Ultrasonographic anatomy of the pelvis including its 3





















- Slides: 72


Ultrasonographic anatomy of the pelvis including its 3 D aspects Frédéric Chantraine, ULg

Introduction • Anatomy of the pelvis • Ultrasound techniques • Female organs in the pelvis • Uterus • Ovaries • Fallopian Tubes

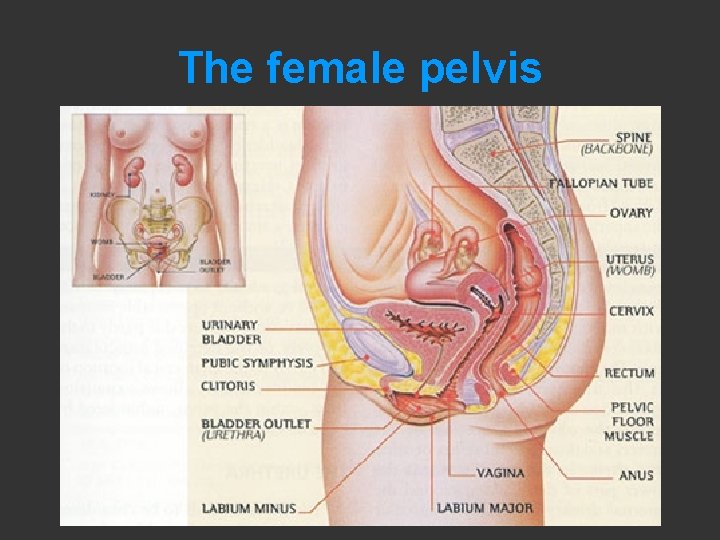
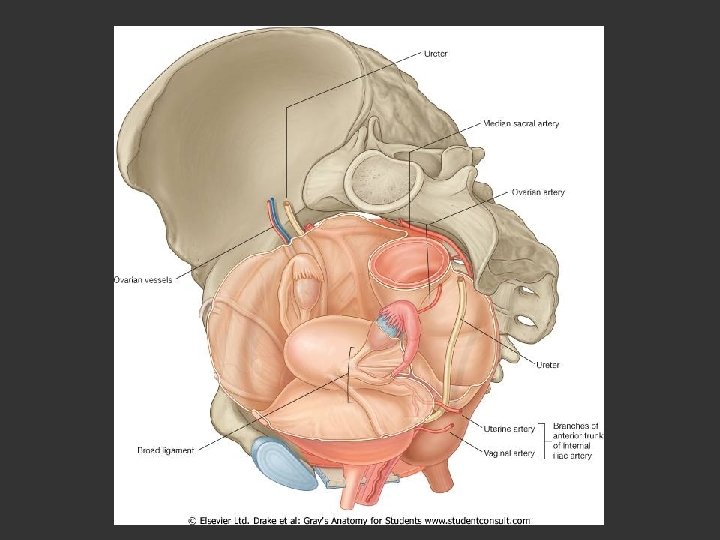
The female pelvis


And in ultrasound? • Different approaches: – Transvaginal • Bladder is empty – Transabdominal • Bladder is filled – Transrectal – Transperineal

And in ultrasound? • Different techniques – Classic “ 2 D” – Colour and Pulsed Doppler – Volumetric “ 3 D”

Uterus

Uterus • Organ of reference in the pelvis • Different orientation – Ante-, retroflexion – Ante-, retroversion • Three main parts – Corpus – Isthmus – Cervix

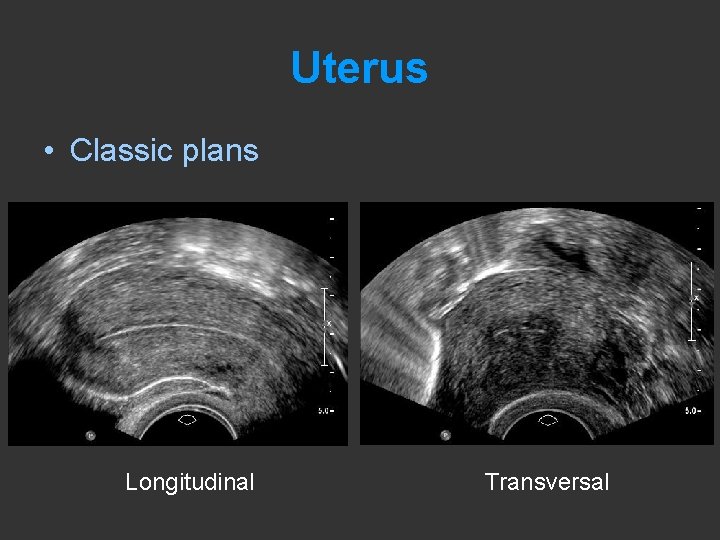
Uterus • Classic plans Longitudinal Transversal

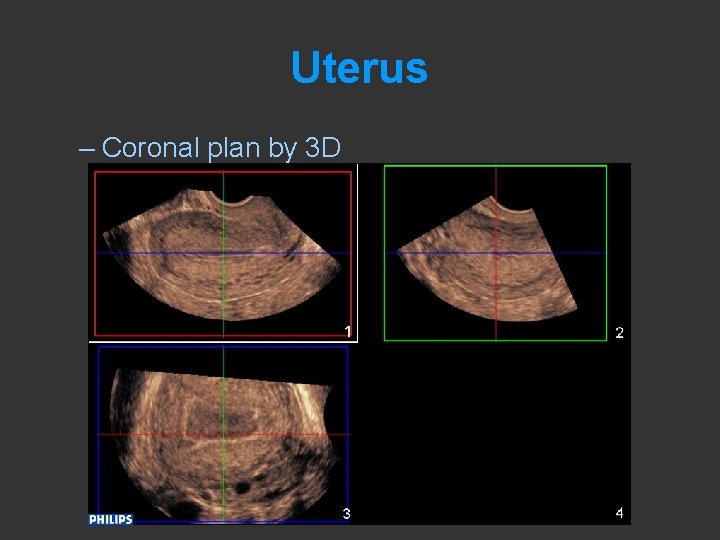
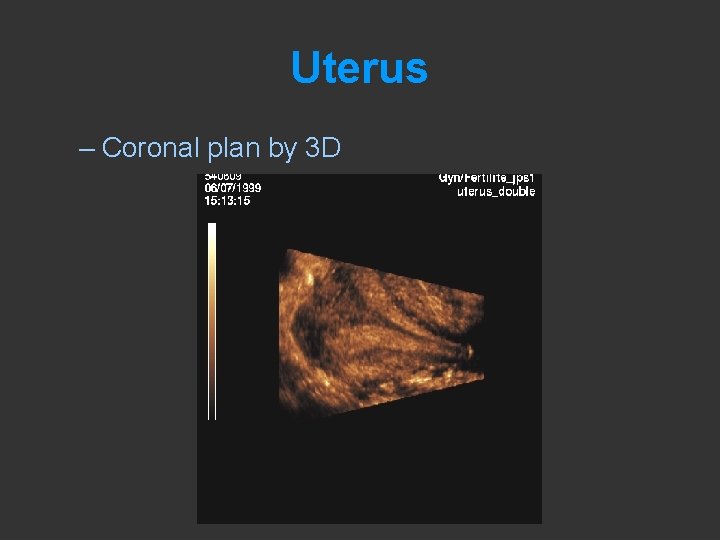
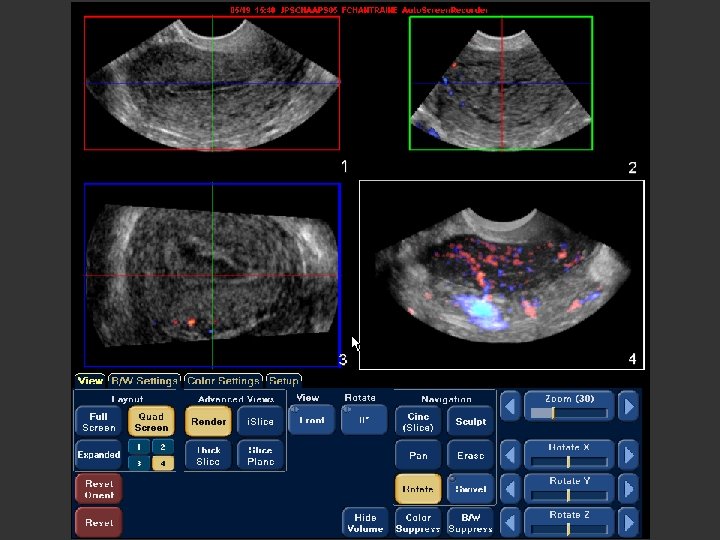
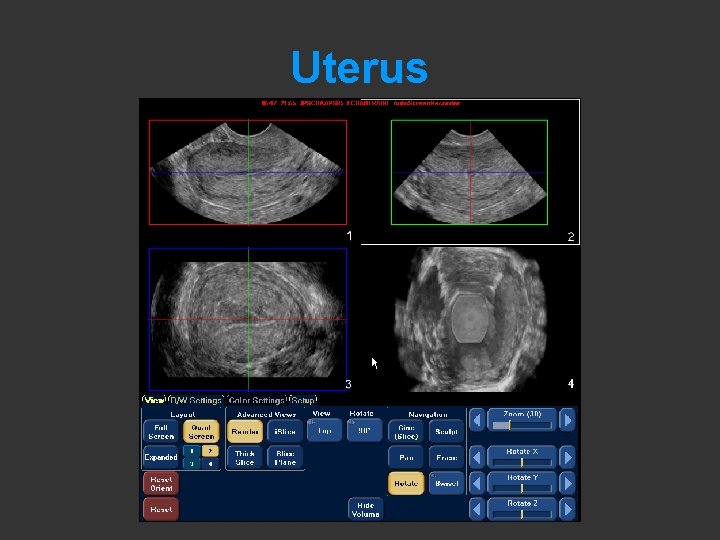
Uterus – Coronal plan by 3 D

