Understanding Blood Pressure Heart Parts Arteries Capillaries Veins

Understanding Blood Pressure

Heart Parts: • Arteries • Capillaries • Veins Your heart sends blood to the whole body • Oxygen • Nutrients • Carries away waste
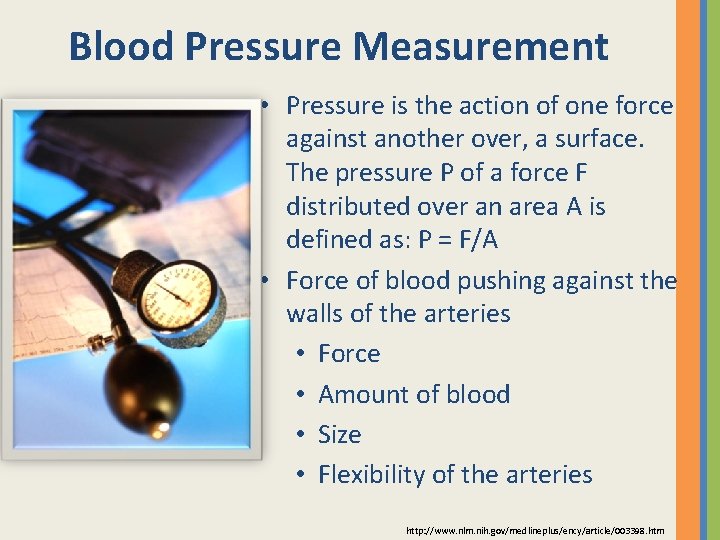
Blood Pressure Measurement • Pressure is the action of one force against another over, a surface. The pressure P of a force F distributed over an area A is defined as: P = F/A • Force of blood pushing against the walls of the arteries • Force • Amount of blood • Size • Flexibility of the arteries http: //www. nlm. nih. gov/medlineplus/ency/article/003398. htm

• The force of the blood against arterial walls. • Maximum blood pressure is exerted on the walls of arteries when the left ventricle of the heart pushes blood through the aortic valve into the aorta at the beginning of systole. • Pressure rises as the ventricle contracts and falls as the heart relaxes. • This continuous contraction and relaxation of the left ventricle creates a pressure wave that is transmitted through the arterial system.

What Does Your Blood Pressure Reading Mean? Normal • Less than 120 • Less than 80 Pre-hypertension • 120 -139 • 80 -89 High Blood Pressure – Stage 1 • 140 -159 • 90 – 99 High Blood Pressure – Stage 2 • 160 or higher • 100 or higher http: //familydoctor. org/online/famdocen/home/common/heartdisease/treatment/128. html http: //www. nhlbi. nih. gov/health/dci/Diseases/Hbp/HBP_What. Is. html
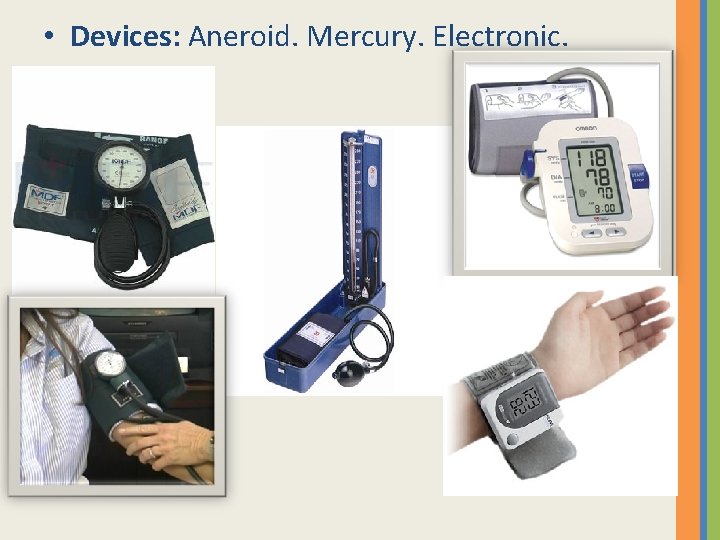
• Devices: Aneroid. Mercury. Electronic.

Blood Pressure measurement Devices • Features: 1 - Ease of use. Electronic > Aneroid > Mercury 2 - Cost. Electronic > Mercury > Aneroid 3 - Accuracy. Mercury > Aneroid > Electronic 4 - Memory. Electronic only.
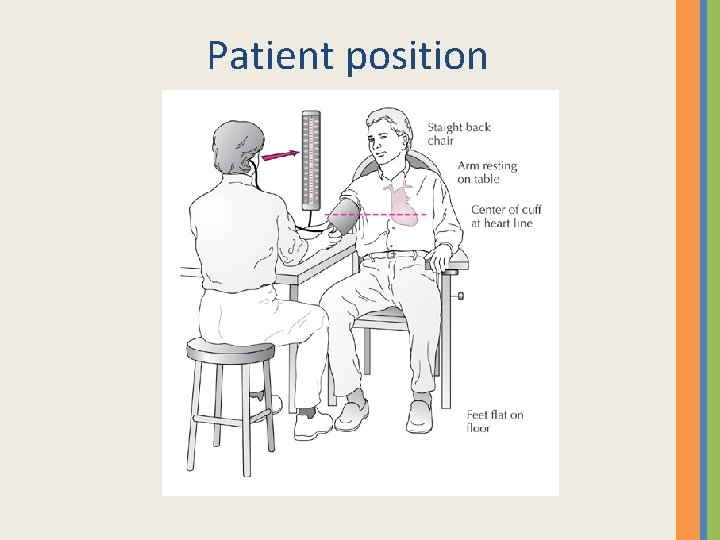
Patient position

Tips for Accurate Use • Same time of day • Use the same arm – Left • Don’t measure – immediately upon waking up, or – immediately after exercising. • Wait an hour.

