as figure eights, shuttle runs or cariocas. Other tests include: side stepping, vertical jumps, hopping for time and distance,

Return to Sport/Activity Criteria Individual can return to their sport activity as soon as: muscle strength, endurance, and power are restored Balance & Neuromuscular control are regained Cardiorespiratory fitness is at pre-injury level Functional Testing is within 85%-90% of unaffected side
- Slides: 55