Tumours of Nasopharynx Dr Mubeena ANATOMY OF NASOPHARYNX

Tumours of Nasopharynx Dr Mubeena
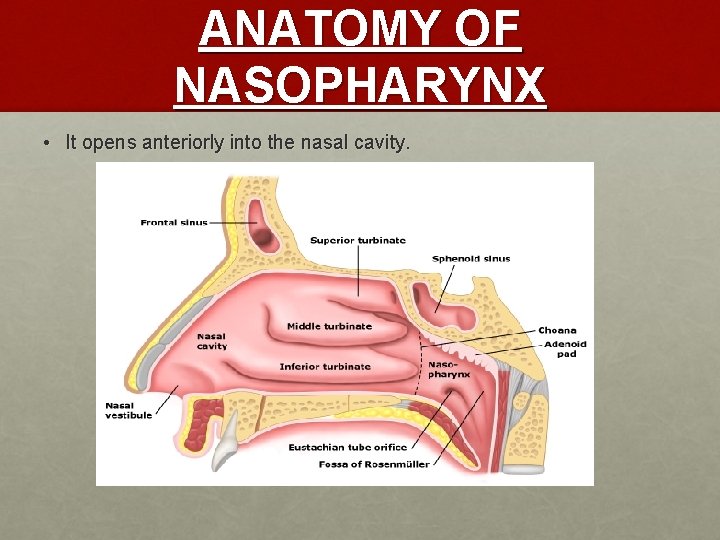
ANATOMY OF NASOPHARYNX • It opens anteriorly into the nasal cavity.
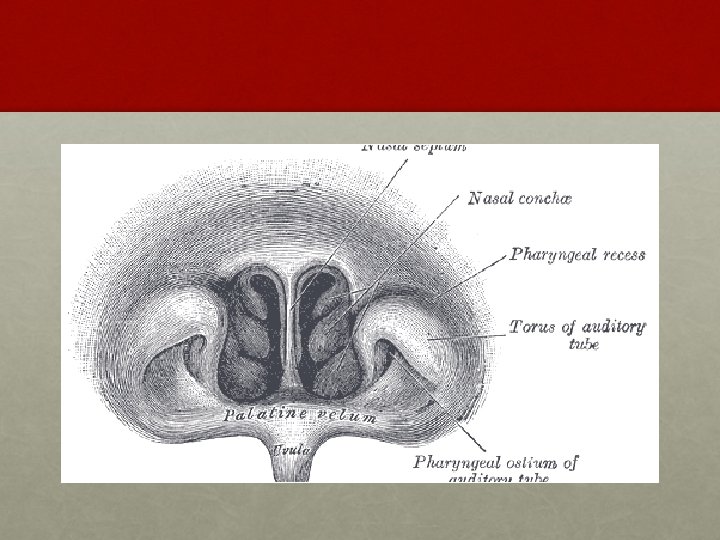

Benign tumors of nasopharynx

Juvenile nasopharyngeal angiofibroma
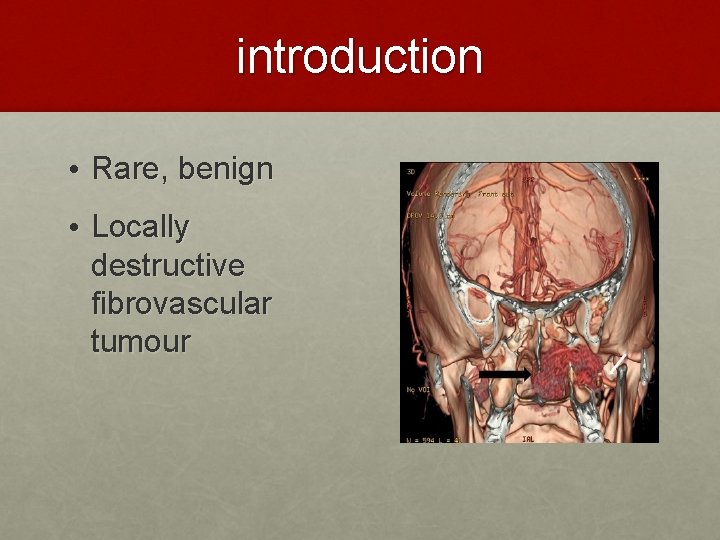
introduction • Rare, benign • Locally destructive fibrovascular tumour

