TUBERCULOSIS Prof E Sevda zdoan TUBERCULOSIS Infectious disease

TUBERCULOSIS Prof. E. Sevda Özdoğan

TUBERCULOSIS Infectious disease (airborne infection) Lungs and all the tissues can be involved Mycobacterium tuberculosis (AFB)

Source of infection is the ill (Pulmonary TB) patient: Speaking: 0 -210 bacillei Coughing: 0 -3500 bacillei Sneezing: 4500 -1 million bacillei Droplet nuclei (Flugge droplets)
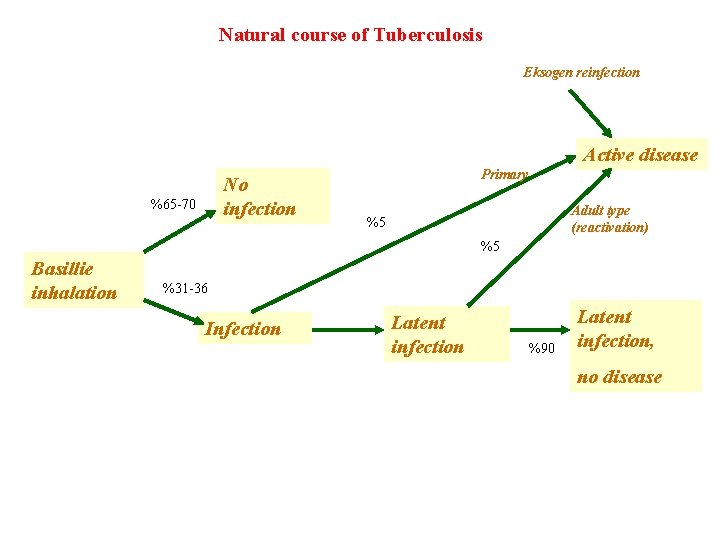
Natural course of Tuberculosis Eksogen reinfection Active disease No infection %65 -70 Primary Adult type (reactivation) %5 %5 Basillie inhalation %31 -36 Infection Latent infection %90 Latent infection, no disease
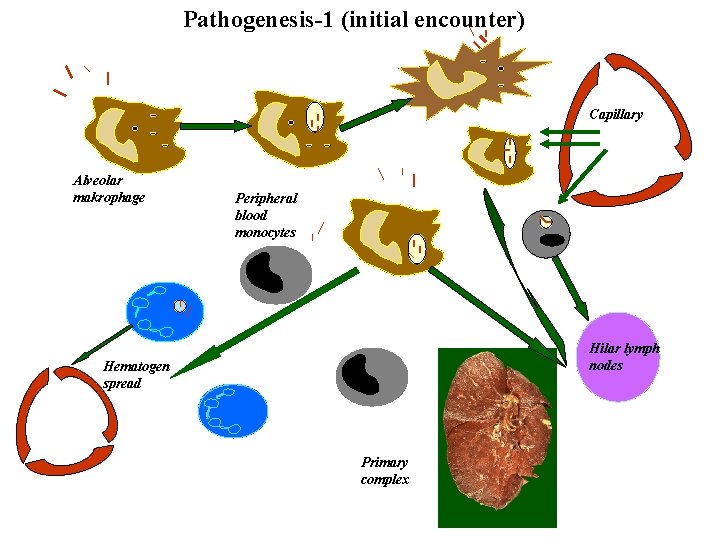
Pathogenesis-1 (initial encounter) Capillary Alveolar makrophage Peripheral blood monocytes Hilar lymph nodes Hematogen spread Primary complex
Evolution of Cellular immunity and Delayed type HS Option 1 (Primary infection) Bacterial proliferation is halted and bacillary population falls substantially The primary lesion and the metastatic foci involute, leaving minimal residues The tuberculin skin test becomes reactive (2 -12 wk) Option 2 (Primary disease) An insufficient immune response occurs and the patient experience progressive lung or extrapulmonary disease