METHODS FOR OBTAINING A BP • DIRECT – Direct intra-arterial measurement with a catheter arterial (ICU, surgery) • INDIRECT – Compression of the brachial artery using a sphygmomanometer(blood pressure cuff) or using automatic equipment

• Systolic pressure– the highest pressure • Diastolic pressure– the lowest pressure • Pulse pressure – the difference between Systolic and Diastolic pressure.
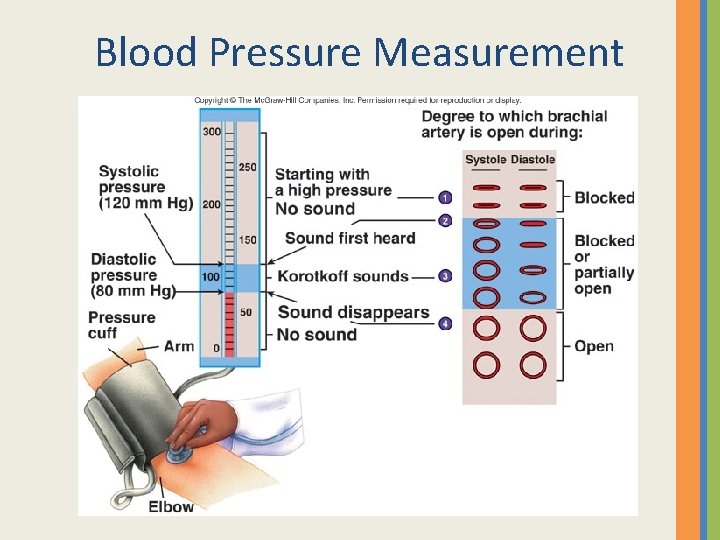
Blood Pressure Measurement

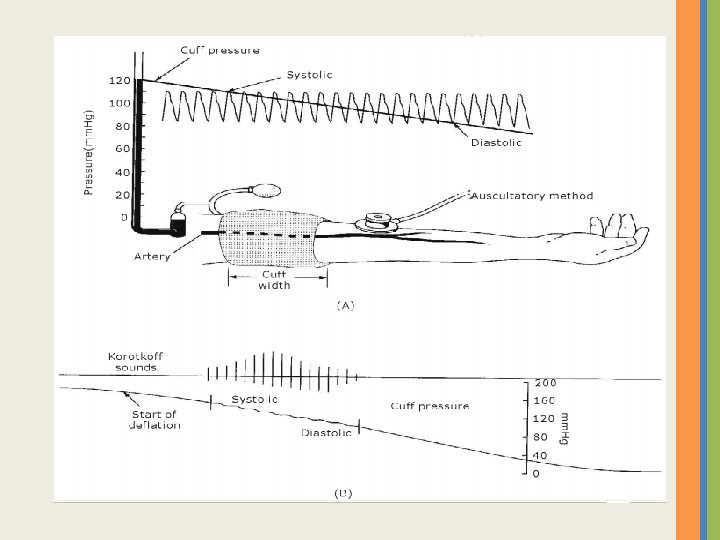
INDIRECT MEASUREMENT OF BLOOD PRESSURE We use a uscultatory method with an inflatable cuff and manometer we call a sphygmomanometer. We place the stethoscope over the brachial artery and inflate the cuff until it is well above systolic pressure then lower slowly
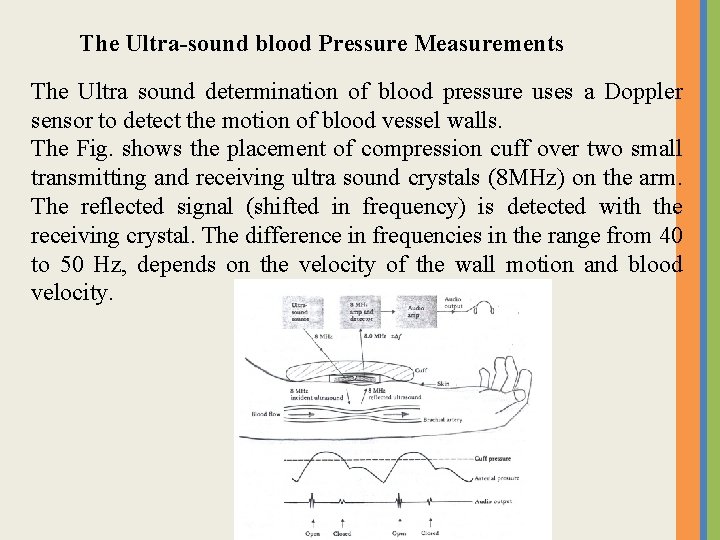
The Ultra-sound blood Pressure Measurements The Ultra sound determination of blood pressure uses a Doppler sensor to detect the motion of blood vessel walls. The Fig. shows the placement of compression cuff over two small transmitting and receiving ultra sound crystals (8 MHz) on the arm. The reflected signal (shifted in frequency) is detected with the receiving crystal. The difference in frequencies in the range from 40 to 50 Hz, depends on the velocity of the wall motion and blood velocity.

• As the cuff pressure increased above the diastolic pressure (80 mm. Hg) but below the systolic pressure, the vessel opens and close with each heart beat, the opening and closing of vessel are detected by ultra sound system. • As pressured increased as shown in Fig. the time between the opening and closing decreases until they coincide. The reading at this point in the manometer or dial gauge is the systolic pressure. • Conversely, when the pressure in the cuff is reduced, the time between opening and closing increases until the closing signal on pulse coincide with opening signal of the next one. The reading in this case is the diastolic pressure. • The advantages of the Ultra sound method • can be used with infants • can be used in high noise environment
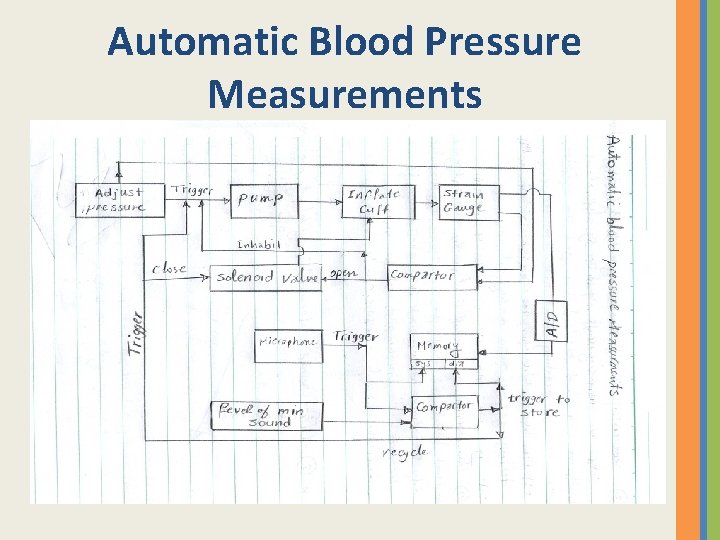
Automatic Blood Pressure Measurements

Automatic Blood Pressure Measurements 1 - The user adjusts the pressure of the system (by touching digital bottoms) this expected pressure above the expected systolic pressure 2 - The pump triggers and gives a pressure to the cuff 3 - The cuff pressure is measured using strain gauge system (calibrated) 4 - The adjusted pressure from step 1 and the measured pressure by strain gauge and applied by the pump (step 2) are compared through a comparator 5 - When the values of 2 pressures are equal, the comparator works in 2 ways (a) Give signal to stop the pump (b) Give signal to solenoid valve to start to release the cuff pressure gradually

