Ultrasound breast Kanjanaporn Mahatthanaphak Objectives 1 Indication of

Ultrasound breast Kanjanaporn Mahatthanaphak

Objectives 1. Indication of breast ultrasound 2. Technique of breast ultrasound 3. Ultrasound interpretation

Diagnosis of breast diseases • • History Physical examination Breast imaging Biopsy
Breast Imaging • • Mammography Ultrasonography (US) Magnetic resonance imaging (MRI) Nuclear medicine – Sentinel node (Tc 99 m-sulfur colloid) – Breast specific gamma imaging (Tc 99 m-sestamibi) – PET (positron emission tomogram)

Ultrasonography • • Advantage Cheap No radiation Non invasive Widely available Disadvantage • Need high resolution US for breast • Operator dependent

Indications for US 1. Differentiate cyst from solid mass 2. Palpable mass in women < 30 yrs, pregnant and lactation 3. Evaluate dense breast with palpable mass 4. Evaluation for breast abscess 5. Evaluation problem with breast implants 6. Interventional procedure 7. Evaluation for multicentric or multifocal CA, bilateral CA, axillary lymph node involvement 8. Evaluate focal asymmetry seen on mammogram 9. Breast cancer screening
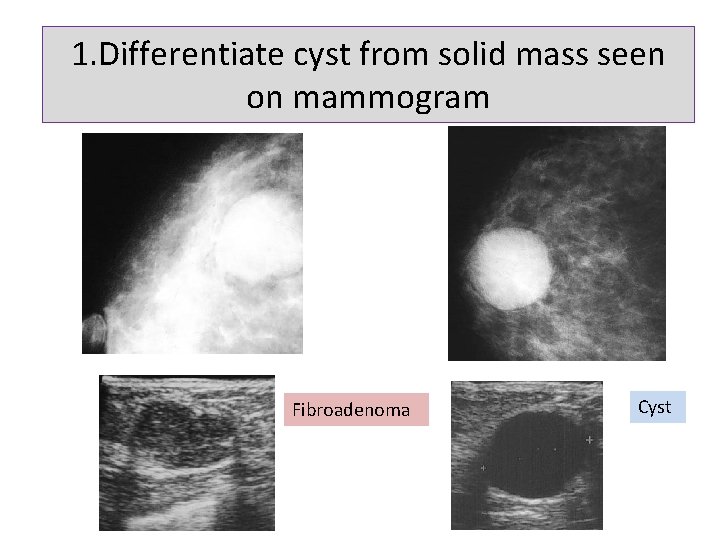
1. Differentiate cyst from solid mass seen on mammogram Fibroadenoma Cyst
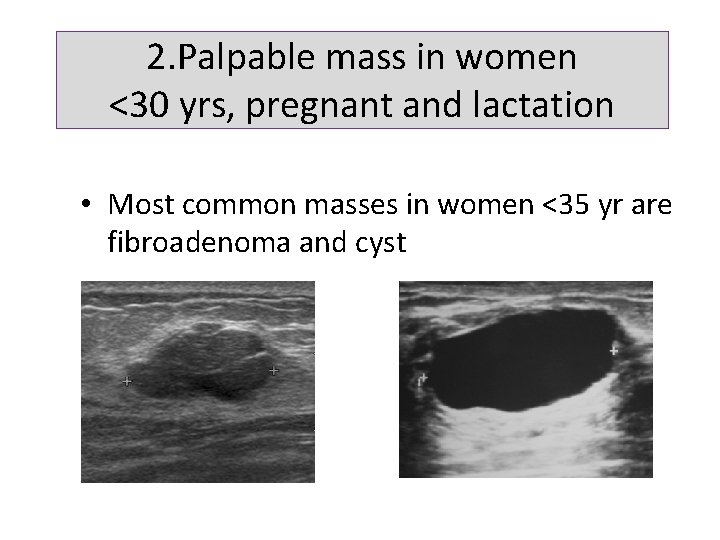
2. Palpable mass in women <30 yrs, pregnant and lactation • Most common masses in women <35 yr are fibroadenoma and cyst
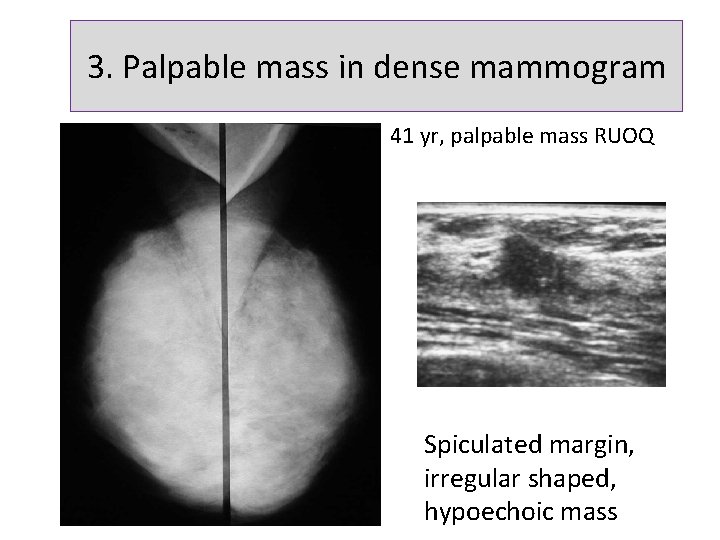
3. Palpable mass in dense mammogram 41 yr, palpable mass RUOQ Spiculated margin, irregular shaped, hypoechoic mass
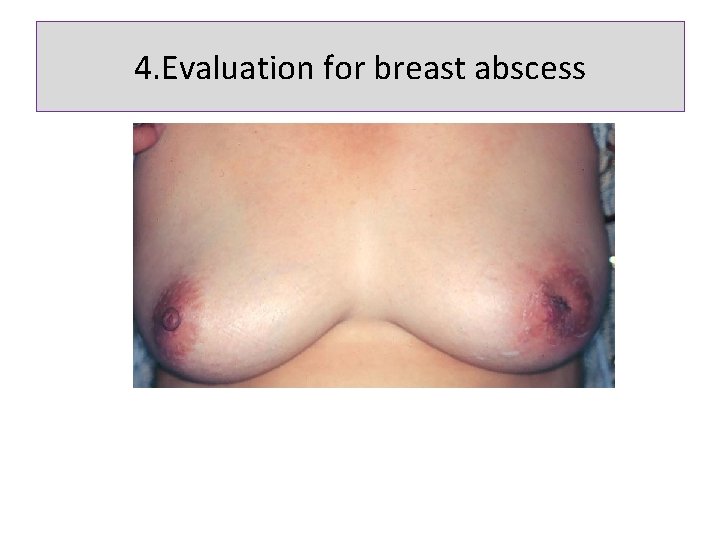
4. Evaluation for breast abscess