Liquefaction and accelerated bacillary proliferation (Postprimary disease) Pulmonary focus reactivates and undergoes liquefaction with cavity formation Extracellular bacilli multiply exponentially during this accelerated bacillary proliferation Patient expectorates bacillei, another person inhales them, cycle is completed
Immunologic reactions Cell mediated immunity Delayed type hypersensitivity (Type IV immune response) 2 -12 weeks Tuberculin skin test (+)

Tb Infection: Infection with M. tuberculosis manifested by significant tuberculin skin test reaction without any sign of clinically and/or radiologically active disease Tb disease: Clinically, bacteriologically, histologically and/or radiologically active disease
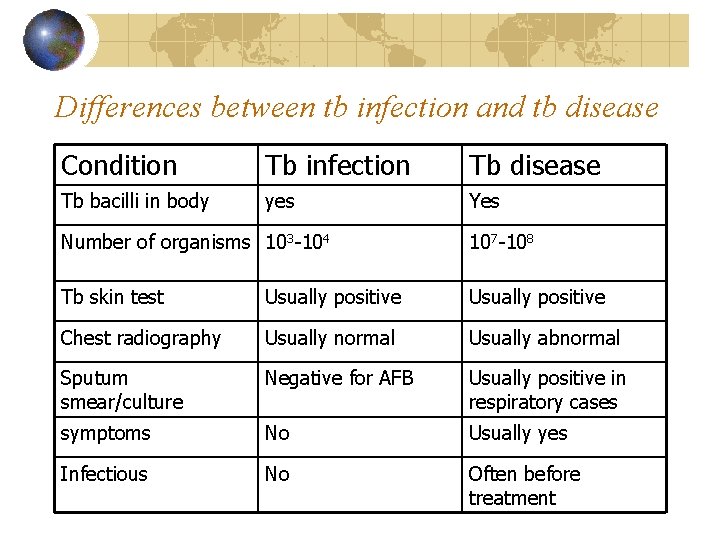
Differences between tb infection and tb disease Condition Tb infection Tb disease Tb bacilli in body yes Yes Number of organisms 103 -104 107 -108 Tb skin test Usually positive Chest radiography Usually normal Usually abnormal Sputum smear/culture Negative for AFB Usually positive in respiratory cases symptoms No Usually yes Infectious No Often before treatment

Risk Factors for Infection Infectious person Number of the bacilli in sputum (Cavitary, larhynx) Cough frequency, sneeze Live bacilli Virulence of the bacilli Environmental Close contact (family) Ventilation Ultraviolet Crowded and bad living conditions

Host factors Nonspecific immunity (Ch 1 BCGr-BCGs region) Concomitant diseases (that increase the risk of infection) Duration of exposure to the source of infection EPİDEMİOLOGİCAL VIEW: Number of infectious patients in the community Delay in diagnosis Delay in treatment

Risk Factors for disease progression Recent infection (first 2 years) Smoking Long term corticosteroid use (15 mg/day>4 weeks) Sequel infiltration (simon foci) To be <5 -10 % of the ideal body weight To be in 0 -5 or old age group

HIV Diabetus mellitus Silikosis Kr. Malabsorbtion Organ Transplant. Chronic renal failure Gastrectomy Jejunoileal by-pass Iv drug abuse Leukemia, lymphoma Head and neck cancers Immunosuppressive treatment

World tb 1/3 of the world population is infected with tb 8 million new tb cases are detected each year 1, 5 million people die from tb Starwing, poverty, war, immigration, HIV infection cause the difficulties in disease control

