UGI Bleeding Epidemiology of Upper GI Bleeding Bleeding
UGI Bleeding

Epidemiology of Upper GI Bleeding • • • Bleeding from a source above the ligament of Treitz 1 case/1, 000 adults/year 50% of cases are peptic ulcer disease (25% rebleed) 40 -80% of cases of bleeding cease spontaneously 10% mortality rate

Prognostic Factors • Hemodynamic instability • Hematochezia from upper GI source • Increasing number of units transfused • Age > 60 years • Concurrent illness (cardiac, respiratory, renal, neoplastic, CNS) • Onset while hospitalized for other reason Coagulopathy •

Etiology of UGI Bleeding Non GI • Hemopytsis, nose bleed Esophageal • Esophagitis, ulcer, varices, malignancy, MW tear Gastric • Gastritis, ulcer, varices, malignancy, AVM Duodenal • Duodenitis, ulcer, varices, malignacy (rare), AVM, aortoenteric fistula

Etiology Incidence 1. 2. 3. 4. 5. 6. 7. 8. PUD 50% Esophagitis 15% Gastritis 10% Varices 10% Duodenitis 5% MW tear 3% (much more common in young) Esophageal ulcer 3% Carcinoma 3%

Presentation • Melena or hematochezia 70% (charting, iron pepto) • Hematemesis or coffee ground emesis 30% (charting, testing) • Syncope 14%, presyncope 40% • Heartburn 40%, epigastric pain 20% • Dysphagia 10% • Wt. loss 12%

Important History • Evidence of complications CP/SOB/presyncope • Appearance, frequency and amount of vomit/BM (elderly unreliable) • Duration of symptoms • Use of NSAID/ASA/corticosteroids • Previous history of GI bleeding • Co-morbidities = cardiac, respiratory, neoplastic, CNS

Physical Exam • • ABC’s Vitals Orthostatic bp (scoping) Rectal exam (what does –ve OB really mean)

