Ultrasound Guided Celiac Plexus Block and Neurolysis Dr

Ultrasound. Guided Celiac Plexus Block and Neurolysis Dr. A. Hosseinipour Pain Fellowship

Introduction o Celiac plexus block has been used in various upper abdominal malignant and nonmalignant pain syndromes with variable success o Pain signals stemming from visceral structures that are innervated by the celiac plexus can be interrupted by blocking the celiac plexus or the splanchnic nerves

Introduction o These structures include 1. Pancreas 2. Liver 3. Gallbladder 4. Mesentery 5. Omentum 6. Gastrointestinal tract from the lower esophagus to the transverse colon

Indications o acute pancreatitis: a) relief of pain b) reduce the morbidity and morbidity o ischemic bowel: a) Management of abdominal angina b) aid in bowel preservation o arterial embolization of the liver procedures to treat liver tumors

Indications o The most common application of neurolytic celiac plexus block is upper abdominal malignancy, especially pancreatic cancer o Kappis M. Erfahrungen mit lokalanasthesie bei bauchoperationen. Verh Dtsch Ges Chir. 1914; 43: 87– 9

Anatomy o The celiac plexus is a dense network of autonomic nerves that lies anterior to the aorta and the crus of the diaphragm at L 1 level o extends for few centimeters in front of the aorta surrounding the celiac trunk and the superior mesentric artery (SMA)

Anatomy o Fibers within the plexus: 1) efferent sympathetic preganglionic nerves a. greater splanchnic nerve T 5–T 9 b. lesser splanchnic nerve T 10–T 11 c. least splanchnic nerve T 12 2) parasympathetic preganglionic nerves (vagus, posterior trunk), 3) sensory nerves from the phrenic and vagus nerves 4) sympathetic postganglionic fibers

Anatomy o Afferent nociception fibers from the abdominal viscera pass diffusely through the celiac plexus and accompany the sympathetic fibers o Three pairs of ganglia exist within the plexus: 1. the celiac ganglia 2. the superior mesenteric ganglia 3. the aortic renal ganglia
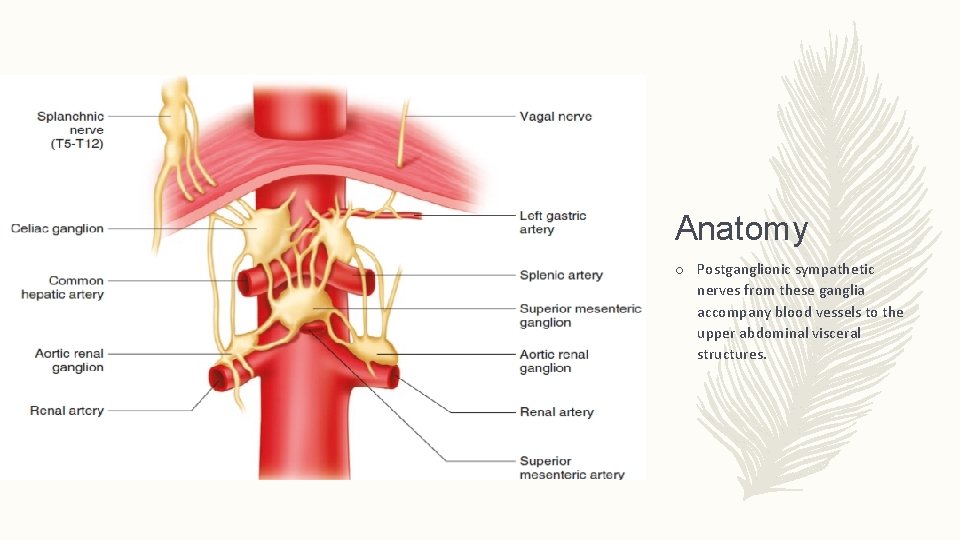
Anatomy o Postganglionic sympathetic nerves from these ganglia accompany blood vessels to the upper abdominal visceral structures.
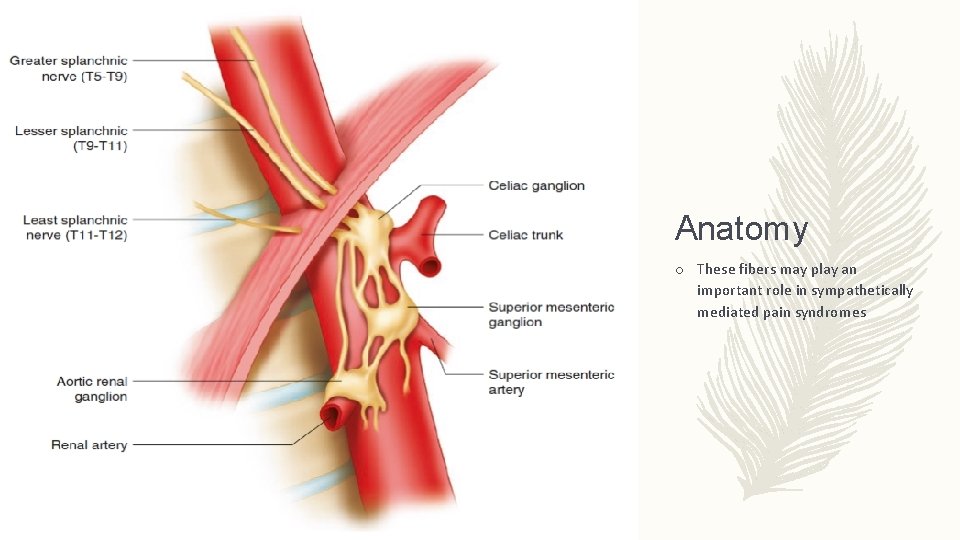
Anatomy o These fibers may play an important role in sympathetically mediated pain syndromes

