Tuberculosis other mycobacterial infections II Assoc Prof Meral

Tuberculosis & other mycobacterial infections II Assoc Prof Meral Sönmezoğlu Division of Infectious Diseases Yeditepe University Hospital

Tuberculosis • Important new findings at the global level are: • The absolute number of TB cases has been falling since 2006 (rather than rising slowly as indicated in previous global reports); • TB incidence rates have been falling since 2002 (two years earlier than previously suggested); • Estimates of the number of deaths from TB each year have been revised downwards; • In 2009 there were almost 10 million children who were orphans as a result of parental deaths caused by TB.

Tuberculosis • In 2010, there were 8. 8 million (range, 8. 5– 9. 2 million) incident cases of TB, • 1. 1 million (range, 0. 9– 1. 2 million) deaths from TB among HIV-negative people and • an additional 0. 35 million (range, 0. 32– 0. 39 million) deaths from HIV-associated TB.

Tuberculosis: current problems • About 3. 8 million cases per year; 90% (and 98% of the 3 million deaths) are in developing countries • Multidrug resistance (“MDR-TB”) • AIDS: atypical presentations and distribution • Nosocomial spread • Foreign-born

Millennium Development Goals set for 2015 Goal : Combat HIV/AIDS, malaria and other diseases Target: Halt and begin to reverse the incidence of malaria and other major diseases Indicator: Incidence, prevalence and death rates associated with TB Indicator: Proportion of TB cases detected and cured under DOTS Stop TB Partnership targets set for 2015 and 2050 By 2015: Reduce prevalence and death rates by 50%, compared with their levels in 1990 By 2050: Reduce the global incidence of active TB cases to <1 case per 1 million population per year

• World TB Day 24 th March 1882 when Dr Robert Koch astounded the scientific community by announcing that he had discovered the cause of tuberculosis, the TB bacillus He was presented with the Nobel Prize in Physiology or Medicine in 1905 "for his investigations and discoveries in relation to tuberculosis. " • Themes by • 2013: Stop TB in my lifetime Call for a world free of TB. • 2012: Stop TB in my lifetime Call for a world free of TB. • 2011: On the move against TB: Transforming the fight towards elimination • 2010: On the move against TB: Innovate towards action • 2009: I am stopping TB