Initial Management • • • ABC’s Npo Head down, raise legs 2 IV’s CBC Urea/Cr (? upper vs lower bleeding, ? reliable) G&T LFTs Coagulation status ECG/cardiac enzymes NG?
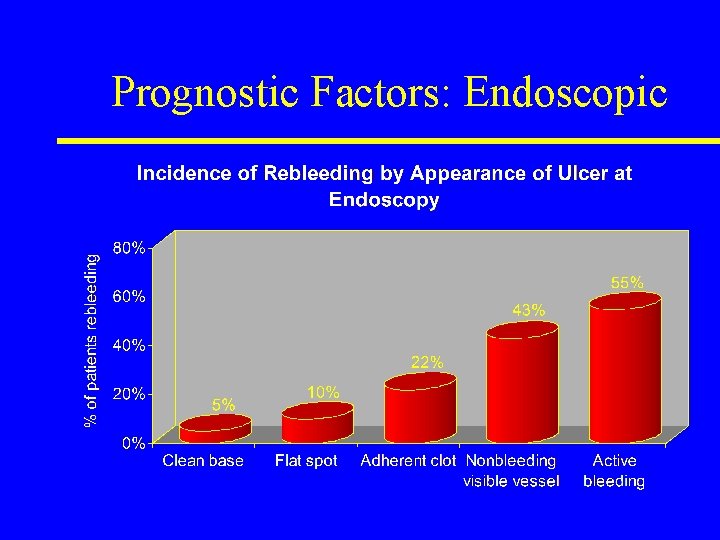
Prognostic Factors: Endoscopic Laine, Peterson, N Engl J Med 1994.
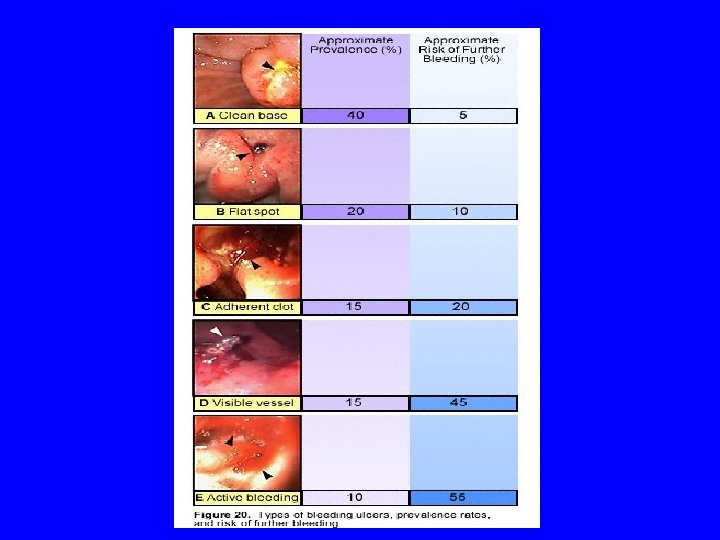
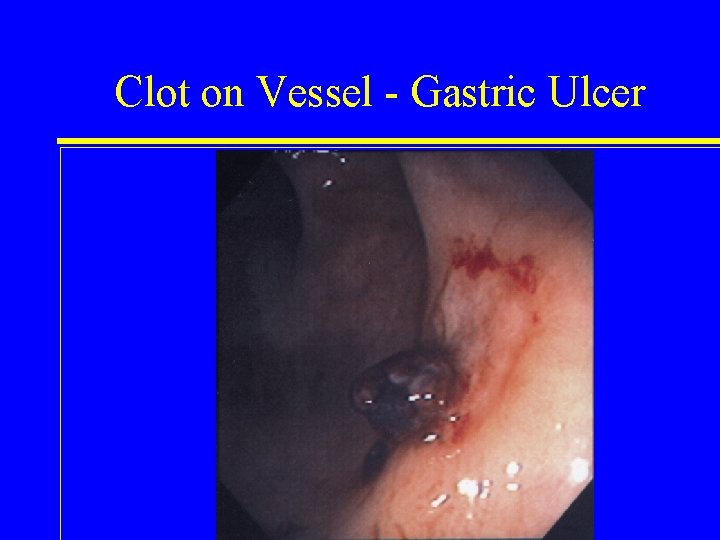
Clot on Vessel - Gastric Ulcer

Overview of Management • Initial management • Endoscopic therapy • Surgical therapy • Pharmacologic therapy

Endoscopic Therapy • Perform early (ideally within 24 h) • Indications for haemostatic therapy: • (1) +/-Adherent clot, (2) Nonbleeding visible vessel, (3) Active bleeding (oozing, spurting) (Laine, Peterson. 1994) • Heater probe, bipolar electrocoagulation or injection therapy • Decreases in rebleeding, surgery and mortality (Cook, et al. 1992, Sacks, et al. 1990)

Surgical Therapy • Endoscopic management failure • Other extenuating circumstances • Patient survival improved by optimal timing • Individualized by clinical context, endoscopic and surgical expertise

Surgical Therapy Outcomes in 92 patients with rebleeding after endoscopic therapy: endoscopic retreatment vs. surgery. Lau, et al. NEJM 1999. N/A=not

Pharmacologic Therapy • Splanchnic blood pressure modifiers • • Anti-fibrinolytic agents • • vasopressin, somatostatin, octreotide tranexamic acid Acid suppressing agents • H 2 -receptor antagonists (H 2 RAs), proton pump inhibitors (PPIs)

Somatostatin/Octreotide • Effects: • • Lowers splanchnic blood pressure Decreases gastric acid secretion Increases duodenal bicarbonate secretion Meta-analysis: (Imperiale, Birgisson, 1997) • • 14 trials (n=1, 829); SOM (12 trials), OCT (2 trials) 0. 53 risk of rebleeding vs. H 2 RAs RR=0. 73 among investigator-blinded trials Studies did not control for confounders, i. e. , endoscopic therapy