Epidemiology • Males • Teenage, young adult • Hamartomatous nidus of vascular tissue which get activated to form angiofibroma when male sex hormone is released. • Extremely rare in female/ patient older than 25
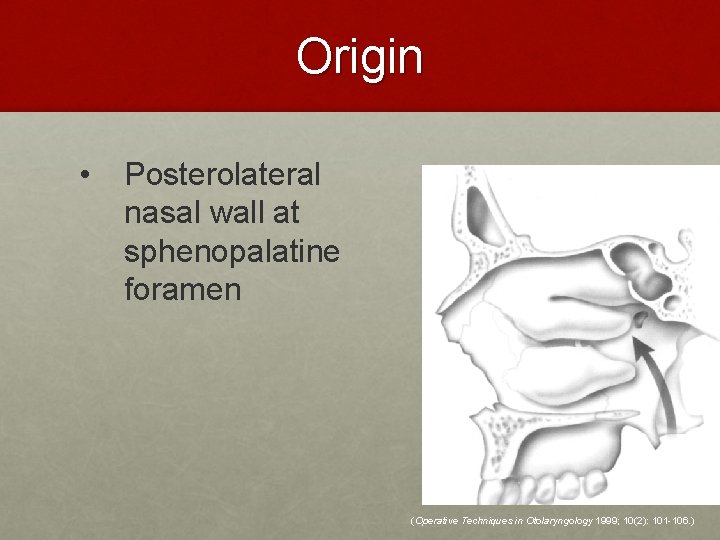
Origin • Posterolateral nasal wall at sphenopalatine foramen (Operative Techniques in Otolaryngology 1999; 10(2): 101 -106. )
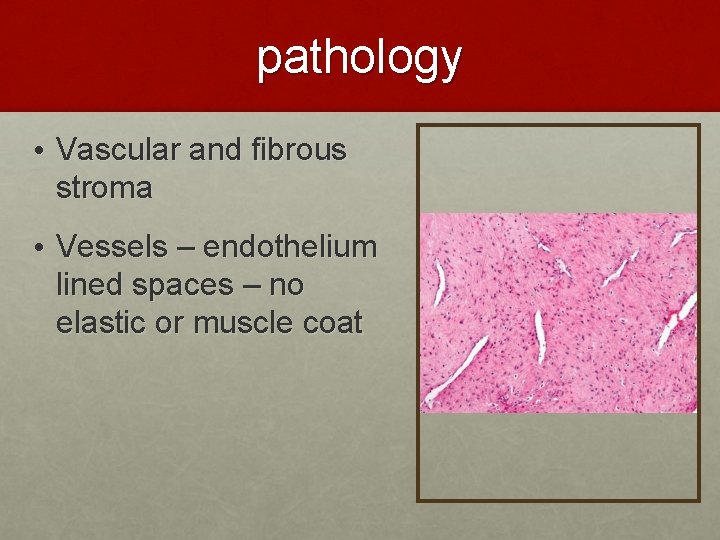
pathology • Vascular and fibrous stroma • Vessels – endothelium lined spaces – no elastic or muscle coat