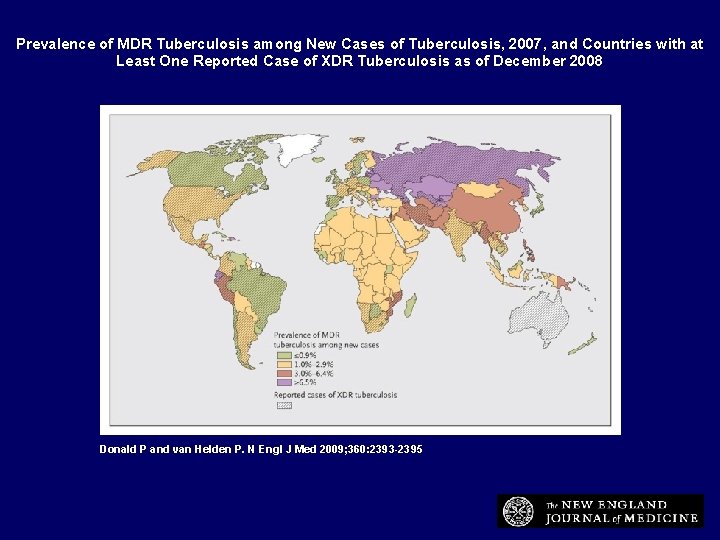
Prevalence of MDR Tuberculosis among New Cases of Tuberculosis, 2007, and Countries with at Least One Reported Case of XDR Tuberculosis as of December 2008 Donald P and van Helden P. N Engl J Med 2009; 360: 2393 -2395
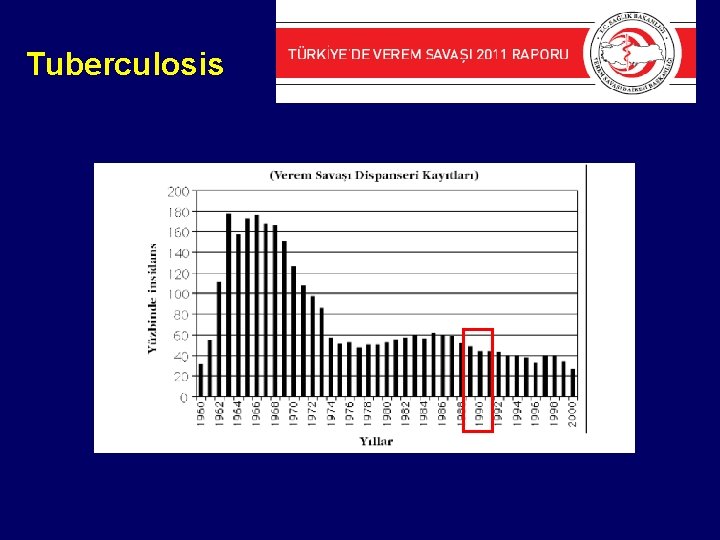
Tuberculosis
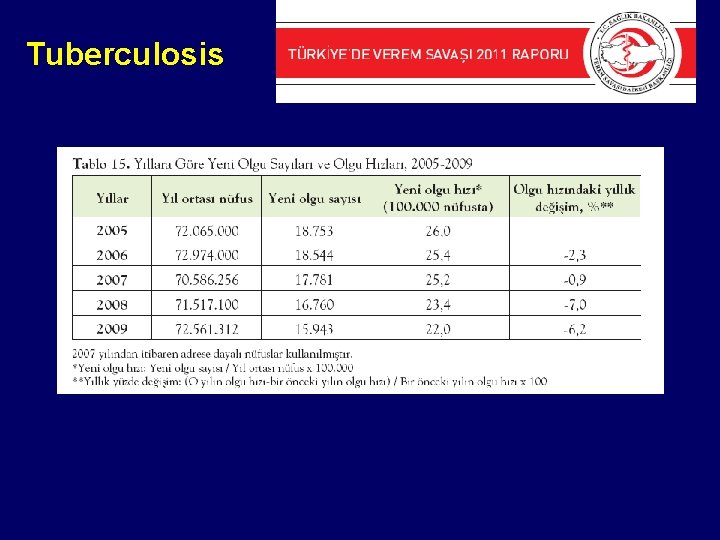
Tuberculosis
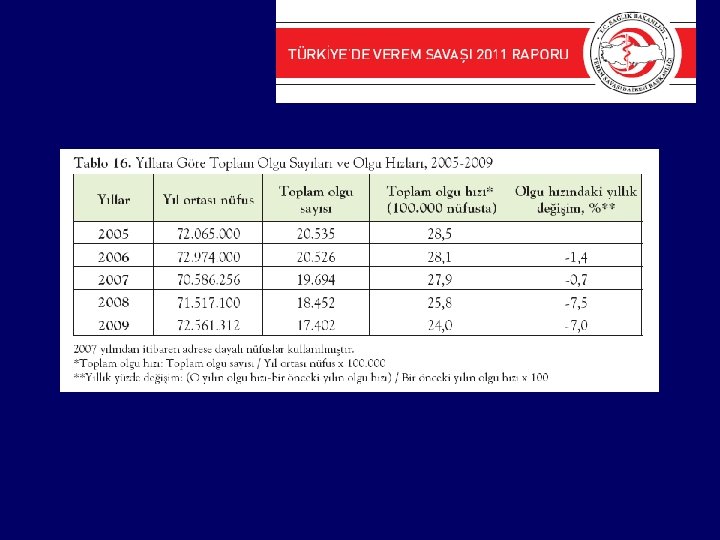
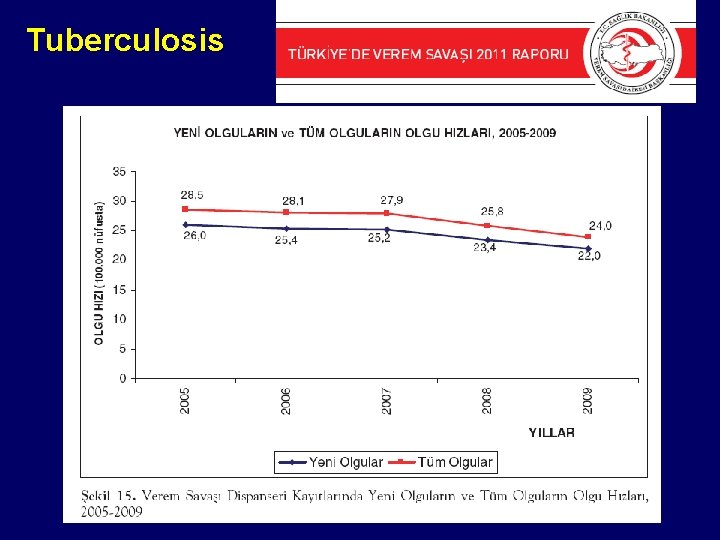
Tuberculosis
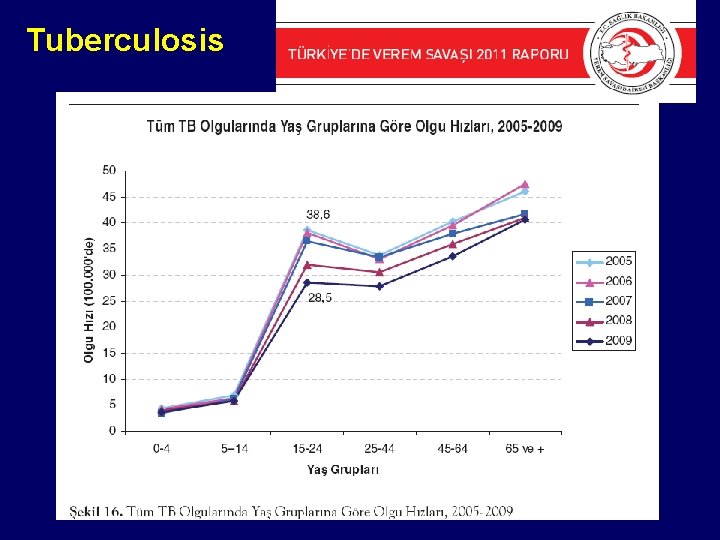
Tuberculosis
Tuberculosis
Tuberculosis
Tuberculosis
Tuberculosis
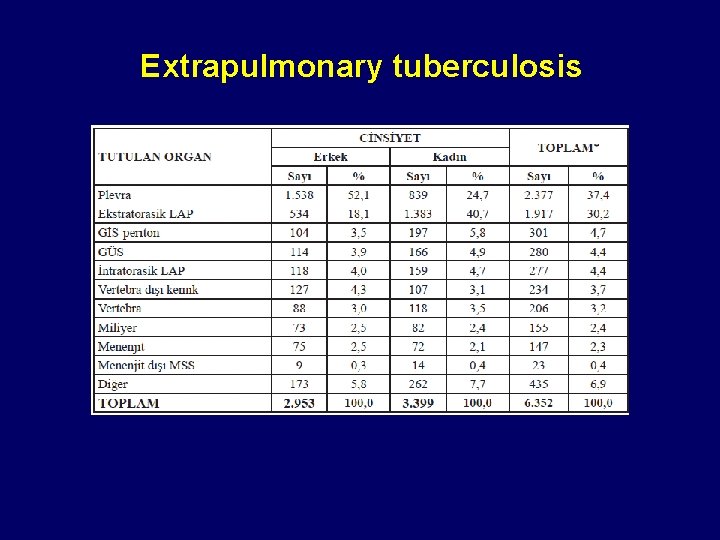
Extrapulmonary tuberculosis
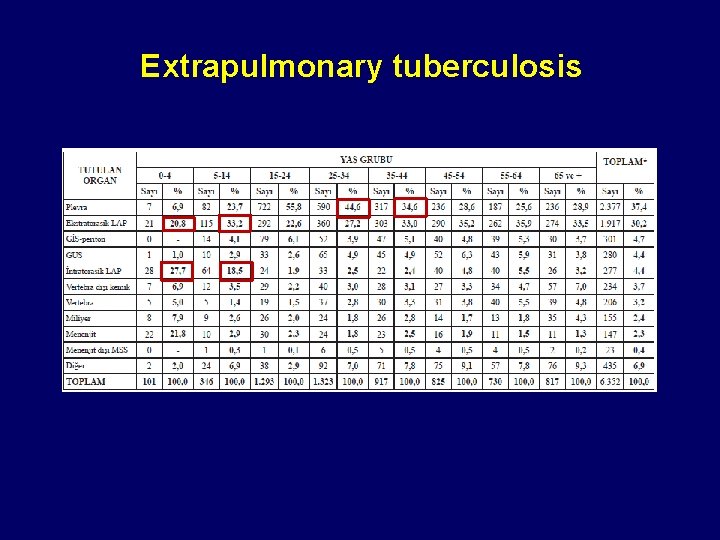
Extrapulmonary tuberculosis