Techniques for Celiac Plexus Block o Depending on the final needle placement relative to the diaphragm: 1. Retrocrural : deep splanchnic nerve block or classic approach a. spread of injectate cephalad and posterior to the diaphragmatic crura b. commonly performed with fluoroscopy or CT guidance at L 1 level c. prone position

Techniques for Celiac Plexus Block 2. Transcrural approach or “true” celiac plexus block a) with CT guidance needle is advanced through the diaphragmatic crura, and the tip is positioned on each side of the anterior aspect of the aorta b) with fluoroscopic guidance “transaortic approach” the needle is advanced through the aorta

Techniques for Celiac Plexus Block 3. Anterocrural approach or true “anterior” approach: a. This was described initially using anatomical landmarks then later with CT and ultrasound guidance b. final position anterior to the aorta at the level of the celiac plexus

Advantages of US-Guided Anterior Approach a. Ease of performance b. Speed of performance c. Performed with patient in supine position obviating need for patient to lie prone d. Can be performed at bedside in critically ill patients e. No radiation f. Less perioperative pain g. Precrural needle placement avoiding potential for nerve root trauma or inadvertent epidural, subdural, or subarachnoid injection

Limitations 1. Technically challenging in obese patients 2. Distortion of the anatomy by large pancreatic tumors or intra-abdominal masses anterior to the plexus will and will make it very challenging to identify the aorta and the celiac trunk. 3. vascular mass anterior to the plexus (by a prior CT or MRI) or as identified by ultrasound examination the anterior approach should be abounded.