Spread

CLINICAL FEATURES: § Profuse and recurrent epistaxis. § Progressive nasal obstruction and hyponasal voice. § Conductive hear loss and middle ear effusion. § Extension of tumor in different directions produces symptoms like facial swelling, proptosis, diplopia, broadening of nasal bridge, palatal buldge and cranial nerve palsies.
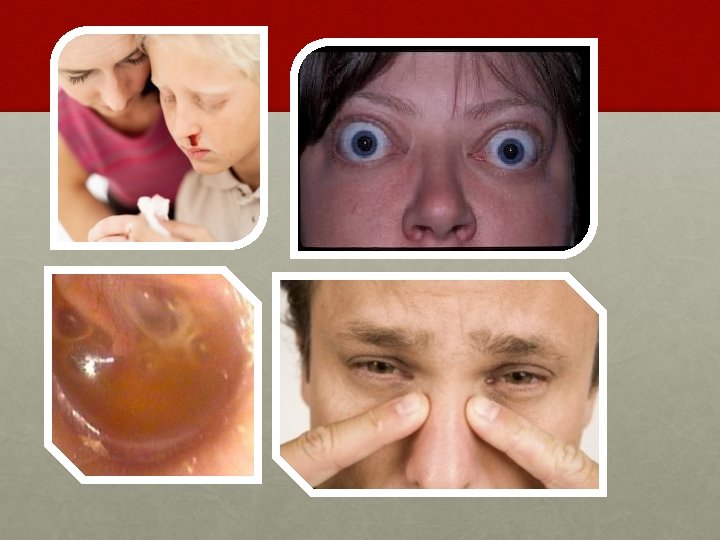
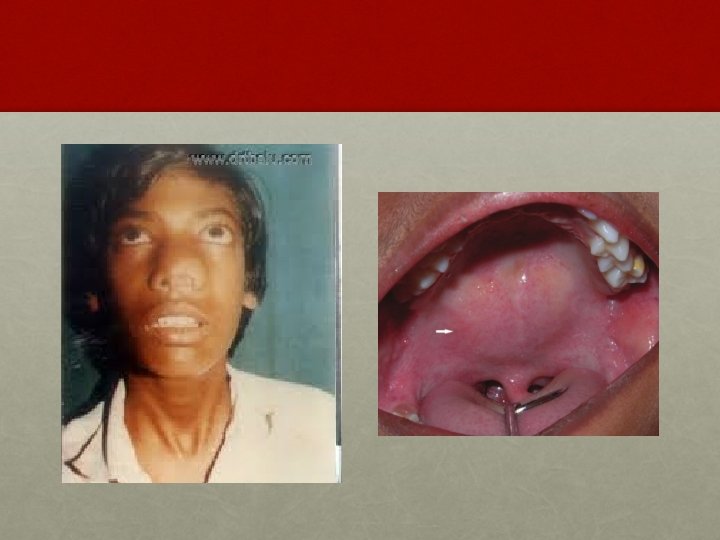

