Tubular Reabsorption A selective transepithelial process All organic

Tubular Reabsorption • A selective transepithelial process • All organic nutrients are reabsorbed • Water and ion reabsorption are hormonally regulated • Includes active and passive process • Two routes • Transcellular • Paracellular
Tubular Reabsorption • Transcellular route • Luminal membranes of tubule cells • Cytosol of tubule cells • Basolateral membranes of tubule cells • Endothelium of peritubular capillaries

Tubular Reabsorption • Paracellular route • Between cells • Limited to water movement and reabsorption of Ca 2+, Mg 2+, K+, and some Na+ in the PCT where tight junctions are leaky
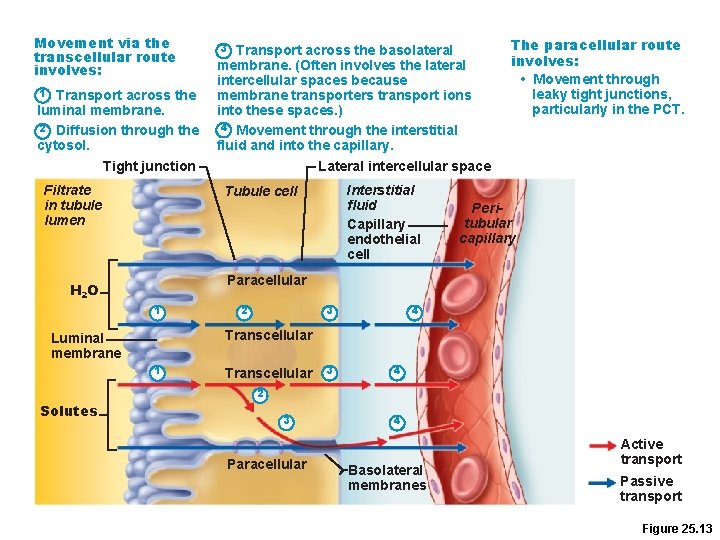
Movement via the transcellular route involves: 1 Transport across the luminal membrane. 2 Diffusion through the cytosol. 3 Transport across the basolateral membrane. (Often involves the lateral intercellular spaces because membrane transporters transport ions into these spaces. ) 4 Movement through the interstitial fluid and into the capillary. Lateral intercellular space Tight junction Filtrate in tubule lumen The paracellular route involves: • Movement through leaky tight junctions, particularly in the PCT. Interstitial fluid Capillary endothelial cell Tubule cell Peritubular capillary Paracellular H 2 O 1 2 3 4 Transcellular Luminal membrane 1 Transcellular 3 4 2 Solutes 3 Paracellular 4 Basolateral membranes Active transport Passive transport Figure 25. 13

Sodium Reabsorption • Na+ (most abundant cation in filtrate) • Primary active transport out of the tubule cell by Na+-K+ ATPase in the basolateral membrane • Na+ passes in through the luminal membrane by secondary active transport or facilitated diffusion mechanisms

Sodium Reabsorption • Low hydrostatic pressure and high osmotic pressure in the peritubular capillaries • Promotes bulk flow of water and solutes (including Na+)

Reabsorption of Nutrients, Water, and Ions • Na+ reabsorption provides the energy and the means for reabsorbing most other substances • Organic nutrients are reabsorbed by secondary active transport • Transport maximum (Tm) reflects the number of carriers in the renal tubules available • When the carriers are saturated, excess of that substance is excreted

Reabsorption of Nutrients, Water, and Ions • Water is reabsorbed by osmosis (obligatory water reabsorption), aided by water-filled pores called aquaporins • Cations and fat-soluble substances follow by diffusion

1 At the basolateral membrane, Nucleus Filtrate in tubule lumen Na+ Tubule cell 3 Na+ 1 2 K+ 3 K+ 4 Lipid-soluble 5 substances Cl–, Ca 2+, K+ and other ions, urea Peritubular capillary 3 Reabsorption of organic 2 3 Na+ Glucose Amino acids Some ions Vitamins H 2 O Interstitial fluid Na+ is pumped into the interstitial space by the Na+-K+ ATPase. Active Na+ transport creates concentration gradients that drive: 2 “Downhill” Na + entry at the luminal membrane. 6 Tight junction Primary active transport Secondary active transport Passive transport (diffusion) Cl– Paracellular route Transport protein Ion channel or aquaporin nutrients and certain ions by cotransport at the luminal membrane. 4 Reabsorption of water by osmosis. Water reabsorption increases the concentration of the solutes that are left behind. These solutes can then be reabsorbed as they move down their concentration gradients: 5 Lipid-soluble substances diffuse by the transcellular route. 6 Cl– (and other anions), K+, and urea diffuse by the paracellular route. Figure 25. 14