Sonoanatomy o The celiac plexus is a conglomerate of tiny nerve fibers and autonomic ganglia o a heterogeneous tissue o that is – to date – not visualized clearly by high-resolution ultrasound o should be familiar with the relevant sonoanatomy in order to safely and accurately perform the procedure o One landmark is the abdominal aorta a. use 2– 5 MHz broadband probes in the median epigastrium b. tubular pulsating more or less anechoic structure
Sonoanatomy
Sonoanatomy
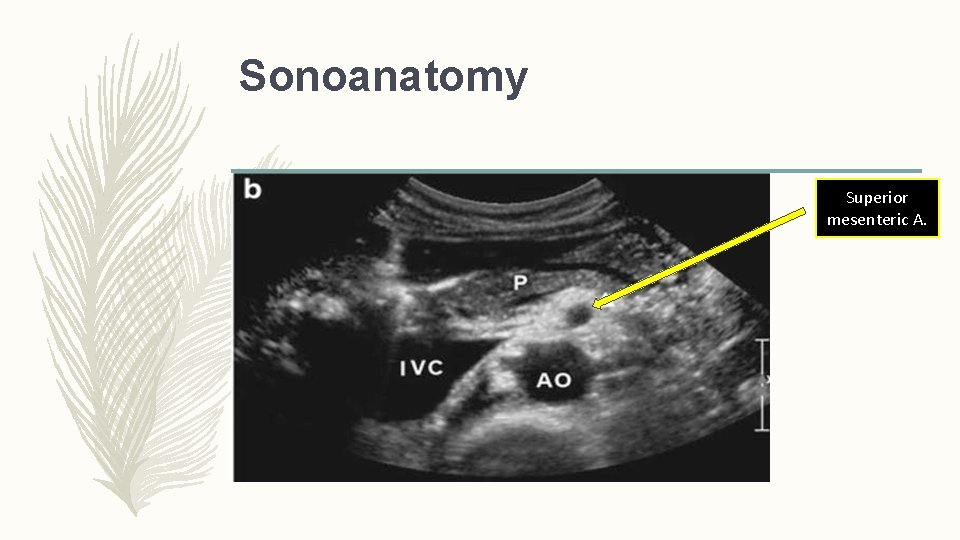
Sonoanatomy Superior mesenteric A.
