Tuberculosis Infection and Pathogenesis EPID 816 September 16

Tuberculosis Infection and Pathogenesis EPID 816 September 16, 2016

Topics q Etiology q Pathogenesis q q § LTBI § Active TB Natural history of infection LTBI – revisiting and revising concept

Etiology of Tuberculosis Mycobacterium tuberculosis complex: M. Tuberculosis - 90% TB in man, rarely in other mammals, except for dogs M. bovis - Main cause in cattle TB, also infect various other mammals, including humans, dogs, cats and pigs. M. africanum – cause human TB, primarily in Africa. M. microti - cause TB in voles and cats M. avium-intracellulare complex (MAC): Cause TB in birds, and can also infect man (immune compromised), dogs and cats.

Co-adaptation of pathogen and human host has resulted in distinct genetic lineages of Mtb Wirth, et al. PLo. S Pathog. 2008 Sep 19; 4(9): e 1000160
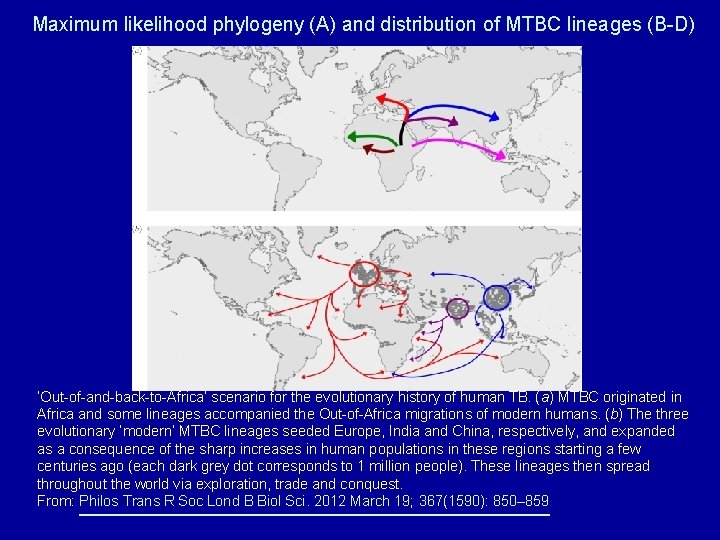
Maximum likelihood phylogeny (A) and distribution of MTBC lineages (B-D) ‘Out-of-and-back-to-Africa’ scenario for the evolutionary history of human TB. (a) MTBC originated in Africa and some lineages accompanied the Out-of-Africa migrations of modern humans. (b) The three evolutionary ‘modern’ MTBC lineages seeded Europe, India and China, respectively, and expanded as a consequence of the sharp increases in human