Reabsorptive Capabilities of Renal Tubules and Collecting Ducts • PCT • Site of most reabsorption • 65% of Na+ and water • All nutrients • Ions • Small proteins

Reabsorptive Capabilities of Renal Tubules and Collecting Ducts • Loop of Henle • Descending limb: H 2 O • Ascending limb: Na+, K+, Cl

Reabsorptive Capabilities of Renal Tubules and Collecting Ducts • DCT and collecting duct • Reabsorption is hormonally regulated • Ca 2+ (PTH) • Water (ADH) • Na+ (aldosterone and ANP)

Reabsorptive Capabilities of Renal Tubules and Collecting Ducts • Mechanism of aldosterone • Targets collecting ducts (principal cells) and distal DCT • Promotes synthesis of luminal Na+ and K+ channels • Promotes synthesis of basolateral Na+-K+ ATPases

Tubular Secretion • Reabsorption in reverse • K+, H+, NH 4+, creatinine, and organic acids move from peritubular capillaries or tubule cells into filtrate • Disposes of substances that are bound to plasma proteins

Tubular Secretion • Eliminates undesirable substances that have been passively reabsorbed (e. g. , urea and uric acid) • Rids the body of excess K+ • Controls blood p. H by altering amounts of H+ or HCO 3– in urine

Regulation of Urine Concentration and Volume • Osmolality • Number of solute particles in 1 kg of H 2 O • Reflects ability to cause osmosis

Regulation of Urine Concentration and Volume • Osmolality of body fluids • Expressed in milliosmols (m. Osm) • The kidneys maintain osmolality of plasma at ~300 m. Osm, using countercurrent mechanisms

Countercurrent Mechanism • Occurs when fluid flows in opposite directions in two adjacent segments of the same tube • Filtrate flow in the loop of Henle (countercurrent multiplier) • Blood flow in the vasa recta (countercurrent exchanger)

Countercurrent Mechanism • Role of countercurrent mechanisms • Establish and maintain an osmotic gradient (300 m. Osm to 1200 m. Osm) from renal cortex through the medulla • Allow the kidneys to vary urine concentration
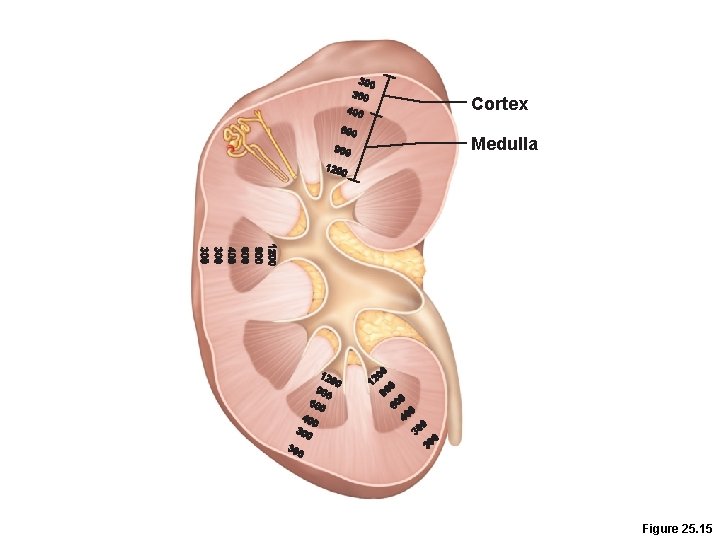
Cortex Medulla Figure 25. 15

Countercurrent Multiplier: Loop of Henle • Descending limb • Freely permeable to H 2 O, which passes out of the filtrate into the hyperosmotic medullary interstitial fluid • Filtrate osmolality increases to ~1200 m. Osm

