ULVYE ATILGANOLU MD Kadky Florence Nightingale Hospital Dermatology

















- Slides: 79

ULVİYE ATILGANOĞLU, MD Kadıköy Florence Nightingale Hospital Dermatology Department TURKEY SKIN MANIFESTATIONS OF SYSTEMIC DISEASE

SKIN The skin should not be considered as an isolated organ. The skin is a functioning system that communicates with the internal environment. The disease of all of the organs may be caused or associated with skin symptoms and signs.

SKIN MANIFESTATIONS of SYSTEMIC DISEASE Some of them may be a clue of more serious underlying systemic disease Some of them may be the sole expression of asymptomatic systemic disorders Some of them may be the initial presentation of systemic disease/malignancy Some of them may be the marker of systemic disease Some of them may be due to treatment

SKIN MANIFESTATIONS of SYSTEMIC DISEASE This session highlights the more common classical and important manifestations in three different groups ? When to look further ? What to look for ? What not to miss

SKIN MANIFESTATIONS of SYSTEMIC DISEASE When to look further: Where dermatologic presentations require further assessment to exclude underlying systemic disease, and guide appropriate management

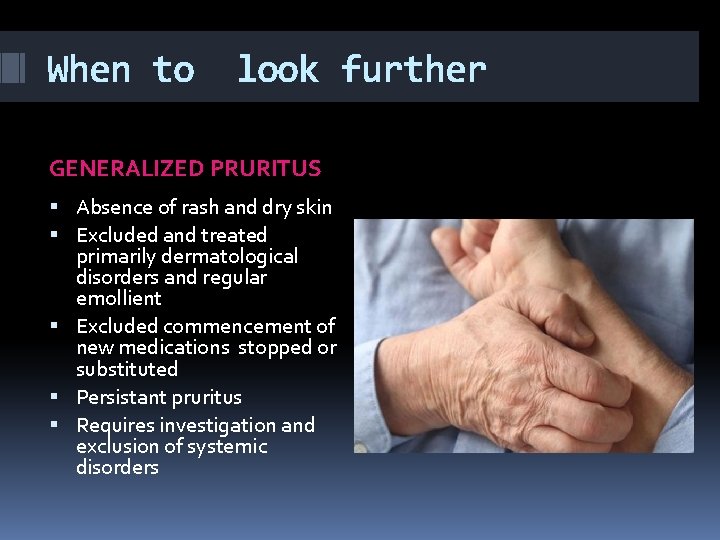
When to look further GENERALIZED PRURITUS Absence of rash and dry skin Excluded and treated primarily dermatological disorders and regular emollient Excluded commencement of new medications stopped or substituted Persistant pruritus Requires investigation and exclusion of systemic disorders

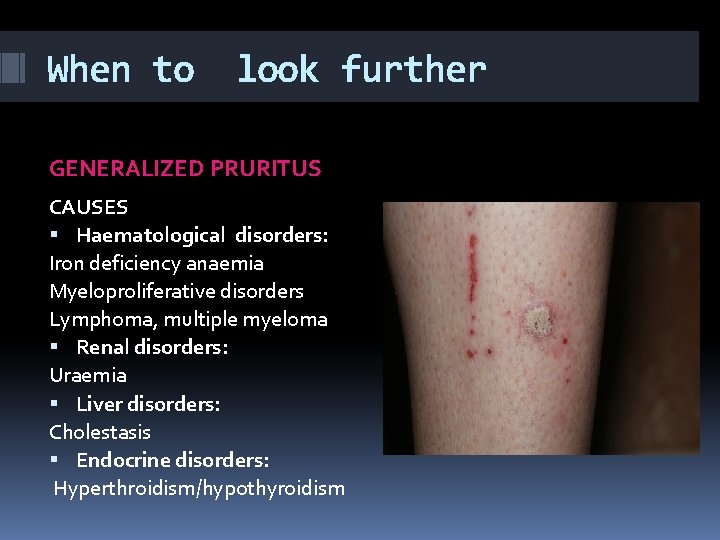
When to look further GENERALIZED PRURITUS CAUSES Haematological disorders: Iron deficiency anaemia Myeloproliferative disorders Lymphoma, multiple myeloma Renal disorders: Uraemia Liver disorders: Cholestasis Endocrine disorders: Hyperthroidism/hypothyroidism

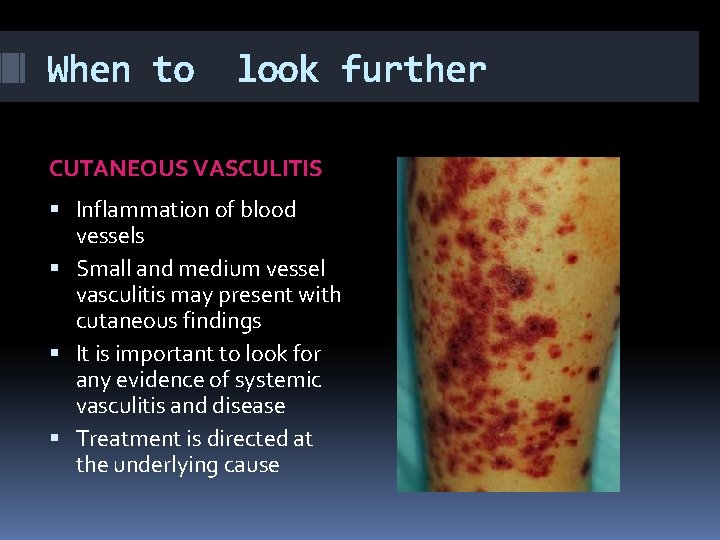
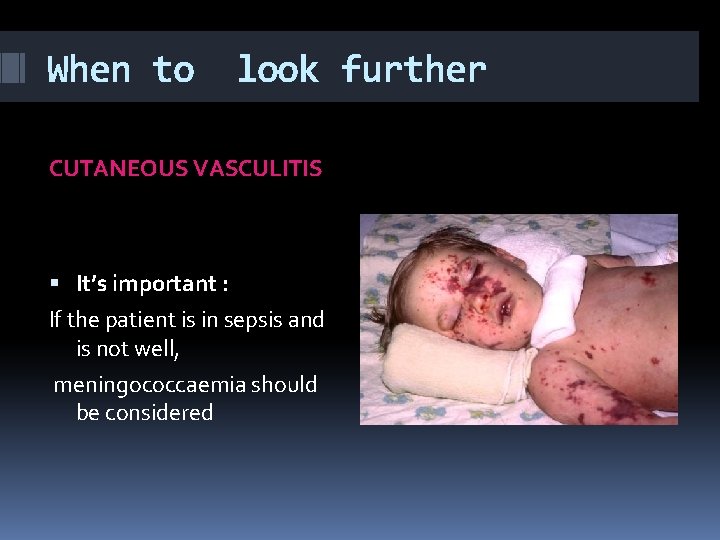
When to look further CUTANEOUS VASCULITIS Inflammation of blood vessels Small and medium vessel vasculitis may present with cutaneous findings It is important to look for any evidence of systemic vasculitis and disease Treatment is directed at the underlying cause

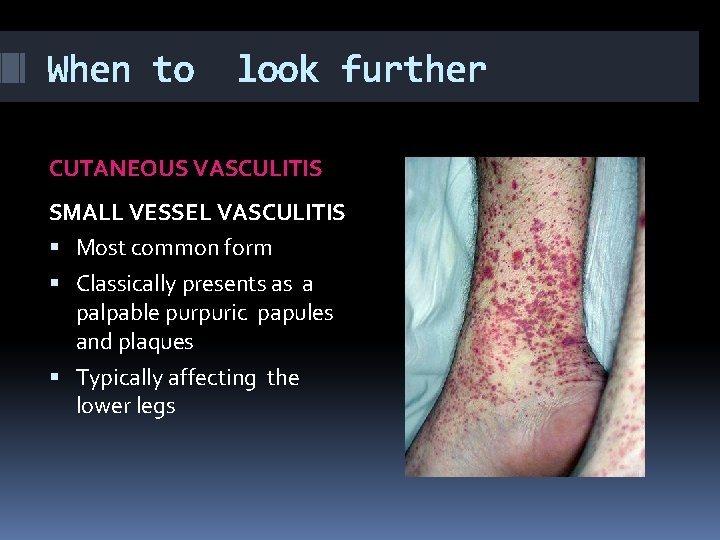
When to look further CUTANEOUS VASCULITIS SMALL VESSEL VASCULITIS Most common form Classically presents as a palpable purpuric papules and plaques Typically affecting the lower legs

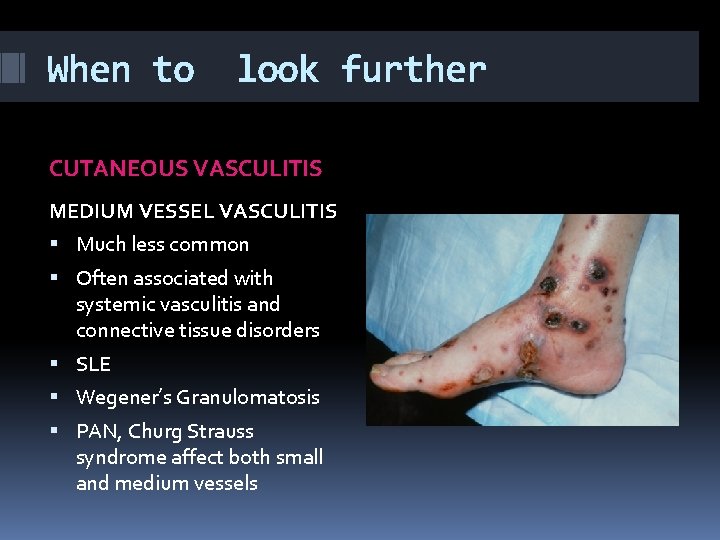
When to look further CUTANEOUS VASCULITIS MEDIUM VESSEL VASCULITIS Much less common Often associated with systemic vasculitis and connective tissue disorders SLE Wegener’s Granulomatosis PAN, Churg Strauss syndrome affect both small and medium vessels

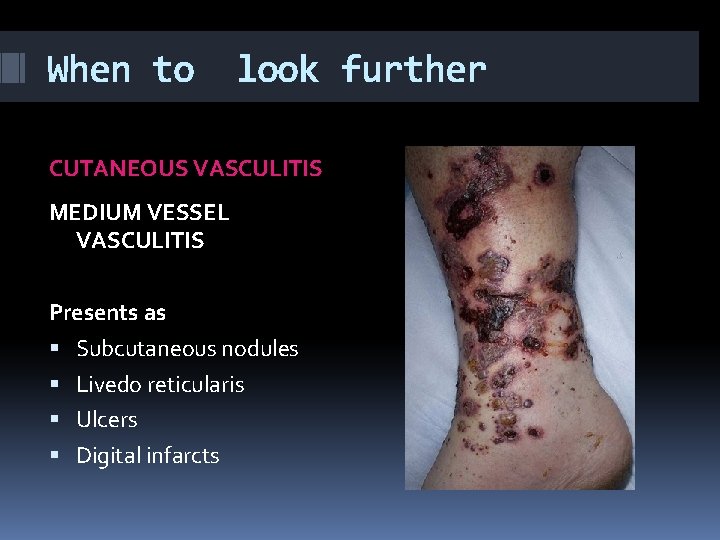
When to look further CUTANEOUS VASCULITIS MEDIUM VESSEL VASCULITIS Presents as Subcutaneous nodules Livedo reticularis Ulcers Digital infarcts

