UHC Reaching the missing middle September 30 th

UHC : Reaching the missing middle September 30 th, 2019 Alok Kumar Adviser Health NITI Aayog AB PMJAY , Manthan September 30 -1 October 2019
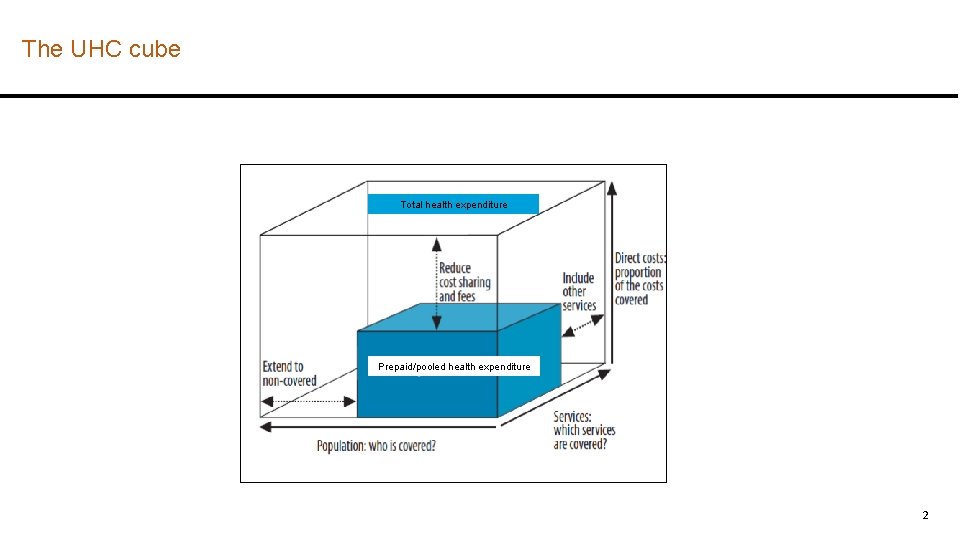
The UHC cube Total health expenditure Prepaid/pooled health expenditure 2
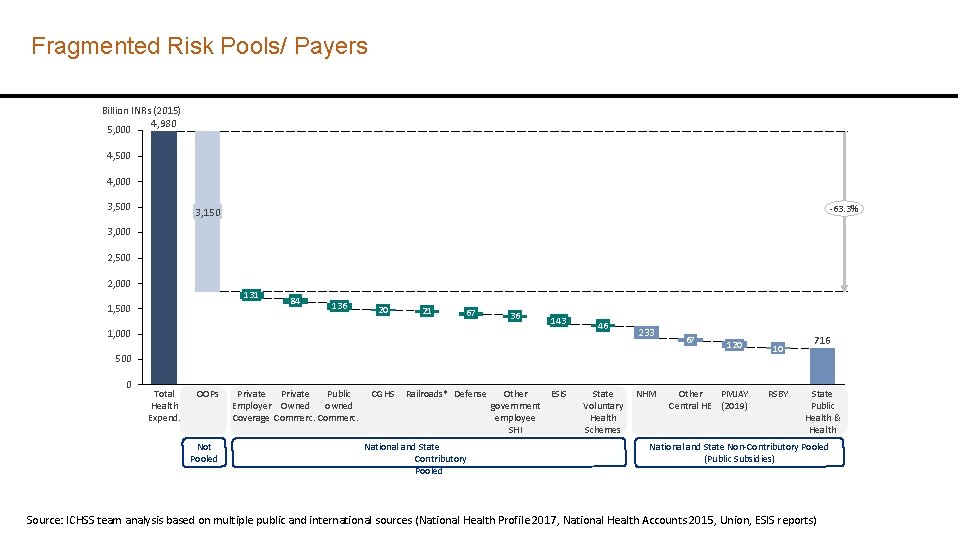
Fragmented Risk Pools/ Payers Billion INRs (2015) 4, 980 5, 000 4, 500 4, 000 3, 500 -63. 3% 3, 150 3, 000 2, 500 2, 000 131 1, 500 84 136 20 21 67 36 1, 000 143 46 233 67 120 500 0 Total Health Expend. OOPs Not Pooled Private Public Employer Owned owned Coverage Commerc. CGHS Railroads* Defense National and State Contributory Pooled Other government employee SHI ESIS State Voluntary Health Schemes NHM Other PMJAY Central HE (2019) 10 RSBY 716 State Public Health & Health National and State Non-Contributory Pooled Coenletders (Public Subsidies) Po (Public Subsidies) Source: ICHSS team analysis based on multiple public and international sources (National Health Profile 2017, National Health Accounts 2015, Union, ESIS reports) 3
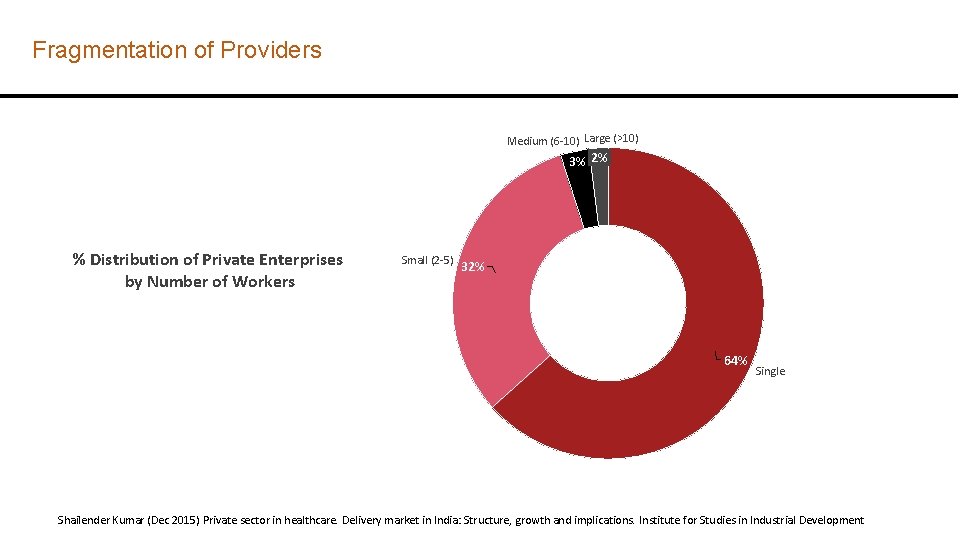
