Ultrasound Physics Have no fear Presentation by Alexis

Ultrasound Physics Have no fear Presentation by Alexis Palley MD Department of Emergency Medicine Cooper University Hospital

“How does it do that? ” Lecture Objectives: Ø Review basic physics vocabulary Ø Explain the principles of sound waves Ø Use ultrasound physics to explain how images are produced Ø Teach how to use these principles to help your diagnostic abilities

Basics Ø Sound is energy traveling though matter as a wave Ø The wave travels by compressing and rarefacting matter Ø Depending on the matter- the wave will travel at different velocities or directions Ø U/S probes emit and receive the energy as waves to form pictures

Physical Principles
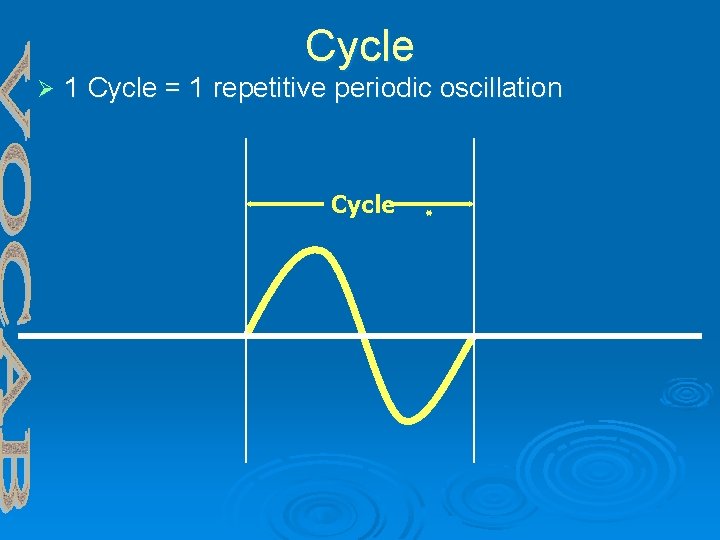
Cycle Ø 1 Cycle = 1 repetitive periodic oscillation Cycle

Frequency Ø # of cycles per second Ø Measured in Hertz (Hz) -Human Hearing 20 - 20, 000 Hz -Ultrasound > 20, 000 Hz -Diagnostic Ultrasound 2. 5 to 10 MHz (this is what we use!)
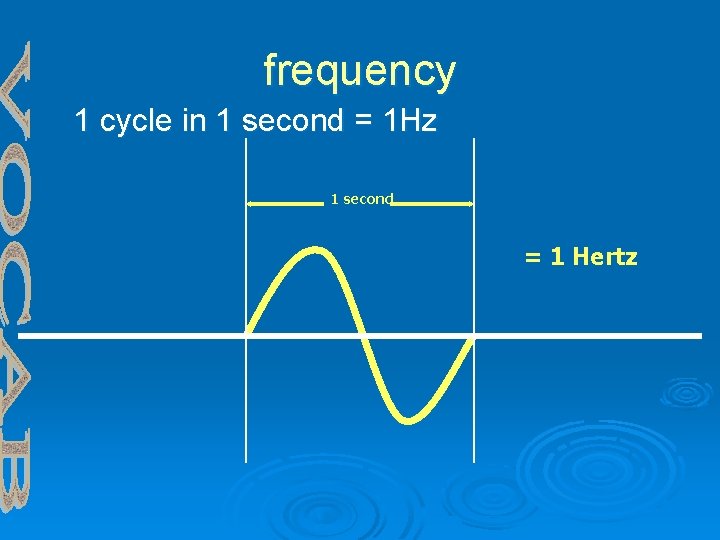
frequency 1 cycle in 1 second = 1 Hz 1 second = 1 Hertz

High Frequency Ø High frequency (5 -10 MHz) greater resolution less penetration Ø Shallow structures vascular, abscess, t/v gyn, testicular

Low Frequency Ø Low frequency (2 -3. 5 MHz) greater penetration less resolution Ø Deep structures Aorta, t/a gyn, card, gb, renal