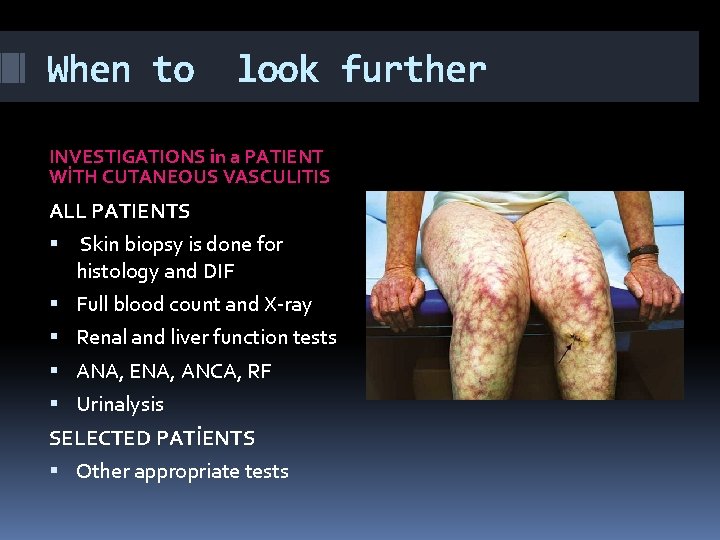
When to look further INVESTIGATIONS in a PATIENT WİTH CUTANEOUS VASCULITIS ALL PATIENTS Skin biopsy is done for histology and DIF Full blood count and X-ray Renal and liver function tests ANA, ENA, ANCA, RF Urinalysis SELECTED PATİENTS Other appropriate tests

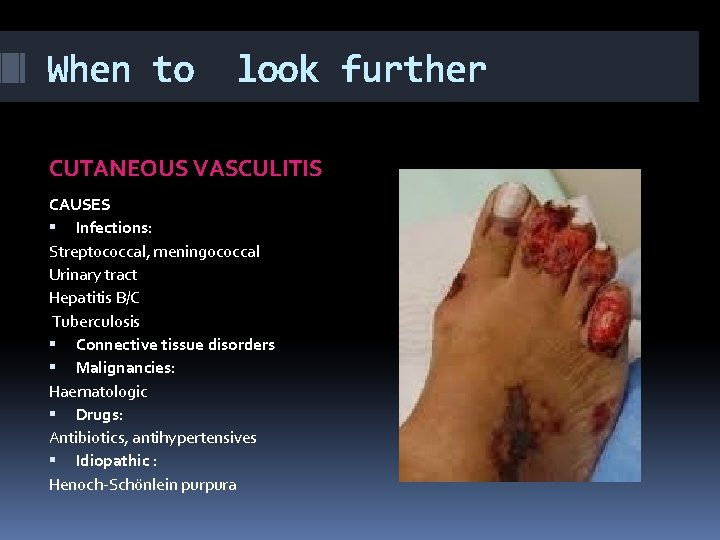
When to look further CUTANEOUS VASCULITIS CAUSES Infections: Streptococcal, meningococcal Urinary tract Hepatitis B/C Tuberculosis Connective tissue disorders Malignancies: Haematologic Drugs: Antibiotics, antihypertensives Idiopathic : Henoch-Schönlein purpura

When to look further CUTANEOUS VASCULITIS It’s important : If the patient is in sepsis and is not well, meningococcaemia should be considered

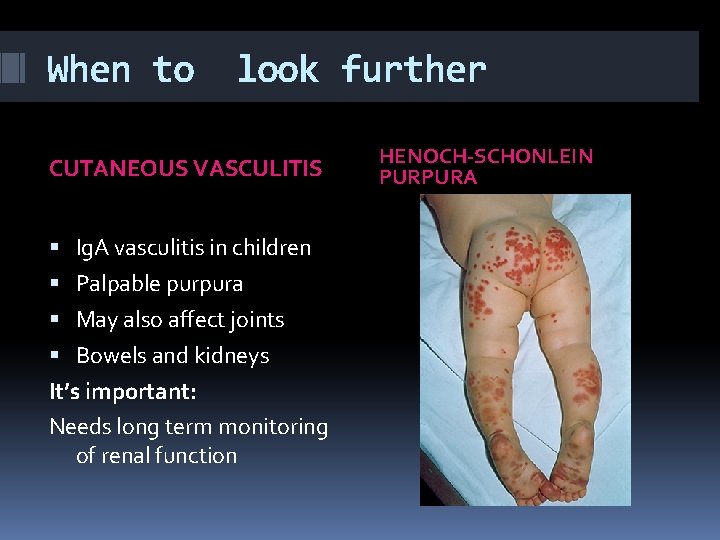
When to look further CUTANEOUS VASCULITIS Ig. A vasculitis in children Palpable purpura May also affect joints Bowels and kidneys It’s important: Needs long term monitoring of renal function HENOCH-SCHONLEIN PURPURA

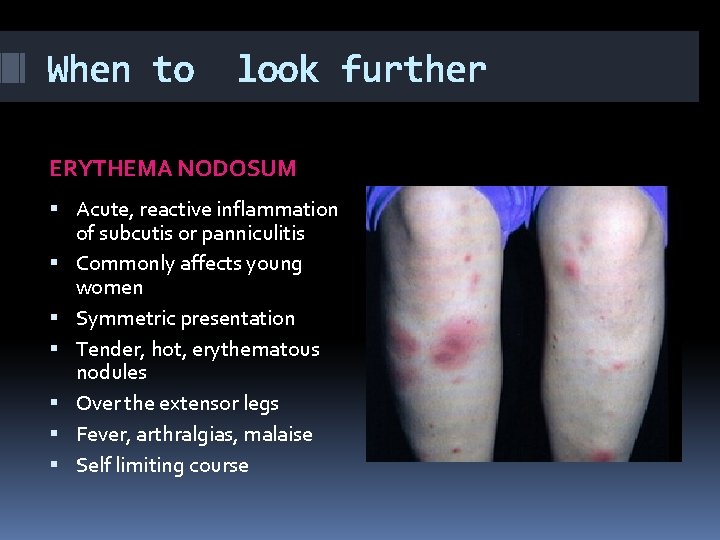
When to look further ERYTHEMA NODOSUM Acute, reactive inflammation of subcutis or panniculitis Commonly affects young women Symmetric presentation Tender, hot, erythematous nodules Over the extensor legs Fever, arthralgias, malaise Self limiting course

When to look further ERYTHEMA NODOSUM CAUSES Infections: Tuberculosis Sarcoidosis Inflammatory bowel disease Malignancy Postradiotherapy Pregnancy Behçet’s disease Drugs

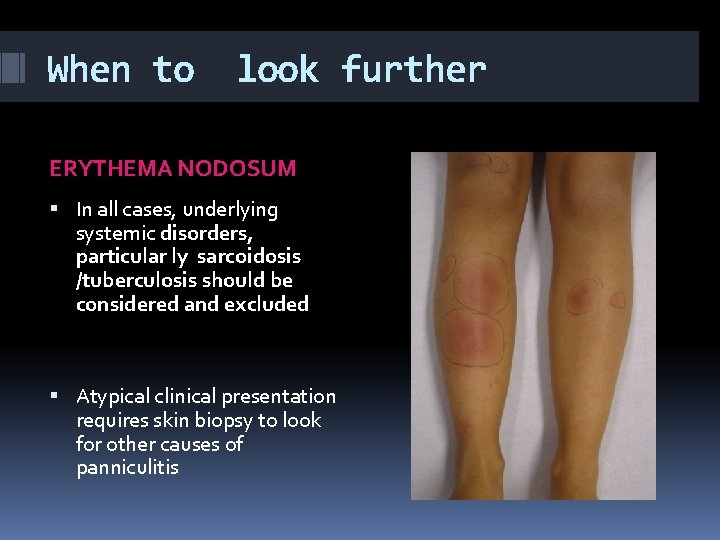
When to look further ERYTHEMA NODOSUM In all cases, underlying systemic disorders, particular ly sarcoidosis /tuberculosis should be considered and excluded Atypical clinical presentation requires skin biopsy to look for other causes of panniculitis

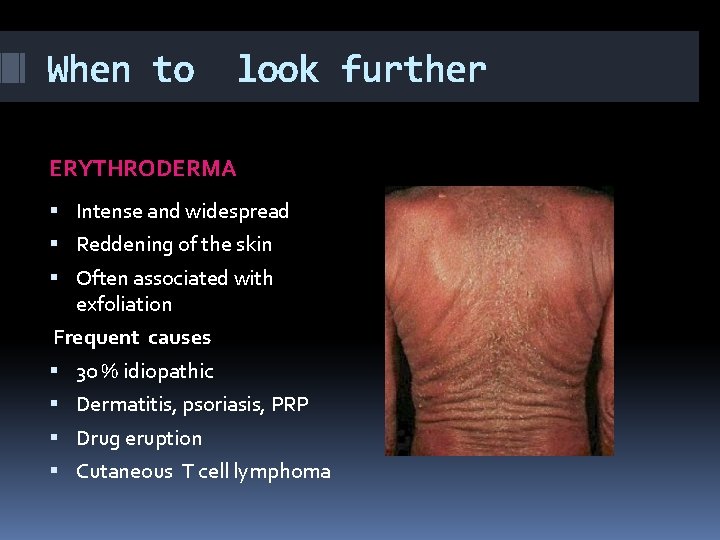
When to look further ERYTHRODERMA Intense and widespread Reddening of the skin Often associated with exfoliation Frequent causes 30 % idiopathic Dermatitis, psoriasis, PRP Drug eruption Cutaneous T cell lymphoma

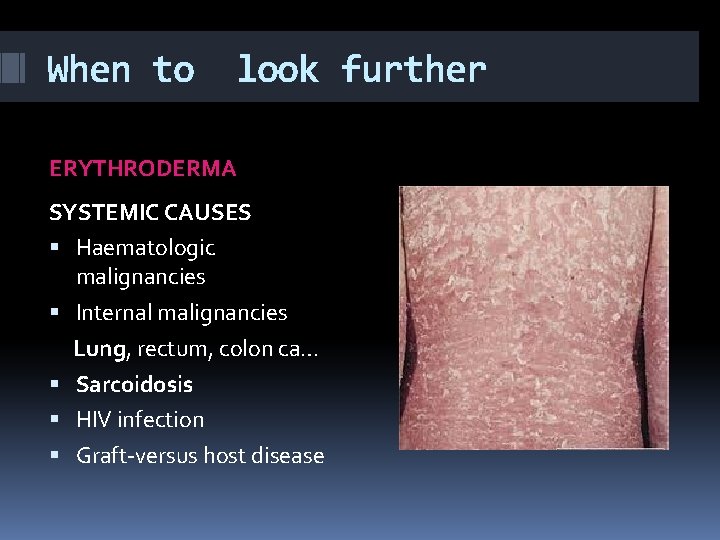
When to look further ERYTHRODERMA SYSTEMIC CAUSES Haematologic malignancies Internal malignancies Lung, rectum, colon ca… Sarcoidosis HIV infection Graft-versus host disease

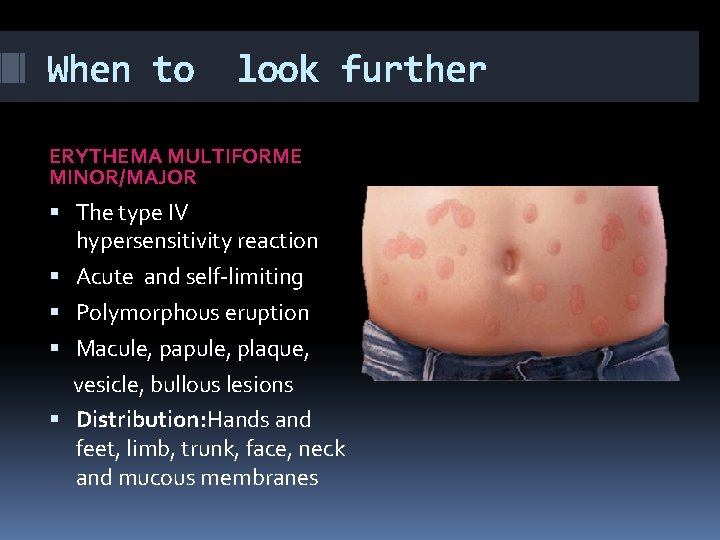
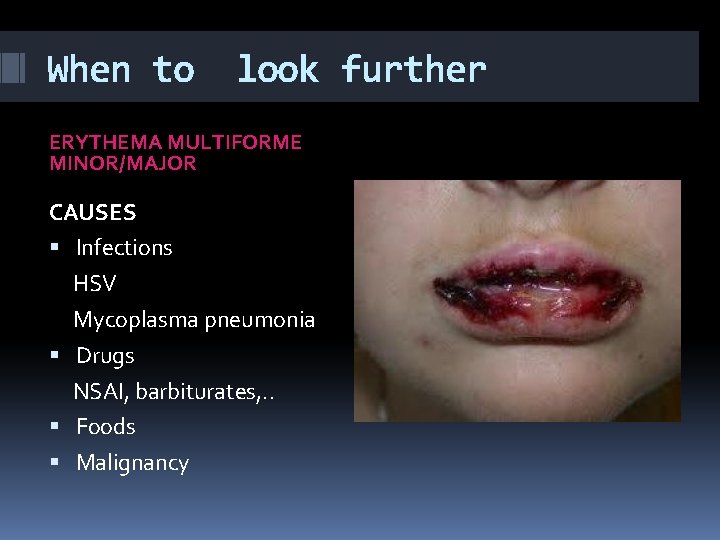
When to look further ERYTHEMA MULTIFORME MINOR/MAJOR The type IV hypersensitivity reaction Acute and self-limiting Polymorphous eruption Macule, papule, plaque, vesicle, bullous lesions Distribution: Hands and feet, limb, trunk, face, neck and mucous membranes