INVESTIGATION: • Contrast enhanced CT scan of nose and PNS • Holman Miller sign/ Antral sign • MRI – soft tissue extent
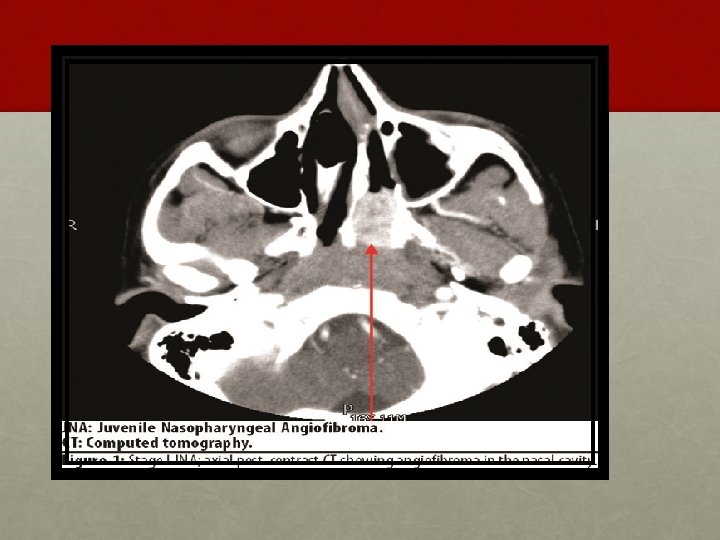
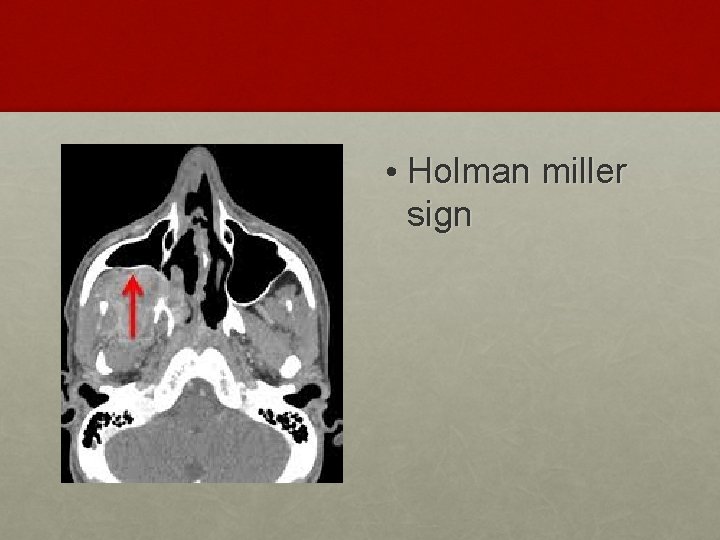
• Holman miller sign
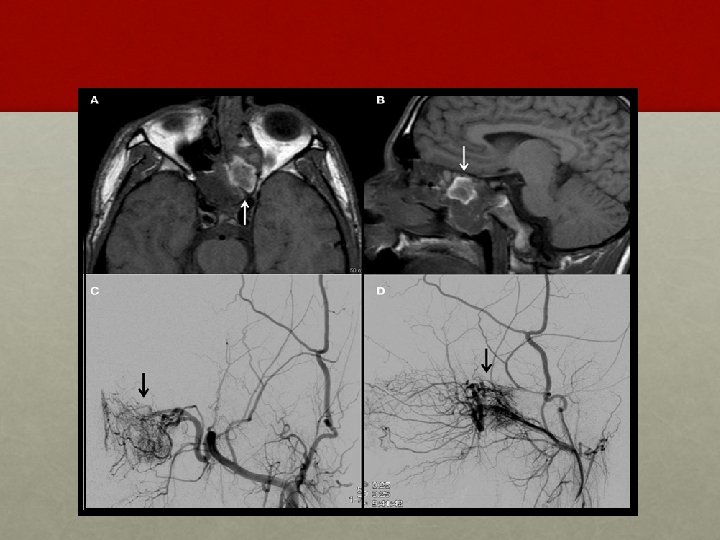
• ANGIOGRAPHY: • Carotid or four vessel angiography - vascular nature of the tumour, its feeding vessels and extension of the tumour. • In addition during angiography embolization of the feeding vessel with gelfoam can be done pre-operatively to shrink the tumour and reduce bleeding during surgery. • BIOPSY: controversial
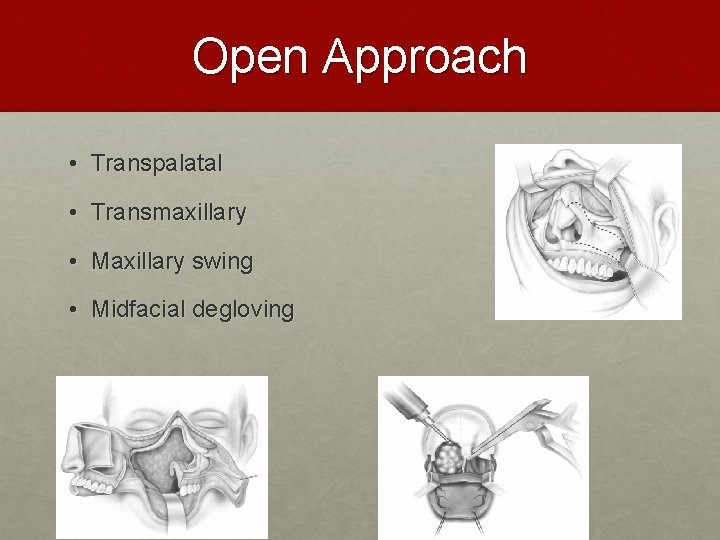
Open Approach • Transpalatal • Transmaxillary • Maxillary swing • Midfacial degloving