Wavelength Ø The length of one complete cycle Ø A measurable distance
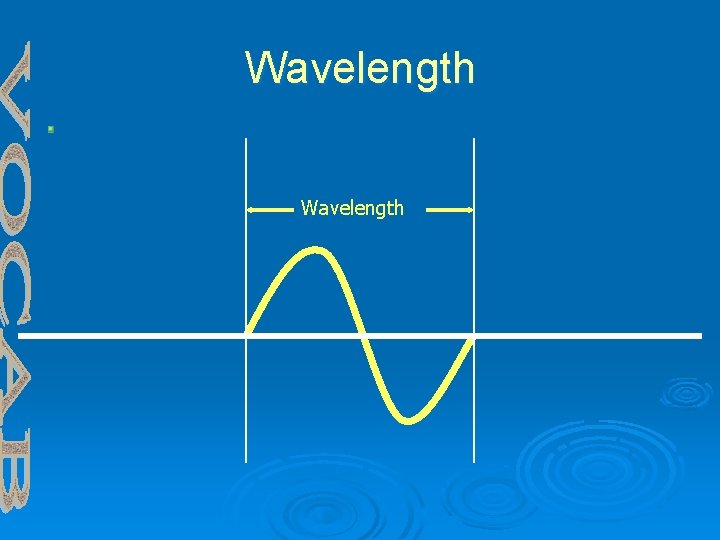
Wavelength
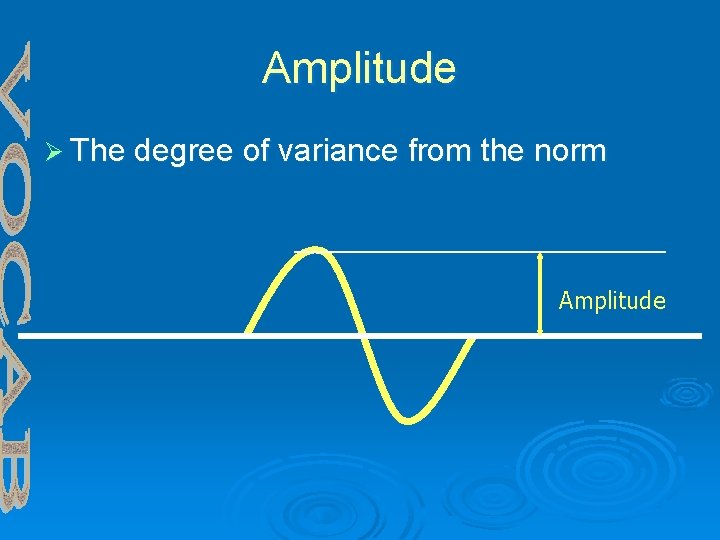
Amplitude Ø The degree of variance from the norm Amplitude

Producing an image Ø Probe emits a sound wave pulse- measures the time from emission to return of the echo Ø Wave travels by displacing matter, expanding and compressing adjacent tissues Ø It generates an ultrasonic wave that is propagated, impeded, reflected, refracted, or attenuated by the tissues it encounters

Producing an image Ø Important concepts in production of an U/S image: • Propagation velocity • Acoustic impedance • Reflection • Refraction • Attenuation

Propagation Velocity Sound is energy transmitted through a mediumØ Each medium has a constant velocity of sound (c) Ø Tissue’s resistance to compression Ø l density or stiffness Product of frequency (f) and wavelength (λ) c=fλ Ø Frequency and Wavelength therefore are directly proportional- if the frequency increases the wavelength must decrease. Ø

Propagation Velocity Ø Propagation velocity Increased by increasing stiffness Reduced by increasing density Ø Bone: 4, 080 m/sec Ø Air: 330 m/sec Ø Soft Tissue Average: 1, 540 m/sec

Impedance Ø Acoustic impedance (z) of a material is the product of its density and propagation velocity Z= pc Ø Differences in acoustic impedance create reflective interfaces that echo the u/s waves back at the probe Ø Impedance mismatch = ΔZ

Acoustic Impedance Ø Homogeneous mediums reflect no sound Ø acoustic interfaces create visual boundaries between different tissues. Ø Bone/tissue or air/tissue interfaces with large Δz values reflect almost all the sound Ø Muscle/fat interfaces with smaller Δz values reflect only part of the energy

Refraction A change in direction of the sound wave as it passes from one tissue to a tissue of higher or lower sound velocity Ø U/S scanners assume that an echo returns along a straight path Ø Distorts depth reading by the probe Ø Minimize refraction by scanning perpendicular to the interface that is causing the refraction Ø

Reflection Ø The production of echoes at reflecting interfaces between tissues of differing physical properties. Ø Specular - large smooth surfaces Ø Diffuse – small interfaces or nooks and crannies

Specular Reflection Ø Large smooth interfaces (e. g. diaphragm, bladder wall) reflect sound like a mirror Ø Only the echoes returning to the machine are displayed Ø Specular reflectors will return echoes to the machine only if the sound beam is perpendicular to the interface

Diffuse Reflector Ø Most echoes that are imaged arise from small interfaces within solid organs Ø These interfaces may be smaller than the wavelength of the sound Ø The echoes produced scatter in all directions Ø These echoes form the characteristic pattern of solid organs and other tissues
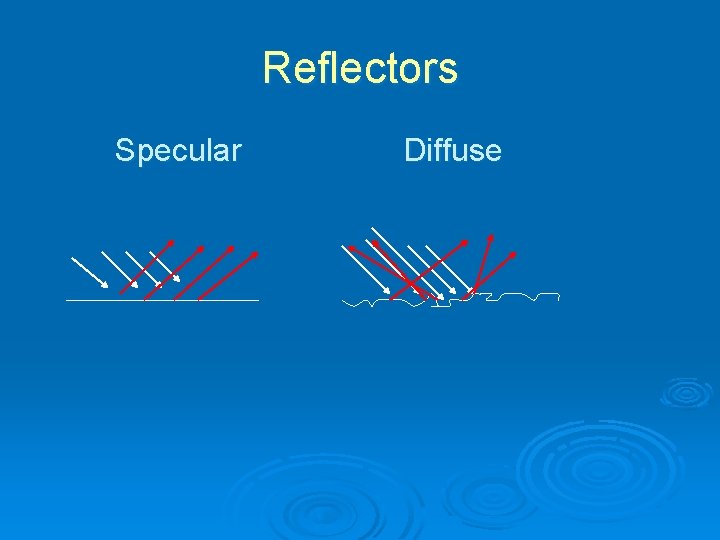
Reflectors Specular Diffuse

Attenuation Ø The intensity of sound waves diminish as they travel through a medium Ø In ideal systems sound pressure (amplitude) is only reduced by the spreading of waves Ø In real systems some waves are scattered and others are absorbed, or reflected Ø This decrease in intensity (loss of amplitude) is called attenuation.

