Ultrasonic Nonlinear Imaging Contrast Imaging History 1968 Gramiak

















































- Slides: 93

Ultrasonic Nonlinear Imaging. Contrast Imaging

History • 1968 Gramiak et al published observation of echo signal from LV injection of indocyanine dye • Subsequent research showed this phenomenon occurred with just about any liquid injected through small needle

More History • First work was with free gas bubbles – bubbles didn’t last very long – size too big to go through lungs, needed intra-arterial injection • Late ‘ 80’s - early ‘ 90’s - development of numerous agents – more stable – smaller size

Motivation • X-ray, CT, nuclear, and MR all need it. • Enhance backscatter signal from blood – Blood signal typically 40 d. B below tissue • Provide visualization of low velocity flow normally masked by tissue motion – measure of microvasculature important in many disease states

Desired Properties • Non-toxic/easily eliminated • Able to be injected intravenously • Small enough to pass through microcirculation • Physically stable • Acoustically active

Contrast Imaging • Contrast agents are used to provide higher contrast. The three commonly seen contrast agents are backscatter, attenuation and sound velocity. • Contrast agents could be solid particles, emulsion, gas bubbles, encapsulated gas, or liquid.

Contrast Imaging • Primary clinical benefits: – Enhanced contrast resolution between normal and diseased tissues. – Outline of vessels or heart chambers. – Tissue characterization by using tissue specific agents. – Increasing blood flow signals. – Dynamic study using washout curve.

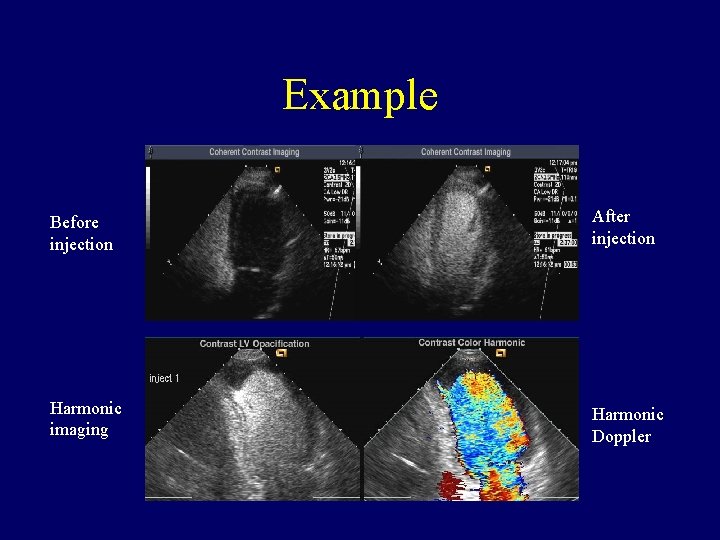
Example Before injection After injection Harmonic imaging Harmonic Doppler

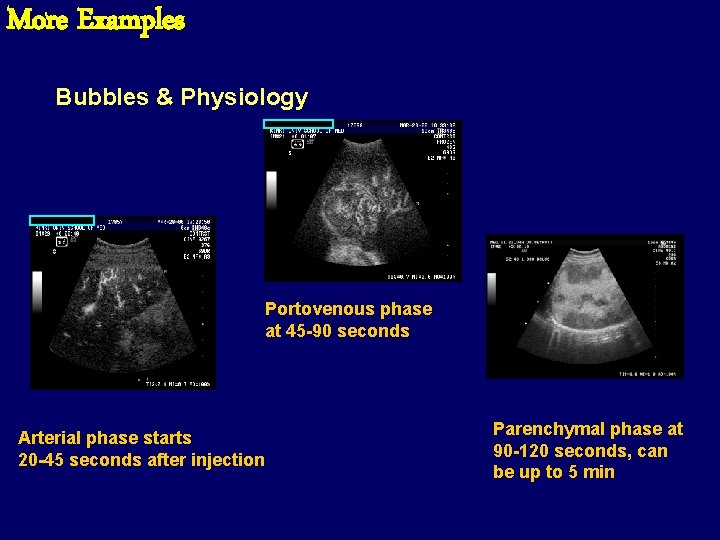
More Examples Bubbles & Physiology Portovenous phase at 45 -90 seconds Arterial phase starts 20 -45 seconds after injection Parenchymal phase at 90 -120 seconds, can be up to 5 min

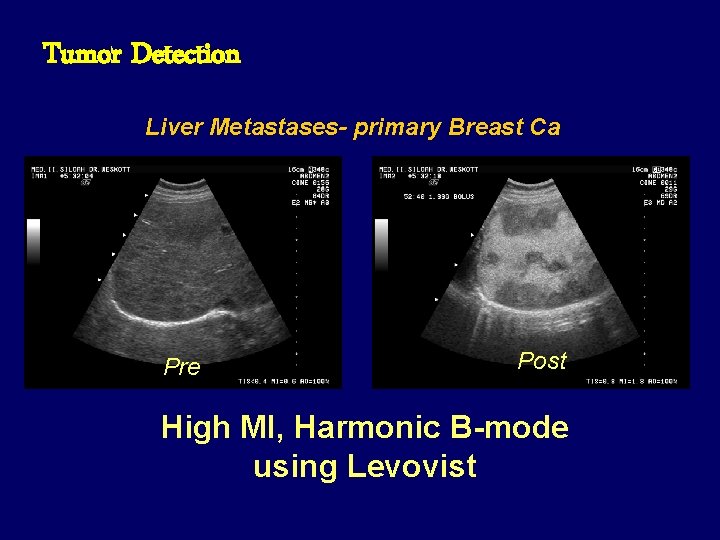
Tumor Detection Liver Metastases- primary Breast Ca Pre Post High MI, Harmonic B-mode using Levovist

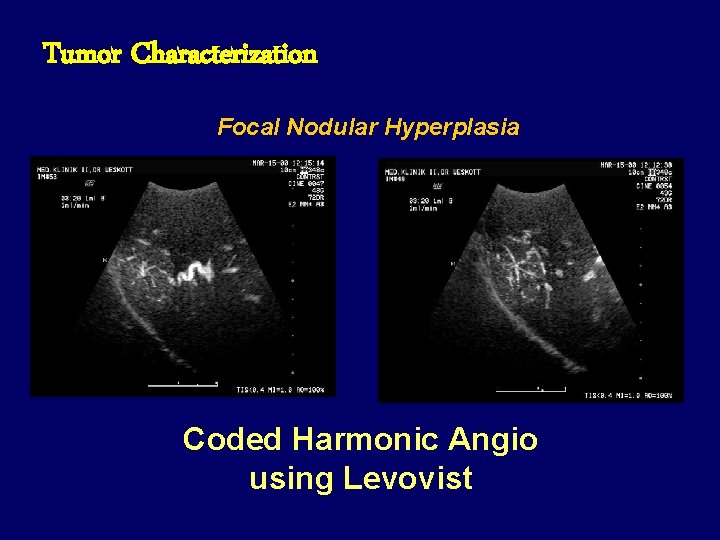
Tumor Characterization Focal Nodular Hyperplasia Coded Harmonic Angio using Levovist

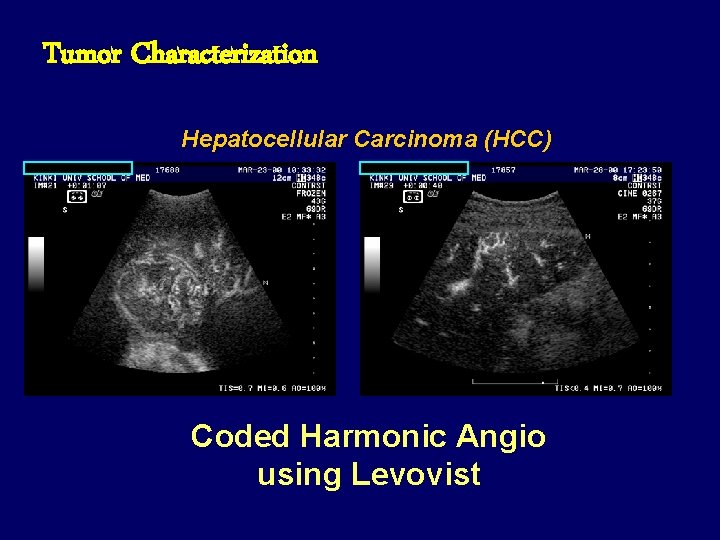
Tumor Characterization Hepatocellular Carcinoma (HCC) Coded Harmonic Angio using Levovist