Uterus – Coronal plan by 3 D

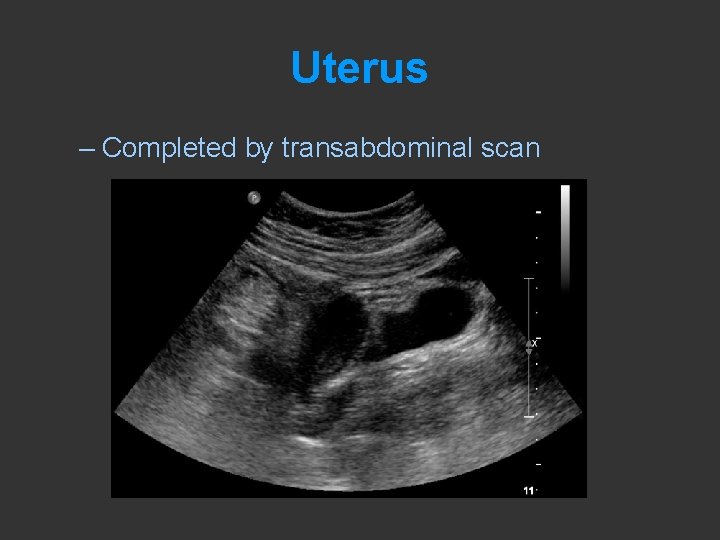
Uterus – Completed by transabdominal scan

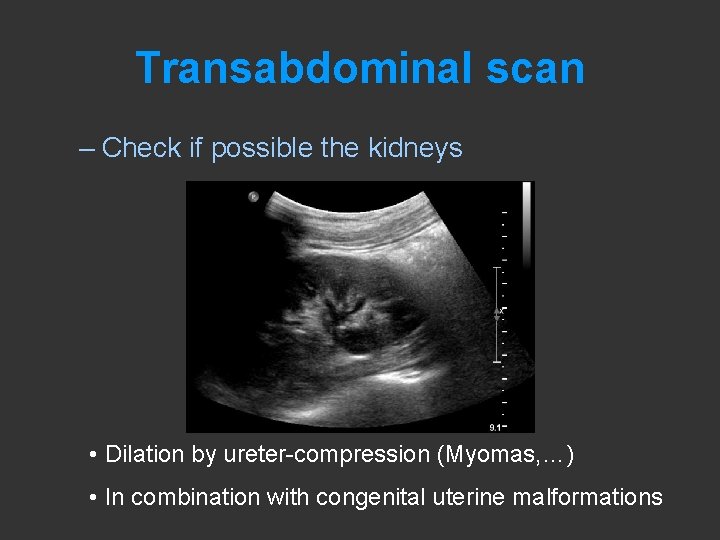
Transabdominal scan – Check if possible the kidneys • Dilation by ureter-compression (Myomas, …) • In combination with congenital uterine malformations

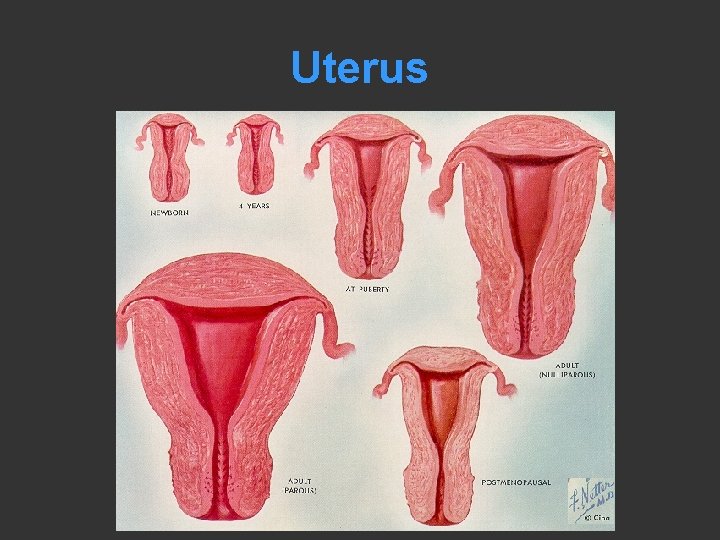
Uterus • Volume depends – Patient age – Number of gestations – Endocrinal level

Uterus

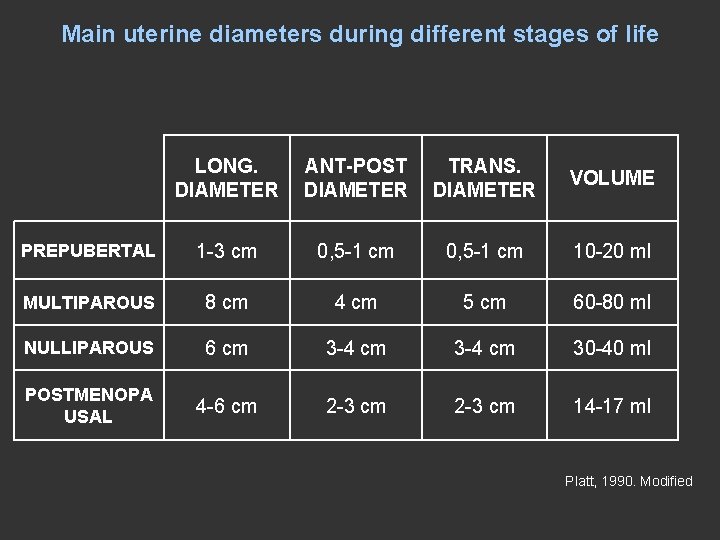
Main uterine diameters during different stages of life LONG. DIAMETER ANT-POST DIAMETER TRANS. DIAMETER VOLUME PREPUBERTAL 1 -3 cm 0, 5 -1 cm 10 -20 ml MULTIPAROUS 8 cm 4 cm 5 cm 60 -80 ml NULLIPAROUS 6 cm 3 -4 cm 30 -40 ml POSTMENOPA USAL 4 -6 cm 2 -3 cm 14 -17 ml Platt, 1990. Modified

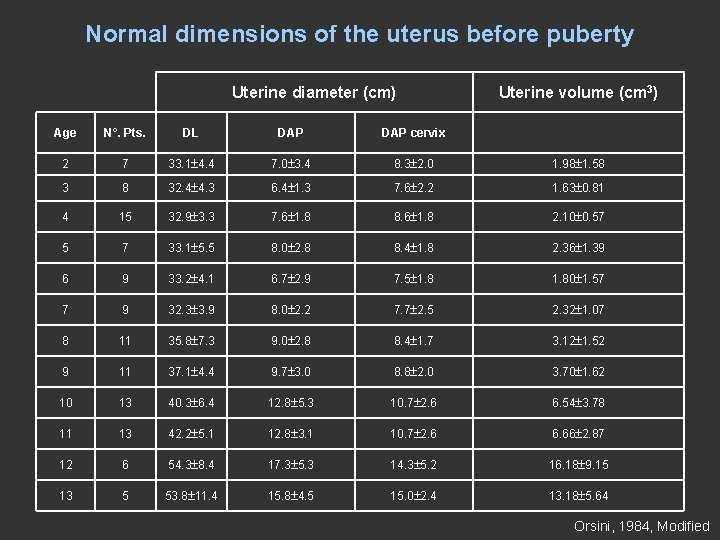
Normal dimensions of the uterus before puberty Uterine diameter (cm) Uterine volume (cm 3) Age N°. Pts. DL DAP cervix 2 7 33. 1 4. 4 7. 0 3. 4 8. 3 2. 0 1. 98 1. 58 3 8 32. 4 4. 3 6. 4 1. 3 7. 6 2. 2 1. 63 0. 81 4 15 32. 9 3. 3 7. 6 1. 8 8. 6 1. 8 2. 10 0. 57 5 7 33. 1 5. 5 8. 0 2. 8 8. 4 1. 8 2. 36 1. 39 6 9 33. 2 4. 1 6. 7 2. 9 7. 5 1. 80 1. 57 7 9 32. 3 3. 9 8. 0 2. 2 7. 7 2. 5 2. 32 1. 07 8 11 35. 8 7. 3 9. 0 2. 8 8. 4 1. 7 3. 12 1. 52 9 11 37. 1 4. 4 9. 7 3. 0 8. 8 2. 0 3. 70 1. 62 10 13 40. 3 6. 4 12. 8 5. 3 10. 7 2. 6 6. 54 3. 78 11 13 42. 2 5. 1 12. 8 3. 1 10. 7 2. 6 6. 66 2. 87 12 6 54. 3 8. 4 17. 3 5. 3 14. 3 5. 2 16. 18 9. 15 13 5 53. 8 11. 4 15. 8 4. 5 15. 0 2. 4 13. 18 5. 64 Orsini, 1984, Modified