The Machine

Ultrasound scanners Ø Anatomy of a scanner: l l l Transmitter Transducer Receiver Processor Display Storage

Transmitter Ø a crystal makes energy into sound waves and then receives sound waves and converts to energy Ø This is the Piezoelectric effect Ø u/s machines use time elapsed with a presumed velocity (1, 540 m/s) to calculate depth of tissue interface Ø Image accuracy is therefore dependent on accuracy of the presumed velocity.

Transducers Ø Continuous mode l l l continuous alternating current doppler or theraputic u/s 2 crystals – 1 talks, 1 listens Ø Pulsed mode l l Diagnostic u/s Crystal talks and then listens

Receiver Ø Sound waves hit and make voltage across the crystalØ The receiver detects and amplifies these voltages Ø Compensates for attenuation

Signal Amplification Ø TGC (time gain compensation) l l l Manual control Selective enhancement or suppression of sectors of the image enhance deep and suppress superficial *blinders Ø Gain l l l Manual control Affects all parts of the image equally Seen as a change in “brightness” of the images on the entire screen *glasses
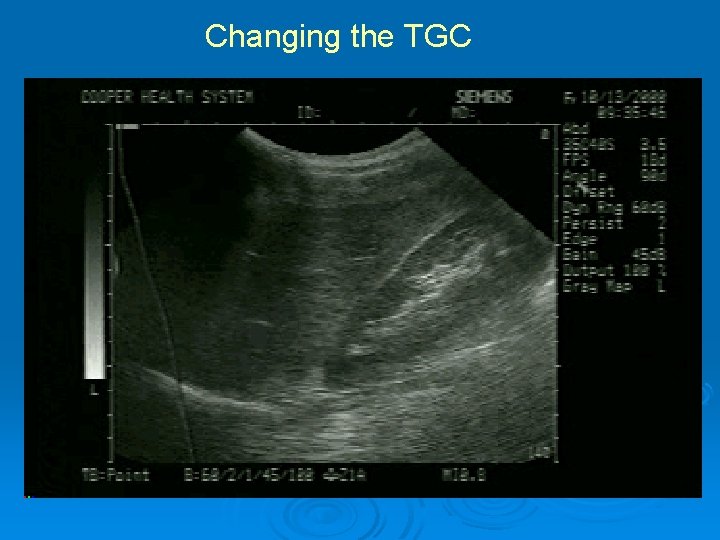
Changing the TGC
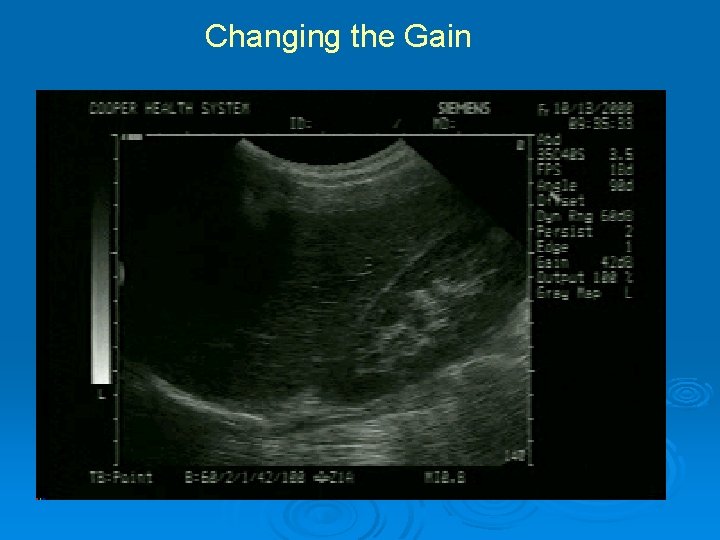
Changing the Gain