6 - The pressure is always measured by the strain gauges and recorded all the time using a memory system 7 - The microphone (which placed under the cuff) detect the first sound when the cuff pressure equal the systolic pressure. This will trigger the memory and then store s the systolic value 8 - The output of microphone is connected with a comparator with a minimum level of sound can be recorded 9 - When the pressure reaches to the diastolic pressure the microphone output sound reaches to the value of minimum level of sound, then the comparator works and gives a signal to the memory to record the value of diastolic pressure , , also it gives a signal to repeat the process again (a) Close the solenoid (b) Trigger the pump to be ready to work again
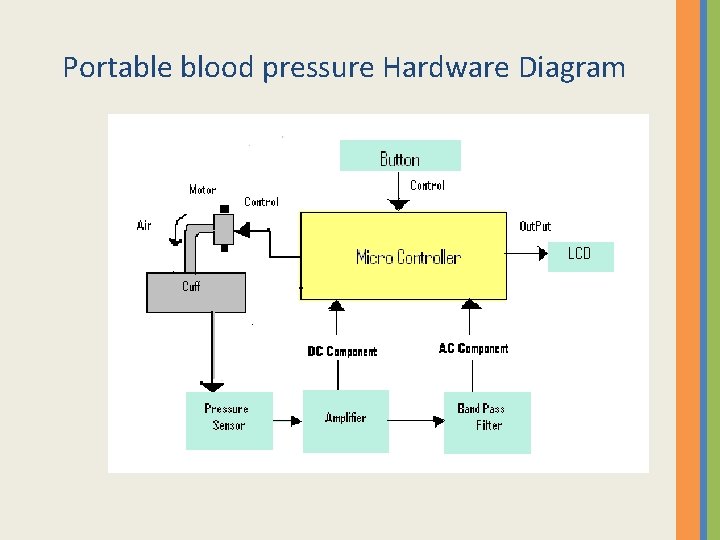
Portable blood pressure Hardware Diagram
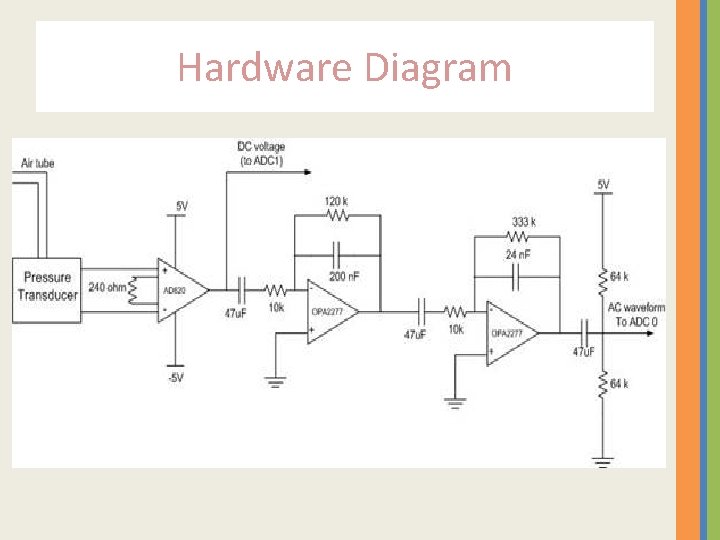
Hardware Diagram

NOTES • The output voltage of the pressure sensor will be proportional to the difference between the pressure in the cuff and the air pressure in the room. • The output voltage from the pressure sensor is very small (in m. V), so we used a DC Amplifier (AD 620) that amplifies according this equation RG=49. 4 KOhm/(G-1).

NOTES • We used a Band-Pass filter to red of the DC voltage and amplify the AC voltage. • We used an AC coupling stage to provide the DC bias level. Given this bias level, it is easier for us to process the AC signal using the on-chip ADC in the microcontroller.
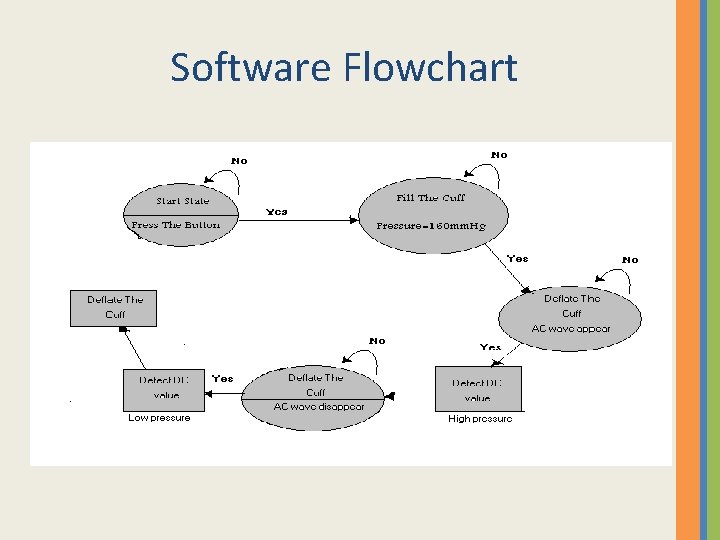
Software Flowchart
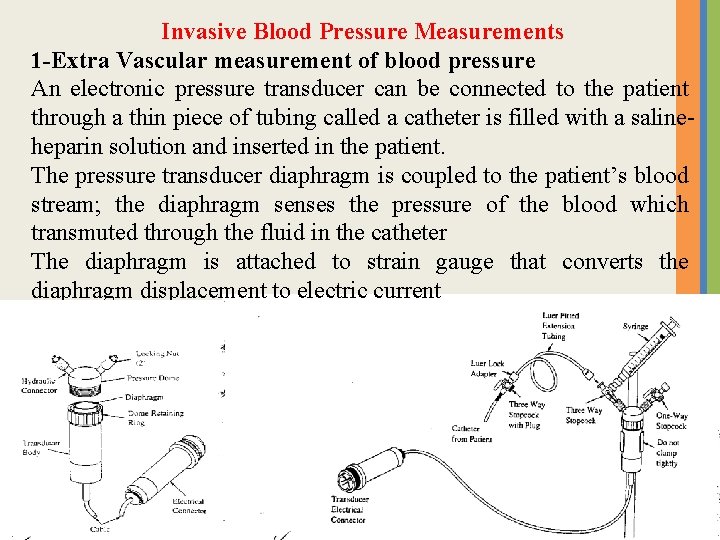
Invasive Blood Pressure Measurements 1 -Extra Vascular measurement of blood pressure An electronic pressure transducer can be connected to the patient through a thin piece of tubing called a catheter is filled with a salineheparin solution and inserted in the patient. The pressure transducer diaphragm is coupled to the patient’s blood stream; the diaphragm senses the pressure of the blood which transmuted through the fluid in the catheter The diaphragm is attached to strain gauge that converts the diaphragm displacement to electric current