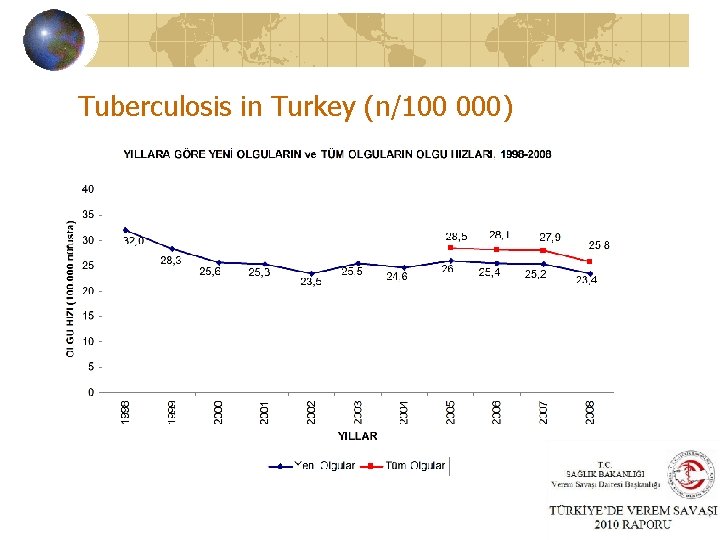
Tuberculosis in Turkey (n/100 000)

Diagnosis History Physical examination Chest x ray Microbiology or pathology Tuberculin test (PPD) diagnostic) (Gold Standart) (Not definitive

Symptoms Pulmonary Cough > 3 weeks Sputum and Hemopthysis Chest pain, side pain Breathlessnes Hoarseness General Fatique Loss of appetide and weight Fever Night sweats

Clinical Presentation Primary Tuberculosis Usually asymptomatic Contact history + PPD Typical radiology Complications Postprimary Tuberculosis Typical symptoms Typical radiology
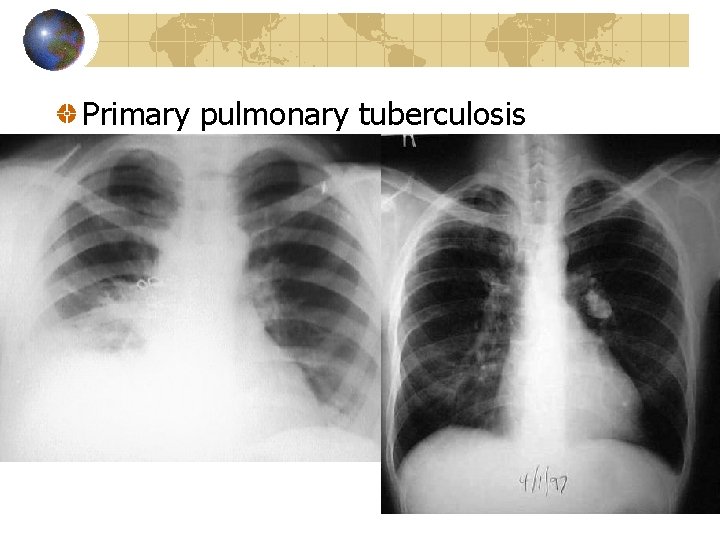
Primary pulmonary tuberculosis
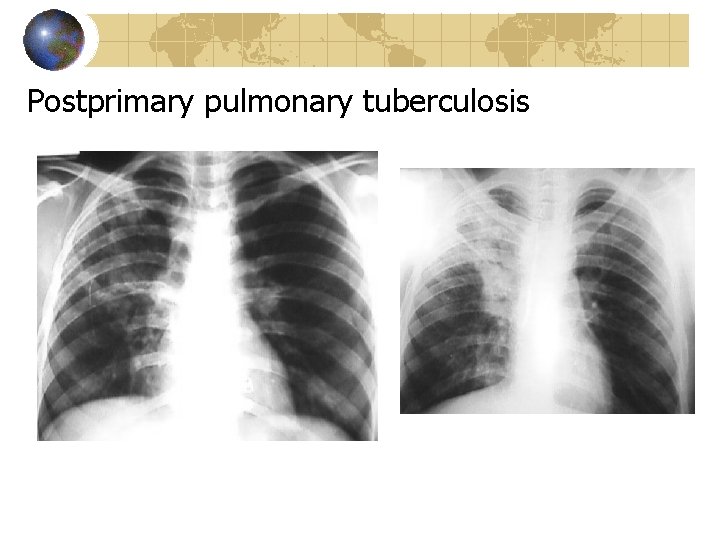
Postprimary pulmonary tuberculosis