Acid Suppressing Agents • H 2 -receptor antagonists (H 2 RAs) • • Cimetidine, ranitidine, famotidine, nizatidine Proton pump inhibitors (PPIs) • • • Pantoprazole, omeprazole (oral, IV) Esomeprazole (Nexium) (oral) Lansoprazole (oral)

Role of Acid in Hemostasis • Impairs clot formation • • Accelerates clot lysis • • Impairs platelet aggregation & causes disaggregation Predominantly acid-stimulated pepsin May impair integrity of mucus/bicarbonate barrier
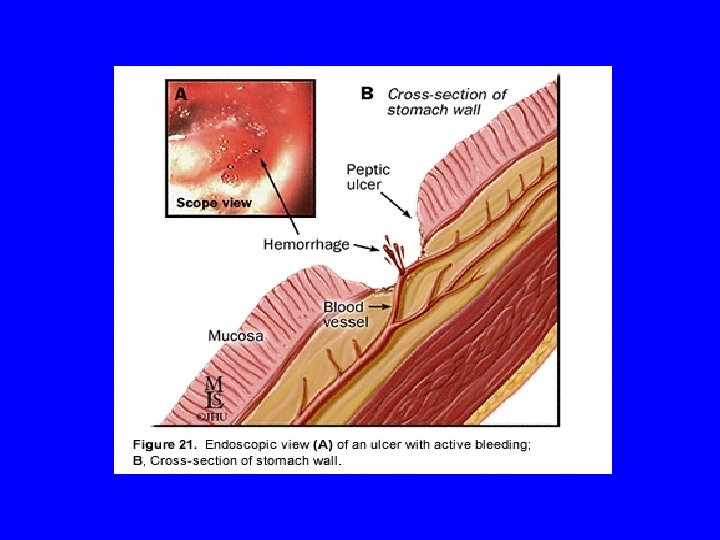

Effect of PPI on Gastric p. H • Increase intragastric p. H • p. H>6. 0 for 84 ->99% of day • Continuous infusion (CI) superior to intermittent bolus administration • Clinical improvements in rebleeding and/or surgery with: Bolus 80 mg + CI 8 mg/h

Role of PPI For UGI Bleeding: Summary of Clinical Trials • 10 RCTs • PPI (n=1, 150); controls (n= 1, 142) • Minimal benefit with intermittent bolus • Clinical benefits with bolus plus continuous infusion (CI) • • Decreased need for surgery and/or rebleeding Dose: Bolus 80 mg + CI 8 mg/h x 3 d

Role of PPI For Upper GI Bleeding: Summary • H 2 RAs • Unlikely to provide necessary p. H increases • • • Tolerance a problem Minimal benefit in clinical trials PPIs can provide profound acid suppression • • • p. H>6. 0 over 24 -hours Suggested benefits on rebleeding and/or need for surgery Mortality benefits not yet demonstrated

Role of PPI For Upper GI Bleeding: Summary • Reasonable to consider initiating as soon as possible following presentation to hospital • Administer as bolus + continuous infusion (CI) • IV bolus 80 mg + CI 8 mg/h x 3 d • Continue therapy, probably with an oral PPI • Likely most beneficial for patients with high risk, nonactively bleeding lesions • Further trials needed to determine optimal patient group for acute IV PPI therapy
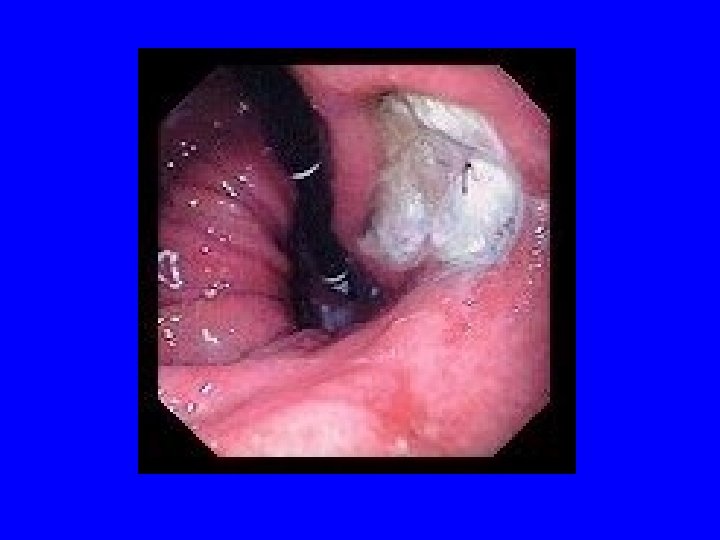