Endoscopic • Shift towards endoscopic approach in last 10 years • Mostly for early disease

Endoscopic Technique

§ RADIOTHERAPY: § A dose of 3000 to 3500 c. Gy in 15 -18 fractions is delivered in 3 weeks. Tumour regresses slowly in about a year sometimes even upto 3 years. § CHEMOTHERAPY: § Recurrent and residual lesions - doxorubicin, vincristine, and dacarbazine in combination. § HORMONAL: Diethylstilboestrol and flutamide.

OTHER BENIGN TUMORS • TERATOMA • PLEOMORPHIC ADENOMA • CHORDOMA • HAMARTOMA • CHORISTOMA • PARAGANGLIOMA

Malignant tumors of nasopharynx

Nasopharyngeal carcinoma

Epidemiology • Chinese native > Chinese immigrant > North American native • Both genetic and environmental factors • India – uncommon except North East drtbalu 26

Aetiology 1. Genetic HLA histocompatibility loci possible markers 2. Viruses EBV Viral Capsid Antigen & Early Antigen 3. Environmental Nitrosamines - salted fish Others - polycyclic hydrocarbons, air pollution, tobacco smoking, smoke from burning wood drtbalu 27

Age & sex Distribution • The age incidence of NPC is different from other cancers. • It begins to rise at the end of IInd decade reaches a peak at IVth decade then stays at a plateau. • Bimodal age distribution. • Male : Female drtbalu – 3: 1 28

Classification • WHO classes übased on light microscopy findings • 3 histological types ütype I – Keratinizing SCC (25%) ütype II – Nonkeratinizing Differentiated Carcinoma (12%) ütype III – Nonkeratinizing Undifferentiated Carcinoma ( 63%) 29

Pathology • Grossly the tumour presents in 3 forms üProliferative growth causing nasal obstruction üUlcerative causing epistaxis üInfiltrative which causes cranial nerve involvement 30