Mycobacterium tuberculosis • MTB is a bacterium belonging to the Mycobacterium genus • Its identification is based on the following characteristics: shape of the colonies, growth rate, and biochemical reactivity. • subdivided in two main groups based on their growth rates (fast vs. slow)

Mycobacterium tuberculosis • The rapidly growing Mycobacterium species (Mycobacterium abscessus, M. fortuitum, M. porcinum), whereas the majority are nonpathogenic • Majority of the slowly growing Mycobacterium species are pathogenic for humans and/or animals (e. g. , all the species of the MTB complex [MTBC], M. leprae, M. ulcerans, M. avium), and only a few of them are nonpathogenic (e. g. , M. terrae, M. gordonae). • MTB complex: MTB (Koch, 1882), M. bovis (Karlsen and Lessel, 1970), M. africanum [25], M. microti (Reed, 1957), “M. canettii’

Mycobacterium tuberculosis • rod-shaped bacteria (0. 2– 0. 6 m wide, 1– 10 m long), nonmotile, nonencapsulated, Grampositive, • aerobes (growing most successfully in tissues with a high oxygen content such as lungs), or facultative anaerobes. • They are facultative intracellular pathogens, usually infecting mononuclear phagocytes (e. g. , macrophages).

Mycobacterium tuberculosis • An obligate aerobe: prefers P 02 of 130 torr • Replicates every 20 hours • Natural resistance to one drug is one in every 105 to 107 cells • Natural resistance to two or more drugs is 1 in every 109 to 1012 cells

Tuberculosis: the basics • The Mycobacterium tuberculosis complex: M. tuberculosis, M. bovis, M. africanum • Transmitted primarily by airborne droplet nuclei • Persons with positive AFB sputum smears are especially effective transmitters • Between 5% and 15% of infected persons will develop active disease (involving any organ) within two years

Tuberculosis: the basics (2) • Populations at increased risk of infection: medically-underserved, low-income groups; immigrants; residents of long-term care or correctional facilities • Infected persons with increased risk of active disease: close contacts of cases; children < 5 years old; persons with chronic diseases (renal failure; silicosis; diabetes); immunosuppressed; HIV-positive persons

Immunology of tuberculosis • Tubercle bacillus + macrophages --> processed antigen • Antigen recognition by lymphocytes --> activated lymphocytes --> lymphokines • Lymphokines--> attraction, stimulation, and retention of macrophages at antigen site • Activated macrophages--> lytic enzymes with mycobactericidal but also tissue-necrosing capacity
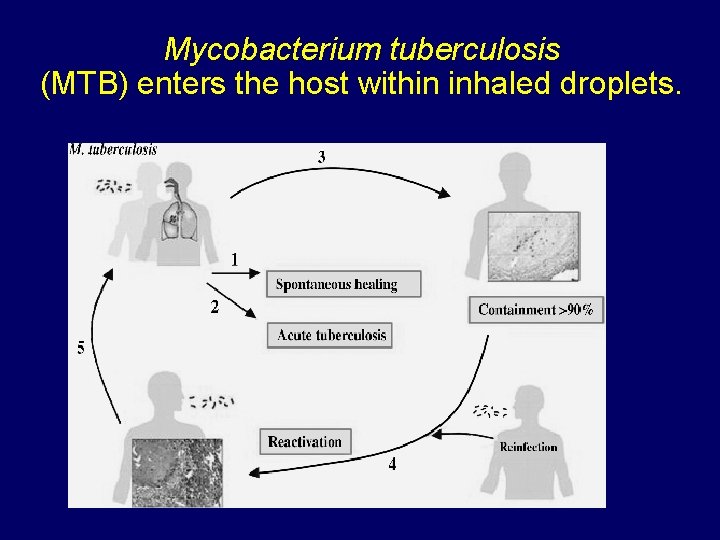
Mycobacterium tuberculosis (MTB) enters the host within inhaled droplets.

Immunology of tuberculosis (2) • Interferon-gamma probably stimulates macrophages to produce interferon-alfa and 1, 25 -dihydroxyvitamin D, both of which are mycobacterial inhibitors • Cytokines secreted by alveolar macrophages: interleukin 1 (fever); interleukin 6 (hyperglobulinemia), and tumor necrosis factor alpha (killing of organisms, granuloma formation, fever and weight loss)
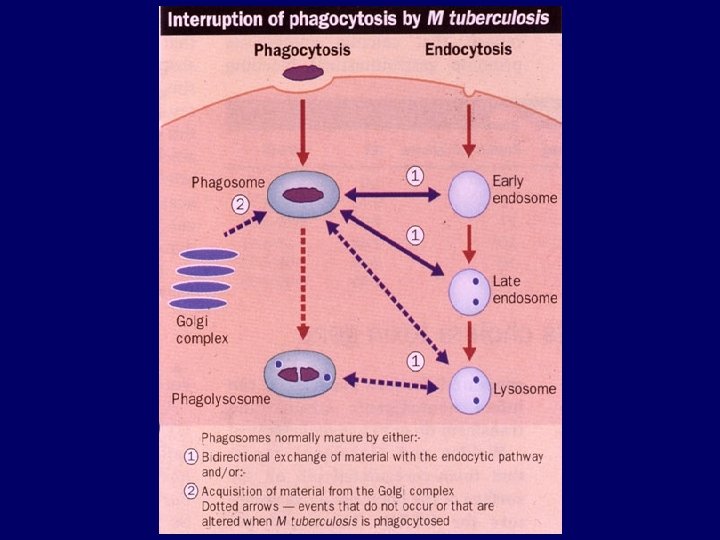