Peptic Ulcer Disease Causes: • Infectious: H. P. , Herpes, CMV • Drugs: NSAIDS, corticosteroids • Neoplastic • ICU Stress Types: • DU = pain between meals • GU = pain with meals, epigastric
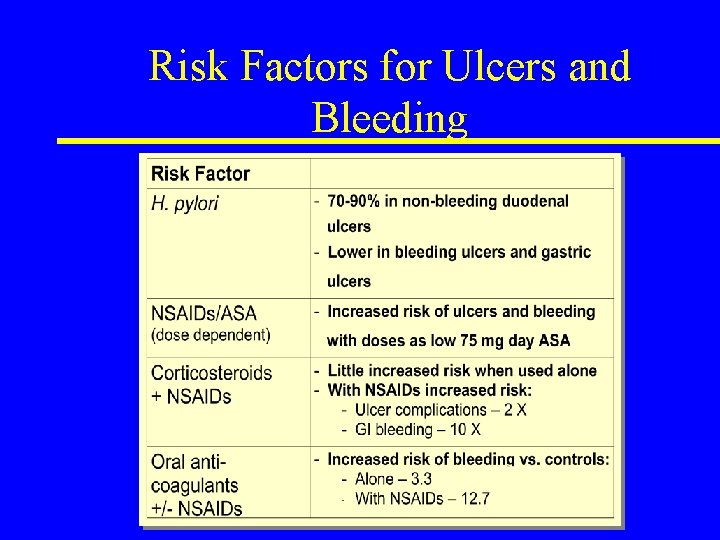
Risk Factors for Ulcers and Bleeding

Peptic Ulcer Disease – Helicobacter Pylori • Most common chronic bacterial infection in man • 15% of infected go on to PUD • Dx via C 13/C 14 breath testing, histology, serology, urease testing (5 -15% false negative) – false negative if ABO or acid suppression within the last week (except serology) • Serology $30 (not for eradication) • Breath Testing 13 C non-radioactive urea metabolized to CO 2 exhaled and quantified

Peptic Ulcer Disease – When to Test for H. P. • GU = test for H. P. as other causes of GU are common, especially NSAID induced ulcers, maliganancy (repeat endoscopy) • DU = if not on NSAID may treat empirically for H. P.

Helicobacter Pylori Eradication • Proven to decrease ulcer recurrence/bleeding • Tx if any history of upper GI bleeding and H. P. positive Treatment Options: • PCA= PPI + Clarithomycin 500 mg bid + Amoxil 1 g bid for 7 days • PCM = PPI + Clarithoromycin 500 mg bid + Metronidazole 500 mg bid X 7 days (resistance)

H. P. Eradication • Antibiotics are very effective • Test for eradication only in complicated ulcer disease eg. bleeding, pyloric outlet obstruction, recurrent ulceration or persistent symptoms • Most cost effective method = breath testing – 1/12 after antibiotics are complete – 7/7 after stopping acid suppression