P 23 ID PHYSIOLOGICAL PRESSURE TRANSDUCER

Typical Calibration Method • 1 - zero or balance Is used to adjust the amplifier output to zero volt under zero pressure condition • 2 - sensitivity or gain Adjust the gain of the amplifier to produce the correct amplifier output voltage to represent a specific calibration pressure • 3 - calibrate or a control yielding some specific pressure in mm. Hg (the best accuracy method)

Pressure Amplifier Designs • • 1 - DC amplifier 2 - Isolated DC 3 - Pulsed Excitation 4 - AC Carrier
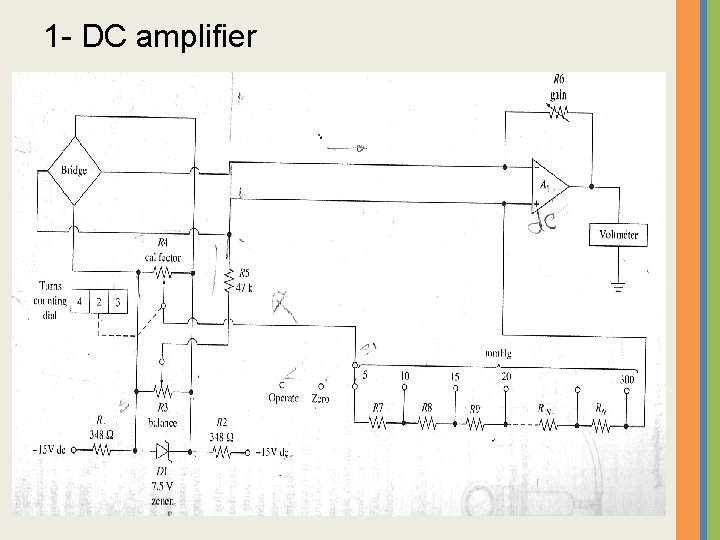
1 - DC amplifier

• A 1 is a dc amplifier • Pressure transducer is a resistive Wheatstone bridge strain gage • Diode d 1 provide the 7. 5 vdc excitation to the transducer& the potentials for the balance and call factor controls

