Understanding Cardiotocography CTGs Max Brinsmead MB BS Ph

Understanding Cardiotocography – “CTGs” Max Brinsmead MB BS Ph. D May 2015
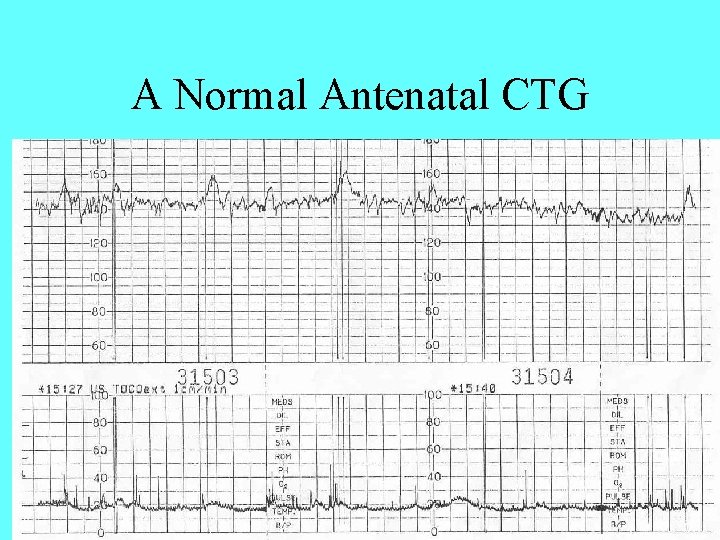
A Normal Antenatal CTG

Features of a CTG • • • Baseline Short term variability Accelerations Decelerations Response to stimuli • Contractions • Fetal movements • Other

Baseline Fetal Heart Rate • • • 110 to 150 bpm at term Faster in early pregnancy Below 100 = baseline bradycardia Below 80 = severe bradycardia Tachycardia common with maternal fever Tachycardia with reduced STV = early hypoxia

Accelerations • • • Must be >15 bpm and >15 sec above baseline Should be >2 per 15 min period Always reassuring when present May not occur when fetus is “sleeping” Should occur in response to fetal movements or fetal stimulation • Non reactive periods usually do not exceed 45 min • (>90 min and no accelerations is worrying)

Short Term Variability (or Beat to Beat Variability with a Scalp Clip) • Should be >5 bpm • The most important feature of any CTG • Is a reflection of competing acceleratory and decelerating CNS influences on the fetal heart • And therefore represents the best measure of CNS oxygenation • Will be affected by drugs • Will be reduced in the pre term fetus

Decelerations • Early: mirrors the contraction • Typically occurs as the head enters the pelvis and is compressed, i. e. it is a vagal response • Late: Follows every contraction and exhibits a slow return to baseline • Is quite rare but is the response of a hypoxic myocardium • Variable: Show no relationship to contractions • Mild • Moderate • Severe • In practice many “decels” or “dips” are MIXED
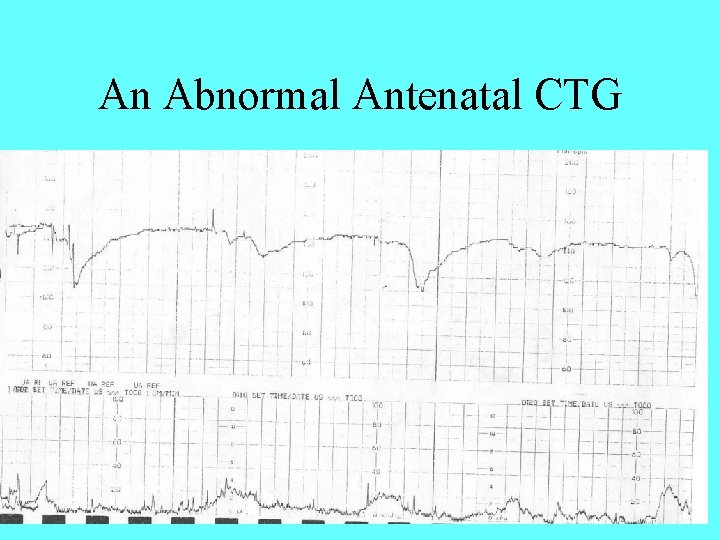
An Abnormal Antenatal CTG
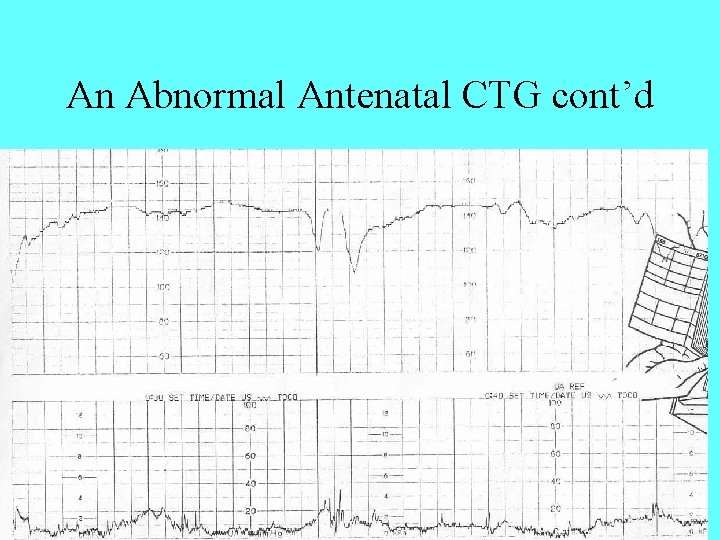
An Abnormal Antenatal CTG cont’d