NSAID And Upper GI Ulceration • 2 -4% annual risk of PUD related complication on NSAID (bleeding, outlet obstruction, symptomatic ulcer) • Lowest possible dose of NSAID/ASA (2 -4 X risk even if <325 mg ASA daily) • Prophylaxis if: – Previous PUD or GI bleed – NSAID + corticosteroids – >65 (75 in Ontario guidelines) – serious comorbidity

NSAIDS & UGI Bleeding • Classic NSAID inhibit COX-1 and COX-2 • Inhibition of COX 1 results in decreased gastric PG and hence poor protective barrier in the GI tract • COX-2 expressed predominantly in actively inflammed tissues, therefore less damage to normal GI tract • COX-2 ulcer risk approx to that of classic NSAID + PPI
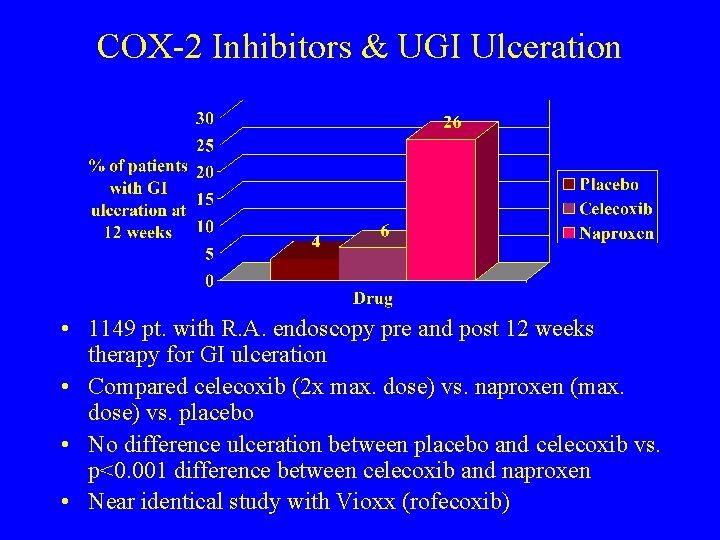
COX-2 Inhibitors & UGI Ulceration • 1149 pt. with R. A. endoscopy pre and post 12 weeks therapy for GI ulceration • Compared celecoxib (2 x max. dose) vs. naproxen (max. dose) vs. placebo • No difference ulceration between placebo and celecoxib vs. p<0. 001 difference between celecoxib and naproxen • Near identical study with Vioxx (rofecoxib)

NSAIDS and UGI Bleeding Prophylaxis Options: • Misoprostol 200 mg qid + standard NSAID – Side effects diarrhea, cramps – $38/month, 4% S/E • PPI + standard NSAID – More effective than Misoprostol – $53/month (Pantoprazole) • Cox – 2 inhibitor ($40 -75/month) – ? Add PPI