Primary tuberculous infection • Inhalation leads to infection at periphery of middle lung zone • Pneumonia 2 to 6 weeks after infection followed by lymphohematogenous dissemination • Cell-mediated immunity (manifested by positive PPD) usually contains the infection • Some organisms remain viable
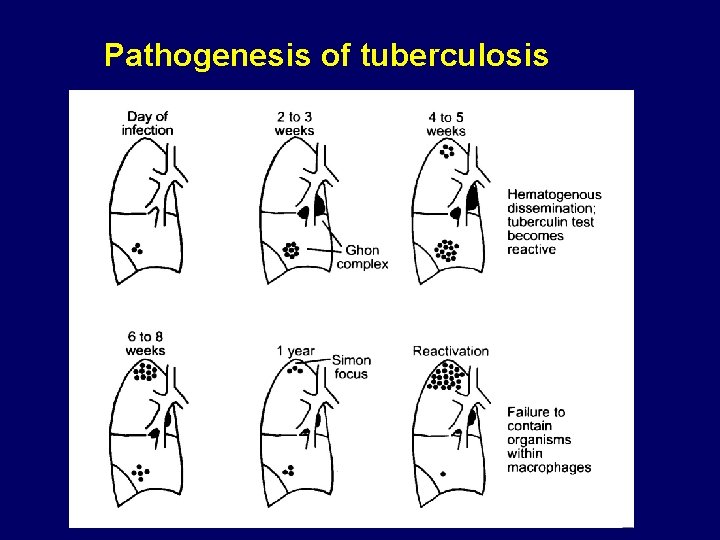
Pathogenesis of tuberculosis

Reactivation of tuberculosis • Occurs most often in persons > 50 years of age; more common in men • Higher risk in elderly persons and in those with malnutrition, diabetes mellitus, post-gastrectomy, immunocompromise, alcoholism, HIV infection, or corticosteroid therapy

Residua of primary infection • Ghon complex (after Anton Ghon, German bacteriologist): calcified peripheral focus of tuberculous infection with calcified regional (hilar) lymph node (also called Ranke complex) • Simon focus (after Georg Simon, German pediatrician): focus at apex of lung, containing viable organisms and manifested on x-ray as “fibrous cap”

Axioms on Simon foci • “If humans did not have apices to their lungs, the tubercle bacillus would not have survived as a human pathogen. ” • “Once a Simon focus has formed, one will eventually die of tuberculosis if something else doesn’t cause death first. ”

Caseous necrosis of tuberculosis • This walled-off, friable, cheesy nodule in the subapical region (a Simon focus) develops from organisms spread hematogenously from the initial focus of infection in the lower half of the lung. Reactivation of this lesion would probably destroy the capsule, and the caseous material would be expectorated leaving a cavity.
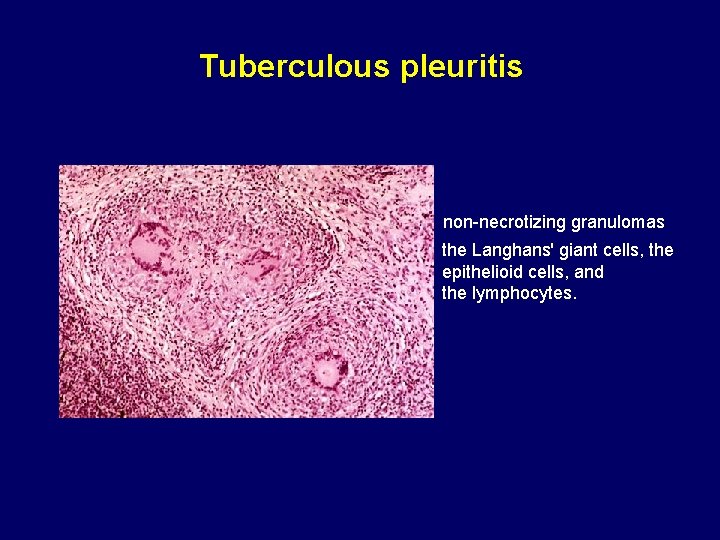
Tuberculous pleuritis non-necrotizing granulomas the Langhans' giant cells, the epithelioid cells, and the lymphocytes.
Progression to active tuberculosis • One year after infection: approximately 5% • Thereafter: approximately 5% (lifetime) • It now seems that many people eventually outlive their tubercle bacilli and are consequently vulnerable to reinfection (Stead, studies in Arkansas, early 1980 s) • Tuberculin-positive persons with HIV infection: risk is 7% to 10% per year

Insights from genotyping of M. tuberculosis isolates (N Engl J Med 2003; 349: 1149 -1155) • Previously, it was thought that 90% of TB cases in industrialized nations resulted from reactivation of infection acquired in remote past. • It now seems that recent transmission causes 40% to 50% of TB cases in urban areas.

The cavity (1) • Formation of the cavity is the pivotal event in the evolution of pulmonary tuberculosis. • Mortality of cavitary pulmonary tuberculosis without treatment approaches 90%. • All therapies prior to 1948 were aimed at closing cavities.
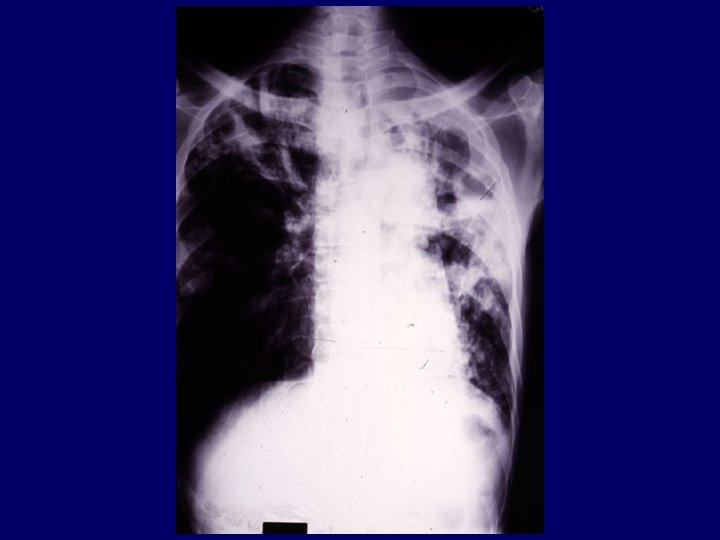
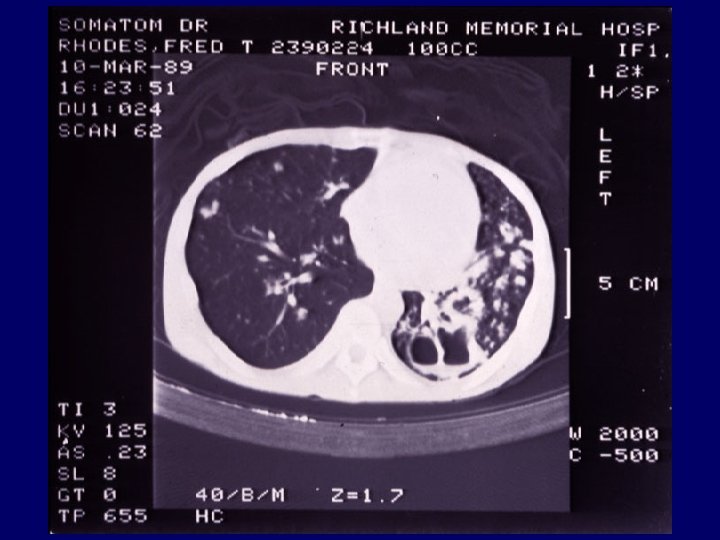

The cavity (2) • Even healed, cavities are unstable. • The walls of cavities contain extensive sheets of bacilli (up to 1011 bacilli/gram). • The cavity is thinnest at the point of penetration of bronchi. • Open cavities may persist for years, constantly draining bacilli into the rest of the bronchial tree.