5. Evaluation problems with breast implants • Questionable implants leak or rupture • MRI is the best imaging modality • US can be used in substituition

6. Interventional procedure • • • Cyst aspiration Drainage Guided fine needle aspiration Guided core biopsy Mark skin for excisional biopsy

Drainage pus
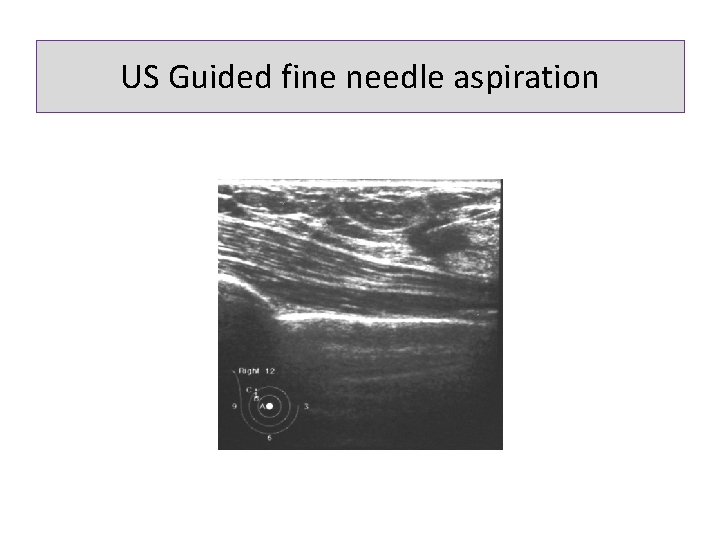
US Guided fine needle aspiration
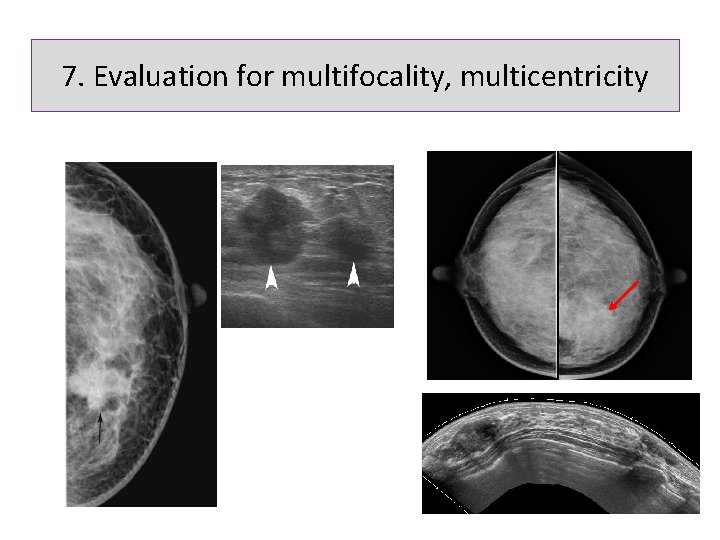
7. Evaluation for multifocality, multicentricity