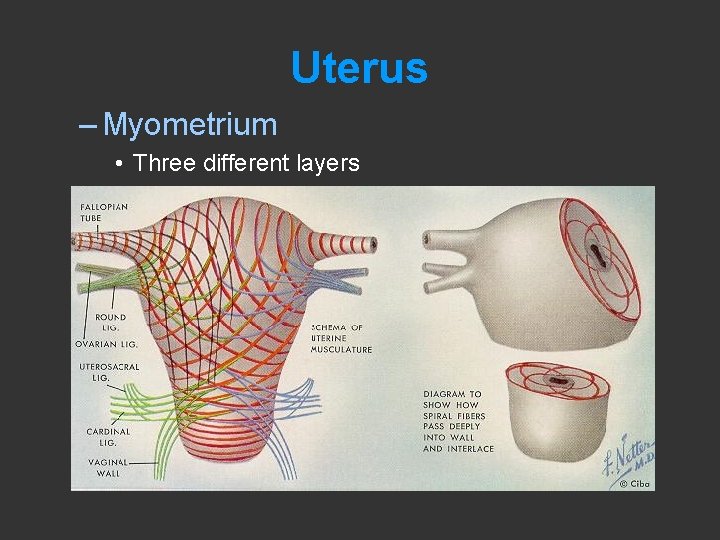
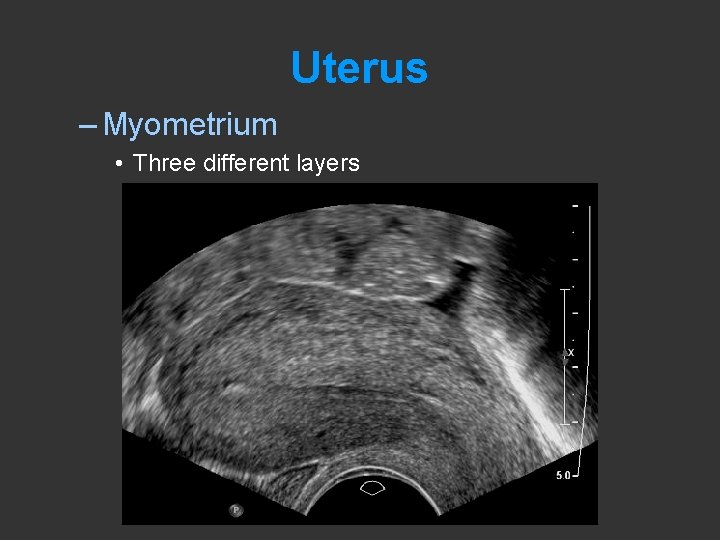
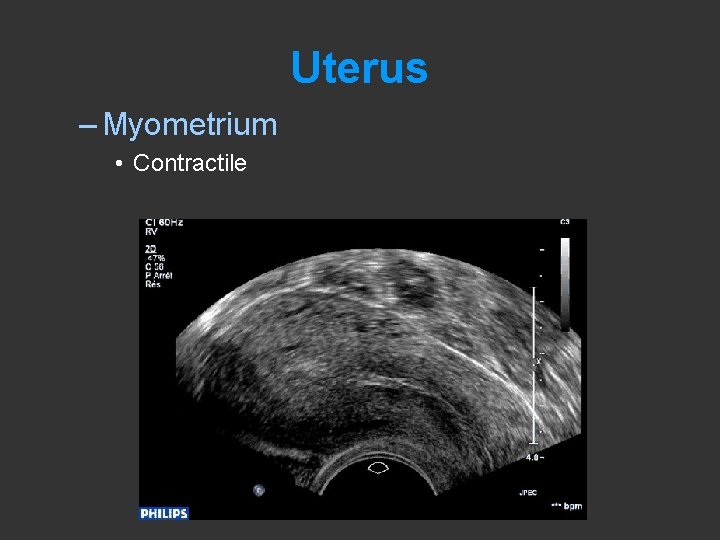
Uterus – Myometrium • Three different layers

Uterus – Myometrium • Three different layers

Uterus – Myometrium • Contractile • bjl

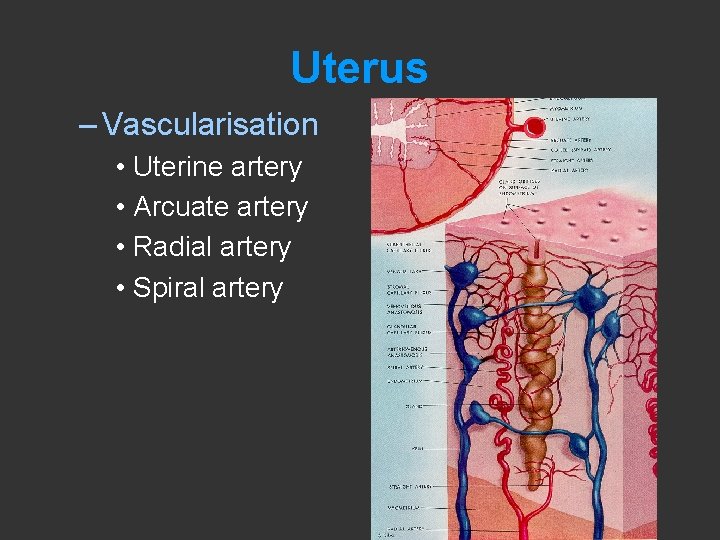
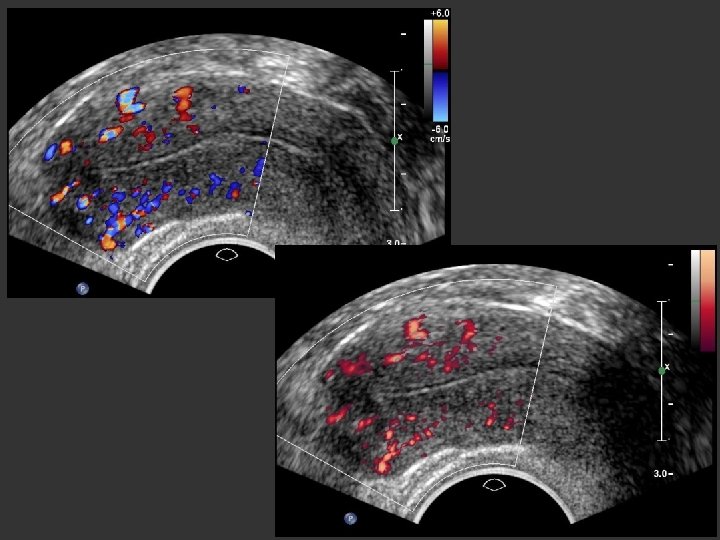
Uterus – Vascularisation • Uterine artery • Arcuate artery • Radial artery • Spiral artery


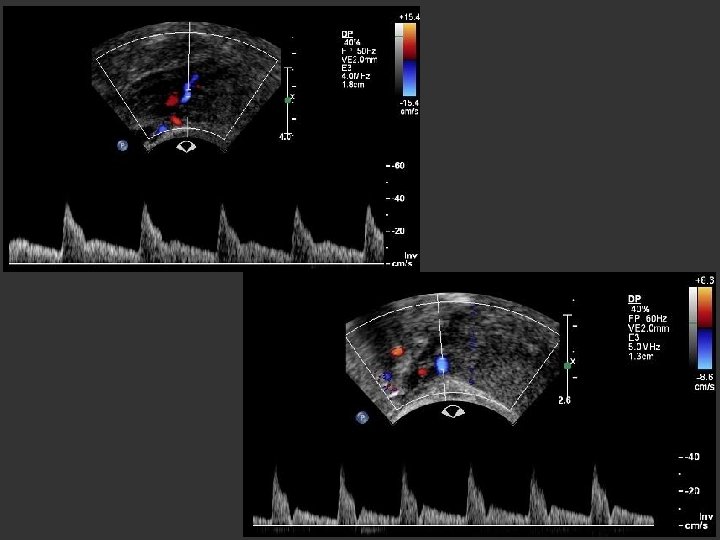
Uterus – Doppler of the uterine artery • Systole: high velocity peak • Diastole: lower flow • Telesystolic Notch • Changes during menstrual cycle