DC Amplifier Calibration 1 - set switch s 1 to operate position, open the transducer stopcock to atmosphere & adjust R 3 for zero volts output
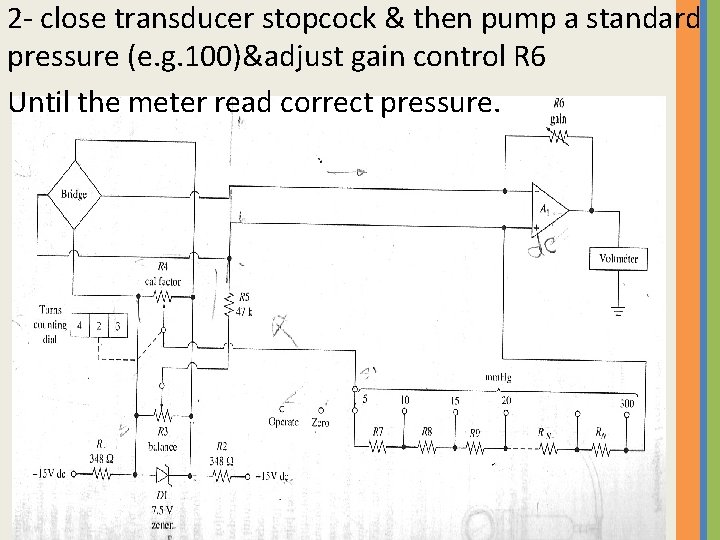
2 - close transducer stopcock & then pump a standard pressure (e. g. 100)&adjust gain control R 6 Until the meter read correct pressure.
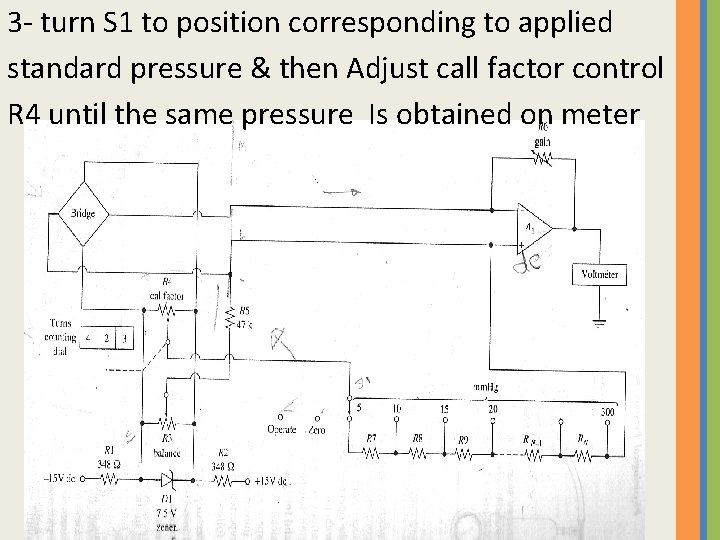
3 - turn S 1 to position corresponding to applied standard pressure & then Adjust call factor control R 4 until the same pressure Is obtained on meter
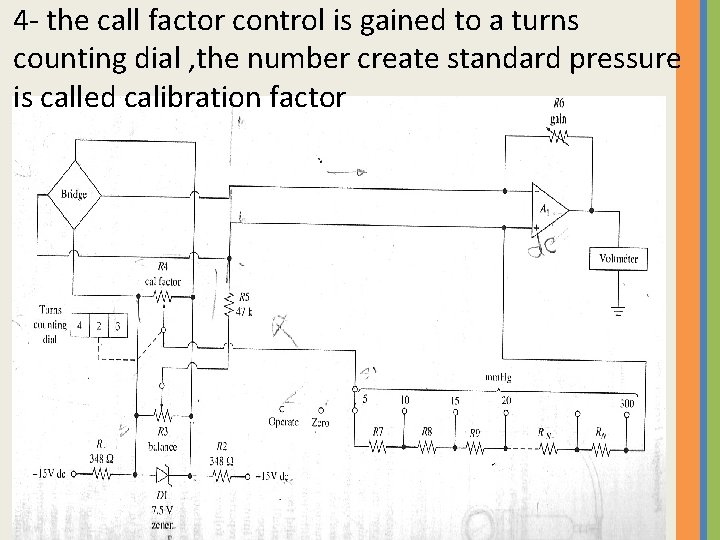
4 - the call factor control is gained to a turns counting dial , the number create standard pressure is called calibration factor
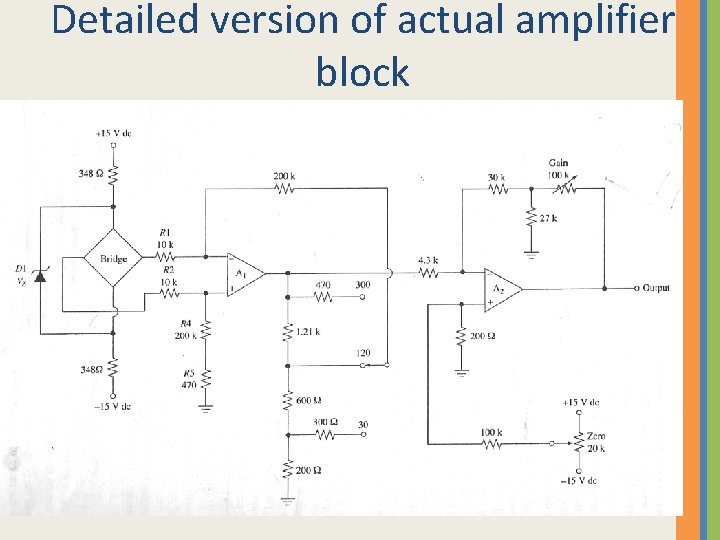
Detailed version of actual amplifier block
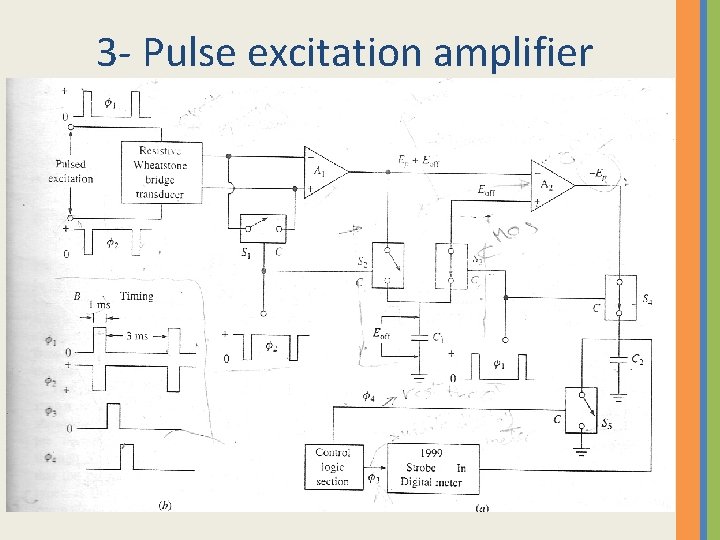
3 - Pulse excitation amplifier
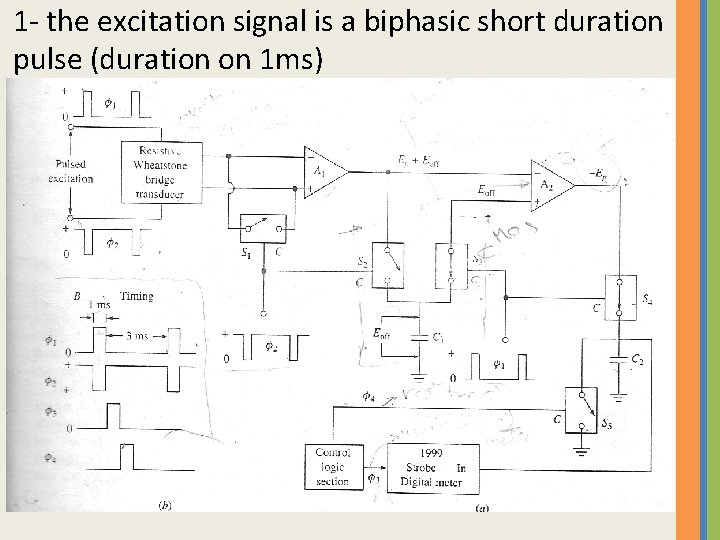
1 - the excitation signal is a biphasic short duration pulse (duration on 1 ms)
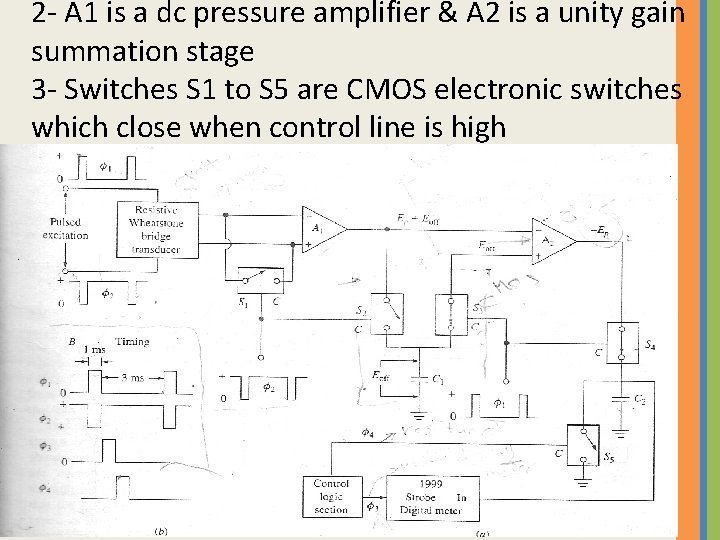