Countercurrent Multiplier: Loop of Henle • Ascending limb • Impermeable to H 2 O • Selectively permeable to solutes • Na+ and Cl– are passively reabsorbed in the thin segment, actively reabsorbed in the thick segment • Filtrate osmolality decreases to 100 m. Osm
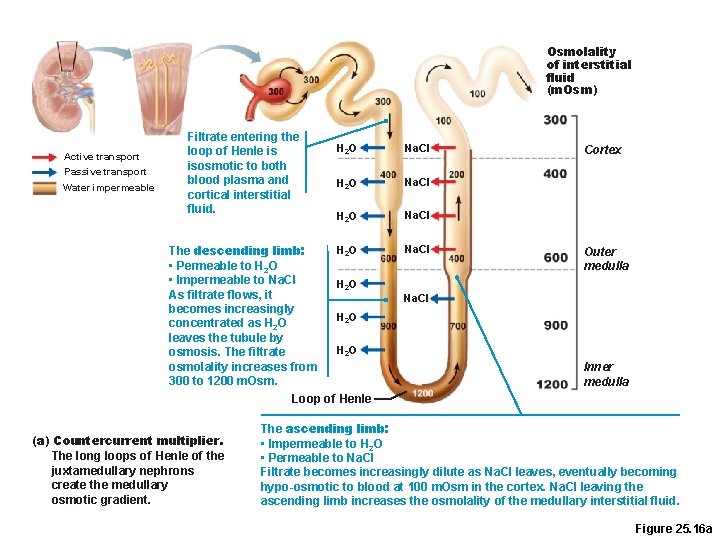
Osmolality of interstitial fluid (m. Osm) Active transport Passive transport Water impermeable Filtrate entering the loop of Henle is isosmotic to both blood plasma and cortical interstitial fluid. H 2 O Na. CI H 2 O The descending limb: • Permeable to H 2 O • Impermeable to Na. Cl H 2 O As filtrate flows, it becomes increasingly H 2 O concentrated as H 2 O leaves the tubule by H 2 O osmosis. The filtrate osmolality increases from 300 to 1200 m. Osm. Loop of Henle (a) Countercurrent multiplier. The long loops of Henle of the juxtamedullary nephrons create the medullary osmotic gradient. Na. CI Cortex Outer medulla Na. CI Inner medulla The ascending limb: • Impermeable to H 2 O • Permeable to Na. Cl Filtrate becomes increasingly dilute as Na. Cl leaves, eventually becoming hypo-osmotic to blood at 100 m. Osm in the cortex. Na. Cl leaving the ascending limb increases the osmolality of the medullary interstitial fluid. Figure 25. 16 a

Urea Recycling • Urea moves between the collecting ducts and the loop of Henle • Secreted into filtrate by facilitated diffusion in the ascending thin segment • Reabsorbed by facilitated diffusion in the collecting ducts deep in the medulla • Contributes to the high osmolality in the medulla

Countercurrent Exchanger: Vasa Recta • The vasa recta • Maintain the osmotic gradient • Deliver blood to the medullary tissues • Protect the medullary osmotic gradient by preventing rapid removal of salt, and by removing reabsorbed H 2 O
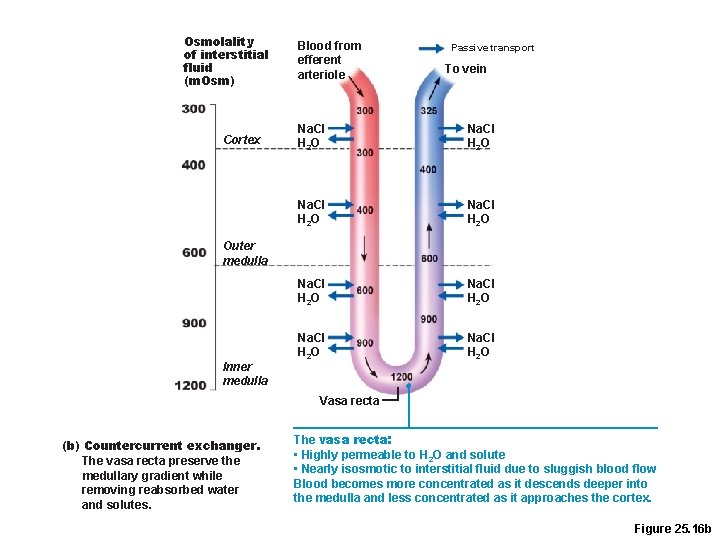
Osmolality of interstitial fluid (m. Osm) Cortex Blood from efferent arteriole Passive transport To vein Na. CI H 2 O Na. CI H 2 O Outer medulla Inner medulla Vasa recta (b) Countercurrent exchanger. The vasa recta preserve the medullary gradient while removing reabsorbed water and solutes. The vasa recta: • Highly permeable to H 2 O and solute • Nearly isosmotic to interstitial fluid due to sluggish blood flow Blood becomes more concentrated as it descends deeper into the medulla and less concentrated as it approaches the cortex. Figure 25. 16 b