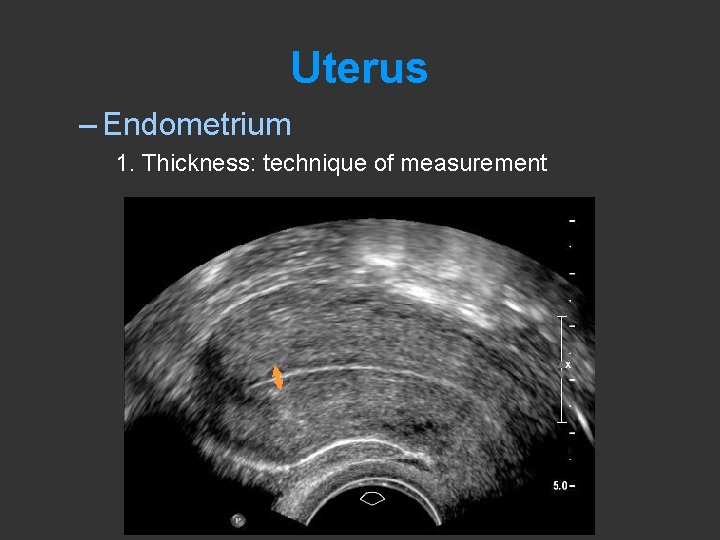
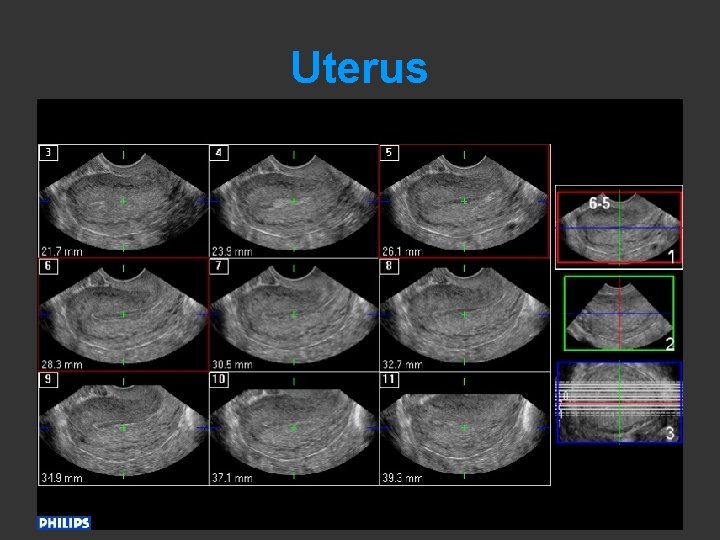
Uterus – Endometrium 1. Thickness: technique of measurement

Uterus

Uterus

Uterus – Endometrium 2. Echostructure – Patients age – Moment of the spontaneous cycle – Eventual hormonal treatment

Uterus –Endometrium • Prepubertal age – Newborn: thickened and hyperechogenic – Up to menarch: thin, <1 mm – Useful in diagnosis of early or delayed puberty • Reproductive age

Uterus – Endometrium • Range of normal endometrial thicknesses THICKNESS (mm) PROLIFERATIVE PHASE 4 -8 PERIOVULATORY PHASE 6 -10 SECRETIVE PHASE 7 -14 POSTMENOPAUSAL PHASE <6

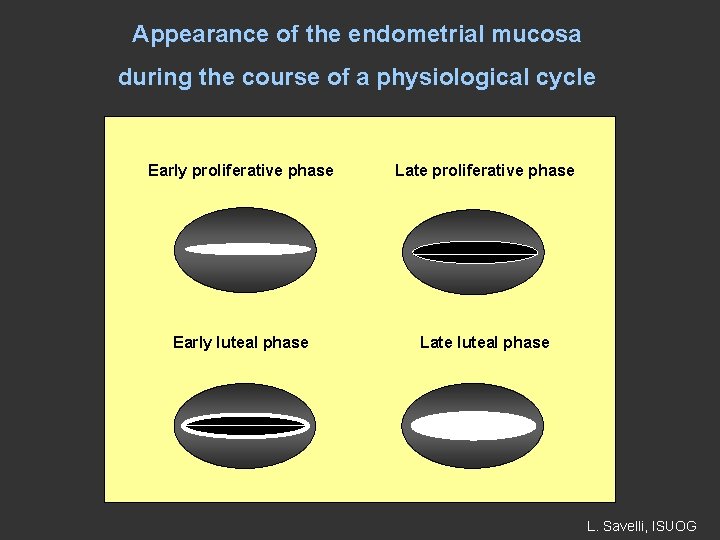
Appearance of the endometrial mucosa during the course of a physiological cycle Early proliferative phase Late proliferative phase Early luteal phase Late luteal phase L. Savelli, ISUOG