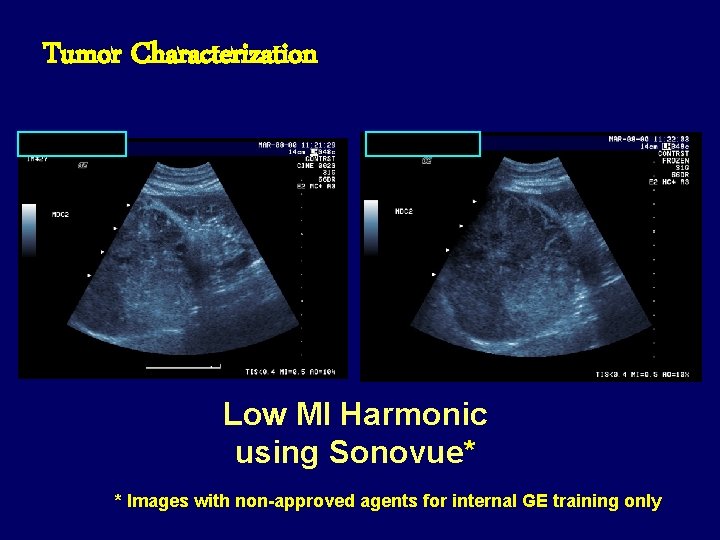
Tumor Characterization Low MI Harmonic using Sonovue* * Images with non-approved agents for internal GE training only

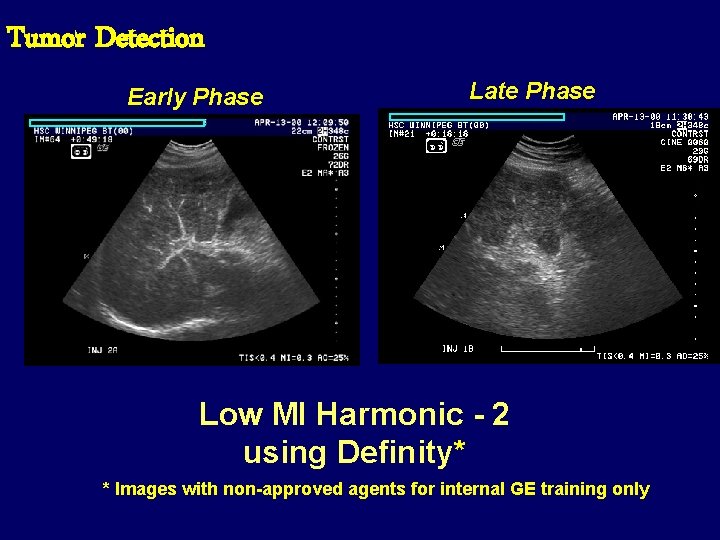
Tumor Detection Early Phase Late Phase Low MI Harmonic - 2 using Definity* * Images with non-approved agents for internal GE training only

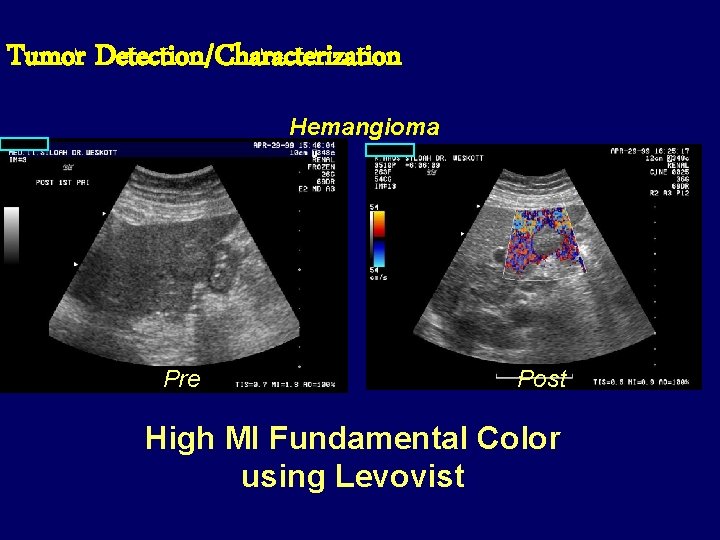
Tumor Detection/Characterization Hemangioma Pre Post High MI Fundamental Color using Levovist

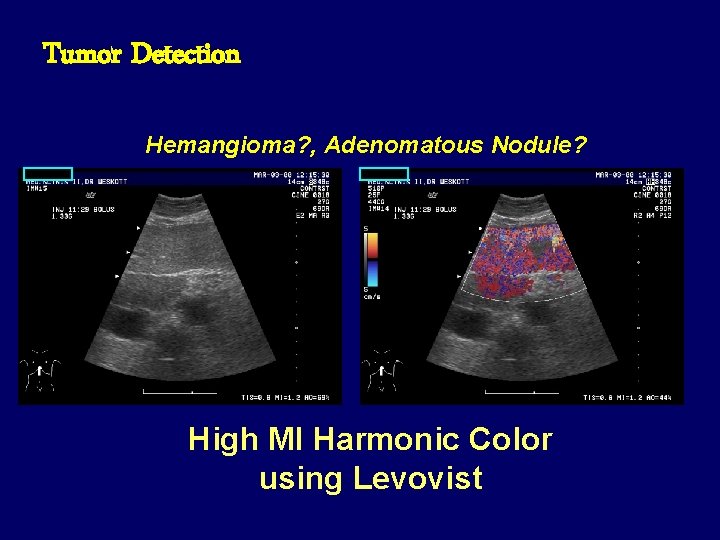
Tumor Detection Hemangioma? , Adenomatous Nodule? High MI Harmonic Color using Levovist

Clinical Values (I) • Tumor Detection • presence or absence of liver, kidney or pancreatic masses • Tumor Characterization • avascular- cyst • hypovascular- metastasis, hemangioma • hypervascular- primary carcinoma, hypervascular met • Others • • enhances vessels for RAS, Carotid stenosis, TCD, etc better visualization of thrombus (IVC, TIPS) post ablation follow up trauma assessment

Clinical Values (II) • • • Endocardial border detection. Left ventricle (LV) function. Valvular regurgitation quantification. LV flow patterns. Perfusion area of coronary artery. Assessment of surgery for ventricular septal defect.

Clinical Values (III) • • • Liver tumor enhancement. Uro-dynamics and kidney functions. Tubal function and placenta perfusion. Transcranial Doppler enhancement. LV pressure measurements.

Current Contrast Agents • • • Aerosomes (Ima. Rx, Tucson, AZ) Albunex (MBI, San Diego, CA) BY 963 (Byk Gulden, Konstanz, Germany) Echovist (Schering, Berlin, Germany) Echo. Gen (Sonus, Bothell, WA) DMP 115 (Du. Pont-Merck, N. Billerica, MA) Imagent US (Alliance, San Diego, CA) Levovist (Schering, Berlin, Germany) NC 100 -100 (Nycomed, Oslo, Norway)

Current Contrast Agents (Cont. ) • • • Optison (MBI, San Diego, CA) approved in US for cardiac Oralex (MBI, San Diego, CA) PESDA (Univ of Nebraska, Omaha, NE) Sono. Rx (Bracco, Princeton, NJ) US approved oral agent Sonovist (Schering, Berlin, Germany) Sonovue (Bracco, Milan, Italy) ST 68 (Drexel Univ, Philadelphia, PA) Quantison (Andaris, Nottingham, UK) Quantison Depot (Andaris, Nottingham, UK) Many more, …

Contrast Mechanisms • Strong backscattering produced by air bubbles. • The backscatter increases roughly linearly with the number of micro-bubbles. • A bubble in liquid acts as a harmonic oscillator. Acoustic resonance provides the major echo enhancement. In addition, strong harmonics are produced.

Contrast Mechanisms • Acoustic attenuation of soft tissues is typically represented by a constant (e. g. , 0. 5 d. B/cm/MHz). • Since contrast agents significantly change the scattering properties, attenuation measurements can also be used for contrast enhancement.

Contrast Mechanisms • Sound velocity is primarily determined by density and compressibility. Apparently, micro -bubble based contrast agents alter sound velocity. • Contrast enhancement based on sound velocity variations is still academic.