pathology • Squamous cell CA – 85% • Lymphomas – 10% • Rhabdomyosarcoma, malignant mixed salivary gland tumor – 5%
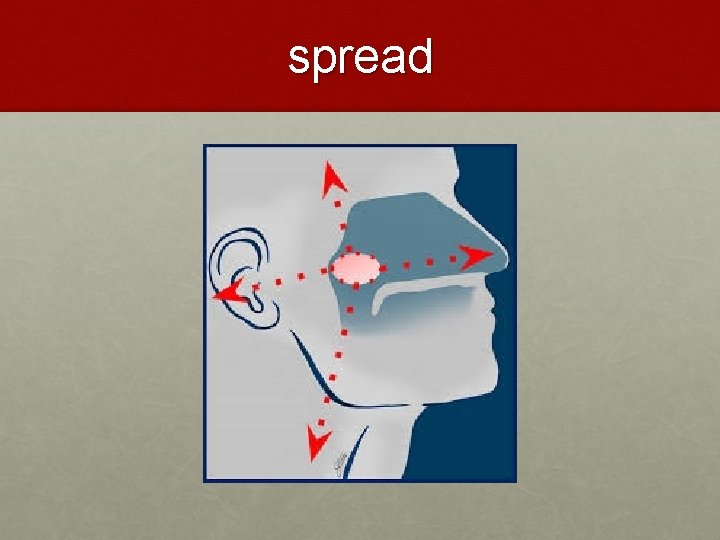
spread
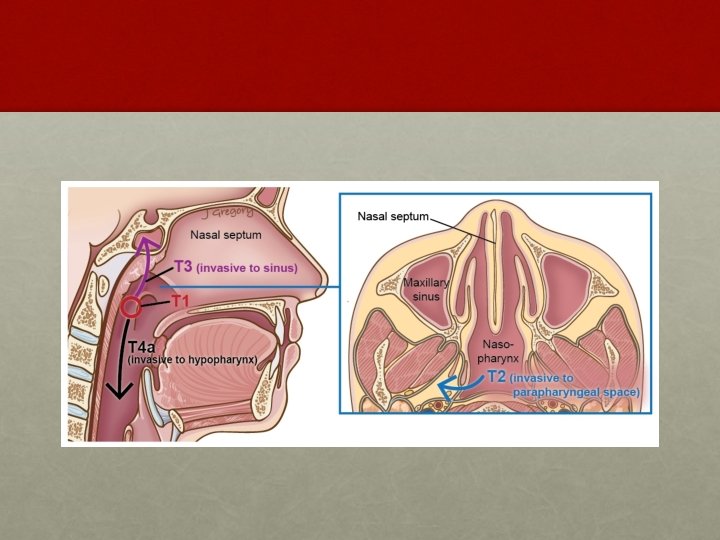
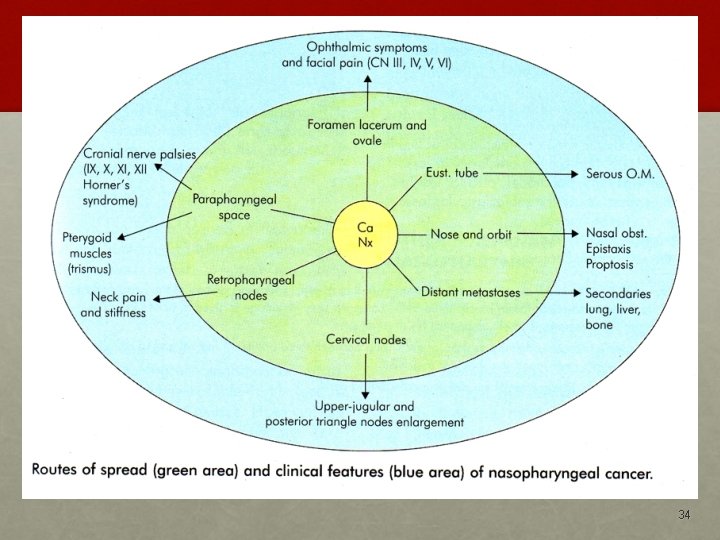
34
Cervical Lymphadenopathy (60%) • tendency for early lymphatic spread • commonest palpable node – jugulodiagastric • contralateral lymph nodes metastasis (nasopharynx is midline structure) 35
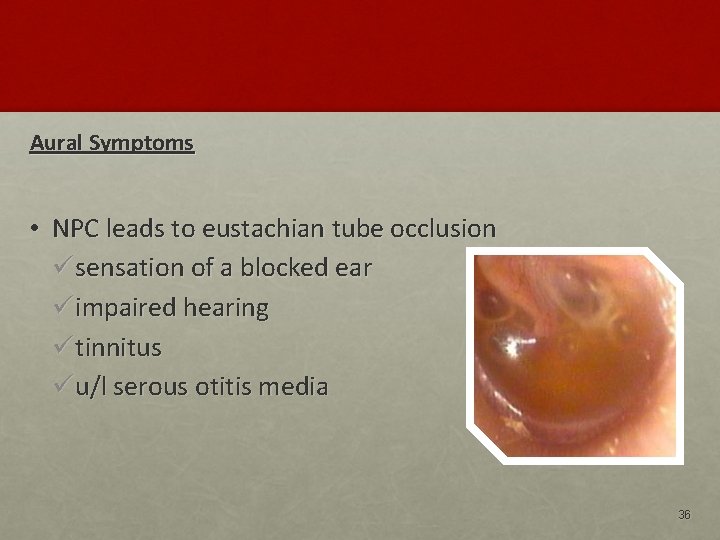
Aural Symptoms • NPC leads to eustachian tube occlusion ü sensation of a blocked ear ü impaired hearing ü tinnitus ü u/l serous otitis media 36
Epistaxis and Nasorespiratory Symptoms • blood stained nasal discharge • profuse epistaxis • nasal obstruction • Hyponasal speech 37