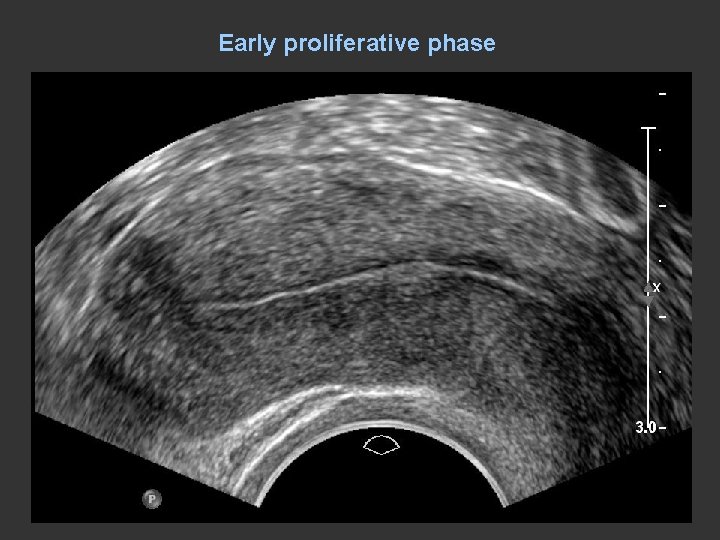
Early proliferative phase

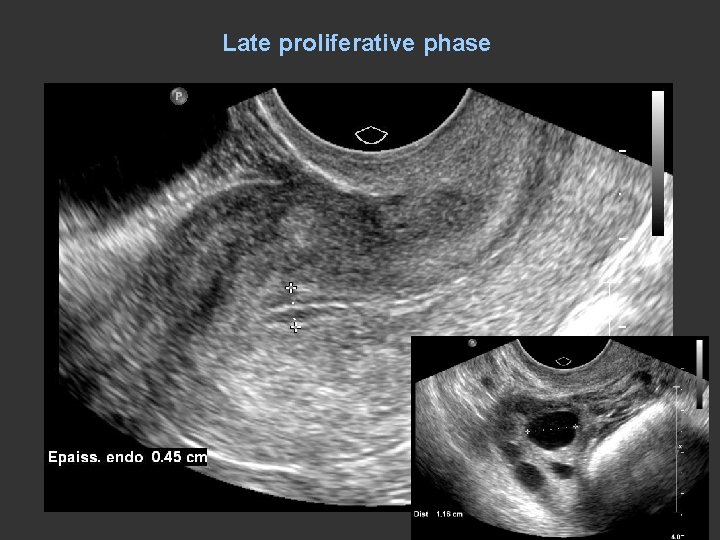
Late proliferative phase

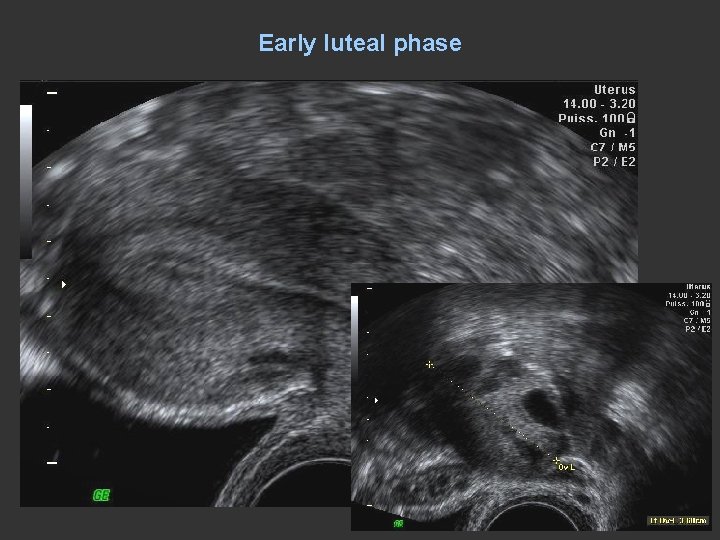
Early luteal phase

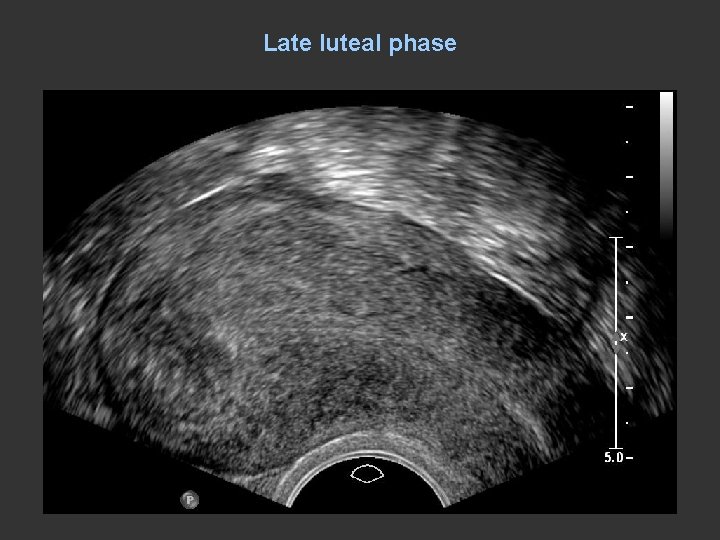
Late luteal phase

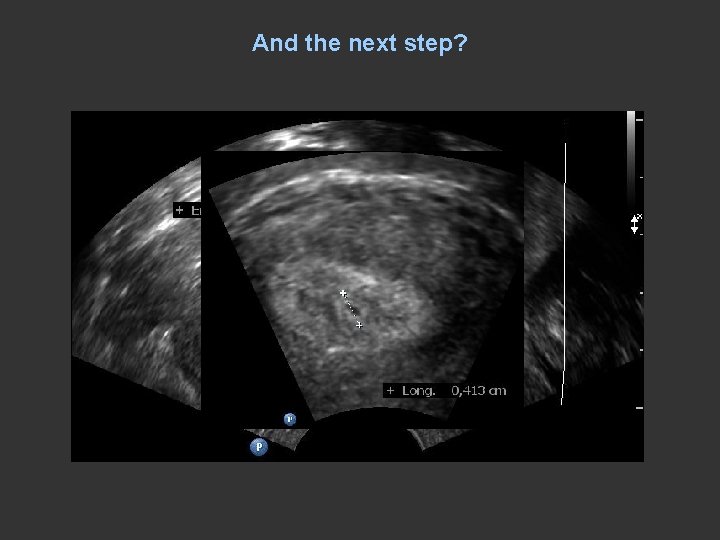
And the next step?

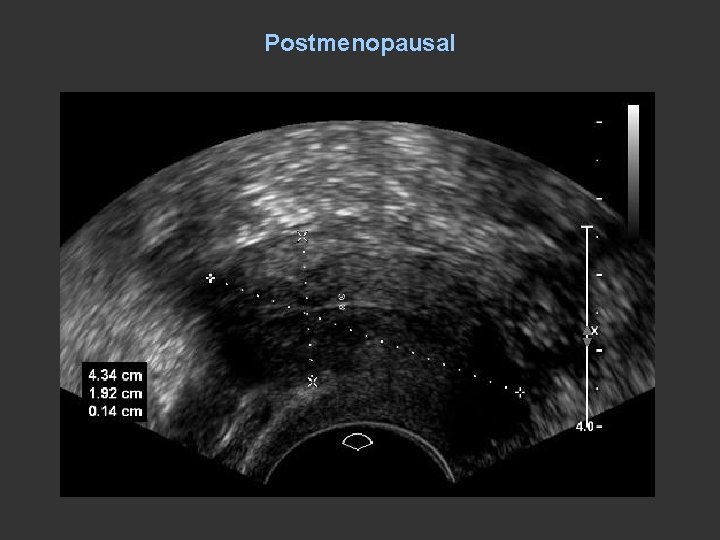
Postmenopausal

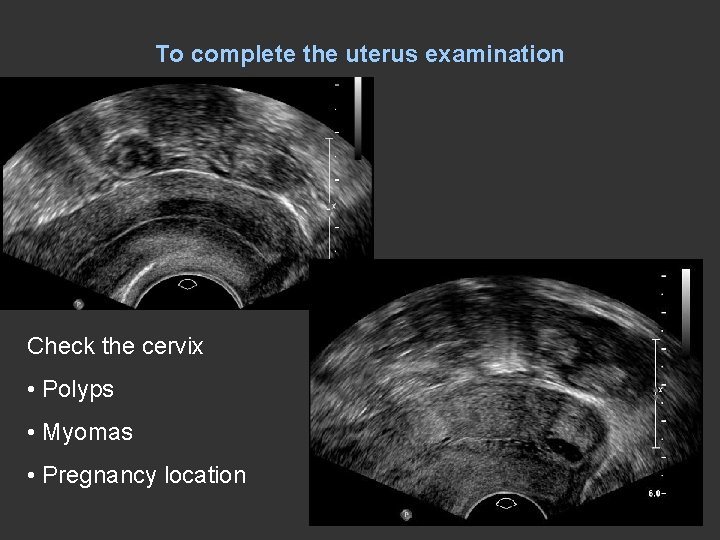
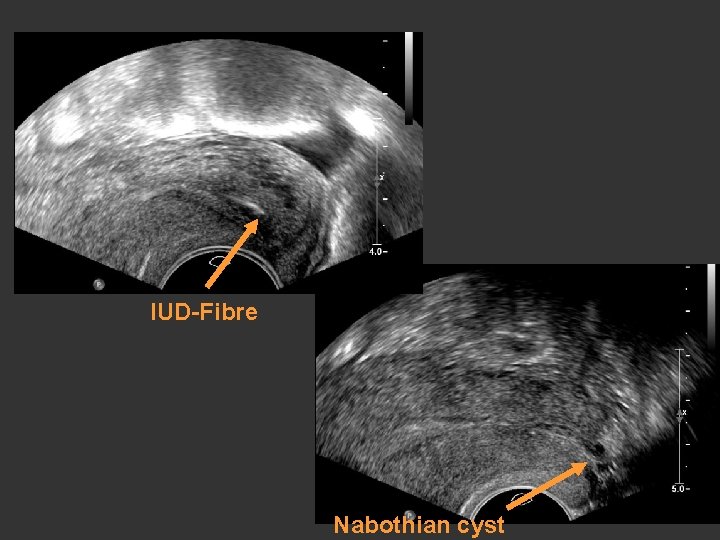
To complete the uterus examination Check the cervix • Polyps • Myomas • Pregnancy location

IUD-Fibre Nabothian cyst

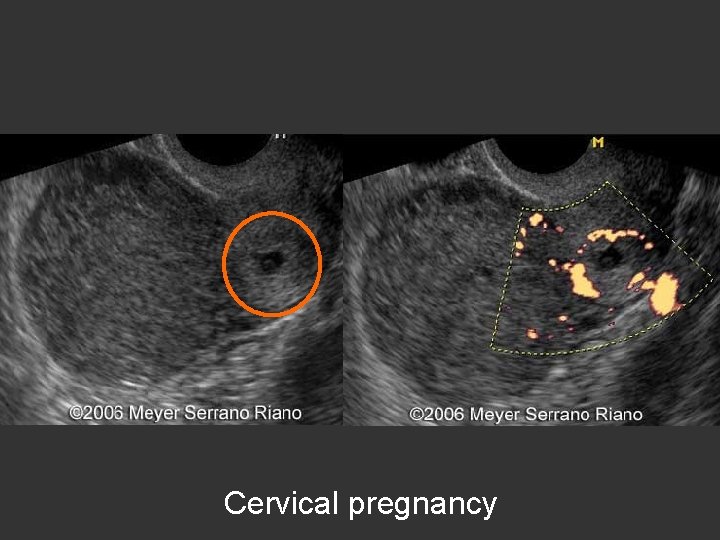
Cervical pregnancy


Ovary

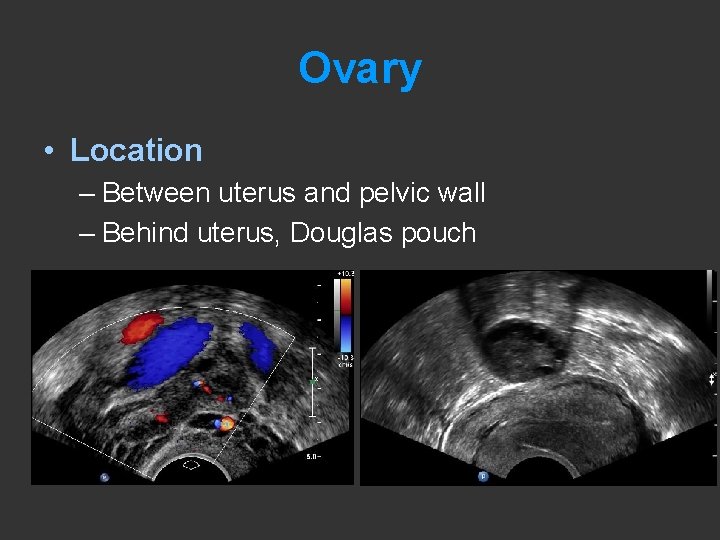
Ovary • Location – Between uterus and pelvic wall – Behind uterus, Douglas pouch