8. Evaluation for focal asymmetrical density • Focal asymmetrical density could be from – Normal variation – Breast mass (benign, malignant) • Check if there is associated palpable mass
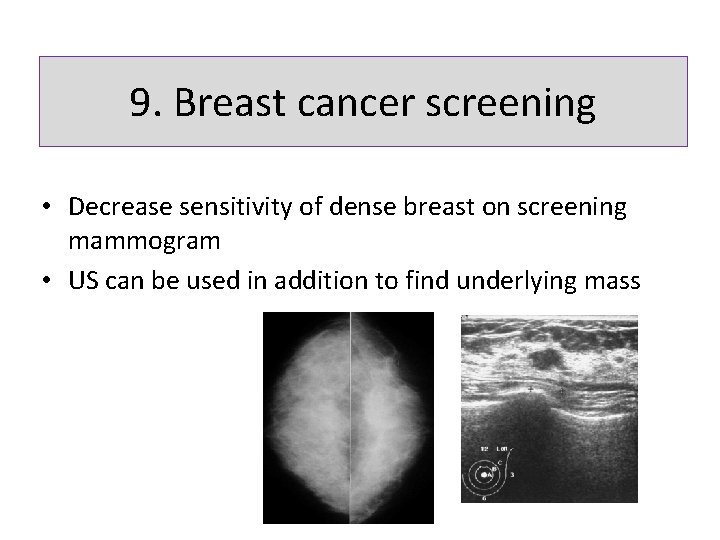
9. Breast cancer screening • Decrease sensitivity of dense breast on screening mammogram • US can be used in addition to find underlying mass