Neurological Palsies • Most frequently involved are: ü VI - Lateral rectus palsy - Diplopia & squint ü III, IV, VI - are commonly affected together (opthalmoplegia) ü V – Facial pain & paraesthesia ü IX, X & XI - Jugular Foramen Syndrome (involvement of the IX, X, and XI CN) • Isolated single C. N. palsy common with nerves V & VI • Horner’s syndrome 38
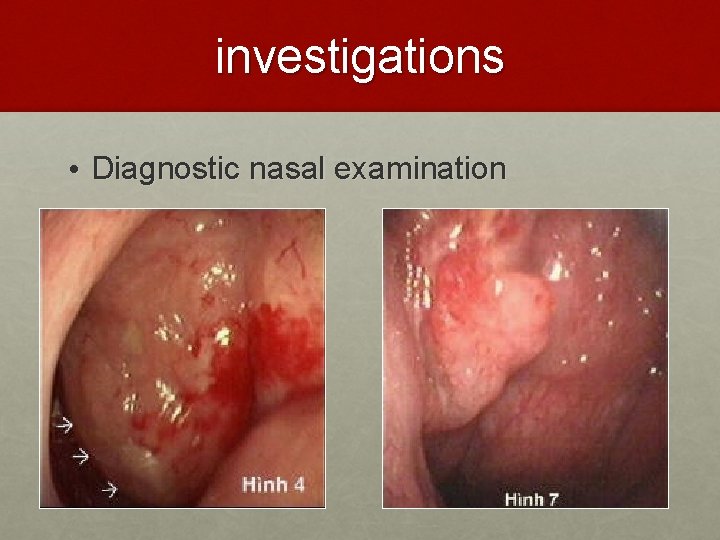
investigations • Diagnostic nasal examination
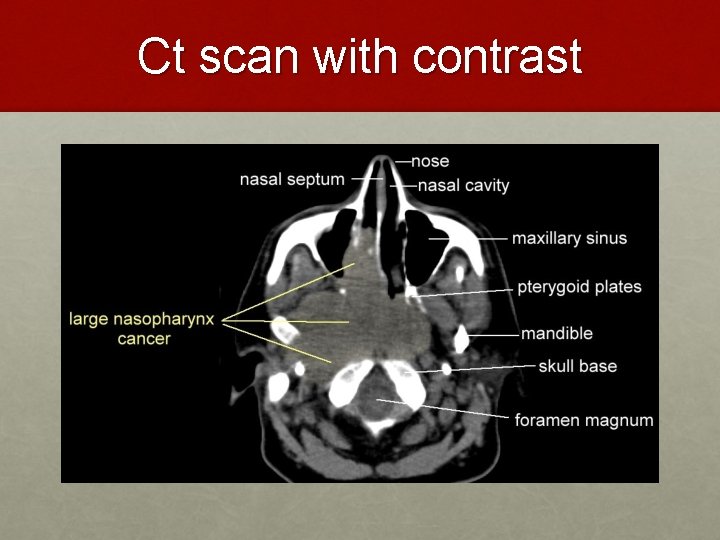
Ct scan with contrast
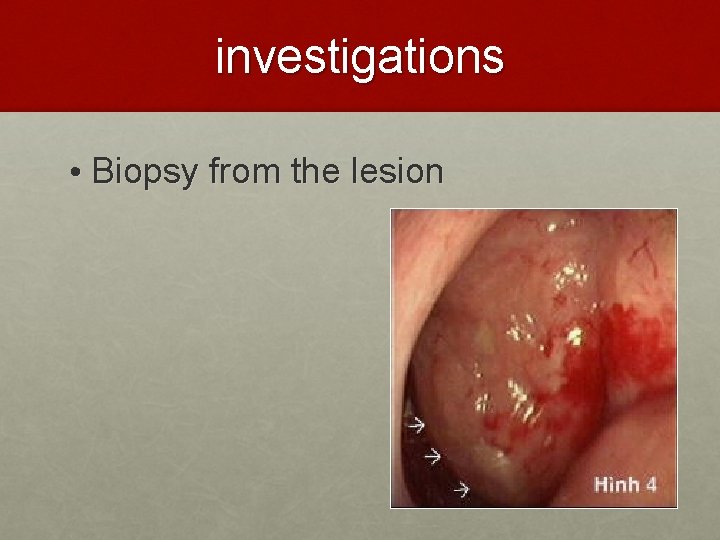
investigations • Biopsy from the lesion