Ovary • Dimension – Pré-ménopause: 3, 5 x 2 x 1, 5 cm – Post-ménopause: 1, 5 x 0, 7 cm • Morphology – Patient age – Moment of the menstrual cycle

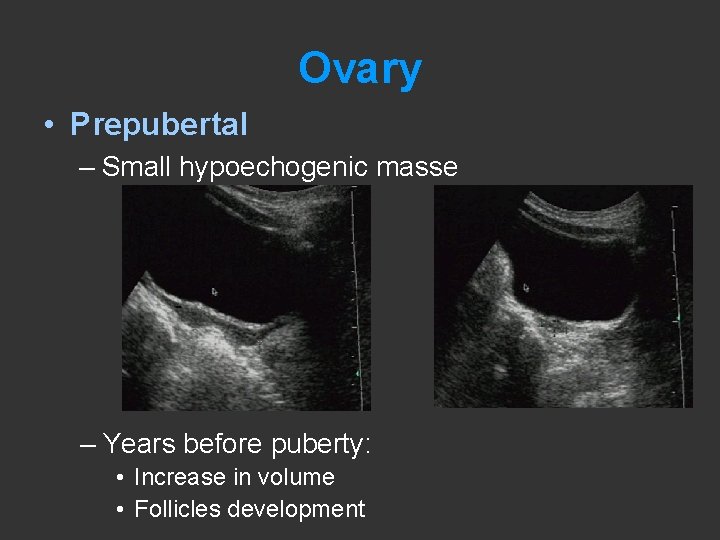
Ovary • Prepubertal – Small hypoechogenic masse – Years before puberty: • Increase in volume • Follicles development

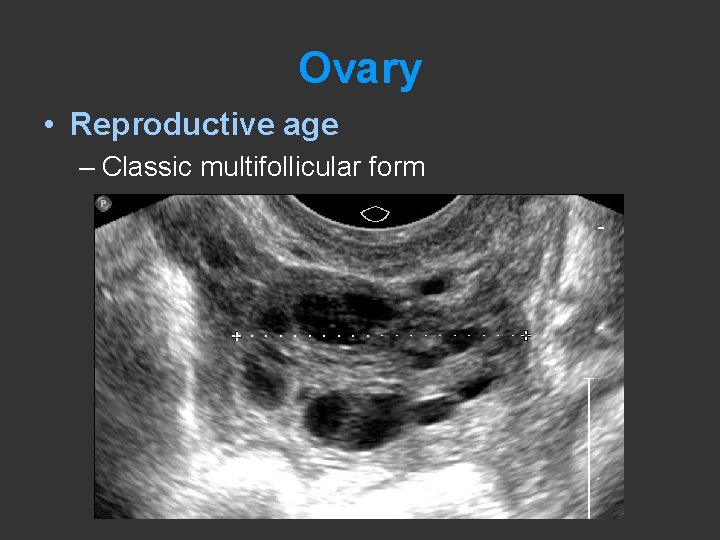
Ovary • Reproductive age – Classic multifollicular form

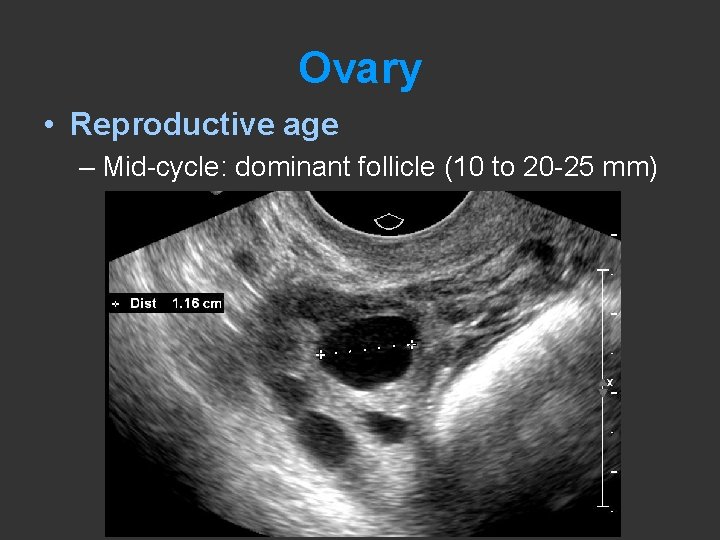
Ovary • Reproductive age – Mid-cycle: dominant follicle (10 to 20 -25 mm)

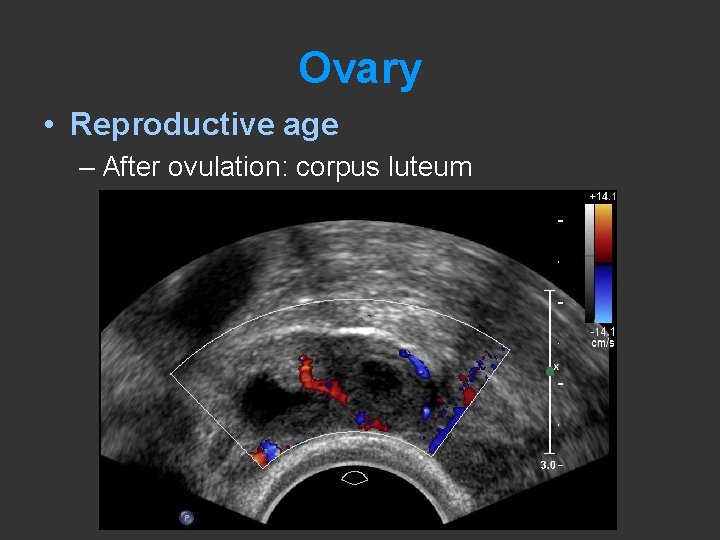
Ovary • Reproductive age – After ovulation: corpus luteum

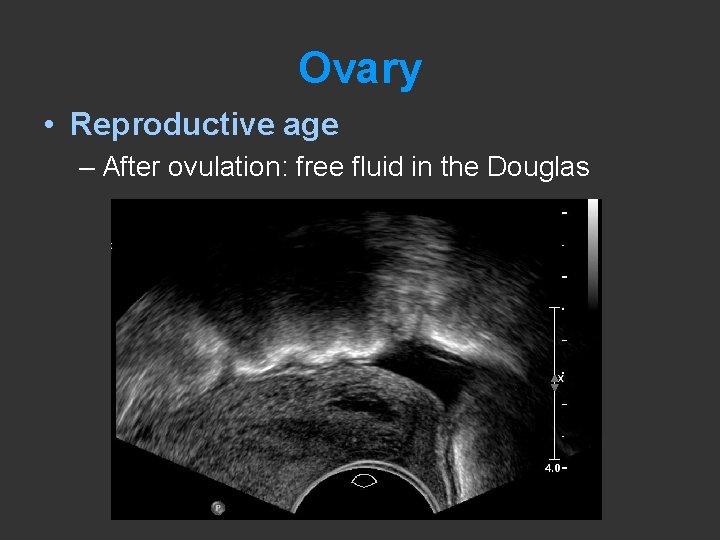
Ovary • Reproductive age – After ovulation: free fluid in the Douglas