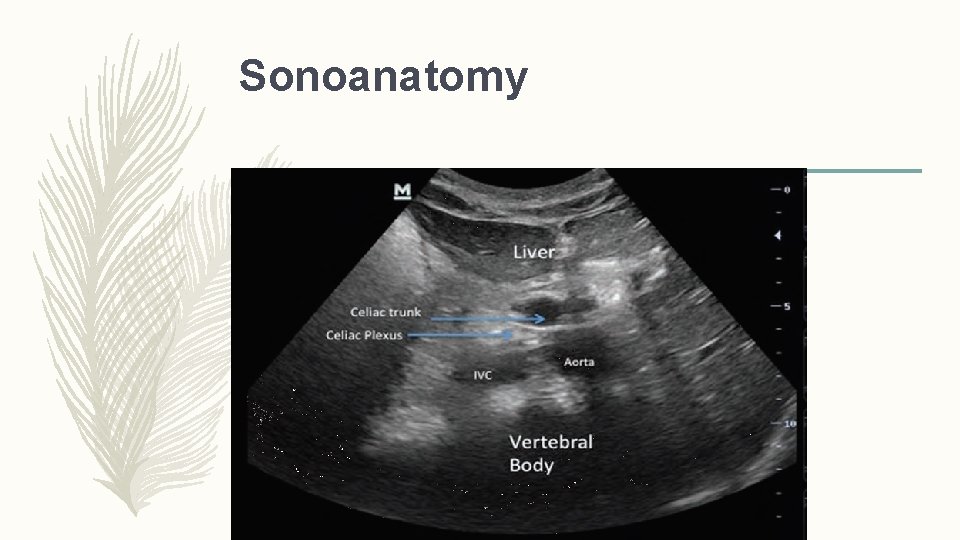
Sonoanatomy
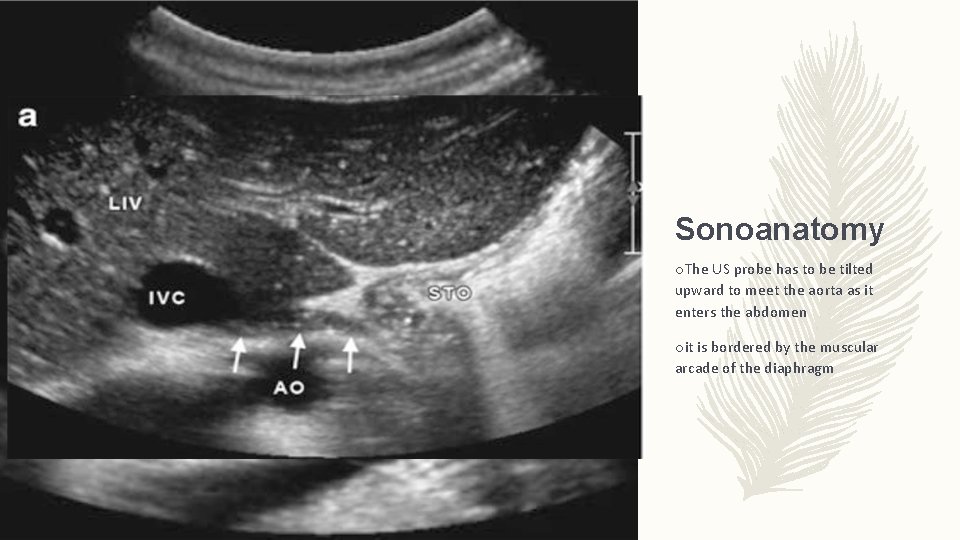
Sonoanatomy o. The US probe has to be tilted upward to meet the aorta as it enters the abdomen oit is bordered by the muscular arcade of the diaphragm
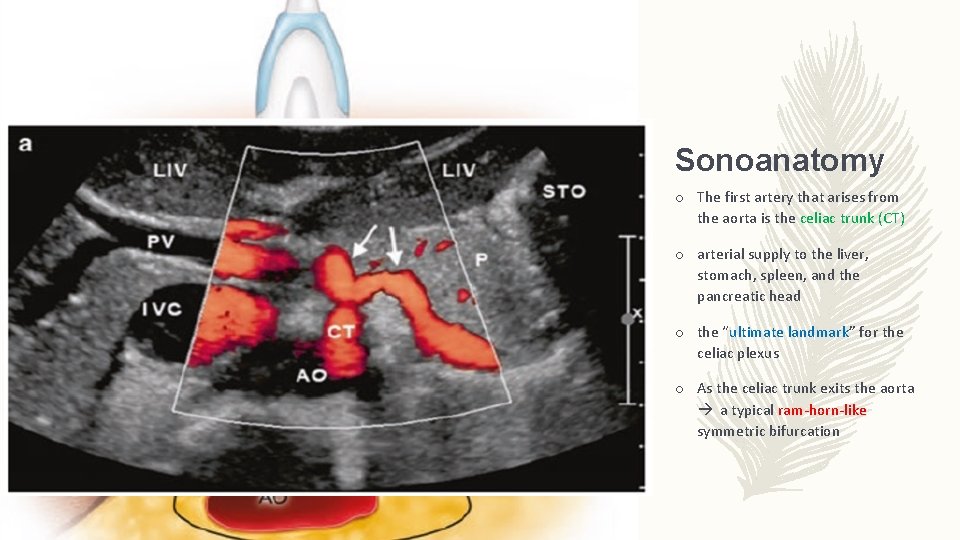
Sonoanatomy o The first artery that arises from the aorta is the celiac trunk (CT) o arterial supply to the liver, stomach, spleen, and the pancreatic head o the “ultimate landmark” for the celiac plexus o As the celiac trunk exits the aorta a typical ram-horn-like symmetric bifurcation