populations in these regions starting a few centuries ago (each dark grey dot corresponds to 1 million people). These lineages then spread throughout the world via exploration, trade and conquest. From: Philos Trans R Soc Lond B Biol Sci. 2012 March 19; 367(1590): 850– 859
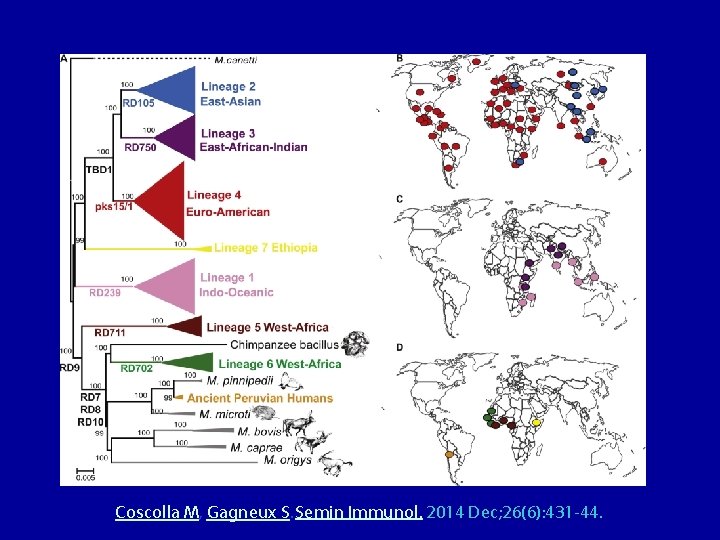
Coscolla M, Gagneux S. Semin Immunol. 2014 Dec; 26(6): 431 -44.
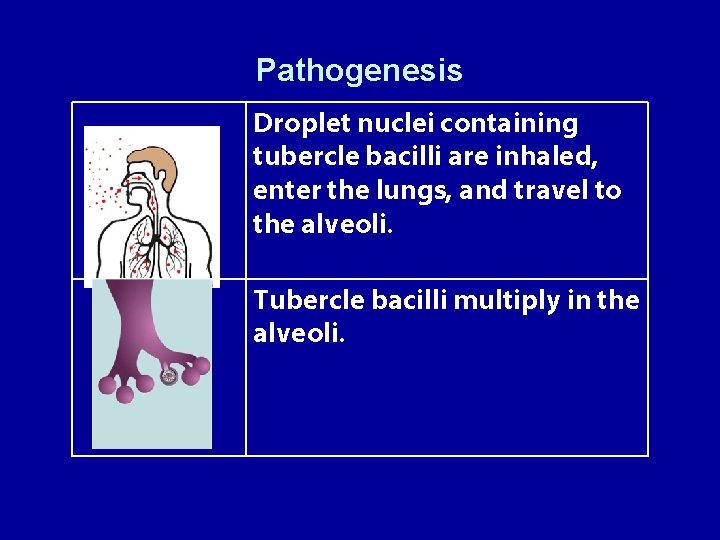
Pathogenesis Droplet nuclei containing tubercle bacilli are inhaled, enter the lungs, and travel to the alveoli. Tubercle bacilli multiply in the alveoli.
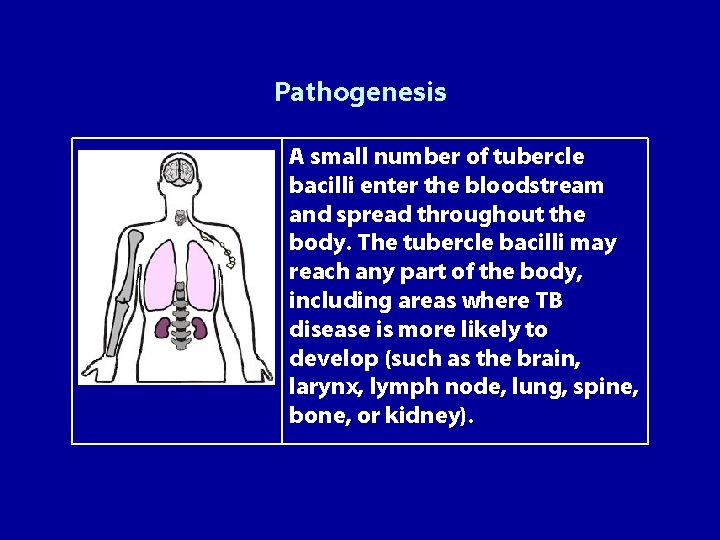
Pathogenesis A small number of tubercle bacilli enter the bloodstream and spread throughout the body. The tubercle bacilli may reach any part of the body, including areas where TB disease is more likely to develop (such as the brain, larynx, lymph node, lung, spine, bone, or kidney).
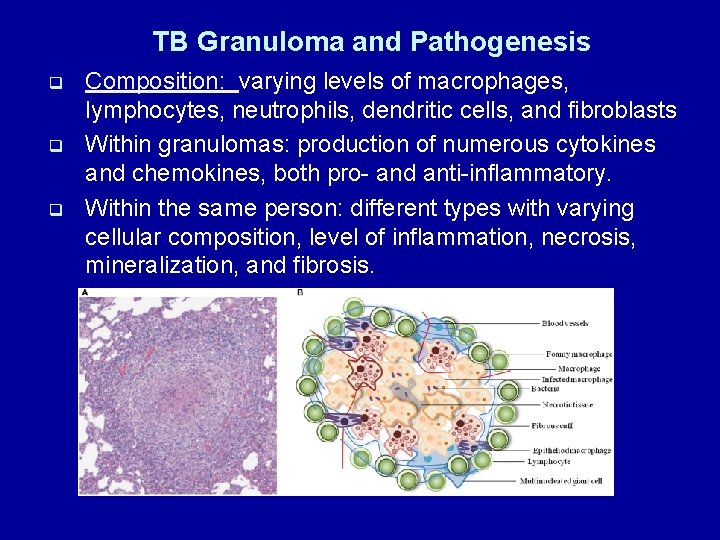
TB Granuloma and Pathogenesis q q q Composition: varying levels of macrophages, lymphocytes, neutrophils, dendritic cells, and fibroblasts Within granulomas: production of numerous cytokines and chemokines, both pro- and anti-inflammatory. Within the same person: different types with varying cellular composition, level of inflammation, necrosis, mineralization, and fibrosis.

