ULCERATIVE LESIONS OF THE ORAL CAVITY Macule flat

























- Slides: 29

ULCERATIVE LESIONS OF THE ORAL CAVITY

Macule: § flat and well-demarcated lesion of any size, characterized by color change in contrast to the surrounding skin. It is generally caused by alteration of melanin pigment.

Papule § Elevated, solid and circumscribed lesion, usually 1 cm or less in diameter.

Plaque Elevated, flat-topped, firm and superficial lesion, usually greater than 1 cm in diameter; may be coalesced papules.

Vesicle Elevated, thin-walled lesion; filled with serous (clear) fluid, less than 1 cm in diameter.

Bulla: § Elevated lesion filled with clear fluid, greater than 1 cm in diameter.

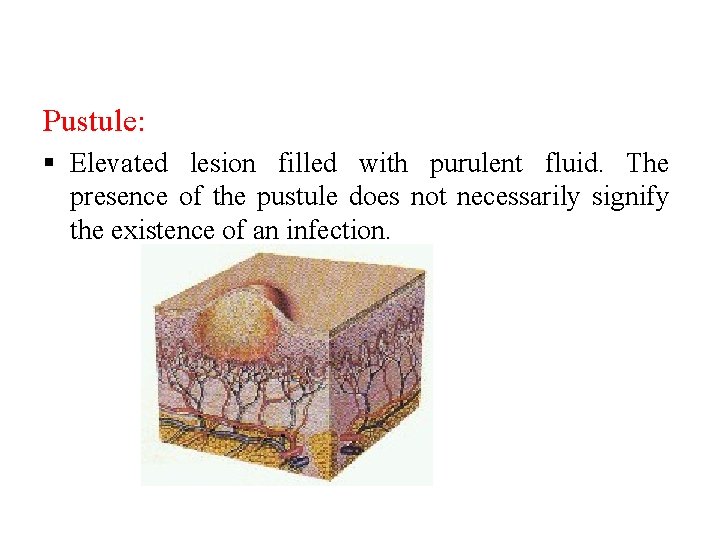
Pustule: § Elevated lesion filled with purulent fluid. The presence of the pustule does not necessarily signify the existence of an infection.

Definition Ulcer – A well circumscribed , often depressed lesion with an epithelial defect that is covered by a fibrin clot, causing a yellow white appearance. Based on the duration ulcers can be broadly classified into § Acute (short term) or § Chronic (long term). Ø Acute ulcers persist no more than three weeks and regress spontaneously Ø Chronic ulcers persist for weeks and months

Example of acute ulcers Ø Ø Aphthous ulcers, Traumatic ulcers Herpetic ulcers and Chancres. Example of Chronic ulcers Ø Ø Ø Major aphthous ulcers, Ulcers from odontogenic infection, Malignant ulcers, gummas, Ulcers secondary to debilitating systemic disease and some traumatic ulcers (with a persistent traumatic element)

Why ulcer in oral cavity lacks characteristic appearance on the skin? ? ? § Oral mucosa is thin and easily traumatized by teeth § Secondary infection by oral flora

Burket’s classification of ulcer Acute multiple ulcers § HSV Infection § VZV Infection § Cytomegalovirus Infection § Coxsackievirus Infection § NUG § Erythema Multiforme § SJS and TEN § Oral Hypersensitivity Reaction

Recurrent Oral Ulcers § Recurrent Apthous Stomatitis § Behcet Disease Chronic Multiple Lesions § PV § Paraneoplastic Pemphigus § Pemphigus Vegetans § Subepithelial Bullous Dermatoses § Bullous Pemphigoid § Mucous Membrane Pemphigoid

§ Linear Ig. A Disease § Epidermolysis Bullosa Aquisita § Chronic Bullous Disease of Childhood Single Ulcer § § § Traumatic Ulcerative Granuloma Histoplasmosis Blastomycosis Mucormycosis

ETIOLIGY OF ORAL ULCERS Vesiculo-Bullous Diseases Infective Primary and recurrent Herpes simplex lesions Herpes Zoster and Chickenpox Hand-foot-and-mouth disease Herpangina Non-infective Pemphigus vulgaris Mucous membrane pemphigoid Erythema multiforme Contact allergy