2 - A 1 is a dc pressure amplifier & A 2 is a unity gain summation stage 3 - Switches S 1 to S 5 are CMOS electronic switches which close when control line is high
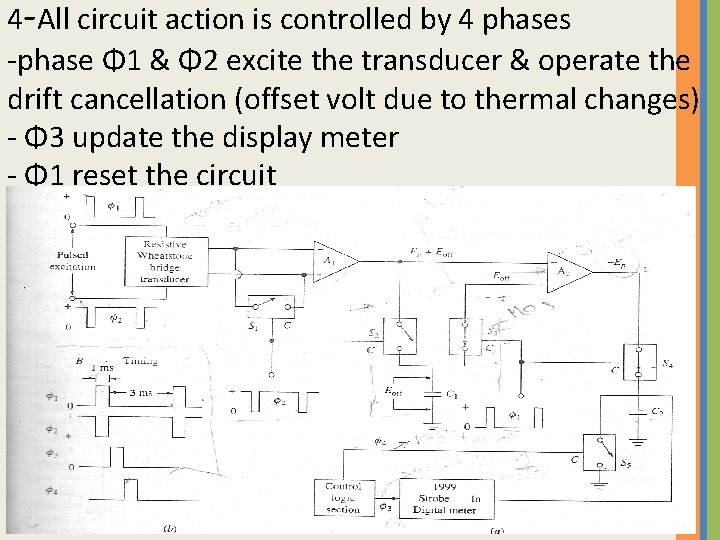
4 -All circuit action is controlled by 4 phases -phase Φ 1 & Φ 2 excite the transducer & operate the drift cancellation (offset volt due to thermal changes) - Φ 3 update the display meter - Φ 1 reset the circuit
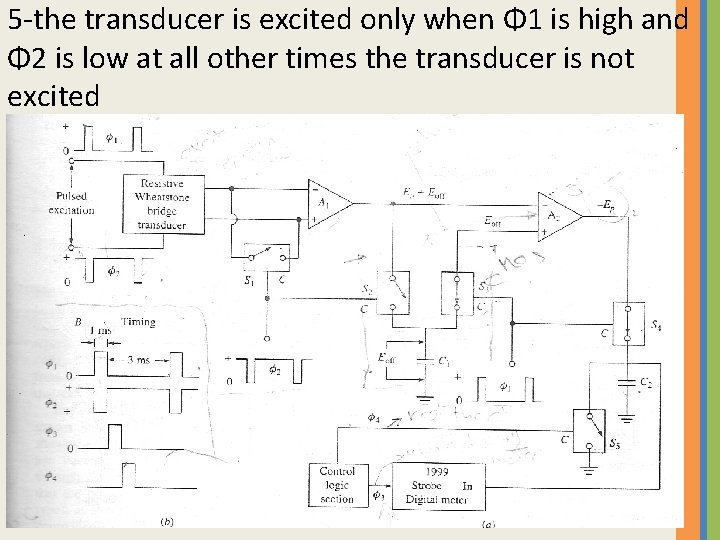
5 -the transducer is excited only when Φ 1 is high and Φ 2 is low at all other times the transducer is not excited
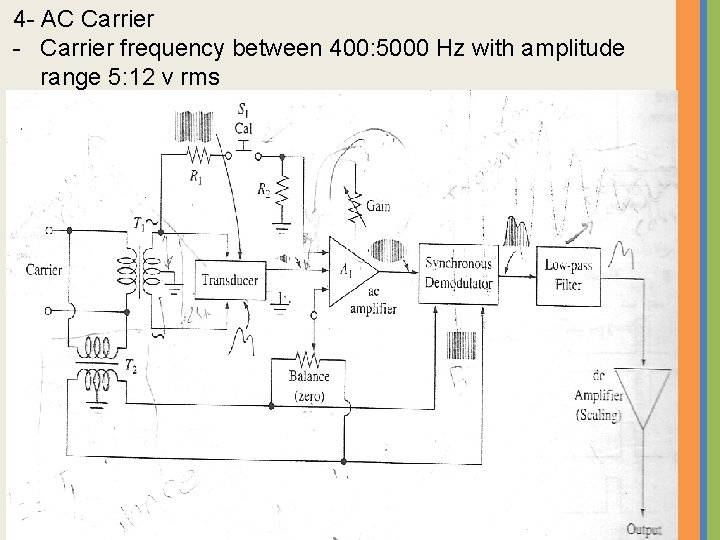
4 - AC Carrier - Carrier frequency between 400: 5000 Hz with amplitude range 5: 12 v rms
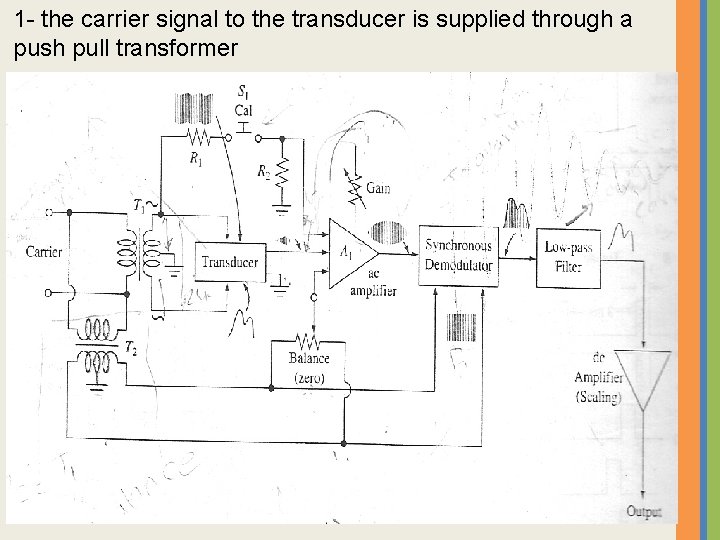
1 - the carrier signal to the transducer is supplied through a push pull transformer
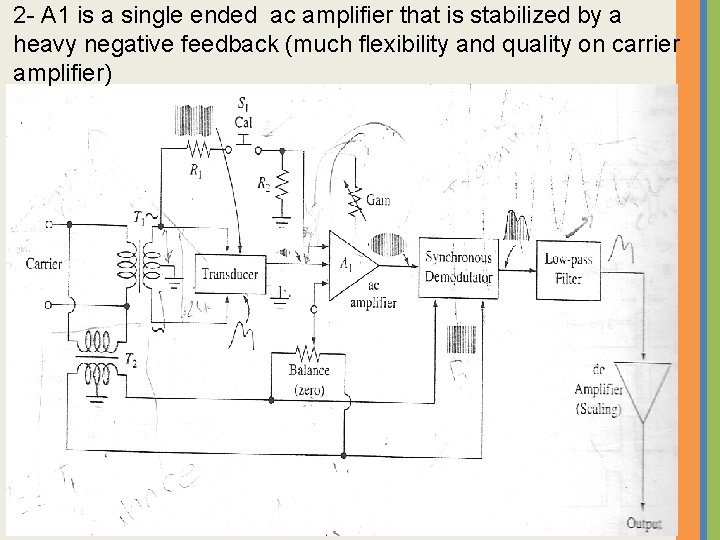
2 - A 1 is a single ended ac amplifier that is stabilized by a heavy negative feedback (much flexibility and quality on carrier amplifier)