Formation of Dilute Urine • Filtrate is diluted in the ascending loop of Henle • In the absence of ADH, dilute filtrate continues into the renal pelvis as dilute urine • Na+ and other ions may be selectively removed in the DCT and collecting duct, decreasing osmolality to as low as 50 m. Osm
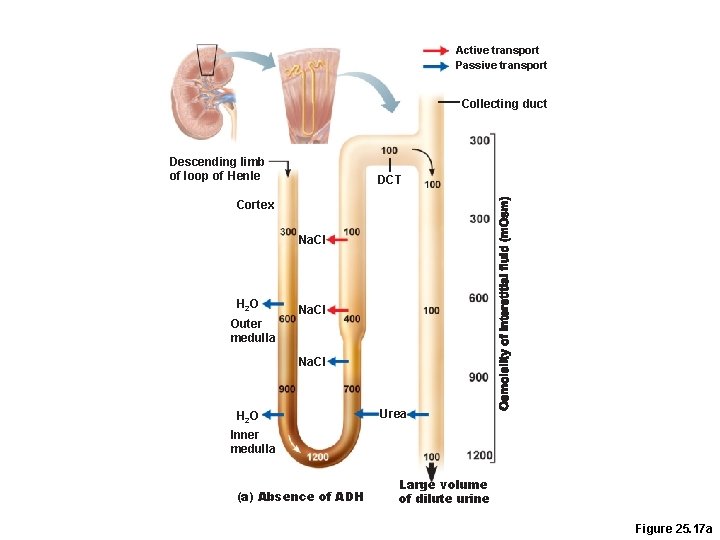
Active transport Passive transport Collecting duct Descending limb of loop of Henle DCT Cortex Na. CI H 2 O Outer medulla Na. CI H 2 O Urea Inner medulla (a) Absence of ADH Large volume of dilute urine Figure 25. 17 a

Formation of Concentrated Urine • Depends on the medullary osmotic gradient and ADH • ADH triggers reabsorption of H 2 O in the collecting ducts • Facultative water reabsorption occurs in the presence of ADH so that 99% of H 2 O in filtrate is reabsorbed
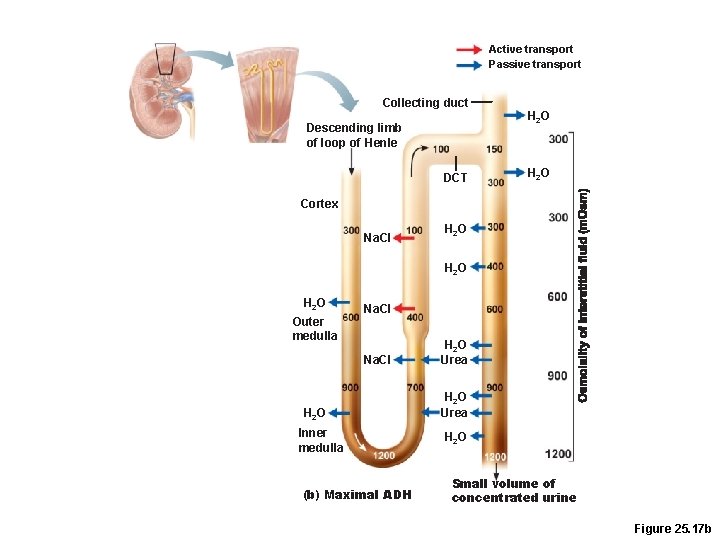
Active transport Passive transport Collecting duct Descending limb of loop of Henle DCT H 2 O Cortex Na. CI H 2 O Outer medulla Na. CI H 2 O Inner medulla (b) Maximal ADH H 2 O Urea H 2 O Small volume of concentrated urine Figure 25. 17 b