Contrast Mechanisms • Micro-bubbles produce strong harmonics when insonified near the resonance frequency. • If such harmonics are stronger than tissue harmonics, contrast can be improved. • Second harmonic signal is most useful due to limited transducer and system bandwidth.

(Encapsulated) Gas Bubbles

Bubble Characteristics • Size • Shell for stabilization Microbubble 2– 8 µm RBC 6– 8 µm – tune for desired acoustic properties • Gas – use high molecular weight, less soluble gas

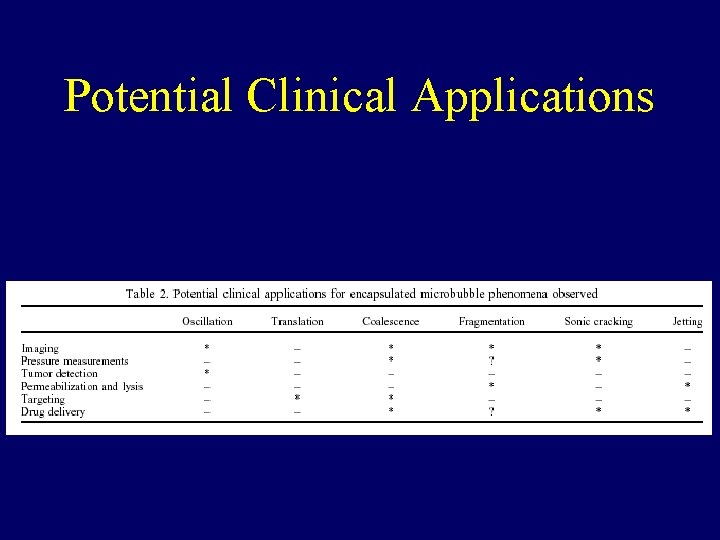
Ultrasound-Induced Encapsulated Microbubble Phenomena • • Oscillation Translation Coalescence Fragmentation Sonic cracking Jetting , …

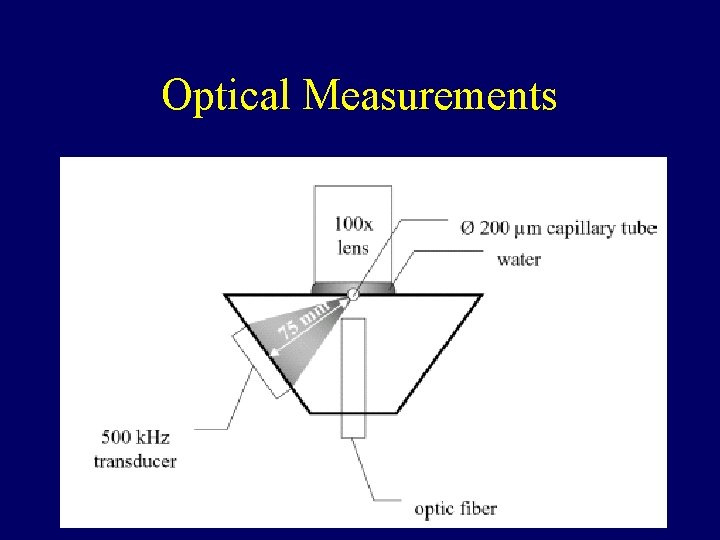
Optical Measurements

Optical Measurements

Optical Measurements 100 Mframes/s camera

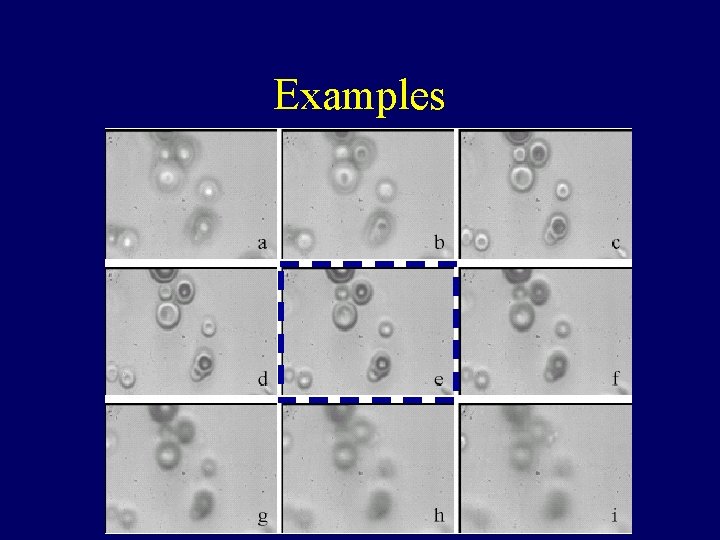
Examples

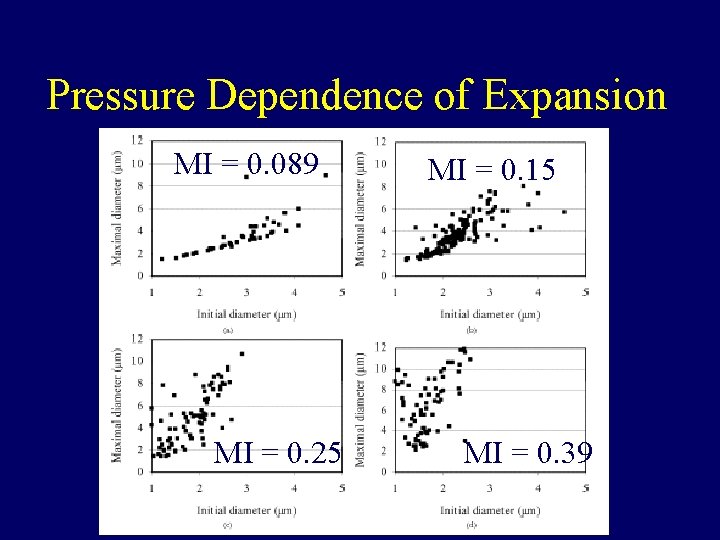
Pressure Dependence of Expansion MI = 0. 089 MI = 0. 25 MI = 0. 15 MI = 0. 39

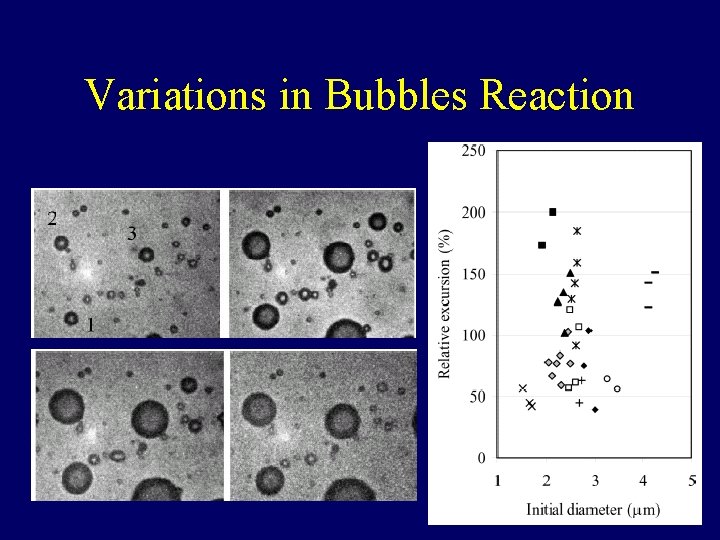
Variations in Bubbles Reaction

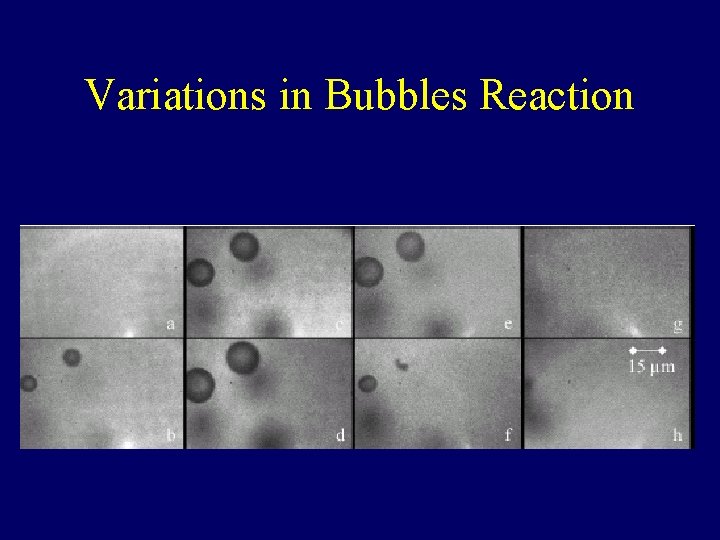
Variations in Bubbles Reaction

Bubble Oscillation

Ultrasound-Induced Oscillation • Moderate: Alternate expansions and contractions with the same amplitude and duration at low driving pressures (stable cavitation). • Violent: At higher pressures, greater bubble expansion amplitude than contraction amplitude, and relatively slow expansion followed rapid contraction (inertial or transient cavitation). • Cavitation threshold: Above which the bubble’s maximum radius is larger than twice the equilibrium radius.