Fragmentation of Providers Medium (6 -10) Large (>10) 3% 2% % Distribution of Private Enterprises by Number of Workers Small (2 -5) 32% 64% Single Source: Shailender Kumar (Dec 2015) Private sector in healthcare. Delivery market in India: Structure, growth and implications. Institute for Studies in Industrial Development 4
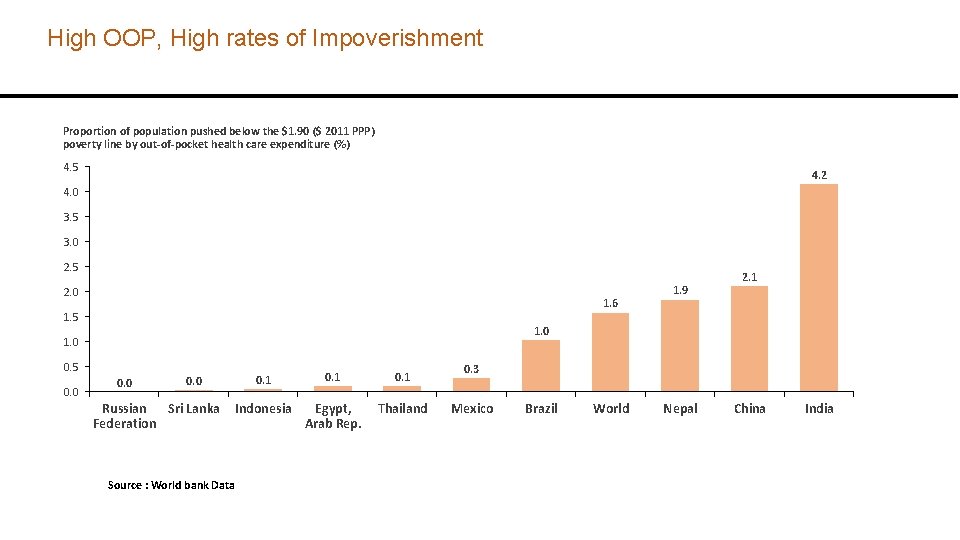
High OOP, High rates of Impoverishment Proportion of population pushed below the $1. 90 ($ 2011 PPP) poverty line by out-of-pocket health care expenditure (%) 4. 5 4. 2 4. 0 3. 5 3. 0 2. 5 2. 0 1. 6 1. 5 2. 1 1. 0 0. 5 0. 0 1. 9 0. 0 Russian Sri Lanka Federation 0. 1 Indonesia Egypt, Arab Rep. Thailand 0. 3 Mexico Brazil World Nepal China India Source : World bank Data source: World Bank Data 5
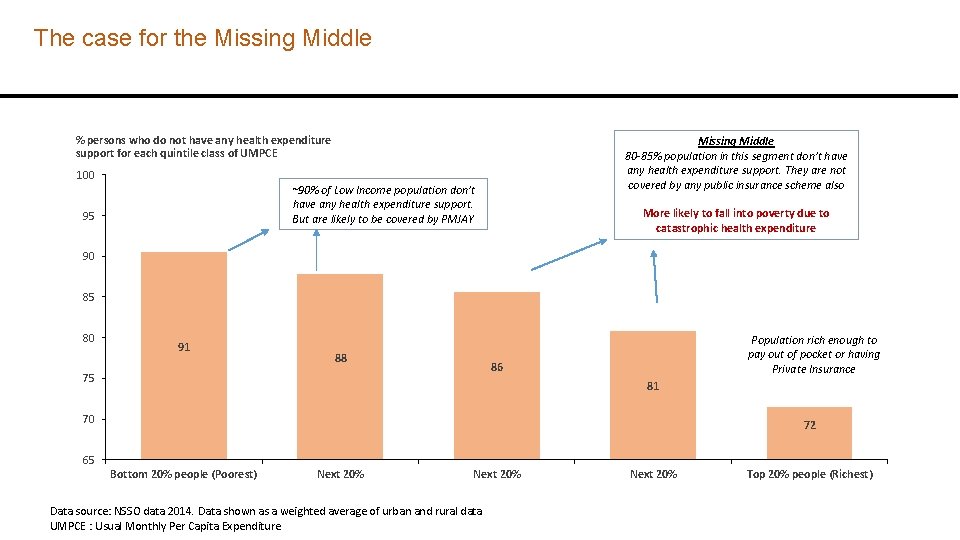
The case for the Missing Middle % persons who do not have any health expenditure support for each quintile class of UMPCE Missing Middle 80 -85% population in this segment don’t have any health expenditure support. They are not covered by any public insurance scheme also 100 ~90% of Low Income population don’t have any health expenditure support. But are likely to be covered by PMJAY 95 More likely to fall into poverty due to catastrophic health expenditure 90 85 80 91 88 Population rich enough to pay out of pocket