Complications of pulmonary tuberculosis • Cough, fever, night sweats, weight loss, anemia • Massive hemoptysis (erosion of a vessel in the wall of a cavity; a dilated vessel in a cavity (Rasmussen’s aneurysm; or an aspergilloma) • Progressive pulmonary disease, rarely ARDS • Hyponatremia due to syndrome of inappropriate secretion of antidiuretic hormone (SIADH)

Major syndromes of extrapulmonary tuberculosis • Disseminated (miliary) tuberculosis • “Serosal” tuberculosis (anatomic spaces or cavities): pleurisy, pericarditis, meningitis, peritonitis, arthritis • Tuberculosis of solid organs: renal (genitourinary), osteomyelitis, adrenal glands (Addison’s disease), lymph nodes
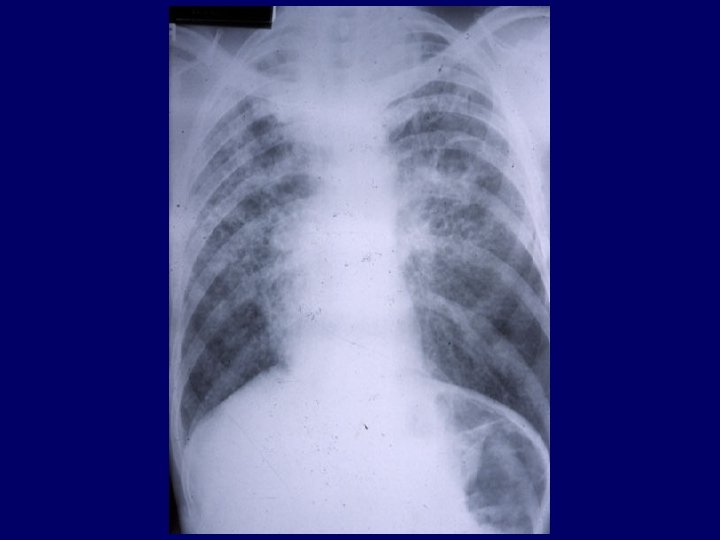


Miliary tuberculosis: diagnostic aids • Repeat physical examination: choroidal tubercles, palpable lymph nodes • Repeat CXR and tuberculin test • Cultures: sputum (up to 63% positive), urine, bone marrow, CSF, gastric aspirate, pleural fluid • Biopsy: palpable nodes, marrow, liver • Therapeutic trial

“Cryptic miliary tuberculosis” • An occult illness with gradual decline in general health • Often no significant fever • Non-reactive tuberculin skin test • Normal chest x-ray
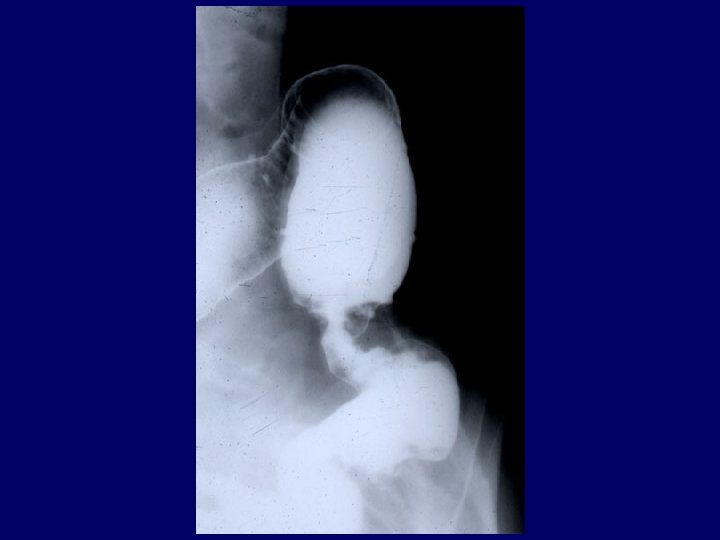
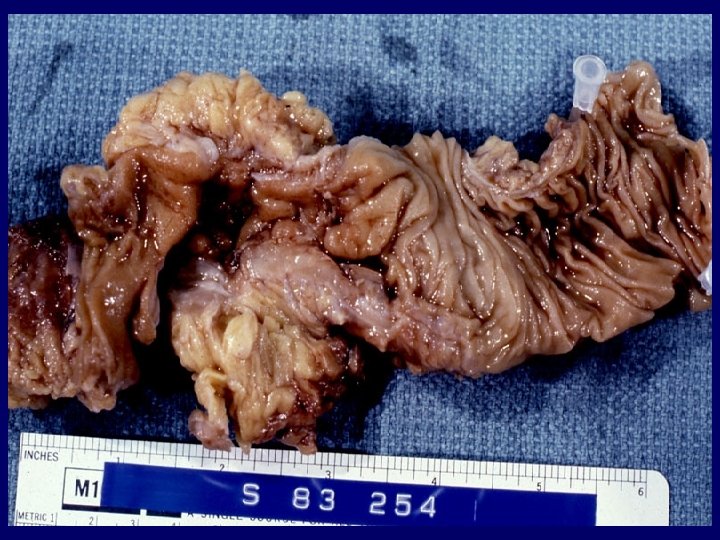
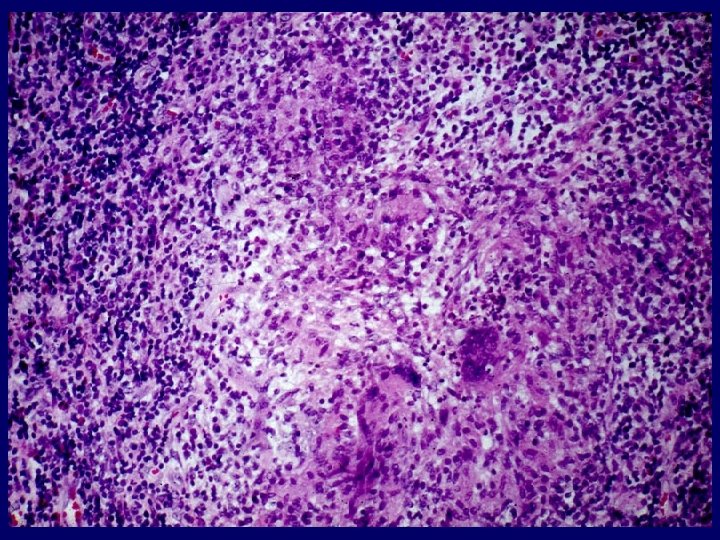