NSAIDS, H. P. And UGIB Prophylaxis • In high risk patients (previous PUD or ongoing dyspepsia), test and treat for H. P. prior to NSAID initiation decreases risk UGI to that of PPI or celebrex • How to test • Time consideration of breath testing • Most bleeds in first month • Previous studies show no benefit for primary prophylaxis with H. P. eradication if already on an NSAID
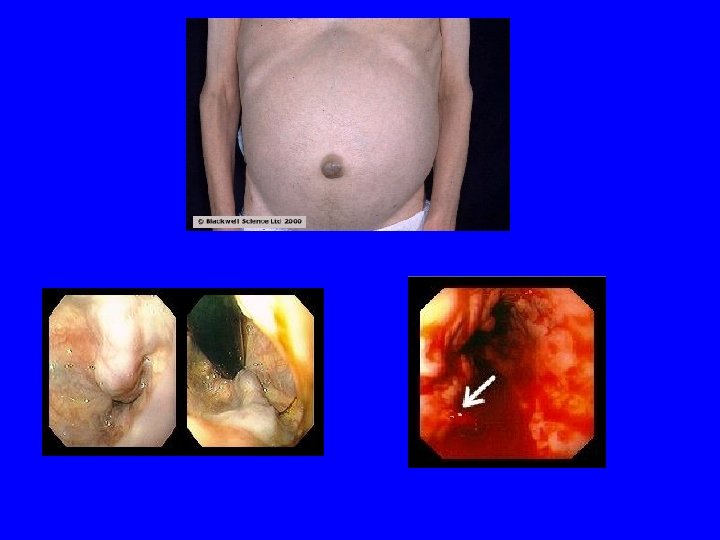
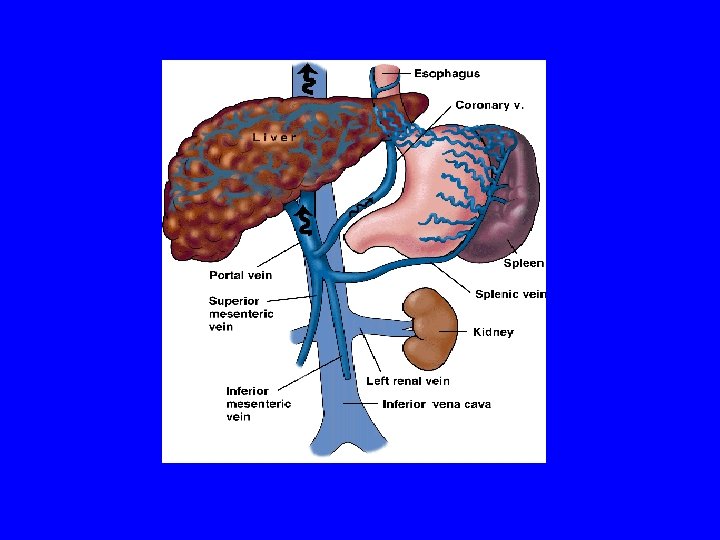