Modeling • Strength of backscatter signal depends on difference in acoustic properties between two materials. . . For a particle of volume V in homogenous medium k = compressibility r = mass density p = particle m = surrounding medium

Modeling • Now need to include shell effects. . . For a shell encapsulated gas bubble of instantaneous radius R: Keff ~ elasticity of shell r = density of surrounding media dtot = total damping coefficient P(t) = incident acoustic energy Accurate only at low pressures

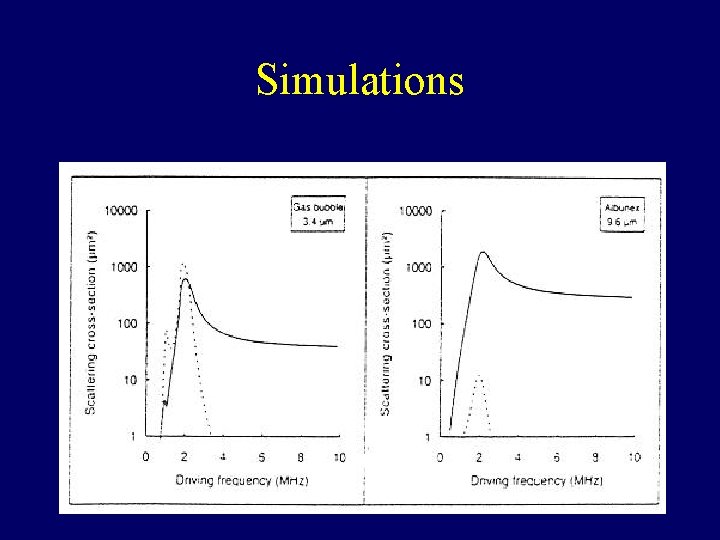
Simulations

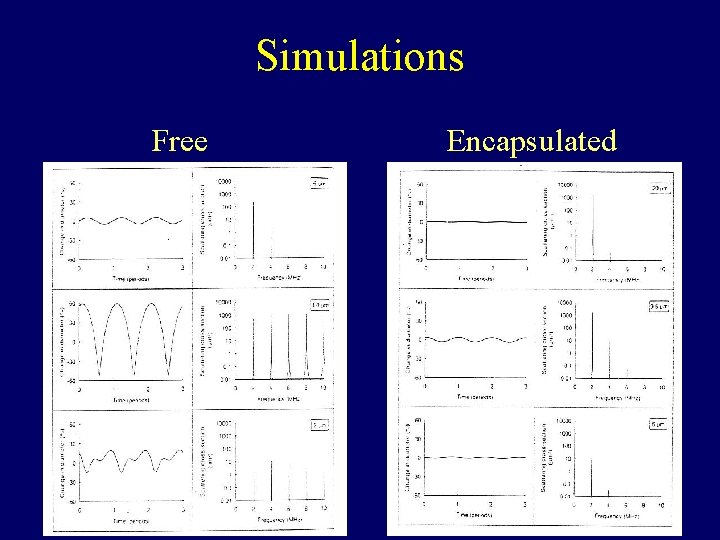
Simulations Free Encapsulated

Simulations

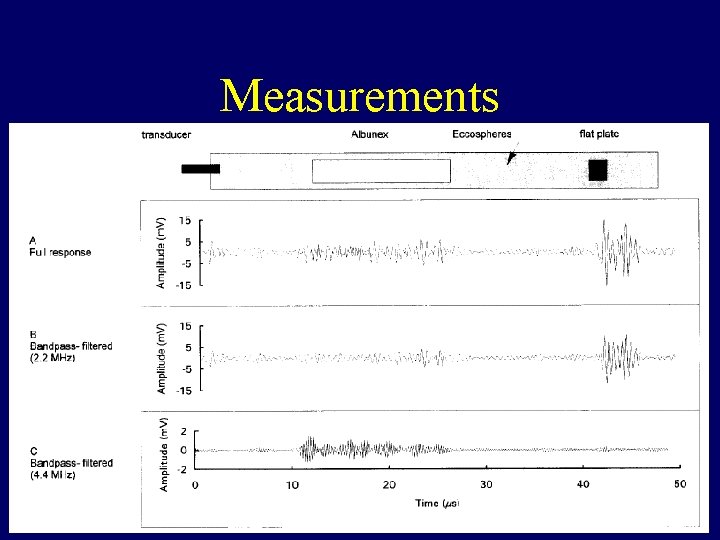
Measurements

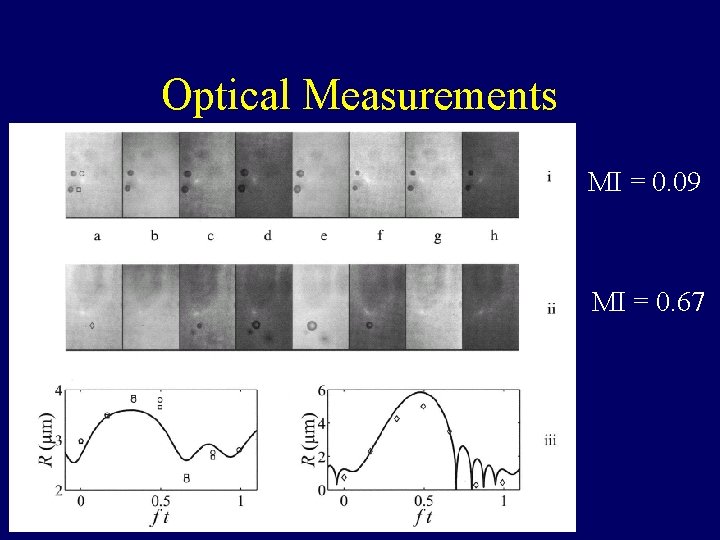
Optical Measurements MI = 0. 09 MI = 0. 67

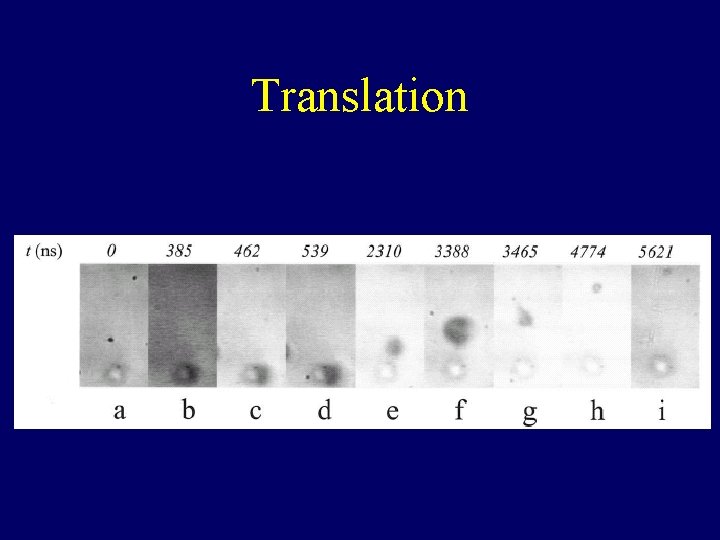
Translation

Translation • Resulted from primary radiation force (pressure gradient across the bubble surface). • Maximal in contraction phase. • Used for active targeting.