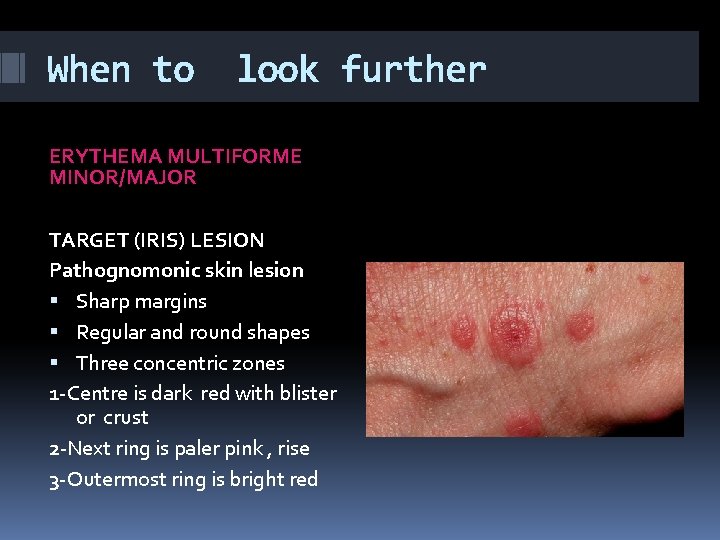
When to look further ERYTHEMA MULTIFORME MINOR/MAJOR TARGET (IRIS) LESION Pathognomonic skin lesion Sharp margins Regular and round shapes Three concentric zones 1 -Centre is dark red with blister or crust 2 -Next ring is paler pink , rise 3 -Outermost ring is bright red

When to look further ERYTHEMA MULTIFORME MINOR/MAJOR CAUSES Infections HSV Mycoplasma pneumonia Drugs NSAI, barbiturates, . . Foods Malignancy

What to look for Certain systemic diseases that have classic cutaneous findings Usually skin biopsy confirms the diagnosis Systemic involvement must be investigated

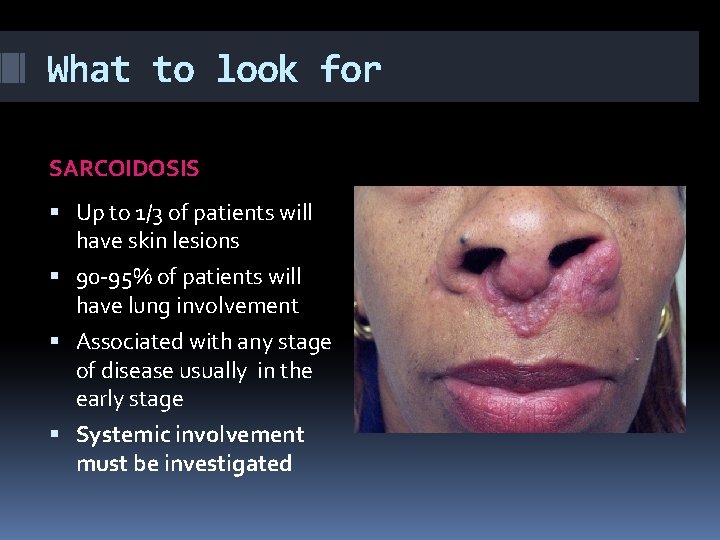
What to look for SARCOIDOSIS Up to 1/3 of patients will have skin lesions 90 -95% of patients will have lung involvement Associated with any stage of disease usually in the early stage Systemic involvement must be investigated

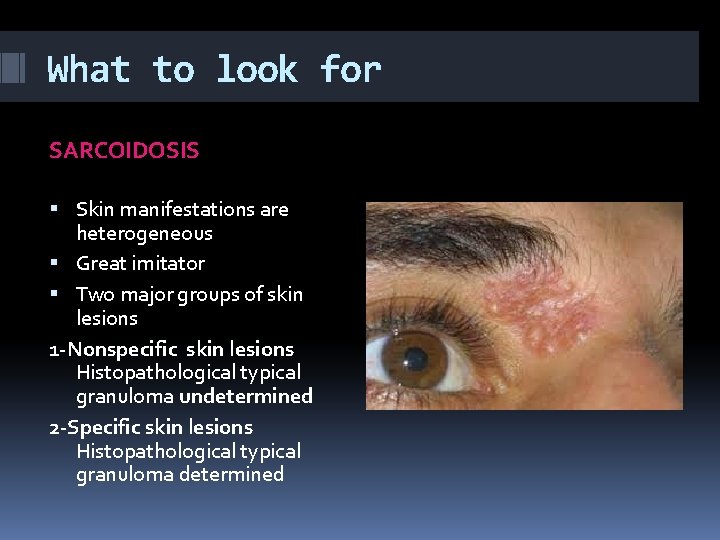
What to look for SARCOIDOSIS Skin manifestations are heterogeneous Great imitator Two major groups of skin lesions 1 -Nonspecific skin lesions Histopathological typical granuloma undetermined 2 -Specific skin lesions Histopathological typical granuloma determined

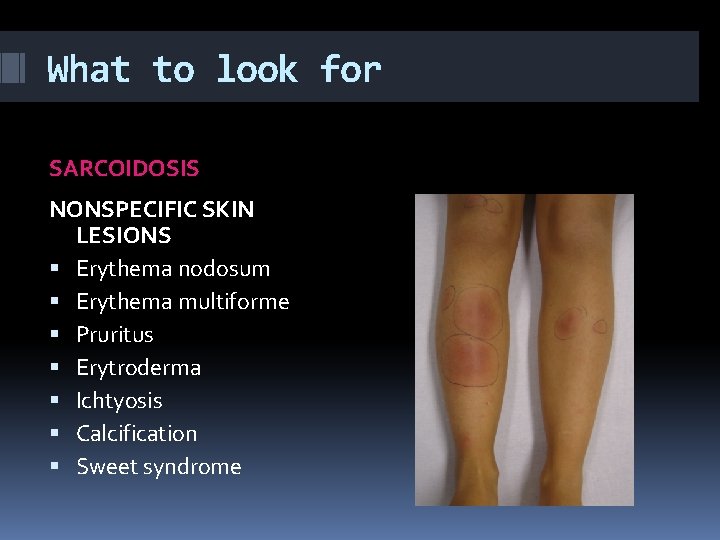
What to look for SARCOIDOSIS NONSPECIFIC SKIN LESIONS Erythema nodosum Erythema multiforme Pruritus Erytroderma Ichtyosis Calcification Sweet syndrome

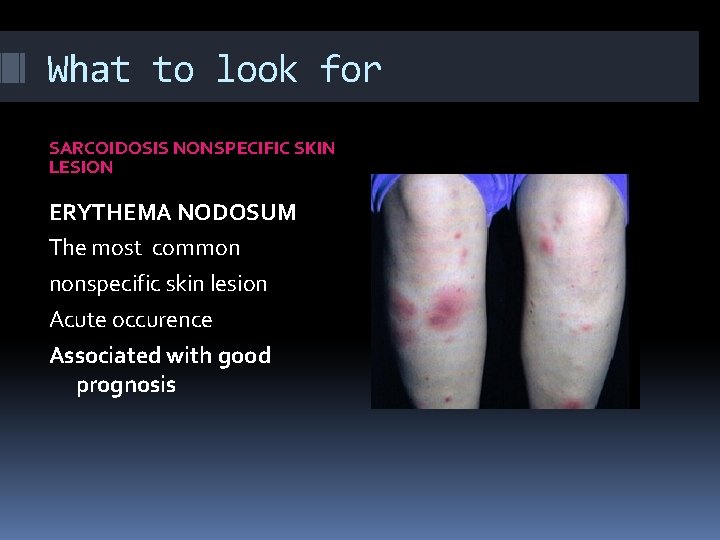
What to look for SARCOIDOSIS NONSPECIFIC SKIN LESION ERYTHEMA NODOSUM The most common nonspecific skin lesion Acute occurence Associated with good prognosis

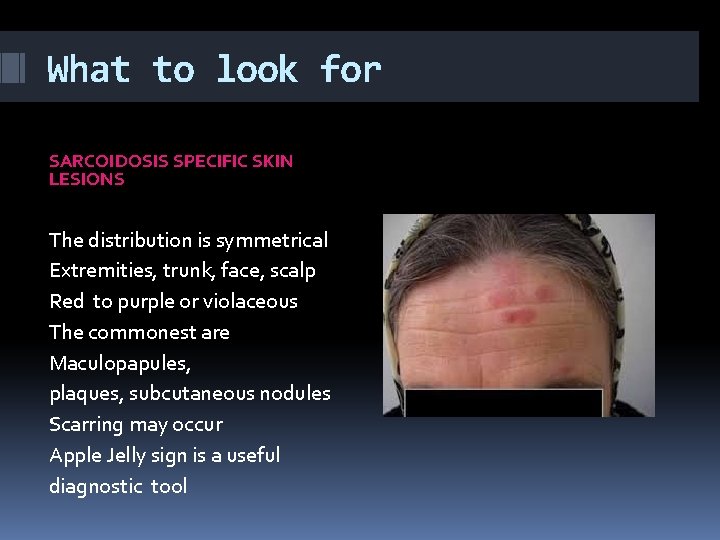
What to look for SARCOIDOSIS SPECIFIC SKIN LESIONS The distribution is symmetrical Extremities, trunk, face, scalp Red to purple or violaceous The commonest are Maculopapules, plaques, subcutaneous nodules Scarring may occur Apple Jelly sign is a useful diagnostic tool

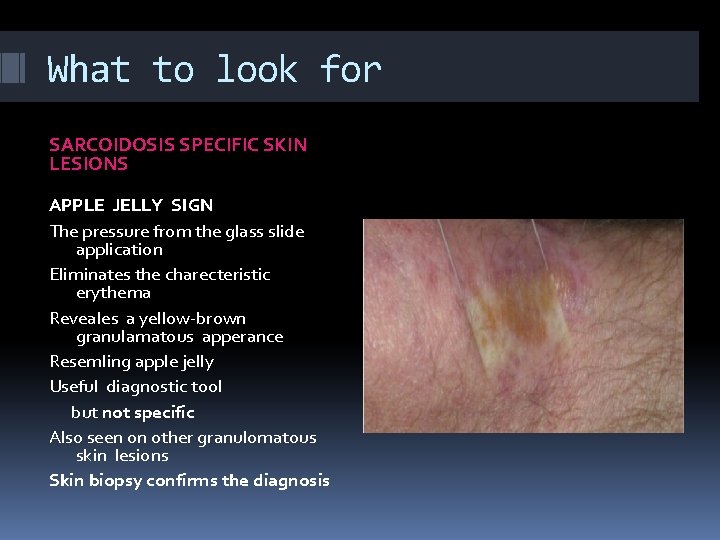
What to look for SARCOIDOSIS SPECIFIC SKIN LESIONS APPLE JELLY SIGN The pressure from the glass slide application Eliminates the charecteristic erythema Reveales a yellow-brown granulamatous apperance Resemling apple jelly Useful diagnostic tool but not specific Also seen on other granulomatous skin lesions Skin biopsy confirms the diagnosis