Diuretics • Chemicals that enhance the urinary output • Osmotic diuretics: substances not reabsorbed, (e. g. , high glucose in a diabetic patient) • ADH inhibitors such as alcohol • Substances that inhibit Na+ reabsorption and obligatory H 2 O reabsorption such as caffeine and many drugs
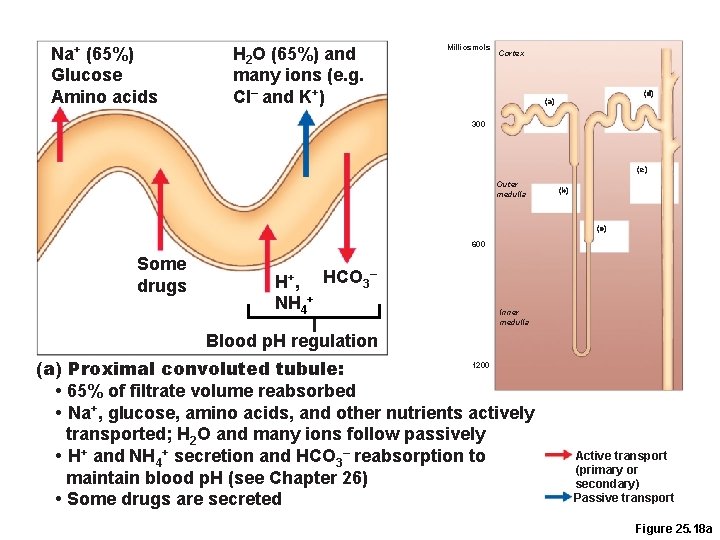
Na+ (65%) Glucose Amino acids H 2 O (65%) and many ions (e. g. Cl– and K+) Milliosmols Cortex (d) (a) 300 (e) Outer medulla (b) (c) 600 Some drugs – H+, HCO 3 NH 4+ Inner medulla Blood p. H regulation 1200 (a) Proximal convoluted tubule: • 65% of filtrate volume reabsorbed • Na+, glucose, amino acids, and other nutrients actively transported; H 2 O and many ions follow passively • H+ and NH 4+ secretion and HCO 3– reabsorption to maintain blood p. H (see Chapter 26) • Some drugs are secreted Active transport (primary or secondary) Passive transport Figure 25. 18 a
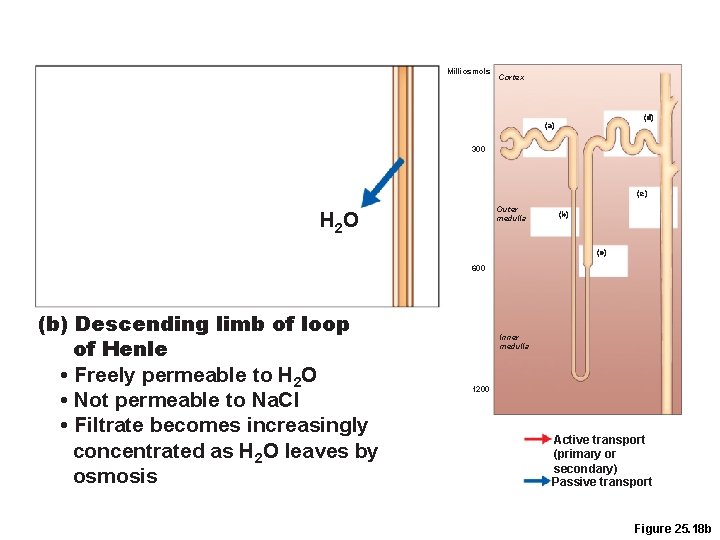
Milliosmols Cortex (d) (a) 300 (e) Outer medulla H 2 O (b) (c) 600 (b) Descending limb of loop of Henle • Freely permeable to H 2 O • Not permeable to Na. Cl • Filtrate becomes increasingly concentrated as H 2 O leaves by osmosis Inner medulla 1200 Active transport (primary or secondary) Passive transport Figure 25. 18 b
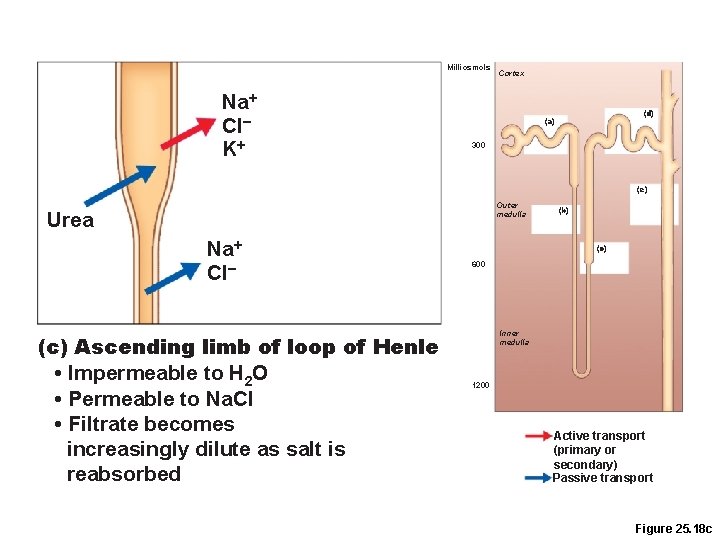
Milliosmols Na+ Cl– K+ Cortex (d) (a) 300 (e) Outer medulla Urea Na+ Cl– (c) Ascending limb of loop of Henle • Impermeable to H 2 O • Permeable to Na. Cl • Filtrate becomes increasingly dilute as salt is reabsorbed (b) (c) 600 Inner medulla 1200 Active transport (primary or secondary) Passive transport Figure 25. 18 c
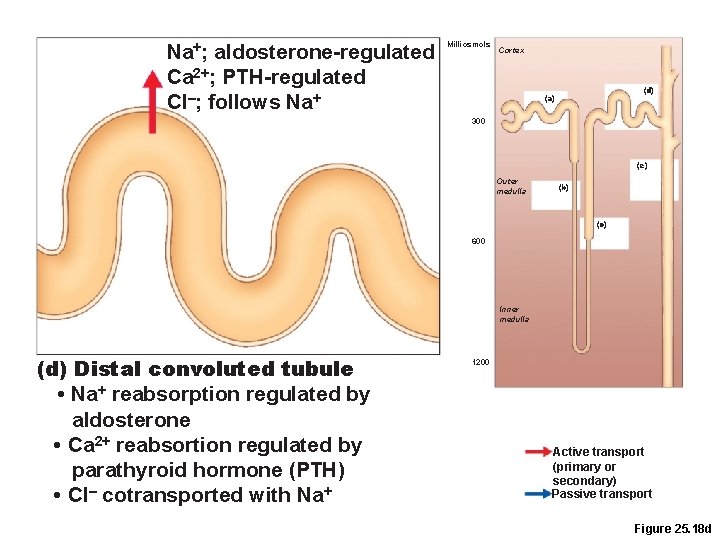
Na+; aldosterone-regulated Ca 2+; PTH-regulated Cl–; follows Na+ Milliosmols Cortex (d) (a) 300 (e) Outer medulla (b) (c) 600 Inner medulla (d) Distal convoluted tubule • Na+ reabsorption regulated by aldosterone • Ca 2+ reabsortion regulated by parathyroid hormone (PTH) • Cl– cotransported with Na+ 1200 Active transport (primary or secondary) Passive transport Figure 25. 18 d
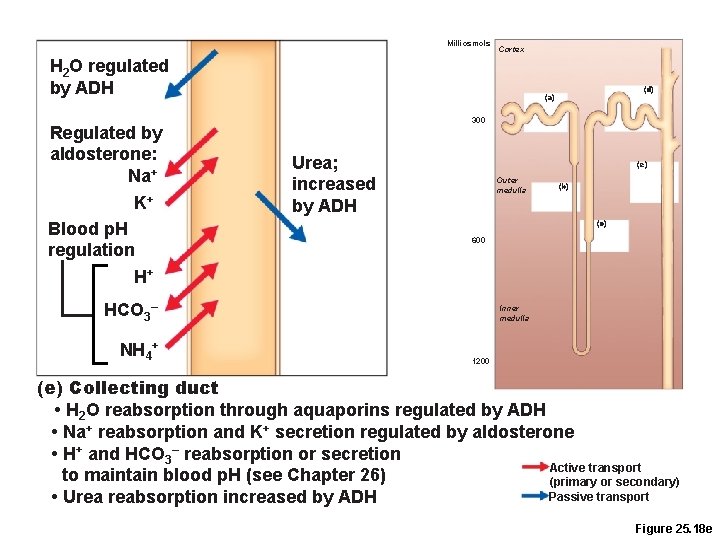
Milliosmols Cortex H 2 O regulated by ADH Regulated by aldosterone: Na+ K+ Blood p. H regulation H+ 300 Urea; increased by ADH (e) Outer medulla (b) (c) 600 HCO 3– NH 4+ (d) (a) Inner medulla 1200 (e) Collecting duct • H 2 O reabsorption through aquaporins regulated by ADH • Na+ reabsorption and K+ secretion regulated by aldosterone • H+ and HCO 3– reabsorption or secretion Active transport to maintain blood p. H (see Chapter 26) (primary or secondary) Passive transport • Urea reabsorption increased by ADH Figure 25. 18 e