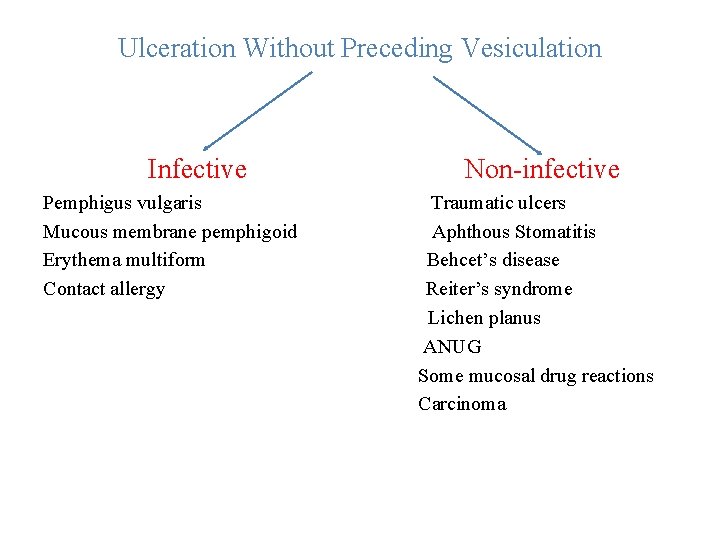
Ulceration Without Preceding Vesiculation Infective Pemphigus vulgaris Mucous membrane pemphigoid Erythema multiform Contact allergy Non-infective Traumatic ulcers Aphthous Stomatitis Behcet’s disease Reiter’s syndrome Lichen planus ANUG Some mucosal drug reactions Carcinoma

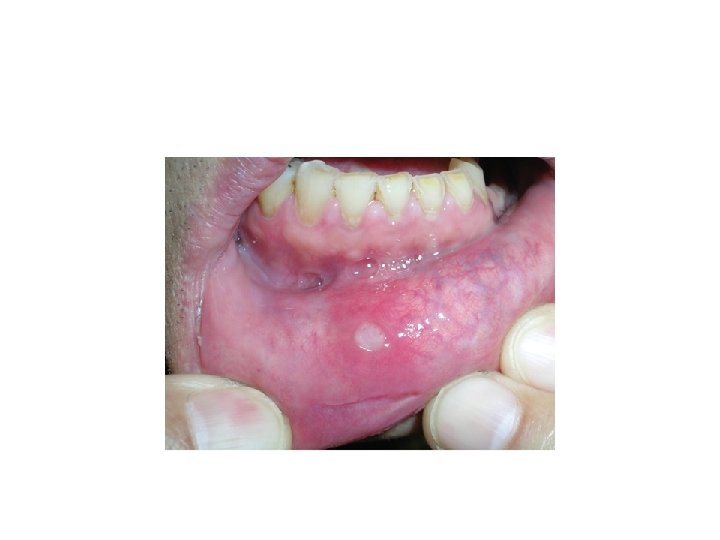
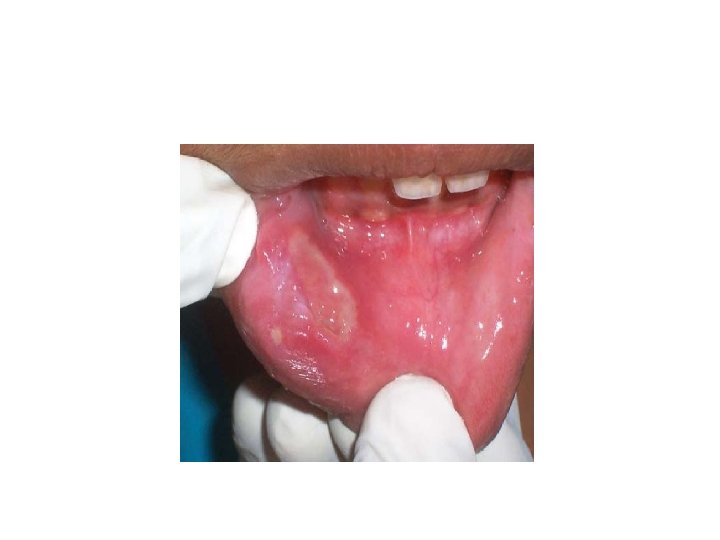
Apthous Ulcer • Also known as a canker sore. • It is characterized by the appearance of initially necrotic ulcers, with well defined limits surrounded by an erythematous halo. • The lesions are located on the oral mucosa, but are infrequent on the gums • RAS is the most frequent chronic disease of the oral cavity, affecting 5 -25% of the population.