TB Granuloma and Pathogenesis q q Serving as an immune microenvironment : § Cells interact to control the infection; § A niche for tubercle bacillus survival § Modulated in part by the bacillus § A balance of pro- and anti-inflammatory factors in granuloma determines the reduction or control of bacterial proliferation (i. e. , control infection) vs. causing excessive inflammation that drives pathology (i. e. lung damage). Understanding the interaction of various cell types in granulomas is the key to elucidating mechanisms of host protective immunity.
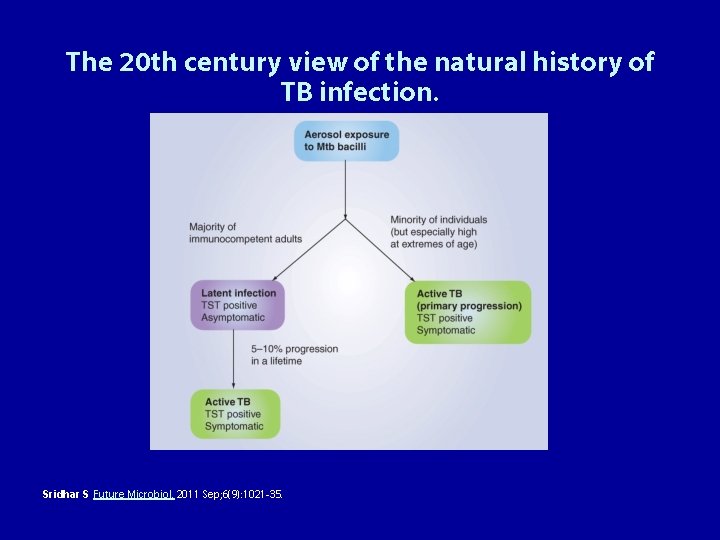
The 20 th century view of the natural history of TB infection. Sridhar S Future Microbiol. 2011 Sep; 6(9): 1021 -35.

Redefining the natural history of TB infection through immunology. Sridhar S Future Microbiol. 2011 Sep; 6(9): 1021 -35.

Latency “The presence of any tuberculosis lesion which fails to produce symptoms of its presence” Amberson JB. “The significance of latent forms of tuberculosis. N. Engl. J. Med 1938; 219: 572 -6.

Classical Studies of MTB Persistence Corpen HJ, Cohn ML. The viability and virulence of old cultures of tubercile bacilli: Studies on twelve-year broth cultures maintained at incubation temperature. Am. Rev. Tuberc. 1933; 28: 856 -74.