or having Private Insurance 86 75 81 70 72 65 Bottom 20% people (Poorest) Next 20% Data source: NSSO data 2014. Data shown as a weighted average of urban and rural data UMPCE : Usual Monthly Per Capita Expenditure Next 20% Top 20% people (Richest) 6
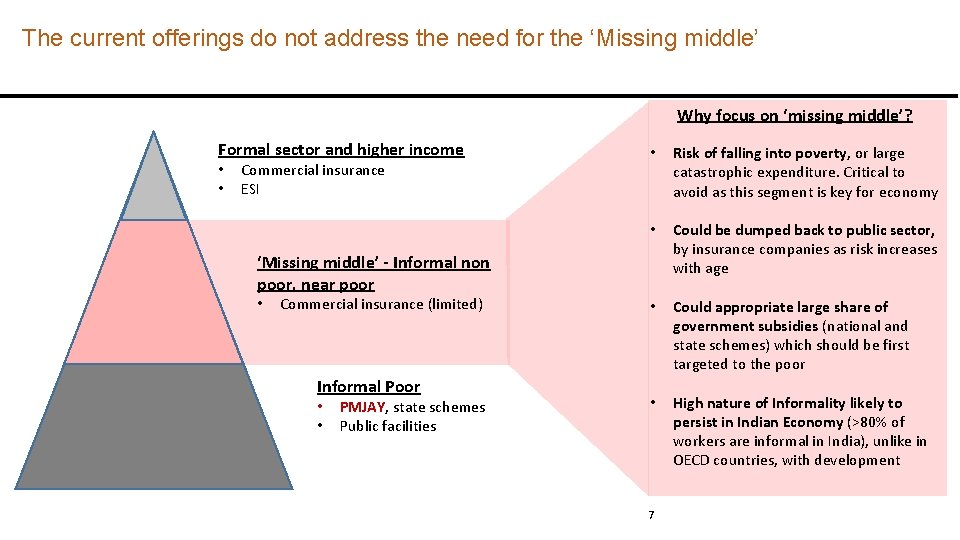
The current offerings do not address the need for the ‘Missing middle’ Why focus on ‘missing middle’? Formal sector and higher income • • Commercial insurance ESI • Risk of falling into poverty, or large catastrophic expenditure. Critical to avoid as this segment is key for economy • Could be dumped back to public sector, by insurance companies as risk increases with age • Could appropriate large share of government subsidies (national and state schemes) which should be first targeted to the poor • High nature of Informality likely to persist in Indian Economy (>80% of workers are informal in India), unlike in OECD countries, with development ‘Missing middle’ - Informal non poor, near poor • Commercial insurance (limited) Informal Poor • • PMJAY, state schemes Public facilities 7