Ovary • Reproductive age – Functional cysts

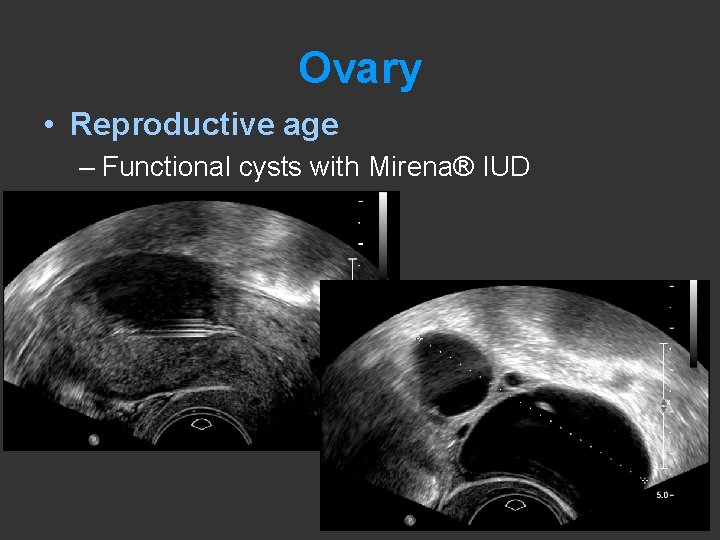
Ovary • Reproductive age – Functional cysts with Mirena® IUD

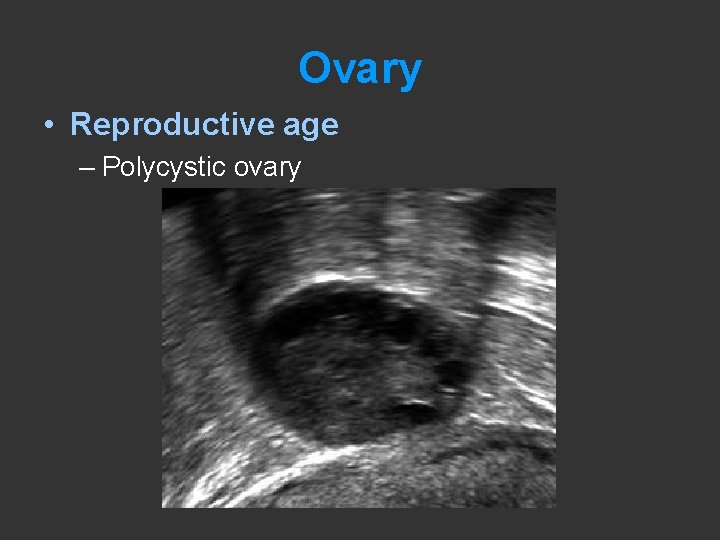
Ovary • Reproductive age – Polycystic ovary

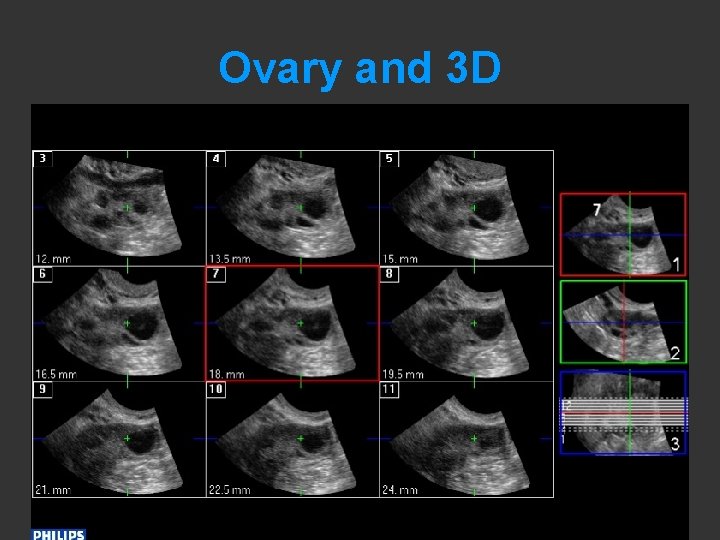
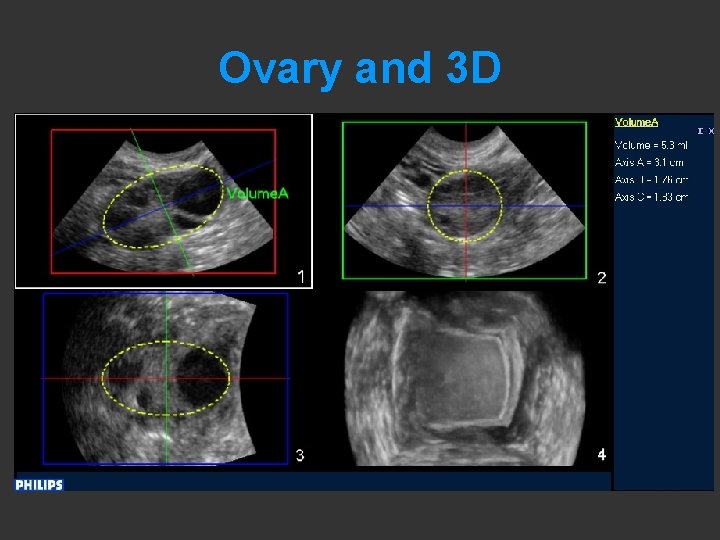
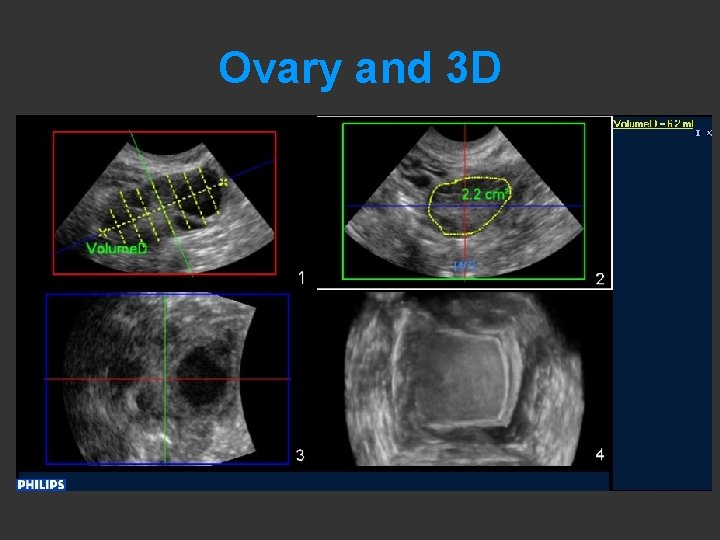
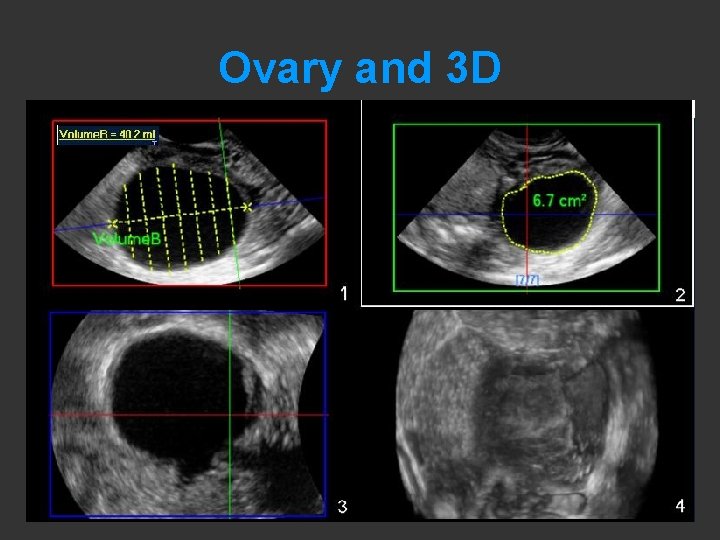
Ovary and 3 D

Ovary and 3 D

Ovary and 3 D

Ovary and 3 D

Ovary and 3 D

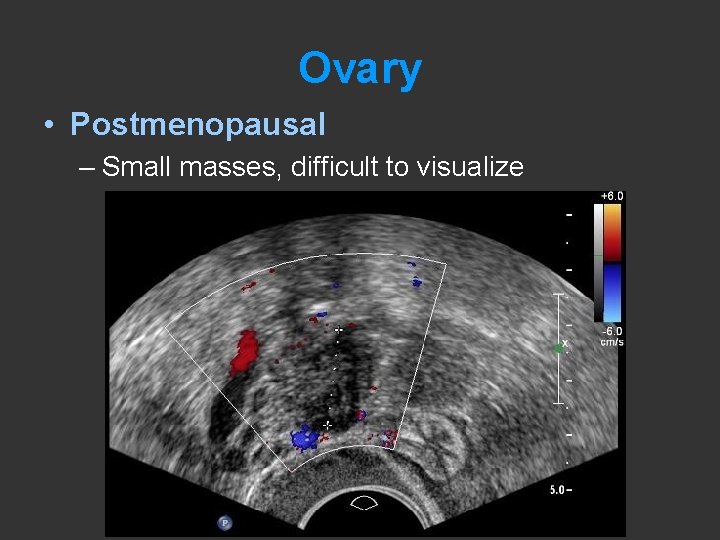
Ovary • Postmenopausal – Small masses, difficult to visualize

