TUBULOINTERSTITIAL DISEASES Terminology u Tubulointerstitial nephritis Primary Inflammation

TUBULOINTERSTITIAL DISEASES Terminology u Tubulointerstitial nephritis: • Primary - Inflammation limited to tubules & with uninvolved • • or minimally involved glomeruli/vessels. – Acute - Sudden onset & rapid decline in renal function associated with interstitial edema – Chronic - Protracted onset and slow decline in renal function associated with interstitial fibrosis Secondary - Tubulointerstitial inflammation associated with primary glomerular/vascular diseases Infectious – Tubulointerstitial inflammation associated with presence of live microorganism Idiopathic – Tubulointerstitial nephritis where etiological agents or causes are not known Reactive – Tubulointerstitial inflammation from the effects of systemic inflammation. Kidney is sterile.

TUBULOINTERSTITIAL DISEASE Terminology ( cont. ) u Urinary tract infection • colonization of excretory system by live microorganism • Pyelonephritis: tubulointerstitial nephritis with pelvis and calyceal involvement – Acute - usually suppurative inflammation involving pelvi-calyceal system and parenchyma – Chronic - involvement of pelvi-calyceal system and parenchyma with prominent scarring

Tubulointerstitial nephritis Causes u Infections: (1) Reactive (2) Infectious u Drug reaction u Obstruction: (1) with infection: pyelonephritis / pyonephrosis (2) without infection : hydronephrosis u Non-obstructive : vesicoureteral reflux u Immune mediated : (1) with anti TBM antibodies, can be 10 or 20 (2) with IC deposition which can be 10 or 20

Tubulointerstitial nephritis Pathogenetic mechanisms u Antibody mediated • Anti-TBM-antibody disease • Immune-complex disease u T-cell mediated u Associated with infections • Reactive • Infectious

Tubuluinterstitial nephritis u Primary anti-TBM-antibody nephritis • Ig. G antibodies directed against tubular basement membrane • Linear staining on immunofluorescence microscopy • Edema and mononuclear cells in interstitium • Glomeruli and blood vessels are unremarkable u Secondary anti-TBM-antibody disease • 20 to 10 glomerulonephritidies, allograft nephropathy

Tubulointerstitial nephritis with immune complexes u Primary immune complex disease • granular staining on IF microscopy on tubular basement membrane • Primary – Rare • Secondary – Usually associated with primary glomerulonephritidies involving TBM and interstitium – e. g SLE, MPGN, Membranous GN etc.

Cell-mediated mechanism u Delayed-type hypersensitivity reaction • Activated CD 4+ T and monocyte / macrophage cells releases cytokines which modulates inflammatory reactions and fibrogenesis • Cytotoxic T-cell injury in which CD 4+ T and CD 8+ T play important role

Pathology of primary IN u bilaterally symmetrical enlargement of kidney u edema u inflammatory cells in interstitium u tubular change including tubulitis, breaks in TBM, necrosis of tubular epithelial cells etc.

Pathology of renal failure acute chronic

Acute renal failure (ARF) u Rapid deterioration of renal function in a relatively short period of time u Sudden inability to maintain normal fluid and electrolyte homeostasis u Marked decrease in renal output u May be of glomerular, tubular, interstitial or vascular origin

Causes of ARF u acute tubular necrosis u infarction & cortical necrosis u organic diseases of renal vessels u severe forms of glomerulonephritis u severe infection u acute tubulointerstitial nephritis u outflow obstruction (post-renal) u impairment of blood flow (pre-renal)

Acute tubular necrosis (ATN) ucommonest cause of acute renal failure udevelops due to : • direct poisoning of tubules (nephrotoxic lesions) • renal ischemia (tubulorrhexic lesions)

Acute tubular necrosis Etiology & Pathogenesis u Ischemic in origin (Tubulorrhexic lesion) Prolonged ischemia due to: Shock: postoperative, intra-operative, post-traumatic, septic, hypotensive Hemorrhage: postpartum hemorrhage, abruptio placentae Other: severe burns, transfusion accidents, dehydration, heat stroke, crushing injuries, non-traumatic rhabdomyolysis, paroxysmal hemoglobinuria etc.