Latency “Once tuberculosis, always tuberculosis. ” J. Infect. Dis. 2002. Lilleback T. Molecular evidence of endogenous reactivation of Mycobacterium tuberculosis after 33 years of latent infect.
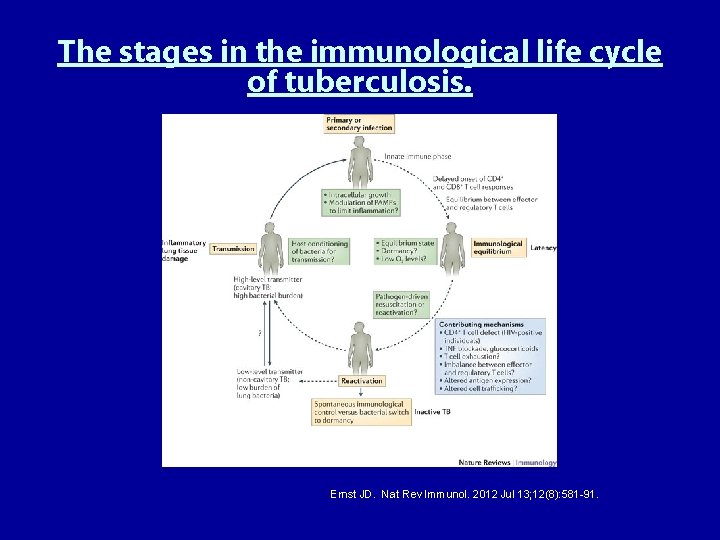
The stages in the immunological life cycle of tuberculosis. Ernst JD. Nat Rev Immunol. 2012 Jul 13; 12(8): 581 -91.
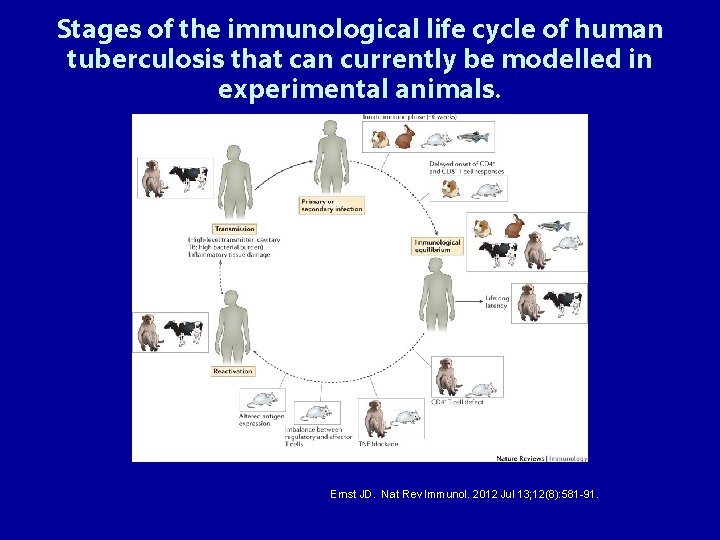
Stages of the immunological life cycle of human tuberculosis that can currently be modelled in experimental animals. Ernst JD. Nat Rev Immunol. 2012 Jul 13; 12(8): 581 -91.

Determinants for TB Infection to Occur q q q Susceptibility of the exposed person Infectiousness of person with TB (i. e. , number of bacilli TB patient expels into the air) Environmental factors that affect the concentration of M. tb organisms Proximity, frequency, and duration of exposure (e. g. , close contacts) Can be transmitted from children, though less likely Transmissibility of M. tb strains

TB Disease q q In some, the granulomas break down, bacilli escape and multiply, resulting in TB disease Can occur soon after infection, or years later Persons with TB disease are usually infectious and can spread bacteria to others Positive M. tb culture confirms TB diagnosis

Risk of Developing Disease Normal Immune System q q Untreated, 5% of infected persons with normal immunity develop TB in first 1– 2 years post infection, another 5% later in life Thus, about 10% of infected persons with normal immunity will develop TB at some point in life if not treated

Risk of Developing Disease (cont. ) Weak Immune System q Persons with weak immunity at increased risk of progressing to TB disease § Untreated HIV infection highest risk factor: risk of developing TB disease is 7%– 10% each year; § Children <5 years of age also at increased risk

Sites of Disease q q q Lungs (pulmonary): most common site; usually infectious Miliary: occurs when bacilli spread to all parts of the body; rare, but fatal if untreated Central nervous system: usually occurs as meningitis, but can occur in brain or spine

Sites of Disease (cont. ) Outside the lungs (extrapulmonary): usually not infectious, unless person has q Concomitant pulmonary disease, q Extrapulmonary disease in the oral cavity or larynx, or q Extrapulmonary disease with open site, especially with aerosolized fluid.
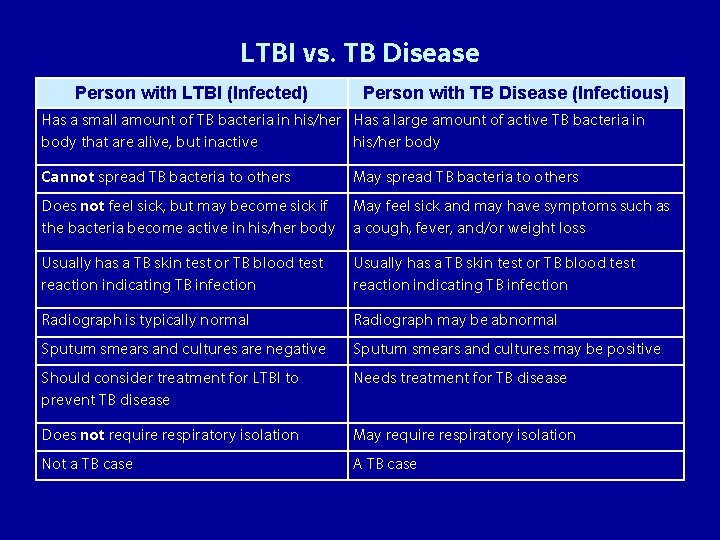
LTBI vs. TB Disease Person with LTBI (Infected) Person with TB Disease (Infectious) Has a small amount of TB bacteria in his/her Has a large amount of active TB bacteria in body that are alive, but inactive his/her body Cannot spread TB bacteria to others May spread TB bacteria to others Does not feel sick, but may become sick if the bacteria become active in his/her body May feel sick and may have symptoms such as a cough, fever, and/or weight loss Usually has a TB skin test or TB blood test reaction indicating TB infection Radiograph is typically normal Radiograph may be abnormal Sputum smears and cultures are negative Sputum smears and cultures may be positive Should consider treatment for LTBI to prevent TB disease Needs treatment for TB disease Does not require respiratory isolation May require respiratory isolation Not a TB case A TB case