Displays Ø B-mode l l Real time gray scale, 2 D Flip book- 15 -60 images per second Ø M-mode l l Echo amplitude and position of moving targets Valves, vessels, chambers
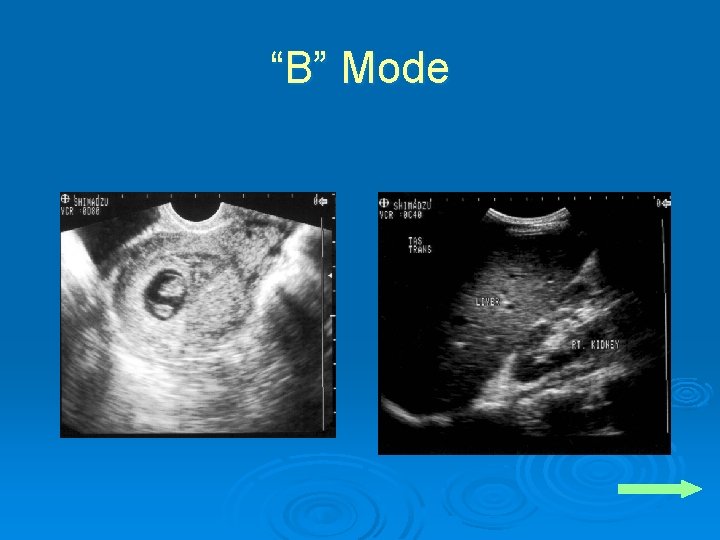
“B” Mode
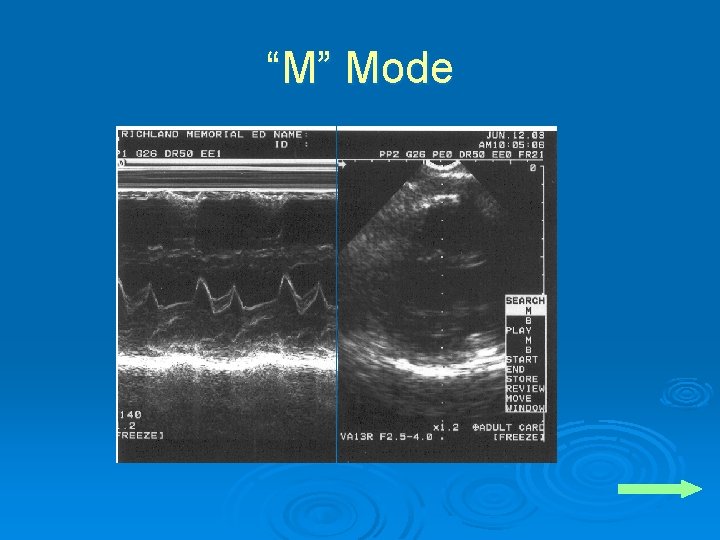
“M” Mode

Image properties Ø Echogenicity- amount of energy reflected back from tissue interface l l l Hyperechoic - greatest intensity - white Anechoic - no signal - black Hypoechoic – Intermediate - shades of gray
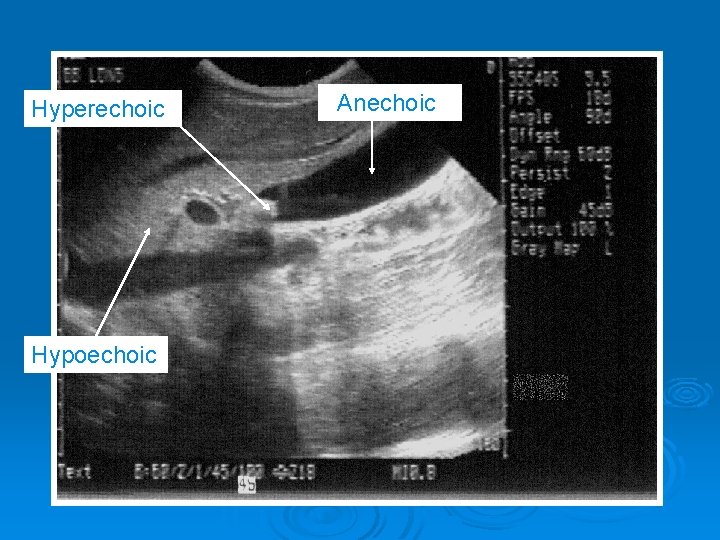
Hyperechoic Hypoechoic Anechoic

Image Resolution Ø Image quality is dependent on l l l Axial Resolution Lateral Resolution Focal Zone Probe Selection Frequency Selection Recognition of Artifacts

Axial Resolution Ø Ability to differentiate two objects along the long axis of the ultrasound beam Ø Determined by the pulse length • Product of wavelength λ and # of cycles in pulse • Decreases as frequency f increases Ø Higher frequencies produce better resolution

Axial Resolution Ø 5 MHz transducer l l Wavelength 0. 308 mm Pulse of 3 cycles Pulse length approximately 1 mm Maximum resolution distance of two objects = 1 mm Ø 10 MHz transducer l l Wavelength 0. 15 mm Pulse of 3 cycles Pulse length approximately 0. 5 mm Maximum resolution distance of two objects = 0. 5 mm
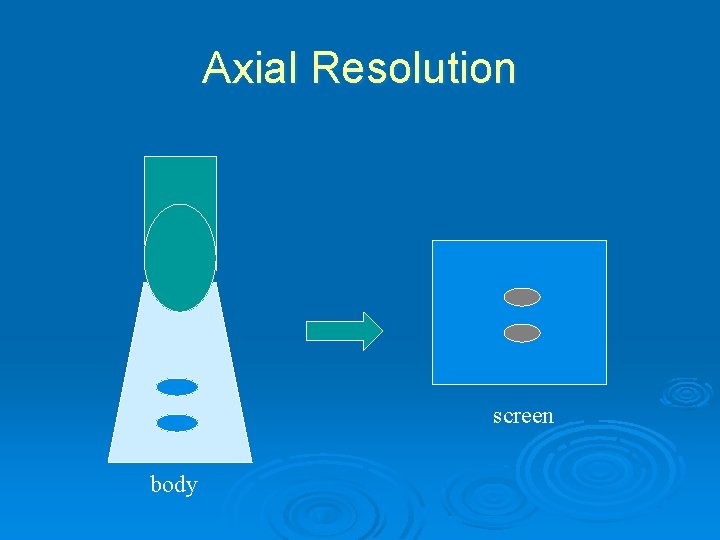
Axial Resolution screen body