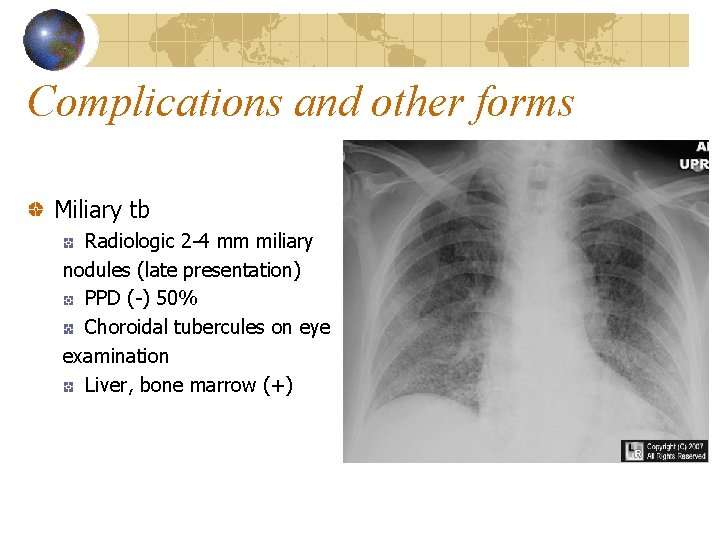
Complications and other forms Miliary tb Radiologic 2 -4 mm miliary nodules (late presentation) PPD (-) 50% Choroidal tubercules on eye examination Liver, bone marrow (+)

Pleural tb Mainly seen in young adults PPD (-) 30% AFB in pleural fluid (+) 2 -10% Exudative effusion, lymphocyte predominance, low glucose, low mesothelial cells, high ADA

Tb lymphadenitis Frequently cervical LAP Fistulization may occur No tenderness Bone tb Vertebral tb (pott) Absscess among the muscless (Psoas) Monoartritis

Physical examination Signs in respiratory system: No signs specific to tuberculosis Occasionaly localised/ posttusive crackles General signs: Erythema nodosum Fluctenular conjunctivitis Lymphadenitis
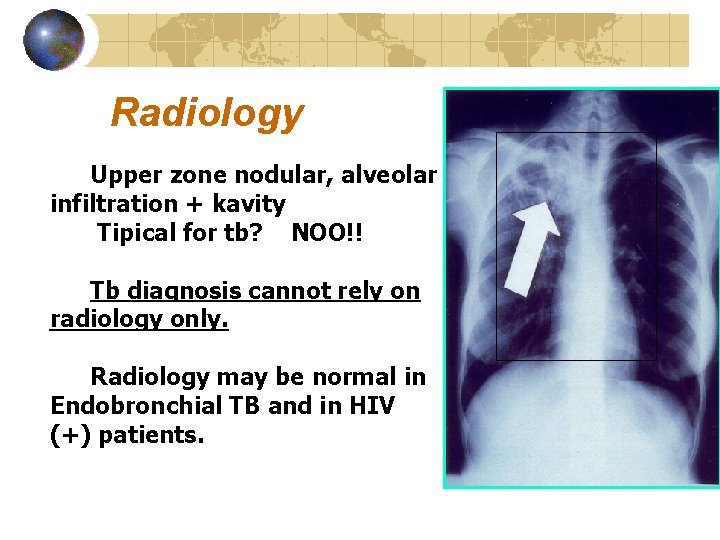
Radiology Upper zone nodular, alveolar infiltration + kavity Tipical for tb? NOO!! Tb diagnosis cannot rely on radiology only. Radiology may be normal in Endobronchial TB and in HIV (+) patients.

Bacteriology Microscopy: Minimum 3 sputum smear should be performed. Culture: Gold standard in diagnosis. Drug sensitivity tests: Performed in Referans laboratory.

Reporting of tb cases is mandatory!!.