Ultrasound technique lighting patient positioning: support elbow, flat, supine ergonomics probe: linear array 7 -13 MHz scanning: radial/antiradial clock face with distance from nipple only caliper things that are REAL correct depth (skin to pectoral fascia) and correct focal zone (up to 2 is OK) • dynamic range: some settings can make a cystic lesion look solid and vice versa • •
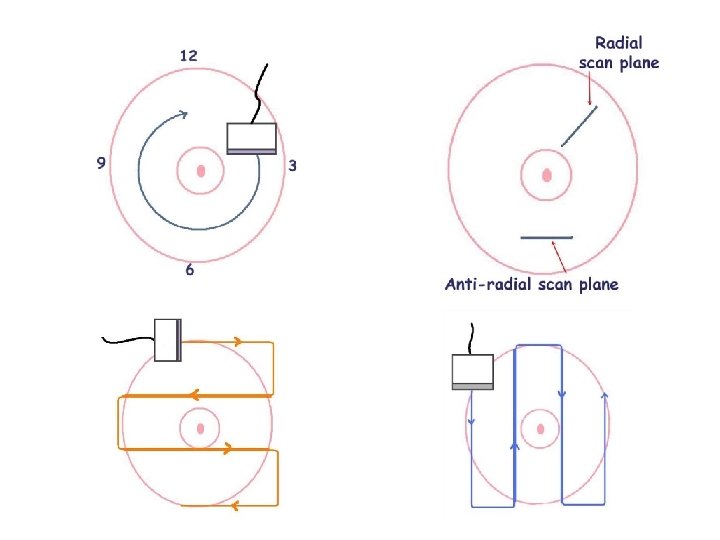
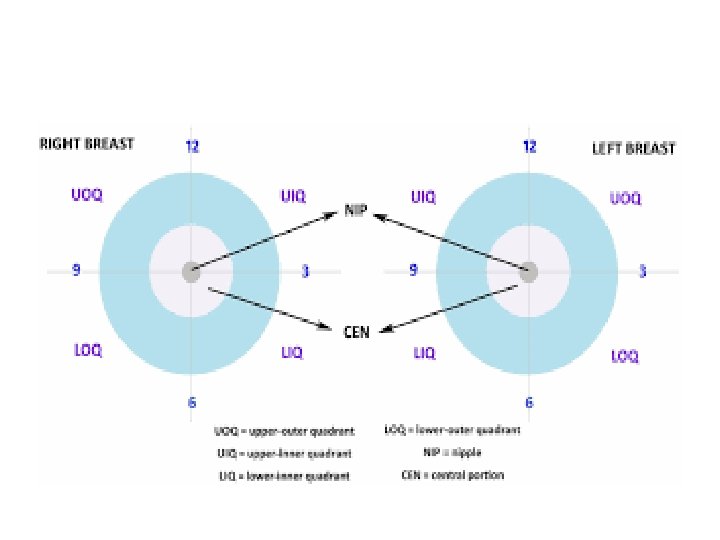
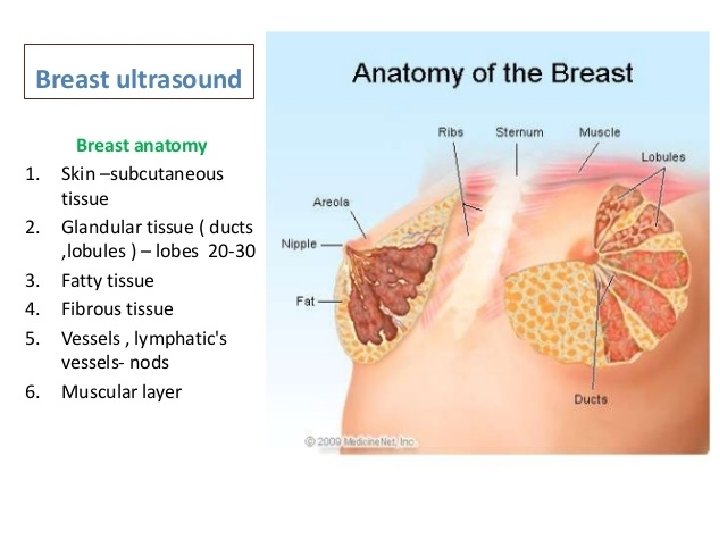
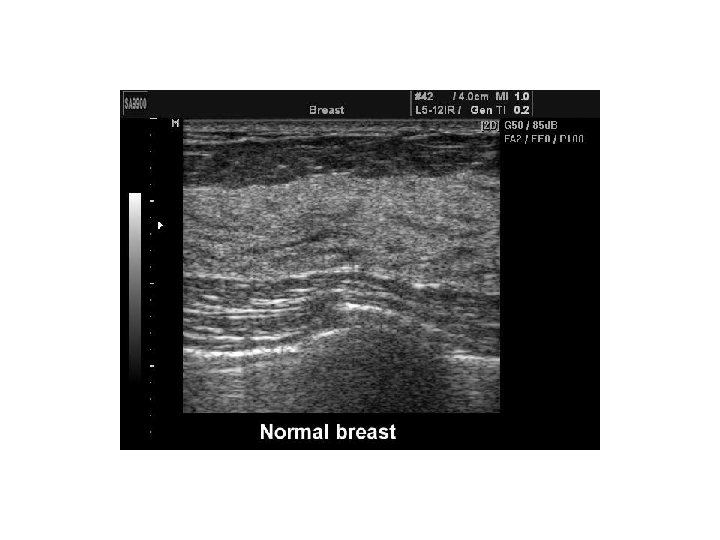

Ultrasound interpretation • • Breast Composition Mass Calcifications Associated features
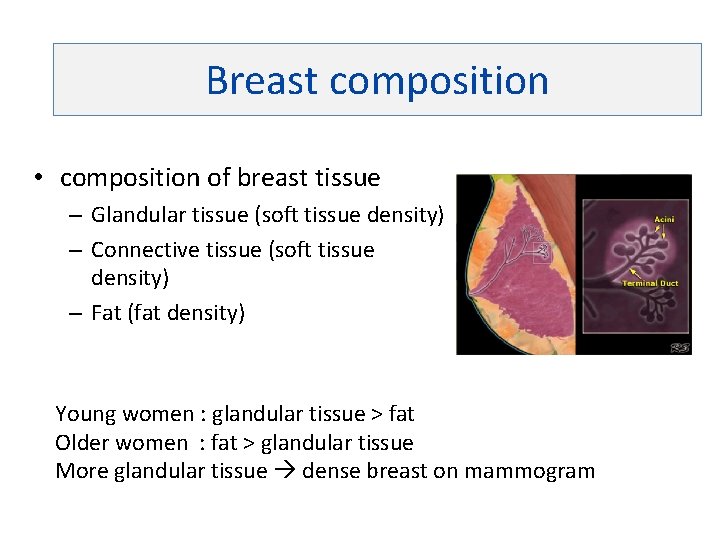
Breast composition • composition of breast tissue – Glandular tissue (soft tissue density) – Connective tissue (soft tissue density) – Fat (fat density) Young women : glandular tissue > fat Older women : fat > glandular tissue More glandular tissue dense breast on mammogram