Lateral Resolution Ø The ultrasound beam is made up of multiple individual beams Ø The individual beams are fused to appear as one beam Ø The distances between the single beams determines the lateral resolution

Lateral resolution Ø Ability to differentiate objects along an axis perpendicular to the ultrasound beam Ø Dependent on the width of the ultrasound beam, which can be controlled by focusing the beam Ø Dependent on the distance between the objects
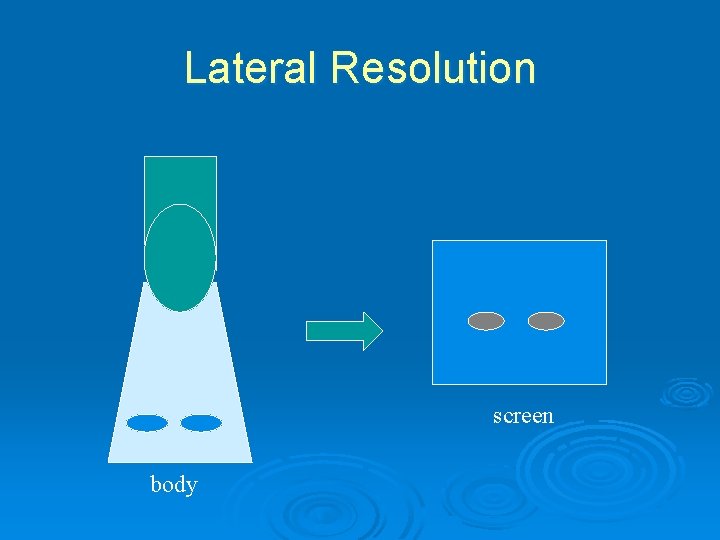
Lateral Resolution screen body
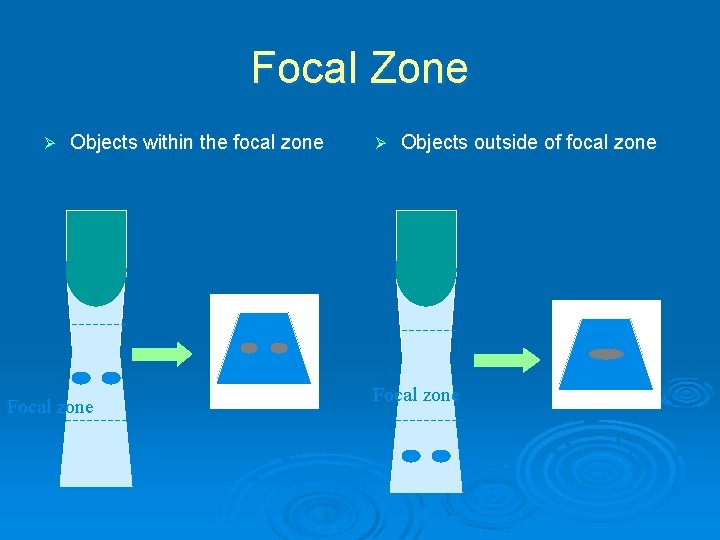
Focal Zone Ø Objects within the focal zone Focal zone Ø Objects outside of focal zone Focal zone
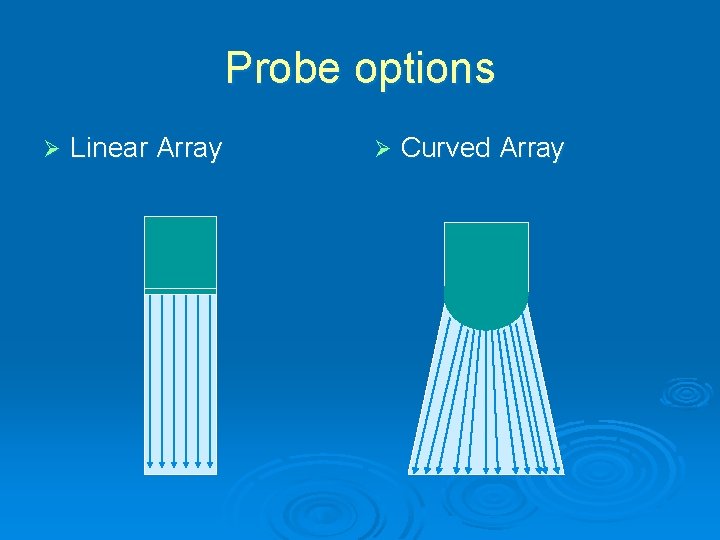
Probe options Ø Linear Array Ø Curved Array

Ultrasound Artifacts Ø Can be falsely interpreted as real pathology Ø May obscure pathology Ø Important to understand appreciate

Ultrasound Artifacts Acoustic enhancement Ø Acoustic shadowing Ø Lateral cystic shadowing (edge artifact) Ø Wide beam artifact Ø Side lobe artifact Ø Reverberation artifact Ø Gain artifact Ø Contact artifact Ø