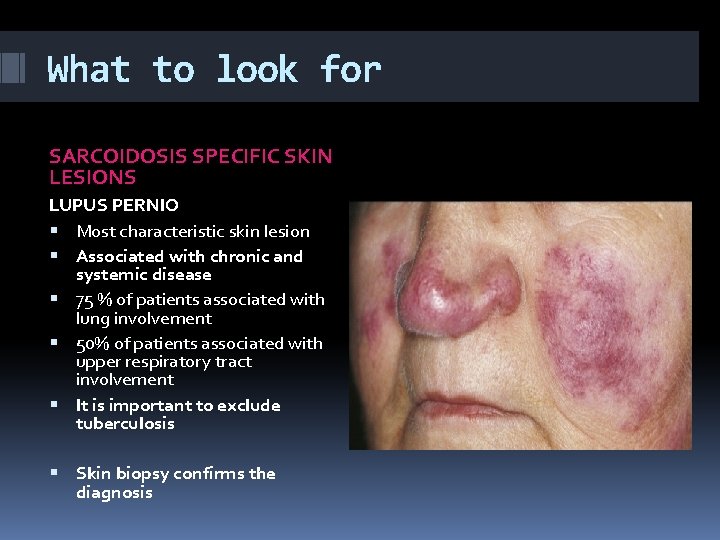
What to look for SARCOIDOSIS SPECIFIC SKIN LESIONS LUPUS PERNIO Most characteristic skin lesion Associated with chronic and systemic disease 75 % of patients associated with lung involvement 50% of patients associated with upper respiratory tract involvement It is important to exclude tuberculosis Skin biopsy confirms the diagnosis

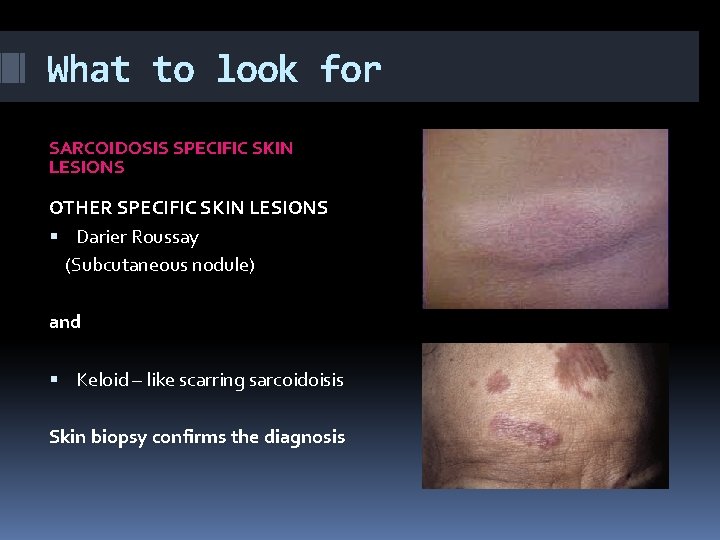
What to look for SARCOIDOSIS SPECIFIC SKIN LESIONS OTHER SPECIFIC SKIN LESIONS Darier Roussay (Subcutaneous nodule) and Keloid – like scarring sarcoidoisis Skin biopsy confirms the diagnosis

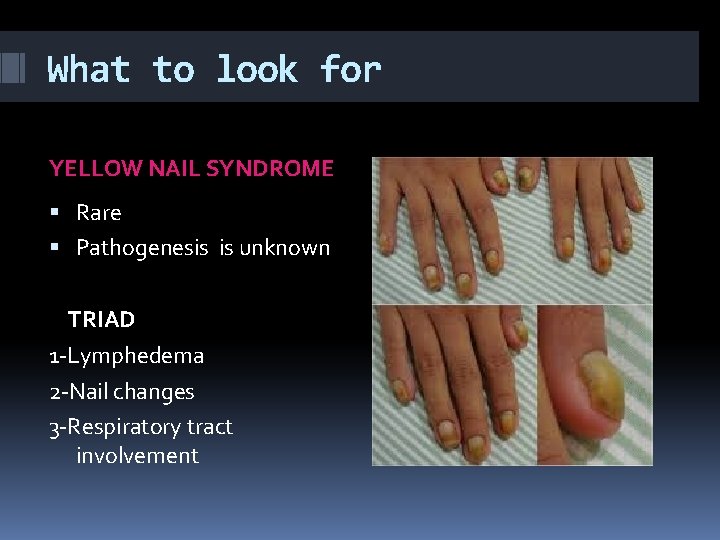
What to look for YELLOW NAIL SYNDROME Rare Pathogenesis is unknown TRIAD 1 -Lymphedema 2 -Nail changes 3 -Respiratory tract involvement

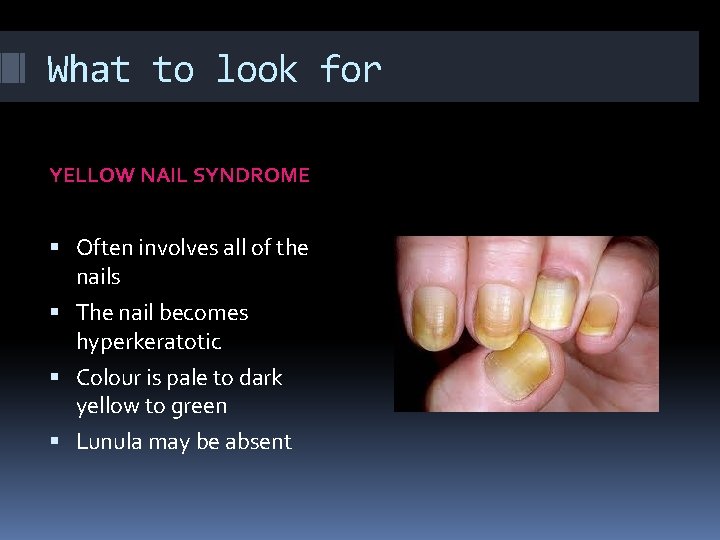
What to look for YELLOW NAIL SYNDROME Often involves all of the nails The nail becomes hyperkeratotic Colour is pale to dark yellow to green Lunula may be absent

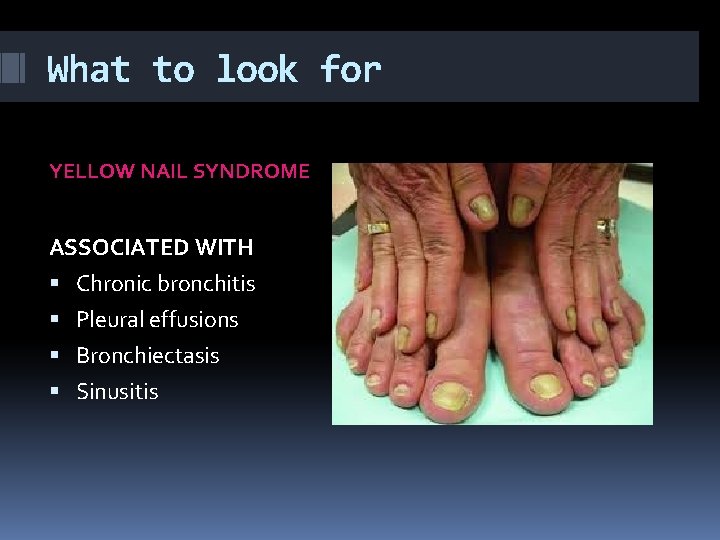
What to look for YELLOW NAIL SYNDROME ASSOCIATED WITH Chronic bronchitis Pleural effusions Bronchiectasis Sinusitis

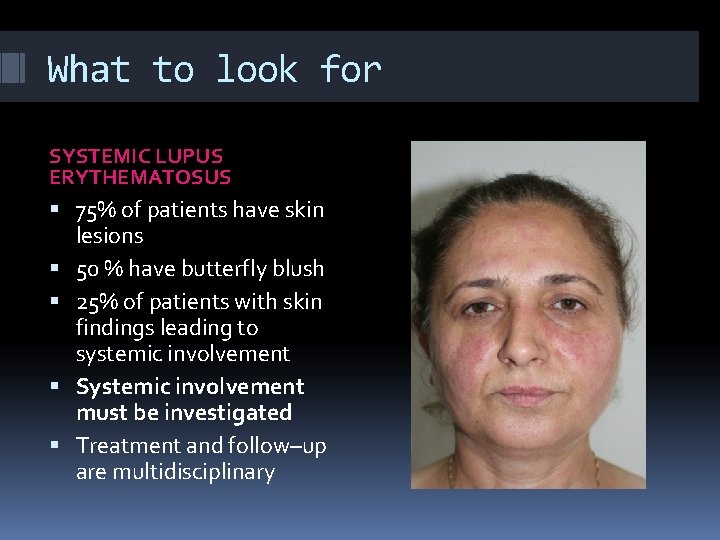
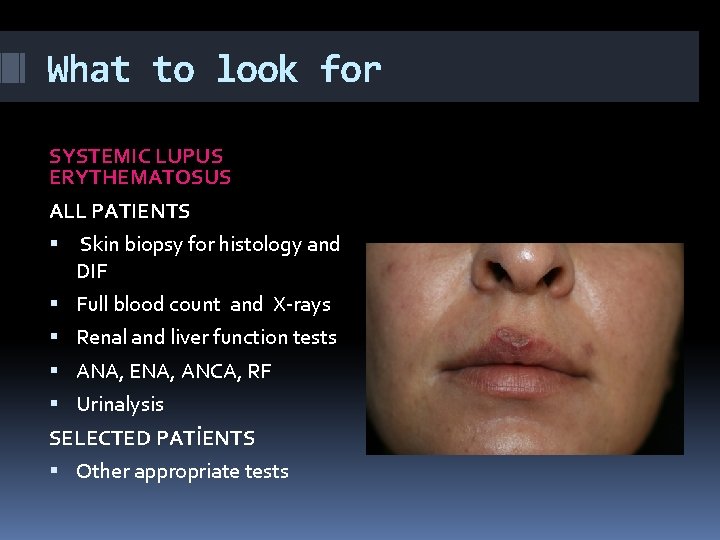
What to look for SYSTEMIC LUPUS ERYTHEMATOSUS 75% of patients have skin lesions 50 % have butterfly blush 25% of patients with skin findings leading to systemic involvement Systemic involvement must be investigated Treatment and follow–up are multidisciplinary

What to look for SYSTEMIC LUPUS ERYTHEMATOSUS COMMON SKIN FINDINGS Butterfly blush(50%) Photosensitivity DLE(chronic discoid lesion)

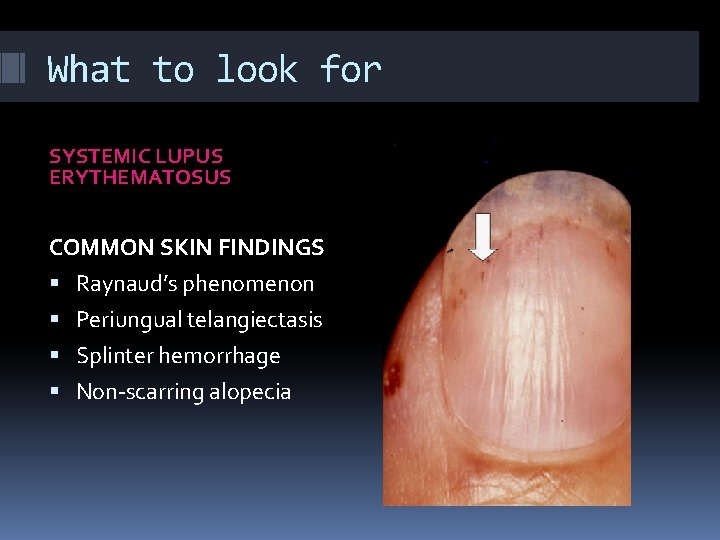
What to look for SYSTEMIC LUPUS ERYTHEMATOSUS COMMON SKIN FINDINGS Raynaud’s phenomenon Periungual telangiectasis Splinter hemorrhage Non-scarring alopecia