• It is more common in patients between 10 -40 years of age, and • Predominantly affects women individuals of higher socioeconomic levels. Etiopathogenesis § Not known § May be localized immune dysregulation. § May be due to Allergies Genetic Predisposition Hematological InfluencesImmunological Factors

• • • Infectious Agents Nutritional Deficiencies Smoking Cessation Stress Trauma Probable three categories Ø Primary Immune Dysregulation Ø Decrease mucosal Barrier Ø Increase in antigenic exposure

• Disease runs in family • If both parents have a history of apthous 90% chances of children's to develop the disease • Stress Immune Dysregulation Apthous • Histocompatibility antigene • Cyclic Neutropenia (systemic immune dysregulation)

Factors affecting the mucosal barrier Ø Trauma Ø Nutritional Deficiency Ø Smoking cessation Ø Hormonal changes Antigenic stimulation Ø Sodium lauryl sulphate in tooth paste Ø NSAIDS Ø Beta blockers Ø Viral infections Ø Cow milk etc.

Clinical presentation • Minor Apthae (Mikulicz’s Disease) Ø Most common (80% cases) Ø Fewest recurrence Ø Shortest duration of ulcer episode among the three variants Ø Almost exclusively on non keratinized mucosa Rare on keratinized mucosa Ø 3 -10 mm in diameter Ø Heals in 7 -14 days 1 -5 ulcer /episode


• Major Apthae (sutton’s Disease/ Periadenitis mucosa necrotica recurrens) Ø Larger than minor apthae Ø Longest duration per episode Ø 1 -3 cm in diametyer Ø 2 -6 weeks to heal Ø 1 -10 ulcer /episode Ø Any oral surface may be affected Ø Onset usually after puberty and recurrent episode upto the age of 20 yrs Ø Healing with scaring may leads to a restricted mouth opening


Herpetiform apthae Ø Demonstrate the greatest number of ulceration. Ø May be 100 ulcers/episode Ø 1 -3 mm in diameter Ø Bears superficial resemblance with HSV lesion. Ø Heals within 7 -10 days and reoccur soon

Systemic disorders associated with recurrent apthous stomatitis Ø Behcet’s Syndrome Ø Celiac Disease Ø Cyclic Neutropenia Ø Nutritional Deficiencies Ø Ig. A Deficiency Ø MAGIC Syndrome Ø PFAPA Syndrome Ø Sweet’s Syndrome

• Tests Conditions to be ruled out 1. Biopsy When mucocutaneous lesions are suspected 2. Full blood picture Ø Hemoglobin To rule out iron deficiency Ø Total and differential count To rule out cyclic neutropenia Ø Red cell indices To rule out iron and folic acid deficiency Ø Iron studies: Serum ferritin levels To rule out iron deficiency Ø Red cell folate assay To assess deficiency of folic acid Ø Serum vitamin B 12 levels

3. Fungal culture/periodic schiff test (PAS) Candidiasis 4. Microimmune-diffusion test: Blastomyces A-antigen Blastomyces enzyme immunoassay 5. Direct immunofluorescence Pemphigus, Cicatric pemphigoid, 6. Indirect immunofluorescence Systemic lupus erythematosus Lichen planus, Dermatitis Herpetiformis 7. Endoscopy, laryngoscopy, small bowel series Crohn’s disease, Behcet’s syndrome, Ulcerative cholitis Colonoscopy, Sigmoidoscopy

8. Serum autoantibodies to desmoplakin I and II Erythema multiforme 9. Antigliadin, antireticulin, antiendomysial enteropathy Celiac disease, gluten sensitive antibody test 10. pp 65 CMV antigenemia test, CMV culture and antibody test For EB virus 11. Virus neutralization test Coxsackie virus 12. HSV culture and antibody test Herpes simplex virus (HSV