Translation

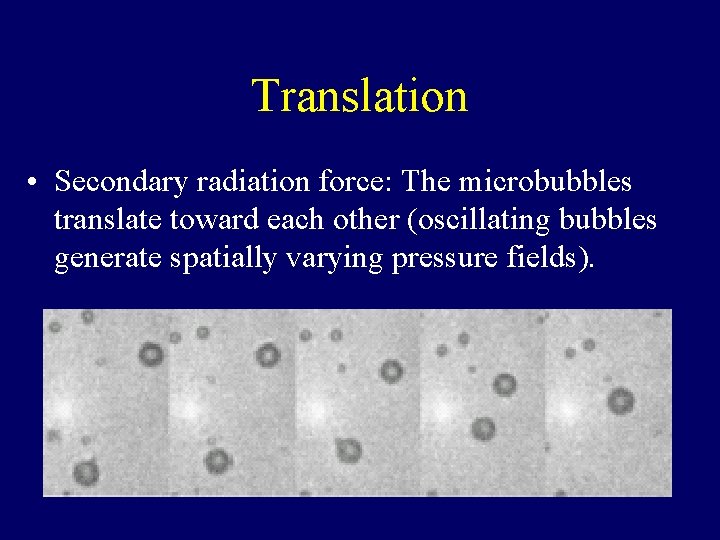
Translation • Secondary radiation force: The microbubbles translate toward each other (oscillating bubbles generate spatially varying pressure fields).

Coalescence

Coalescence • Fusion of two or more bubbles. • As bubbles expand, bubble surfaces flattens and thinning occurs. • When critical thickness is reached (around 0. 1 micron), bubbles rupture and merge with each other.

Coalescence

Fragmentation

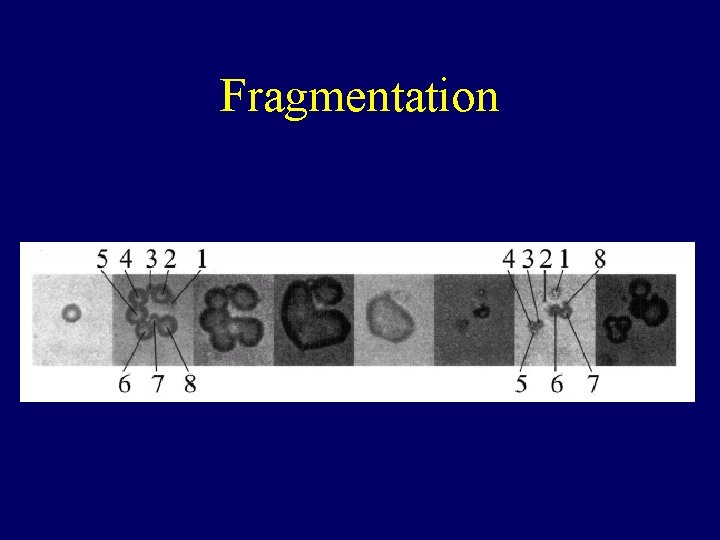
Fragmentation • Fission of a bubble into smaller bubbles.

Fragmentation

Sonic Cracking

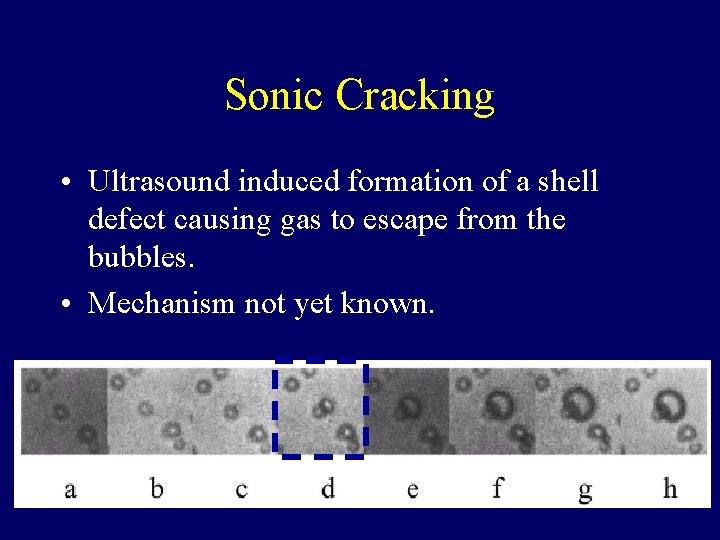
Sonic Cracking • Ultrasound induced formation of a shell defect causing gas to escape from the bubbles. • Mechanism not yet known.

Jetting

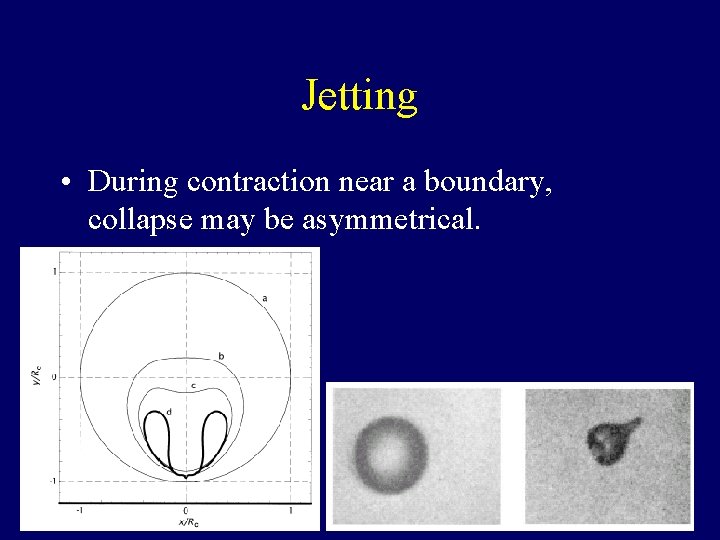
Jetting • During contraction near a boundary, collapse may be asymmetrical.

Potential Clinical Applications

Interference from Tissue Nonlinearities

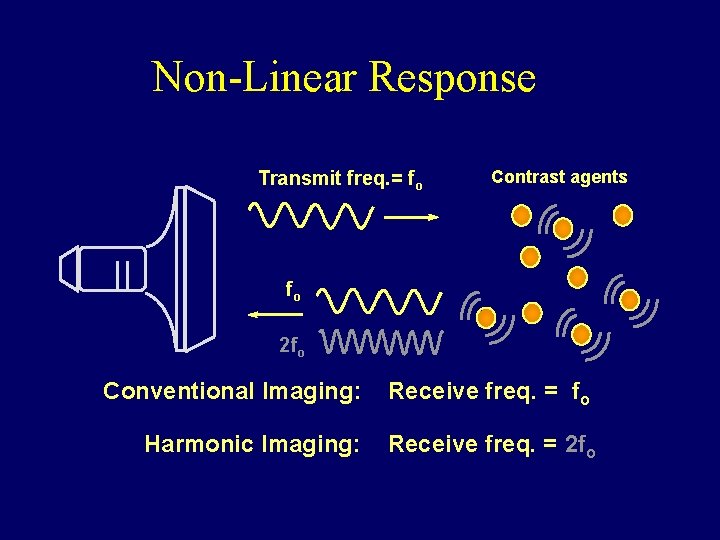
Non-Linear Response Transmit freq. = fo Contrast agents fo 2 fo Conventional Imaging: Receive freq. = fo Harmonic Imaging: Receive freq. = 2 fo

Various Contrast Modes • High MI B-Mode, Harmonic - optimized for SAE harmonic imaging • Low MI B-Mode, Harmonic 1 and 2 - optimized for nondestructive harmonic imaging • High MI colorflow fundamental - optimized for SAE destruction effect • High MI colorflow harmonic - optimized for SAE with reduced tissue flash artifact

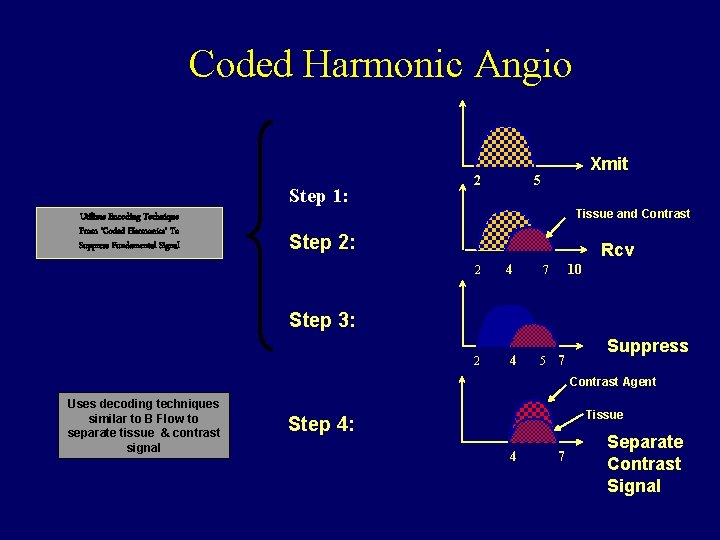
Coded Harmonic Angio Step 1: Utilizes Encoding Technique From ‘Coded Harmonics’ To Suppress Fundamental Signal 2 Xmit 5 Tissue and Contrast Step 2: Rcv 2 4 10 7 Step 3: 2 4 5 7 Suppress Contrast Agent Uses decoding techniques similar to B Flow to separate tissue & contrast signal Tissue Step 4: 4 7 Separate Contrast Signal