Acute tubular necrosis Etiology and Pathogenesis u Direct effects of toxins (Nephrotoxic lesion) Therapeutic agents : • Antibiotics : Aminoglycosides, NSAIDs, chemotherapeutic agents, etc. • Heavy metals: mercury, lead, gold etc. • Radiocontrast agents • Multiple bee stings, scorpion bites etc.

Gross pathology u bilaterally enlarged & swollen kidney due to edema u Cut surface bulges and has a flabby consistency u widened & pale cortex u dark & congested medulla
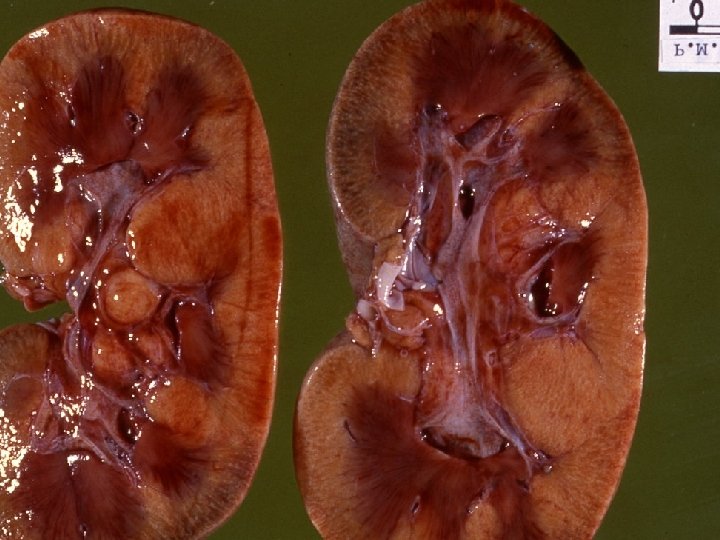
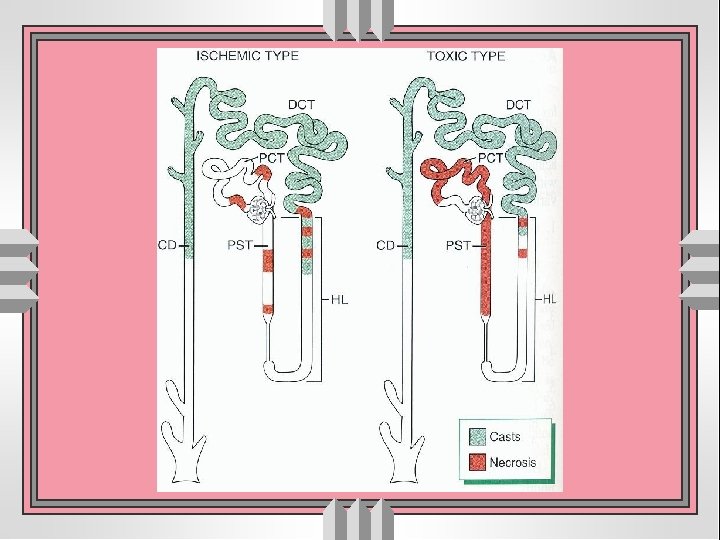

Light microscopy u dilated lumen with flattened epithelial cells u Greatest change in proximal tubules, varies in two forms u loss of brush borders- proximal tubules u evidence of regeneration of epithelial cells u hyaline, granular and pigmented casts u interstitial edema & inflammation u Intra-vascular collection of nucleated red blood cells


ATN- Prognosis u depends upon underlying cause, over all mortality rate 50% u post-traumatic (62%), post-operative (56%), medical (46 %), obstetric (17 %) u Higher in older debilitated pts. & in pts. with multiple organ disease u good for uncomplicated and younger patients

Chronic renal failure u Occurs in all cases of end-stage renal disease of whatever etiology u GFR falls below 20% of normal u End result of all chronic renal disease which can be glomerular, tubulointerstitial or vascular in origin u Characterized by prolonged signs and symptoms of uremia u Is a major cause of death in renal disease

Chronic renal failure u Systemic • • • (visceral) manifestations Enlarged heart & pericarditis Uremic pneumonitis & pleuritis Uremic colitis Uremic encephalopathy Hypoplastic anemia

TUBULO-INTERSTITIAL DISEASE u Urinary tract infection • colonization of excretory system by live microorganism • Most caused by gram negative enteric organism • Most common form of renal involvement is: – Pyelonephritis: bacterial infection of the kidney that affects parenchyma, calyces and pelvis • Acute - usually suppurative inflammation involving – pelvi-calyceal system and parenchyma • Chronic - involvement pelvi-calyceal system and parenchyma with prominent scarring