Breast Composition: • Homogeneous echotexture - fat • Homogeneous echotexture - fibroglandular • Heterogeneous echotexture
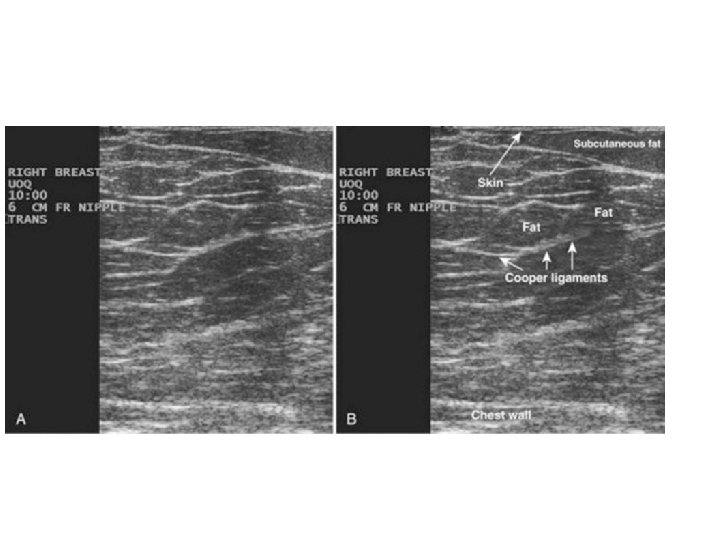
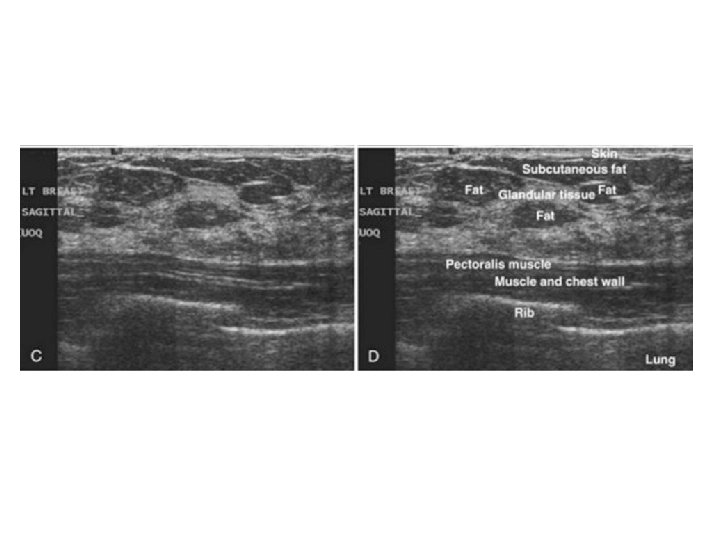
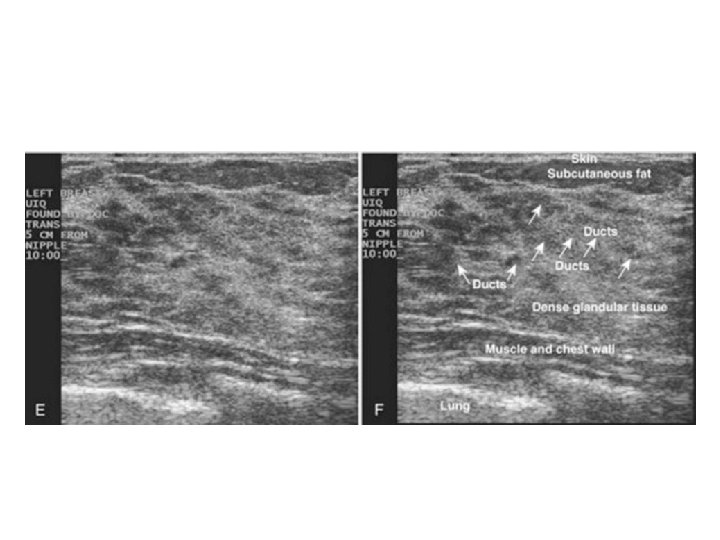
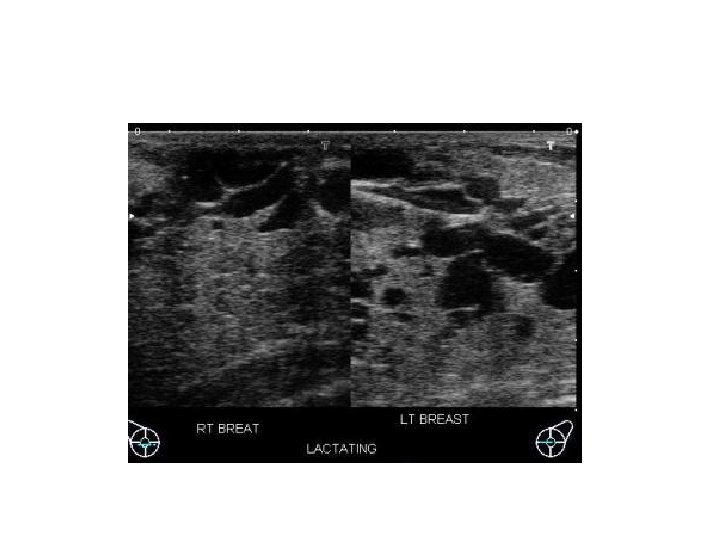