Acoustic Enhancement Ø Opposite of acoustic shadowing Ø Better ultrasound transmission allows enhancement of the ultrasound signal distal to that region
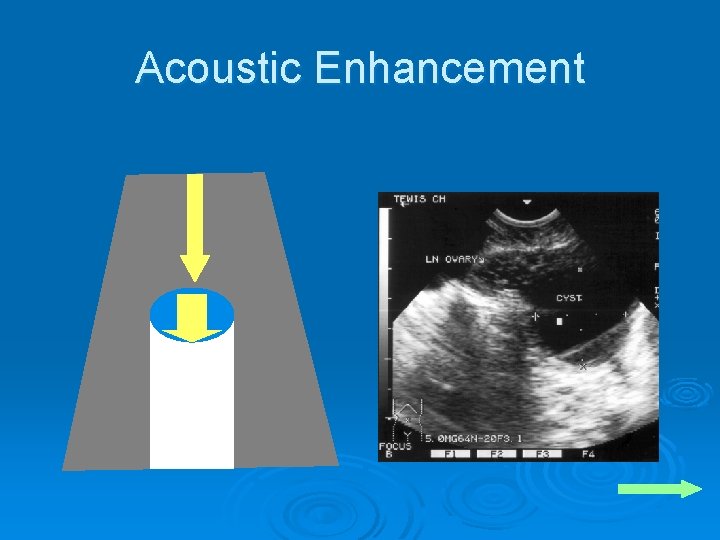
Acoustic Enhancement

Acoustic Shadowing Ø Occurs distal to any highly reflective or highly attenuating surface Ø Important diagnostic clue seen in a large number of medical conditions l l l Biliary stones Renal stones Tissue calcifications

Acoustic Shadowing Ø Shadow may be more prominent than the object causing it Ø Failure to visualize the source of a shadow is usually caused by the object being outside the plane of the ultrasound beam
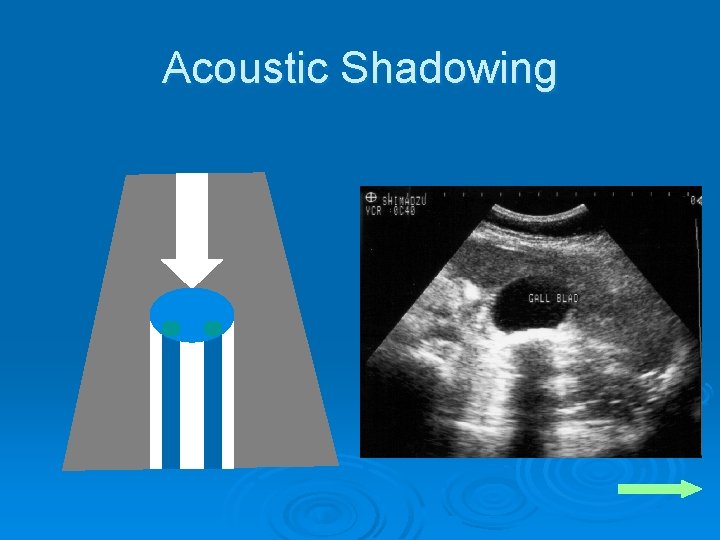
Acoustic Shadowing
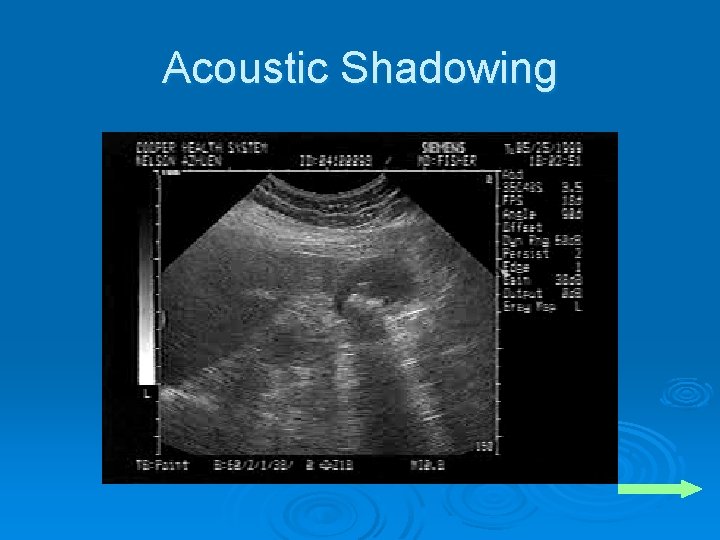
Acoustic Shadowing