Frequency order of extrapulmonary sites 1. Lymph node 2. Pleura 3. Genitourinary tract 4. Bone and joints 5. Meninges 6. Peritoneum

Tuberculous pleurisy • Subpleural focus ruptures into the pleural space • Usually younger adults, 3 to 7 months after primary tuberculous infection • Abrupt or insidious onset. DDx: pneumonia, pulmonary infarct, tumor, others • Natural history untreated: 65% of 141 patients developed active tbc (Roper & Waring)

Tuberculous meningitis • Rupture of subependymal tubercle into subarachnoid space (“Rich focus”; Rich and Mc. Cormack, 1933) • The intrathecal tuberculin reaction (instillation of PPD material into CSF of PPD-positive volunteers) • Usually occurs within first 6 months of infection; now seen in older adults

Tuberculous pericarditis • Rupture of a tuberculous mediastinal lymph node into the pericardial sac • Mortality 80% to 90% without treatment. Major problems even with appropriate Rx • Diagnosis is difficult to make short of total pericardiectomy • Constrictive pericarditis • Can extend into myocardium --> fiber atrophy

Tuberculous peritonitis • Onset is usually insidious. Mortality 45% to 55% untreated but as low as 0% to 4% with treatment • Polar types: plastic or adhesive type (“doughy abdomen”) and exudative or serous peritonitis with ascites • Presentations: debilitating FUO; chronic abdominal pain; ascites of unknown origin

Tuberculous arthritis • Tuberculous focus in bone ruptures into joint space; trauma predisposes • Adults: spine 50%, hips 15% • Children: Knees 15% • Insidious joint pain and swelling, most often involving large weight-bearing joints • Absence of proteolytic enzymes explains preservation of joint space

Genitourinary tuberculosis • Tubercle of the glomerulus ruptures into the calyceal system • May progress to involve the entire kidney (“autonephrectomy”) and/or may spread throughout the GU tract (prostatitis, epididymitis, salpingitis) • Insidious onset

Tuberculous osteomyelitis § Subchondral osteoporosis with surrounding ring of sclerosis § Spine: anterior involvement of vertebral bodies with disk collapse (Pott’s disease) § Suspect: Monoarticular arthritis of insidious onset; paraspinous mass; back pain

Tuberculosis of the adrenal glands (Addison’s disease) • Tuberculosis formerly the major cause of the disease as described by Thomas Addison (now rare; most common cause is idiopathic [autoimmune]) • Wasting, hyperpigmentation, low blood pressure, hyponatremia, hyperkalemia

Tuberculosis in HIV-positive patients • Present in 5% to 35% of patients diagnosed with AIDS • Precedes diagnosis of AIDS in 67% of patients • Although most of these cases result from reactivation, CXR often resembles progressive primary tuberculosis • Multiple drug resistance a major problem

Diagnosis of TB Disease Medical Evaluation Bacteriologic Examination 69

Bacteriologic Examination Nucleic Acid Amplification Tests (NAA) • NAA tests directly identify M. tuberculosis from sputum specimens by: – Amplifying (copying) DNA and RNA segments • Can help guide clinician’s decision for patient therapy and isolation • Does not replace need for AFB smear, culture, or clinical judgment 70

Bacteriologic Examination Nucleic Acid Amplification Tests (NAA) • If NAA test and AFB smears are positive: – Patients are presumed to have TB and should begin treatment • If NAA test is negative and AFB smears are positive: – Patients may have nontuberculous mycobacteria infection (NTM) 71
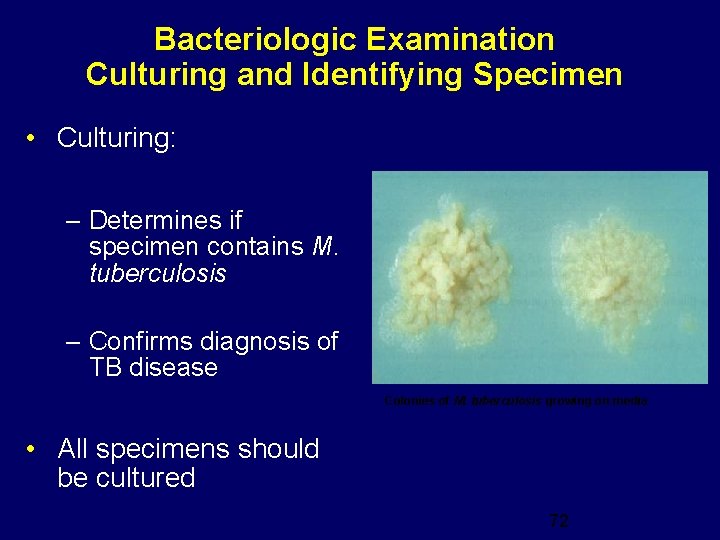
Bacteriologic Examination Culturing and Identifying Specimen • Culturing: – Determines if specimen contains M. tuberculosis – Confirms diagnosis of TB disease Colonies of M. tuberculosis growing on media • All specimens should be cultured 72

Bacteriologic Examination Culturing and Identifying Specimen • Step 1: Detect growth of mycobacteria – Solid media: 3 - 6 weeks – Liquid media: 4 - 14 days • Step 2: Identify organism that has grown – Nucleic acid probes: 2 - 4 hours – Biochemical tests: 6 - 12 weeks 73