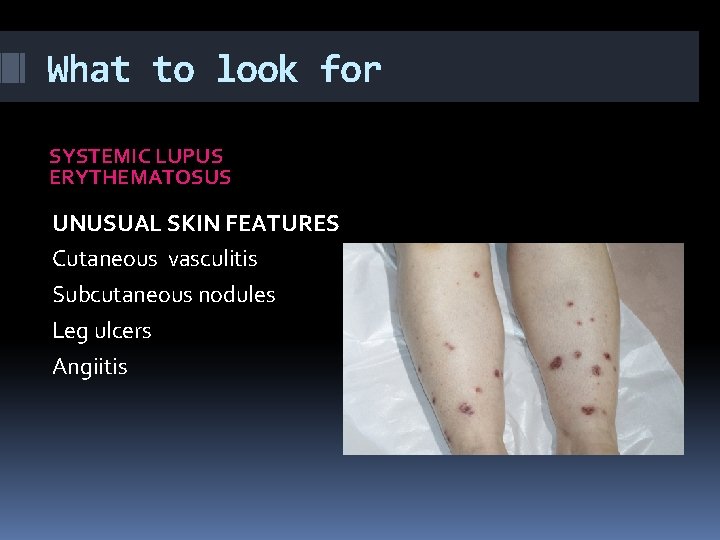
What to look for SYSTEMIC LUPUS ERYTHEMATOSUS UNUSUAL SKIN FEATURES Cutaneous vasculitis Subcutaneous nodules Leg ulcers Angiitis

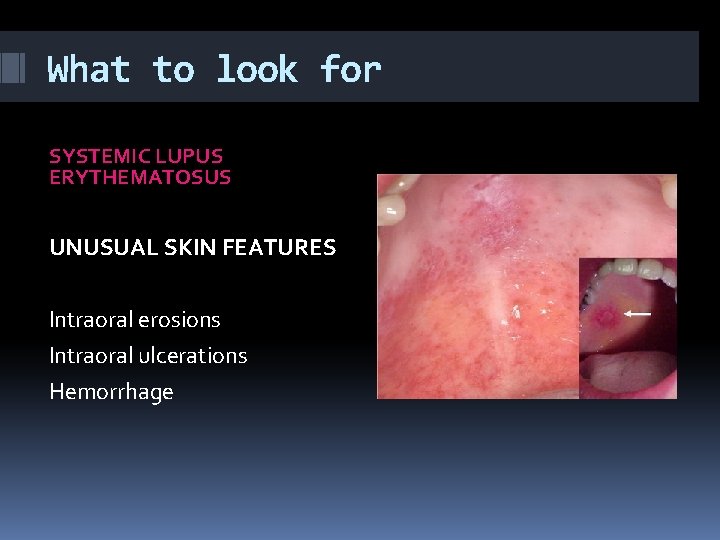
What to look for SYSTEMIC LUPUS ERYTHEMATOSUS UNUSUAL SKIN FEATURES Intraoral erosions Intraoral ulcerations Hemorrhage

What to look for SYSTEMIC LUPUS ERYTHEMATOSUS ALL PATIENTS Skin biopsy for histology and DIF Full blood count and X-rays Renal and liver function tests ANA, ENA, ANCA, RF Urinalysis SELECTED PATİENTS Other appropriate tests

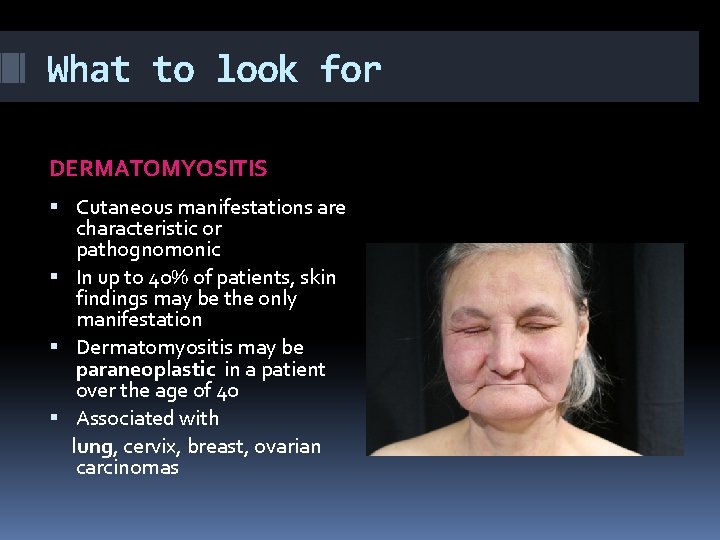
What to look for DERMATOMYOSITIS Cutaneous manifestations are characteristic or pathognomonic In up to 40% of patients, skin findings may be the only manifestation Dermatomyositis may be paraneoplastic in a patient over the age of 40 Associated with lung, cervix, breast, ovarian carcinomas

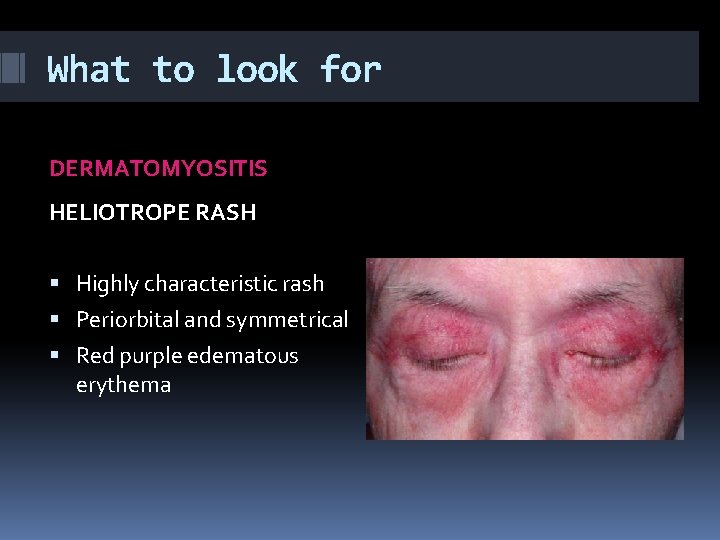
What to look for DERMATOMYOSITIS HELIOTROPE RASH Highly characteristic rash Periorbital and symmetrical Red purple edematous erythema

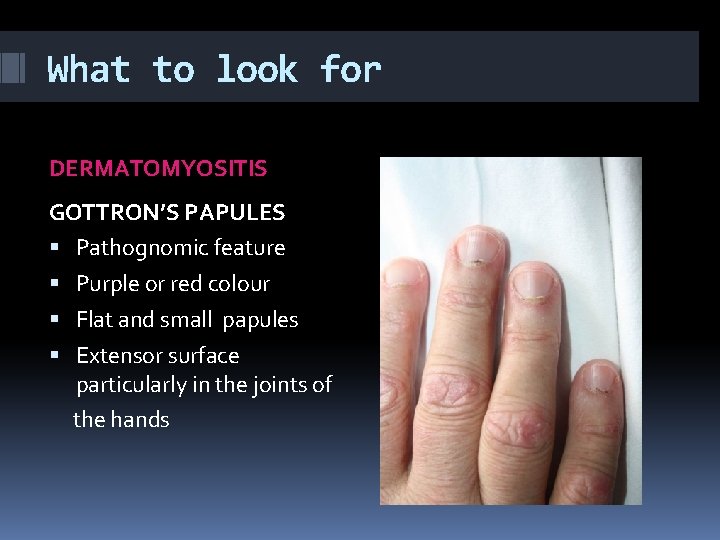
What to look for DERMATOMYOSITIS GOTTRON’S PAPULES Pathognomic feature Purple or red colour Flat and small papules Extensor surface particularly in the joints of the hands

What to look for SCLERODERMA(SYSTEMIC SCLEROSIS) Skin sclerosis is a cardinal feature Skin thickening and shiny areas developing around mouth, nose, face, fingers, hands and bony areas Usually develops first in the fingers and hands

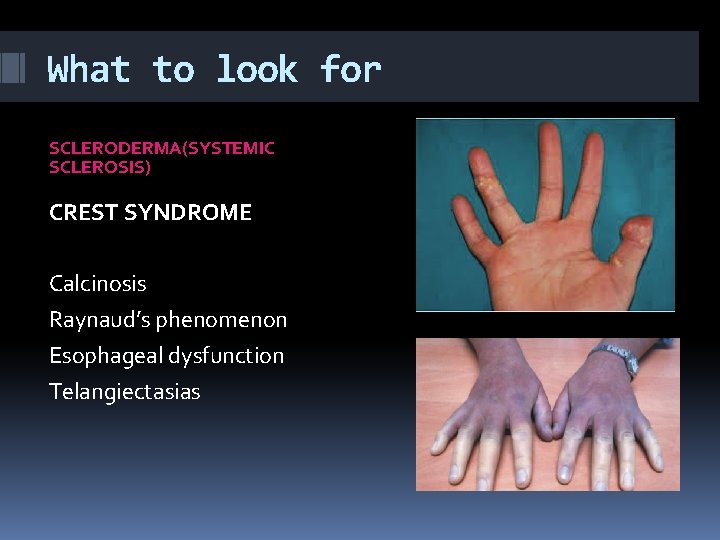
What to look for SCLERODERMA(SYSTEMIC SCLEROSIS) HAND SKIN MANIFESTATIONS Raynaud’s phenomenon Non-pitting oedema Thicken and disabling sclerosis Sclerodactyly Painful digital ulcers Gangrene, autoamputation

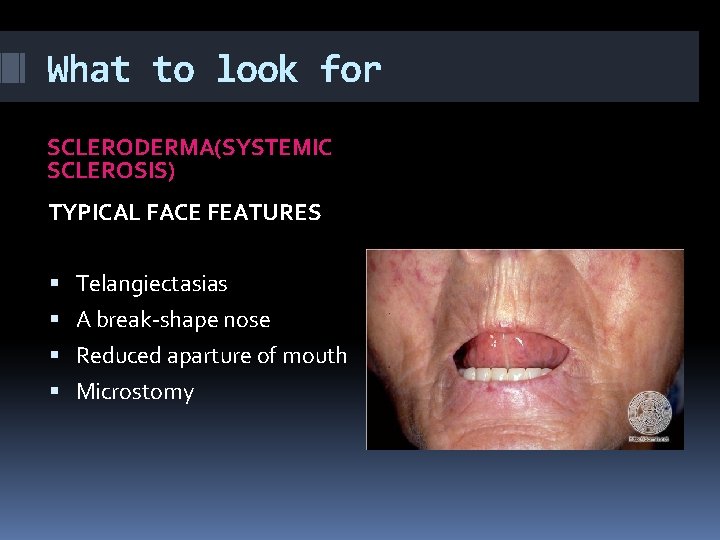
What to look for SCLERODERMA(SYSTEMIC SCLEROSIS) TYPICAL FACE FEATURES Telangiectasias A break-shape nose Reduced aparture of mouth Microstomy

What to look for SCLERODERMA(SYSTEMIC SCLEROSIS) TYPICAL FACE FEATURES As the skin thickens and hardens The face develops an expresessionless image Mask-like stiffness Appears ‘mummified’

What to look for SCLERODERMA(SYSTEMIC SCLEROSIS) CREST SYNDROME Calcinosis Raynaud’s phenomenon Esophageal dysfunction Telangiectasias

What not to miss Two important aspects of dermatology 1 -to recognize and manage common skin conditions 2 -to acquire the ability to recognize more serious underlying problems Skin signs of systemic disease especially of internal malignancy

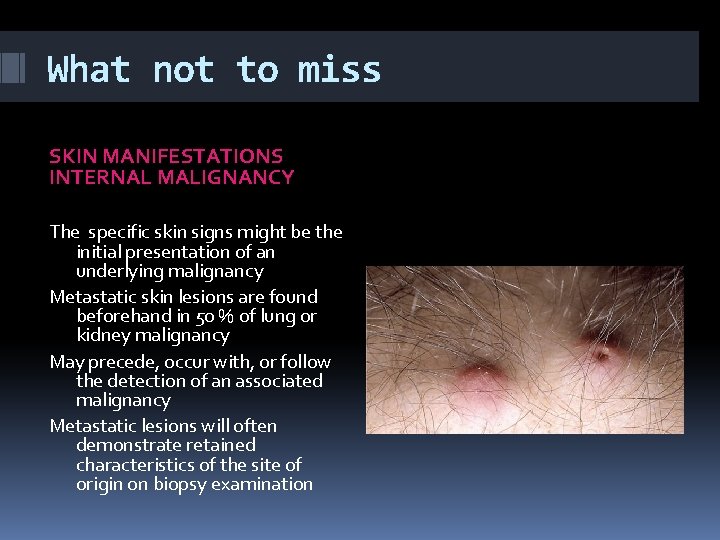
What not to miss SKIN MANIFESTATIONS INTERNAL MALIGNANCY The specific skin signs might be the initial presentation of an underlying malignancy Metastatic skin lesions are found beforehand in 50 % of lung or kidney malignancy May precede, occur with, or follow the detection of an associated malignancy Metastatic lesions will often demonstrate retained characteristics of the site of origin on biopsy examination