Situation for middle India (informal non poor) today Covered today Inadequate coverage: Multiple exclusions, waiting periods of 3 -4 years, retail offerings preferably to the healthy and the young population High premium contributions– More than Rs. 15, 000 per annum for a cover of Rs. 5 Lakh for a family of 3 - 1. 5 -2 x higher than group insurance >10 x higher than PMJAY Not covered No adequate product at right price offered – Covers only IPD and day care with waiting periods Distribution limited to tier I and II cities mostly No incentives to join contributory schemes vs using fully subsidized healthcare Low claims payout for individual health segment 8

Design elements • Standardized, simple PMJAY+ product offering • Channeled through choice of contributory insurers via enrollment of groups • Some Government support/subsidy to stabilize the product for middle India • An institutional mechanism to ensure quick roll out • Strong governance and regulations to ensure success 9

Approach COLLABORATION & CONSULTATIONS EXPERIMENTATION & INNOVATION • IRDAI • Insurers (general, life, health, ESI) • Professional Groups • Digital companies • Experts • Others • Group enrollment for informal middle India • Right benefits package • Low cost distribution, exchanges • Reduced overhead costs • . . 10

Coverage for all 11
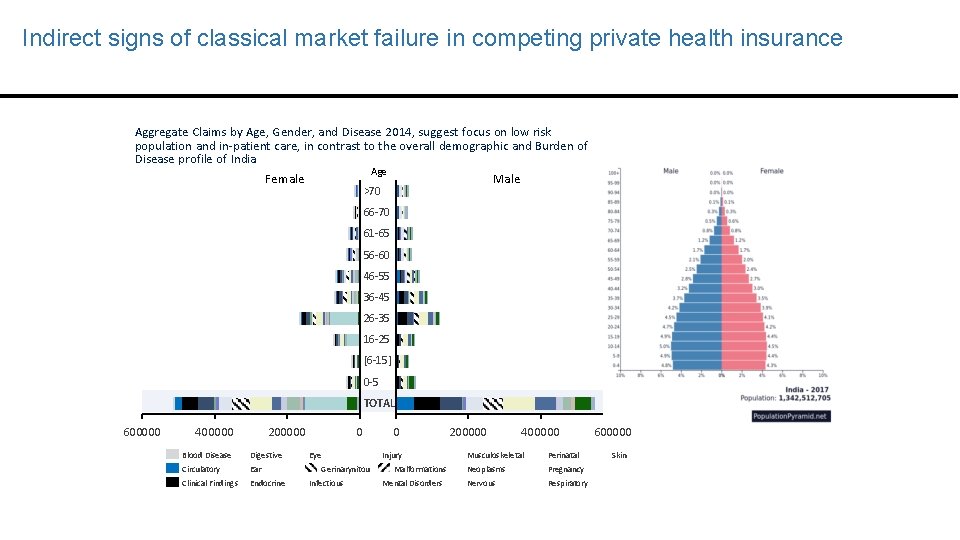