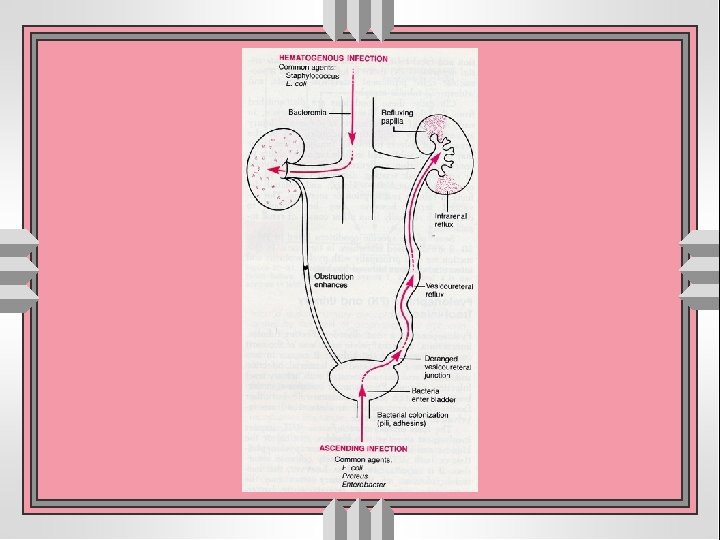
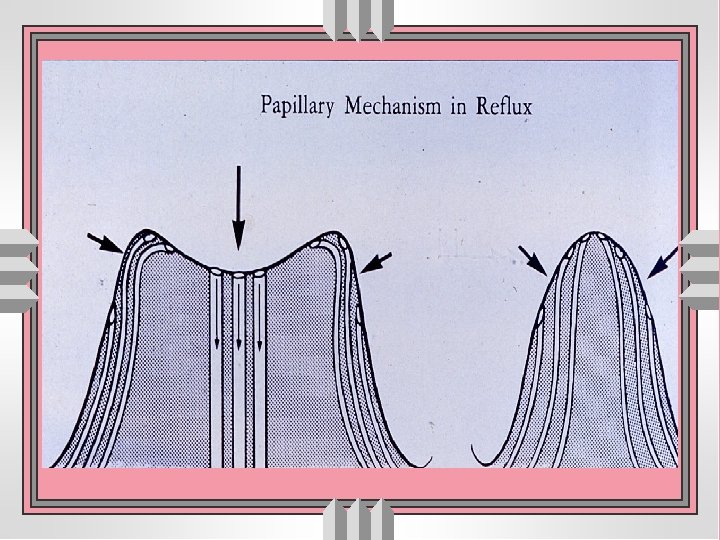
Pyelonephritis • Acute: usually suppurative, often associated (1) with / without obstruction (2) ascending infection through vesicoureteral reflux (3) from hematogenous dissemination. • Chronic: inflammation with prominent scarring; may be (1) obstructive with recurrent infection (2) non-obstructive with vesicoureteral reflux → reflux nephropathy

Acute Pyelonephritis Predisposing factors u Urinary obstruction: congenital or acquired u Instrumentation of urinary tract u Vesicoureteral reflux u Pregnancy: 4 -6% develops bacteriuria u Gender and age u Preexisting renal lesions u Diabetes mellitus, immunosuppression & immunodeficiency