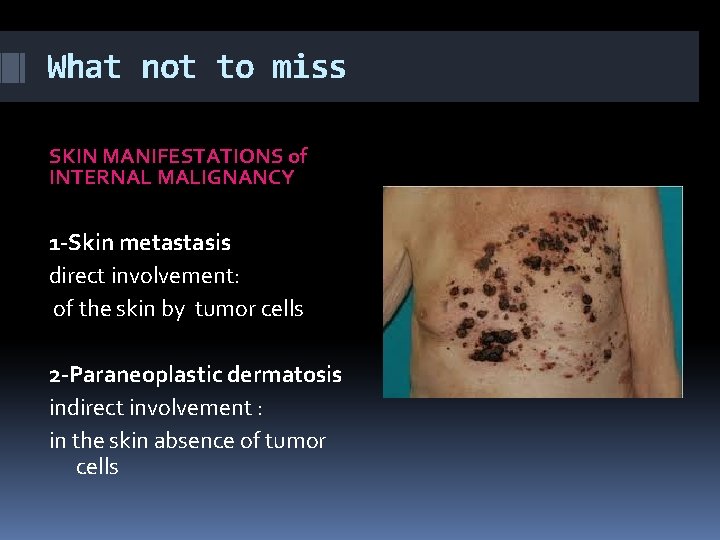
What not to miss SKIN MANIFESTATIONS of INTERNAL MALIGNANCY 1 -Skin metastasis direct involvement: of the skin by tumor cells 2 -Paraneoplastic dermatosis indirect involvement : in the skin absence of tumor cells

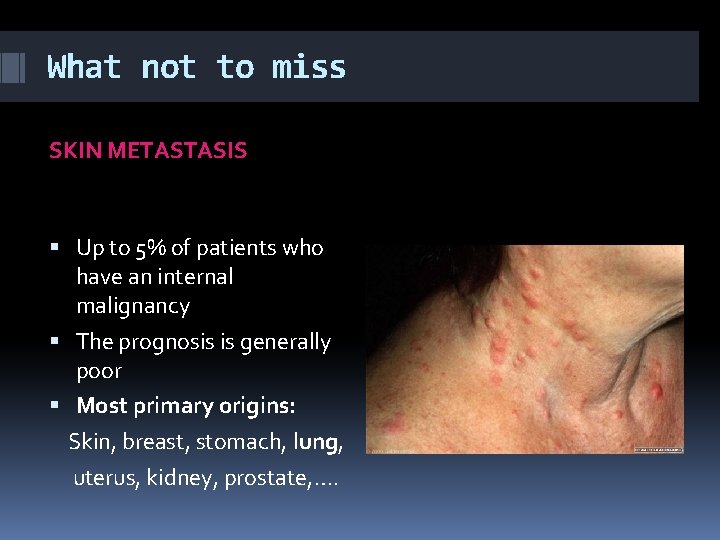
What not to miss SKIN METASTASIS Up to 5% of patients who have an internal malignancy The prognosis is generally poor Most primary origins: Skin, breast, stomach, lung, uterus, kidney, prostate, ….

What not to miss SKIN METASTASIS The sites of predilection: Scalp: breast, lung, genitourinary system carcinomas Chest: breast carsinoma Abdomen: genitourinary ca

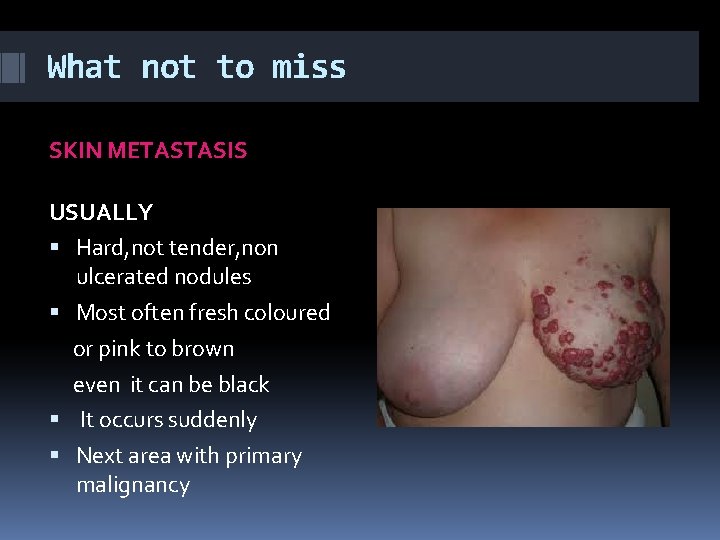
What not to miss SKIN METASTASIS USUALLY Hard, not tender, non ulcerated nodules Most often fresh coloured or pink to brown even it can be black It occurs suddenly Next area with primary malignancy

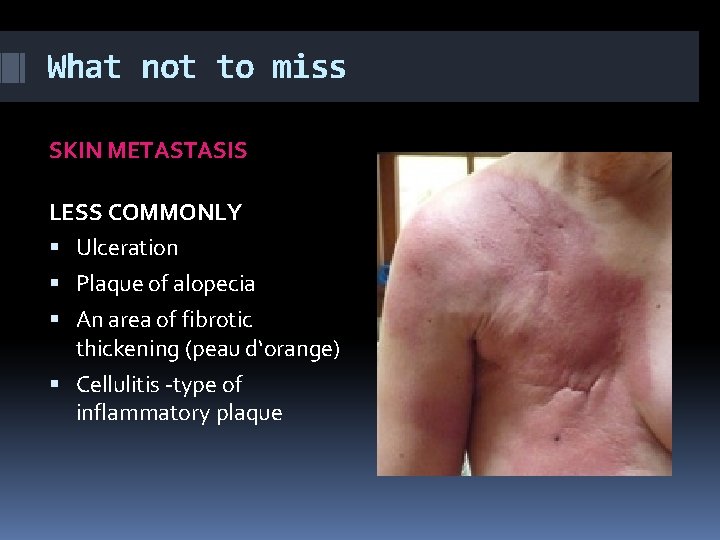
What not to miss SKIN METASTASIS LESS COMMONLY Ulceration Plaque of alopecia An area of fibrotic thickening (peau d‘orange) Cellulitis -type of inflammatory plaque

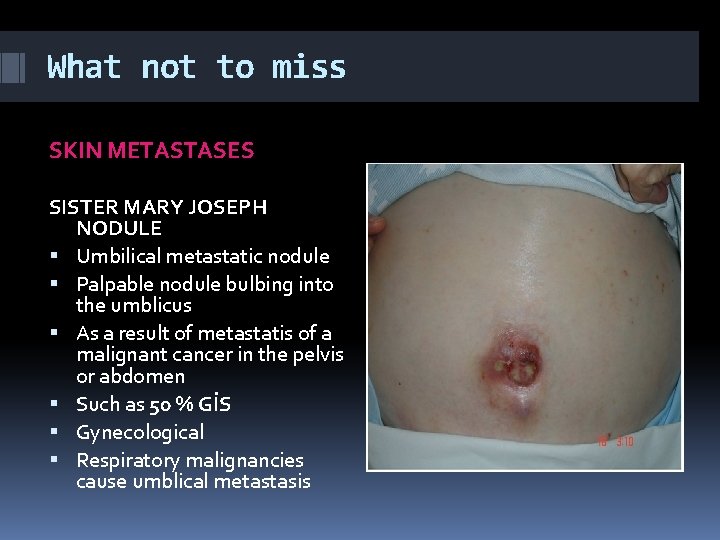
What not to miss SKIN METASTASES SISTER MARY JOSEPH NODULE Umbilical metastatic nodule Palpable nodule bulbing into the umblicus As a result of metastatis of a malignant cancer in the pelvis or abdomen Such as 50 % GİS Gynecological Respiratory malignancies cause umblical metastasis

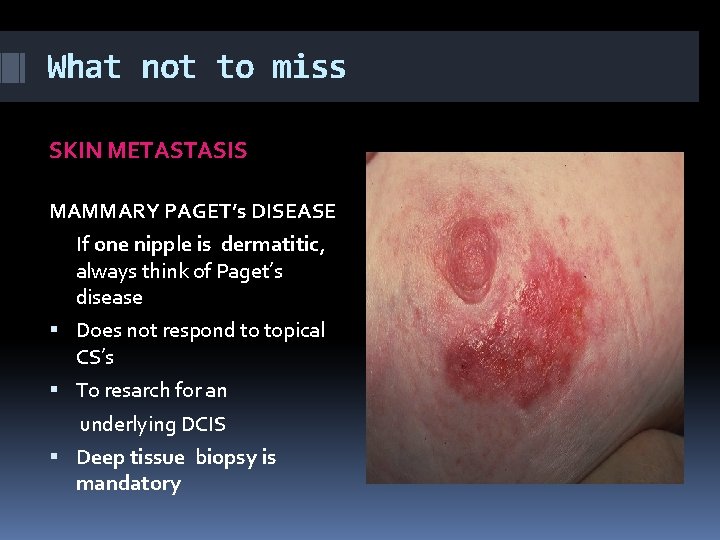
What not to miss SKIN METASTASIS MAMMARY PAGET’s DISEASE If one nipple is dermatitic, always think of Paget’s disease Does not respond to topical CS’s To resarch for an underlying DCIS Deep tissue biopsy is mandatory

What not to miss SKIN METASTASIS EXTRAMAMMARY PAGET’S DISEASE Less often Mammary Paget’s Location on adjacent to genitals Associated with underlying adnexal carcinoma Skin biopsy of any persistent eczematous lesion in this area is obligatory

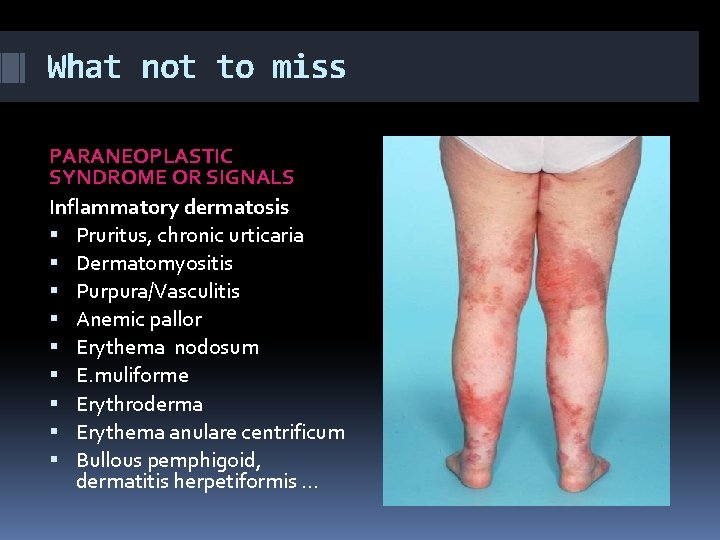
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Inflammatory dermatosis Pruritus, chronic urticaria Dermatomyositis Purpura/Vasculitis Anemic pallor Erythema nodosum E. muliforme Erythroderma Erythema anulare centrificum Bullous pemphigoid, dermatitis herpetiformis …