Esophageal Variceal Bleeding • BE SUPICIOUS, if patient is cirrhotic/heavy drinker think varices first • 30 -50% mortality without early intervention • Causes of death are classically aspiration, sepsis, renal failure or encephalopathy • Treatment options: - Medical - endoscopic - Tamponade - TIPS - Surgical
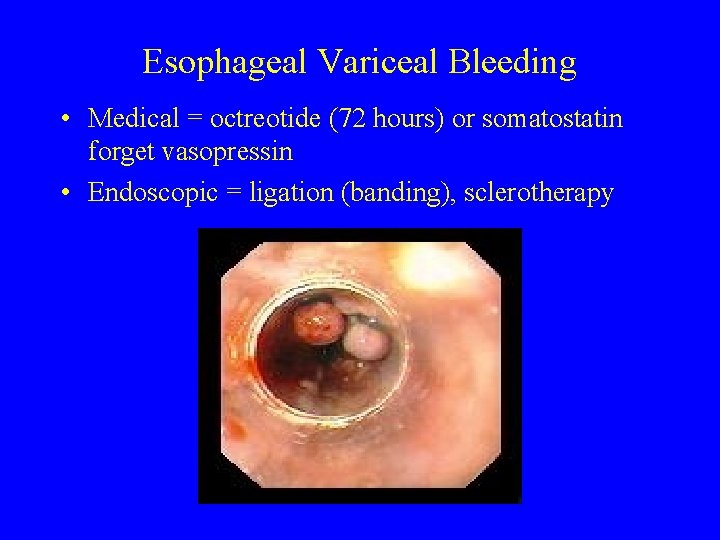
Esophageal Variceal Bleeding • Medical = octreotide (72 hours) or somatostatin forget vasopressin • Endoscopic = ligation (banding), sclerotherapy