Definitions Localization of tb disease Bacteriologic condition Previous treatment history

Localization of TB disease Lung paranchyma Pulmonary TB All tb forms without lung involvement Extrapulmonary TB Pulmonary and extrapulmonary together Pulmonary and extrapulmonary TB

Bacteriology Smear positive case Smear negative case

Smear positive case A patient whose sputum smear is positive for AFB in at least 2 specimens One AFB positivity in sputum smear with a clinicians judgement that the patient’s clinical and/or radiological signs and/or symptoms are compatible with tb One AFB positivity in sputum smear with positive culture

Smear negative case Smear negative in specimens examined twice in 2 weeks time but radiological signs compatible with active tb and no clinical or radiological response to 1 week nonspecific antibiotic treatment This decision should be made hospital based with all the differential diagnostic examination!

Treatment History New Case Relaps Treatment Failure Treatment after interruption Chronic case

New Case A patient who has never had drug treatment for tb or who has taken antitb drugs for<4 weeks Relapse A patient who has been declared cured of any form of tb in the past and has developed sputum smear or culture positive disease

Treatment First line antitb drugs INH RIF PZA EMB SM Second line antitb drugs Thiacetasone PAS Cycloserine Ethionamide Canamycin Capreomycin

Principles of Treatment Combination Therapy (6 months) 4 or 5 drugs in the initial phase; 2 or 3 drugs in the continuation phase Adequate dose and duration of treatment to avoid relaps Regular drug intake Start the tx immediately after the diagnosis
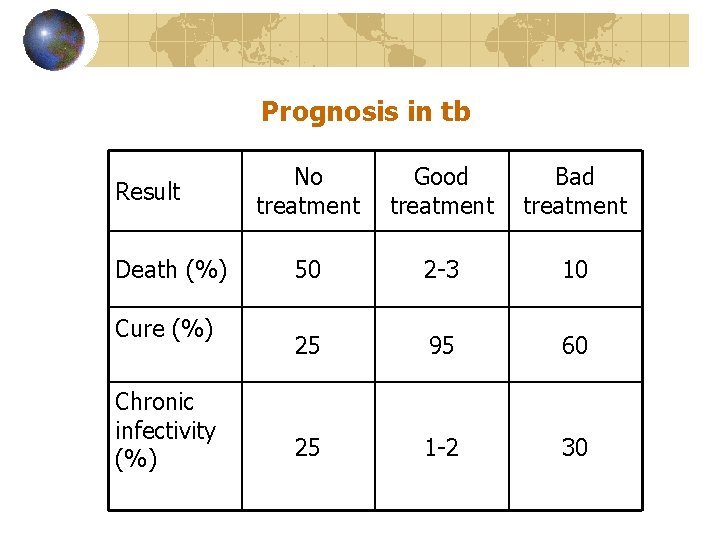
Prognosis in tb Result Death (%) Cure (%) Chronic infectivity (%) No treatment Good treatment Bad treatment 50 2 -3 10 25 95 60 25 1 -2 30

Prevention Efective Treatment of infectious cases Kemoprophylaxis (INH 6 -9 months) BCG Infection control measures (institutions)

Tuberculin skin test (PPD) BCG (+) 0 -5 mm Negative 6 -14 mm due to BCG 15 mm < Positive (infection) BCG (-) 0 -5 mm Negative If 6 -9 mm repeat test 1 week later, again 6 -9 mm Negative, 10 mm < Positive 10 mm< Positive

Kemoprophlaxis without known contact PPD (+), <15 years age New infection PPD convertion Being + in the last 2 years time or 6 mm increased enduration Sequel fibrotic lesion on chest x ray <35 years age, no history of treatment Immunodeficient PPD (+) person PPD (+) that will receive immunosuppressive treatment PPD: positive if >=5 mm

Contact with TB patients People <35 years age Kemoprophylaxis for 6 months, in children <6 years age if PPD (-) in the end of treatment BCG vaccination Kemoprophylaxis: INH 300 mg/day 6 -9 months

Thank you
- Slides: 46