Abnormal CTG Features • Reduced STV • No accelerations • Decelerations after most contractions with a slow return to baseline

In Practice a CTG is best regarded as a screening tool: • High negative predictive value • >98% of fetuses with a normal CTG will be OK • Poor positive predictive value • Up to 50% of fetuses with an abnormal CTG will be hypoxic and acidotic but 50% will be OK • Therefore the CTG should always be interpreted in its clinical context • And backed by fetal blood sampling PRN

A Classification of CTGs • Normal = all 4 features are reassuring • Suspicious = One non reassuring feature • Pathological = Two or more non reassuring features or a abnormal pattern

Non Reassuring Features of a CTG • • • Baseline <110>100 or >160<180 STV <5 for >40 min but <90 min Early decelerations Variable decelerations A single prolonged deceleration up to 3 min

A CTG is abnormal when: • • • Baseline is <100 or >180 bpm STV is <5 for >90 min Late decelerations are repeated Atypical variable decelerations occur Two prolonged decelerations for >3 min occur • Sinusoidal pattern >10 min

It is best to regard CTG as screening for fetal hypoxia:

An ideal screening test:

CTG as a screening test

CTG as a Screening Test • Positive predictive value = the chance that a screen positive individual will have the disease • For CTG this is never more than 50% • i. e. at least 50% of the time it will be unnnecessarily alarming

A screening test is more likely to be a true positive if

A screening test is more likely to be a true positive if It is positive in a high risk group

So always consider the clinical context

And be prepared to back up with a diagnostic test

Which, for the diagnosis of fetal hypoxia, is Scalp Blood p. H or lactate

Problems with Screening: • FALSE POSITIVES – And the resources required to deal with them • UNREALISTIC EXPECATATIONS – i. e. misunderstanding about the sensitivity of the test

Meta analysis of RCTs of Intrapartum CTG monitoring • 12 Trials (as of 2008) • In 10 centres in the US, Australia, Europe and Africa • 58, 855 women and 59, 324 babies • Both high and low risk pregnancies • Compared routine EFM with intermittent auscultation

Meta analysis Results • A significant decrease in: – rate of 1 minute Apgar scores less than 4 (RR = 0. 82 and CI 0. 65 - 0. 98) – Neonatal seizures (RR=0. 50 and CI 0. 32 - 0. 82)

Meta analysis Results • A significant increase in: The rate of intervention by Caesarean section and operative delivery (RR=1. 23 and CI 1. 15 - 1. 31)

Meta analysis Results • No effect on: – rate of 1 min Apgar scores <7 – rate of admissions to NICU – Perinatal death rate – 5 min Apgar scores – rate of Cerebral palsy

Any Questions? Please leave a note on the Welcome Page of this website
- Slides: 29