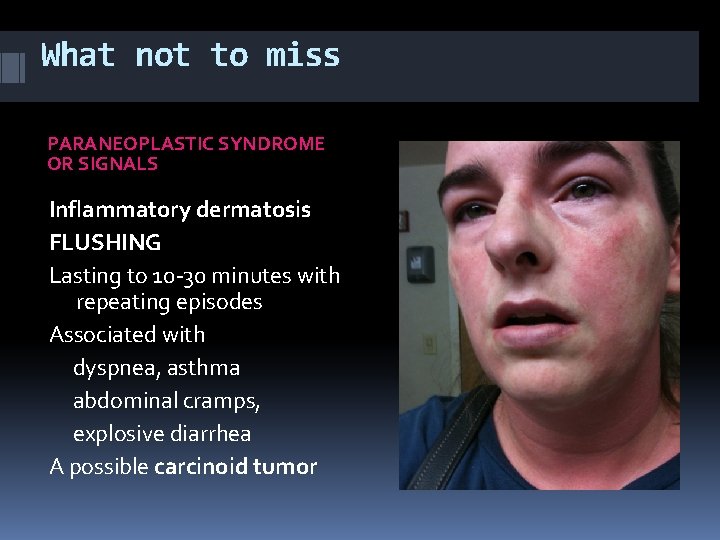
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Inflammatory dermatosis FLUSHING Lasting to 10 -30 minutes with repeating episodes Associated with dyspnea, asthma abdominal cramps, explosive diarrhea A possible carcinoid tumor

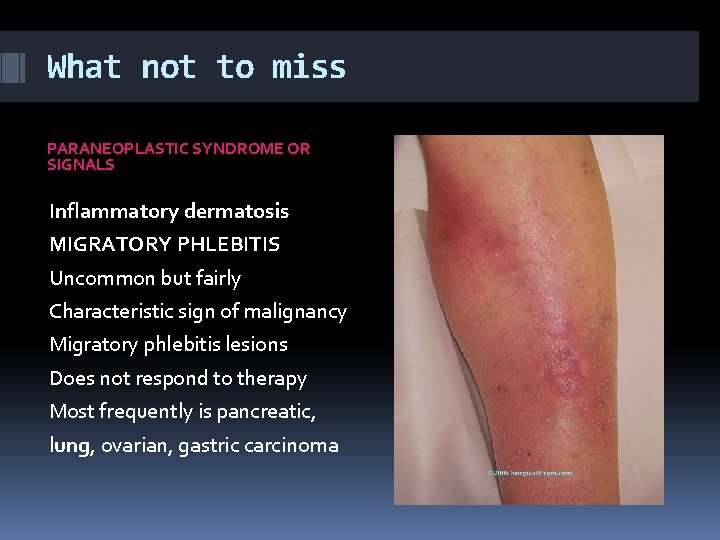
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Inflammatory dermatosis MIGRATORY PHLEBITIS Uncommon but fairly Characteristic sign of malignancy Migratory phlebitis lesions Does not respond to therapy Most frequently is pancreatic, lung, ovarian, gastric carcinoma

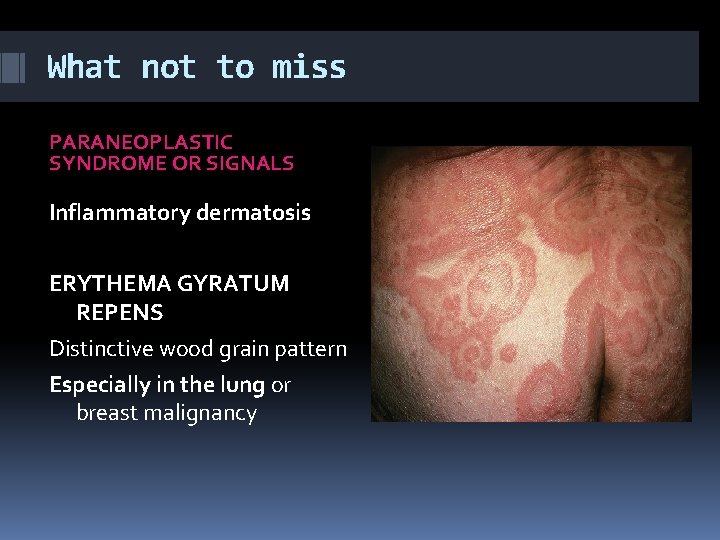
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Inflammatory dermatosis ERYTHEMA GYRATUM REPENS Distinctive wood grain pattern Especially in the lung or breast malignancy

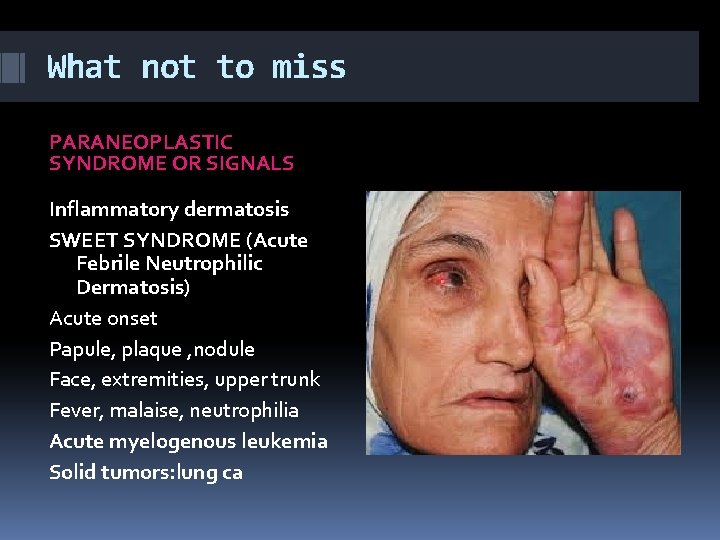
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Inflammatory dermatosis SWEET SYNDROME (Acute Febrile Neutrophilic Dermatosis) Acute onset Papule, plaque , nodule Face, extremities, upper trunk Fever, malaise, neutrophilia Acute myelogenous leukemia Solid tumors: lung ca

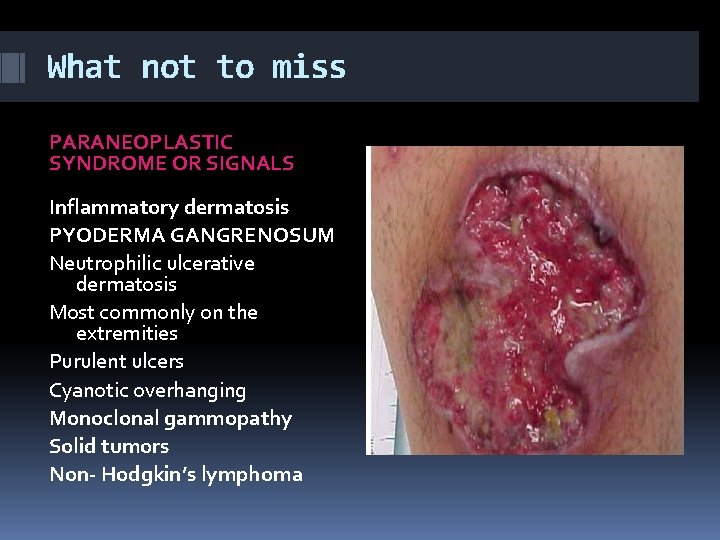
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Inflammatory dermatosis PYODERMA GANGRENOSUM Neutrophilic ulcerative dermatosis Most commonly on the extremities Purulent ulcers Cyanotic overhanging Monoclonal gammopathy Solid tumors Non- Hodgkin’s lymphoma

What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Proliferative dermatosis Acquired Ichtyosis Dry scaling Particularly over the extensor surface of extremities Might be sign of Hodgkin’s disease Myeloma

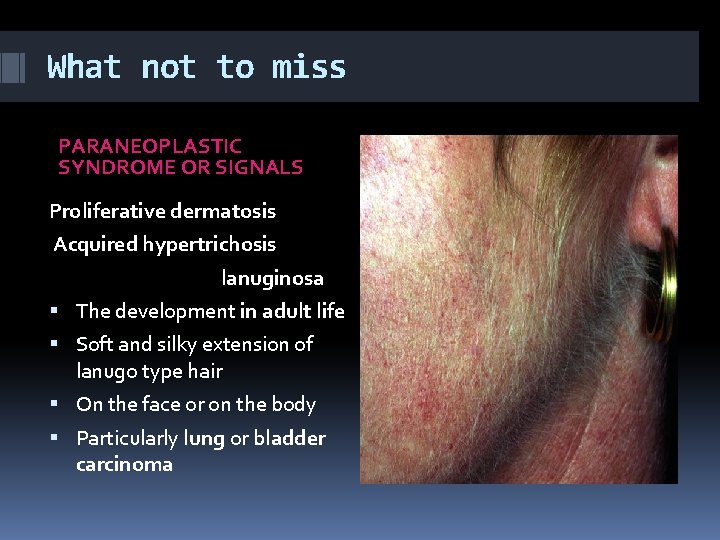
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Proliferative dermatosis Acquired hypertrichosis lanuginosa The development in adult life Soft and silky extension of lanugo type hair On the face or on the body Particularly lung or bladder carcinoma

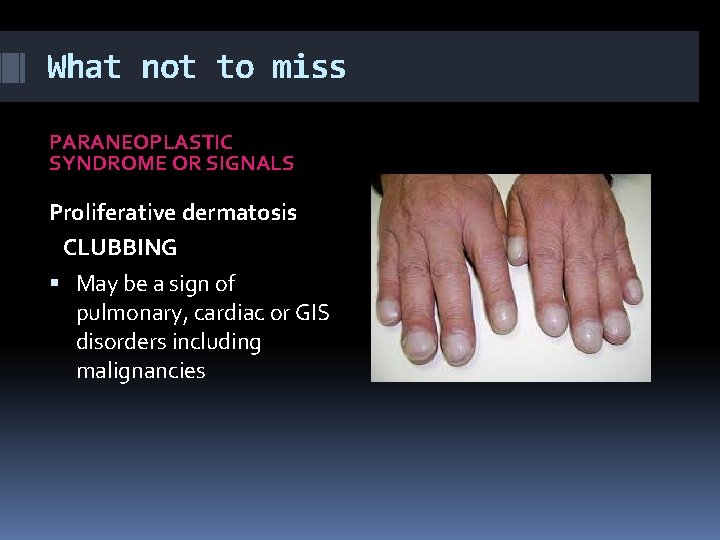
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Proliferative dermatosis CLUBBING May be a sign of pulmonary, cardiac or GIS disorders including malignancies

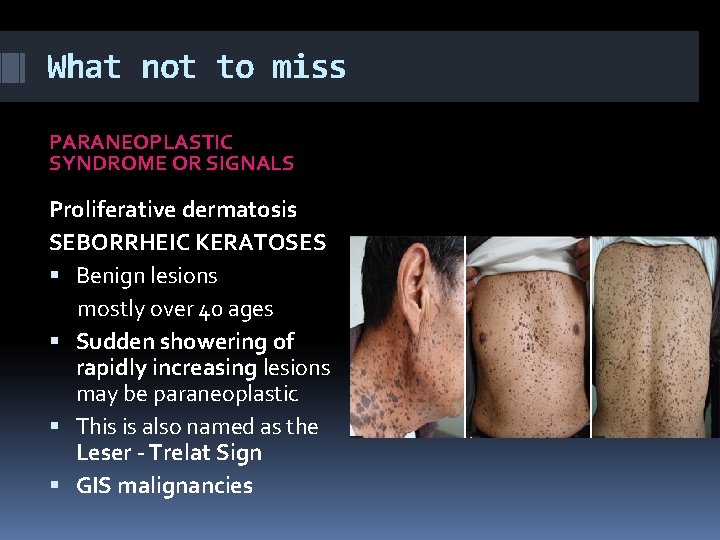
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Proliferative dermatosis SEBORRHEIC KERATOSES Benign lesions mostly over 40 ages Sudden showering of rapidly increasing lesions may be paraneoplastic This is also named as the Leser - Trelat Sign GIS malignancies