Detecting Blood Reflectors Problem: Blood echoes are very weak and sometimes moving too slow for Doppler techniques Tissue Blood Noise

Detecting Blood Reflectors Problem: Blood echoes are very weak and sometimes moving too slow for Doppler techniques Solution: Inject contrast agents to enhance signal Tissue Agent Noise

Detecting Blood Reflectors Problem: Blood echoes are very weak and sometimes moving too slow for Doppler techniques Solution: Inject contrast agents to enhance signal Use codes to 1) detect harmonic return signal Tissue Agent Noise

Detecting Blood Reflectors Problem: Blood echoes are very weak and sometimes moving too slow for Doppler techniques Solution: Inject contrast agents to enhance signal Use codes to 1) detect harmonic return signal 2) Suppress tissue signal Tissue Agent Noise

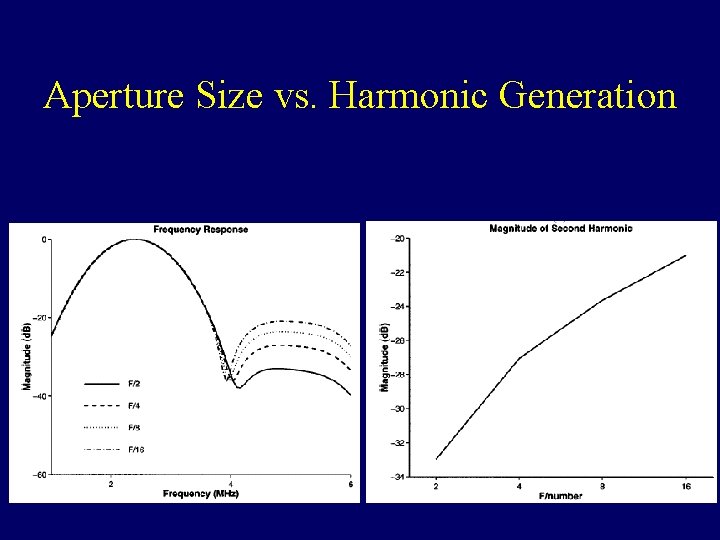
Harmonic Interference • In contrast imaging, in which the tissue harmonic signals are un-desirable, the amplitude of the propagating wave needs to minimized. • Large apertures (smaller f-numbers) may be used. • It was reported that tissue harmonic signal can be reduced by 3 d. B by doubling the aperture size.

Reduction of Interference from Tissue • • Harmonic cancellation system. Sub-harmonic imaging. Pulse-inversion Doppler (clutter). Pulse-inversion fundamental imaging.

Harmonic Cancellation System

Aperture Size vs. Harmonic Generation

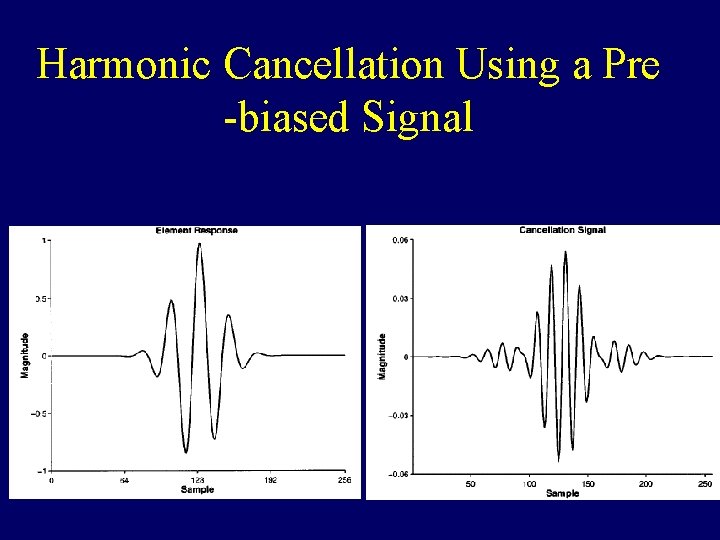
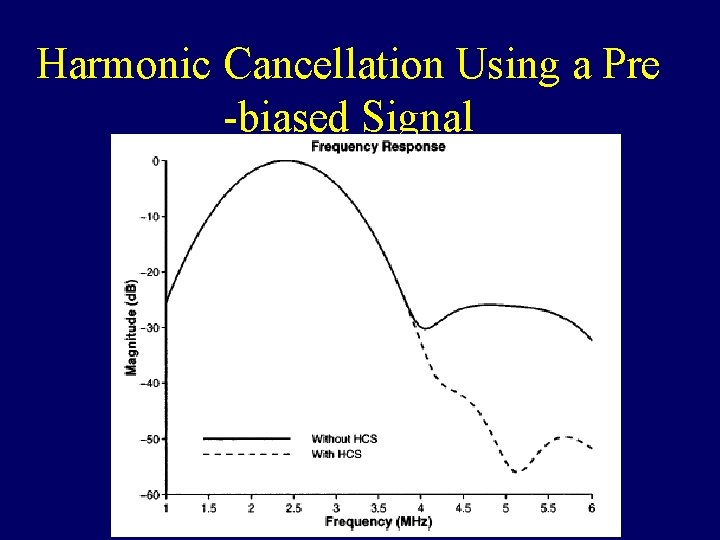
Harmonic Cancellation Using a Pre -biased Signal

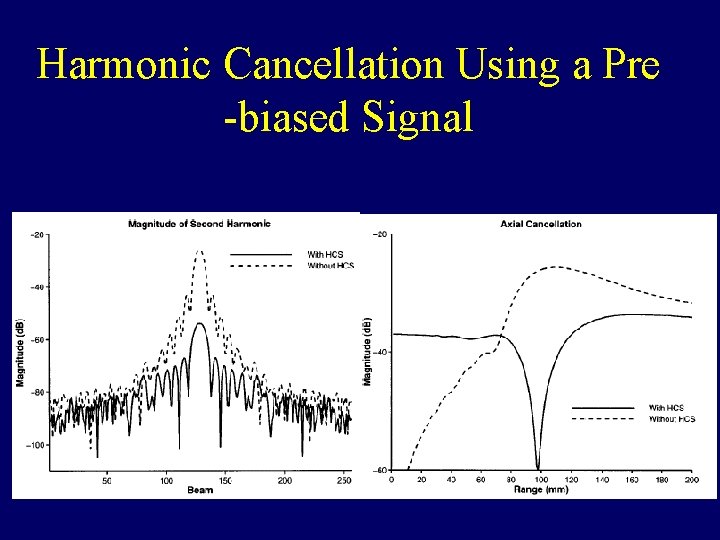
Harmonic Cancellation Using a Pre -biased Signal

Harmonic Cancellation Using a Pre -biased Signal

Sub-Harmonic Imaging

Sub-Harmonic Imaging • Tissue propagation does not generate significant sub-harmonic signals. • Sub-harmonic signals may be generated with microbubbles in proper acoustic fields. • Sub-harmonic imaging can thus be used for reduction of tissue nonlinear signals.