Lateral Cystic Shadowing Ø A type of refraction artifact Ø Can be falsely interpreted as an acoustic shadow (similar to gallstone)
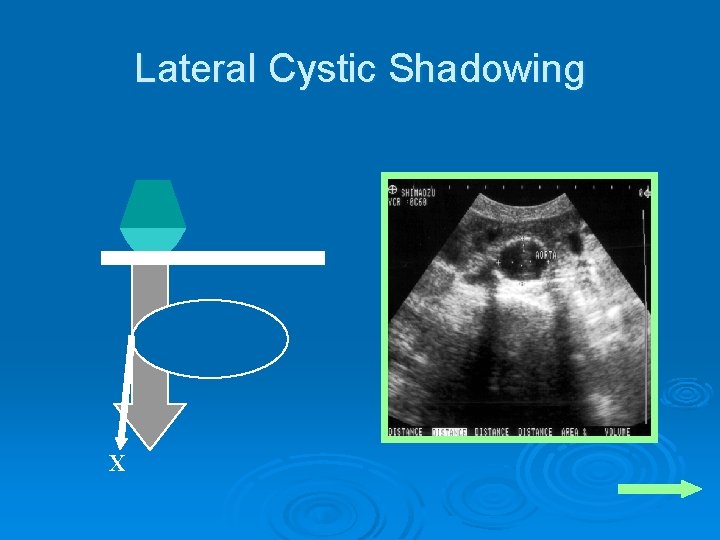
Lateral Cystic Shadowing X

Beam-Width Artifact Ø Gas bubbles in the duodenum can simulate a gall stone Ø Does not assume a dependent posture Ø Do not conform precisely to the walls of the gallbladder
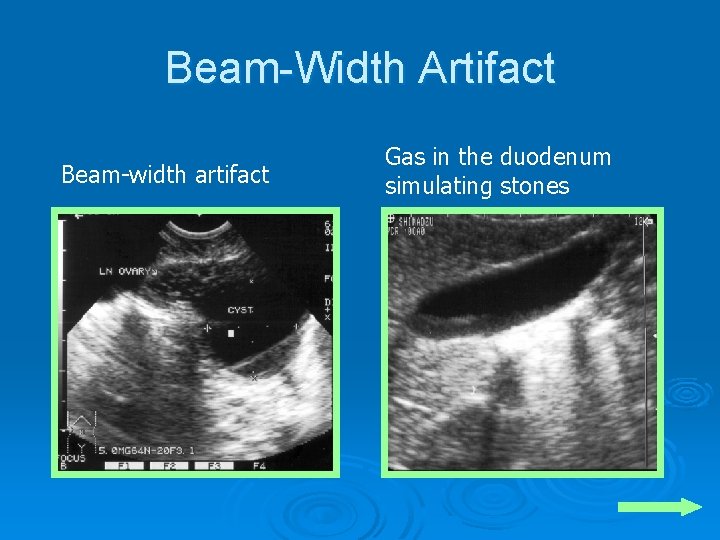
Beam-Width Artifact Beam-width artifact Gas in the duodenum simulating stones

Side Lobe Artifact Ø More than one ultrasound beam is generated at the transducer head Ø The beams other than the central axis beam are referred to as side lobes Ø Side lobes are of low intensity

Side Lobe Artifact Occasionally cause artifacts Ø The artifact by be obviated by alternating the angle of the transducer head Ø
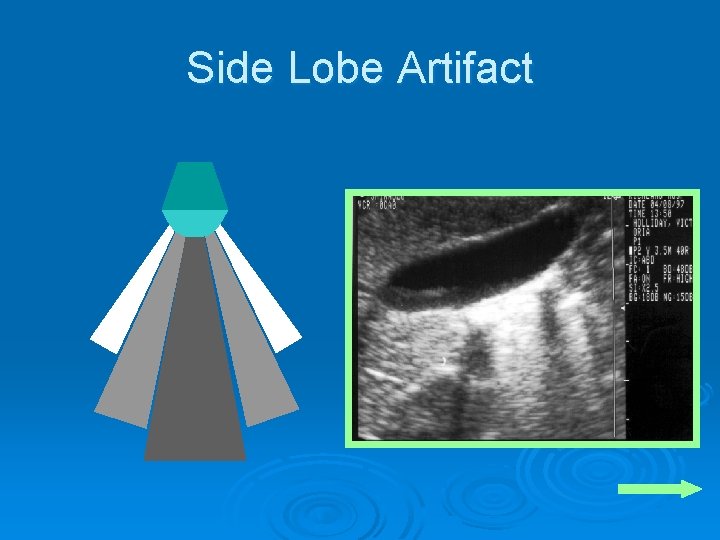
Side Lobe Artifact

Reverberation Artifacts Ø Several types Ø Caused by the echo bouncing back and forth between two or more highly reflective surfaces