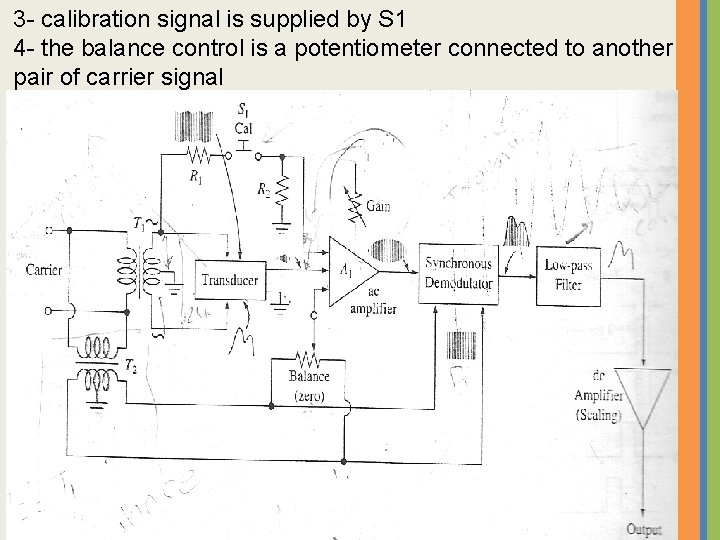
3 - calibration signal is supplied by S 1 4 - the balance control is a potentiometer connected to another pair of carrier signal
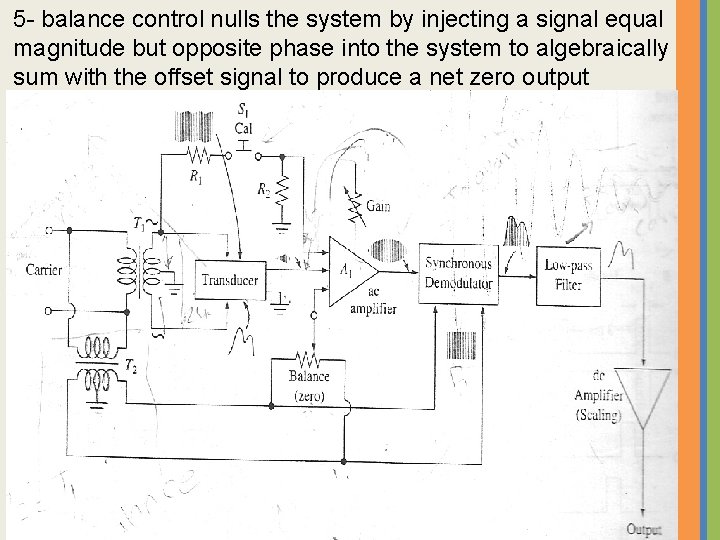
5 - balance control nulls the system by injecting a signal equal magnitude but opposite phase into the system to algebraically sum with the offset signal to produce a net zero output
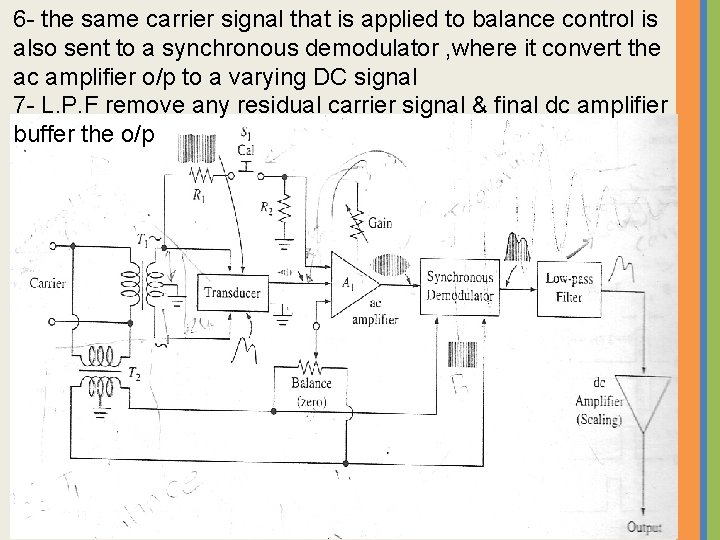
6 - the same carrier signal that is applied to balance control is also sent to a synchronous demodulator , where it convert the ac amplifier o/p to a varying DC signal 7 - L. P. F remove any residual carrier signal & final dc amplifier buffer the o/p
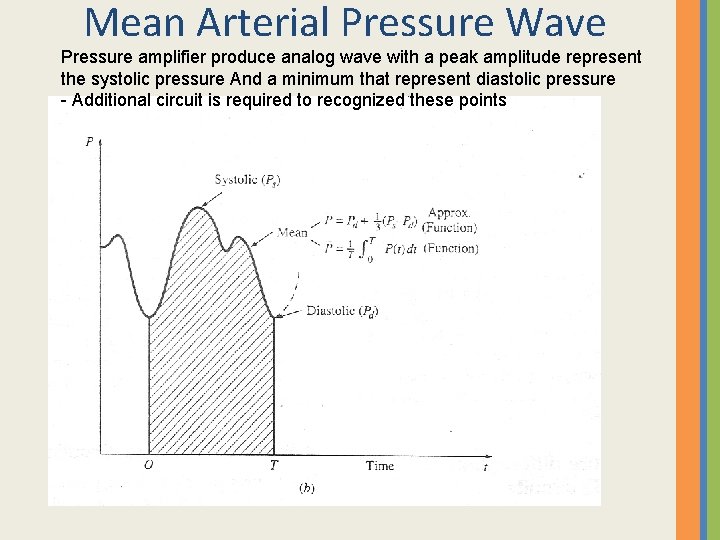
Mean Arterial Pressure Wave Pressure amplifier produce analog wave with a peak amplitude represent the systolic pressure And a minimum that represent diastolic pressure - Additional circuit is required to recognized these points