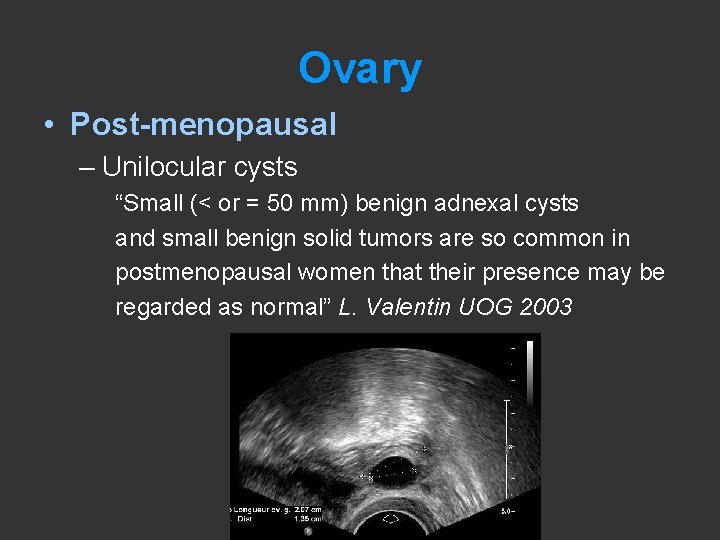
Ovary • Post-menopausal – Unilocular cysts “Small (< or = 50 mm) benign adnexal cysts and small benign solid tumors are so common in postmenopausal women that their presence may be regarded as normal” L. Valentin UOG 2003

Fallopian Tubes

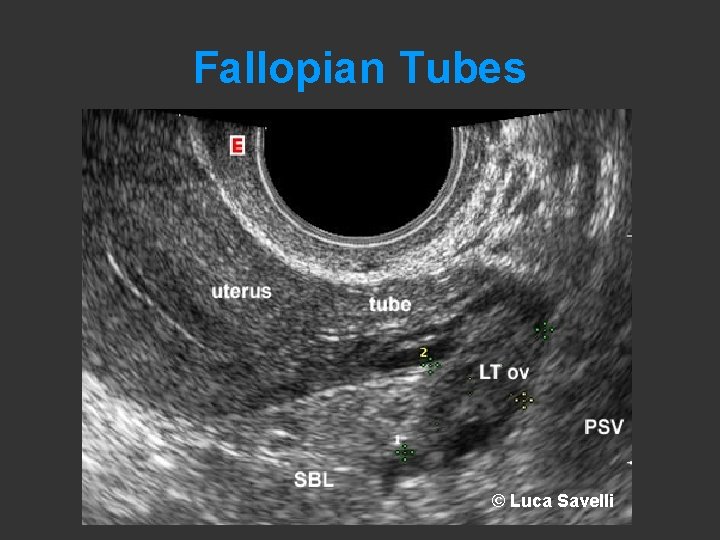
Fallopian Tubes • Anatomy – Interstitielle – Isthmus – Ampulla • Difficult to visualize – Fluid around – Hydrosalpinx

Fallopian Tubes © Luca Savelli

And what else?


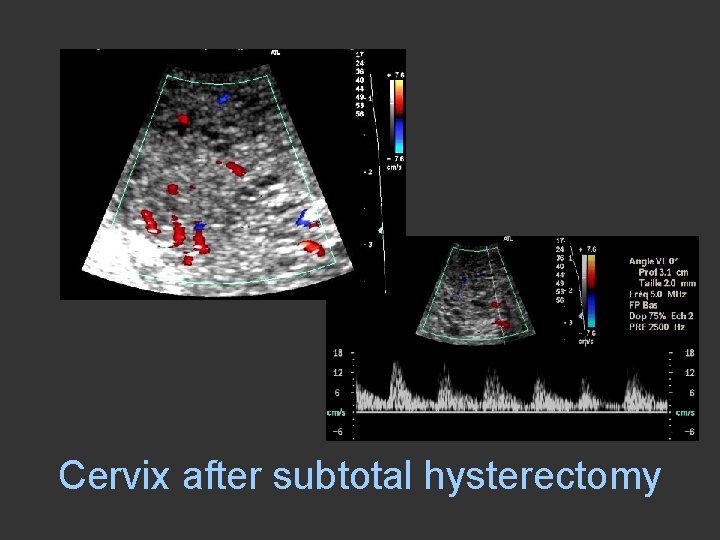
Cervix after subtotal hysterectomy

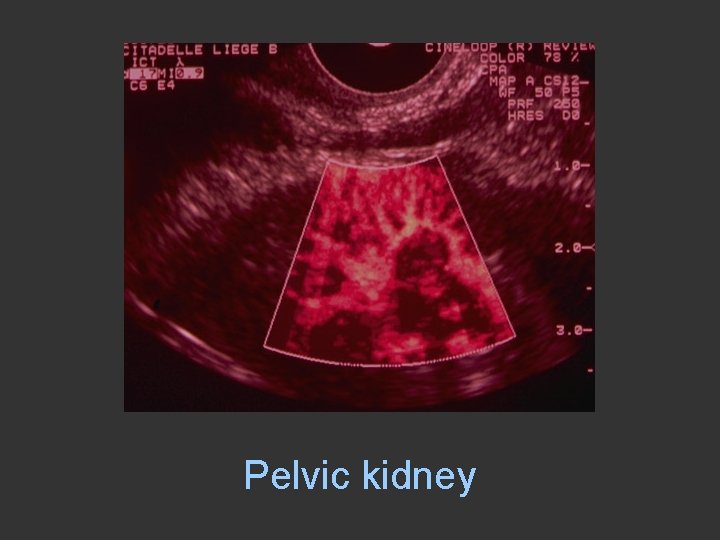
Pelvic kidney

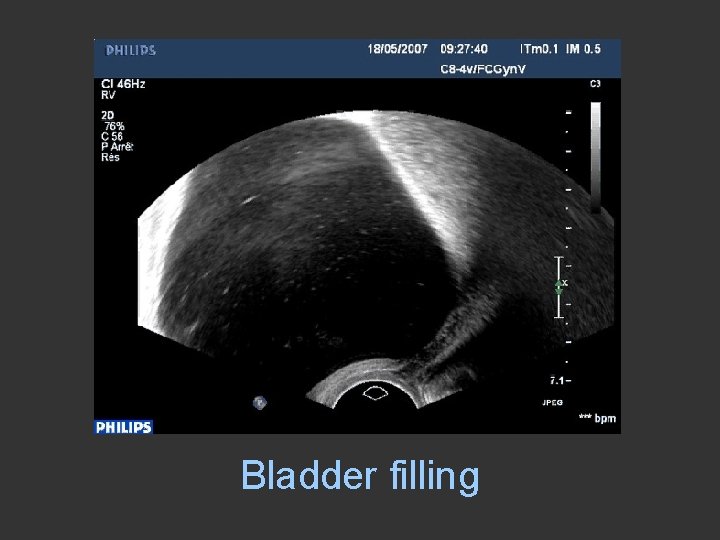
Bladder filling

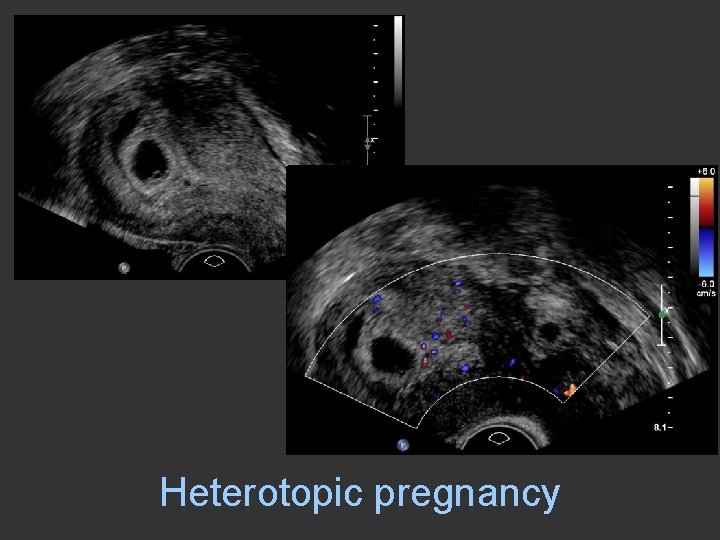
Heterotopic pregnancy

Dank uw ! Questions?

Don’t worry, they normally look like little humans during the early scans