Ulcerative Colitis Extraintestinal Manifestations Kimberly Persley MD April

Ulcerative Colitis & Extraintestinal Manifestations Kimberly Persley, MD April 20, 2005

Case Presentation • 36 yo WP transfer from OSH with severe, steriod refractory UC – 11/2004 – Bloody diarrhea and abdominal pain • Treated with Colazol 6. 75 gm/d • Prednisone 60 mg /d – 12/2004 – Imuran started secondary to refractory symptoms but developed ITP and the Imuran stopped

Case Presentation – 2/26/2005 – underwent colonoscopy that showed “mild to moderately active colitis in the left colon – 2/28/2005 – admitted to OSH with fevers, increased bloody diarrhea and abdominal pain • Negative ID workup – 3/6/2005 – transfer to PHD for further management • 10 -12 bloody bowel movements daily, abdominal pain, persistent fever, anorexia • No joint pain, oral ulcers or rashes

Case Presentation • PMH – ITP – first diagnosed 11/2004 • Bone marrow biopsy – megakaryocytic hyperplasia • Treated with steroids, Win. Rho and IVIG – Patent foramen ovale • Meds – Flagyl, Cipro, Solumedrol, Morphine and Phenergan • Family History – Paternal Grandfather with colon cancer

Case Presentation • Physical Exam – BP 124/69, Pulse 96, Temp 98. 4 – No skin lesions – CV – RRR with systolic murmur – Abdomen – NABS, tenderness in the lower abdomen, no masses, no splenectomy – Ext – no edema

Case Presentation • Labs – WBC 15. 3 (45% segs, 38% bands) – Hgb 12 g/dl, ferritin 150, vit B 12 1163 pg/ml – Platelet 137 k, ESR 67 – K 3. 1, chol 123 – Creat 0. 9 – Stool and blood cultures - neg

Case Presentation • Hospital Course – Repeated stool and blood cultures – Solumedrol 60 mg IV continuous infusion – Platelet count decrease • Treated with IVIG – IV Cyclosporine (2 mg/kg) started without significant improvement (received 13 days) • Flex sig – grade 4 colitis (severe)
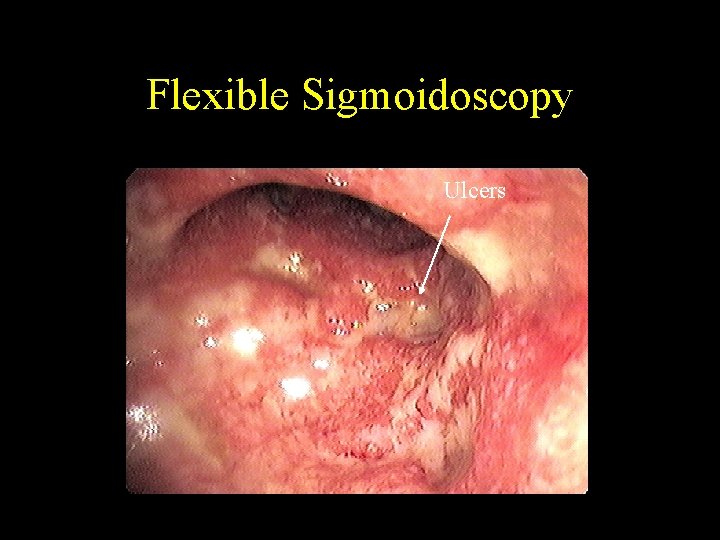
Flexible Sigmoidoscopy Ulcers
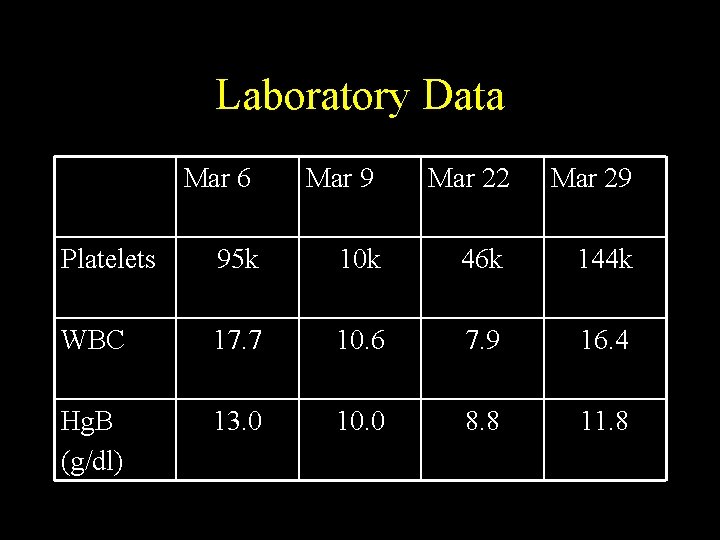
Laboratory Data Mar 6 Mar 9 Mar 22 Mar 29 Platelets 95 k 10 k 46 k 144 k WBC 17. 7 10. 6 7. 9 16. 4 Hg. B (g/dl) 13. 0 10. 0 8. 8 11. 8