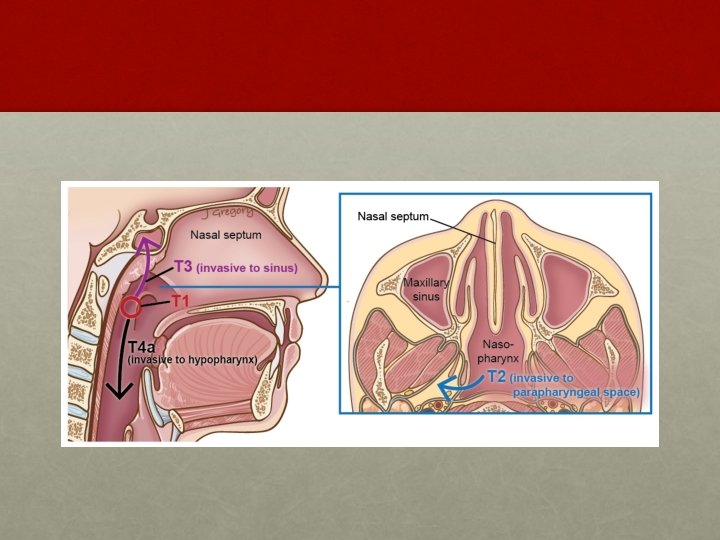
AJCC system: T staging • T 1: • Tumor confined to the nasopharynx • T 2: • Tumor extends to soft tissues • T 2 a : Extends to the oropharynx or the nasal fossa • T 2 b : With parapharyngeal extension • T 3: • Tumor invades bony structures and/or paranasal sinuses • T 4: • Tumor with intracranial extension and/or involvement of cranial nerves, infratemporal fossa, hypopharynx, orbit, or masticator space Department of Radiotherapy, PGIMER, Chandigarh

• N 0: AJCC system: N staging • No regional lymph node metastasis • N 1: • Unilateral metastasis in lymph node(s), < 6 cm in greatest dimension, above the supraclavicular fossa • N 2: • Bilateral metastasis in lymph node(s), < 6 cm in greatest dimension, above the supraclavicular fossa • N 3: • • N 3 a: Metastasis in a lymph node(s) >6 cm N 3 b: Extension to the supraclavicular fossa PGIMER, Chandigarh Ho’s Triangle

treatment • External Beam Radiotherapy üprimary mode of management of NPC – 6000 - 7000 c. Gy üat the primary site and in the neck ümainly because of tumor's high degree of sensitivity to radiation as well as the anatomical constraints for surgical access

Treatment • Chemotherapy ücan be delivered before (neoadjuvant), during (concurrent), or following (adjuvant) radiation therapy üactive chemotherapeutic - cisplatin, 5 fluorouracil (5 -FU) 46

treatment • Surgery: • Residual / recurrent primary tumour • Radical neck dissection for persistent disease

Other malignant tumors • Lymphomas • Rhabdomyosarcoma • Plasmacytoma • Chordoma • Adenoid cystic carcinoma • Melanoma

Thank you
- Slides: 49