Sonoanatomy the shofar or ram’s horn
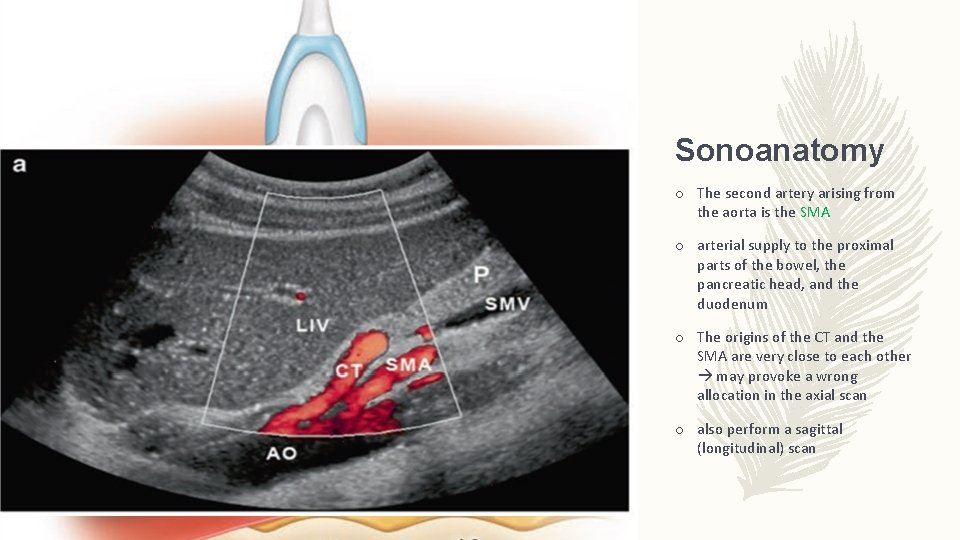
Sonoanatomy o The second artery arising from the aorta is the SMA o arterial supply to the proximal parts of the bowel, the pancreatic head, and the duodenum o The origins of the CT and the SMA are very close to each other may provoke a wrong allocation in the axial scan o also perform a sagittal (longitudinal) scan
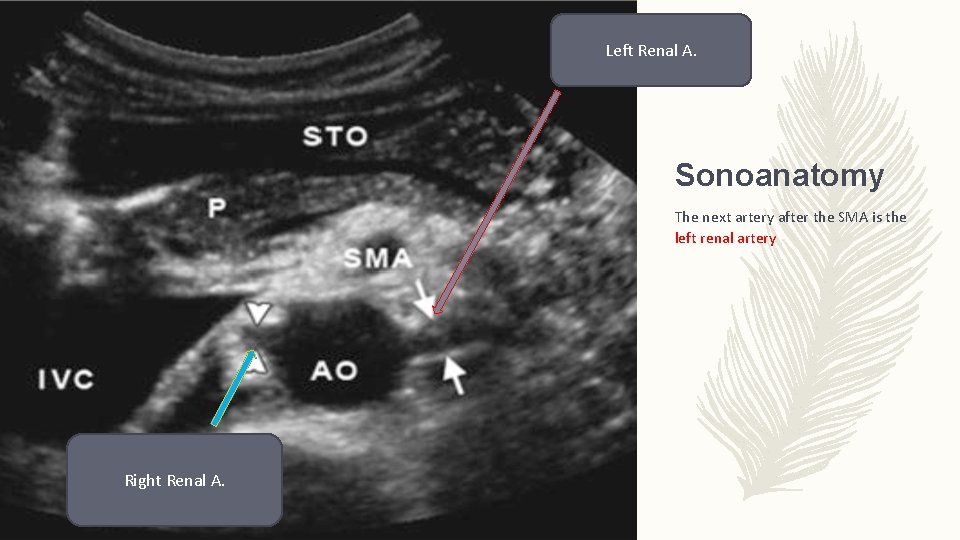
Left Renal A. Sonoanatomy The next artery after the SMA is the left renal artery Right Renal A.
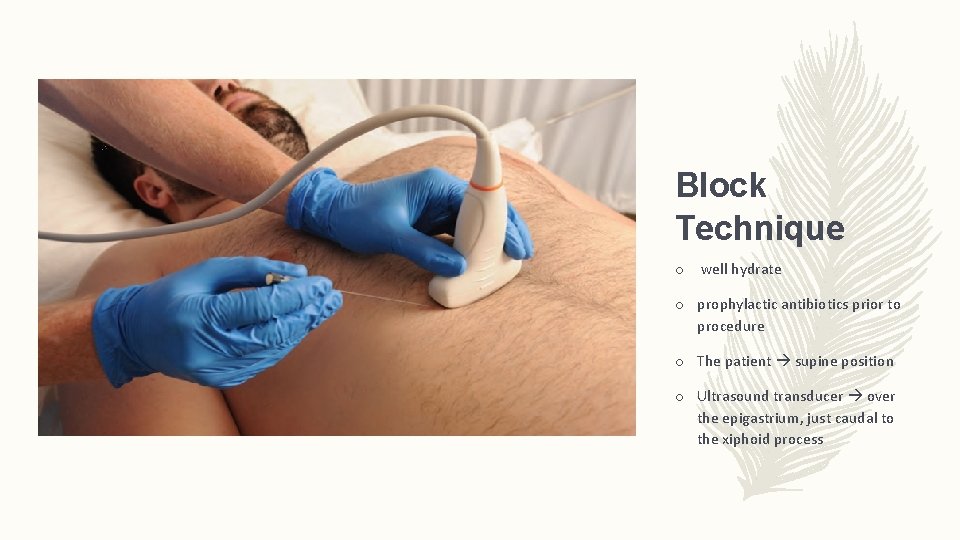
Block Technique o well hydrate o prophylactic antibiotics prior to procedure o The patient supine position o Ultrasound transducer over the epigastrium, just caudal to the xiphoid process
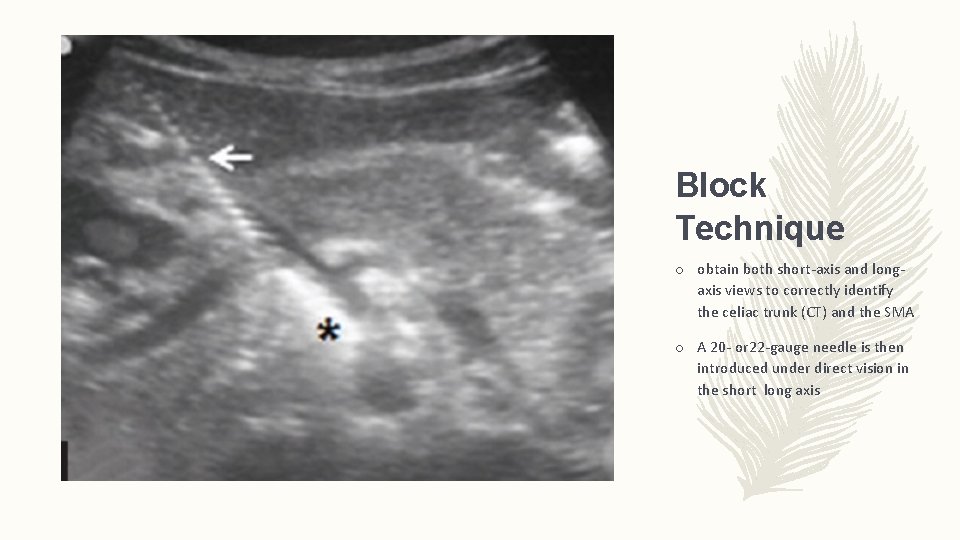
Block Technique o obtain both short-axis and longaxis views to correctly identify the celiac trunk (CT) and the SMA o A 20 - or 22 -gauge needle is then introduced under direct vision in the short long axis

Block Technique o survey scan identify the aorta, viscera including the liver, and the vertebral body o advance the needle from the lateral side of the transducer (short-axis view) to lie just cephalad to the origin of the CT and not between the CT and SMA

Block Technique o diagnostic or prognostic blocks a total of 12 to 15 m. L of local anesthetic is drawn up in a 20 -m. L sterile syringe o inflammatory component 40 to 80 mg of depot steroid is added to the local anesthetic o Neurolytic blocks 12 to 15 m. L of aqueous phenol or absolute alcohol

COMPLICATIONS o possibility of needle-induced trauma to the aorta, gastric artery, celiac trunk, superior mesenteric, and renal arteries o needle-induced trauma to abdominal viscera o Peritonitis and intraabdominal abscess o Post-block diarrhea occurs in ~50% of patients o Needle placement that is too posterior epidural, subdural, or subarachnoid injections or trauma to the spinal cord and exiting nerve roots neurologic deficits, paraplegia o Intra-discal placement discitis.

- Slides: 31