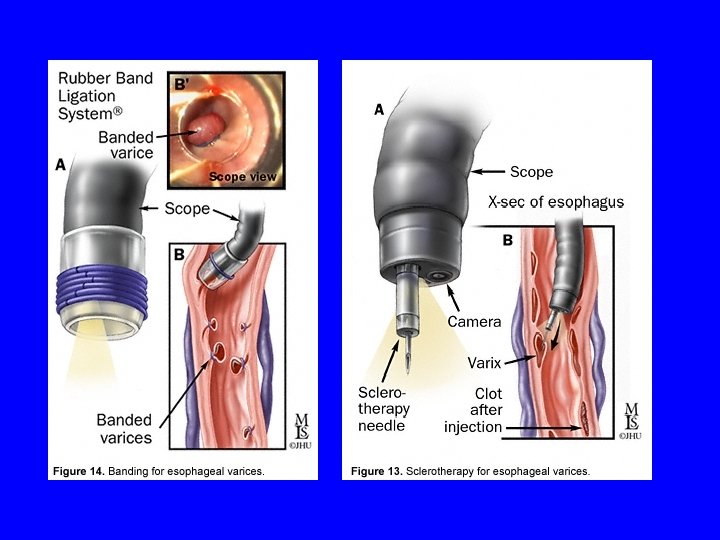
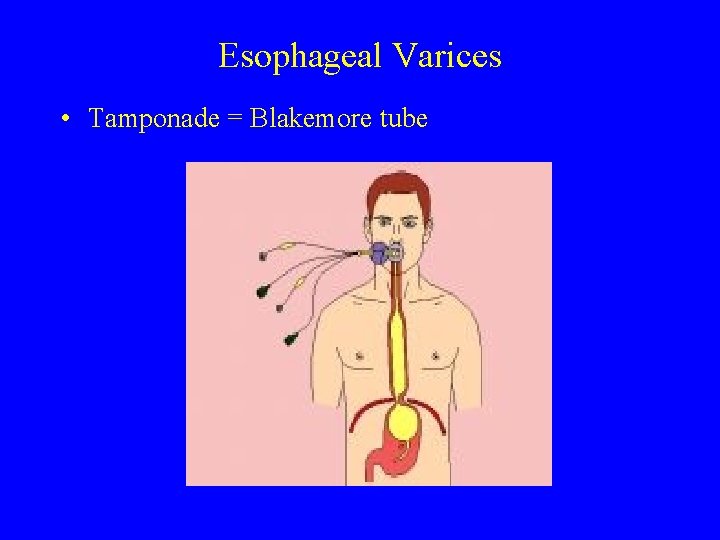
Esophageal Varices • Tamponade = Blakemore tube
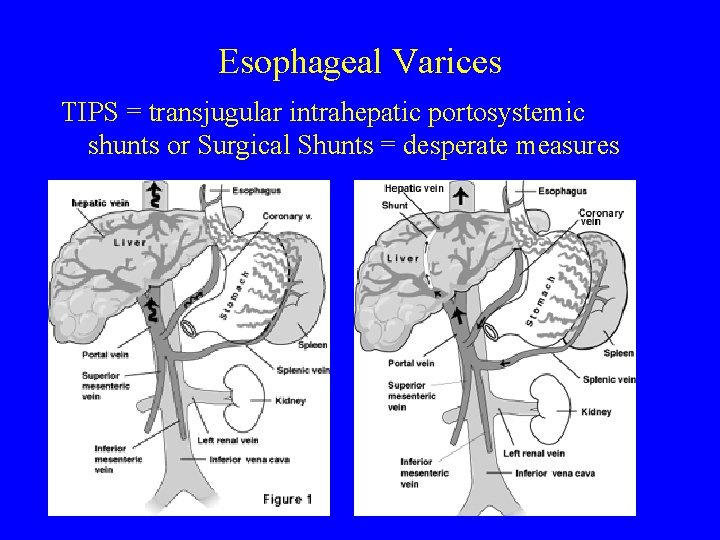
Esophageal Varices TIPS = transjugular intrahepatic portosystemic shunts or Surgical Shunts = desperate measures
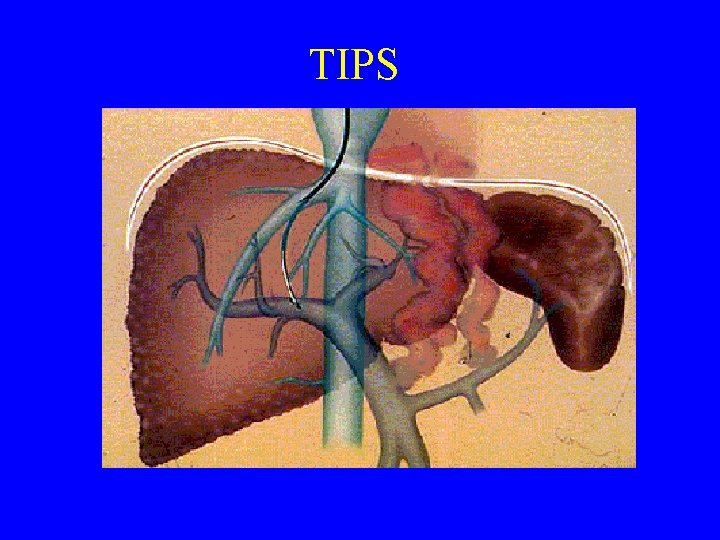
TIPS
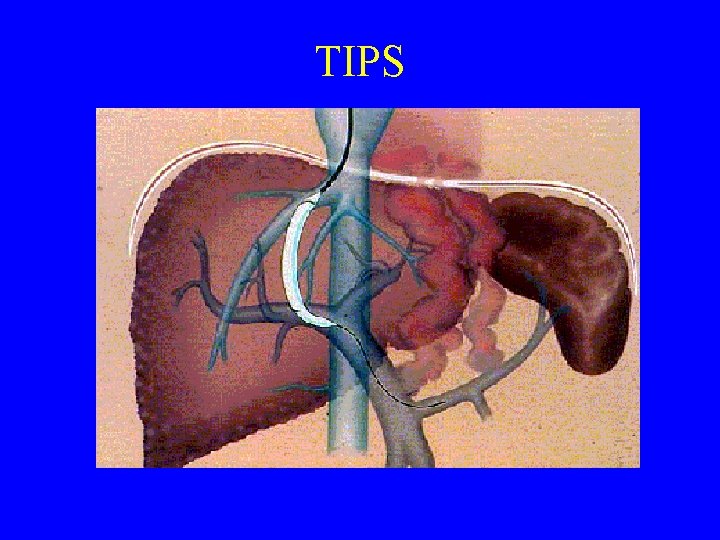
TIPS
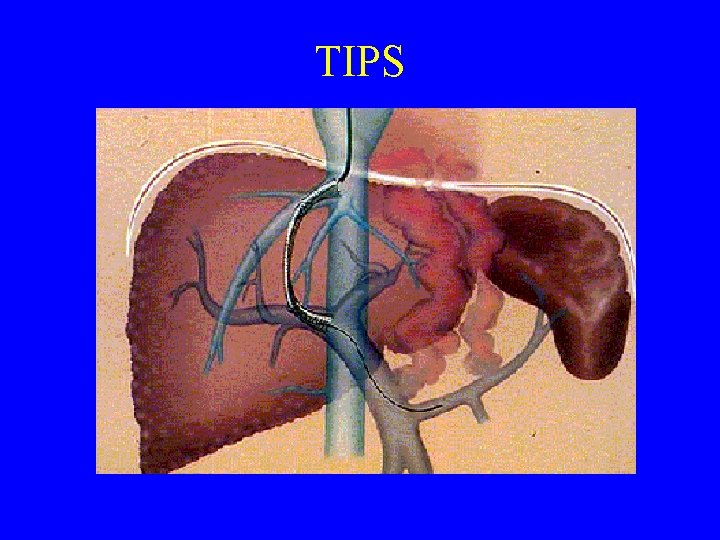
TIPS

- Slides: 49