Reverberation Artifacts Ø On the monitor parallel bands of reverberation echoes are seen Ø This causes a “comet-tail” pattern Ø Common reflective layers l l l Abdominal wall Foreign bodies Gas
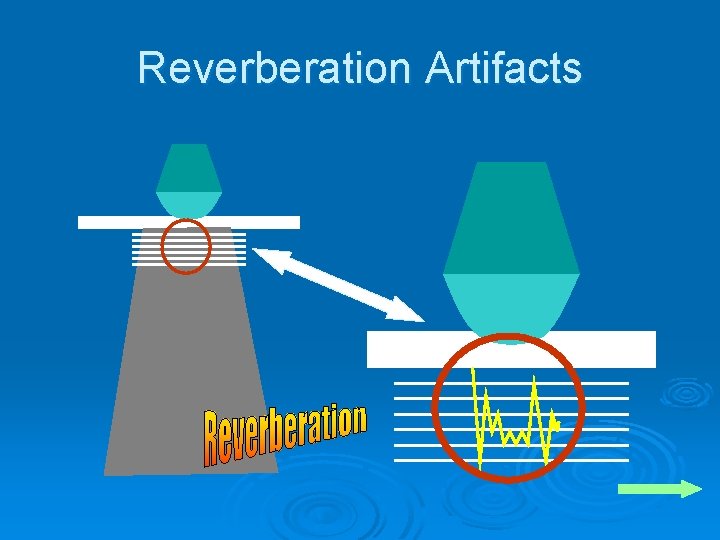
Reverberation Artifacts
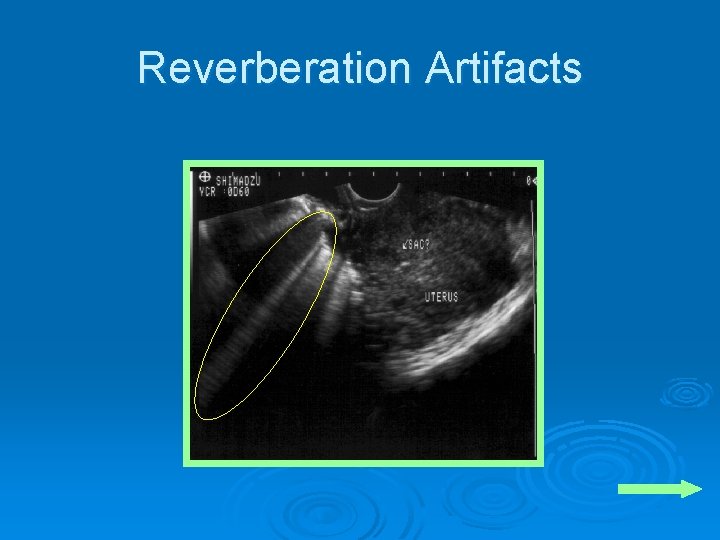
Reverberation Artifacts
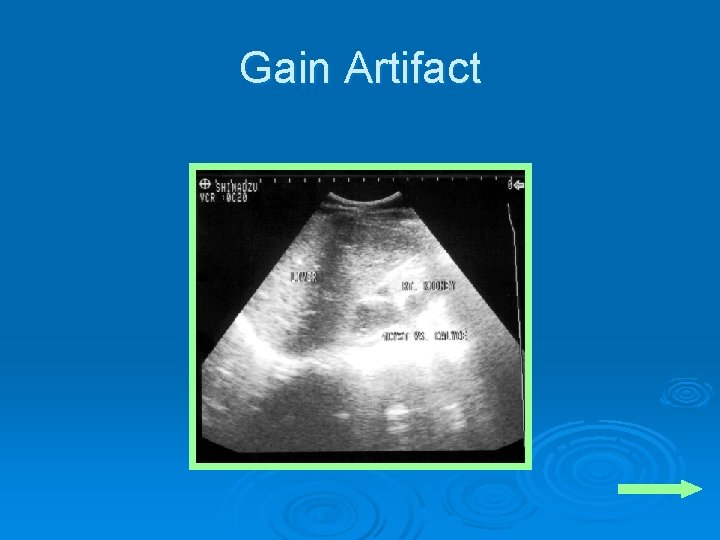
Gain Artifact
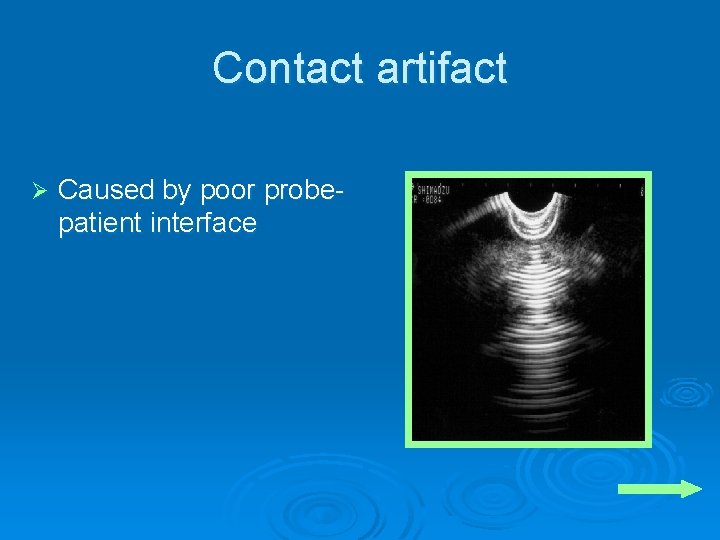
Contact artifact Ø Caused by poor probepatient interface

Take homes!

review Ø u/s uses waves echoed off reflective interfaces to display the structures of the bodyØ works by “talking and listening” Ø Must be careful when interpreting images Ø We have more control than we thought!
Think before you ultrasound!

Think before you ultrasound! Choose the right frequency probe – frequency = shallow & detailed Ø Hold the probe perpendicular to the organ wall being studied Ø Adjust the depth, tgc and gain to help your image Ø Artifact may be affecting your image Ø Use knowledge of physical properties of tissues to help with positioning- ie. use bladder for acoustic window to ta u/s. Ø

Thank you Any questions?
- Slides: 72