Acute pyelonephritis u route of invasion : • via blood stream • ascending route u obstructive u non-obstructive role of vesicoureteral reflux and infected urine
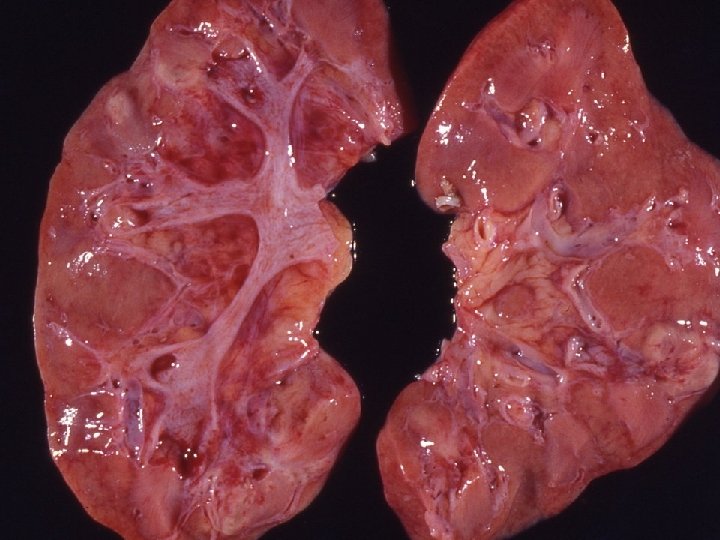
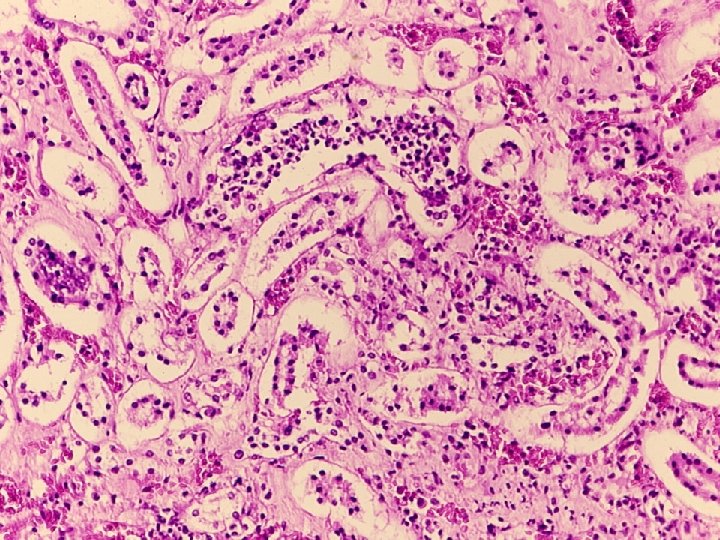



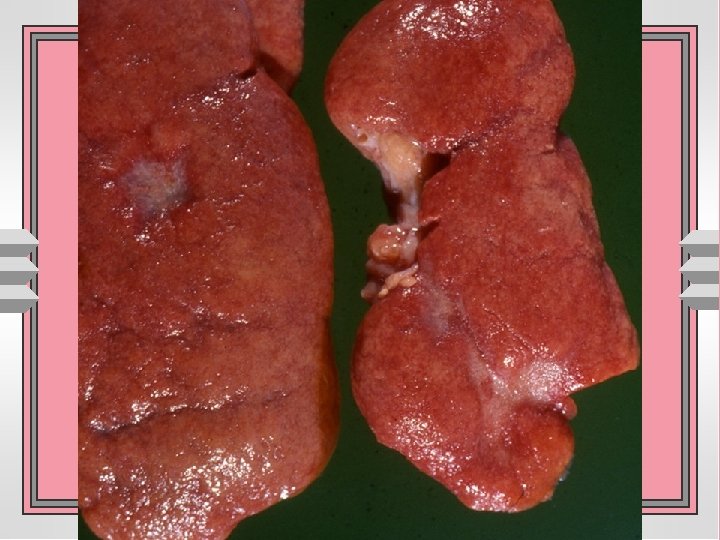
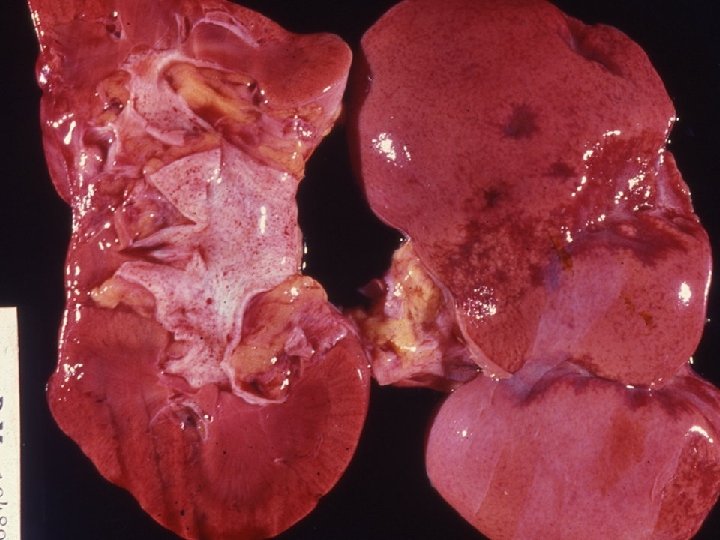
Chronic pyelonephritis u. It is a chronic tubulointerstitial inflammation involving renal parenchyma, pelvis and calyces associated with scarring unon-obstructive • reflux nephropathy uobstructive
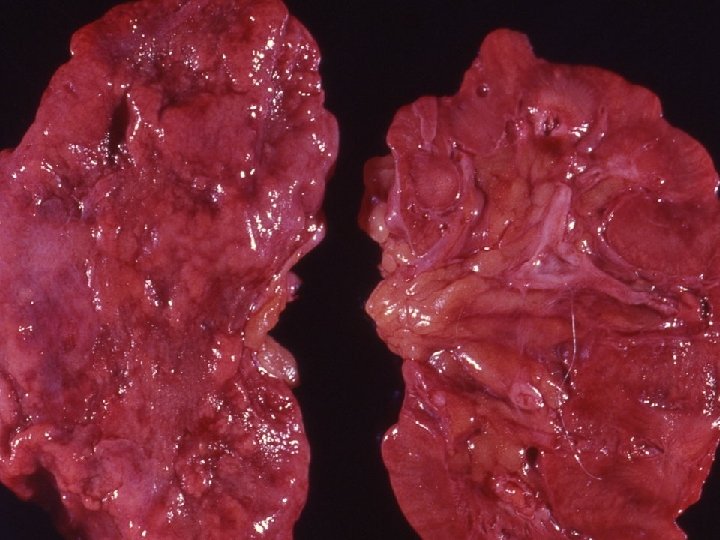