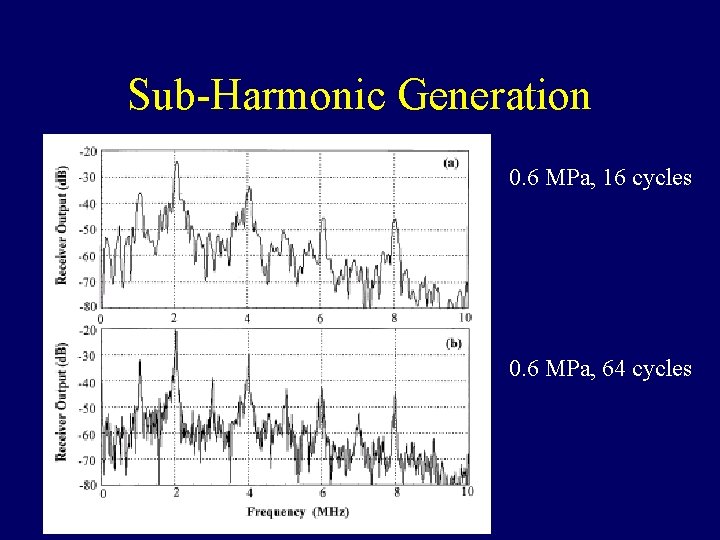
Sub-Harmonic Generation 0. 6 MPa, 16 cycles 0. 6 MPa, 64 cycles

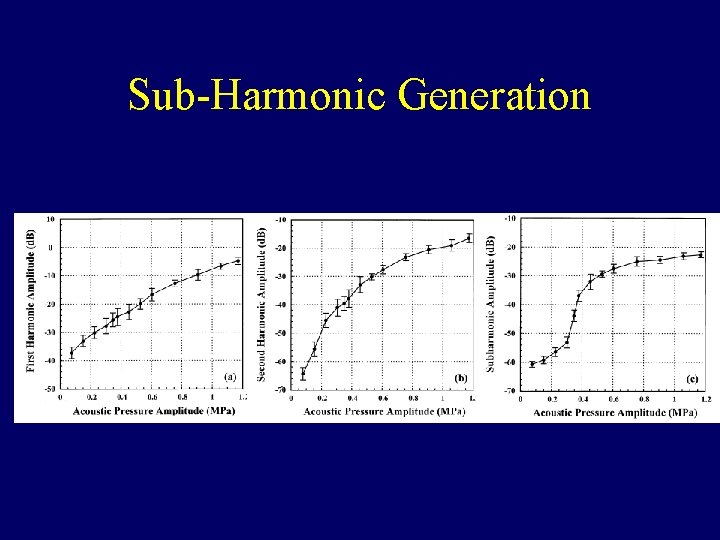
Sub-Harmonic Generation

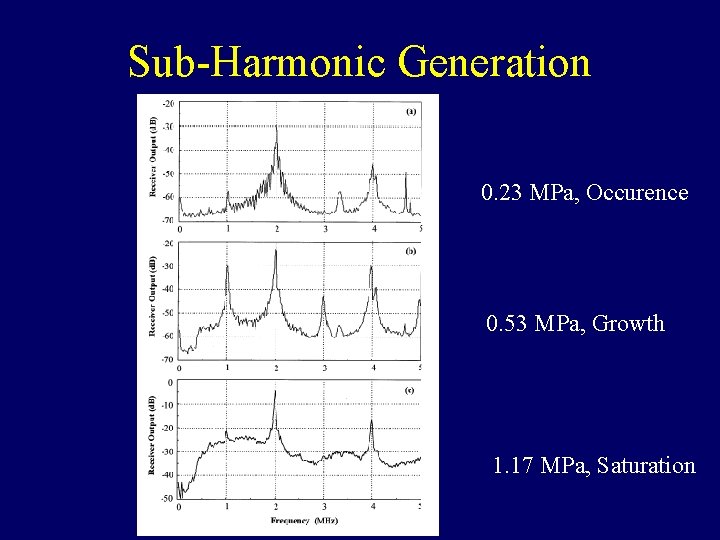
Sub-Harmonic Generation 0. 23 MPa, Occurence 0. 53 MPa, Growth 1. 17 MPa, Saturation

Pulse Inversion Doppler (for Clutter Reduction)

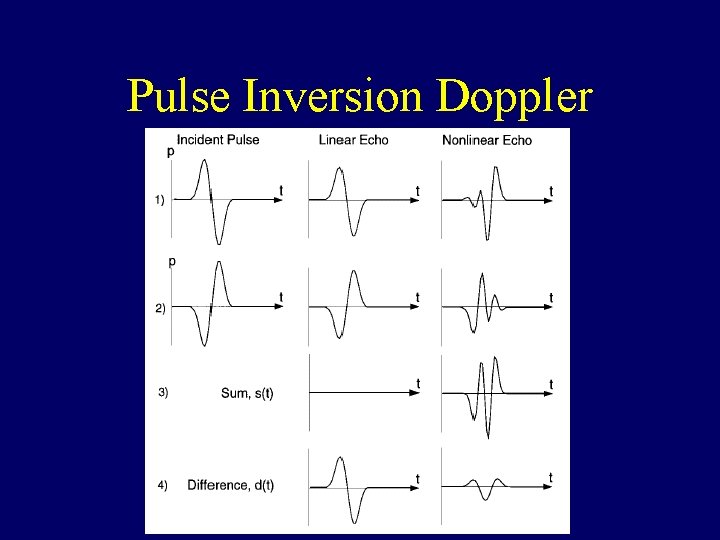
Pulse Inversion Doppler

Pulse Inversion Doppler (Linear)

Pulse Inversion Doppler (Non-Linear)

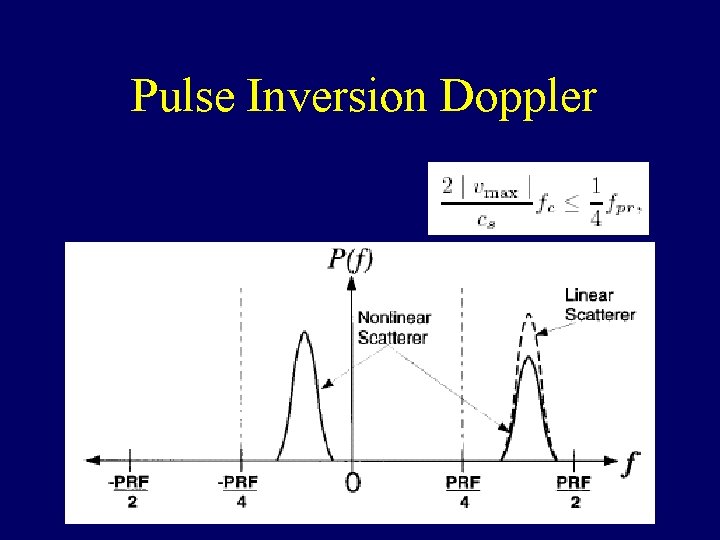
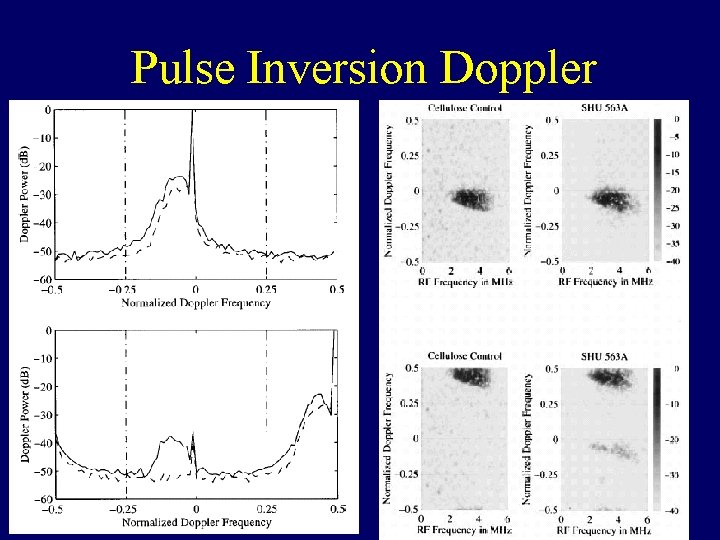
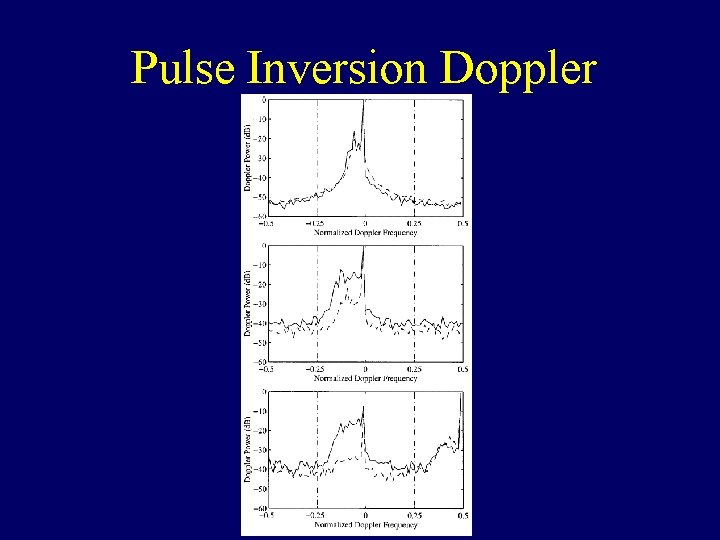
Pulse Inversion Doppler