Indirect signs of classical market failure in competing private health insurance Aggregate Claims by Age, Gender, and Disease 2014, suggest focus on low risk population and in-patient care, in contrast to the overall demographic and Burden of Disease profile of India Age Female Male >70 66 -70 61 -65 56 -60 46 -55 36 -45 26 -35 16 -25 [6 -15] 0 -5 TOTAL 600000 400000 200000 Blood Disease Digestive Circulatory Ear Clinical Findings Endocrine 0 Eye Gerinarynitou Infectious 0 Injury Malformations Mental Disorders 200000 400000 Musculoskeletal Perinatal Neoplasms Pregnancy Nervous Respiratory 600000 Skin
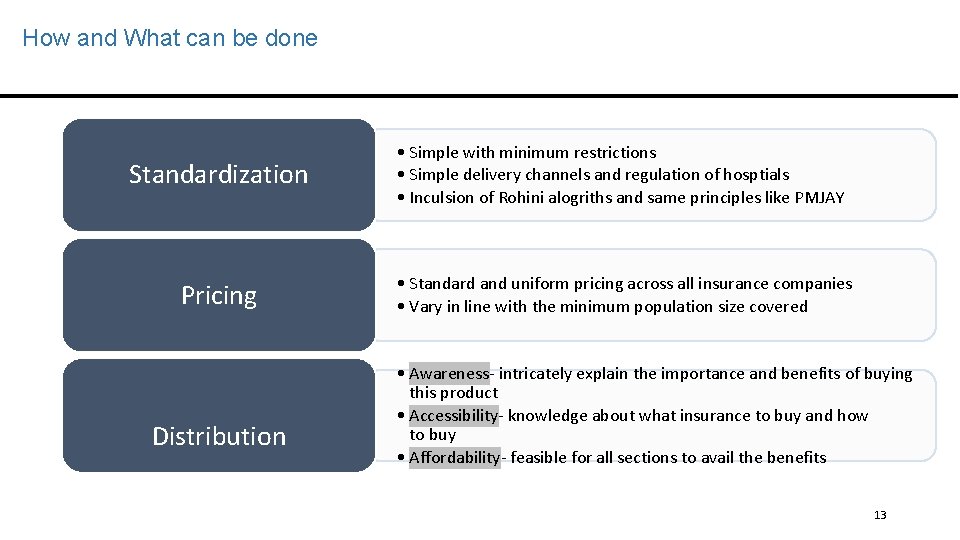
How and What can be done Standardization • Simple with minimum restrictions • Simple delivery channels and regulation of hosptials • Inculsion of Rohini alogriths and same principles like PMJAY Pricing • Standard and uniform pricing across all insurance companies • Vary in line with the minimum population size covered Distribution • Awareness- intricately explain the importance and benefits of buying this product • Accessibility- knowledge about what insurance to buy and how to buy • Affordability- feasible for all sections to avail the benefits 13
- Slides: 13