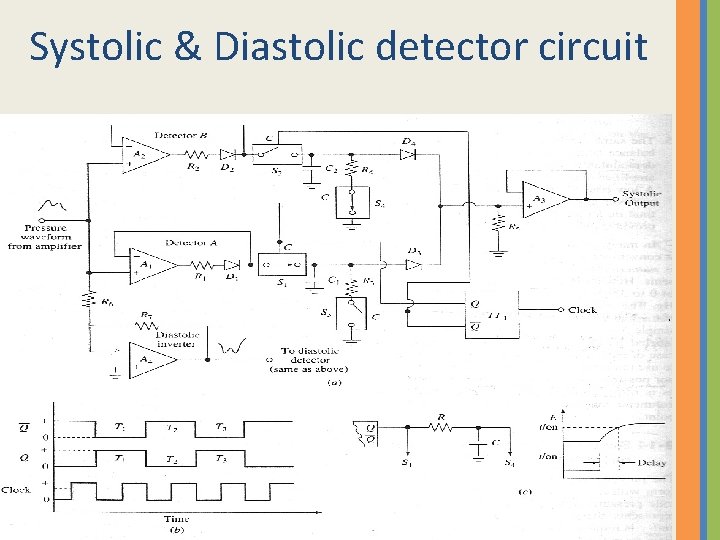
Systolic & Diastolic detector circuit
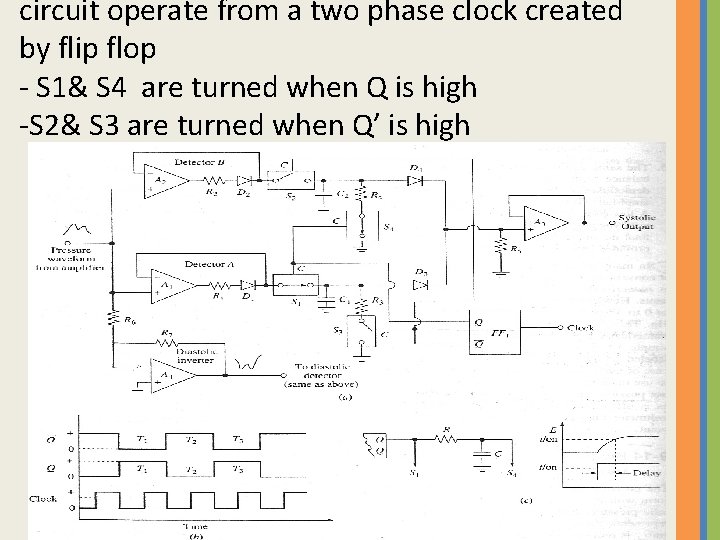
circuit operate from a two phase clock created by flip flop - S 1& S 4 are turned when Q is high -S 2& S 3 are turned when Q’ is high
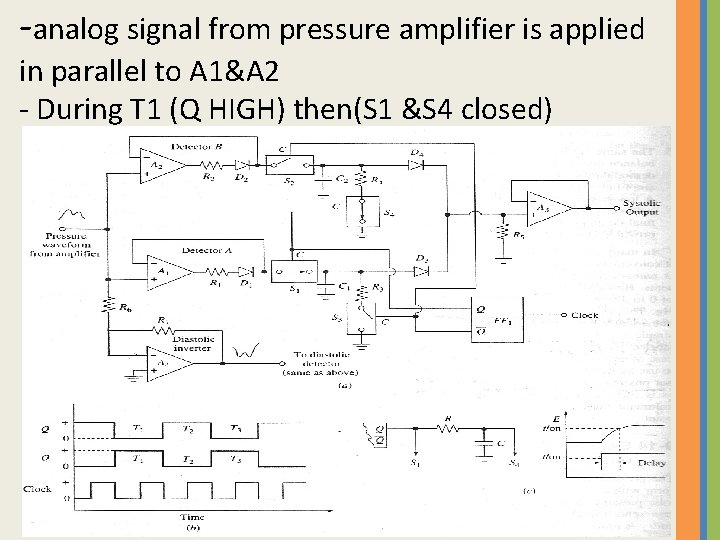
-analog signal from pressure amplifier is applied in parallel to A 1&A 2 - During T 1 (Q HIGH) then(S 1 &S 4 closed)
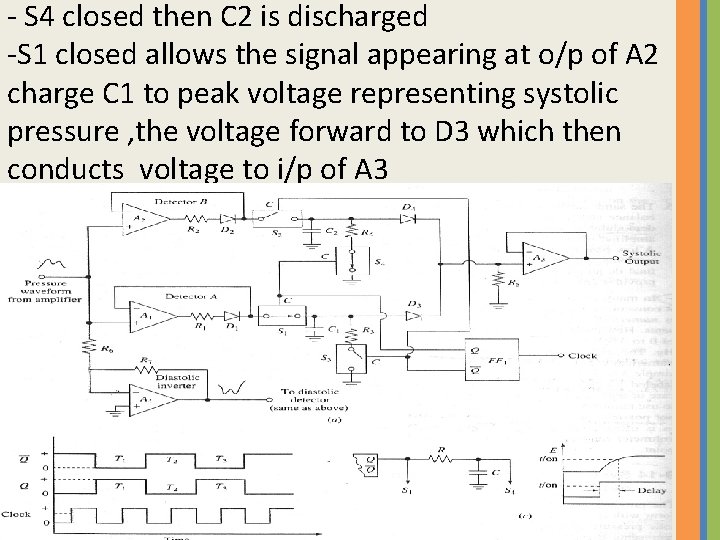
- S 4 closed then C 2 is discharged -S 1 closed allows the signal appearing at o/p of A 2 charge C 1 to peak voltage representing systolic pressure , the voltage forward to D 3 which then conducts voltage to i/p of A 3
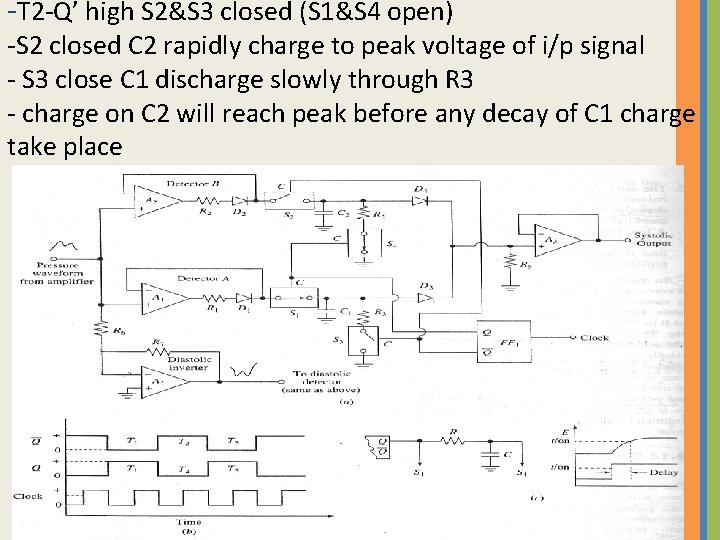
-T 2 -Q’ high S 2&S 3 closed (S 1&S 4 open) -S 2 closed C 2 rapidly charge to peak voltage of i/p signal - S 3 close C 1 discharge slowly through R 3 - charge on C 2 will reach peak before any decay of C 1 charge take place

Questions?
- Slides: 53