Pulse Inversion Doppler

Pulse Inversion Doppler

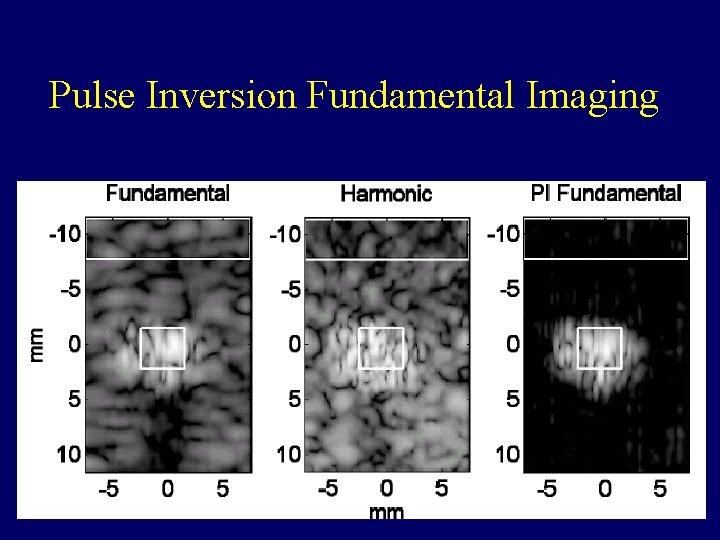
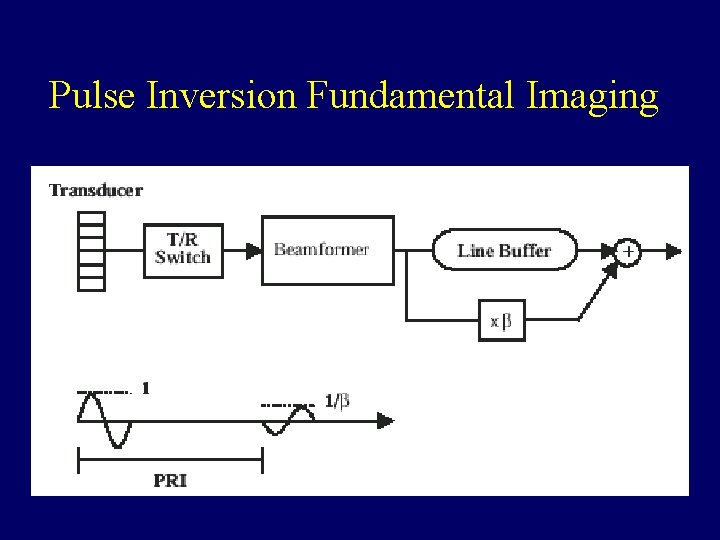
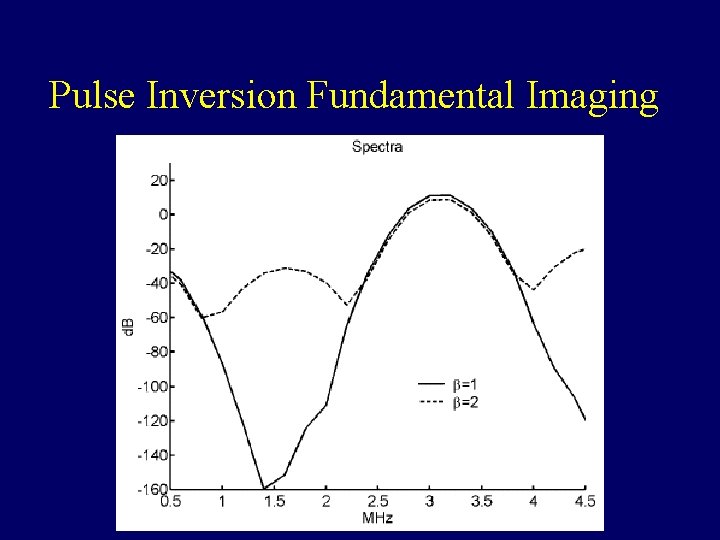
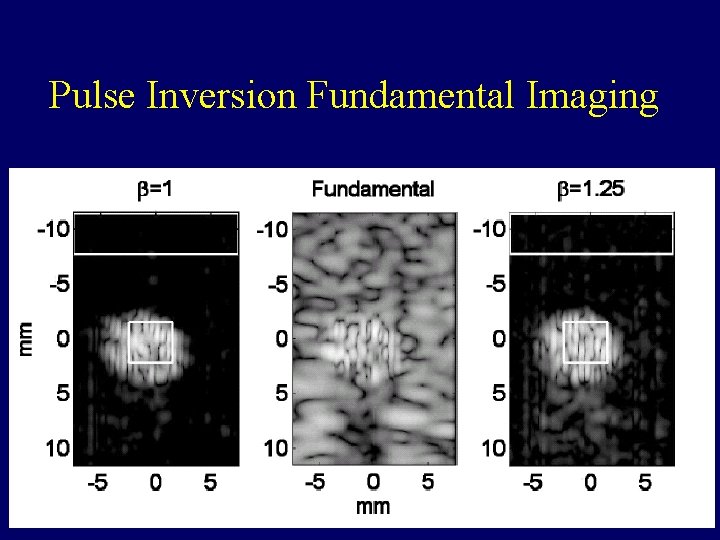
Pulse Inversion Fundamental Imaging

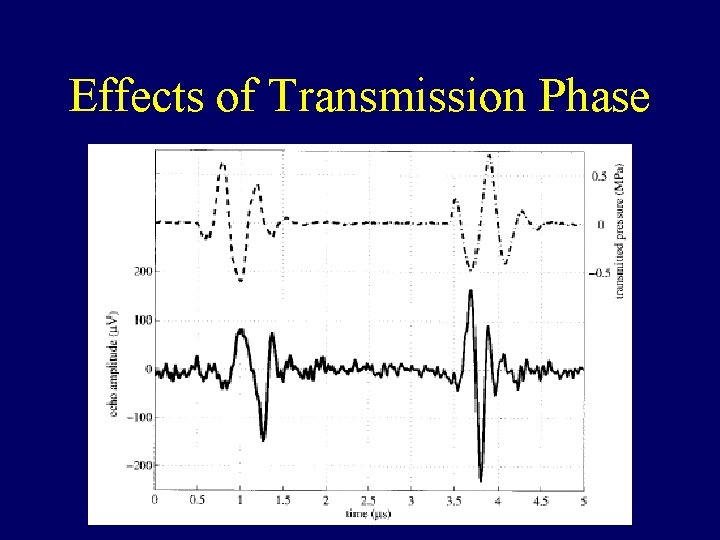
Effects of Transmission Phase

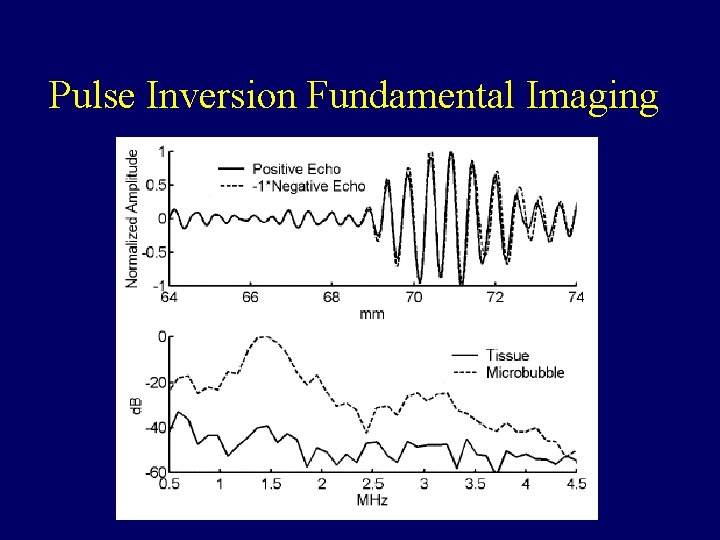
Pulse Inversion Fundamental Imaging

Pulse Inversion Fundamental Imaging

Pulse Inversion Fundamental Imaging

Pulse Inversion Fundamental Imaging

Pulse Inversion Fundamental Imaging