Natural history of tuberculosis: duration and fatality of untreated pulmonary tuberculosis in HIV negative patients: a systematic review. PLo. S One. 2011 Apr 4; 6(4): e 17601. Tiemersma EW et. al. BACKGROUND: The prognosis, specifically the case fatality and duration, of untreated tuberculosis is important as many patients are not correctly diagnosed and therefore receive inadequate or no treatment. Furthermore, duration and case fatality of tuberculosis are key parameters in interpreting epidemiological data.

Natural history of tuberculosis: duration and fatality of untreated pulmonary tuberculosis in HIV negative patients: a systematic review. PLo. S One. 2011 Apr 4; 6(4): e 17601. Tiemersma EW et. al. METHODOLOGY AND PRINCIPAL FINDINGS: To estimate the duration and case fatality of untreated pulmonary tuberculosis in HIV negative patients we reviewed studies from the pre-chemotherapy era. Untreated smearpositive tuberculosis among HIV negative individuals has a 10 year case fatality variously reported between 53% and 86%, with a weighted mean of 70%. Ten-year case fatality of culturepositive smear-negative tuberculosis was nowhere reported directly but can be indirectly estimated to be approximately 20%. The duration of tuberculosis from onset to cure or death is approximately 3 years and appears to be similar for smearpositive and smear-negative tuberculosis.

Natural history of tuberculosis: duration and fatality of untreated pulmonary tuberculosis in HIV negative patients: a systematic review. PLo. S One. 2011 Apr 4; 6(4): e 17601. Tiemersma EW et. al. CONCLUSIONS: Current models of untreated tuberculosis that assume a total duration of 2 years until self-cure or death underestimate the duration of disease by about one year, but their case fatality estimates of 70% for smear -positive and 20% for culture-positive smear-negative tuberculosis appear to be satisfactory.

Latent Tuberculosis Infection – Revisiting and Revising Concepts Padmini Salgame et. al. , Tuberculosis Volume 95 (2015), Issue 4, Pages 373– 384 q q q q Outcome (cure, latency, or active disease) of infection with Mtb is determined by a complex interplay of host- and pathogen-specific factors with the environment LTBI is a continuum between self-cure and asymptomatic, yet active TB disease Stage of this continuum is determined by: Strain virulence Intensity of exposure to the index case Size of the bacterial inoculum Host factors (age and co-morbidities) Current diagnosis of LTBI does not reflect the activity of the infectious focus or the risk of progression to active TB.

References q q q CDC Core Curriculum on Tuberculosis: What the Clinician Should Know. Http: //www. cdc. gov/tb/education/corecurr/default. htm Kirschner DE, Young D, Flynn JL. Tuberculosis: global approaches to a global disease. Curr Opin Biotechnol. 2010 Aug; 21(4): 524 -31. Sridhar S, Pollock K, Lalvani A. Redefining latent tuberculosis. Future Microbiol. 2011 Sep; 6(9): 1021 -35. Ernst JD. The immunological life cycle of tuberculosis. Nat Rev Immunol. 2012 Jul 13; 12(8): 581 -91. Tiemersma EW, van der Werf MJ, Borgdorff MW, Williams BG, Nagelkerke NJ. Natural history of tuberculosis: duration and fatality of untreated pulmonary tuberculosis in HIV negative patients: a systematic review. PLo. S One. 2011 Apr 4; 6(4): e 17601. Padmini Salgame et. al. , Tuberculosis Volume 95 (2015), Issue 4, Pages 373– 384
- Slides: 29