Case Presentation 3/23/2005 - underwent lap assisted colectomy with ileostomy 3/27/2005 - discharged home
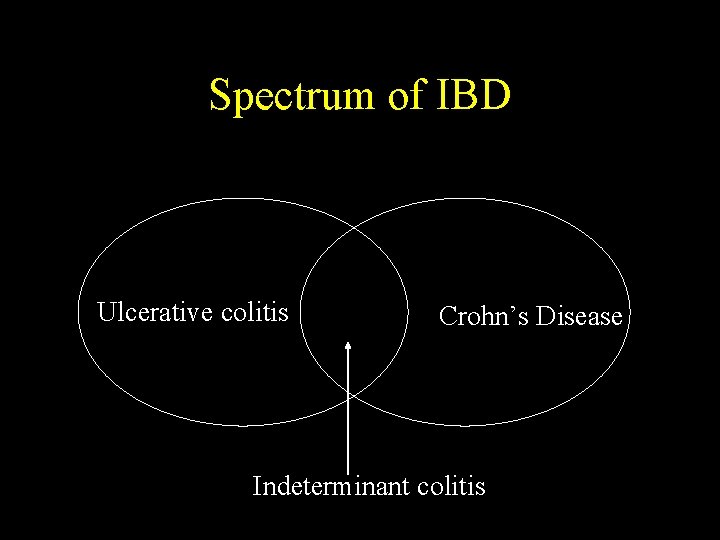
Spectrum of IBD Ulcerative colitis Crohn’s Disease Indeterminant colitis
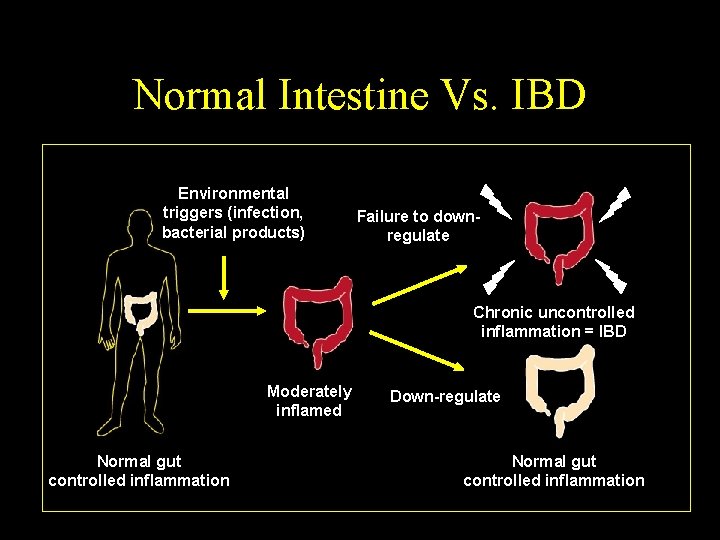
Normal Intestine Vs. IBD Environmental triggers (infection, bacterial products) Failure to downregulate Chronic uncontrolled inflammation = IBD Moderately inflamed Normal gut controlled inflammation Down-regulate Normal gut controlled inflammation
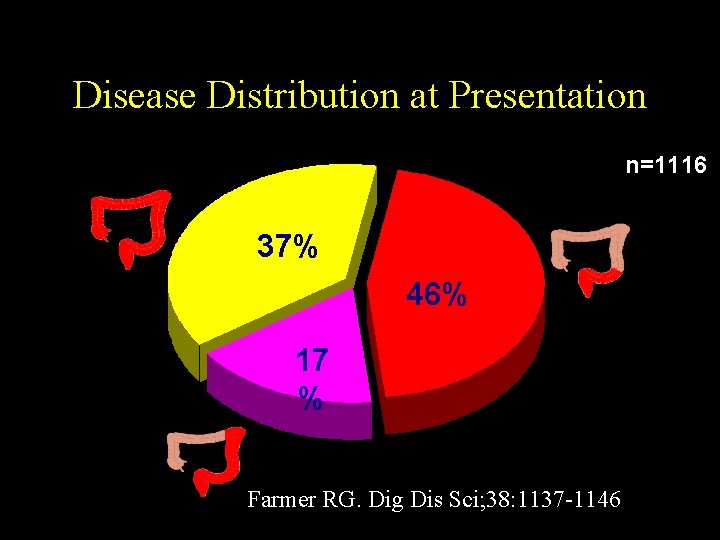
Disease Distribution at Presentation n=1116 37% 46% 17 % Farmer RG. Dig Dis Sci; 38: 1137 -1146
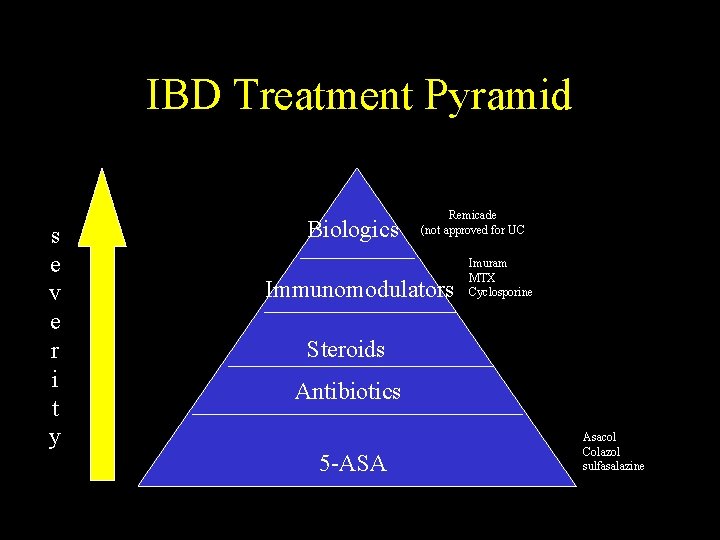
IBD Treatment Pyramid s e v e r i t y Biologics Remicade (not approved for UC Immunomodulators Imuram MTX Cyclosporine Steroids Antibiotics 5 -ASA Asacol Colazol sulfasalazine
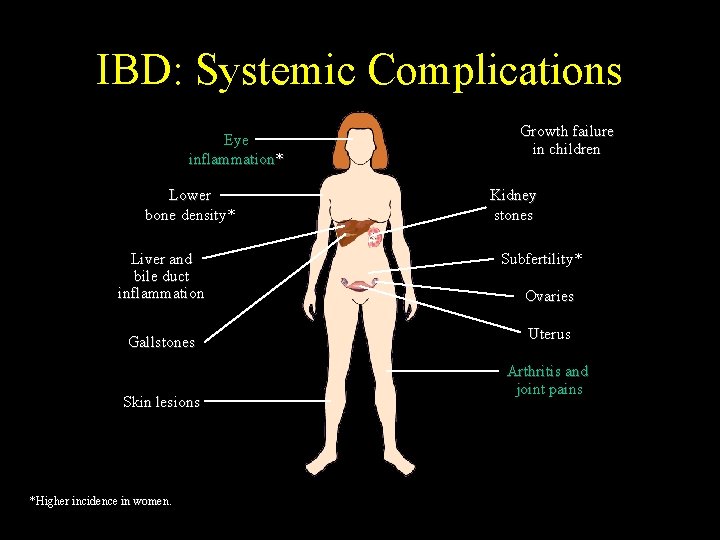
IBD: Systemic Complications Eye inflammation* Lower bone density* Liver and bile duct inflammation Gallstones Skin lesions *Higher incidence in women. Growth failure in children Kidney stones Subfertility* Ovaries Uterus Arthritis and joint pains