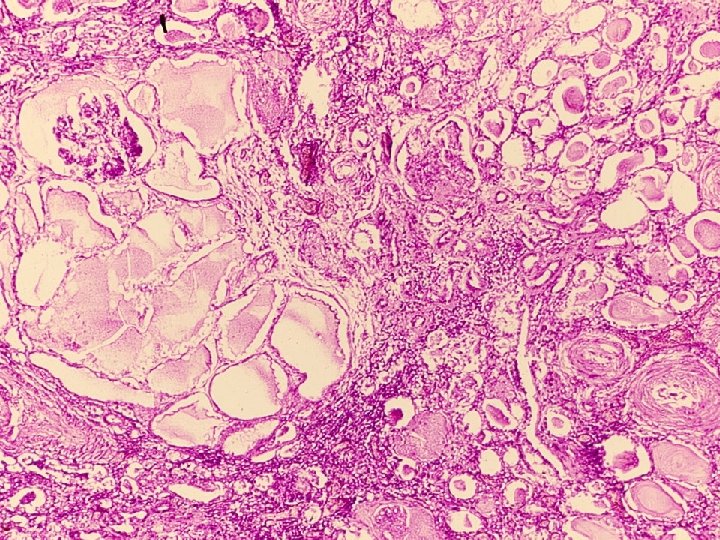
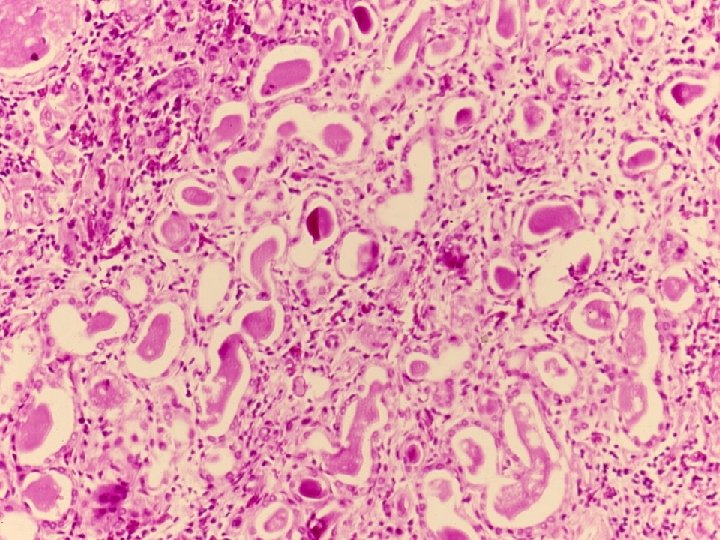

- Slides: 40