Renal Clearance • Volume of plasma cleared of a particular substance in a given time • Renal clearance tests are used to • Determine GFR • Detect glomerular damage • Follow the progress of renal disease

Renal Clearance RC = UV/P RC = renal clearance rate (ml/min) U = concentration (mg/ml) of the substance in urine V = flow rate of urine formation (ml/min) P = concentration of the same substance in plasma

Renal Clearance • For any substance freely filtered and neither reabsorbed nor secreted by the kidneys (e. g. , insulin), RC = GFR = 125 ml/min • If RC < 125 ml/min, the substance is reabsorbed • If RC = 0, the substance is completely reabsorbed • If RC > 125 ml/min, the substance is secreted (most drug metabolites)

Physical Characteristics of Urine • Color and transparency • Clear, pale to deep yellow (due to urochrome) • Drugs, vitamin supplements, and diet can alter the color • Cloudy urine may indicate a urinary tract infection

Physical Characteristics of Urine • Odor • Slightly aromatic when fresh • Develops ammonia odor upon standing • May be altered by some drugs and vegetables

Physical Characteristics of Urine • p. H • Slightly acidic (~p. H 6, with a range of 4. 5 to 8. 0) • Diet, prolonged vomiting, or urinary tract infections may alter p. H • Specific gravity • 1. 001 to 1. 035, dependent on solute concentration

Chemical Composition of Urine • 95% water and 5% solutes • Nitrogenous wastes: urea, uric acid, and creatinine • Other normal solutes • Na+, K+, PO 43–, and SO 42–, • Ca 2+, Mg 2+ and HCO 3– • Abnormally high concentrations of any constituent may indicate pathology
Ureters • Convey urine from kidneys to bladder • Retroperitoneal • Enter the base of the bladder through the posterior wall • As bladder pressure increases, distal ends of the ureters close, preventing backflow of urine