Mass • • • Shape Margin Orientation Echo pattern Posterior features
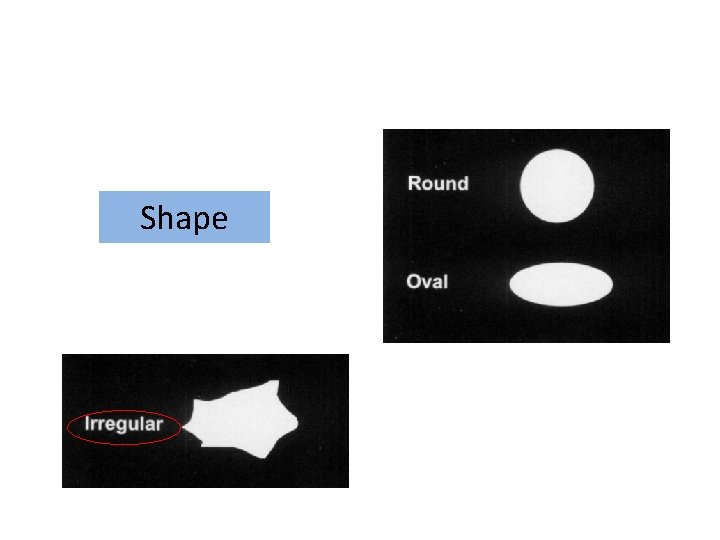
Breast mass Shape
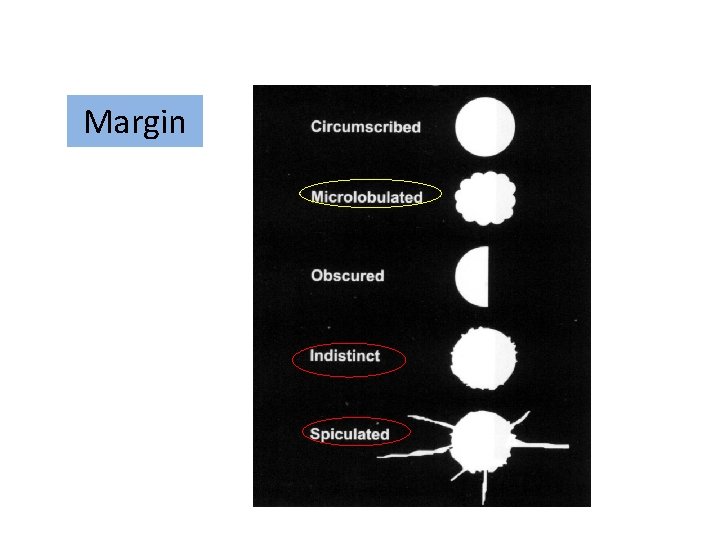
Breast mass Margin

Orientation: • unique to US-imaging, and defined as parallel (benign) or not parallel (suspicious finding) to the skin.

Echo pattern • • Anechoic Hypoechoic, Complex cystic Solid: isoechoic, hyperechoic, heterogeneous.

Posterior features: • Enhancement • Shadowing.

Calcifications: • On US poorly characterized compared with mammography, but can be recognized as echogenic foci, particularly when in a mass.

Associated features: • • • Architectural distortion Duct changes Skin changes Edema Vascularity Elasticity assessment

Findings suggestive of malignancy • Spiculation or thick echogenic halo • Angular margin • Microlobulation • Shape taller than wide • Duct extension or branch pattern • Acoustic shadowing • Microcalcifications • Hypoechogenicity

Findings suggestive of benign • • • No suggestive findings of malignancy Hyperechogenicity (compare to fat) Wider than tall Well circumscribed, less than 3 lobulations Thin echogenic pseudocapsule

Ultrasound Features Suggestive of Benign and Malignant Nodules. Feature Benign Malignant Shape Round, wider than tall Taller than wide Margins Smooth Irregular, angular, spicular Lobulations None or up to 3 Multiple Capsule Encapsulated No capsule Halo Absent Echogenic halo Fixity None Fixed to surrounding issue and/or underlying muscles Shadowing or enhancement Enhancement, edge shadowing Shadowing behind lesion Substance echogenicity Anechoic (cystic), Hyperechoic Hypoechoic, calcification