AFB smears • Three morning specimens • Fluorescent methods are more sensitive than traditional Kinyoun or Ziehl-Neelsen method • Predictive value of a positive test decreases strikingly as prevalence of the disease decreases (Bayes’ s theorem)
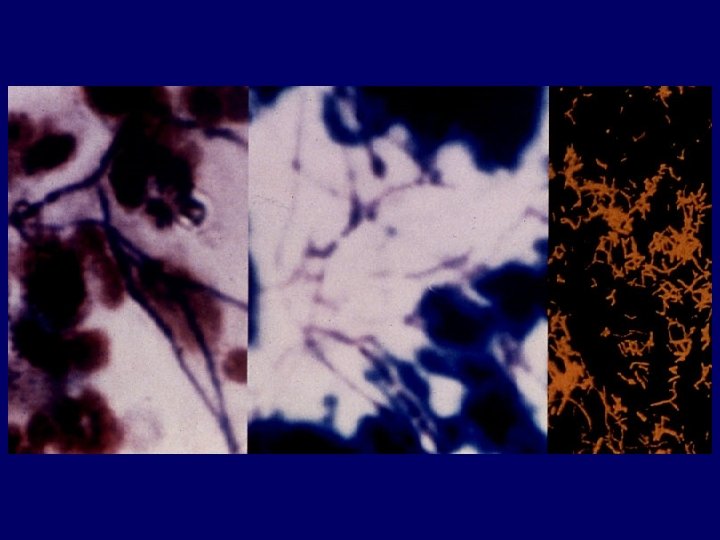
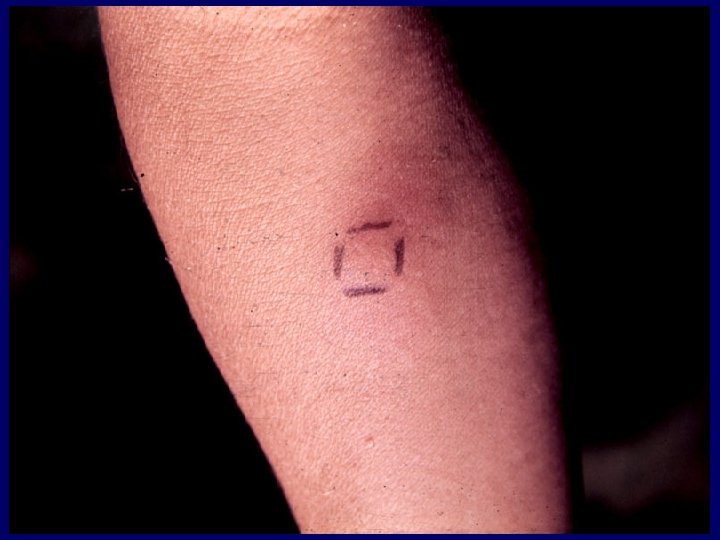
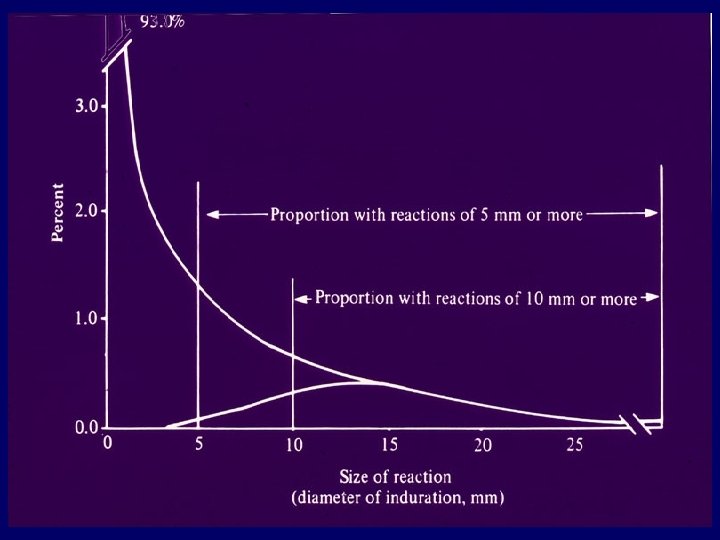

Tuberculin skin test guidelines • 5 mm for close contacts; for persons with compatible chest x-rays; and for HIV-infected persons • 10 mm for recently-infected persons, persons with high-risk medical conditions, and high-risk patients under 35 years of age • 15 mm for low-risk persons under age 35

Rapid laboratory confirmation • Fluorochrome smear on concentrated specimens • Rapid methods of detection: Bactec system; polymerase chain reaction • Rapid mechanisms of identification: DNA probes; HPLC • Rapid methods of susceptibility testing • Handle reports as critical laboratory values

Nontuberculous mycobacteria (NTM) • Synonyms: atypical mycobacteria, mycobacteria other than tuberculosis (MOTT), nontuberculous mycobacteria (NTM) • Numerous species; widespread • Can be difficult to treat • “MAC” = M. avium-intracelluare complex

Pulmonary disease due to NTM in immunocompetent persons • Isolation of organism from sputum does not necessarily imply disease • M. avium-intracelluare (especially in the Southeast) and M. kansasii (especially in the west) cause disease resembling tuberculosis (clinically milder but more difficult-to-treat)
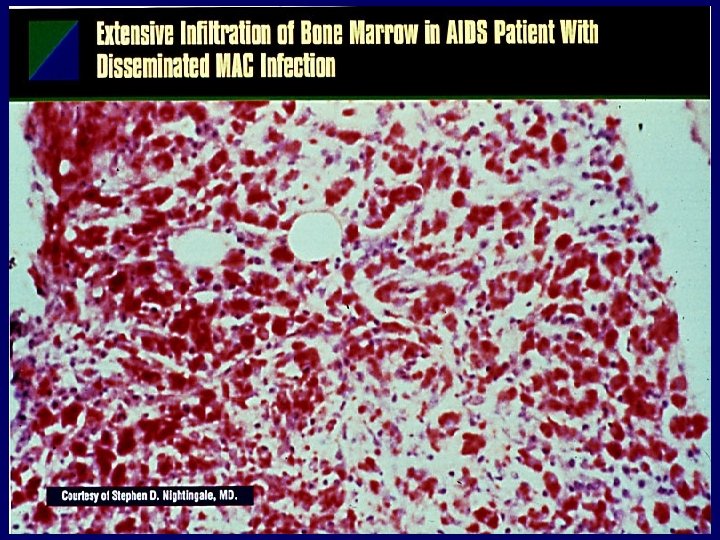

Mycobacterium avium-intracelluare (“MAC”) in HIV disease • Disseminated “MAC” infection with or without pulmonary involvement • Prolonged fever, weight loss, hepatosplenomegaly, diarrhea, abdominal pain • Positive blood cultures; AFB also found in bone marrow, liver, and often stool