Ureters • Three layers of wall of ureter 1. Lining of transitional epithelium 2. Smooth muscle muscularis • Contracts in response to stretch 3. Outer adventitia of fibrous connective tissue
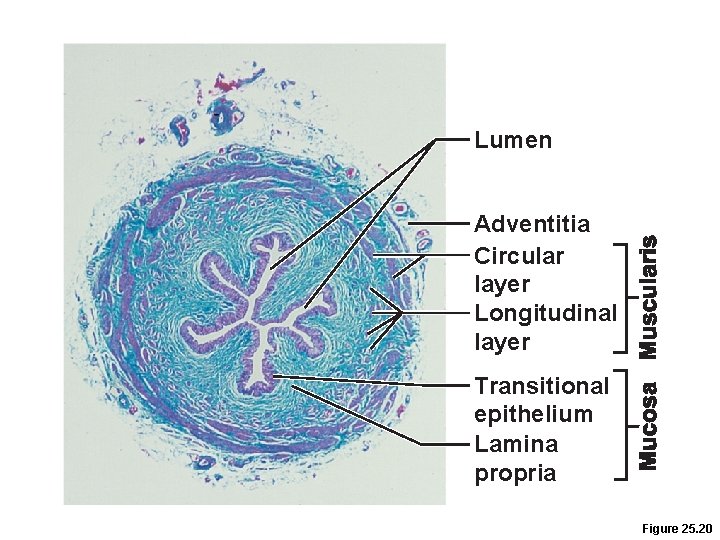
Lumen Adventitia Circular layer Longitudinal layer Transitional epithelium Lamina propria Figure 25. 20

Renal Calculi • Kidney stones form in renal pelvis • Crystallized calcium, magnesium, or uric acid salts • Larger stones block ureter, cause pressure and pain in kidneys • May be due to chronic bacterial infection, urine retention, Ca 2+ in blood, p. H of urine

Urinary Bladder • Muscular sac for temporary storage of urine • Retroperitoneal, on pelvic floor posterior to pubic symphysis • Males—prostate gland surrounds the neck inferiorly • Females—anterior to the vagina and uterus

Urinary Bladder • Trigone • Smooth triangular area outlined by the openings for the ureters and the urethra • Infections tend to persist in this region

Urinary Bladder • Layers of the bladder wall 1. Transitional epithelial mucosa 2. Thick detrusor muscle (three layers of smooth muscle) 3. Fibrous adventitia (peritoneum on superior surface only)

Urinary Bladder • Collapses when empty; rugae appear • Expands and rises superiorly during filling without significant rise in internal pressure
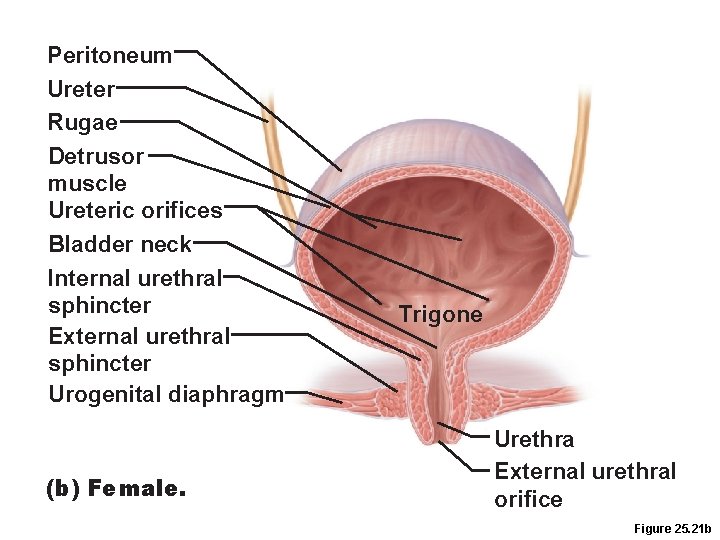
Peritoneum Ureter Rugae Detrusor muscle Ureteric orifices Bladder neck Internal urethral sphincter External urethral sphincter Urogenital diaphragm (b) Female. Trigone Urethra External urethral orifice Figure 25. 21 b

Urethra • Muscular tube • Lining epithelium • Mostly pseudostratified columnar epithelium, except • Transitional epithelium near bladder • Stratified squamous epithelium near external urethral orifice

Urethra • Sphincters • Internal urethral sphincter • Involuntary (smooth muscle) at bladderurethra junction • Contracts to open • External urethral sphincter • Voluntary (skeletal) muscle surrounding the urethra as it passes through the pelvic floor