EIMs and Response to Treatment • Responds to treatment of underlying bowel disease – Peripheral arthritis – Erythema nodosum – Episcleritis • Independent of treatment of underlying bowel disease – Axial arthritis – Pyoderma gangrenosum – Uveitis – PSC

IBD and Hematology • Anemia is common in patients with IBD – Iron loss – Defective iron transport – Impaired Vitamin B 12 and Folate absorption – Insufficient erythropoietin production – Autoimmune Hemolytic Anemia

ITP and IBD • Not a frequent association • Usually associated with Ulcerative Colitis • Decrease in platelet counts observed during flares • Various treatment modalities used to induce remission

ITP and IBD • 24 cases of IBD in ITP reported – 21 Ulcerative Colitis – 3 Crohn’s Colitis • IBD usually preceeded ITP be several months to years • No standardized approach to therapy • No other cases reported with colectomy only
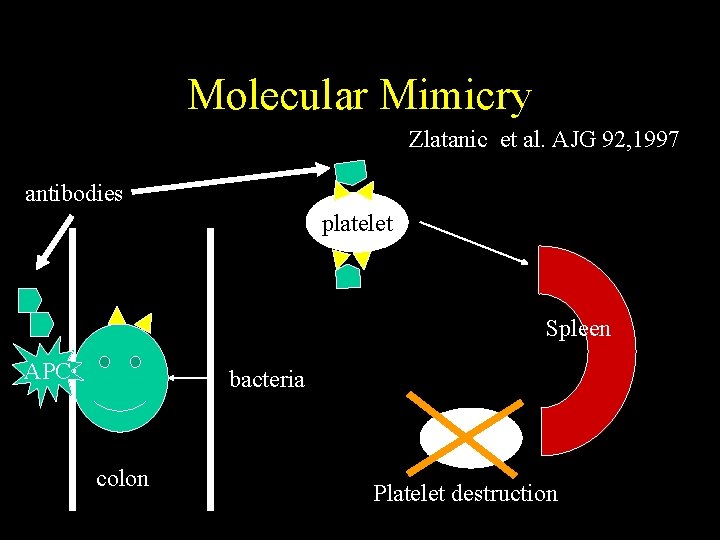
Molecular Mimicry Zlatanic et al. AJG 92, 1997 antibodies platelet Spleen APC bacteria colon Platelet destruction

ITP and IBD • Treatment – Short course of steroids – IVIG – Splenectomy may be required to maintain platelet count • + colectomy if active colitis – Colectomy should be considered if colitis remains active despite medical therapy

Case Presentation (follow up) • Platelet count 275 k on March 31, 2005 • On prednisone taper • Will return in next 2 -3 months for a Ileal pouch anal anastomosis
- Slides: 22