Special cases with a unique diagnosis or pathognomonic ultrasound appearance: • Simple cyst • Complicated cyst • Clustered microcysts • Mass in or on skin • Foreign body including implants • Lympnodes- intramammary • Lymph nodes- axillary • Vascular abnormalities • Postsurgical fluid collection • Fat necrosis
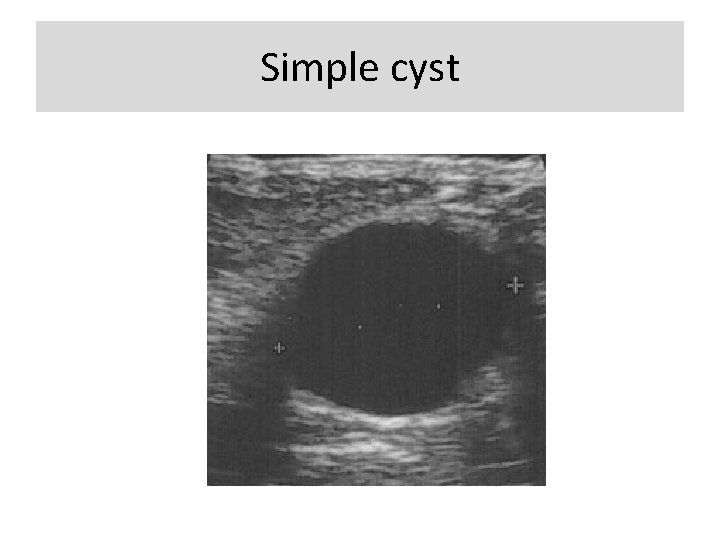
Simple cyst
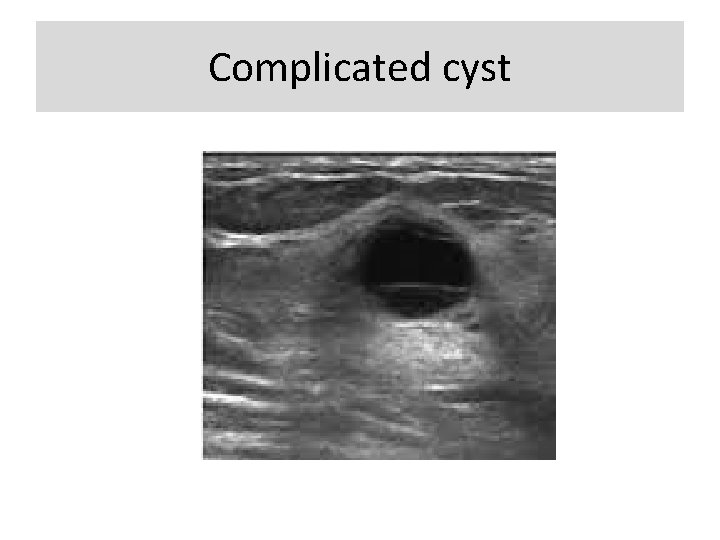
Complicated cyst
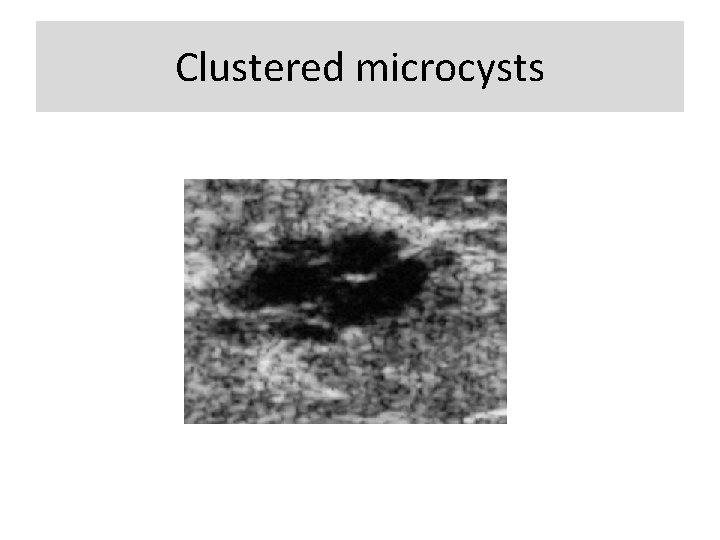
Clustered microcysts
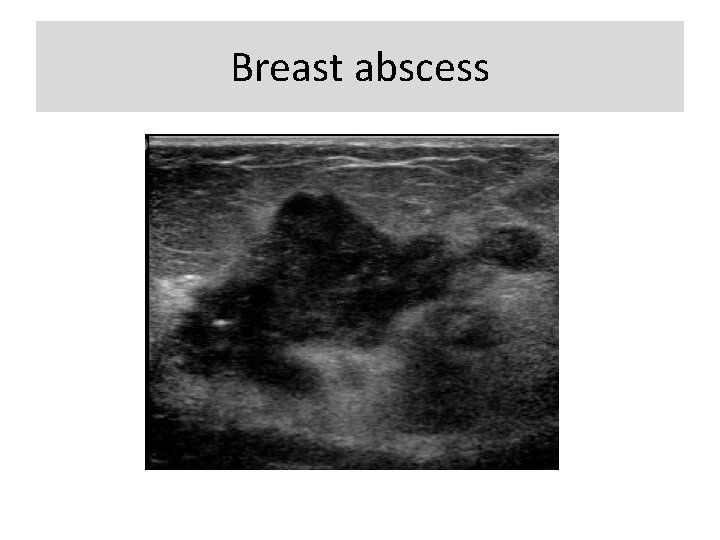
Breast abscess
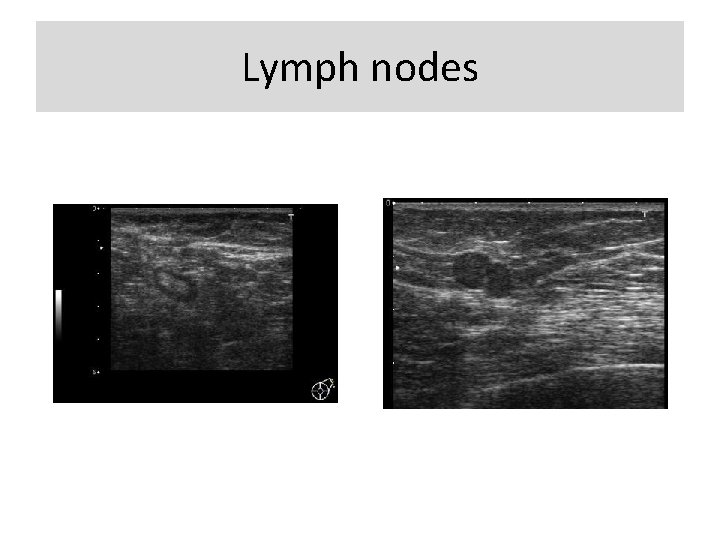
Lymph nodes
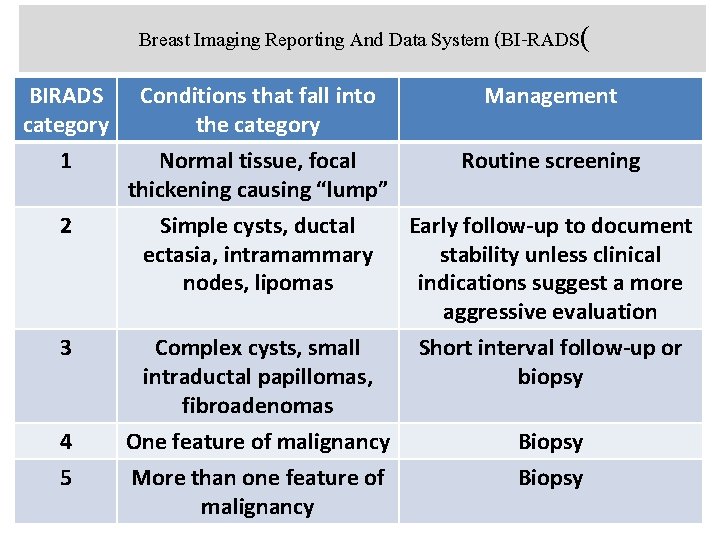
Breast Imaging Reporting And Data System (BI-RADS( BIRADS category 1 Conditions that fall into the category Normal tissue, focal thickening causing “lump” 2 Simple cysts, ductal ectasia, intramammary nodes, lipomas 3 Complex cysts, small intraductal papillomas, fibroadenomas One feature of malignancy More than one feature of malignancy 4 5 Management Routine screening Early follow-up to document stability unless clinical indications suggest a more aggressive evaluation Short interval follow-up or biopsy Biopsy

Breast Imaging Reporting And Data System (BI-RADS) Mammography Help clinicians for management § Category 0. . . incomplete assessment additional imaging is needed § Category I. . . negative routine follow up (1 year) § Category II … benign finding routine follow up (1 year) § Category III … probably benign finding follow up 6 months § Category IV … suspicious abnormality biopsy § Category V… highly suggestive of malignancy biopsy § Category VI …known biopsy proven malignancy appropriate treatment

• http: //www. radiologyassistant. nl/
- Slides: 50