Urethra • Female urethra (3– 4 cm): • Tightly bound to the anterior vaginal wall • External urethral orifice is anterior to the vaginal opening, posterior to the clitoris
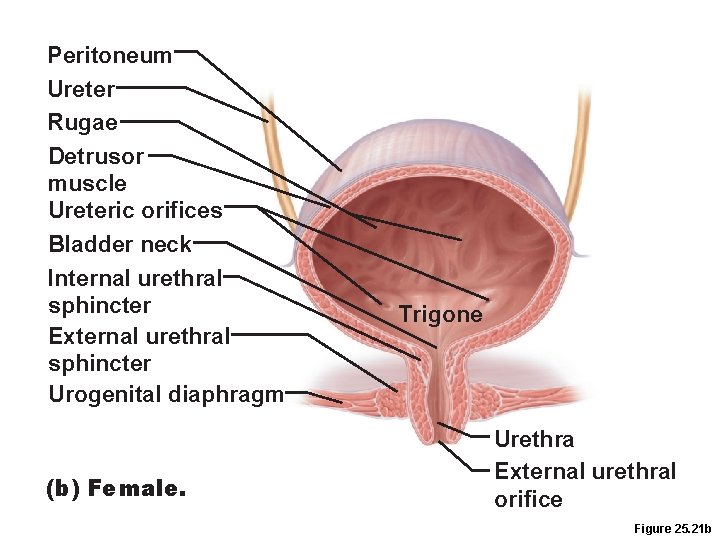
Peritoneum Ureter Rugae Detrusor muscle Ureteric orifices Bladder neck Internal urethral sphincter External urethral sphincter Urogenital diaphragm (b) Female. Trigone Urethra External urethral orifice Figure 25. 21 b
Urethra • Male urethra • Carries semen and urine • Three named regions 1. Prostatic urethra (2. 5 cm)—within prostate gland 2. Membranous urethra (2 cm)—passes through the urogenital diaphragm 3. Spongy urethra (15 cm)—passes through the penis and opens via the external urethral orifice
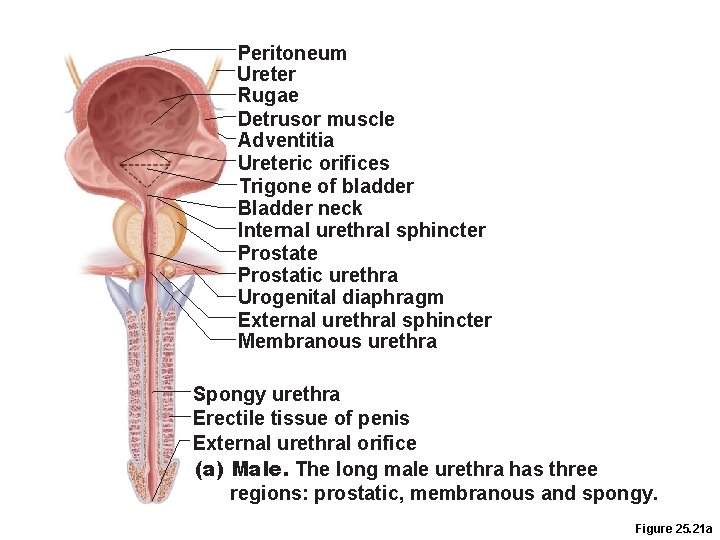
Peritoneum Ureter Rugae Detrusor muscle Adventitia Ureteric orifices Trigone of bladder Bladder neck Internal urethral sphincter Prostate Prostatic urethra Urogenital diaphragm External urethral sphincter Membranous urethra Spongy urethra Erectile tissue of penis External urethral orifice (a) Male. The long male urethra has three regions: prostatic, membranous and spongy. Figure 25. 21 a

Micturition • Urination or voiding • Three simultaneous events 1. Contraction of detrusor muscle by ANS 2. Opening of internal urethral sphincter by ANS 3. Opening of external urethral sphincter by somatic nervous system
Micturition • Reflexive urination (urination in infants) • Distension of bladder activates stretch receptors • Excitation of parasympathetic neurons in reflex center in sacral region of spinal cord • Contraction of the detrusor muscle • Contraction (opening) of internal sphincter • Inhibition of somatic pathways to external sphincter, allowing its relaxation (opening)

Micturition • Pontine control centers mature between ages 2 and 3 1. Pontine storage center inhibits micturition: • Inhibits parasympathetic pathways • Excites sympathetic and somatic efferent pathways 2. Pontine micturition center promotes micturition: • Excites parasympathetic pathways • Inhibits sympathetic and somatic efferent pathways
- Slides: 61