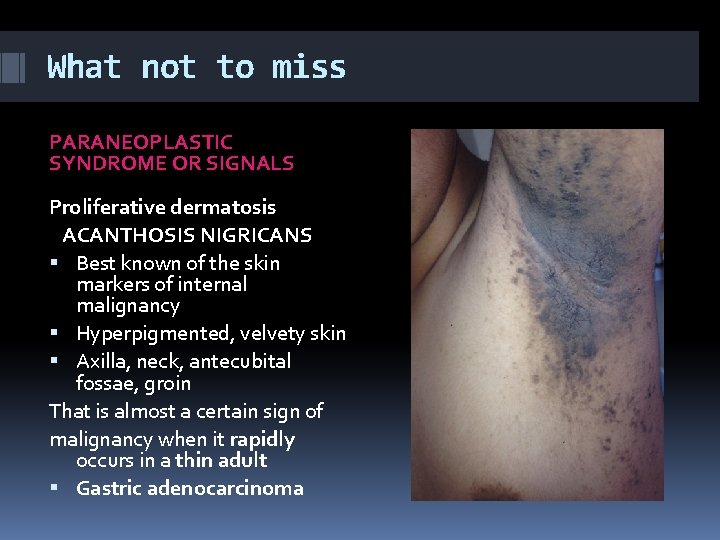
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Proliferative dermatosis ACANTHOSIS NIGRICANS Best known of the skin markers of internal malignancy Hyperpigmented, velvety skin Axilla, neck, antecubital fossae, groin That is almost a certain sign of malignancy when it rapidly occurs in a thin adult Gastric adenocarcinoma

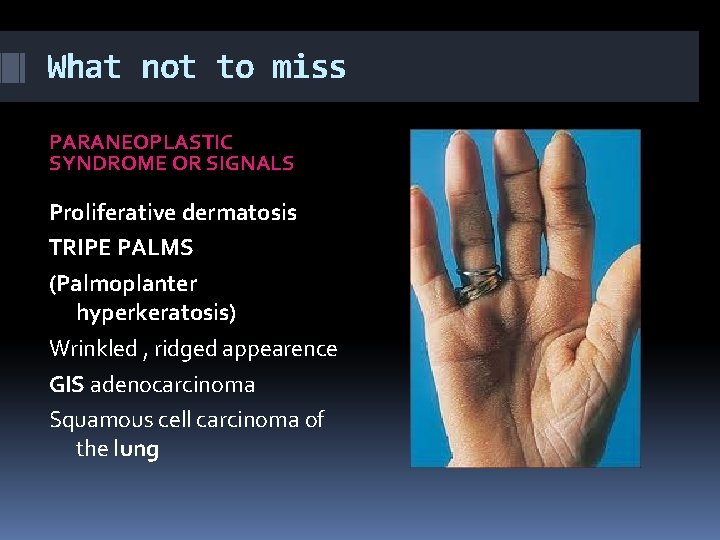
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Proliferative dermatosis TRIPE PALMS (Palmoplanter hyperkeratosis) Wrinkled , ridged appearence GIS adenocarcinoma Squamous cell carcinoma of the lung

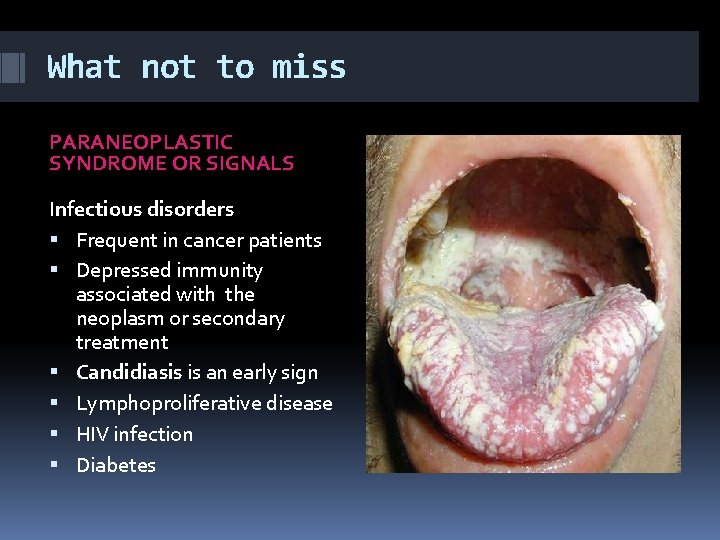
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS Infectious disorders Frequent in cancer patients Depressed immunity associated with the neoplasm or secondary treatment Candidiasis is an early sign Lymphoproliferative disease HIV infection Diabetes

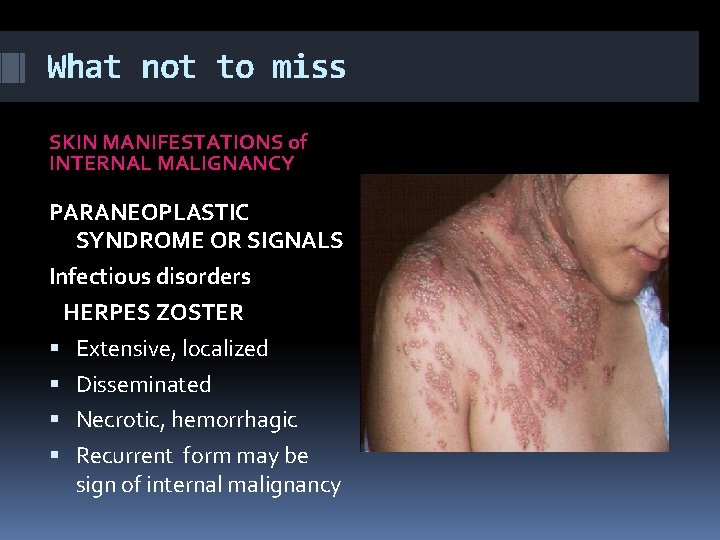
What not to miss SKIN MANIFESTATIONS of INTERNAL MALIGNANCY PARANEOPLASTIC SYNDROME OR SIGNALS Infectious disorders HERPES ZOSTER Extensive, localized Disseminated Necrotic, hemorrhagic Recurrent form may be sign of internal malignancy

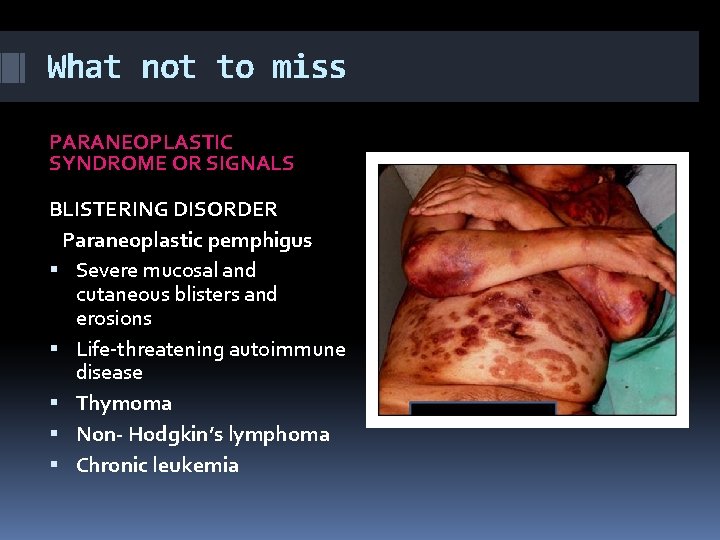
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS BLISTERING DISORDER Paraneoplastic pemphigus Severe mucosal and cutaneous blisters and erosions Life-threatening autoimmune disease Thymoma Non- Hodgkin’s lymphoma Chronic leukemia

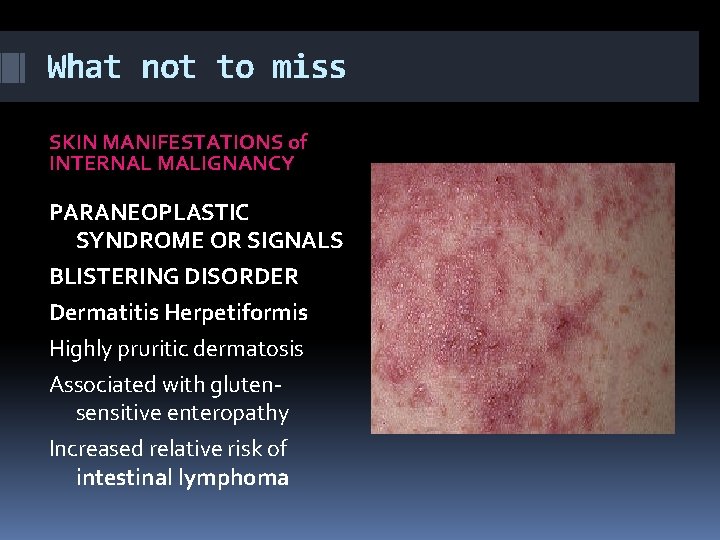
What not to miss SKIN MANIFESTATIONS of INTERNAL MALIGNANCY PARANEOPLASTIC SYNDROME OR SIGNALS BLISTERING DISORDER Dermatitis Herpetiformis Highly pruritic dermatosis Associated with glutensensitive enteropathy Increased relative risk of intestinal lymphoma

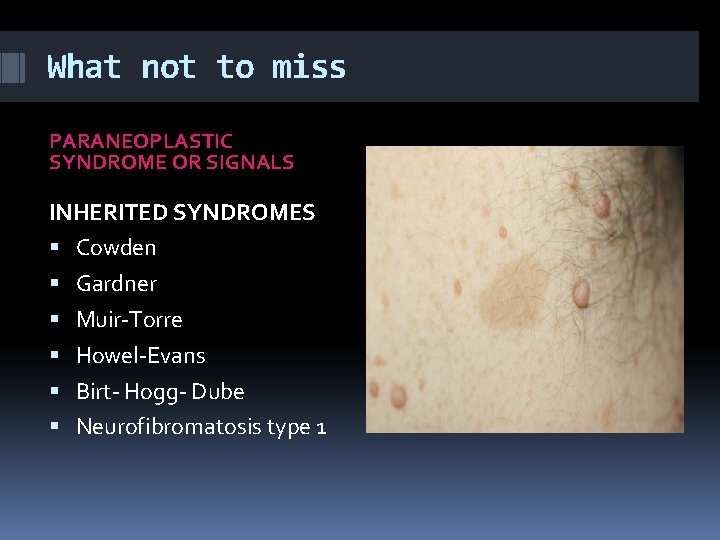
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS INHERITED SYNDROMES Cowden Gardner Muir-Torre Howel-Evans Birt- Hogg- Dube Neurofibromatosis type 1

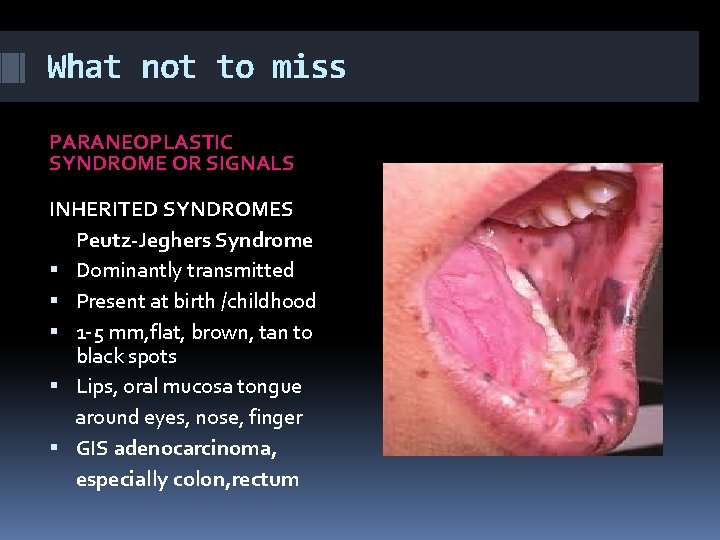
What not to miss PARANEOPLASTIC SYNDROME OR SIGNALS INHERITED SYNDROMES Peutz-Jeghers Syndrome Dominantly transmitted Present at birth /childhood 1 -5 mm, flat, brown, tan to black spots Lips, oral mucosa tongue around eyes, nose, finger GIS adenocarcinoma, especially colon, rectum

SKIN Although a plethora of specialized modern diagnostic tests are available The skin still remains the only organ of the body that is immediately and completely accessible to direct clinical examination

SKIN MANIFESTATIONS of SYSTEMIC DISEASE The skin has the potential to provide a window into the patient The skin is an important aid in the diagnosis of systemic disease THANKS FOR YOUR ATTENDANCE