Lymphadenitis due to NTM • Usually due to M. scrofulaceum or M. avium-intracelluare • “Scrofula”: cervical lymphadenitis, usually in children • Usual treatment of choice: surgical excision without chemotherapy
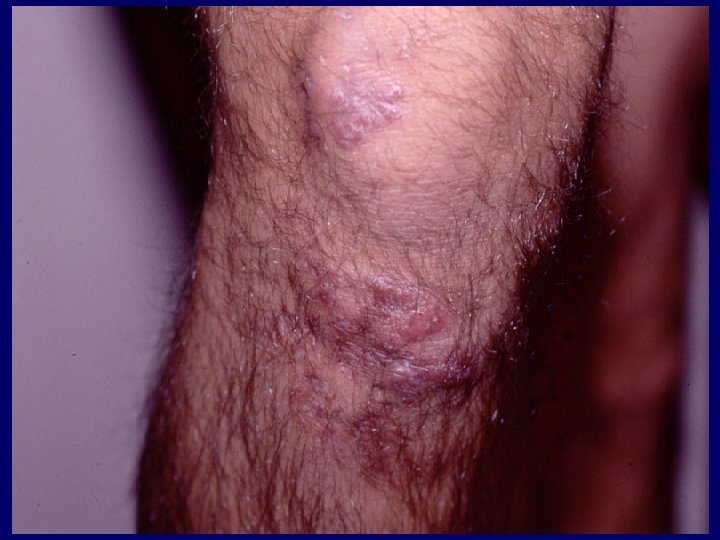

Swimming pool and fish-tank granuloma • Caused by Mycobacterium marinum • Small violet nodule or pustule at the site of minor trauma may evolve into crusted ulcer or abscess • Multiple lesions can resemble lymphocutaneous sporotrichosis
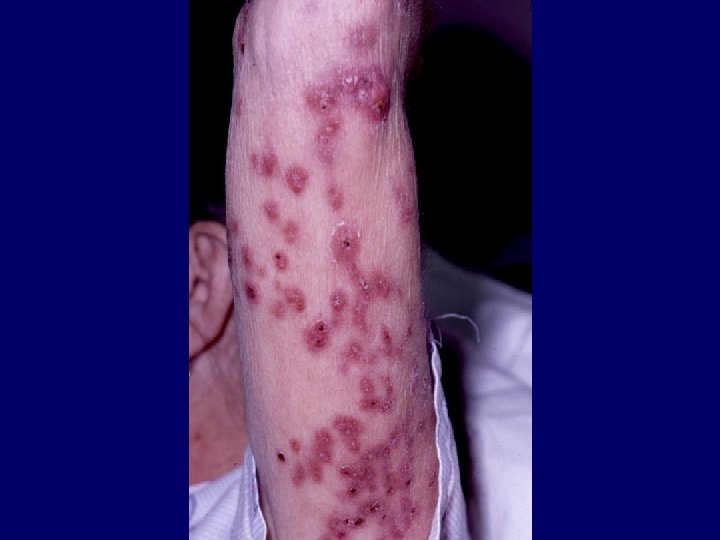

Infections related to injections or surgery • “M. fortuitum complex”: Mycobacterium fortuitum, M. chelonae, M. abscessus (all “rapidly-growing mycobacteria”) • Opportunistic pathogens causing wound infections (which can be epidemic) and skin infections

Fundamental Responsibility and Approach in TB Treatment • Provider (or program) responsible for prescribing appropriate regimen AND ensuring successful completion of therapy • Directly observed therapy (DOT) with patientcentered case management is preferred approach

Antituberculosis Drugs First-Line Drugs Second-Line Drugs • Isoniazid • Streptomycin • Rifampin • Cycloserine • Pyrazinamide • p-Aminosalicylic acid • Ethambutol • Ethionamide • Rifabutin* • Amikacin or kanamycin* • Rifapentine • Capreomycin • Levofloxacin* • Moxifloxacin* • Gatifloxacin* * Not approved by the U. S. Food and Drug Administration for use in the treatment of TB

Drug Abbreviations Ethambutol EMB Isoniazid INH Pyrazinamide PZA Rifampin RIF Rifapentine RPT Streptomycin SM

TUS 2012 • Çocukluk döneminde akciğer dışı tüberkülozun en sık görülen şekli aşağıdakilerden hangisidir? • A) Tüberküloz menenjit B) Renal tüberküloz C) Tüberküloz lenfadenit D) Tüberküloz peritonit E) Tüberküloz perikardit

TUS 2012 • Çocukluk döneminde akciğer dışı tüberkülozun en sık görülen şekli aşağıdakilerden hangisidir? • A) Tüberküloz menenjit B) Renal tüberküloz C) Tüberküloz lenfadenit D) Tüberküloz peritonit E) Tüberküloz perikardit

TUS 2012 • Tüberküloz enterit, bağırsakta en sık aşağıdaki lokalizasyonların hangisinde görülür? • A) Duodenum B) Proksimal-orta jejunum C) Sigmoid kolon ve rektum D) Transvers kolon E) Distal ileum ve çekum

TUS 2012 • Tüberküloz enterit, bağırsakta en sık aşağıdaki lokalizasyonların hangisinde görülür? • A) Duodenum B) Proksimal-orta jejunum C) Sigmoid kolon ve rektum D) Transvers kolon E) Distal ileum ve çekum

TUS 2012 • Antitüberküloz tedavi alan bir hastada gelişen hepatotoksisiteden sorumlu olma ihtimali en az olan ilaç aşağıdakilerden hangisidir? • A) Rifampisin • B) İzoniazid • C) Etambutol • D) Pirazinamid • E) Rifabutin

TUS 2012 • Antitüberküloz tedavi alan bir hastada gelişen hepatotoksisiteden sorumlu olma ihtimali en az olan ilaç aşağıdakilerden hangisidir? • A) Rifampisin • B) İzoniazid • C) Etambutol • D) Pirazinamid • E) Rifabutin

TUS 2012 • Aşağıdaki hastalıklardan hangisinde kapalı plevralbiyopsinin tanı değeri en yüksektir? • A) Tüberküloz plörezisi B) Romatoid artrite bağlı plörezi C) Şilotoraks D) Parapnömonik efüzyon E) Asbest’e ikincil efüzyon

TUS 2012 • Aşağıdaki hastalıklardan hangisinde kapalı plevral biyopsinin tanı değeri en yüksektir? • A) Tüberküloz plörezisi B) Romatoid artrite bağlı plörezi C) Şilotoraks D) Parapnömonik efüzyon E) Asbest’e ikincil efüzyon
- Slides: 99